Drugs for Pain and Sleep Problems Module G

Drugs for Pain and Sleep Problems • Module G Part 3 Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Objectives • Identify personal factors that affect a patient’s perception of pain. • Compare the features of acute pain with those of chronic pain. • Describe the different types of pain-control drugs. • Compare the features of drugs classified as controlled substances. • Explain what to do before and after giving an opioid drug for pain control. • List the names, actions, usual adult dosages, possible side effects, and adverse effects of commonly prescribed opioid drugs for pain control. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 2

Objectives (cont’d) • Explain what to teach patients about opioid drugs for pain control, including what to do, what not to do, and when to call the prescriber. • List the names, actions, usual adult dosages, possible side effects, and adverse effects of commonly prescribed nonopioid drugs for pain control. • Explain what to teach patients about nonopioid drugs for pain control, including what to do, what not to do, and when to call the prescriber. • Describe life span considerations for pain-control drugs. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 3

Pain • Unpleasant sensory and emotional experience associated with tissue damage • Pain perceived with all senses • Fifth vital sign – unrelieved/undertreated pain is common but avoidable health problem Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 4
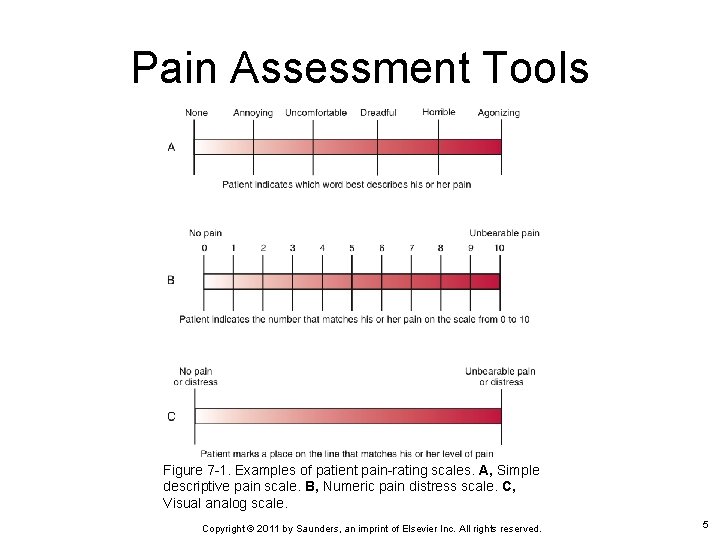
Pain Assessment Tools Figure 7 -1. Examples of patient pain-rating scales. A, Simple descriptive pain scale. B, Numeric pain distress scale. C, Visual analog scale. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 5
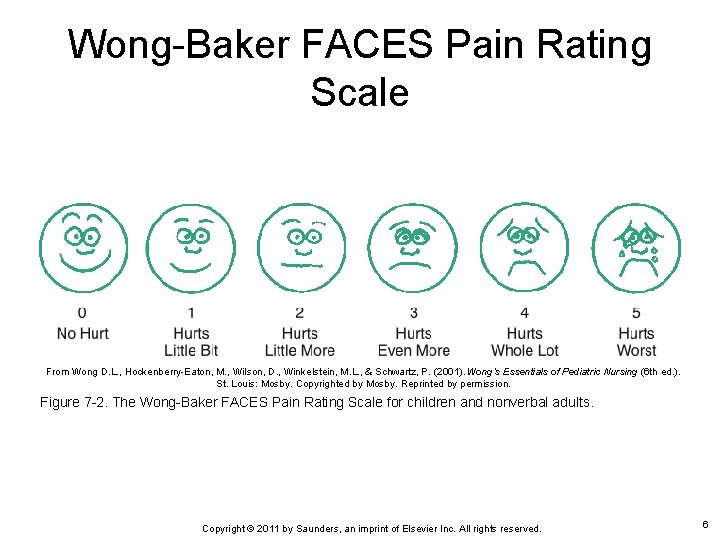
Wong-Baker FACES Pain Rating Scale From Wong D. L. , Hockenberry-Eaton, M. , Wilson, D. , Winkelstein, M. L. , & Schwartz, P. (2001). Wong’s Essentials of Pediatric Nursing (6 th ed. ). St. Louis: Mosby. Copyrighted by Mosby. Reprinted by permission. Figure 7 -2. The Wong-Baker FACES Pain Rating Scale for children and nonverbal adults. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 6

