Dry Needling of a Powerlifter with Cervicobrachial Pain

Dry Needling of a Powerlifter with Cervicobrachial Pain Syndrome and Subscapular Nerve Impingement: A Level 3 Case Study Mills G. A. , Lumpkin K. J. , Coots J. G. Liberty University, Lynchburg, VA

Background • Cervicobrachial Pain Syndrome (CBPS) is considered neck pain associated with tingling, numbness or discomfort in the arm, upper back and upper chest with or without an associated headache. 1 • Prevalence in the United States is estimated to range from 3 to 80 per 1, 000 population. 2
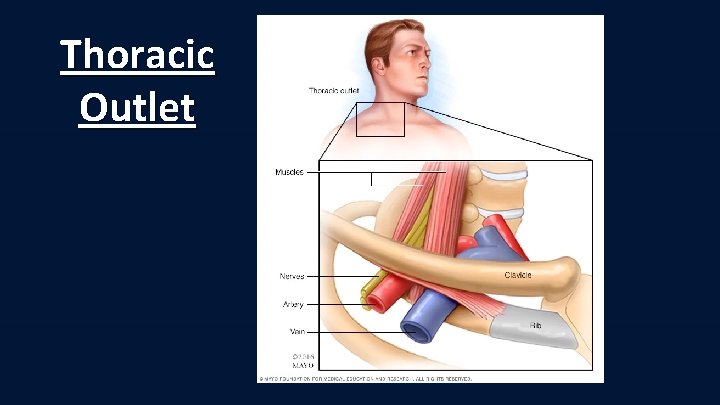
Thoracic Outlet

Patient • 41 yo M powerlifter – 23 yrs experience • No HX of prior injury • No pre-existing conditions
Patient • Insidious onset of pain, paresthesia, instability, and weakness in the right extremity • Pain in the posterior rotator cuff with numbness extending down the medial forearm into the fourth and fifth digits • Bench press dropped over one hundred pounds in a week

Initial Examination by Athletic Trainer • Minimal point tenderness • Normal AROM • MMT at 5/5 except for subscapularis (3/5) • TX: (approx. 2 weeks) – Manual release therapy – Massage – E-stim and ultrasound (combo) – Therapeutic exercises for possible rotator cuff strain
Examination by Chiropractor • Significant atrophy of the right triceps and pectoralis major • Bilateral diminished deep tendon reflexes of the biceps and triceps • Cervical AROM was slightly limited and thoracic rotation was significantly limited • RROM was at 5/5 for all shoulder motions, except 4/5 for abduction and internal rotation. • Sensory testing showed • • hypersensitivity of C 6 in the right extremity Trigger points were found in the upper trapezius, scalenes, sternocleidomastoid, and the pectoralis minor Jackson’s, Cervical Distraction, Apley’s, and Empty Can tests were positive
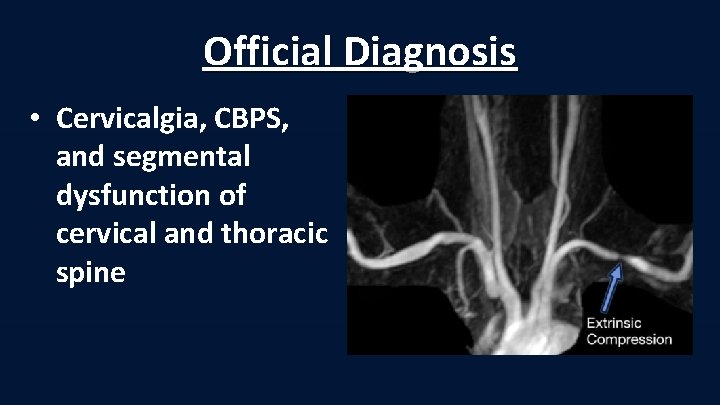
Official Diagnosis • Cervicalgia, CBPS, and segmental dysfunction of cervical and thoracic spine

Intervention or Treatment • One week of chiropractic care: – One session dry needling of trapezius, scalenes, pectoralis major and minor – One session of manipulation of the cervical spine – Two sessions of manipulation of the thoracic spine – Thoracic mobilization exercises

Intervention or Treatment • After chiropractic care, AT’s treatment consisted of: – Therapeutic exercises (target rotator cuff) – Manual release (pectoralis muscles) – Shoulder stretching – Electrical stimulation and ultrasound • The patient refrained from lifting for one week and then progressively returned to normal lifting within four weeks.

Outcomes or Other Comparisons • In patients who have persistent neurologic symptoms, muscle atrophy, or a progressive deficit, surgery is warranted. 3 • In this case, however, dry needling decreased neurological symptoms quickly and prevented the possibility of persistent symptoms.

Outcomes or Other Comparisons • Initially the patient’s Pain Disability Questionnaire score was a 22; after two chiropractic visits his score was a 3. • Research supports the use of manipulation and manual therapy such as dry needling for pain relief in upper quadrant pain syndromes 4. • This case reiterates findings that treatment based classification approach places greater emphasis on matching the patient to optimal interventions based on signs and symptoms collected during the evaluation rather than the pain generator diagnosis. • These treatment approaches resolved the patient’s symptoms without expensive diagnostic testing. 4

Conclusions • Quick referral diminished the time away from sport • Interprofessional collaboration fostered efficient and effective healthcare by integrating specialty services like dry needling and manipulation • The joint treatment plan allowed the athlete to return to competition more quickly than typical CBPS cases and thus far as prevented long term pain management issues

Clinical Bottom Line • In states where athletic trainers are restricted from dry needling, this type of interprofessional collaboration is paramount for quality patient care.

References 1. Lane, E, Clewley, D, Koppenhaver, S. Complaints of Upper Extremity Numbness and Tingling Relieved With Dry Needling of the Teres Minor and Infraspinatus: A Case Report. J Orthop Sports Phys Ther. 2017; 47(4), 287 -292. 2. Huang JH, Zager EL. Thoracic outlet syndrome. Neurosurgery. 2004; 55: 897– 902. 3. Kuhn, JE, Lebus, GF, Bible, JE. (2015). Thoracic Outlet Syndrome. J Am Acad Orthop Sur, 23(4), 222– 232. doi: 10. 5435/JAAOS-D-13 -00215. 4. Isabel de-la-Llave-Rincón A, Puentedura EJ, Fernández-de-las-Peñas C. Clinical presentation and manual therapy for upper quadrant musculoskeletal conditions. J Manip Ther. 2011; 19: 201 -211. Image 1: https: //www. mayoclinic. org/diseases-conditions/thoracic-outlet- syndrome/symptoms-causes/syc-20353988 Image 2: http: //www. hmmrmedia. com/2019/06/why-athletes-should-avoid-the-bars/ Image 3: https: //www. menshealth. com/es/fitness/a 27027756/diabetes-crossfitdeporte-alta-intensidad/ Image 4: https: //www. tosmri. com/delayed-diagnosis-of-thoracic-outlet-syndrome/
- Slides: 15