Dyslipidemia after Kidney Transplant Fasika M Tedla MD



![Lipoprotein (a) [Lp(a)] • Modified LDL – Higher affinity to macrophages • Homologous to Lipoprotein (a) [Lp(a)] • Modified LDL – Higher affinity to macrophages • Homologous to](https://slidetodoc.com/presentation_image/5507e6cbe12b3e2bac95c08cc87ff3a2/image-12.jpg)





- Slides: 23

Dyslipidemia after Kidney Transplant Fasika M. Tedla, MD, MSc Medical Director of Transplantation Assistant Professor of Medicine SUNY Downstate Medical Center

Outline • • Background Basics of lipoprotein biology Pathophysiology Outcomes of treatment – Non-dialysis CKD – Dialysis – Transplant • Future directions • Summary

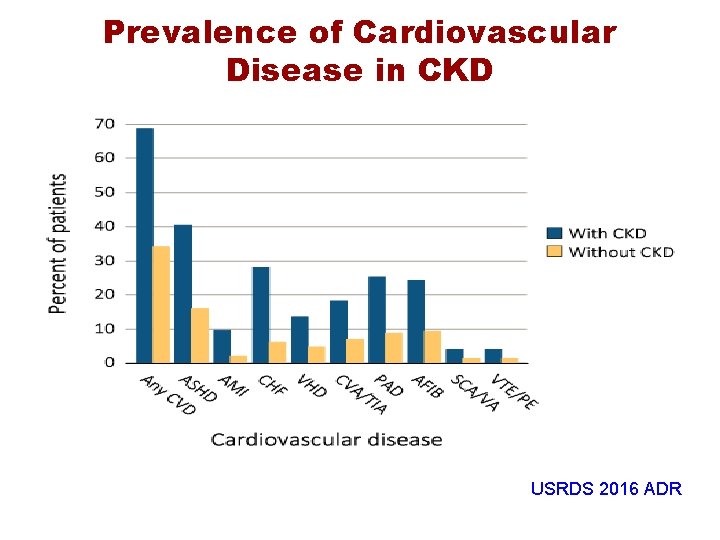
Prevalence of Cardiovascular Disease in CKD USRDS 2016 ADR

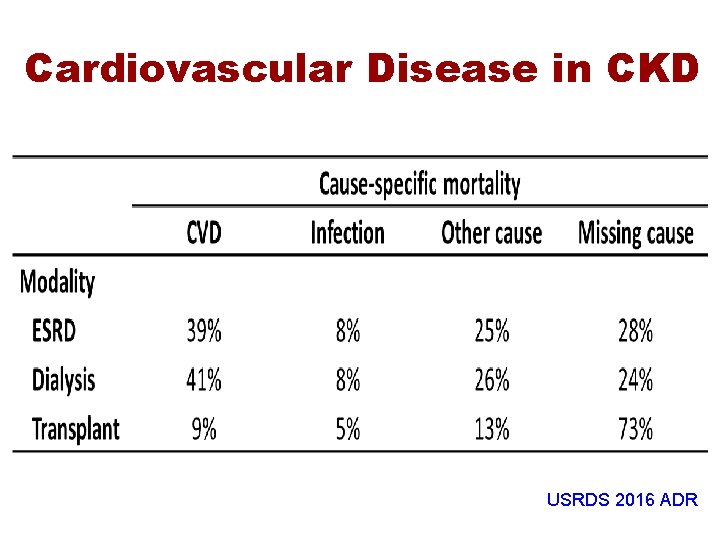
Cardiovascular Disease in CKD USRDS 2016 ADR

Background • 1850’s: • 1901 : - “…plates of cholesterine” – Virchow – Nerking suggested lipids exist in plasma bound to protein • 1950’s: – Biochemical pathway, lipoprotein quantitation – Framingham and other association studies – J-curve • 1980’s: – Cholesterol reduction with sequesterants – ? reduction in cardiovascular mortality • 1990’s - present – HMG-Co. A reductase inhibitors (statins) in tertiary prevention – Statins in secondary prevention – Extension to subpopulations, lower targets

