DRUGS USED IN THE MANAGEMENT OF RESPIRATORY DISEASE





































- Slides: 42

DRUGS USED IN THE MANAGEMENT OF RESPIRATORY DISEASE Oleh: Drh. I Dewa Putu Anom Adnyana, M. Vet Dosen Program Kedokteran Hewan Universitas Brawijaya Praktisi Klinik Hewan Universitas Brawijaya

Kepentingan 1. Kepentingan 2. 3. Dalam mempelajari obat sistem respirasi ada beberapa kepentingan diantaranya adalah : 4. 1. Memahami dan menerangkan arti dan mekanisme 5. 6. ADME yang terjadi dalam obat-obat sistem 7. respirasi. 8. 9. 2. Memahami jenis-jenis obat yng digunakan dalam 10. managemen pengobatan sistem respirasi 11. 12. 2

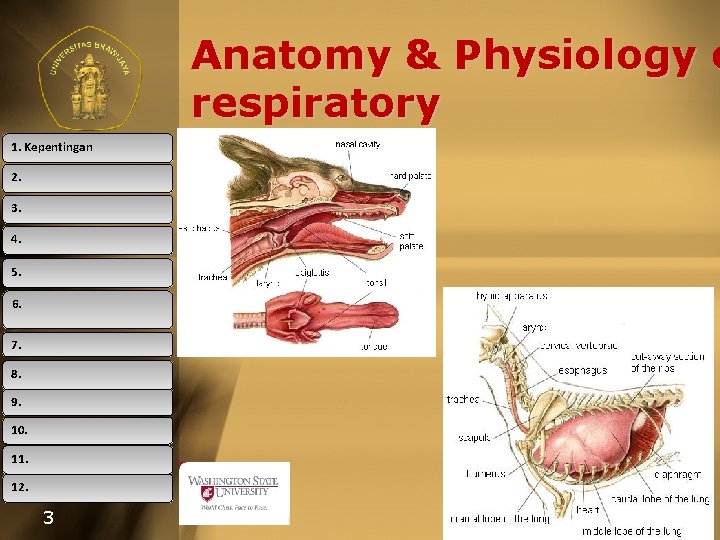
Anatomy & Physiology o respiratory 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 3

Anatomy & Physiology o respiratory 1. Kepentingan 1. 2. 3. 4. 5. The Upper respiratory tract nares, nasal cavity, pharynx, & larynx 6. 2. The Lower respiratory tract 7. trachea, bronchioles, 8. 9. alveoli, & alveolar-capillary membrane 10. 11. 12. 4

Ventilation & Respiration 1. Kepentingan > Ventilation is the movement of air from the atmosphere through the upper & lower airways to the alveoli > Respiration the process whereby gas exchange occurs at the alveolarcapillary membrane 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 5

Phases of respiration 1. Kepentingan 1. Ventilation in which oxygen passes through the airways 2. 3. 2. Perfusion 4. in which blood from the pulmonary 5. circulation is adequate at the alveolar-capillary bed 6. 3. Diffusion of gases 7. 8. in which oxygen passes into the capillary 9. bed to be circulated and carbon dioxide leaves the capillary bed & diffuses into the alveoli for ventilatory excretion 10. 11. 12. 6

Lung compliance 1. Kepentingan 2. 1. 2. Connective tissue (collagen & elastin) Surface tension in the alveoli (by surfactant) 3. Control of respiration 4. 5. > 6. Chemoreceptors changes of concentration O 2, CO 2, H+ The central chemoreceptors : in the medulla near the respiratory center & cerebrospinal fluid (by: CO 2 & p. H * Peripheral chemoreceptors : in the carotid & aortic bodie changes of oxygen levels) * 7. 8. 9. 10. 11. 12. 7

Bronchial smooth muscle 1. Kepentingan > Contraction constricts the airway 2. 3. 4. * The vagus nerve (parasympathetic nervous system) acetylcholine bronchoconstriction 5. 6. 7. 8. * The sympathetic nervous system epinephrine bronchodilatation 9. 10. 11. 12. 8

Drugs affecting the Respiratory Systems 1. Kepentingan 2. 3. 4. > Drugs for asthma 1. anti-inflammatory agents 2. bronchodilators 5. > Drugs for rhinitis, cough, & colds 1. nasal decongestans 2. antihistamines 3. anti-inflammatory agents 4. antitussives 5. Expectorants & mucolytics 6. 7. 8. 9. 10. 11. 12. 9

