Dr Toba kazemi Associate Professor of Cardiology BUMSBCRC

Dr. Toba kazemi Associate Professor of Cardiology BUMS-BCRC 17 Esfand 1390

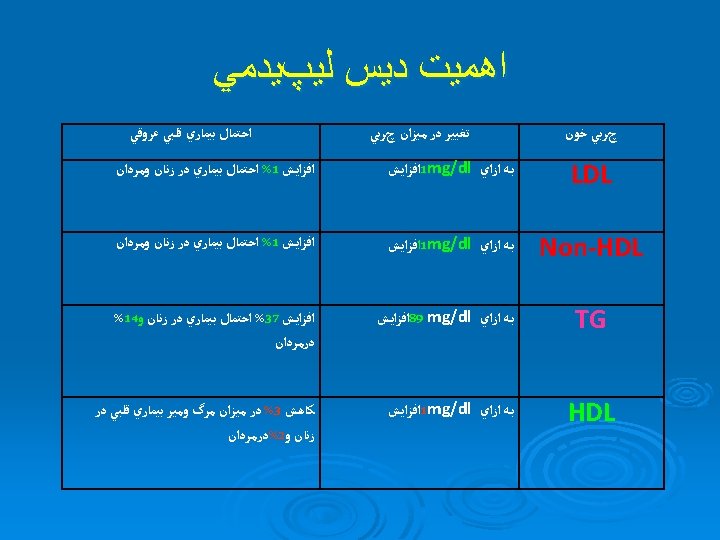
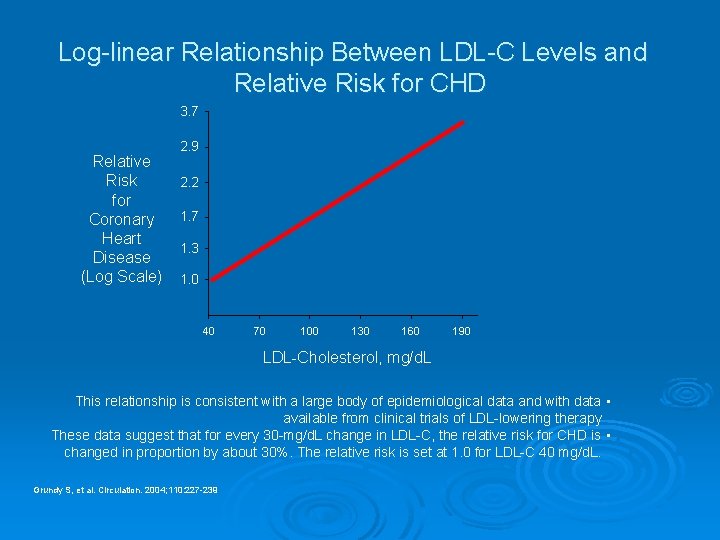
Log-linear Relationship Between LDL-C Levels and Relative Risk for CHD 3. 7 Relative Risk for Coronary Heart Disease (Log Scale) 2. 9 2. 2 1. 7 1. 3 1. 0 40 70 100 130 160 190 LDL-Cholesterol, mg/d. L This relationship is consistent with a large body of epidemiological data and with data • available from clinical trials of LDL-lowering therapy These data suggest that for every 30 -mg/d. L change in LDL-C, the relative risk for CHD is • changed in proportion by about 30%. The relative risk is set at 1. 0 for LDL-C 40 mg/d. L. Grundy S, et al. Circulation. 2004; 110: 227 -239
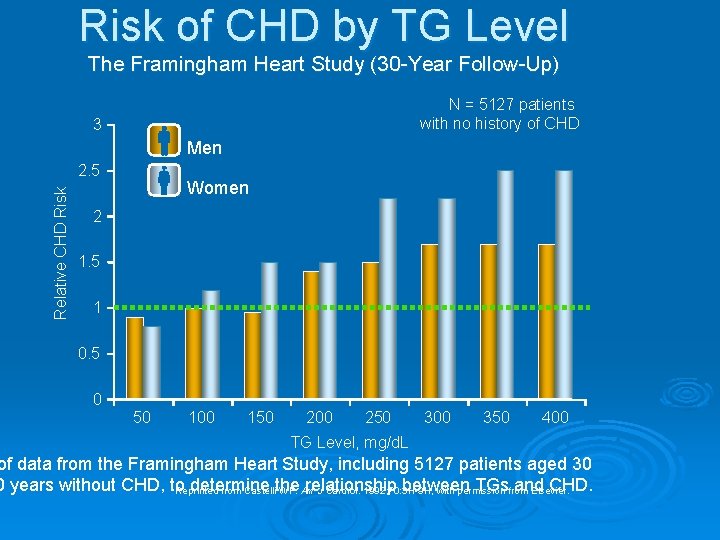
Risk of CHD by TG Level The Framingham Heart Study (30 -Year Follow-Up) N = 5127 patients with no history of CHD 3 Men Relative CHD Risk 2. 5 Women 2 1. 5 1 0. 5 0 50 100 150 200 250 300 350 400 TG Level, mg/d. L of data from the Framingham Heart Study, including 5127 patients aged 30 0 years without CHD, to determine relationship between TGsfrom and CHD. Reprinted from Castellithe WP. Am J Cardiol. 1992; 70: 3 H-9 H, with permission Elsevier.

