DRUG TREATMENT OF INFLAMMATORY BOWEL DISEASE Objectives n

DRUG TREATMENT OF INFLAMMATORY BOWEL DISEASE

Objectives n Describe the mechanism of action, pharmacokinetics and adverse effects of drugs in IBD

INFLAMMATORY BOWEL DISEASE n Ulcerative Colitis n Crohn’s disease

Inflammatory bowel disease n Inappropriate inflammatory response to intestinal microbes in a genetically susceptible host
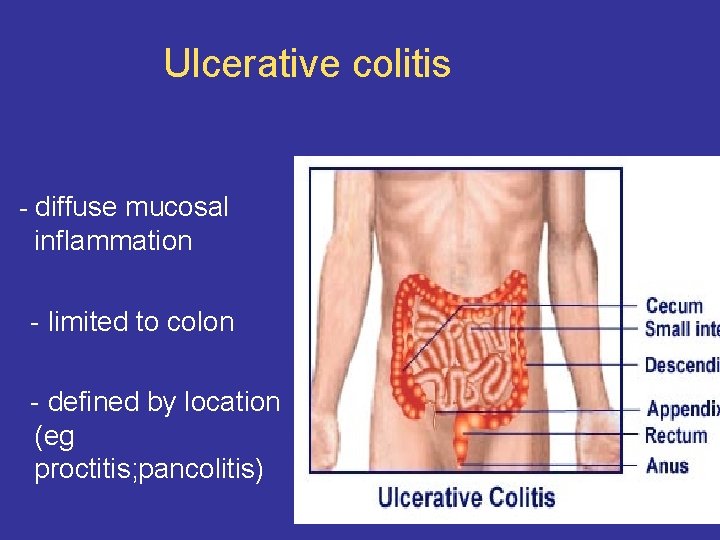
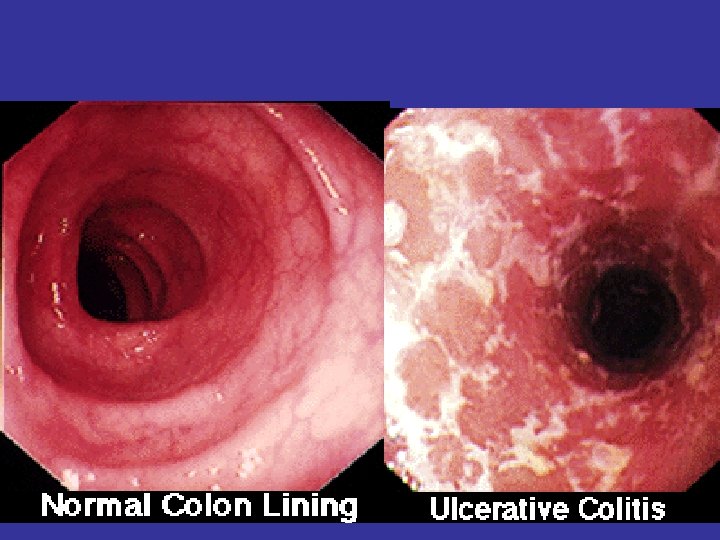
Ulcerative colitis - diffuse mucosal inflammation - limited to colon - defined by location (eg proctitis; pancolitis)
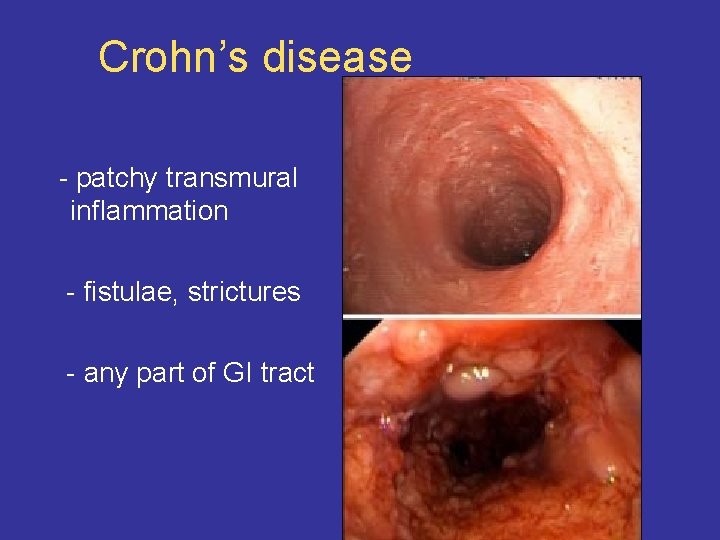
Crohn’s disease - patchy transmural inflammation - fistulae, strictures - any part of GI tract

AIMS OF THERAPY n Suppress inflammatory response n Suppress the immune reaction
n n Aminosalicylates Acute maintenance corticosteroids acute