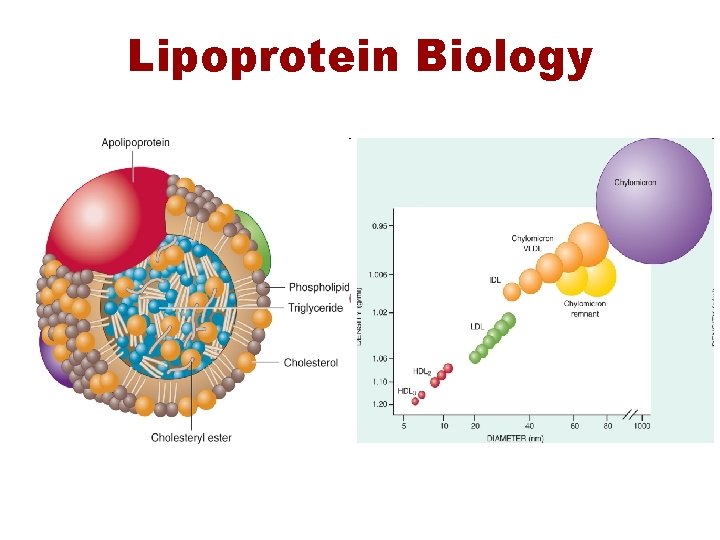
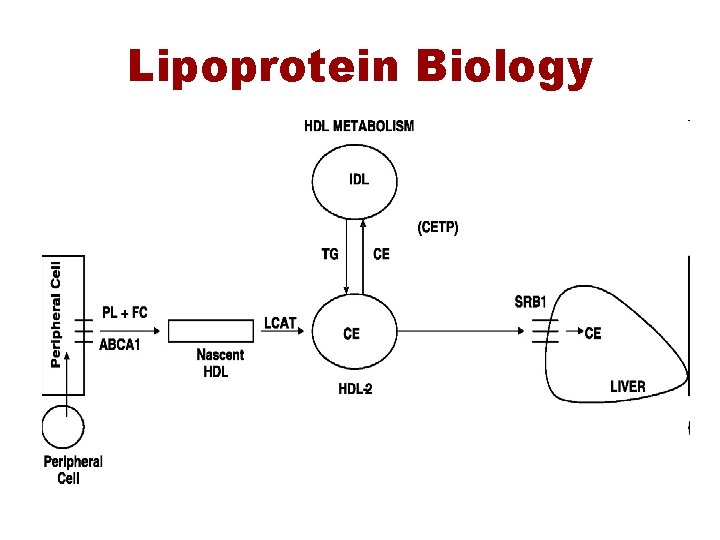
Lipoprotein Biology

