Drug Overdose DO Overview September 2006 Intensive Care

Drug Overdose (DO) Overview September, 2006 Intensive Care United Christian Hospital

DO Evaluation • • Motive (intentional Vs incidental) Co-morbidity Related Drug Time of exposure and presentation Co-ingestion Other poison, corrosives exposure/ injury Symptoms & Vital Signs (VS)

DO Evaluation • Co-morbidity CVS: HT, IHD, arrhythmia, CHF Resp: Chronic respiratory insufficiency Renal: CRF GI: liver impairment, chronic hepatitis Alcoholism Drug addiction

DO Evaluation • Related Drug 1. Types (e. g. salicylates, CCB) 2. Amount (e. g. dose, concentration) 3. Single Vs Multiple dose 4. Formula, preparation e. g. liquid, dispersible, enteric-coated, sustained-release, IV 5. Time of exposure and presentation

DO Evaluation • Co-ingestion: (Maybe >2 agents) 1. paracetamol + salicylates 2. paracetamol + opioids 3. alcohol + paracetamol 4. alcohol + sedatives • Other poison, corrosives exposure/ injury 1. Carbon monoxide 2. Dettol 3. Bleaching agents 4. 通渠水
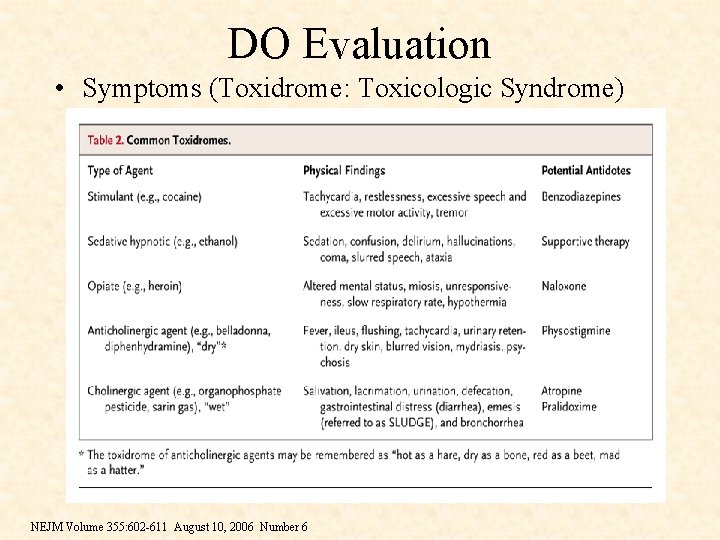

DO Evaluation • Symptoms (Toxidrome: Toxicologic Syndrome) NEJM Volume 355: 602 -611 August 10, 2006 Number 6

DO Evaluation • Hypothermia ethanol, sedatives, barbiturates, hypoglycaemics, opioids, carbon monoxide beta-blockers (BB) • Hyperthermia Cocaine, amphetamines, neuroleptics, anticholinergics, lithium, salicylates, sympathomimetics

DO Evaluation • Hypotension CCB, BB, antihypertensives, barbiturates, TCA, opioids, ethanol, theophylline, diuretics • Hypertension Amphetamine, cocaine, sympathomimetics, MAOI, anticholinergics, phenothiazines

DO Evaluation • Hyperventilation Amphetamine, cocaine, anticholinergics, ethanol, methaemoglobin inducers, salicylates, theophylline, isoniazid • Hypoventilation Barbiturates, opioids, colchicine, ethanol, sedative-hypnotics, TCA

DO Evaluation • Bradycardia CCB, BB, digoxin, opioids • Tachycardia Amphetamine, cocaine, anticholinergics, sympathomimetics, theophylline, TCA

DO Evaluation • • Bedside blood glucose test Sp. O 2 ECG Serum chemistry blood gas, electrolytes (e. g. Na, K, i. Ca 2+) R//LFT CBP, clotting profile Drug level Toxicology screen (blood, urine, gastric fluid) CXR/AXR

Management • • A, B, C GI Tract Decontamination Enhance Elimination Antidotes

GI Tract Decontamination • • Emesis Orogastric Lavage Activated Charcoal Whole Bowel Irrigation

