DRAFT For Discussion Purposes Only Infosys Consulting Health










- Slides: 27

DRAFT – For Discussion Purposes Only Infosys Consulting – Health. Care Provider / Payer COVID – 19 April 2020 1 © Infosys Consulting 2020

COVID-19 Statistics (as of 20 Apr 2020) GLOBAL STATISTICS USA STATISTICS • Number of Global Cases: 2, 416, 135 • Number of USA Cases: 770, 564 • Number of Deaths: 165, 939 • Number of Deaths: 41, 114 COVID-19 New Daily Cases Worldwide by Region Key Takeaway Business Disruption Across Ecosystem Patient Access As governments intensify restrictions business leaders are faced with the challenges of business continuity risks, sudden changes in volume, real-time decisionmaking, workforce productivity and security risks. Low income population is affected due to lack of primary care. 97% physician practices experienced revenue cut by half as patient volume declines. Exhausted Front Line Workers Consumer Debt Mentally and physically exhausted with long working hours, inadequate protection and risk of infection. Over 22, 000 front line workers are infected with over 100 deaths worldwide (till 15 Apr). (WHO) Increasing default by consumer on loans, due to joblessness. More than 1 in 4 Americans have trouble paying medical bills hence increased hesitance in getting treatment or undergoing medical tests. Financial Insolvency Hospital Care Supply Chain Worldwide frozen markets leading to credit crunch likely to be followed by corporate bankruptcy. 70% of US market is consumer driven and unemployment is predicted to rise by 20% in USA (Moody’s). Hospital routine services and elective surgeries have ceased, non essential staff are being furloughed. Supply Chain is disrupted. Sudden surge in demand for drugs, vitamins, antibiotics, and other medical necessities. Newer export and transport restrictions stranded supplies which hospitals need to fight infection. 2

COVID 19 - The World was Position for Pandemic On a global level the Healthcare Industry has been transitioning through a very disruptive time Pre-COVID-19 with a change in business model. A lot of factors are responsible for the current fragile state of Healthcare systems making the global environment ripe for a world wide pandemic. Global Travel Unrestricted global travel for reasons like business, tourism, religious and medical purpose helped spread the virus in every country on the map. Lack of Primary Care Primary care can take care of the majority of people’s healthcare needs. However, developed countries spend more on expensive infrastructure and specializations than inexpensive primary care, preventive medicine and generic medications. Fragile & Vulnerable Population • Expanding and aging populations. • 70% of the deaths worldwide are due to cancer, diabetes and heart diseases. • Economically unstable population with compromised immune system Medication Response • Development of micro-resistance in people against a ntivirals, antibiotics and antimalarial medications • Lack of access of vaccine in some while vaccine hesitancy in other cases due to lack of trust in vaccines Healthcare Infrastructure • • Rising labor cost and staff shortage Operating hospitals at close to capacity in order to maximize profits. Hospital beds/1000 people Japan – 13. 4 South Korea – 11. 5 Russia – 8. 2 Switzerland – 4. 7 China – 4. 2 Australia – 3. 8 Italy – 3. 4 USA – 2. 9 UK – 2. 8 3

Story from the front- Getting ready for COVID War I have just finished the night shift on the COVID-19 ward. I look at myself in the mirror: I have a C on my nose from the FFP 2 (N 95) mask I wear all the time, deep marks on my face left by the elastic bands; my eyes look tired, my hair is damp with sweat. I am not a doctor and a woman any longer — now I am just a doctor, a soldier in the war against the virus. ” “This is not a time for panic but a time for action driven by cooperation and concern for safety—not short-term profits “Before starting my shift, I have to don the protective gear — this is when I get the adrenaline rush: you are in the room with your colleagues, you try cracking a joke, but our eyes reflect our worry about protecting ourselves adequately as we carry out correctly all the steps in dressing: gloves, gown, second pair of gloves, glasses, cap, mask, visor, shoes, shoe covers…and tape over tape to keep everything sealed. The person who helps you dress writes your name and your role on your lab coat with a red marker, because when we are so costumed nobody recognizes anybody else. And when she says “Done, ” it’s time to enter the ward. ” 4

The pandemic could be an agent of change for the Healthcare industry Today Future Payer Industry wide call for value-based models instead of fee for service model & offering premier customer experience at low transparent costs. Quest for efficiency and control leading to mergers & acquisitions Increasing focus on making holistic Insurance Products, faster claims processing driven by technology. Urgent need of cybersecurity as work moves online & new ways of creating provider-payer contract. Provider Inadequate number of large government/private facilities with critical care units & ventilators, medical products and frontline workers. Increased adoption of Telehealth, RPM, focus on primary care, use of alternative medicine & improved provider to people ratio as per regions. Regulatory Agencies Regulatory bodies like CMS pushed towards value-based models, tightening HIPAA privacy guidelines & continued efforts to expand health coverage options esp. focused on Individual health market. Introduction of sweeping array of flexibilities, norms to expand care capacity and rapid measures to ramp up healthcare workforce. Supply Chain Just in time healthcare supply chain led to unavailability of gear needed to fight COVID. A lack of view from planning to procurement into the medical records. Agile processess envisioned and designed via the use of technology to deliver the better outcomes in the healthcare industry. Patient Eroding primary care and historical practice model of face to face care. Vaccine hesitancy and compromised immune system. Stress for heathy life-style, primary care and new entrants in healthcare provision like increased adoption of telehealth, medical devices and lower resistance to vaccine adoption. Diagnostic Inadequate technology, processess and resources to manage the dynamics of disease identification, categorisation and diagnosis. New enhanced technology, accelerate interoperability, and EHR used for disease diagnosis which result in better prognosis. 5