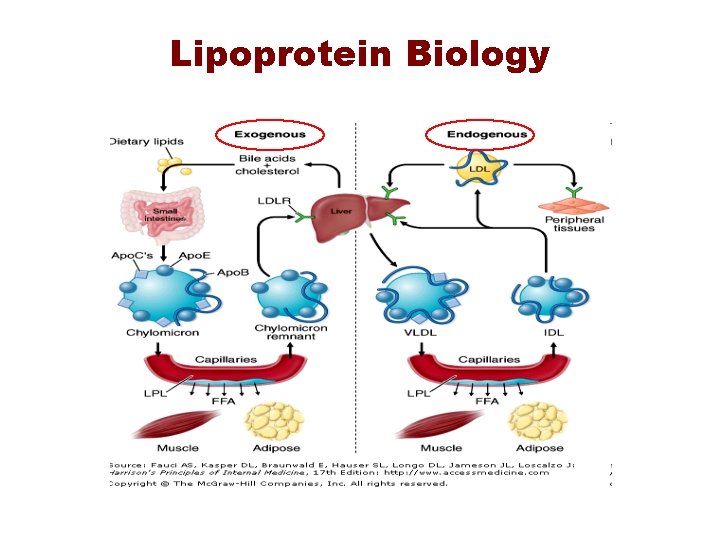
Lipoprotein Biology

Lipoprotein Biology

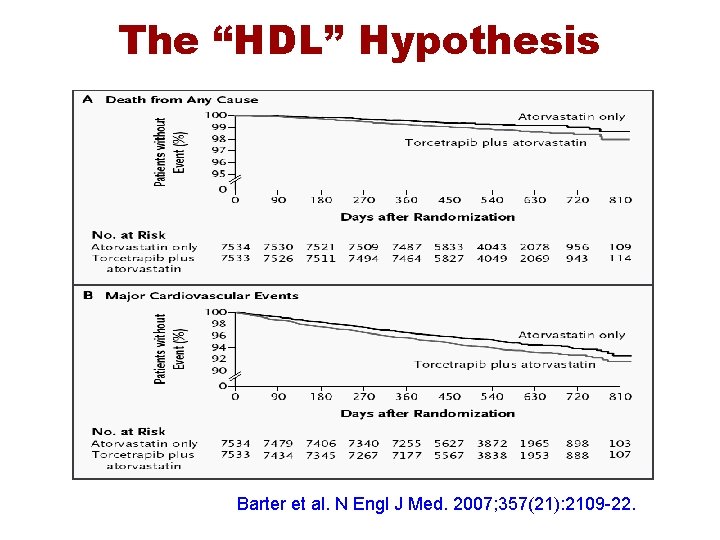
The “HDL” Hypothesis Barter et al. N Engl J Med. 2007; 357(21): 2109 -22.

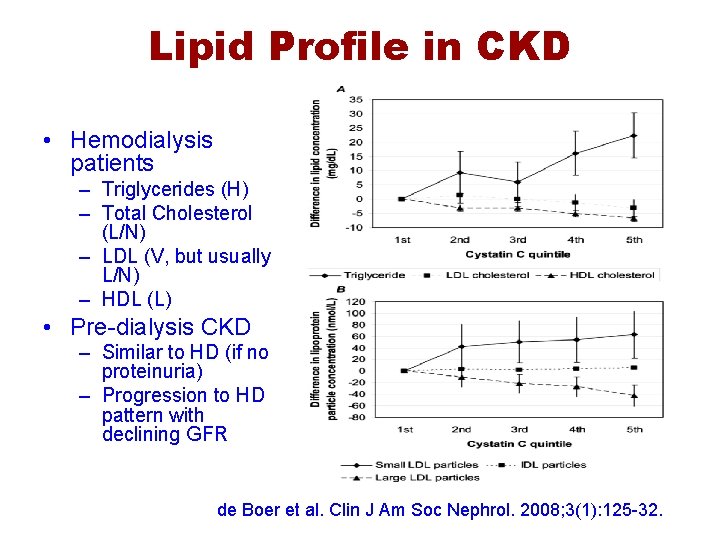
Lipid Profile in CKD • Hemodialysis patients – Triglycerides (H) – Total Cholesterol (L/N) – LDL (V, but usually L/N) – HDL (L) • Pre-dialysis CKD – Similar to HD (if no proteinuria) – Progression to HD pattern with declining GFR de Boer et al. Clin J Am Soc Nephrol. 2008; 3(1): 125 -32.

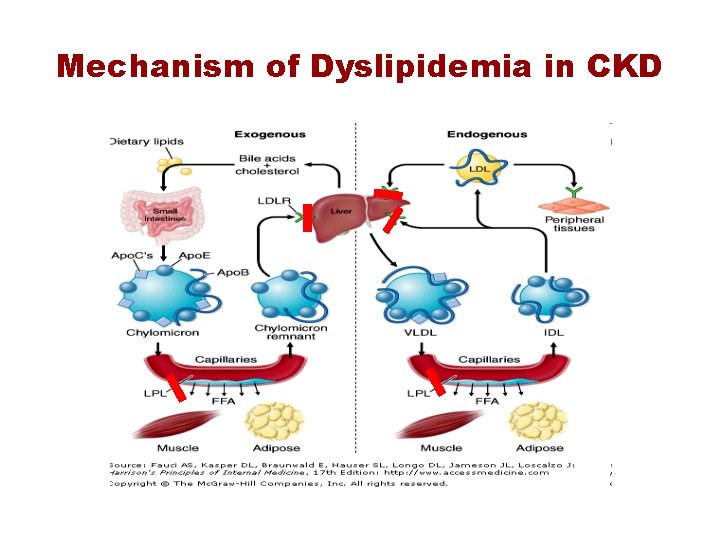
Mechanism of Dyslipidemia in CKD
![Lipoprotein a Lpa Modified LDL Higher affinity to macrophages Homologous to Lipoprotein (a) [Lp(a)] • Modified LDL – Higher affinity to macrophages • Homologous to](https://slidetodoc.com/presentation_image/5507e6cbe12b3e2bac95c08cc87ff3a2/image-12.jpg)
Lipoprotein (a) [Lp(a)] • Modified LDL – Higher affinity to macrophages • Homologous to plasminogen – Impairs fibrinolysis • Variable size • Levels – determined by genetics – Stable over time • Associated with CAD • Levels of larger moieties increase in CKD