Aminosalicylates • precise MOA unknown • act on epithelial cells • anti-inflammatory • modulate release of cytokines and reactive oxygen species
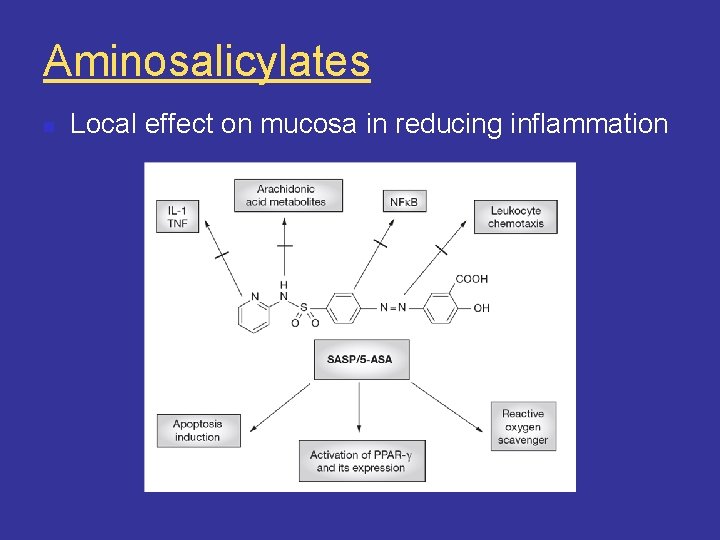
Aminosalicylates n Local effect on mucosa in reducing inflammation

Aminosalicylates Sulfasalazine Mesalamine Olsalazine

Aminosalicylates Sulfasalazine Mesalamine Olsalazine
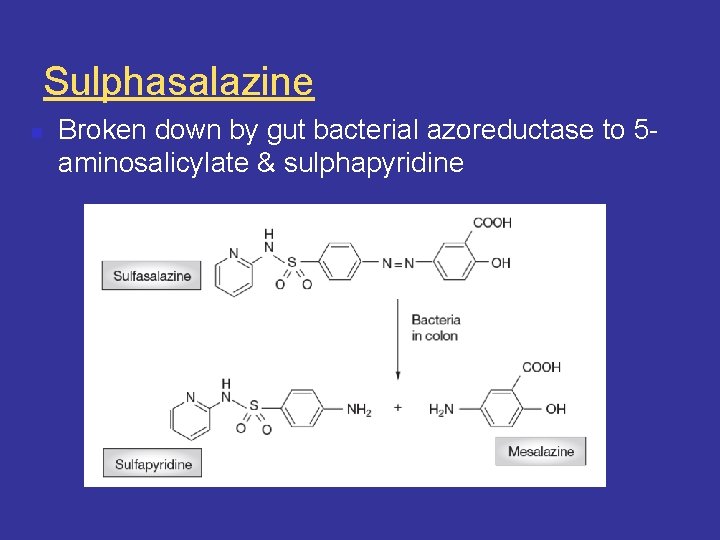
Sulphasalazine n Broken down by gut bacterial azoreductase to 5 aminosalicylate & sulphapyridine
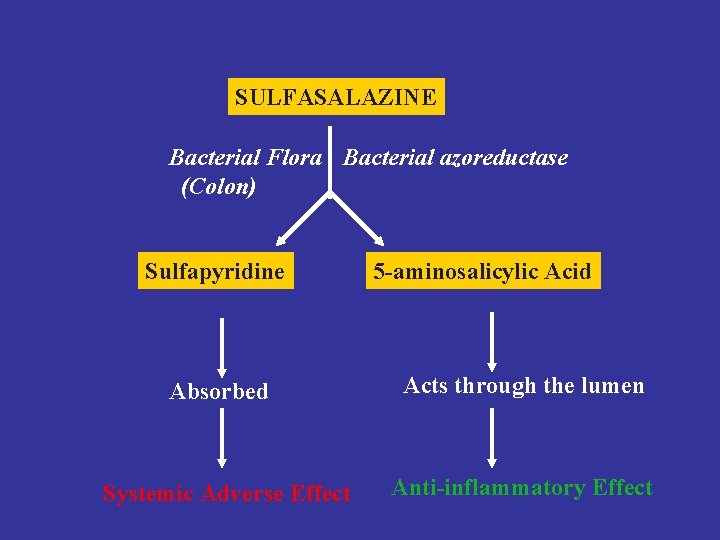
SULFASALAZINE Bacterial Flora Bacterial azoreductase (Colon) Sulfapyridine Absorbed Systemic Adverse Effect 5 -aminosalicylic Acid Acts through the lumen Anti-inflammatory Effect

Aminosalicylates n 5 -ASA absorbed in small intestine n Acetylated by N- acetyltransferase-1 n Excreted in urine

Indications n n Maintaining remission in UC Reduce risk of colorectal cancer by 75% (long term Rx for extensive disease) Less effective for maintenance in CD Inducing remission in mild UC/CD (higher doses)

