DRUGS FOR BUGS ANTIBIOTICS ANTIVIRALSA ANTIFUNGALS ANTITUBERCULAR ANTIMALARIAL

DRUGS FOR BUGS ? ? ANTIBIOTICS ANTIVIRALSA ANTIFUNGALS ANTI-TUBERCULAR ANTIMALARIAL ANTIHELMINTHIC ANTIMYCOBACTERIAL ANTIVIRALS ANTIBIOTICS COMMONLY KNOWN AS ANTIMICROBIALS Winter 2013 1

WHAT IS AN INFECTION? A disease or condition caused by a microorganism that releases toxins or invade body tissues ◦ Localized infection ◦ Systemic infection Winter 2013 2

WHO IS MORE LIKELY TO GET AN INFECTION? SKIN NOT INTACT BLOOD SUPPLY IMPAIRED NEUTROPENIA MALNUTRITION SUPPRESSION OF NORMAL BACTERIAL BALANCE SUPPRESSION OF THE IMMUNE SYSTEM DIABETES CHRONIC ILLNESS ADVANCED AGE Winter 2013 3

Infections: Sites of Origin Community-associated infections ◦ An infection that is acquired by a person who has not been hospitalized or had a medical procedure (such as dialysis, surgery, catheterization) within the past year Winter 2013 4

Infections: Sites of Origin (cont’d) Healthcare-associated infections ◦ Contracted in a hospital or institutional setting ◦ Were not present or incubating in the patient on admission to the facility ◦ More difficult to treat because causative microorganisms are often drug resistant and the most virulent ◦ One of top ten leading causes of death in the U. S. ◦ MRSA most common Winter 2013 ◦ Previously known as nosocomial 5

Healthcare-Associated Infections: Prevention Hand washing Antiseptics Disinfectants Winter 2013 6

Healthcare-Associated Infections: Prevention (cont’d) Disinfectant ◦ Kills organisms ◦ Used only on nonliving objects Antiseptic ◦ Generally only inhibits the growth of microorganisms but does not necessarily kill them ◦ Applied exclusively to living tissue Winter 2013 7

FUNCTIONS OF ANTIBIOTICS v BACTERICIDAL – Kills or destroys microorganisms v BACTERIOSTATIC – Retards the growth of microorganisms Winter 2013 8

IDENTIFICATION OF BACTERIA v. GRAM TESTING v. CULTURE AND SENSITIVITY TESTING v. SEND SPECIMEN FIRST !!!!! v. START ANTIBIOTIC BEFORE CULTURE RESULTS ARE KNOWN (EMPIRIC THERAPY) v. RX MAY CHANGE WHEN CULTURE IS GROWN Winter 2013 9
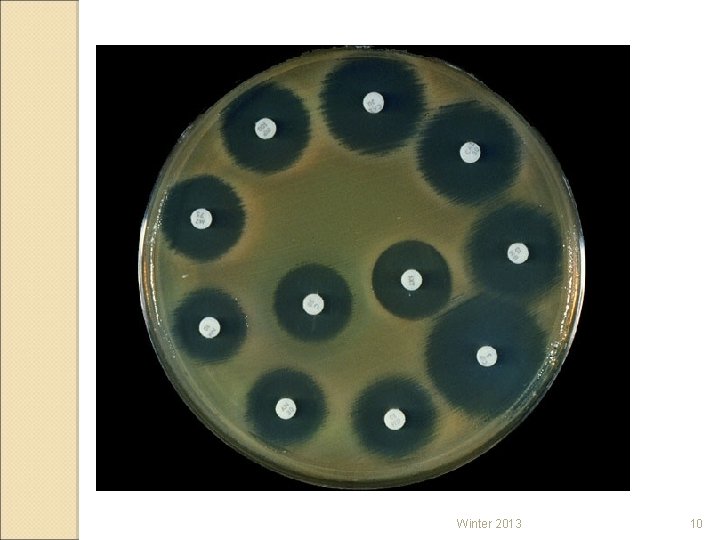
Winter 2013 10

BACTERIAL RESISTANCE Bacterial resistance ◦ PENICILLINASE USED BY BACTERIA TO DESTROY PCN ◦ BETA-LACTAMASE BREAKS DOWN THE STRUCTURE OF THE ABX INACTIVATING THE DRUG Winter 2013 11

ANTIMICROBIAL RESISTANCE UNWISE USE OF ANTIBIOTICS ◦ ANTIBIOTICS ARE NOT EFFECTIVE AGAINST VIRAL INFECTIONS ◦ WHEN VIRAL SYMPTOMS PERSIST, ABX WILL BE USED FOR A SECONDARY BACTERIAL INFECTION ANTIBIOTICS MAY BE PRESCRIBED AS PROPHYLACTIC TO ANOTHER TREATMENT OR PROCEDURE Winter 2013 12

ANTIMICROBIAL RESISTANCE METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS MRSA ◦ HAND WASHING AND GLOVING ◦ GOAL IS TO AVOID HEALTHCARE ASSOCIATED INFECTIONS ◦ “COLONIZED” MEANS HARBORS THE BACTERIA Winter 2013 13

ANTI-INFECTIVES / ANTIBIOTICS PROPER DOSE AND DURATION OF THERAPY ◦ AVERAGE OF 7 – 10 DAYS OF THERAPY ◦ SPECIFY TIME OF DAY TO TAKE THE DRUGS TO MAINTAIN THERAPEUTIC LEVELS ◦ PATIENT MUST COMPLETE ENTIRE RX ◦ NEVER SAVE FOR USE AT ANOTHER TIME ◦ NEVER SHARE WITH ANOTHER PERSON Winter 2013 14

ADVERSE REACTIONS TO ABX HYPERSENSITIVITY (allergy) Requires at least one exposure to the drug ◦ Mild – Rash, pruritus, urticaria ◦ Severe – Anaphylaxis Laryngospasms (wheezing) Dyspnea Decrease in blood pressure Winter 2013 15
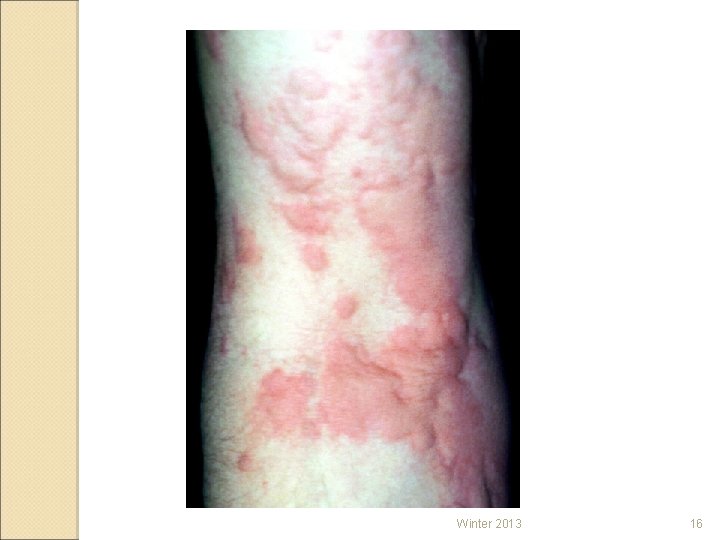
Winter 2013 16
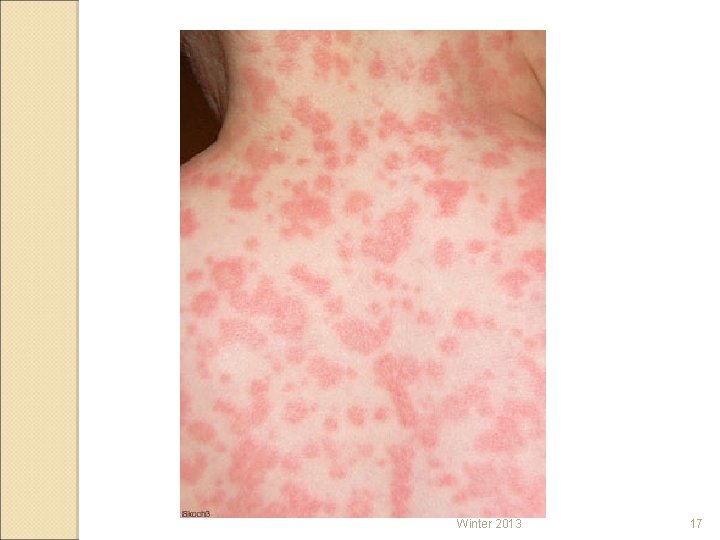
Winter 2013 17