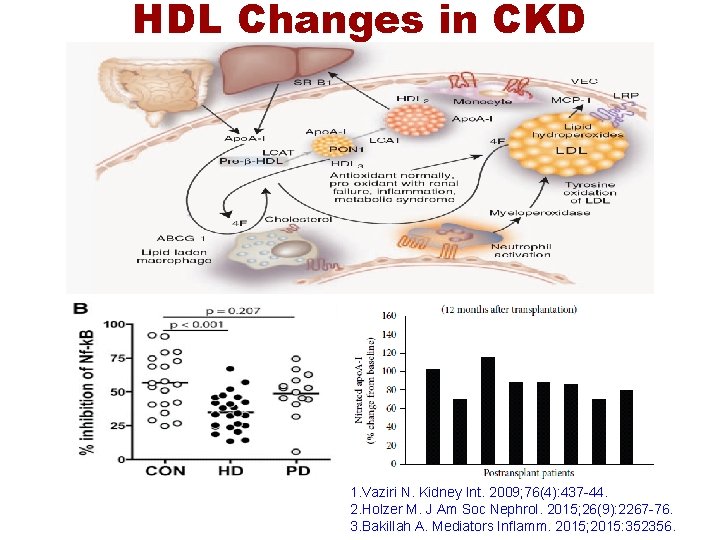
HDL Changes in CKD 1. Vaziri N. Kidney Int. 2009; 76(4): 437 -44. 2. Holzer M. J Am Soc Nephrol. 2015; 26(9): 2267 -76. 3. Bakillah A. Mediators Inflamm. 2015; 2015: 352356.

Changes After Transplant • Complex factors – – Proteinuria Graft dysfunction New-onset or worsening diabetes Immunosuppressants • Sirolimus > Cyclosporine > tacrolimus • Mechanism unknown – Impaired activity of lipases • Overall – Lipid profile similar to non-CKD patients – Lp(a) levels decline – HDL function may improve

Effect of Statin Therapy: non -dialysis CKD • • Study of Heart and Renal Protection (SHARP) 9, 200 patients, ~ 1/3 on HD Simvastatin + ezetimibe vs placebo 10 outcome: major atherosclerotic event (coronary event or death, ischemic stroke or revascularization) – 11. 3% vs 13. 4% – Similar side effects – Subgroup analysis • No difference in MI or coronary death • No difference in HD patients (but so if adjusted for reduction in LDL-C) Baigent C et al. Lancet. 2011; 377(9784): 2181.