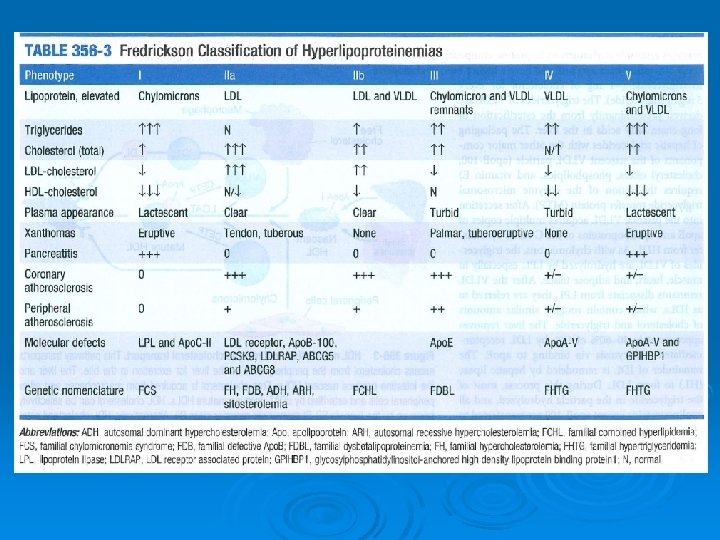


( ﺍﻭﻟﻴﻪ)ژﻨﺘﻴﻚ Primary causes : single or multiple gene mutations that result in either overproduction or defective clearance of TG and LDL cholesterol, or in underproduction or excessive clearance of HDL Ø Primary disorders, the most common cause of dyslipidemia in children, do not cause a large percentage of cases in adults. Ø
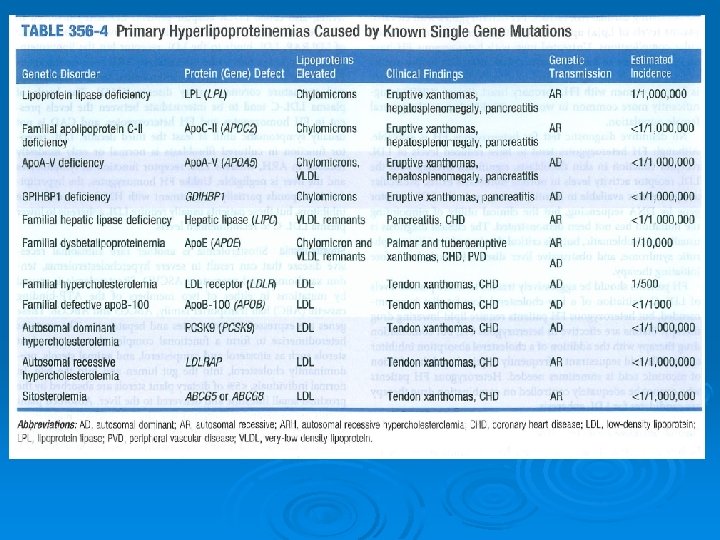