ADVERSE REACTIONS TO ABX CROSS-SENSITIVITY REACTIONS ◦ If allergic to one antibiotic, allergic to antibiotics from same family ◦ EXAMPLE – ALLERGY TO PCN, ALSO MAY BE ALLERGIC TO CEPHALOSPORIN Winter 2013 18

STEVENS-JOHNSON SYNDROME ◦ Severe (can be fatal) hypersensitivity reaction caused by reaction to a medication ◦ Typically involves the skin and mucous membranes developing severe inflammation progressing to necrosis of the tissues. Can also progress to the lining of internal organs. ◦ TABER’S – TOXIC EPIDERMAL NECROLYSIS Winter 2013 19
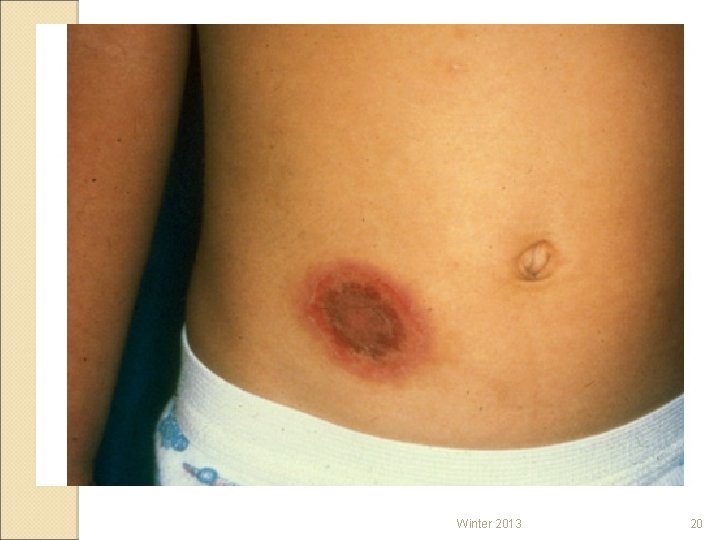
Winter 2013 20
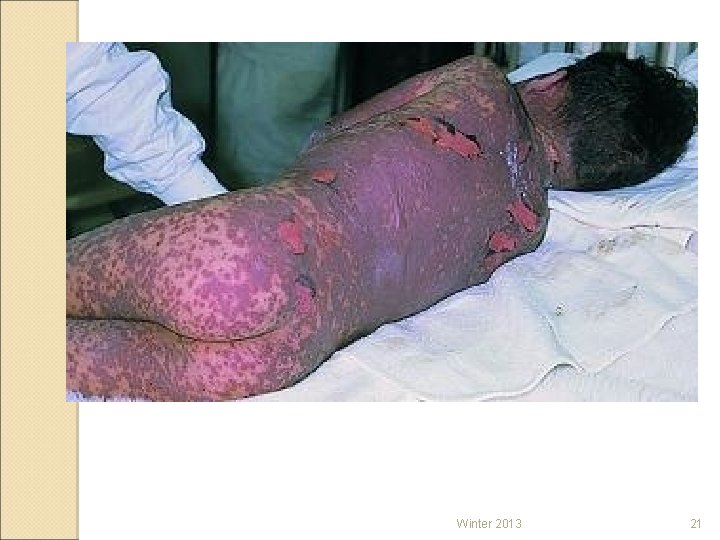
Winter 2013 21
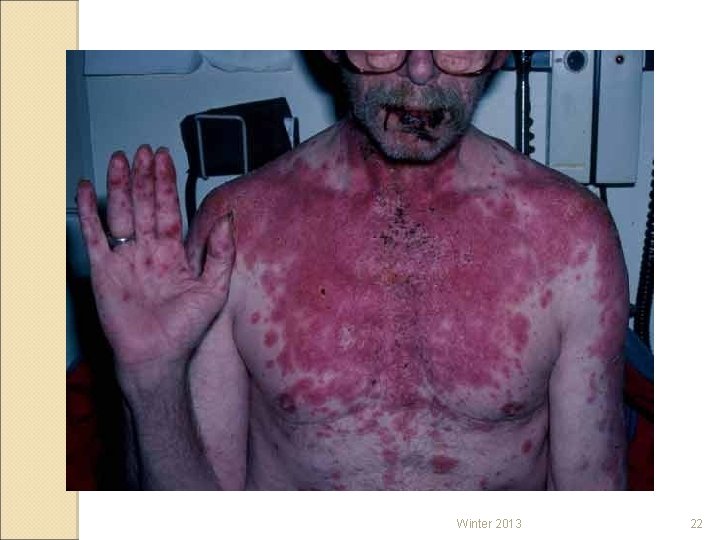
Winter 2013 22

SUPERINFECTION ◦ A secondary infection that occurs during antibiotic therapy in which normal flora are destroyed Winter 2013 23

Superinfection LOCATION OF INFECTION ◦ GROIN ◦ AXILLA ◦ MOUTH ◦ UNDER BREAST TISSUE ◦ ANY WARM MOIST AREA OFFENDING ◦ YEAST ◦ BACTERIA ORGANISM Winter 2013 24
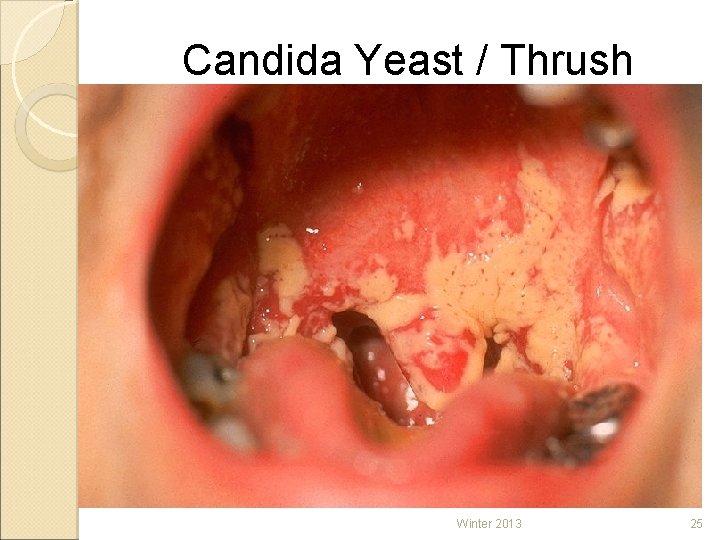
Candida Yeast / Thrush Winter 2013 25