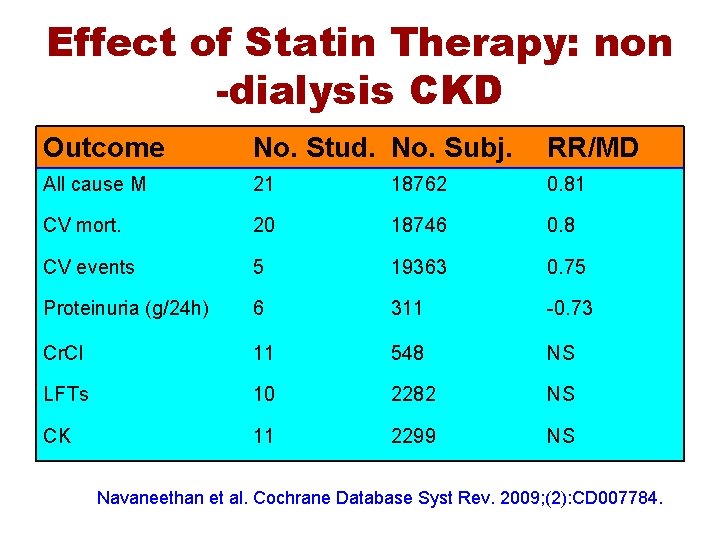
Effect of Statin Therapy: non -dialysis CKD Outcome No. Stud. No. Subj. RR/MD All cause M 21 18762 0. 81 CV mort. 20 18746 0. 8 CV events 5 19363 0. 75 Proteinuria (g/24 h) 6 311 -0. 73 Cr. Cl 11 548 NS LFTs 10 2282 NS CK 11 2299 NS Navaneethan et al. Cochrane Database Syst Rev. 2009; (2): CD 007784.

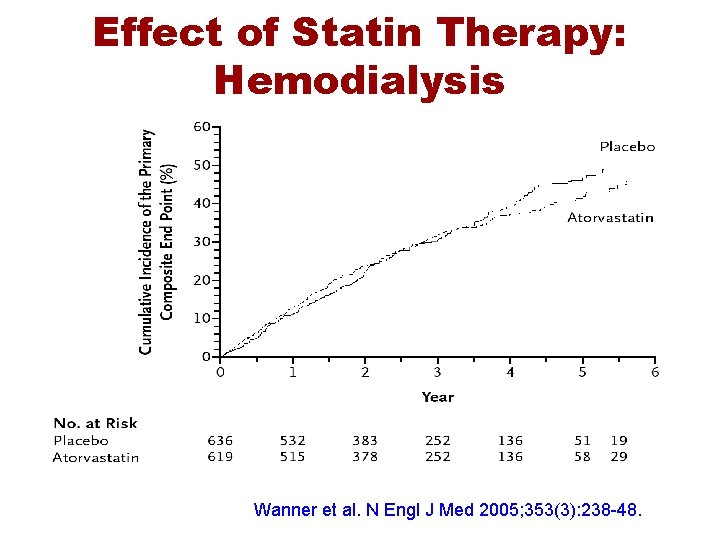
Effect of Statin Therapy: Hemodialysis Wanner et al. N Engl J Med 2005; 353(3): 238 -48.

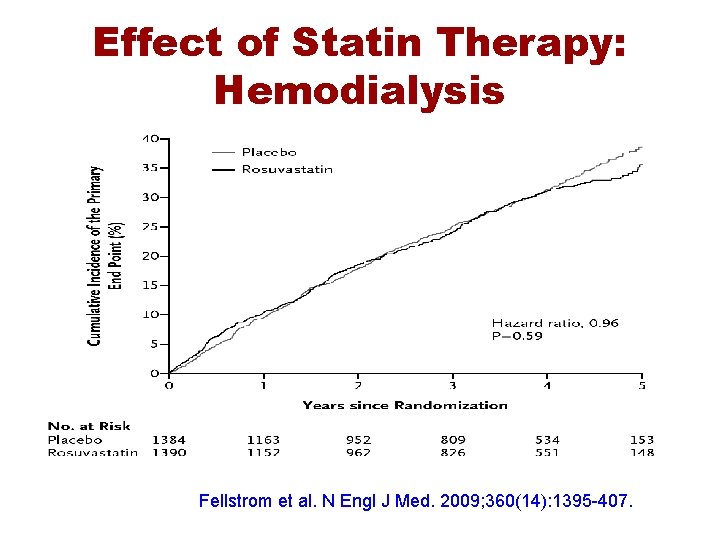
Effect of Statin Therapy: Hemodialysis Fellstrom et al. N Engl J Med. 2009; 360(14): 1395 -407.