Secondary causes contribute to most cases of dyslipidemia in adults. Ø The most important secondary cause in developed countries is a sedentary lifestyle with excessive dietary intake of saturated fat, cholesterol, and trans fats. Ø Other : DM, alcohol overuse, chronic kidney disease, hypothyroidism, primary biliary cirrhosis and liver diseases Ø Drugs: Thiazides, β-blockers, retinoids, highly active antiretroviral agents, estrogen , progestins, Ø

(FH) ﻫﻴپﺮﻛﻠﺴﺘﺮﻭﻟﻤﻲ ﻓﺎﻣﻴﻠﻴﺎﻝ FH is an AD disorder characterized : ü elevated LDL-C + normal TG , tendon xanthomas, premature CAD Ø FH is caused by a large number (>1000) mutations in the LDL receptor gene. Ø The elevated levels of LDL-C in FH are due to an increase in the production of LDL from IDL (since a portion of IDL is normally cleared by LDL receptor-mediated endocytosis) and a delayed removal of LDL from the blood. ü FH homozygotes: 2 mutated LDL receptor ü FH heterozygotes: 1 mutant allele Ø Individuals with FH homozygotes have higher LDL-C levels than those FH heterozygotes Ø

LDL receptor A normal LDL receptor A mutated LDL receptor

Homozygous FH 1 in 1 million persons worldwide. Ø The disease has >90% penetrance so both parents of FH homozygotes usually have hypercholesterolemia. Ø Ø Clinical manifestation: ü cutaneous xanthomas on the hands, wrists, elbows, knees, heels, or buttocks present in childhood CHOL are usually >500 mg/d. L and can be higher than 1000 mgld. L. Important complication of is accelerated atherosclerosis, which can result in disability and death in childhood. Atherosclerosis often develops first in the aortic root, where it can cause aortic valvular or supravalvular stenosis, and typically extends into the coronary ostia, which become stenotic. ü ü ü

Homozygous FH Ø Exams and Tests: A physical examination may reveal xanthomas and corneal arcus. ü A strong family history of familial hypercholesterolemia or early heart attacks ü High levels of LDL in either or both parents. ü Individuals from families with a strong history of early heart attacks should have blood tests done to determine lipid levels. ü

Dysbetalipoproteinemia, , is a rare lipid disorder characterized by high levels of blood cholesterol & TG. Ø CHOL range from 300 -600 mg/d. L. TG are usually >400 mg/d. L and may exceed 1000 mg/d. L. Ø Moderately elevated total cholesterol and triglyceride levels accompanied by the presence of palmar crease xanthomas confirm the diagnosis dysbetalipoproteinemia Ø

Clinical findings Ø Ø Ø Patients may have no physical findings or may have skin lesions called xanthomas, particularly in more severe presentations. Xanthoma striata palmaris Tuberoeruptive and tuberous xanthomas Corneal arcus , Xanthelasmas Obesity or signs of hypothyroidism may be noted.
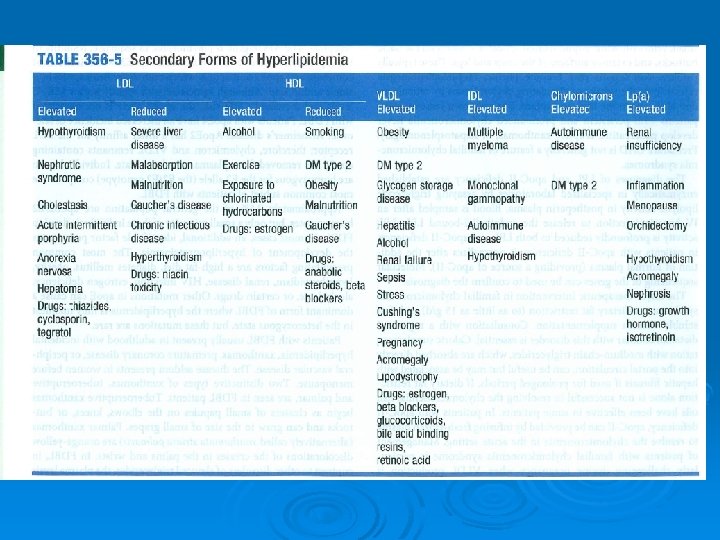