NURSING RESPONSIBILITIES PATIENT’S RESPONSE TO THERAPY ◦ EVALUATE TEMPERATURE, APPETITE AND GENERAL LEVEL OF WELLNESS FLUID ◦ ◦ INTAKE DRUGS ARE NEPHROTOXIC ADVISE PATIENT TO INCREASE PO INTAKE FULL GLASS OF WATER WITH MED WATER WILL DECREASE GI SYMPTOMS OTHER MEDS ◦ LOOK FOR CONTRAINDICATED MEDS ◦ LOOK FOR HERBAL INTERACTIONS Winter 2013 26

CHARACTERISTICS OF ANTIBACTERIALS BROAD SPECTRUM NARROW SPECTRUM MECHANISM OF ACTION Winter 2013 27

BROAD SPECTRUM ANTIBIOTIC AN ANTIBIOTIC THAT IS EFFECTIVE AGAINST BOTH GRAM-NEGATIVE AND GRAM-POSITIVE BACTERIAL SPECIES BROAD-SPECTRUM INCLUDE AGENTS ◦ CARBAPENEMS ◦ EXTENDED-SPECTRUM CEPHALOSPORINS ◦ BETA-LACTAM/BETA-LACTAMASE INHIBITOR COMBINATIONS ◦ FLUOROQUINOLONES Winter 2013 28

AN NARROW SPECTRUM ANTIBIOTIC EFFECTIVE AGAINST A LIMITED NUMBER OF MICROORGANISMS. EXAMPLES OF NARROW-SPECTRUM AGENTS INCLUDE PENICILLIN G MACROLIDES NITROFURANTOIN METRONIDAZOLE AZTREONAM NALIDIXIC ACID Winter 2013 29

MECHANISMS OF ACTION Inhibition of bacterial cell wall synthesis Inhibition of protein synthesis Disruption of cell membranes Inhibits cell reproduction Inhibits cell metabolism Winter 2013 30

Antibiotics: Sulfonamides One of the first groups of antibiotics ◦ Sulfadiazine ◦ Sulfamethoxazole ◦ Sulfisoxazole Often combined with another antibiotic ◦ Sulfamethoxazole combined with trimethoprim (a nonsulfonamide antibiotic), known as Bactrim, Septra, or co-trimoxazole (SMX-TMP) ◦ This combination is used commonly Winter 2013 31

Sulfonamides: Mechanism of Action Bacteriostatic action Prevent synthesis of folic acid required for synthesis of purines and nucleic acid Do not affect human cells or certain bacteria Only affect organisms that synthesize their own folic acid Winter 2013 32

Sulfonamides: Indications Effective against both gram-positive and gram-negative bacteria Treatment of UTIs caused by susceptible strains of: ◦ Enterobacter , Escherichia coli, Klebsiella , Proteus mirabilis, Proteus vulgaris, Staphylococcus aureus Winter 2013 33

Sulfonamides: Indications (cont’d) Urinary Upper tract infections respiratory tract infections Winter 2013 34

Sulfonamides: Adverse Effects Body System Blood Integumentary Johnson Adverse Effects Hemolytic and aplastic anemia, agranulocytosis, thrombocytopenia Photosensitivity, exfoliative dermatitis, Stevenssyndrome, epidermal necrolysis Winter 2013 35

Sulfonamides: Adverse Effects (cont’d) Body System GI Other Adverse Effects Nausea, vomiting, diarrhea, pancreatitis Convulsions, crystalluria, toxic nephrosis, headache, peripheral neuritis, urticaria http: //www. youtube. com/watch? v=if. QMm 2 xuyqc&playn ext=1&list=PL 27024 F 7449 C 9 E 999&feature=results_ main Winter 2013 36

Beta-Lactam Antibiotics Penicillins Cephalosporins Carbapenems Monobactams Winter 2013 37
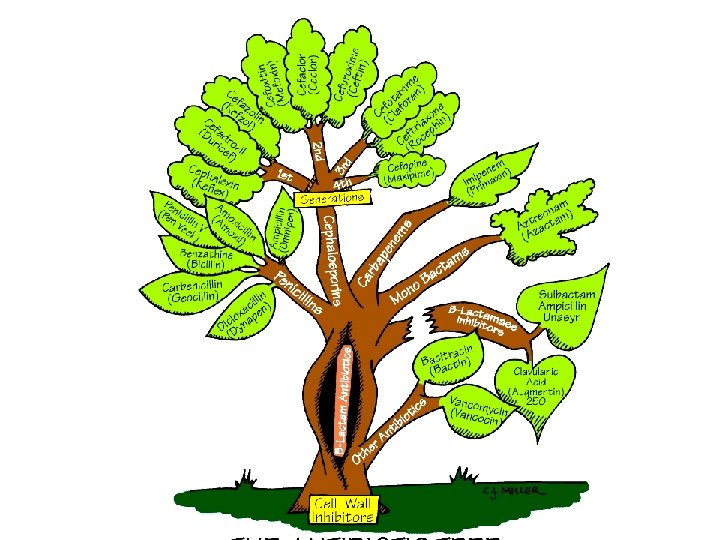
Winter 2013 38

Penicillins First introduced in the 1940 s Bactericidal: inhibit cell wall synthesis Kill a wide variety of bacteria Bacteria produce enzymes capable of destroying penicillins ◦ These enzymes are known as betalactamases ◦ As a result, the medication is not effective Winter 2013 39

Penicillins Natural penicillins Penicillinase-resistant penicillins Aminopenicillins Extended-spectrum penicillins Winter 2013 40

Penicillins (cont’d) Natural penicillins ◦ penicillin G, penicillin V potassium Penicillinase-resistant drugs ◦ cloxacillin, dicloxacillin, nafcillin, oxacillin Winter 2013 41

Penicillins (cont’d) Aminopenicillins ◦ amoxicillin, ampicillin Extended-spectrum drugs ◦ piperacillin, ticarcillin, carbenicillin ◦ Usually used with other drugs; rarely used alone Winter 2013 42

Penicillins (cont’d) Chemicals have been developed to inhibit these enzymes: ◦ Clavulanic acid ◦ Tazobactam ◦ Sulbactam These chemicals bind with betalactamase and prevent the enzyme from breaking down the penicillin, thus making the drug more effective Winter 2013 43

Penicillins (cont’d ) ( Penicillin–beta-lactamase inhibitor combination drugs Ampicillin + sulbactam = Unasyn ◦ Amoxicillin + clavulanic acid = Augmentin ◦ Ticarcillin + clavulanic acid = Timentin ◦ Piperacillin + tazobactam = Zosyn ◦ Winter 2013 44