Impact and Actions – Health Care 6

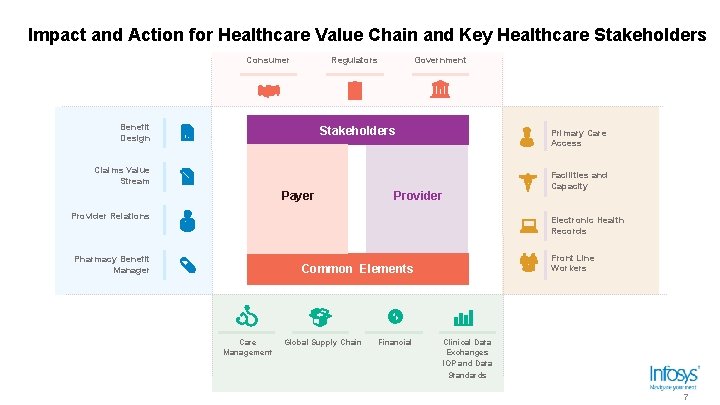
Impact and Action for Healthcare Value Chain and Key Healthcare Stakeholders Consumer Regulators Benefit Design Government Stakeholders Primary Care Access Claims Value Stream Payer Provider Relations Facilities and Capacity Electronic Health Records Pharmacy Benefit Manager Front Line Workers Common Elements Care Management Global Supply Chain Financial Clinical Data Exchanges IOP and Data Standards 7

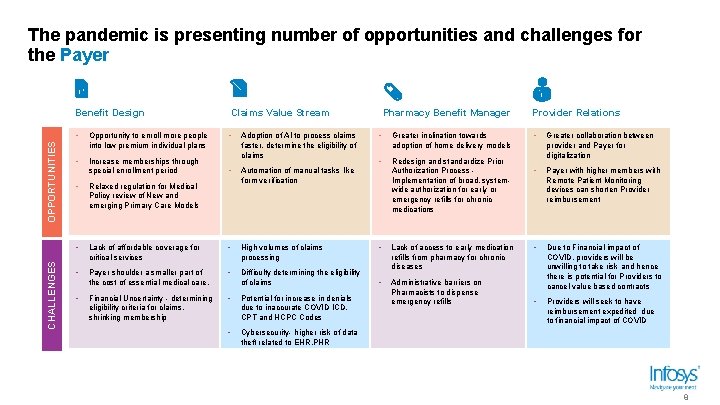
The pandemic is presenting number of opportunities and challenges for the Payer CHALLENGES OPPORTUNITIES Benefit Design • Opportunity to enroll more people into low premium individual plans • Increase memberships through special enrollment period • Adoption of AI to process claims faster, determine the eligibility of claims • Automation of manual tasks like form verification • Relaxed regulation for Medical Policy review of New and emerging Primary Care Models • Lack of affordable coverage for critical services • High volumes of claims processing • Payer shoulder a smaller part of the cost of essential medical care. • Difficulty determining the eligibility of claims Financial Uncertainty - determining eligibility criteria for claims, shrinking membership • Potential for increase in denials due to inaccurate COVID ICD, CPT and HCPC Codes • Cybersecurity- higher risk of data theft related to EHR, PHR • Pharmacy Benefit Manager Claims Value Stream • Greater inclination towards adoption of home delivery models • Redesign and standardize Prior Authorization Process Implementation of broad, systemwide authorization for early or emergency refills for chronic medications • Lack of access to early medication refills from pharmacy for chronic diseases • Administrative barriers on Pharmacists to dispense emergency refills Provider Relations • Greater collaboration between provider and Payer for digitalization • Payer with higher members with Remote Patient Monitoring devices can shorten Provider reimbursement • Due to Financial impact of COVID, providers will be unwilling to take risk and hence there is potential for Providers to cancel value based contracts • Providers will seek to have reimbursement expedited due to financial impact of COVID 8