Drugs for asthma 1. Kepentingan 2. 3. 4. 5. 6. 2 main pharmacologic class: 1. Anti-inflammatory agents: glucocorticoids & cromolyn 2. Bronchodilators: beta 2 agonists > most antiasthmatic drugs can be administered by inhalation, caused: 7. 8. - therapeutic effects are enhanced (by delivering drugs directly to their site of action) - systemic effects are minimized - relief of acute attacks is rapid 9. 10. 11. 12. 10

Bronchodilator & antiasthma 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 11 > Sympathomimetics/Beta 2 -Adrenergic agonist - Examples : epinephrine, isoproterenol, isoetharine, albuterol, terbutaline, ephedrine - Use/ mechanism of action : treat asthma, bronchitis & emphysema by stimulating beta 2 receptors in bronchial smooth muscle to produce bronchodilatation, & thereby relieve bronchospasm - Adverse effect: CNS : restlessness, anxiety, dizziness, headache, insomnia; Cardiovascular : palpitations, cardiac arrhythmias, tachycardia, hypertension, cerebrovascular accidents, angina; GI: nausea, severe vomiting, diarrhea

Sympathomimetics 1. Kepentingan 2. > Adverse effect: Skin: local necrosis & tissue sloughing from extravasated intravenous catecholamines 3. 4. > Contraindication: cardiovascular diseases, 5. phenochromacytoma, hypertension 6. > Precaution: hyperthyroidism, diabetes, & pregna 7. 8. 9. 10. 11. 12. 12

Glucocorticoids (steroid) 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 13 > Examples : dexamethasone, betamethasone, prednison > Use/mechanism of action : steroids reduce symptoms of asthma by suppressing inflammation (decreased synthesis & release of inflammatory mediators; decreased infiltration & activity of inflammatory cells; decreased edema of the airway mucosa) > Adverse effect : inhalation oropharingeal candidiasis & dysphonia (hoarseness & speaking difficulty); oral (in prolonged therapy adrenal suppression, osteoporosis, hyperglycemia, peptic ulcer disease, & suppression of growth (in young patients)

Glucocorticoid 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 14 > Contraindication : systemic fungal infections; individuals receiving live-virus vaccines > Cautions : pediatric, pregnant & breast feeding woman

Cromolyn/ Mast cell stabilizers 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 15 > Examples : Cromolyn, Nedocromyl > Use/ mechanism of action : Cromolyn suppresses inflamation by stabilizing the cytoplasmic membrane of mast cells, thereby preventing release of histamine & other mediators. Cromolyn inhibits eosinophils, macrophages & other inflammatory cells > Adverse effects : cromolyn is the safest of al antiasthmatic medications, the most common reactions are wheezing, coughing & unpleasent taste

Methylxanthines 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 16 > Examples : Theophylline, aminophylline, dyphylline > Use/ mechanism of action : theophylline produces bronchodilatation by relaxing smooth muscle of the bronchi, the most probable mechanism is blockade of receptors for adenosine. > Adverse effects : theophylline has a narrow therapeutic range, & hence dosage must be carefully controlled; at plasma levels > 20μg/ml : nausea, vomiting, diarrhea, insomnia, restlesness, dysrhythmia & convulsion

Anticholinergic/ muscarini antagonist 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 17 > Examples: atropine, ipatropium bromide (atrovent) > Use/ mechanism of action: by blocking muscarinic cholinergic receptors in bronchi, & thereby promotes bronchodilatation > Adverse effects: dryness of oropharynx, cough

Drugs for rhinitis 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 18 > Rhinitis: an inflammation of the nasal mucous membranes > Symptoms: sneezing, rhinorrhea, nasal itching, & n congestion > Allergic & non-allergic > Drugs: (1) nasal decongestants (2) antihistamines ( intranasal anti-inflammatory

Nasal decongestants 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 19 > Examples : phenylephrine, Phenylpropanilamine (ppa) > Use/ mechanism of action : by stimulating alpha adrenergic receptors on smooth muscle of nasa blood vessels vasocontriction shrinkage o swollen membranes nasal drainage; topical administration more rapid & intense than oral administration > Adverse effects : rebound congestion; CNS stimulation; cardiovascular effects widespread casoconstriction > Contraindication & caution: hypertension & CAD