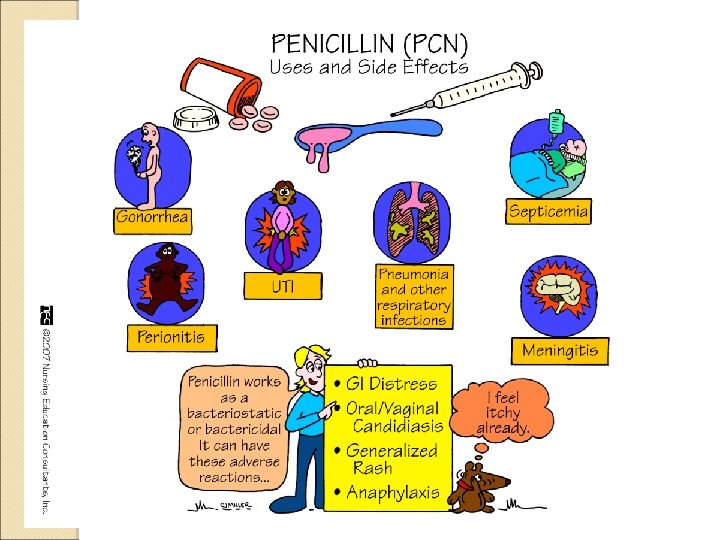
Penicillins: Indications Prevention and treatment of infections caused by susceptible bacteria, such as: ◦ Gram-positive bacteria ◦ Streptococcus, Enterococcus, Staphylococcus Winter 2013 45

Penicillins: Adverse Effects Allergic reactions occur in 0. 7% to 4% of cases ◦ Urticaria, pruritus, angioedema Those allergic to penicillins have a fourfold to sixfold increased risk of allergy to other beta-lactam antibiotics Cross-sensitivity between penicillins and cephalosporins is between 1% and 4% Winter 2013 46

Penicillins: Adverse Effects (cont’d) Common adverse effects ◦ Nausea, vomiting, diarrhea, abdominal pain Other adverse effects are less common Winter 2013 47

Penicillins: Interactions MANY interactions! ◦ NSAIDs ◦ Oral contraceptives – Decreases effectiveness ◦ Warfarin – Enhanced anticoagulant effect r/t decrease in intestinal flora producing vitamin K ◦ Others Winter 2013 48

MRSA METHICILLIN RESISTANT STAPHYLOCOCCUS AUREUS ◦ Hand washing and gloving ◦ Goal is to avoid healthcare associated infections ◦ “Colonized” means harbors the bacterial infection Winter 2013 49

NURSING CONSIDERATIONS FOR PENICILLIN ◦ Take with a full glass of water ◦ Do not skip doses ◦ Take all of the medication as prescribed ◦ Notify MD of adverse reactions Winter 2013 50
Winter 2013 51

Cephalosporins First generation Second generation Third generation Fourth generation Fifth generation (not yet marketed) Winter 2013 52

Cephalosporins (cont’d) Semisynthetic derivatives Structurally and pharmacologically related to penicillins Bactericidal action Broad spectrum Divided into groups according to their antimicrobial activity Winter 2013 53

Cephalosporins: First Generation Good gram-positive coverage Poor gram-negative coverage Parenteral and PO forms Examples ◦ ◦ cefadroxil cephradine cefazolin cephalexin Winter 2013 54

Cephalosporins: First Generation (cont’d) Used for surgical prophylaxis, and for susceptible staphylococcal infections ◦ cefazolin (Ancef and Kefzol): IV or IM ◦ cephalexin (Keflex): PO Winter 2013 55

Cephalosporins: Second Generation Good gram-positive coverage Better gram-negative coverage than first generation Examples: cefaclor cefprozil cefoxitin cefuroxime loracarbef cefotetan Winter 2013 56

Cephalosporins: Second Generation (cont’d) cefoxitin (Mefoxin): IV and IM ◦ Used prophylactically for abdominal or colorectal surgeries ◦ Also kills anaerobes cefuroxime ◦ Zinacef is parenteral form; Ceftin is PO ◦ Surgical prophylaxis ◦ Does not kill anaerobes Winter 2013 57

Cephalosporins: Third Generation Most potent group against gram-negative bacteria Less active against gram-positive bacteria Examples ◦ ceftibuten ◦ cefotaxime ◦ ceftazidime ◦ cefdinir ◦ ceftizoxime ◦ ceftriaxone ◦ ceftazidime Winter 2013 58

Cephalosporins: Third Generation (cont’d) ceftriaxone (Rocephin) ◦ IV and IM, long half-life, once-a-day dosing ◦ Elimination is primarily hepatic ◦ Easily passes meninges and diffused into CSF to treat CNS infections Winter 2013 59

Cephalosporins: Third Generation (cont’d) ceftazidime (Ceptaz) ◦ IV and IM forms ◦ Excellent gram-negative coverage ◦ Used for difficult-to-treat organisms such as Pseudomonas ◦ Eliminated by renal instead of biliary route ◦ Excellent spectrum of coverage ◦ Resistance is limiting usefulness Winter 2013 60

Cephalosporins: Fourth Generation Broader spectrum of antibacterial activity than third generation, especially against gram-positive bacteria Uncomplicated and complicated UTI ◦ cefepime (Maxipime) Winter 2013 61

Cephalosporins: Fifth Generation Ceftobipriole (not available) Broader spectrum of antibacterial activity Effective against a wide variety of organisms ◦ MRSA ◦ Pseudomonas Winter 2013 62

Cephalosporins: Adverse Effects Similar to penicillins ◦ Mild diarrhea, abdominal cramps, rash, pruritus, redness, edema Potential cross-sensitivity with penicillins if allergies exist Winter 2013 63

Carbapenems Very broad-spectrum antibacterial action Reserved for complicated body cavity and connective tissue infections May cause drug-induced seizure activity ◦ This risk can be reduced with proper dosage All given parenterally Winter 2013 64

Carbapenems imipenem/cilastatin (Primaxin) ◦ Used for treatment of bone, joint, skin, and soft-tissue infections; many other uses ◦ Cilastatin inhibits an enzyme that breaks down imipenem meropenem (Merrem) ertapenem (Invanz) doripenem (Doribax) Winter 2013 65

Monobactams Aztreonem (Azactam) Only drug in this catagory Beta-lactam antibiotic Gram negative bacteria ◦ Inhibits cell wall synthesis Common adverse effects Winter 2013 66

Macrolides erythromycin (E-mycin, E. E. S, others) azithromycin (Zithromax) ◦ “Z-Pack” 3 – 5 day dose pack clarithromycin (Biaxin) dirithromycin http: //www. youtube. com/watch? v=2 g-2 o. Lb 0 IQw&feature=related Winter 2013 67

Macrolides: Mechanism of Action Prevent protein synthesis within bacterial cells Considered bacteriostatic Bacteria will eventually die In high enough concentrations, may also be bactericidal Winter 2013 68

Macrolides: Indications Strep infections ◦ Streptococcus pyogenes (group A beta-hemolytic streptococci) Mild to moderate URI and LRI ◦ Haemophilus influenzae Spirochetal infections ◦ Syphilis and Lyme disease Gonorrhea, Chlamydia, Mycoplasma Winter 2013 69