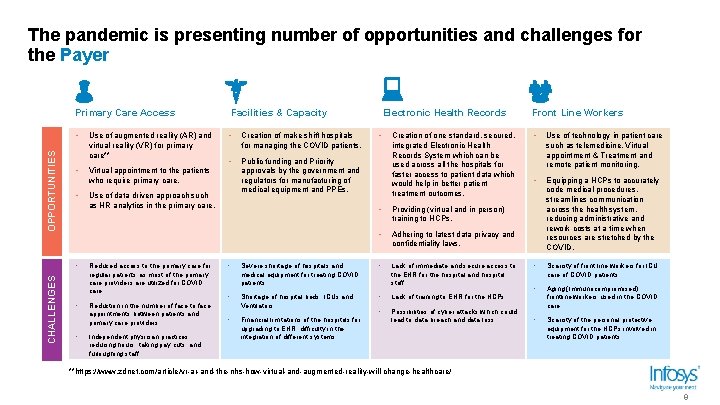
The pandemic is presenting number of opportunities and challenges for the Payer OPPORTUNITIES Primary Care Access • Use of augmented reality (AR) and virtual reality (VR) for primary care** • Virtual appointment to the patients who require primary care. • CHALLENGES • • Creation of make shift hospitals for managing the COVID patients. • Public funding and Priority approvals by the government and regulators for manufacturing of medical equipment and PPEs. Use of data driven approach such as HR analytics in the primary care. Reduced access to the primary care for regular patients as most of the primary care providers are utilized for COVID care. Reduction in the number of face to face appointments between patients and primary care providers. Independent physician practices reducing hours, taking pay cuts, and furloughing staff Electronic Health Records Facilities & Capacity • Creation of one standard, secured, integrated Electronic Health Records System which can be used across all the hospitals for faster access to patient data which would help in better patient treatment outcomes. • Providing (virtual and in person) training to HCPs. • Adhering to latest data privacy and confidentiality laws. • Severe shortage of hospitals and medical equipment for treating COVID patients. • Lack of immediate and secure access to the EHR for the hospital and hospital staff. • Shortage of hospital beds, ICUs and Ventilators. • Lack of training to EHR for the HCPs. • • Financial limitations of the hospitals for upgrading to EHR, difficulty in the integration of different systems, Possibilities of cyber attacks which could lead to data breach and data loss. Front Line Workers • Use of technology in patient care such as telemedicine, Virtual appointment & Treatment and remote patient monitoring. • Equipping a HCPs to accurately code medical procedures, streamlines communication across the health system, reducing administrative and rework costs at a time when resources are stretched by the COVID. • Scarcity of front line workers for ICU care of COVID patients. • Aging (Immunocompromised) frontline workers used in the COVID care. • Scarcity of the personal protective equipment for the HCPs involved in treating COVID patients. **https: //www. zdnet. com/article/vr-ar-and-the-nhs-how-virtual-and-augmented-reality-will-change-healthcare/ 9

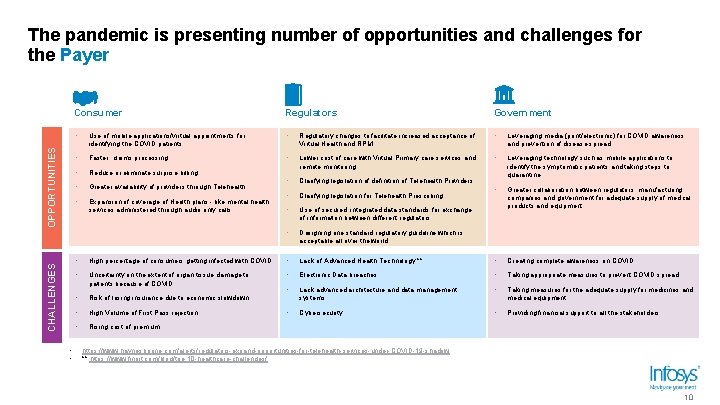
CHALLENGES OPPORTUNITIES The pandemic is presenting number of opportunities and challenges for the Payer • • Consumer Regulators Government • Use of mobile applications/virtual appointments for identifying the COVID patients. • Regulatory changes to facilitate increased acceptance of Virtual Health and RPM. • Leveraging media (print/electronic) for COVID awareness and prevention of disease spread. • Faster claims processing • Reduce or eliminate surprise billing Lower cost of care with Virtual Primary care services and remote monitoring • • • Greater availability of providers through Telehealth • Clarifying legislation of definition of Telehealth Providers Leveraging technology such as mobile applications to identify the symptomatic patients and taking steps to quarantine. Expansion of coverage of Health plans - like mental health services administered through audio only calls • Clarifying legislation for Telehealth Prescribing. • • • Use of secured, integrated data standards for exchange of information between different regulators. Greater collaboration between regulators, manufacturing companies and government for adequate supply of medical products and equipment. • Designing one standard regulatory guideline which is acceptable all over the world. • High percentage of consumers getting infected with COVID. • Lack of Advanced Health Technology ** • Creating complete awareness on COVID • Uncertainty on the extent of organ tissue damage to patients because of COVID. • Electronic Data breaches • Taking appropriate measures to prevent COVID spread. • Lack advanced architecture and data management systems. • Taking measures for the adequate supply for medicines and medical equipment. • Cybersecurity • Providing financial support to all the stakeholders • Risk of losing insurance due to economic slowdown • High Volume of First Pass rejection • Rising cost of premium https: //www. haynesboone. com/alerts/regulators-expand-opportunities-for-telehealth-services-under-COVID-19 -shadow ** https: //www. finoit. com/blog/top-10 -healthcare-challenges/ 10