Contraindications /cautions n n 5 -ASA - Salicylate hypersensitivity Sulfapyridine - G 6 PD deficiency (haemolysis) - Slow acetylator status ( risk of hepatic and blood disorders)

Adverse effects n n Dose-related Idiosyncratic (rare) - blood disorders - skin reactions – lupus like syndrome; Stevens-Johnson syndrome; alopecia

Blood disorders n n Agranulocytosis; aplastic anaemia; leucopenia; neutropenia; thrombocytopenia; methaemoglobinemia Patients should advised to report any unexplained bleeding; bruising; purpura; sore throat; fever or malaise
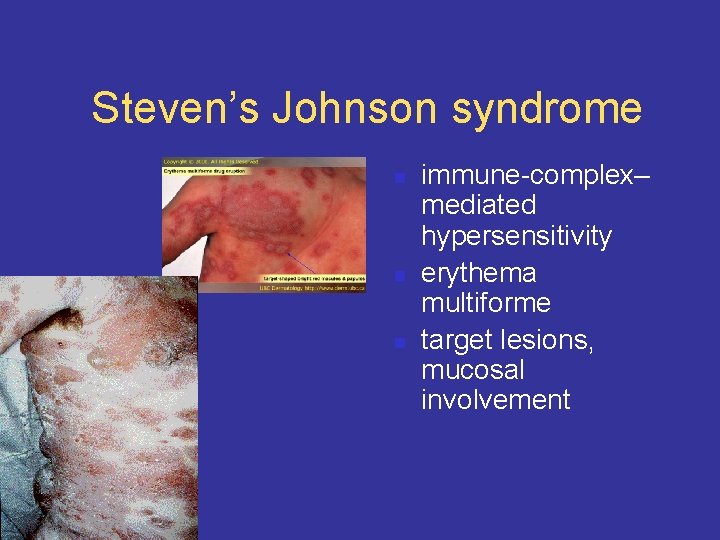
Steven’s Johnson syndrome n n n immune-complex– mediated hypersensitivity erythema multiforme target lesions, mucosal involvement

Newer formulations n Mesalazine (5 -ASA) n Balsalazide (a prodrug of 5 -ASA) n Olsalazine (5 -ASA dimer)

Mesalazine n Available as n n Enteric-coated tablets (for ileal Crohn’s disease) Slow release tablets (for proximal bowel Crohn’s) Enemas, suppositories (for distal colonic disease) Used when sulphasalazine can not be tolerated

Aminosalicylates Sulfasalazine § Oral use Mesalamine (5 -aminosalicylic acid). n n Oral delayed release capsules Enema Olsalazine. n n 5 -ASA-n=n-5 -ASA Bacterial flora breaks it into 5 -ASA

Anti-inflammatory & Immunosuppressive Drugs n Corticosteroids n Prednisolone n Hydrocortisone

Corticosteroids USES n Remission Induction n Route of Administration Oral Intravenous Topical (Enema)

Indications n Moderate to severe relapse UC & CD n No role in maintenance therapy n Combination oral and rectal

Immunomodulators n Azathioprine n Cyclosporine n Infliximab (Anti-TNF- )

Thiopurines Azathioprine n MOA: inhibit ribonucleotide synthesis; induce T cell apoptosis by modulating cell (Rac 1) signalling

Indications n Steroid sparing agents n Active disease CD/UC n Maintenance of remission CD/UC n Generally continue treatment x 3 -4 years

Ciclosporin n MOA: inhibitor of calcineurin preventing clonal expansion of T cells n Indicated in Severe UC n No value in CD

Methotrexate n n n MOA: inhibitor of dihyrofolate reductase; anti-inflammatory Inducing remission/preventing relapse in CD Refractory to or intolerant of Azathioprine

Infliximab n Indicated active and fistulating CD - in severe CD refractory or intolerant of steroids & immunosupressants - for whom surgery is inappropriate n MOA: anti-TNF monoclonal antibody n Potent anti-inflammatory

Antibiotics n n Metronidazole Ciprofloxacin Clarithromycin “Probiotics” (administration of “healthy” bacteria)

n Summary

Drugs for IBD n n n Aminosalicylates Glucocorticoids Immunosuppressives Cytokine modulators Antibiotics

Management of UC to induce remission 1. 2. 3. 4. oral +- topical 5 -ASA +- oral corticosteroids Azathioprine iv steroids/Colectomy/ ciclosporin (severe)

Maintaining remission 1. oral +- topical 5 -ASA 2. +- Azathioprine (frequent relapses)

Management of CD to induce remission 1. oral high dose of 5 -ASA 1. +- oral corticosteroids reducing over 8/52 2. Azathioprine 3. iv steroids/ metronidazole/elemental diet/surgery/infliximab

Maintaining remission +- Azathioprine (frequent relapses) Methotrexate (intolerant of azathioprine) Infliximab infusions (8 weekly)
- Slides: 40