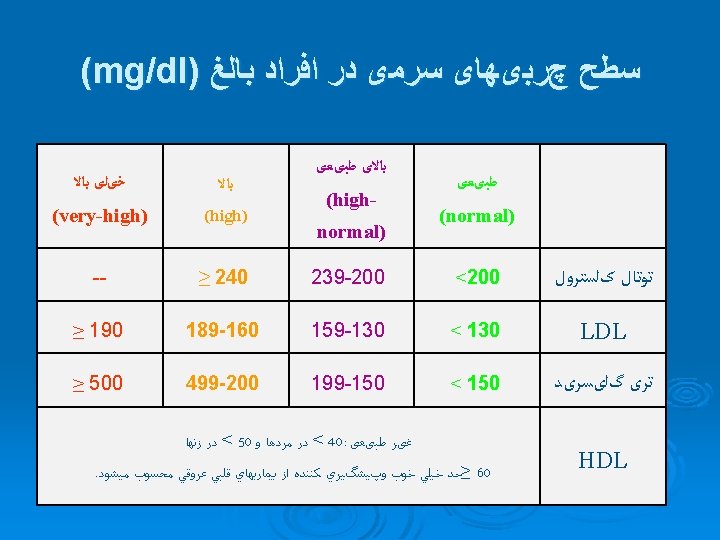
ﻳﺎﻓﺘﻪ ﻫﺎﻱ ﺑﺎﻟﻴﻨﻲ Ø Ø Ø High levels of LDL : eyelid xanthelasmas; arcus corneae; tendinous xanthomas. familial hypercholesterolemia : the above findings plus planar or cutaneous xanthomas severe elevations of TGs can have eruptive xanthomas Patients with dysbetalipoproteinemia can have palmar and tuberous xanthomas Severe hypertriglyceridemia (> 2000 mg/d. L) can give retinal arteries and veins a creamy white appearance (lipemia retinalis). Extremely high lipid levels also give a lactescent (milky) appearance to blood plasma.
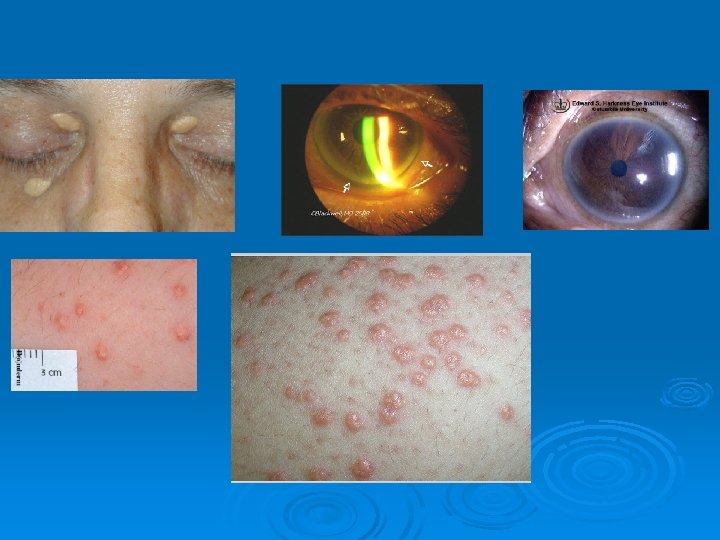
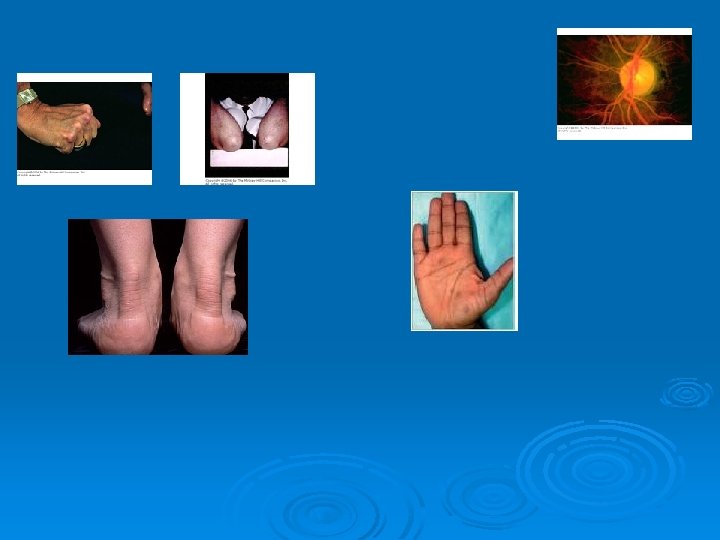