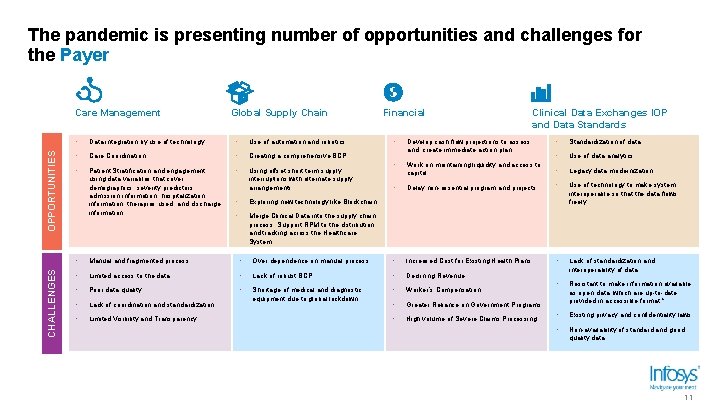
The pandemic is presenting number of opportunities and challenges for the Payer CHALLENGES OPPORTUNITIES Care Management Global Supply Chain • Data integration by use of technology • Use of automation and robotics. • Care Coordination • Creating a comprehensive BCP. • Patient Stratification and engagement using data variables that cover demographics, severity predictors, admission information, hospitalization information, therapies used, and discharge information. • Using offset short term supply interruptions with alternate supply arrangements • Exploring new technology like Blockchain • Merge Clinical Data into the supply chain process. Support RPM to the distribution and tracking across the Healthcare System Financial Clinical Data Exchanges IOP and Data Standards • Develop cash flow projections to assess and create immediate action plan • Standardization of data • Work on maintaining liquidity and access to capital • Use of data analytics • Legacy data modernization Delay non-essential program and projects • • Use of technology to make system interoperable so that the data flows freely • Lack of standardization and interoperability of data • Resistant to make information available as open data, which are up-to-date, provided in accessible format *. • Existing privacy and confidentiality laws. • Non-availability of standard and good quality data. • Manual and fragmented process • Over dependence on manual process. • Increased Cost for Existing Health Plans • Limited access to the data. • Lack of robust BCP • Declining Revenue • Poor data quality • • Worker’s Compensation • Lack of coordination and standardization Shortage of medical and diagnostic equipment due to global lockdown • Greater Reliance on Government Programs • Limited Visibility and Transparency • High volume of Severe Claims Processing 11

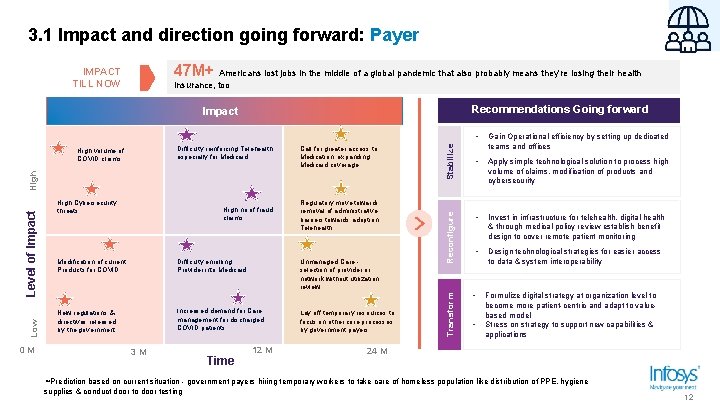
3. 1 Impact and direction going forward: Payer 47 M+ Americans lost jobs in the middle of a global pandemic that also probably means they’re losing their health IMPACT TILL NOW insurance, too Recommendations Going forward Low 0 M High Cybersecurity threats High no of fraud claims Modification of current Products for COVID Difficulty enrolling Provider into Medicaid Unmanaged Care selection of provider or network without utilization review Increased demand for Care management for discharged COVID patients New regulations & directives released by the government 3 M Time Regulatory move towards removal of administrative barriers towards adoption Telehealth 12 M Lay off temporary resources to focus on other core processes by government payers Reconfigure Level of Impact High volume of COVID claims Call for greater access to Medication, expanding Medicaid coverage Transform Difficulty reinforcing Telehealth, especially for Medicaid Stabilize Impact • • • Gain Operational efficiency by setting up dedicated teams and offices • Apply simple technological solution to process high volume of claims, modification of products and cybersecurity • Invest in infrastructure for telehealth, digital health & through medical policy review establish benefit design to cover remote patient monitoring • Design technological strategies for easier access to data & system interoperability Formulize digital strategy at organization level to become more patient-centric and adapt to valuebased model Stress on strategy to support new capabilities & applications 24 M Prediction based on current situation - government payers hiring temporary workers to take care of homeless population like distribution of PPE, hygiene supplies & conduct door to door testing 12