Antihistamines (H 1 -receptor antagonist) 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 20 > Examples : diphenhydramine, chlorpheniramine, promethazine, azatadine (1 st generation), terfenadine, astemizole, loratadine (2 nd generation) > Use/ mechanism of actions : these agents can relieve sneezing, rhinorrhea, & nasal itching by blocking H 1 receptor & thereby preventing the actions histamines at these sites > Adverse effects : sedation (1 st generation), cardiac dysrytmia, dizzines, nausea, vomiting, constipation, dry mouth

Drugs for cough & cold 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 21 > Cough: a complex reflex involving the central & pheripheral nerve systems & muscles of respiration can be initiated by irritation of the bronchial mucosa > (+): remove foreign matter & excess secretions from the bronchial tree > (-): deprive us of comfort & sleep

1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 22 > Common cold: an acute upper respiratory infection of viral origin > Symptoms: rhinorrhea, sneezing, cough, sore throat, headache, malaise, & myalgia > Combination cold remedias, 2 or more of: 1. nasal decongestants 2. antitussives 3. analgesic 4. antihistamines 5. caffeine

Antitussive agents 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 23 > Examples : opioid codeine, hydrocodone; non-opioid dextromethorpan hydrobromide (DMP) > Use/ mechanism of action : suppress coughing by altering response threshold of cough center in the medulla or peripherally by inhibiting pulmonary stretch, thus decreasing impulses to the cough center

Antitussive agents 1. Kepentingan 2. > Adverse effects : - Codeine: impaired alertness or coordination, hypersensitivity, dependence; toxic reactions : euphoria, hyperactivity, nystagmus, uncoordinated movements, stupor, shallow breathing - DMP: drowsiness & GI upset; toxic reaction : miosis, bradycardia, tachycardia, hypotension, narcosis, seizures, circulatory collapse 3. 4. 5. 6. 7. 8. 9. > Contraindication: pregnancy, lactation, known 10. hypersensitivity 11. 12. 24

Antitussive agents 1. Kepentingan 2. > Precautions: benign prostatic hypertrophy, debilitation, thoracotomy, laparotomy, history of drug abuse 3. 4. > Drug interactions: 5. - DMP and MAO (monoamine oxidase) inhibitors: excitation, hyperpyrexia - narcotic/opioid antitussive with MAO inhibitors, alcohol, & other CNS depressants: potentiation of CNS depressive effects 6. 7. 8. 9. 10. 11. 12. 25

Expectorants agents 1. Kepentingan > Examples: ammonium chloride, guaifenesin / glyceryl guaiacolate (GG) 2. 3. > Use/ mechanism of action: facilitate expulsion 4. of mucus by reducing adhesiveness and surface tension of mucus 5. 6. > Precaution: liver and renal insufficiency > Adverse effects: 7. 8. - GG: drowsiness, nausea, vomiting 9. 10. 11. 12. 26

Mucolytic agents 1. Kepentingan 2. > Examples: bromhexin, ambroxol, acetilcistein, hypertonic saline > Use/ mechanism of action: enhance mucolysis 3. by altering molecular composition of mucus, reducing viscosity; ambroxol: stimulate surfactant production of premature infant with respiratory distress syndromes > Precaution: gastric ulcer > Adverse effects : - bromhexin: nausea, serum transaminase level - acetilcistein: bronchial spasm, nausea, vomiting, stomatitis, haemoptysis 4. 5. 6. 7. 8. 9. 10. 11. 12. 27

PATOFISIOLOGI ASMA BRONKHIALE 1. Kepentingan 2. Penyakit inflamasi sal. nafas (sel-sel inflamasi ) 3. 4. Gejala - hiperresponsif bronkhus thd stimuli penyempitan bronkhus 5. 6. 7. Gamb. patologi * bronkhokonstriksi * penebalan mukosa ok edema & infiltrasi sel * sekresi mukus > 8. 9. 10. 11. 12. 28