Diagnosis Ø Lipid profile measurement Ø Testing should be postponed until after resolution of acute illness, because TGs increase and cholesterol levels decrease in inflammatory states. Lipid profiles can vary for about 30 days after an acute MI; however, results obtained within 24 h after MI are usually reliable enough to guide initial lipid-lowering therapy. TC, TGs, and HDL cholesterol are measured directly. LDL cholesterol = TC − [HDL cholesterol + (TGs ÷ 5)] (Friedewald formula). This calculation is valid only when TGs are < 400 mg/d. L and patients are fasting Ø Ø Ø

Ø Screening: A fasting TC, TGs, HDL cholesterol, and calculated LDL cholesterol should be obtained in all adults ≥ 20 yr and should be repeated every 5 yr. Ø screening patients < 20 yr: atherosclerotic risk factors, such as diabetes, hypertension, cigarette smoking, and obesity; premature CAD in a parent, grandparent, or sibling; or a cholesterol level > 240 mg/d. L or known dyslipidemia in a parent. Ø 12 hours fasting

Other tests Ø ü ü Ø Ø 1 - Lp(a) measurement : Patients with premature atherosclerotic cardiovascular disease with normal or near-normal lipid levels high LDL levels refractory to drug Patients with an extensive family history of heart disease 2 -C-reactive protein and homocysteine measurement may be considered in the same populations. 3 -Tests for secondary causes

Ø ü ü ü v Ø ü 3 -Tests for secondary causes : FBS, liver enzymes, Creatinin TSH urinary protein For who? (newly diagnosed dyslipidemia , when a component of the lipid profile has changed for the worse. A definite age after which no require screening ? ? into their 80 s, especially in the presence of atherosclerotic cardiovascular disease.
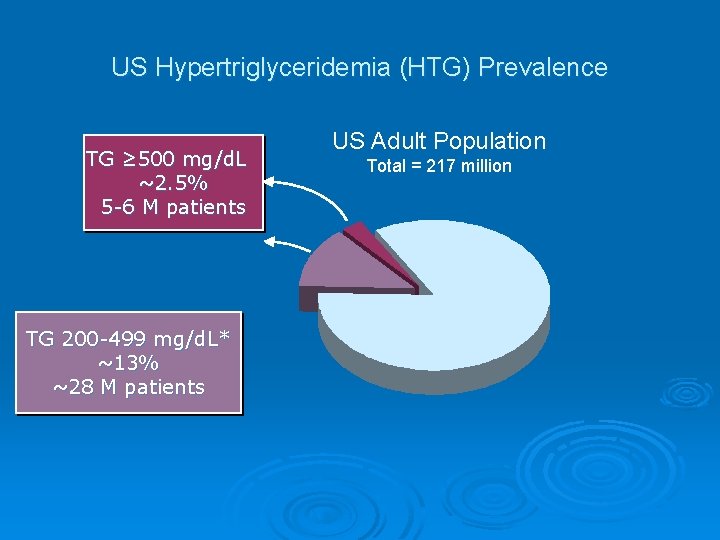
US Hypertriglyceridemia (HTG) Prevalence TG ≥ 500 mg/d. L ~2. 5% 5 -6 M patients TG 200 -499 mg/d. L* ~13% ~28 M patients US Adult Population Total = 217 million