Macrolides: Indications (cont’d) azithromycin and clarithromycin ◦ Recently approved for mycobacterium aviumintracellular complex infection (opportunistic infection associated with HIV/AIDS) clarithromycin ◦ Recently approved for use in combination with omeprazole for treatment of active ulcer disease associated with Helicobacter pylori infection Winter 2013 70

Macrolides: Indications (cont’d) Fidaxomicin (Dificid) ◦ Treatment of Clostridium difficileassociated diarrhea in adults ≥ 18 years of age. ◦ Following oral administration, only minimal systemic absorption occurs; remains mainly confined to and acts locally in the GI tract. Winter 2013 71

Macrolides: Adverse Effects GI effects, primarily with erythromycin ◦ Nausea, vomiting, diarrhea, hepatotoxicity, flatulence, jaundice, anorexia ◦ Newer drugs, azithromycin and clarithromycin: fewer GI adverse effects, longer duration of action, better efficacy, better tissue penetration Winter 2013 72

Ketolide telithromycin (Ketek) ◦ Only drug in this class ◦ Better antibacterial coverage than macrolides ◦ Active against gram-positive bacteria, including multi–drug-resistant strains of S. pneumoniae ◦ Associated with severe liver disease ◦ Use is limited Winter 2013 73

Tetracyclines demeclocycline (Declomycin) oxytetracycline doxycycline (Doryx, Vibramycin) minocycline tigecycline (Tygacil) Winter 2013 74

Tetracyclines (cont’d) Natural and semisynthetic Obtained from cultures of Streptomyces Bacteriostatic—inhibit bacterial growth Inhibit protein synthesis Stop many essential functions of the bacteria Winter 2013 75

Tetracyclines: Indications Broad spectrum ◦ Gram-negative and gram-positive organisms, protozoa, Mycoplasma, Rickettsia, Chlamydia, syphilis, Lyme disease, acne, others Demeclocycline is also used to treat SIADH by inhibiting the action of ADH Winter 2013 76

Tetracyclines (cont’d) Bind (chelate) to Ca 2+ and Mg 2+ and Al 3+ ions to form insoluble complexes Thus, dairy products, antacids, and iron salts reduce oral absorption of tetracyclines Should not be used in children under age 8 or in pregnant/lactating women because tooth discoloration will occur if the drug binds to the calcium in the Winter 2013 77

Tetracyclines: Adverse Effects Strong affinity for calcium ◦ Discoloration of permanent teeth and tooth enamel in fetuses and children, or nursing infants if taken by the mother ◦ May retard fetal skeletal development if taken during pregnancy ◦ http: //www. youtube. com/watch? v=AMAq. U 7 MJ_sc Winter 2013 78

Tetracyclines: Adverse Effects (cont’d) Alteration in intestinal flora may result in: ◦ Superinfection (overgrowth of nonsusceptible organisms such as Candida) ◦ Diarrhea ◦ Pseudomembranous colitis Winter 2013 79

Tetracyclines: Adverse Effects (cont’d) May also cause: ◦ Vaginal candidiasis ◦ Gastric upset ◦ Enterocolitis ◦ Maculopapular rash ◦ Other effects Winter 2013 80

Winter 2013 81

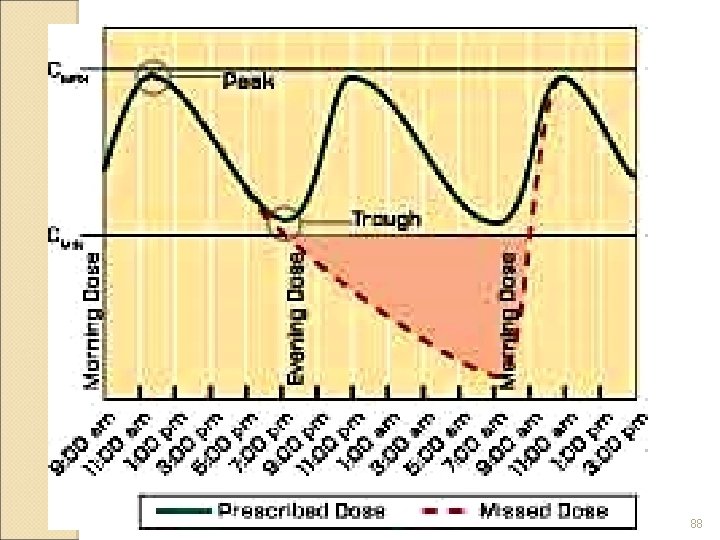
Antibiotic Therapy: Toxicities Ototoxicity ◦ Temporary or permanent hearing loss, balance problems Nephrotoxicity ◦ Varying degrees of reduced renal function ◦ Rising serum creatinine may indicate reduced creatinine clearance Monitor trough levels every 5 to 7 days while on therapy or as ordered Monitor serum creatinine levels at least every 3 days as an index of renal function Winter 2013 82

Aminoglycosides gentamicin (Garamycin) neomycin (Neo-fradin) tobramycin (Nebcin) amikacin (Amikin) kanamycin streptomycin Winter 2013 83

Aminoglycosides (cont’d) Natural and semisynthetic Produced from Streptomyces Poor oral absorption; no PO forms Very potent antibiotics with serious toxicities Bactericidal; prevent protein synthesis Kill mostly gram-negative bacteria; some gram-positive also Winter 2013 84

Aminoglycosides: Indications Used to kill gram-negative bacteria such as Pseudomonas, E. coli, Proteus, Klebsiella, Serratia Often used in combination with other antibiotics for synergistic effects Used for certain gram-positive infections that are resistant to other antibiotics Winter 2013 85

Aminoglycosides: Indications (cont’d) Aminoglycosides are poorly absorbed through the GI tract, and given parenterally Exception: neomycin ◦ Given orally to decontaminate the GI tract before surgical procedures ◦ Also used as an enema for this purpose Winter 2013 86

Aminoglycosides: Adverse Effects Cause serious toxicities ◦ Nephrotoxicity (renal damage) ◦ Ototoxicity (auditory impairment and vestibular impairment [eighth cranial nerve]) Must monitor drug levels to prevent toxicities Winter 2013 87
Winter 2013 88

Aminoglycosides: Adverse Effects (cont’d) Ototoxicity and nephrotoxicity are the most significant ◦ Headache ◦ Paresthesia ◦ Fever ◦ Superinfections ◦ Vertigo ◦ Skin rash ◦ Dizziness Winter 2013 89

Quinolones ciprofloxacin (Cipro) norfloxacin (Noroxin) levofloxacin (Levaquin) moxifloxacin (Avelox) Winter 2013 90

Quinolones (cont’d) Also called “fluoroquinolones” Excellent oral absorption Absorption reduced by antacids Effective against gram-negative organisms and some grampositive organisms Winter 2013 91

Quinolones: Mechanism of Action Bactericidal Alter DNA of bacteria, causing death Do not affect human DNA Winter 2013 92

Quinolones: Indications Gram-negative bacteria such as pseudomonas Respiratory infections Bone and joint infections GI infections Skin infections Sexually transmitted diseases Anthrax Winter 2013 93

Fluoroquinolones: Adverse Effects Body System CNS fatigue, GI increased Cardiac Adverse Effects Headache, dizziness, depression, restlessness, insomnia Nausea, vomiting, diarrhea, constipation, thrush, liver function studies, others Prolonged QT interval Winter 2013 94