Pain Physiology and Pathophysiology • Origin and transmission • Perception – Threshold – Tolerance • Types – Acute – Chronic – Cancer Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 7
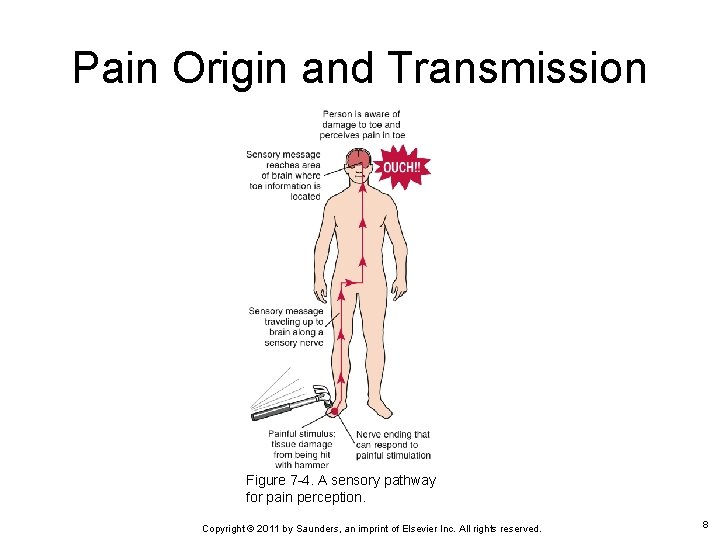
Pain Origin and Transmission Figure 7 -4. A sensory pathway for pain perception. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 8

Analgesic Drug Therapy • Analgesics – drugs to control pain – Opioids – Nonsteroidal anti-inflammatory drugs (NSAIDs) – Non-opioid miscellaneous drugs • Controlled substances – drugs containing addictive ingredients Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 9

Administering Analgesic Drugs • Check before: – Pain intensity using appropriate pain scale – When the last dose was given • Check after: – Amount of pain relief (check in 30 min, then hourly) • Patient teaching: – Instruct how to achieve best pain relief Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 10

Opioids (Narcotics) • Bind to opioid receptor sites in brain, altering perception of pain • Side effects – constipation, nausea/ vomiting, drowsiness, dizziness • Adverse effects – respiratory depression, addiction, dependence, tolerance, withdrawal Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 11

Administering Opioids • Check before: – Respiratory rate, O 2 saturation – Dose, drug name • Check after: – Respiratory rate and O 2 saturation at least hourly, bowel pattern • Patient teaching: – – – Take with food Do not drive or operate heavy machinery Change positions slowly Increase fluids, fiber, and activity Use stool softeners or laxatives as ordered Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 12

Life Span Considerations for Opioids • Pediatric: – Dosage based on age, size (weight in kg), health, pain severity • Pregnancy and breastfeeding: – Newborn addiction/withdrawal can occur – Monitor newborns closely for respiratory depression if opioids given during labor – Avoid breastfeeding if taking opioids for more than 2 days • Older adults: – Pain often undertreated – Visual impairment; risk for falls – Avoid meperidine (Demerol) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 13

Anti-Inflammatory Drugs Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Nonsteroidal Anti-Inflammatory Drugs (NSAIDs) • Suppress part of the inflammatory pathway • Side effects: – – Reduce clotting (especially aspirin) Headache Irritation of GI tract Reduce blood flow to kidney, slow urine output, lead to high blood pressure and kidney damage (except aspirin) • Adverse effects: – Induction of asthma – Salicylate poisoning (aspirin only) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 15

Administering NSAIDs • Check before: – Previous problems with NSAIDs, including OTCs – Give after meals with full glass of water or milk – Blood pressure • Check after: – Bleeding, even with one dose – Sensitivity reaction • Patient teaching: – Do not take on an empty stomach – Monitor for bleeding – Do not take with warfarin (Coumadin) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 16

Life Span Considerations for NSAIDs • Pediatric: – Only ibuprofen is recommended – Avoid aspirin (Reye’s syndrome) • Pregnancy: – Category C drug for first 6 months – Avoid during last 3 months • Older adults: – Cardiac problems Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 17