Emesis Seldom use, have Risk • Acute ingestion of potentially toxic substance ( < 1 hr) • Only potentially useful in pre-hospital setting with long transport time to medical care

Orogastric Lavage (GL) • Large-bore fenestrated orogastric tube (3640 Fr) • Require protected airway • Amount of poison ingested is potentially life threatening • Within 60 minutes of ingestion (Except anticholinergic < 12 hr ingestion; salicylate < 24 hr ingestion)

Orogastric Lavage • Contraindications: Caustic/ Corrosive ingestion Large foreign bodies or sharp objects Airway not protected Suspected UGI injury Hypoxia

Activated Charcoal (AC) • One gram of activated carbon has the surface area (>400 m 2) of approximately two tennis courts (260 m 2) ! • Single Dose • Multiple Dose

Activated Charcoal (AC) • Used in: 1. Enterohepatic Circulation: Digoxin, amitriptyline, phenobarbitone, dozepin 2. Theophylline, salicylates

Activated Charcoal (AC) • Not bind well to: Lithium, strong acids and bases, and most inorganic minerals (examples of these are sodium, iron, lead), Alcohol (such as ethanol, methanol, isopropyl alcohol, and glycols), ammonia

Single Dose AC • ~1 gram/ Kg • Adult dose: 60 to 90 grams

Multiple Dose AC • Phenobarbital, dapsone, theophylline, digoxin, phyentoin, carbamazepine, aspirin • SR products, Enteric-coated product, Concretion formation • Enterohepatic circulation, low proetinbinding, long half-life • Dose: 0. 5 g/kg Q 2 -6 H (till “charcoal stools” and also depending on D. O. severity)

AC Contraindications • • I. O. Ileus GI perforation Loss of airway protection

Whole Bowel Irrigation (WBI) • mechanically flushing the ingested poison out of the gastrointestinal tract before it can be absorbed into the body • iso-osmolar solution of polyethylene glycol • Rate: 1 -2 L per hour (minimally) • P. O. or R/T • Entire procedure usually takes 4 to 6 hours • Till rectal effluent clear

Whole Bowel Irrigation (WBI) • • Indicatios: potentially toxic ingestion of substance that not well-absorbed by activated charcoal (e. g. Fe, Li, Pb, Zn) Sustained release/ Enteric coasted preparation Rising drug level despite GL/AC

Whole Bowel Irrigation (WBI) • Contraindications: I. O. Ileus GI perforation GIB Compromised airway

Enhance Elimination • Urinary alkalinization • Saline diuresis • Haemodialysis and haemoperfusion

Urinary alkalinization • By ion trapping mechanism • Urine p. H >7. 5 • Method: Stat 1 -2 m. Eq/kg of Na. HCO 3 Continuous infusion Na. HCO 3 in D 5 e. g. 1 LD 5+Na. HCO 3 150 mmol+ 40 mmol KCl Q 8 H Monitor serum p. H, avoid >7. 55 Maintain normokalaemia

Urinary alkalinization • • Salicylates Methotrexate Chlorpropamide Phenobarbital

Saline diuresis • Saline diuresis NOT equal to Forced diuresis • Forced diuresis: use diuretics to increase urinary elimination of toxin—generally NOT helpful • Saline diuresis For lithium