Fluoroquinolones: Adverse Effects (cont’d ) ( Body System Integumentary Other vision, Adverse Effects Rash, pruritus, urticaria, flushing, photosensitivity (with lomefloxacin) Fever, chills, blurred tinnitus Black box warning: increased risk of tendonitis and tendon rupture Winter 2013 95

Other Antibiotics clindamycin (Cleocin) linezolid (Zyvox) metronidazole (Flagyl) nitrofurantoin (Macrodantin) quinupristin and Dalfopristin (Synercid) daptomycin (Cubicin) vancomycin (Vancocin) colistimethate (Coly-mycin) Winter 2013 96

Other Antibiotics (cont’d) clindamycin (Cleocin) ◦ Used for chronic bone infections, GU infections, intra-abdominal infections, other serious infections ◦ May cause pseudomembranous colitis Winter 2013 97

Other Antibiotics (cont’d) linezolid (Zyvox) ◦ New class: oxazolidinones ◦ Used to treat vancomycin-resistant Enterococcus faecium (VREF, VRE), hospital-acquired skin and skin structure infections, including those with MRSA ◦ May cause hypotension, serotonin syndrome if taken with SSRIs, and reactions if taken with tyramine-containing foods Winter 2013 98

Other Antibiotics (cont’d) metronidazole (Flagyl) ◦ Used for anaerobic organisms ◦ Intra-abdominal and gynecologic infections ◦ Protozoal infections ◦ Several drug interactions Winter 2013 99

Other Antibiotics (cont’d) nitrofurantoin (Macrodantin) ◦ Primarily used for UTIs (E. coli, S. aureus, Klebsiella , Enterobacter) ◦ Use carefully if renal function is impaired ◦ Drug concentrates in the urine ◦ May cause fatal hepatotoxicity ◦ Usually well-tolerated if patient is kept well -hydrated Winter 2013 100

Other Antibiotics (cont’d) quinupristin and dalfopristin (Synercid) ◦ 30: 70 combination, work synergistically ◦ Used for bacteremia and infections caused by vancomycin-resistant Enterococcus (VRE) and other complicated skin infections ◦ May cause arthralgias, myalgias Winter 2013 101

Other Antibiotics (cont’d) daptomycin (Cubicin) ◦ New class: lipopeptide ◦ Used to treat complicated skin and soft-tissue infections Winter 2013 102

Other Antibiotics (cont’d) vancomycin (Vancocin) ◦ Natural, bactericidal antibiotic ◦ Destroys cell wall ◦ Treatment of choice for MRSA and other gram-positive infections ◦ Must monitor blood levels to ensure therapeutic levels and prevent toxicity ◦ May cause ototoxicity and nephrotoxicity ◦ Should be infused over 60 minutes ◦ Rapid infusions may cause hypotension Winter 2013 103

Other Antibiotics (cont’d) vancomycin (Vancocin) (cont’d) ◦ Monitor IV site closely ◦ Red man syndrome may occur Flushing/itching of head, neck, face, upper trunk Antihistamine may be ordered to reduce these effects ◦ Ensure adequate hydration (2 L fluids/24 hr) if not contraindicated to prevent nephrotoxicity ◦ Monitor trough levels carefully Winter 2013 104

Nursing Implications It is ESSENTIAL to obtain cultures from appropriate sites BEFORE beginning antibiotic therapy Instruct patients to take antibiotics exactly as prescribed and for the length of time prescribed; they should not stop taking the medication early when they feel better Winter 2013 105

Nursing Implications (cont’d) Aminoglycosides ◦ Monitor peak and trough blood levels of these drugs to prevent nephrotoxicity and ototoxicity ◦ Symptoms of ototoxicity include dizziness, tinnitus, and hearing loss ◦ Symptoms of nephrotoxicity include urinary casts, proteinuria, and increased BUN and serum creatinine levels Winter 2013 106

ANTIVIRAL MEDICATIONS Winter 2013 107

Understanding Viruses Viral replication ◦ A virus cannot replicate on its own ◦ It must attach to and enter a host cell ◦ It then uses the host cell’s energy to synthesize protein, DNA, and RNA Winter 2013 108

Understanding Viruses (cont’d) Viruses are difficult to kill because they live inside the cells ◦ Any drug that kills a virus may also kill cells Winter 2013 109

Viral Illnesses Most viral illnesses are bothersome, but survivable Effective vaccines have prevented some illnesses Effective drug therapy is available for a small number of viral infections Winter 2013 110

Antiviral Drugs Antiviral drugs kill or suppress the virus by destroying virions or inhibiting ability to replicate viruses controlled by current antiviral therapy Winter 2013 111

Antiviral Drugs (cont’d) Viruses controlled by current antiviral therapy Cytomegalovirus (CMV) Hepatitis viruses Herpes viruses Human immunodeficiency virus (HIV) Influenza viruses (the “flu”) Respiratory syncytial virus (RSV) Winter 2013 112

Antiviral Drugs (cont’d) Key characteristics of antiviral drugs Able to enter the cells infected with virus Interfere with viral nucleic acid synthesis and/or regulation Some drugs interfere with ability of virus to bind to cells Some drugs stimulate the body’s immune system Winter 2013 113

Antiviral Drugs (cont’d) Opportunistic infections Occur in immunocompromised patients Would not normally harm an immunocompetent person Require long-term prophylaxis and antiinfective drug therapy Can be other viruses, fungi, bacteria, or protozoa Winter 2013 114

Antiviral Drugs (cont’d) Antiviral drugs ◦ Used to treat infections caused by viruses other than HIV Antiretroviral drugs ◦ Used to treat infections caused by HIV, the virus that causes AIDS Winter 2013 115