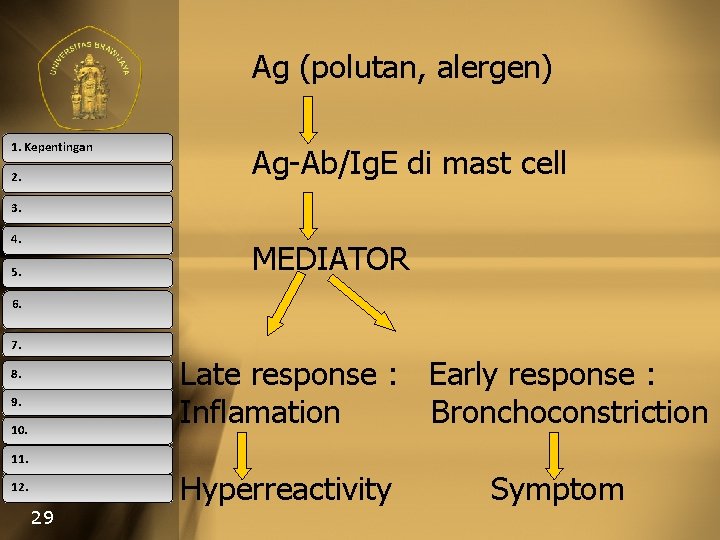
Ag (polutan, alergen) 1. Kepentingan 2. Ag-Ab/Ig. E di mast cell 3. 4. MEDIATOR 5. 6. 7. Late response : Early response : Inflamation Bronchoconstriction 8. 9. 10. 11. 12. 29 Hyperreactivity Symptom

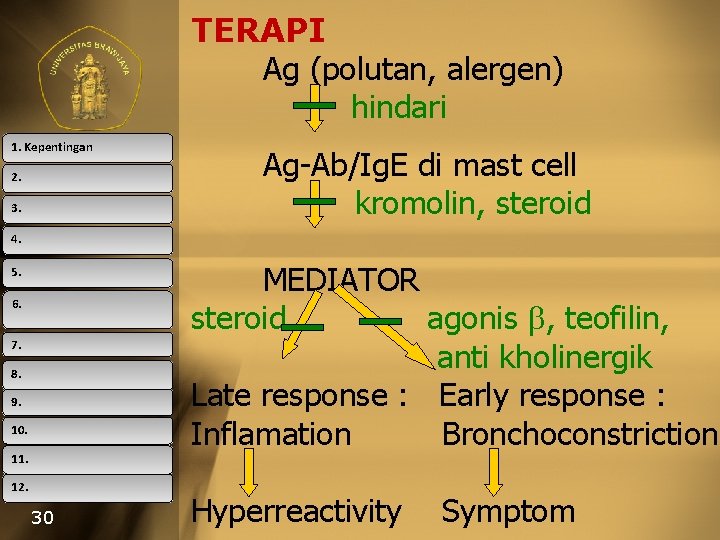
TERAPI Ag (polutan, alergen) hindari 1. Kepentingan 2. 3. Ag-Ab/Ig. E di mast cell kromolin, steroid 4. MEDIATOR steroid agonis , teofilin, anti kholinergik Late response : Early response : Inflamation Bronchoconstriction 5. 6. 7. 8. 9. 10. 11. 12. 30 Hyperreactivity Symptom

TERAPI 1. Kepentingan 2. 1. BRONKHODILATOR 2. ANTIINFLAMASI 3. 4. 3. LAIN-LAIN 5. 6. 7. 8. 9. 10. * * * mukolitik antitusif, ekspektoran antihistamin antibiotik jk. perlu preventif kromolin steroid CATATAN : JIKA HIPOKSIA (pd status asmatikus) OKSIGEN 11. 12. 31

BRONCHODILATOR 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 32 1. SIMPATOMIMETIK/ ADRENERGIK - adrenalin/ epinefrin - efedrin - isoproterenol, isoprenalin - agonis 2 selektif 2. DERIVAT XANTIN - teofilin 3. ANTIKHOLINERGIK - atropin - ipatropium bromid