Antidotes • • • Acetaminophen Benzodiazepine Beta blockers Calcium blockers Iron or Aluminum Isonizide (INH) Methemoglobinemia Methanol Opioid TCA anti-depressants Coumarin N-acetylcysteine Flumazenil Glucagon Calcium Deferroxamine Vit B 6 Methylene bluce Alcohol Naloxone Sodium bicarbonate Vit K 1
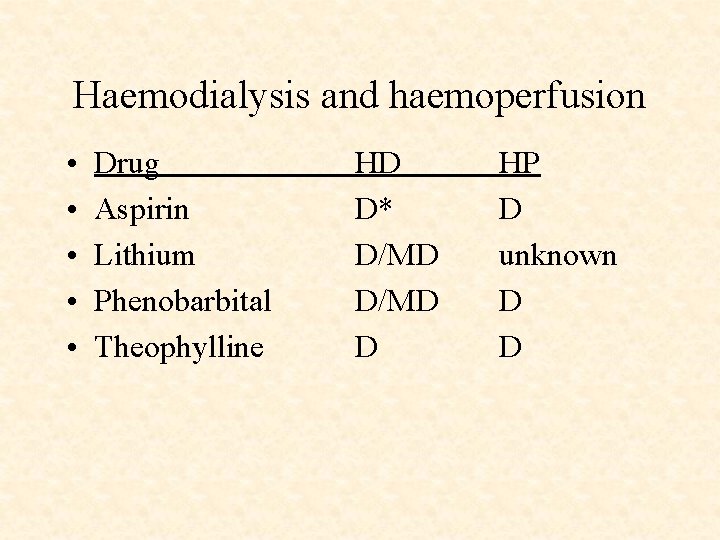
Haemodialysis and haemoperfusion • • • Drug Aspirin Lithium Phenobarbital Theophylline HD D* D/MD D HP D unknown D D

Haemodialysis and haemoperfusion • Not Useful in TCA Digoxin Valporic acid Dilantin

Drug Overdose • • • Antipyretic & Analgesic Antidepressants Cardiovascular Medications “Sleeping Pills” Antipsychotics, Neuroleptics & Mood Stabilizers • Hypoglycaemic Agents • Anticonvulsants

Antipyretic & Analgesic • Paracetamol • Salicylates • Non-Steroidal Anti-Inflammatory Drugs (NSAID)

Case 1 • • 28/F worked as clerk Non-drinker Thin-built Suicidal D. O. Claimed took 10 tab panadol + 40 tab 靈芝 丸 at 03: 00 attended AED 13: 00 • Panadol level at 13: 00 >150 mcg/ml • NAC started, developed rash, so stopped NAC temporally , given anti-histamine and resumed NAC at slower rate

Case 1 • • • INR 1. 5 --1. 7 -- > 2 AST rising trend p. H Normal INR still on rising trend AST > 3000 (peak) Transferred to QMH liver transplant team Responsive to medical Rx

Paracetamol

Paracetamol Only • • • Acetaminophen Tylenol, Tempra, Datril (USA) Panadol (UK, HK) 必理痛 Progesic Fortolin幸福止痛素

Medications with Paracetamol • Saridon 散利痛 250 mg paracetamol+65 mg caffeine • Dologesic 325 mg paracetamol+32. 5 mg dextropropoxyphene • Coltalin-ND, Coltalin cold tabs 幸福傷風素 325 mg paracetamol+phenylephrine+chlorpheniramine, etc

Paracetamol • International Union of Pure and Applied Chemistry (IUPAC) name: N-(4 -hydroxyphenyl)acetamide Other chemical names: N-acetyl-para-aminophenol and para-acetyl-aminophenol APAP • Chemical Formula: C 8 H 9 NO 2

Paracetamol • Pharmacokinetic data Absorption a) Peak serum levels i. 1 -2 hrs at therapeutic dose ii. 2 -4 hrs in overdose Bioavailability almost 100% Low protein binding

Paracetamol • Metabolism (therapeutic dose): 90 -95% hepatic t 1/2: 2 -3 hrs in therapeutic doses 1. >90% non-toxic sulfate & glucuronide conjugates 2. <5% by cytochrome P 450 2 E 1 to N-acetyl-parabenzoquinoneimine (NAPQI), strong oxidizing agent NAPQI is reduced by glutathione into non-toxic mercaptate conjugate

Paracetamol • Metabolism (Overdose) 90 -95% hepatic t 1/2: prolonged in overdose 1. non-toxic sulfate & glucuronide conjugates pathway(Saturated) 2. Increase in NAPQI, depletes glutathione stores-->NAPQI accumulate -->hepatocellular centribular necrosis and renal injury

Paracetamol • Factors favor NAPQI toxic pathway a) Enzyme inducers: smoking, barbiturates, phenytoin, INH, alcohol, carbamazepine b) Reduced glutathione stores: malnutrition, alcoholism, fasting, HIV, chronic disease, long-term use of paracetamol