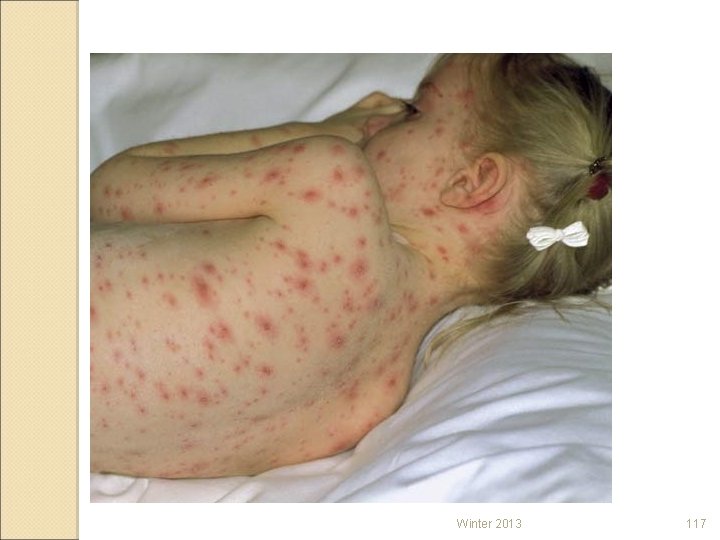
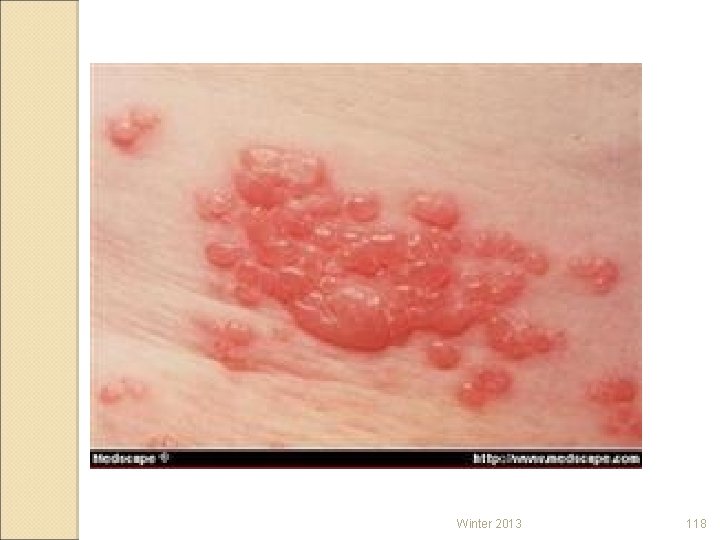
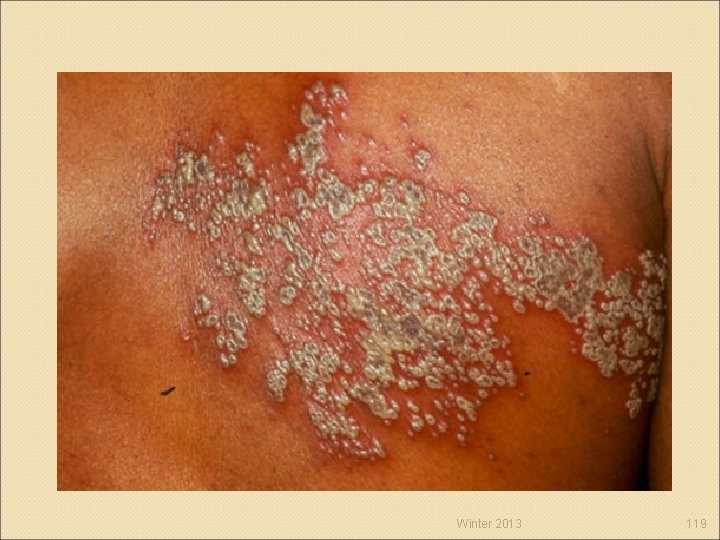
Virus Infections Herpes-simplex viruses ◦ HSV-1 (oral herpes) ◦ HSV-2 (genital herpes) Human herpesvirus/VZV ◦ Chickenpox and shingles (HHV-3 or VZV) Shingles http: //www. youtube. com/watch? v=MEvypt. IJsu E ◦ Epstein-Barr (HHV-4) ◦ Cytomegalovirus (HHV-5) ◦ Kaposi’s sarcoma (HHV-8) Winter 2013 116
Winter 2013 117
Winter 2013 118
Winter 2013 119

Antiviral Drugs (non-HIV) Mechanism of action ◦ Inhibit viral replication Used to treat non-HIV viral infections ◦ Influenza viruses ◦ HSV, VZV ◦ CMV ◦ Hepatitis A, B, C (HAV, HBV, HCV) Winter 2013 120

Antiviral Drugs (non-HIV) (cont’d) Adverse effects ◦ Vary with each drug ◦ Healthy cells are often killed also, resulting in serious toxicities Winter 2013 121

Antiviral Drugs (non-HIV) (cont’d) amantadine (Symmetrel) ◦ Narrow antiviral spectrum; active only against influenza A ◦ 2008 CDC guidelines do not recommend use for treatment or prevention of flu ◦ CNS effects: insomnia, nervousness, lightheadedness ◦ GI effects: anorexia, nausea, others Winter 2013 122

Antiviral Drugs (non-HIV) (cont’d) rimantadine (Flumadine) ◦ Same spectrum of activity, mechanism of action, and indications as amantadine ◦ Fewer CNS adverse effects ◦ Causes GI upset Winter 2013 123

Antiviral Drugs (non-HIV) (cont’d) acyclovir (Zovirax) ◦ Synthetic nucleoside analog ◦ Used to suppress replication of: HSV-1, HSV-2, VZV ◦ Drug of choice for treatment of initial and recurrent episodes of these infections ◦ Oral, topical, parenteral forms Winter 2013 124

Antiviral Drugs (non-HIV) (cont’d) ganciclovir (Cytovene) ◦ Synthetic nucleoside analog ◦ Used to treat infection with cytomegalovirus (CMV) ◦ Oral, parenteral forms ◦ CMV retinitis Ophthalmic form surgically implanted Ocular injection (fomivirsen) Winter 2013 125

Antiviral Drugs (non-HIV): Dose-Limiting Toxicities ganciclovir ◦ Bone marrow toxicity foscarnet and cidofovir ◦ Renal toxicity Winter 2013 126

Antiviral Drugs (non-HIV): Neuraminidase Inhibitors oseltamivir (Tamiflu) and zanamivir (Relenza) ◦ Active against influenza types A and B ◦ Reduce duration of illness ◦ Oseltamivir: causes nausea and vomiting ◦ Zanamivir: causes diarrhea, nausea, sinusitis ◦ Treatment should begin within 2 days of influenza symptom onset Winter 2013 127

Antiviral Drugs (non-HIV): Ribavirin Synthetic nucleoside analog Given orally, or oral or nasal inhalation Inhalation form (Virazole) used for hospitalized infants with RSV infections Winter 2013 128

HIV and AIDS Human immunodeficiency virus (HIV) infection and acquired immune deficiency syndrome (AIDS) ◦ ELISA (enzyme-linked immunosorbent assay) Detects HIV exposure based on presence of human antibodies to the virus in the blood ◦ Retrovirus ◦ Transmitted by sexual activity, intravenous drug use, perinatally from mother to child Winter 2013 129

Four Stages of HIV Infection* Stage 1: asymptomatic infection Stage 2: early, general symptoms of disease Stage 3: moderate symptoms Stage 4: severe symptoms, often leading to death *WHO model Winter 2013 130

Opportunistic Infections Protozoal ◦ Toxoplasmosis of the brain, others Fungal ◦ Candidiasis of the lungs, esophagus, trachea ◦ Pneumocystis jirovecii pneumonia, others Viral ◦ CMV disease, HSV infection, others Winter 2013 131

Opportunistic Infections (cont’d) Bacterial ◦ Various mycobacterial infections ◦ Extrapulmonary TB Opportunistic neoplasias ◦ Kaposi’s sarcoma, others HIV wasting syndrome ◦ Major weight loss, chronic diarrhea, chronic fever Winter 2013 132

Antiretroviral Drugs HAART Highly active antiretroviral therapy Includes at least three medications ◦ “Cocktails” These medications work in different ways to reduce the viral load Winter 2013 133

Antiretroviral Drugs (cont’d) Reverse transcriptase inhibitors (RTIs) ◦ Block activity of the enzyme reverse transcriptase, preventing production of new viral DNA Protease inhibitors (PIs) ◦ Inhibit the protease retroviral enzyme, preventing viral replication Fusion inhibitors ◦ Inhibit viral fusion, preventing viral replication Entry inhibitor-CCR 5 coreceptor antagonists HIV integrase strand transfer inhibitors Winter 2013 134