3. 1 Impact and direction going forward: Provider IMPACT TILL NOW $16 billion - estimated out-of-pocket costs for hospital stays & doctor visits Recommendations Going forward Increased reliance technology and on digital data Shortage of hospitals for COVID care Building makeshift hospitals for treating COVID patients Increased focus on Virtual treatment and preventive care Focusing on available patient data for treatment and better prognosis Complete revival and functioning of the hospitals Use of alternative methods such as digital platform for treating non-COVID patients Limited access to primary care 3 M Time 12 M • Creating awareness on COVID and taking appropriate measures to prevent disease spread. • Providing assistance to the HCPs by giving them PPE and financial support. • Develop strategies to leverage technology and EHR, e. PROs, e-diaries for disease and patient management. • Review Medical Malpractice to include Virtual Healthcare Services. • Increased focus on virtual treatment and moving towards preventive care. Transform Level of Impact Low 0 M Lack of Infrastructure for upgrading to EHR Stabilize Use of volunteers, recruiting retired HCPs and providing ICU crash courses to other physicians High Shortage of HCPs which is resulting in long working hours Reconfigure Impact • • • Increase Provider capacity through virtual Healthcare services and RPM. Use NLP/ML to create FAQ on consumer /patient portals to create social media medical neighborhoods to assist in self care. Maximize the usage of technology such as EHR, e. PROs, e -diaries for patient care. 24 M S&P estimates that Americans on insurer plans could wind up paying $3. 5 billion in out-of-pocket costs collectively under a moderate outbreak scenario, for hospital stays and doctor visits beyond initial testing. Under a severe outbreak, patient out-of-pocket costs could top $16 billion. 13

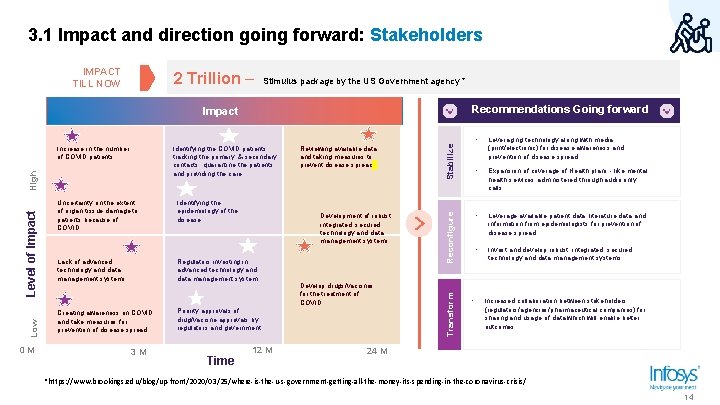
3. 1 Impact and direction going forward: Stakeholders IMPACT TILL NOW 2 Trillion – Stimulus package by the US Government agency * Recommendations Going forward Identifying the epidemiology of the disease Development of robust, integrated, secured technology and data management systems Lack of advanced technology and data management systems Regulators investing in advanced technology and data management system Creating awareness on COVID and take measures for prevention of disease spread Priority approvals of drug/vaccine approvals by regulators and government. 3 M Time 12 M Develop drugs/vaccines for the treatment of COVID. Reconfigure Level of Impact Low 0 M Uncertainty on the extent of organ tissue damage to patients because of COVID Reviewing available data and taking measures to prevent disease spread Transform Identifying the COVID patients, tracking the primary & secondary contacts, quarantine the patients and providing the care. High Increase in the number of COVID patients Stabilize Impact • • Leveraging technology along with media (print/electronic) for disease awareness and prevention of disease spread. • Expansion of coverage of Health plans - like mental health services administered through audio only calls • Leverage available patient data, literature data and information from epidemiologists for prevention of disease spread. • Invest and develop robust, integrated, secured technology and data management systems. Increased collaboration between stakeholders (regulators/agencies/pharmaceutical companies) for sharing and usage of data which will enable better outcomes. 24 M *https: //www. brookings. edu/blog/up-front/2020/03/25/where-is-the-u-s-government-getting-all-the-money-its-spending-in-the-coronavirus-crisis/ 14