HIGH TG Ø INDEPENDENT RISK FACTOR FOR HEART ATTACK Ø INDEPENDENT RISK FACTOR FOR STROKE Ø ASSOCIATED WITH LOW HDL Ø ASSOCIATED WITH INCREASED CLOTTING VIA HIGH PLASMINOGEN ACTIVATOR INHIBITOR ACTIVITY, HYPOFIBRINOLYSIS (CAN’T CHOP UP BLOOD CLOTS EASILY) Ø A FUNDAMENTAL PART OF


Familial hypertriglyceridemia Ø Ø Ø Ø Familial hypertriglyceridemia is a common disorder passed down through families in which the level of TG are higher than normal. The condition is not associated with a significant increase in cholesterol levels. An autosomal dominant fashion Familial hypertriglyceridemia does not usually become noticeable until puberty or early adulthood. Obesity, hyperglycemia (high blood glucose levels), and high levels of insulin are often also present and may cause even higher triglyceride levels. about 1 in 500 individuals in the United States. Risk factors are a family history of hypertriglyceridemia or a family history of heart disease before the age of 50.

Familial hypertriglyceridemiaØ Exams and Tests Ø People with a family history of this condition should have blood tests to check very low density lipoprotein (VLDL) and triglyceride levels. Blood tests usually show a mild to moderate increase in triglycerides (about 200 to 500 mg/d. L)




Ddiagnostic approach-summary 1 -Measure fasting lipoproteins 2 -primary/secondary 3 - Identify CAD or CAD equivalents & CAD risk factors Slide 32 4 - If ≥ 2 major risk factors without CAD or CAD equivalent, assess 10 -yr risk of MI or CAD death using Framingham risk tables 5 -refer to NCEP ATP III Guidelines for Treatment of Hyperlipidemia

Ø Ø Ø Rule out secondary causes(FBS, U/A, CR, TSH, LFT) Sedentary lifestyle, obesity, and smoking are all associated with low HDL-C levels, and patients should be counseled about these issues. Patients with hyperlipidemia, especially hypertriglyceridemia, who drink alcohol should be encouraged to decrease their intake. Drugs Attempts should be made to diagnose the primary lipid disorder