Antiretroviral Drugs (cont’d) Reverse (RTIs) transcriptase inhibitors ◦ Nucleoside RTIs (NRTIs) ◦ Nonnucleoside RTIs (NNRTIs) Examples ◦ abacavir (Ziagen) ◦ delavirdine (Rescriptor) ◦ didanosine (Videx) ◦ lefavirenze (Sustiva) Winter 2013 135

Antiretroviral Drugs (cont’d) zidovudine (Retrovir) ◦ First anti-HIV medication ◦ Nucleoside reverse transcriptase inhibitor ◦ Can be given to pregnant HIVpositive women and newborn babies to prevent maternal transmission of HIV ◦ Major dose-limiting adverse effect: bone marrow suppression Winter 2013 136

Antiretroviral Drugs (cont’d) Protease inhibitors (PIs) ◦ Inhibit the protease retroviral enzyme, preventing viral replication ◦ amprenavir (Agenerase) ◦ indinavir (Crixivan) ◦ nelfinavir (Viracept) ◦ ritonavir (Norvir) Winter 2013 137

Antiretroviral Drugs (cont’d) Fusion inhibitors ◦ Inhibit viral fusion, preventing viral replication ◦ A newer class of antiretroviral drugs ◦ Example: enfuvirtide (Fuzeon) Winter 2013 138

Antiretroviral Drugs (cont’d) CCR 5 antagonist ◦ maraviroc (Selzentry) HIV integrase strand transfer inhibitor ◦ raltegravir (Isentress) Winter 2013 139

Antiretroviral Drugs (cont’d) Combinations of multiple antiretroviral medications are common Adverse effects vary with each drug and may be severe; monitor for doselimiting toxicities Monitor for signs of opportunistic diseases Winter 2013 140

Nursing Implications Be sure to teach proper application technique for ointments, aerosol powders, and so on Emphasize hand washing before and after administration of medications to prevent site contamination and spread of infection Instruct patients to wear a glove or finger cot when applying ointments or solutions to affected areas Winter 2013 141

Antitubercular Drugs Winter 2013 142

Antitubercular Drugs Tuberculosis (TB) ◦ Caused by Mycobacterium tuberculosis Antitubercular drugs treat all forms of Mycobacterium Winter 2013 143

Mycobacterium Infections Common infection sites Lung (primary site) Brain Bone Liver Kidney Winter 2013 144

Mycobacterium Infections (cont’d) Aerobic bacillus Passed from infected: ◦ Humans ◦ Cows (bovine) and birds (avian) Much less common Winter 2013 145

Mycobacterium Infections (cont’d) Tubercle bacilli are conveyed by droplets Droplets are expelled by coughing or sneezing, and then gain entry into the body by inhalation Tubercle bacilli then spread to other body organs via blood and lymphatic systems Tubercle bacilli may become dormant, or walled off by calcified or fibrous tissue Winter 2013 146

Antitubercular Drugs First-line ◦ ◦ ◦ ◦ drugs isoniazid (INH)* ethambutol rifampin rifabutin pyrazinamide (PZA) Rifapentine streptomycin *Primary drug used Winter 2013 147

Antitubercular Drugs (cont’d) Second-line ◦ ◦ ◦ ◦ drugs capreomycin amikacin cycloserine levofloxacin ethionamide ofloxacin kanamycin para-aminosalicyclic acid (PAS) Winter 2013 148

Antitubercular Drug Therapy Considerations Perform drug-susceptibility testing on the first Mycobacterium that is isolated from a patient specimen to prevent the development of MDR-TB Even before the results of susceptibility tests are known, begin a regimen with multiple antitubercular drugs (to reduce chances of development of resistance) Winter 2013 149

Antitubercular Drug Therapy Considerations (cont’d ) ( Adjust drug regimen once the results of susceptibility testing are known Monitor patient compliance closely during therapy Problems with successful therapy occur because of patient nonadherence to drug therapy and the increased incidence of drugresistant organisms Winter 2013 150

Antitubercular Therapy Effectiveness depends upon: ◦ Type of infection ◦ Adequate dosing ◦ Sufficient duration of treatment ◦ Adherence to drug regimen ◦ Selection of an effective drug combination Winter 2013 151

Antitubercular Therapy (cont’d) Problems ◦ Drug-resistant organisms ◦ Drug toxicity ◦ Patient nonadherence Multidrug-resistant TB (MDR-TB) Winter 2013 152

Isoniazid (INH) Drug of choice for TB Resistant strains of Mycobacterium emerging Metabolized in the liver through acetylation—watch for “slow acetylators” Used alone or in combination with other drugs Contraindicated with liver disease Winter 2013 153

Adverse Effects INH ◦ Peripheral neuropathy, hepatotoxicity ethambutol ◦ Retrobulbar neuritis, blindness rifampin ◦ Hepatitis; discoloration of urine, stools, and other body fluids Winter 2013 154

Nursing Implications Perform liver function studies in patients who are to receive isoniazid or rifampin (especially in elderly patients or those who use alcohol daily) Winter 2013 155

Nursing Implications (cont’d) Patient education is critical Therapy may last for up to 24 months Take medications exactly as ordered, at the same time every day Emphasize the importance of strict adherence to regimen for improvement of condition or cure Winter 2013 156

Nursing Implications (cont’d) Remind patients that they are contagious during the initial period of their illness—instruct in proper hygiene and prevention of the spread of infected droplets Teach patients to take care of themselves, including adequate nutrition and rest Winter 2013 157

Nursing Implications (cont’d) Patients should not consume alcohol while on these medications or take other medications, including over-thecounter medications, unless they check with their physician Rifampin causes oral contraceptives to become ineffective; another form of birth control will be needed Winter 2013 158

Nursing Implications (cont’d) Patients who are taking rifampin should be told that their urine, stool, saliva, sputum, sweat, or tears may become reddish orange; even contact lenses may be stained Pyridoxine may be needed to combat neurologic adverse effects associated with INH therapy Oral preparations may be given with meals to reduce GI upset, even though recommendations are to take them 1 hour before or 2 hours after meals Winter 2013 159

Nursing Implications (cont’d) COMPLIANCE AND DOT THERAPY ◦ Because of the length of treatment, it is difficult to be sure patient will comply ◦ Family education may improve compliance ◦ DOT = DIRECT OBSERVATION THERAPY Winter 2013 160

Antifungal Drugs Winter 2013 161

Indications Systemic and topical fungal infections Drug of choice for the treatment of many severe systemic fungal infections is amphotericin B Choice of drug depends on type and location of infection Winter 2013 162

Adverse Effects: Amphotericin B Fever Chills Cardiac dysrhythmias Nausea and GI upset Renal toxicity Headache Malaise Hypotension Tingling, numbness in hands and feet Lowered potassium and Winter 2013 magnesium levels 163

Adverse Effects: Amphotericin B (cont’d) Main concerns: ◦ *Renal toxicity ◦ *Neurotoxicity: seizures and paresthesias Many other adverse effects Winter 2013 164

Nursing Implications (cont’d) amphotericin B ◦ To reduce the severity of the infusion-related reactions, pretreatment with an antipyretic (acetaminophen), antihistamines, antiemetics, and corticosteroids may be given ◦ Use an IV infusion pump Winter 2013 165
- Slides: 165