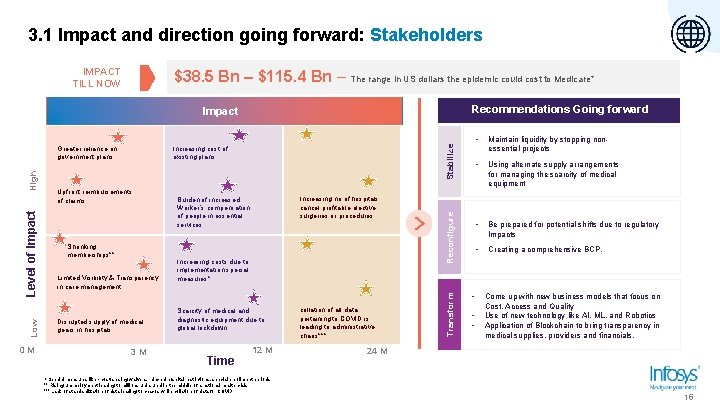
3. 1 Impact and direction going forward: Stakeholders IMPACT TILL NOW $38. 5 Bn – $115. 4 Bn – The range in US dollars the epidemic could cost to Medicare* Recommendations Going forward 0 M Upfront reimbursements of claims Shrinking memberships** Limited Visibility & Transparency in care management Disrupted supply of medical gears in hospitals 3 M Increasing no of hospitals cancel profitable elective surgeries or procedures Burden of increased Worker’s compensation of people in essential services Increasing costs due to implementation special measures* Scarcity of medical and diagnostic equipment due to global lockdown Time 12 M Special measures like - cost-sharing waivers, relaxed hospital restrictions, special enrollment periods ** Rising unemployment leading to millions uninsured in the middle of a national health crisis *** Lack of standardization of data leading to chaxos while collation of data for COVID collation of all data pertaining to COVID is leading to administrative chaos*** Reconfigure Increasing cost of existing plans Transform Low Level of Impact High Greater reliance on government plans Stabilize Impact • • Maintain liquidity by stopping nonessential projects • Using alternate supply arrangements for managing the scarcity of medical equipment • Be prepared for potential shifts due to regulatory Impacts • Creating a comprehensive BCP. Come up with new business models that focus on Cost, Access and Quality Use of new technology like AI, ML, and Robotics Application of Blockchain to bring transparency in medical supplies, providers and financials. 24 M 15

Digital – A new Frontier 16

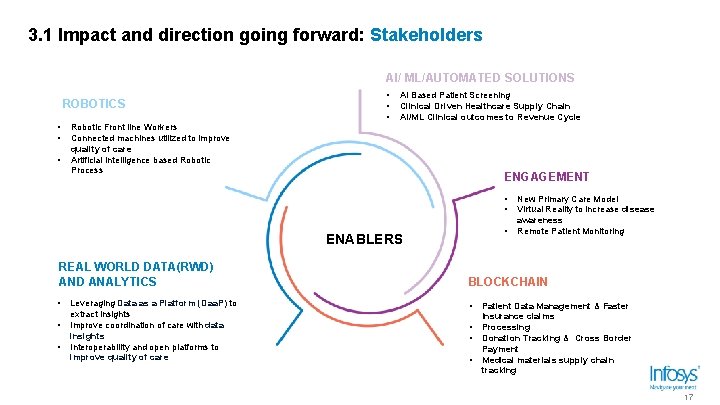
3. 1 Impact and direction going forward: Stakeholders AI/ ML/AUTOMATED SOLUTIONS ROBOTICS • • • AI Based Patient Screening Clinical Driven Healthcare Supply Chain AI/ML Clinical outcomes to Revenue Cycle Robotic Front line Workers Connected machines utilized to improve quality of care Artificial Intelligence based Robotic Process ENGAGEMENT • • • ENABLERS New Primary Care Model Virtual Reality to increase disease awareness Remote Patient Monitoring REAL WORLD DATA(RWD) AND ANALYTICS BLOCKCHAIN • • Leveraging Data as a Platform (Daa. P) to extract insights Improve coordination of care with data insights Interoperability and open platforms to improve quality of care • • • Patient Data Management & Faster Insurance claims Processing Donation Tracking & Cross Border Payment Medical materials supply chain tracking 17

AI/ ML/Automated solutions 1 2 COVID AI Patient Screening AI technologies being deployed in recent days and weeks are sensors to predict which COVID-19 patients are at risk of developing complications such as sepsis or respiratory failure and virtual clinical assistants to screen patients before they arrive at a facility • • • AI platform was able to analyze coughing sounds and crowd size collected by the handheld device in real-time, then use that data to accurately predict daily illness rates in each clinic, • 3 Assessment of Healthcare Supply Chain Advance prep work to meet the demands of the consumer and provider as the spread of COVID 19 has broken the weak links in the health care supply chain. Adoption of AI/ML provides new insights into a wide range of aspects Including logistics, warehouse management, collaboration, and supply chain Demand matching – A more transparent supply chain with full connections to clinical data will reveal weak points before they are stressed in times of crisis AI/ML in an clinical outcome based connected Revenue Cycle • Integrating improved outcomes to reimbursement , showing true costs incentivize health care stakeholders to commit to broader data sharing and integration. Implementing and integrating digital systems. • Medical text understanding of claims data through ML to reduce claim time and FWA claims by quickly identifying procedure inaccuracies. • Link Clinical outcomes to reimbursement across the health care supply chain 18