Acetaminophen • Effective for pain relief • Commonly combined with other drugs (especially opioids) • Toxic when taken at high doses, too often, or with alcohol • Risk for permanent liver or kidney damage • Pediatric considerations: – Toxic to liver and kidneys at high doses – Must calculate doses accurately – Parents must READ LABELS to determine strength Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 18

Antidepressants • Reduce some types of chronic and cancer pain • Different dose given for pain control • Patients experience relief in 1 -2 weeks • Side effects – constipation, dry mouth, urinary retention, sweating, sexual dysfunction, intraocular pressure Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 19

Life Span Considerations for Antidepressants • Pediatric: – Not recommended, except for cancer pain – Suicidal behavior • Pregnancy and breastfeeding: – Categories B and C – Benefit must outweigh risk – Avoid breastfeeding • Older adults: – Heart problems – Worsen urinary problems – Worsen glaucoma Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 20

Anticonvulsants • Reduce some types of pain – Neuropathic pain – Migraines • Common drugs – Gabapentin (Neurontin) – Pregabalin (Lyrica) • Side effects – drowsiness, confusion, blurred vision, clumsiness, muscle aches, weakness Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 21

Life Span Considerations for Anticonvulsants • Pediatric: – Aggressive behavior can be side effect • Pregnancy and breastfeeding: – Category C – Benefit must outweigh risk – Avoid breastfeeding Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 22

Objectives • List the names, actions, usual adult dosages, possible side effects, and adverse effects of drugs for sleep problems. • Explain what to do before and after giving a drug for sleep problems. • Explain what to teach patients about drugs for sleep problems. • Describe life span considerations related to drugs for sleep problems. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 23

Drugs for Insomnia • Most common sleep problem • Sedatives – Benzodiazepine receptor agonists (first line drugs) – Benzodiazepines – Antihistamines – Sedating antidepressants Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 24

Drugs for Insomnia (cont’d) • Cause general depression of CNS, OR drowsiness and mild sedation • Intended response – relief of insomnia, improved sleep • Common side effects: – Drowsiness, dizziness, dry mouth, headache, GI discomfort • Adverse effects: – Psychological/physical dependence (benzodiazepines) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 25

Administering Drugs for Insomnia • Check before: – List of drugs taken by patient, including herbals and OTCs – Possible causes of insomnia – Mental status, vital signs • Check after: – Vital signs, level of consciousness • Patient teaching: – Call for help when getting out of bed – Do not double-dose – Do not drive or operate heavy machinery Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 26

Life Span Considerations for Drugs for Insomnia • Pediatric: – Antihistamines may cause increased excitement • Pregnancy and breastfeeding: – Benzodiazepines – categories D and X – Zolpidem (Ambien) – categories B and C – Most cross placenta, enter breast milk • Older adults: – Lower doses because of increased sensitivity – More likely to experience side effects – Increased risk for falls Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 27

Narcolepsy • Sleep disorder – uncontrollable urge to sleep – Cataplexy – Vivid hallucinations – Total paralysis • Drugs: – Methylphenidate (Ritalin) – general CNS stimulant – Modafinil (Provigil) – selective CNS stimulant – Sodium oxybate (Xyrem) – sedative Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 28

Drugs for Narcolepsy • Intended responses – increased attention span, motor activity, and mental alertness during waking hours; decreased fatigue and episodes of inappropriately falling asleep • Side effects: – Stimulatory drugs: insomnia, diarrhea, upset stomach, tremors – Sodium oxybate (Xyrem): sleep-walking • Adverse effects: – Seizures, abnormal heart rhythm, chest pain Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 29

Administering Drugs for Narcolepsy • Check before: – List of drugs taken by patient, including herbals and OTCs – Vital signs • Check after: – Vital signs every shift, daily weights – Seizure activity • Patient teaching: – Take exactly as directed – Medical follow-up important – Do not take missed dose of methylphenidate (Ritalin) close to bedtime – Avoid caffeine-containing drinks and alcohol Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 30

Life Span Considerations with Drugs for Narcolepsy • Pediatric: – Methylphenidate can slow growth (height and weight) • Pregnancy and breastfeeding: – Not recommended • Older adults: – Start on lower doses – Risk for changes in thinking patterns, problems with movement Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved. 31