Paracetamol Overdose • Clinical presentation • Toxic dose >150 mg/kg ; massive overdose >1 g/kg Phase 1 (0. 5 -24 h) minimal symptoms; metabolic acidosis in massive overdose Phase 2 (24 -72 h) RUQ pain, elevation of hepatic enzymes. 25% of hepatotoxic patients have impaired renal function Phase 3 (72 -96 h) marked hepatic dysfunction including hepatic encephalopathy. Death is related to hepatic failure Phase 4 (4 -14 days) resolution of hepatic dysfunction

Paracetamol Overdose Evaluation • History: Time of ingestion Amount ingested (150 mg/kg potentially toxic) • Serum level: 4 hrs post-ingestion/ as soon as possible thereafter Nomogram -Without NAC, 60% of those with initial drug level above toxic line will have aminotransferase > 1000 IU/L
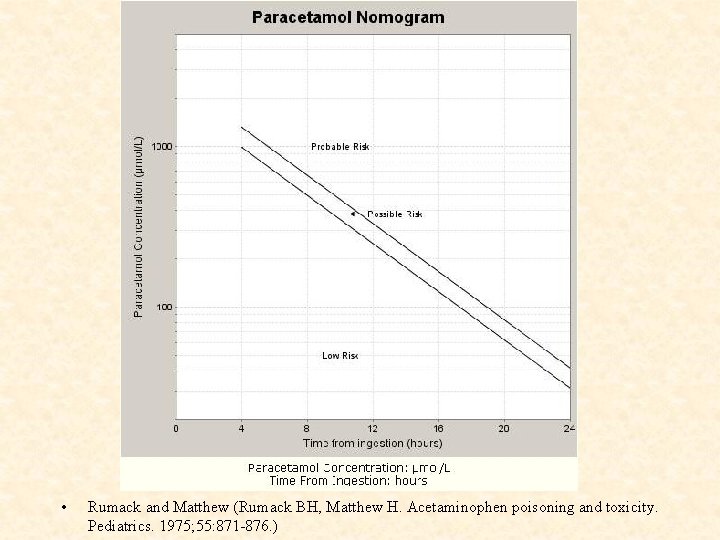
• Rumack and Matthew (Rumack BH, Matthew H. Acetaminophen poisoning and toxicity. Pediatrics. 1975; 55: 871 -876. )

Treatment of Paracetamol D. O. • Gastric lavage Consider only for coingestants • Activated charcoal Only of benefit within 4 hours of ingestion 1 gm/kg • N-acetylcysteine (NAC) Protection of NAC is 100% if given within 8 hrs of ingestion

N-acetylcysteine (NAC) • Mechanism: Precursor for glutathione Increase non-toxic sulfation metabolism Prevent covalent binding of NAPQI to hepatocytes • Dose: (Load)150 mg/ kg in 200 ml-500 ml D 5 over 15 min to 1 hr (then)50 mg/kg in 500 ml D 5 over 4 hrs (then)100 mg/kg in 1 L D 5 over 16 hrs

N-acetylcysteine (NAC) • Paracetamol level above treatment line • All patients with potentially hepatotoxic overdose (> 150 mg/kg). Treatment can be stopped if paracetamol concentration is below standard treatment line (Level taken >/=4 hr of ingestion & not extended release type) • All paracetamol ingestions who present late (>24 hours) with either detectable serum paracetamol or elevated tansaminases • All patients with evidence of severe toxicity or fulminant hepatic failure, regardless of time since overdose. Continue or start NAC 150 mg/kg/day until recovery from encephalopathy or patient dies • Chronic large ingestions (>4 g/day in adult), especially those who are high risk and deranged LFT

N-acetylcysteine (NAC) • Patients with history of asthma are more likely to have adverse drug reaction (~3 X) • Adverse drug reaction (Rash, bronchospasm, hypotension etc) to Nacetylcysteine is common (6 -23%), usually mild. Reduce dose Stop infusion and restart NAC at slower rate IV antihistamines +/- hydrocortisone