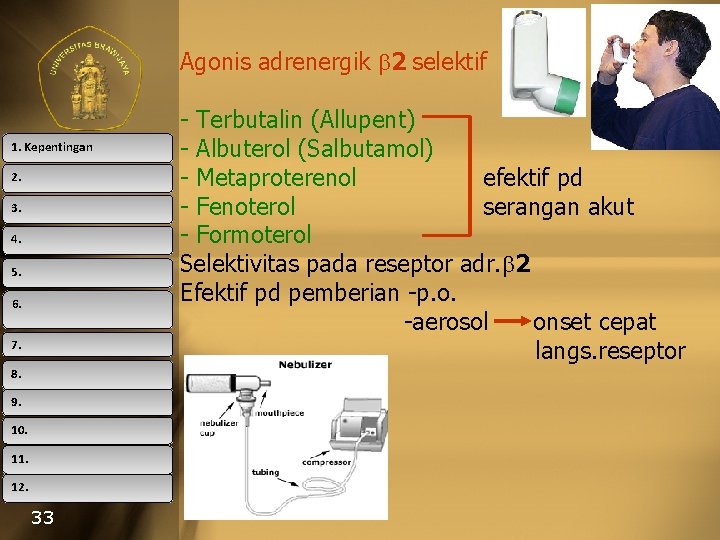
Agonis adrenergik 2 selektif 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 33 - Terbutalin (Allupent) - Albuterol (Salbutamol) - Metaproterenol efektif pd - Fenoterol serangan akut - Formoterol Selektivitas pada reseptor adr. 2 Efektif pd pemberian -p. o. -aerosol onset cepat langs. reseptor

EFEK SAMPING 1. Kepentingan 2. 3. 4. 5. 6. -aritmia ok stimulasi 1 jantung -tremor, musc. cramps -gangguan metabolisme -iritasi pada penggunaan inhaler -penggunaan lama reseptor desensitif 7. tolerans 8. 9. 10. 11. 12. 34

DERIVAT XANTIN 1. Kepentingan METYLXANTIN 2. 3. TEOFILLIN TEOBROMIN CAFFEIN 4. 5. EFEK 6. 7. 8. 9. 10. 11. 12. 35 - Relaksasi otot polos bronkhus - Stimulasi SSP - Stimulasi otot jantung - Diuresis - Asam lambung - Otot bergaris

FARMAKOKINETIK 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 36 - absorpsi baik : - p. o. , “sustained release” kadar stabil di plasma - p. e. iv - distribusi : slrh tubuh plasenta, ASI - metabolisme: hepar ok -induksi enz o/ rifampin, fenobarbtal, etanol -rokok ok -inhibisi enz o/ simetidin, eritromisin, alopurinol -gagal jantung, liver dis. -orang tua

EFEK SAMPING 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 37 -iv. cepat aritmia jantung, hipotensi -Sakit kepala, palpitasi, dizziness, nausea, hipotensi, nyeri prekordial -Indeks terapi sempit dosis besar takikardia, agitasi kejang, emesis, Gx. GIT

ANTIKHOLINERGIK 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 38 *ATROPIN : iv; aerosol *IPATROPIUM BROMID : aerosol Mekanisme : -Antagonis res. kholinergik M # otot polos bronkhodilatasi # kelenjar mukus Efek sistemik : -Mulut kering, retensi urin, mata kabur, takikardi Efektif u/ hiperreaktif bronkhokonstriksi bronkhitis kronis

ANTIINFLAMASI KORTIKOSTEROID 1. Kepentingan 2. 3. 4. 5. EFEK : -langsung otot polos bronkus (-) -inflamasi -hiperreaktivitas -efek pd reseptor adr. : kepekaan 6. Obat : prednison, prednisolon mild asma : inhaler 7. 8. 9. 10. 11. 12. 39 p. o

EFEK SAMPING 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 40 -lokal : kandidiasis, iritasi -sistemik : supresi adrenal retensi Na dan air osteophorosis ulkus peptikum metab. KH “moon face”, “buffalo hump”

KROMOLIN 1. Kepentingan 2. 3. 4. 5. 6. 7. 8. 9. 10. 11. 12. 41 -per inhalasi -stabilisasi mast cell degranulasi (-) -efek samping : Batuk, edem laryng, nyeri sendi, sakit kepala, rash, nausea -indikasi : - preventif serangan asma

Oleh: I Dewa Putu Anom Adnyana. drh. , M. Vet Dosen Program Kedokteran Hewan Universitas Brawijaya Praktisi Klinik Kedokteran Hewan UB