• Anti-Inflammatory Drugs Objectives Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Objectives • Explain how inflammation is different from infection. • Describe the basis for the five major signs and symptoms of inflammation. • List the names, actions, usual adult dosages, possible side effects, and adverse effects of commonly prescribed corticosteroids. • Describe what to do before and after giving corticosteroids. • Explain what to teach patients taking corticosteroids, including what to do, what not to do, and when to call the prescriber. • Describe life span considerations for corticosteroids Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Inflammation vs. Infection • Inflammation – Normal reactions of tissues/blood vessels in response to injury or invasion – Invasion may be environmental or pathogenic microorganisms • Infection – Invading microorganisms disturb normal environment and cause harm – Usually accompanied by inflammation Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Inflammation Physiology and Pathophysiology • Signs and symptoms: – Warmth – Redness – Swelling – Pain – Decreased function • Stage I: vascular • Stage II: exudate • Stage III: tissue repair Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.
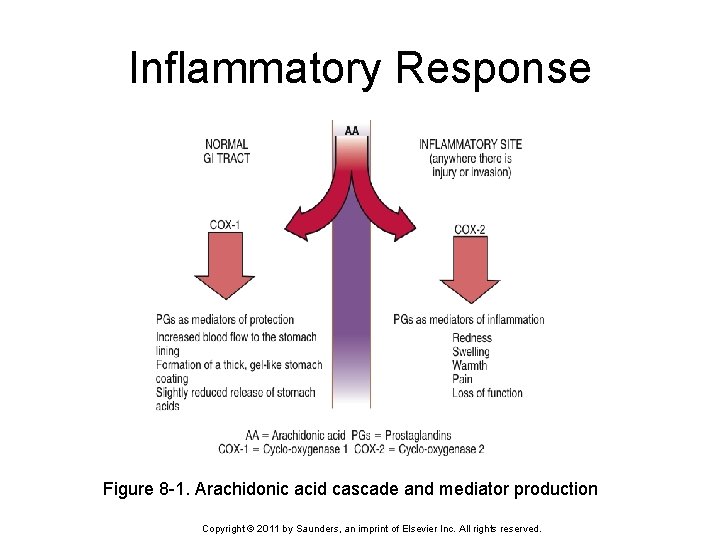
Inflammatory Response Figure 8 -1. Arachidonic acid cascade and mediator production Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Anti-Inflammatory Drugs • Prevent or limit tissue and blood vessel responses to injury or invasion • Increase comfort and prevent tissue-damaging complications • Three main categories: – Corticosteroids – NSAIDs – Antihistamines Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Corticosteroids • Prevent or limit inflammation by slowing or stopping all known pathways of inflammatory mediator production • Drug forms and routes: – – – – Oral Parenteral Inhalation (asthma) Topical (skin problems) Injected into joints Rectal (hemorrhoids) Drops (eye problems) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Corticosteroids (cont’d) • Intended responses: – Reduced redness, pain, swelling at site of inflammation; increased function of affected area • Side effects: – Short term therapy – hypertension, acne, insomnia, nervousness – Long term therapy – adrenal gland suppression, reduced immune function, delayed wound healing, “Cushingoid appearance” • Adverse effects: – Adrenal gland atrophy, masking of infection Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.
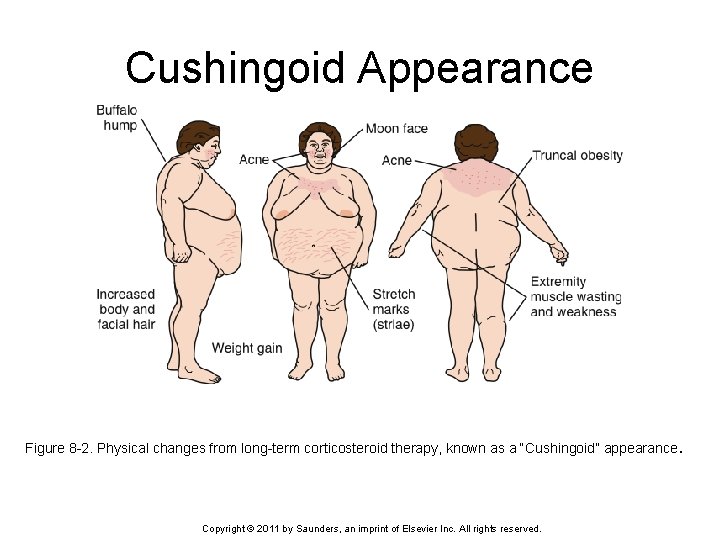
Cushingoid Appearance Figure 8 -2. Physical changes from long-term corticosteroid therapy, known as a “Cushingoid” appearance. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Corticosteroid Administration • Check before: – Dose and specific drug name – Symptoms of infection – Blood pressure and weight • Check after: – Vital signs at least once per shift – Weekly weights • Patient teaching: – Do not suddenly stop taking drug – Take with food – Avoid crowds Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Life Span Considerations for Corticosteroids • Pediatric: – At risk for same side effects as adults • Pregnancy and breastfeeding: – Drugs cross placenta, are excreted in breast milk • Older adults: – Extra precautions to avoid infection – Monitor blood glucose levels Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Objectives • List the names, actions, usual adult dosages, possible side effects, and adverse effects of commonly prescribed nonsteroidal anti-inflammatory drugs (NSAIDs). • Describe what to do before and after giving NSAIDs. • Explain what to teach patients taking NSAIDs, including what to do, what not to do, and when to call the prescriber. • Describe life span considerations for NSAIDs. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