Paracetamol D. O. Prognosis 1. p. H < 7. 3 two days after overdose after adequate volume resuscitation 2. Coexistence PT>100 sec, serum Cr >300 umol/L, hepatic encephalopathy (Type III/IV) 3. Factor VIII/V ratio > 30 4. Serum lactate >3 mmol/L 5. Serum PO 4 > 1. 2 mmol/L 40 -92 hr post overdose

Paracetamol D. O. • Refer to specialist liver unit if INR > 2 at 24 hrs, 4 at 48 hrs or 6 at 72 hrs or if patient develops: hypoglycaemia, renal failure, acidosis, hypotension or encephalopathy

Paracetamol D. O. • Extended Relief Preparation • Current practice • check drug level a least 4 hours post ingestion 1. If the level is over nomogram line, treat with full course of NAC 2. If the level is under nomogram line, repeat in 4 hours a. If it is over the nomogram line, treat with full course of NAC b. If it is still under the nomogram line, no therapy

REFERENCE • http: //www. aic. cuhk. edu. hk/web 8/paracetamol. htm • Hong Kong Clinical Toxicology Course Book (New York City Poison Control Center, New York University & Bellevue Hospital Center; HK College of Emergency Medicine; HK Poison Information Centre) • http: //en. wikipedia. org/wiki/Paracetamol#Treatment • http; //www. emedicine. com

Case 2 • • • 18/F unemployed Attended AED x vomit Claimed “incidental” D. O. Got aspirin tab from Store Took 50 tab aspirin with beer ~ 4 hr before admission because of “headache” ? Co-ingestion ? Tab preparation ABG: mild resp. alkalosis Salicylates level: ~ 2. 2 mmol/L Panadol/ ethanol level unremarkable

Case 2 • • • ECG/ CXR/ AXR unremarkable GL at AED MDAC given Started vigorous fluid replacement Urine alkalinization Monitor Na. K blood gas Q 1 H K replacement given Monitor salicylates level Q 2 H-Q 4 H Salicylates level downtrend and symptoms subsided

Salicylates
Salicylates • 2 -Hydroxybenzoic acid • C 7 H 6 O 3 • Aspirin (acetylsalicylic acid) Doloxene Co, Cortal tab for adults • Methyl Salicylates (冬青油, 紅花油)

Salicylates • Absorption Rapid for methyl salicylates Prolonged for enteric coated tab or overdose • Peak Level 1 -2 hrs, maybe prolonged in overdose due to delayed gastric emptying, prolonged dissolution and concretion formation

Aspirin (acetylsalicylic acid) • Pharmacokinetic data Bioavailability: rapid & complete Protein binding: 99. 5% (in therapeutic dose) Half life: 300 -650 mg dose 3. 1 -3. 2 hours 1 g dose 5 hours 2 g dose 9 hours Metabolism: liver Excretion: renal

Salicylates • Weak acid (p. Ka=3. 0) • Remains ionised at p. H ~7. 4 • In overdose, acidosis develops, salicylates shift to non-ionised form and crosses bloodbrain barrier rapidly

Salicylates Overdose • Uncouples oxidative phosphorylation O 2 consumption rises Heat production> hyperthermia>increase energy demand>glycogenolysis, lipolysis>ketones, glucose>hypoglycaemia • Inhibits enzymes in Krebs cycle anaerobic metabolism>lactate and pyruvate

Salicylates Overdose • Initial respiratory alkalosis • Metabolic acidosis (lactate, ketone, salicylate)---> Mixed acid/base picture, p. H>7. 4, respiratory alkalosis predominant • Acidaemia (p. H<7. 4) severe ingestion, high morbidity, poor prognostic marker Vicious cycle (more non-ionised salicylates and free salicylates formation)

Salicylates Overdose • Dehydration and electrolyte imbalance Vomiting Diaphoresis Insensible water loss via tachypnoea Renal loss of Na, HCO 3 Hypokalaemia (renal loss)

Salicylates Overdose • • Toxicity depends on the amount ingested >150 mg/kg clinical toxicity 300 mg/kg severe toxicity >500 mg/kg potentially fatal