Ø CAD equivalents: ü ü Peripheral arterial disease Abdominal aortic aneurysm Symptomatic carotid artery disease Diabetes mellitus Ø Major CAD risk factors in dyslipidemia: ü ü ü Cigarette smoking Hypertension (BP ≥ 140/90 or on antihypertensive drug) Low HDL (≤ 40 mg/d. L [1. 03 mmol/L]) Family history of premature CAD (CAD in a male 1 st-degree relative < 55 or in a female 1 st-degree relative < 65) Age (men ≥ 45, women ≥ 55)
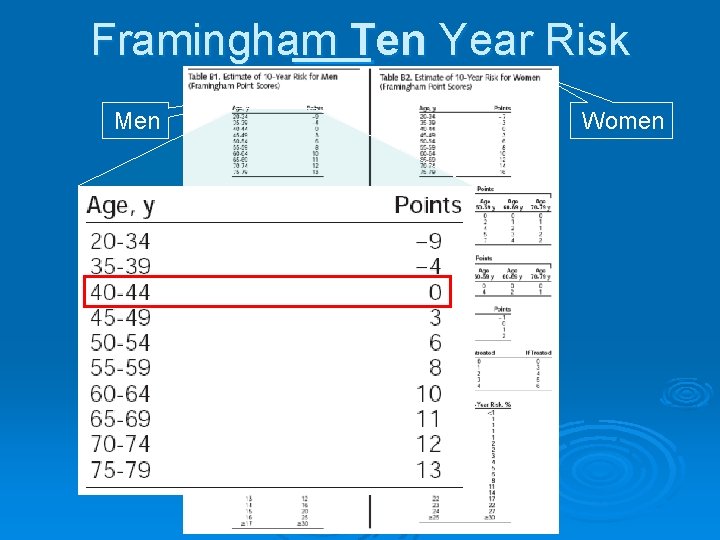
Framingham Ten Year Risk Men Women
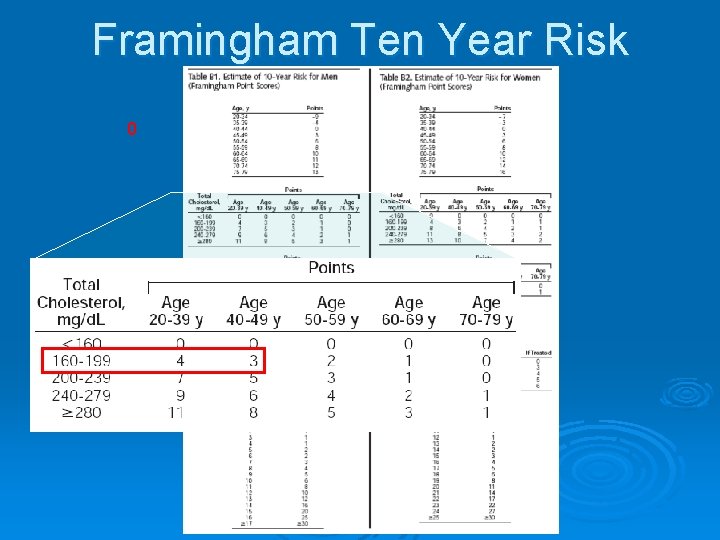
Framingham Ten Year Risk 0
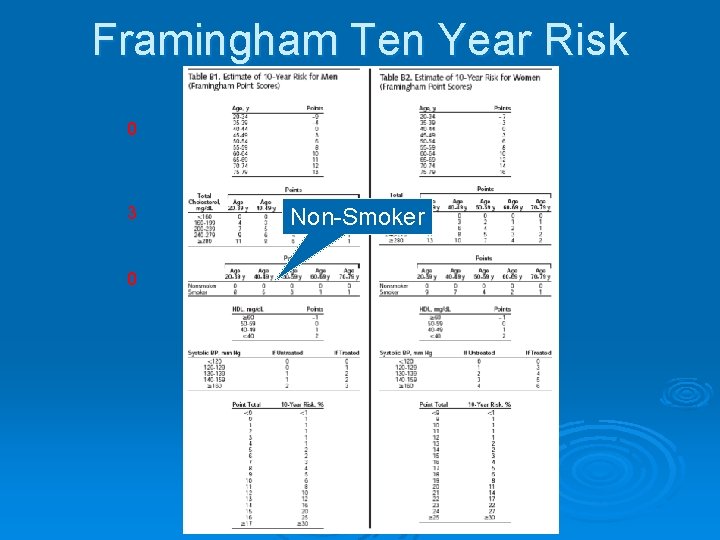
Framingham Ten Year Risk 0 3 0 Non-Smoker