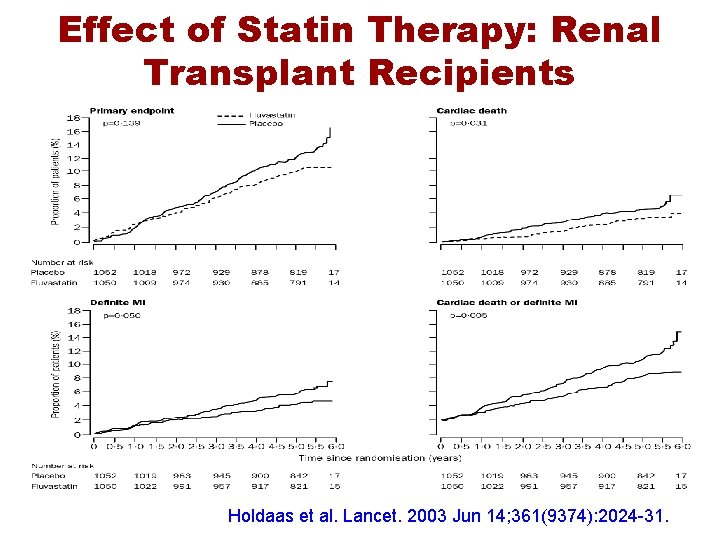
Effect of Statin Therapy: Renal Transplant Recipients Holdaas et al. Lancet. 2003 Jun 14; 361(9374): 2024 -31.

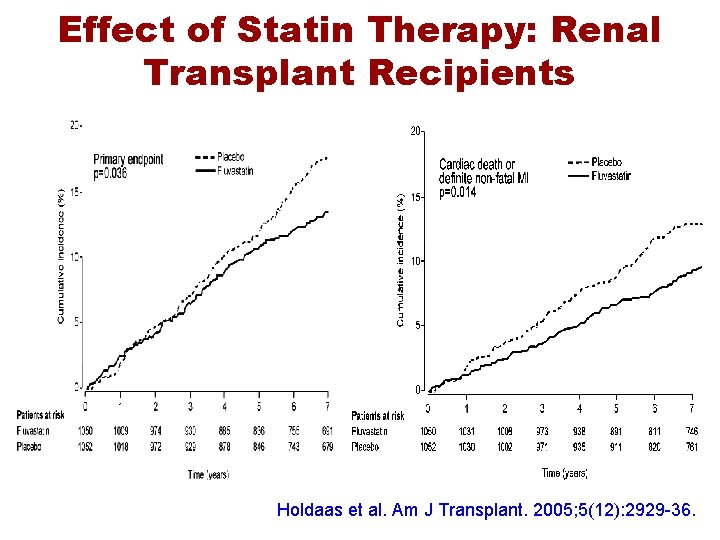
Effect of Statin Therapy: Renal Transplant Recipients Holdaas et al. Am J Transplant. 2005; 5(12): 2929 -36.

Treatment Guidelines • KDIGO: – Treatment for • Non-dialysis CKD – ≥ 50 – 18 -59 with known stroke or CAD or 10 -yr risk >10% • Dialysis – Continue for dialysis patients already on treatment – Do not start • NKF/K-DOQI/AST: not recently updated • Dialysis – symptomatic coronary disease or stroke after HD start? – Non-obstructive CAD or carotid disease identified on testing? KDIGO 2013

Future Directions • Reason for lack of effect in HD: • ? agent, duration, subpopulation, target • ? CV death due to arrhythmia/CHF • What is the target for lipid lowering in CKD? • β-lipoproteins? • metabolic pathways other than cholesterol – e. g. MTP, HDL pathway, PPAR-α agonists • Effect of treatment in modern era? • Newer ISx • Longer dialysis vintage

Summary • Lipoprotein, not simply cholesterol level, associated with atherosclerosis • Both quantitative and qualitative lipoprotein abnormalities • Treatment of Dyslipidemia – of benefit in non-dialysis CKD – Probably of benefit to renal transplant recipients – No evidence for benefit in hemodialysis patients – Statins are safe in CKD or after transplant