Salicylates Overdose • Acute overdose - Mortality rate of less than 2% (Higher in chronic overdose) • Drug Level: Acute>2. 2 mmol/L (30 mg/d. L): signs & symptoms +ve >7. 2 mmol/L (100 mg/d. L): need HD Chronic toxicity. Limited use, can be critically poisoned with level 50 mg/d. L (3. 6 mmol/L)

Salicylates Overdose Management • • A, B, C Volume (Fluid) resuscitation GL MDAC (2 -4 doses) WBI (enteric coated or concretion) Watch out for hyperthermia Urine alkalinization {Sign & Symptoms or level >40 mg/d. L (2. 9 mmol/L)} • HD

Salicylates Overdose - HD Indications • • Pulmonary edema Altered mental state Coagulopathy Clinical deterioration despite adequate supportive care • Inability or intolerable to urine alkalinization • Acute > 100 mg/d. L (7. 3 mmol/L) • Chronic >60 mg/d. L (4. 4 mmol/L)

Antidepressants • • • Tricyclic Antidepressants (TCA) Selective Serotonin Reuptake Inhibitors (SSRI) Monoamine Oxidase Inhibitors (MAOI) Mianserin (Tolvon) Venlafaxine (Efexor)

Tricyclic Antidepressants (TCA)

TCA • • • Amitriptyline clomipramine doxepin imipramine nortriptyline

TCA • Anticholinergic property: delayed absorption • Half-life: 10 -20 hrs • Highly protein bound: 85%-96%

TCA Overdose • In overdose: 1. fast inward sodium channel blockage: widen QRS, arrhythmia 2. anticholinergic effect: confusion, agitation, hyperthermia, tachycardia, dry skin, ileus, AROU, seizure, coma 3. alpha-adrenergic antagonist: vasodilation, hypotension 4. ant-GABA: seizure 5. anti-histamines: sedative

TCA Overdose ECG is mandatory NEJM Volume 313: 474 -479 August 22, 1985 Number 8 Boehnert & Lovejoy QRS duration limb leads QRS < 100 msec no significant toxicity QRS > 100 msec 1/3 had seizures QRS > 160 msec 1/2 had ventricular arrhythmia

TCA Overdose Management • A, B, C • GL, AC , MDAC Serum alkalinization (QRS>100 msec) Na. HCO 3 first dose (FR/Bolus) Endpoint: p. H 7. 5 -7. 55 • If not tolerate to Na/ fluid load, consider hyperventilation to induce respiratory alkalosis • Noradrenaline is the prefered vasopressor

TCA Overdose Management • Physostigmine and flumazenil are contraindicated • Dilantin is not recommended for seizure control Fails in animal study May exacerbate cardiotoxicity
Cardiovascular Medications • • Beta-blockers Calcium Channel Blockers Digoxin Wafarin

Case 3 • 85/F ADL-I • Known Hx of IHD, CHF, HT, renal impairment • Attended AED for dizziness and confusion • Na K i. Ca 2+ unremarkable • H”stix 3. 0 • BP 75/50 • AR 35 /min ECG: Junctional bradycardia • Sa. O 2 100% NRM
Case 3 • Reviewed medical Hx • Medication changed from betaloc 12. 5 mg bd to 50 mg QD for better BP control • Also on diltiazem 30 mg tds • But patient took 50 mg BD actually

Case 3 • • • Resuscitation Stat D 50 Trail of atropine, Ca. Cl--> not responsive Put on Temp. tranvenous pacing Given glucagon, HR/ BP normalised

Beta-blockers

Beta-blockers • • • Propranolol (Inderal) Tenormin Betaloc sotalol Carvidilol

Beta-blockers Overdose Antidote • Glucagon • Activates adenyl cyclase (Via Gs protein) • Initially 2 -5 mg IV slowly, repeated in 510 min if indicated up to max. total 10 mg • Continuous infusion: rate equal to minimal effective dose (mg/hr) • Monitor electrolytes and blood glucose • Watch out for VOMIT