Framingham Ten Year Risk 0 3 0 1 HDL = 43
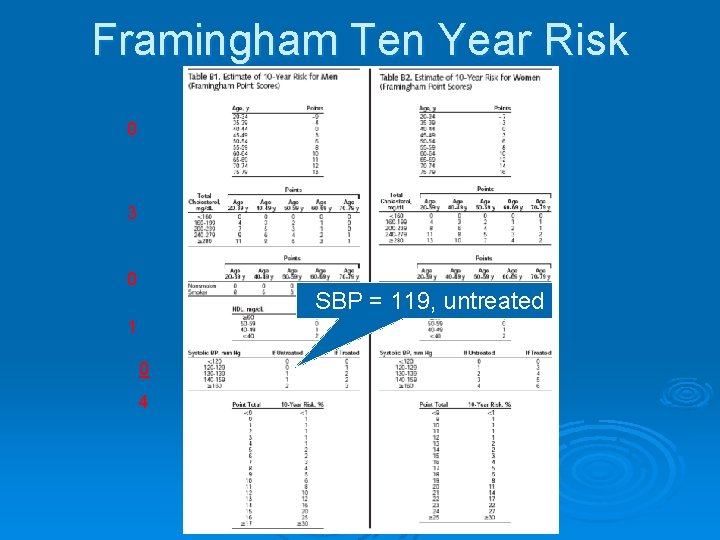
Framingham Ten Year Risk 0 3 0 SBP = 119, untreated 1 0 4
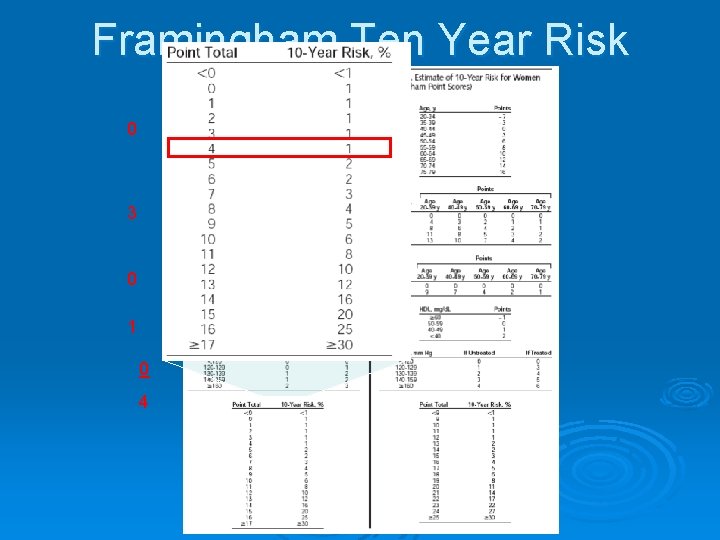
Framingham Ten Year Risk 0 3 0 1 0 4
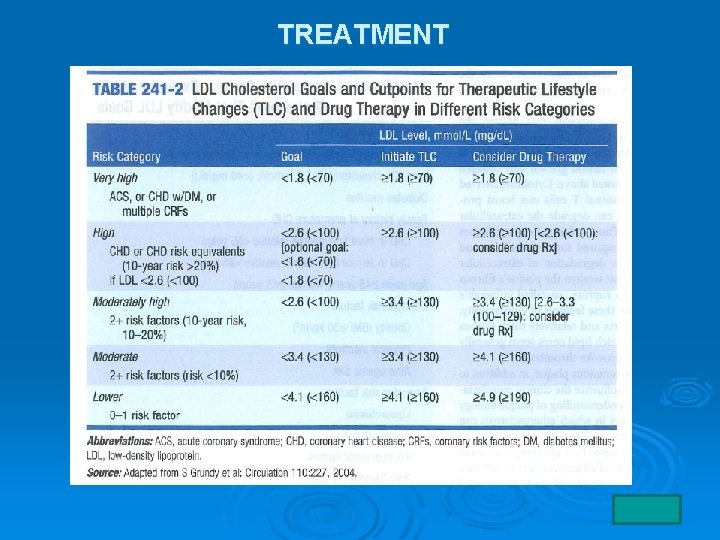
TREATMENT

Ddiagnostic approach-summary 1 -Measure fasting lipoproteins 2 -primary/secondary 3 - Identify CAD or CAD equivalents & CAD risk factors 4 - If ≥ 2 major risk factors without CAD or CAD equivalent, assess 10 -yr risk of MI or CAD death using Framingham risk 5 -refer to NCEP ATP III Guidelines for Treatment of Hyperlipidemia


- Slides: 50