Robotics 1 • • 2 Robotic Front Line Workers Using Telepresence Robots to reduce the unnecessary risk to healthcare Workers. Telepresence robots ask basic questions, brief history to screen the possible COVID patient Utilized for repetitive tasks so focus is on more complex tasks 3 AI based Robotic Process • Smart machines that increase productivity for healthcare providers to get the information they need. • Robots are currently used in some surgical procedures, dispensing medications and transporting items within a Hospital • Test results and scan reports are immediate and can be shared with patient and doctor in realtime • Design human centered AI to develop autonomous Machines to expand robotic fleet. • ACO has introduced an AI based predictive model that analyzes patient demographics, social determinants of health, claims and clinical activity to determine which patients need the most outreach . Solution that autonomously navigate a hospital to perform collaborative tasks with nursing staff. Establish central management of growing robotic fleets, and create collaboration between Human Healthcare workers, Patients, and Robots Connected machines (IOT) utilized to improve quality of care • COVID has accelerated the use of Robotic front line workers. In a US Senior Care Facility in CT, a telepresence robot delivers items to residents and some have computer screen face to allow communication with Doctors, Nurses and family 19

Real World Data (RWD) and Analytics 1 • • • Leveraging Data as a Platform (Daa. P) to extract insights Daa. P – utilization to gain traction with value based care model proposed in the U. S. market Government leveraging large sets of data to review trends: • Ex: population health demographics, healthcare expenditures, diseases trends Create new product development for medical and consumer devices 2 Improve coordination of care with data insights • Improve financials reviewing claims data and improve payer / provider relationships • Leverage data to improve patients understanding of treatment plans • Big data analytics to examine unstructured data to uncover patient patterns and correlations 3 Interoperability and open platforms to improve quality of care • Fuel Internet of Medical Things (Io. MT) to bring together patient and performance data • Work group collaboration to improve processes and data control in research and academia • Increase partnership opportunities promoting a shared culture and mindset. 20

Engagement 1 Post COVID- New Primary Care Model 2 • Reducing physical barriers regardless of geographical area. Vital in pandemics like COVID-19 • Provider productivity and quality of care significantly increases. As well as a reduction in cost of care. • Providers are using AI based online screening and triage tools to assure that patients gain access to the right level of care • • • Virtual Reality to increase disease awareness Leveraging Virtual Reality for application with educational value: • Ex: Clinicians trained in 3 D surgical environment Creating new ways of assisting patients with pain management & mental illnesses find a better way to cope. 3 COVID – Remote Patient Monitoring • Continuous ongoing monitoring of patient vitals and relay information back to the Provider • A growing shift of Providers relying on wireless connectivity • The “smart pill’ – swallowed by patients to get real-time information on patient’s well-being. First smart pill approved in U. S. by FDA in 2017 Tele behavioral Health- Artificial intelligence and data analytics to power a comprehensive remote monitoring platform. 21

Blockchain 1 • • Patient Data Management & Faster Insurance claims Processing 2 Single source of information: securely manage health records ensuring interoperability without compromising patient privacy & security. Records include patients’ data, treatments given, and any progress detected. • Insurance claims: Blockchain-based collective claim-sharing platform can function to process coronavirus claims, helping the firm to reduce paperwork & back-and-forth document delivery to clinics & mitigate the risk of infection from face-to-face contact. • Donation Tracking & Cross Border Payment Donation-tracking platform: Distrust regarding donations has been an issue during COVID. With Blockchain, donors can see where funds are most urgently needed & track their donations until provided with a verification that their donations have been received. Cross-border payments: UN World Food Program introduced Blockchain technology for projects, such as distributing aid to vendors, arranging money transfers for more than 10, 000 refugees, and auditing beneficiary spending, it managed to reduce bank transfer fees by almost 98%. . 3 • • • Medical materials supply chain tracking Blockchain-based platforms can enable users to trace the demand the supply chains of medical supplies, included the recording and tracking of epidemic prevention materials, such as masks, gloves and other protective gear. Smart Contracts between stakeholders - rulebased protocols where contracts are executed when conditions are met. Blockchain can provide a mechanism for health systems to continually update factories with the latest product requirements and specifications, almost like a production auction. 22

Path Forward 23

Path Forward STABILIZE Address the near term and immediate needs to stabilize the industry needs RECONFIGURE Retool and reconfigure the approach, processes and tools to address the medium term challenges TRANSFORM Provide a clear roadmap around how the changes across the spectrum would impact your business 24