Calcium Channel Blockers Ref: NEJM Volume 355: 602 -611 August 10, 2006 Number 6
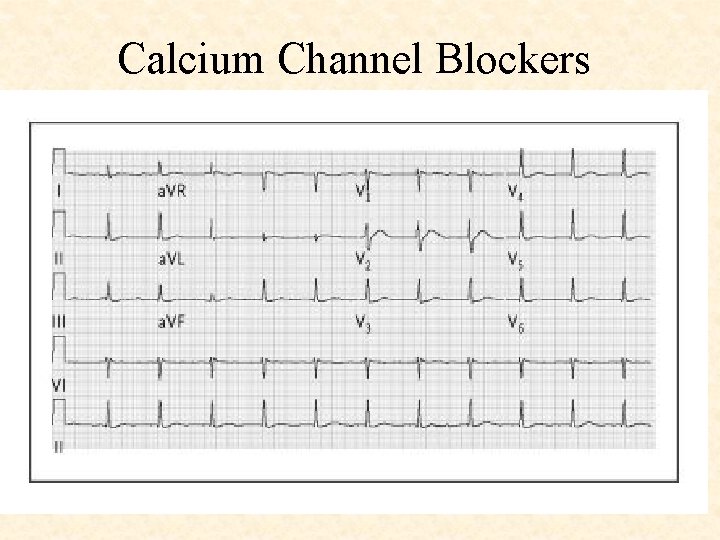
Calcium Channel Blockers

Calcium Channel Blockers Overdose • • A, B, C GL, WBI in selected case (e. g. SR formula) Volume Replacement Calcium Therapy a. Supratherapeutic doses of calcium salts b. 10 % calcium chloride solution yields 27 mg of elemental calcium per milliliter; an identical concentration of calcium gluconate yields a concentration of 9 mg per milliliter tissue necrosis if extravasation occurs

Calcium Channel Blockers Overdose • Circulatory Support atropine Temp. pacing Inotropes Vasopressors • Hyperinsulinemia–Euglycemia Therapy Hypothesis inherent activity of insulin as a positive inotrope, improving carbohydrate metabolism in cardiac myocytes

Hyperinsulinemia-Euglycemia Therapy and Other Options for the Treatment of an Overdose of Calcium-Channel Blockers Harris N. N Engl J Med 2006; 355: 602 -611

“Sleeping Pills” • • Benzodiazepines Zoplicone & Zolpidem Promethazine Diphenhydramine

Antipsychotics, Neuroleptics & Mood Stabilizers • • Antipsychotics/ Neurolpetics Lithium Valporic Acid Carbamazepine

Hypoglycaemic Agents • Sulfonylureas • Biguanides

Anticonvulsants • Valporic Acid • Phenytoin

Valporic Acid

Valporic Acid • Mechanism of action Increases GABA level Prolongs Na channel from recovery Affects fatty-acid metabolism and urea cycle

Valporic Acid • Absorption: fast, peak serum conc. 1 -4 hr • Protein binding: 85 -95% (reduced in acute overdose e. g. serum conc. > 150 mg/L protein binding < 70%) • Metabolism: Liver • Most are active metabolites, so toxicity will be ongoing even valporate serum level return to normal

Valporic Acid • Half-life: 8 -17 hrs, up to 30 hrs in acute overdose Serum Level Px >450 mg/L Serious intoxication >850 mg/L Coma >850 -1000 mg/L Metabolic acidosis

Valporic Acid • • • A, B, C GL, AC, WBI in selected case (e. g. chrono) L-carnitine HD Monitor electrolytes, glucose, R/LFT and ammonia level

• L-carnitine: -benefit, particularly in patients with concomitant hyperammonemia, encephalopathy, and/or hepatotoxicity -VPA combines L-carnitine, disrupting the longchain fatty acid metabolism - PO/IV administration and optimum dose of Lcarnitine not yet determined. -50 mg/kg slow IV stat then 50 mg/kg in 3 to 4 divided dose over next 24 hr then 50 mg/kg/day -oral 50 -100 mg/kg/day in divided dose, max 3 gm

Thank You
- Slides: 100