NSAIDs • Prevent or limit tissue/blood vessel responses to injury or invasion by slowing the production of one or more inflammatory mediators • Different groups: – Cyclo-oxygenase 1 (COX-1) – COX-2 • Based on chemical makeup • Inhibit action of cyclo-oxygenase Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

NSAIDs (cont’d) • Intended responses – reduced redness, pain, swelling, and warmth at site of inflammation; increased function; reduced fever • Side effects – bleeding, GI ulcers, GI pain, fluid retention, hypertension • Adverse effects – possible kidney damage, induction of asthma and allergic reactions Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

NSAID Administration • Check before: – Previous problems with NSAIDs, including OTCs – Give after meals with full glass of water or milk – Blood pressure • Check after: – Bleeding, even with one dose – Sensitivity reaction • Patient teaching: – Do not take on an empty stomach – Monitor for bleeding – Do not take with warfarin (Coumadin) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Life Span Considerations for NSAIDs • Pediatric: – Only ibuprofen is recommended – Avoid aspirin (Reye’s syndrome) • Pregnancy: – Category C drug for first 6 months – Avoid during last 3 months • Older adults: – Cardiac problems Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Objectives • List the names, actions, usual adult dosages, possible side effects, and adverse reactions of commonly prescribed antihistamines and leukotriene inhibitors. • Describe what to do before and after giving antihistamines and leukotriene inhibitors. • Explain what to teach patients taking antihistamines or leukotriene inhibitors, including what to do, what not to do, and when to call the prescriber. Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Antihistamines (Histamine Blockers) • Reduce inflammation by preventing inflammatory mediator (usually histamine or leukotriene) from binding to its receptor • Histamine – Cause changes that lead to inflammatory responses • H 1 receptors in blood vessels, respiratory mucous membranes • H 2 receptors in stomach lining – Main mediator of inflammation and capillary leak • Leukotriene – maintains inflammatory response Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Antihistamines (cont’d) • Intended responses – blood vessels do not dilate; reduced swelling; mucus, other nasal, eye, respiratory secretions are reduced; narrowed airways widen; hives decrease in size, itchiness • Side effects – sleepiness, dry mouth, blurred vision, tachycardia, urinary retention • Adverse effects - seizures (rare), increased intraocular pressure Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Antihistamine Administration • Check before: – Glaucoma, high blood pressure, prostate enlargement – Other drugs being taken that cause sedation • Check after: – Vital signs – Assist patient when getting out of bed • Patient teaching: – Avoid alcohol – Avoid driving or operating machinery within 6 hours of administration Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Leukotriene Inhibitors • Intended responses – reduced swelling of oral, nasal, eye, respiratory mucous membranes; reduced secretions; narrowed airways open • Side effects: – Headache – Abdominal pain • Adverse effects (rare): – Liver impairment – Allergic reactions (including hives and anaphylaxis) Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.

Leukotriene Inhibitor Administration • Check before: – Any liver problems • Check after: – Liver problems (regular follow-up) • Patient teaching: – Report symptoms of liver problems Copyright © 2011 by Saunders, an imprint of Elsevier Inc. All rights reserved.
- Slides: 53