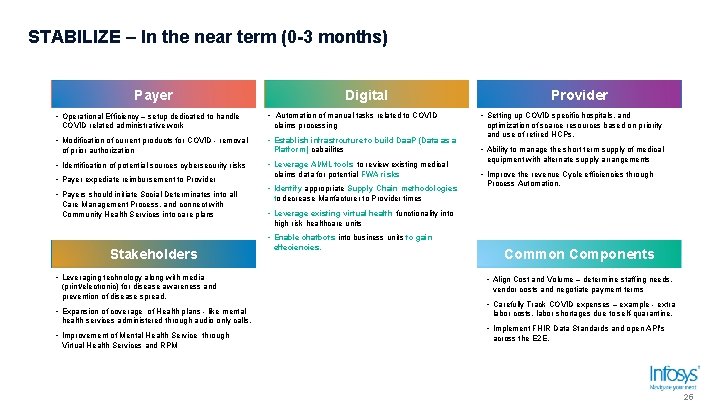
STABILIZE – In the near term (0 -3 months) Payer • Operational Efficiency – setup dedicated to handle COVID related administrative work • Modification of current products for COVID - removal of prior authorization • Identification of potential sources cybersecurity risks • Payer expediate reimbursement to Provider • Payers should initiate Social Determinates into all Care Management Process, and connect with Community Health Services into care plans Digital • Automation of manual tasks related to COVID claims processing • Establish infrastrcuture to build Daa. P (Data as a Platform) cabailites • Leverage AI/ML tools to review existing medical claims data for potential FWA risks • Identify appropriate Supply Chain methodologies Provider • Setting up COVID specific hospitals, and optimization of scarce resources based on priority and use of retired HCPs. • Ability to manage the short term supply of medical equipment with alternate supply arrangements • Improve the revenue Cycle efficiencies through Process Automation. to decrease Manfacturer to Provider times • Leverage existing virtual health functionality into high risk healthcare units • Enable chatbots into business units to gain Stakeholders • Leveraging technology along with media (print/electronic) for disease awareness and prevention of disease spread. • Expansion of coverage of Health plans - like mental health services administered through audio only calls. • Improvement of Mental Health Service through Virtual Health Services and RPM effeciencies. Common Components • Align Cost and Volume – determine staffing needs, vendor costs and negotiate payment terms • Carefully Track COVID expenses – example - extra labor costs, labor shortages due to self-quarantine. • Implement FHIR Data Standards and open API's across the E 2 E. 25

RECONFIGURE – In the medium term (4 -12 months) Payer • Business Continuity Plan - re-evaluate to deal with Digital • Use AI/ML to screen cases that need Care Management, eligibilty determinatin for COVID claims not just physical, natural disaster but also medical disaster like COVID, Improve access to care • Remove all cost for COVID Testing, Cover the cost of vaccines, removing co-pays for Vaccines • Submit plans to meet the new requirements to the State Department of Insurance and other regulatory agencies. • Use Cloud Services to implement a layered, indepth cyber-defense strategy across data and networks • Scale Daa. P across pipleline for high impact areas across all healthcare channels • AI/ML functionalites enabled to review more Provider • Investment in Information Technology which will help all the stakeholders involved in Healthcare industry • Expediate Interoperability across all facilities, functions, and workforce. • Review Medical Malpractice to include Virtual Healthcare Services • Develop a fully connected supply chain driven by clinical data, from Patient diagnosis to Discharge. complex with Predictive Analytics to reduce bottlenecks Stakeholders • Develop strategies to leverage technology and Electronic Health Records, e. PROs, e-diaries for disease management. • Invest in training of HCPs and building of infrastructure for chatbots, analytics, telemedicine, digital health and Remote Patient Monitoring (RPM). • Automate supply chain functionalites within various departments plus leverage Predictive Analytics to increase effciencies and meet consumer demands • Virtual health –continuously introduce healthcare applications to leverage RWD to improve quality of care Common Components • Develop a financial rescue plan and communicate to all stakeholders. • Use AI/Predictive Analytics to identify and managed the volume of COVID patients and create treatment protocols 26

RECONFIGURE – In the medium term (4 -12 months) Payer • • • Focus on expanding access to coverage to various group of population Follow an infrastructure strategy to support new capabilities and applications Patient – Centric Approach - Formulize digital strategy at organization level to become more patient-centric and adapt to value-based model Digital • • • Stakeholders • Increased collaboration between stakeholders (regulators/agencies/pharmaceutical companies) for sharing and usage of information. • Usage of Global Data Standards for exchange of data for consistent and credible analytics and reporting. • • AI and Automation to help free up more resources and time to focus on other core processes Integrate & provide access to patient record information, claims, benefits, costs, patient registration, and staff management for better claims processing Leverage cloud functionality with RWD and encourage data sharing while protecting patient identifiers with robust functionality Establish a mature Daa. P across all healthcare business units Build out a mature medical claims review process with AI/ML for FWA while introducing road maps and preventive measures Reimagine Supply Chain with digital tools to decrease overall costs and overhead Increase overall satisifaction of Patient and Provider with fully integrated virtual health capabilites Provider • Move from the traditional value based care to preventive care • Increase Provider capacity through virtual Healthcare services and remote patient monitoring • Use NLP/ML to create FAQ on consumer /patient portals to create social media medical neighborhoods to assist in self care • Evaluating the COLUMBIA-SUICIDE SEVERITY RATING SCALE for the HCPs and taking appropriate measures for HCPs recovery. Common Components • • • Introduce lower premium individual health plans to cover costs in case of pandemics like COVID. Introducing new business models that focus on Cost, Access and Quality Use of new technology like AI, ML, and Robotics etc. 27