Dr Nasser Mohamed Abd allah Prof of Tropical

Dr. Nasser Mohamed Abd allah Prof. of Tropical Medicine Alexandria University

q Acute illness caused by ingestion of food contaminated by bacteria, bacterial toxins, viruses, natural poisons, or harmful chemical substances q. It is characterized by a short IP (1 wk or less). q. The symptoms vary and include abdominal pain, vomiting, diarrhea, headache, and prostration q. Serious cases can result in life-threatening neurologic , hepatic, and renal syndromes leading to permanent disability or death.
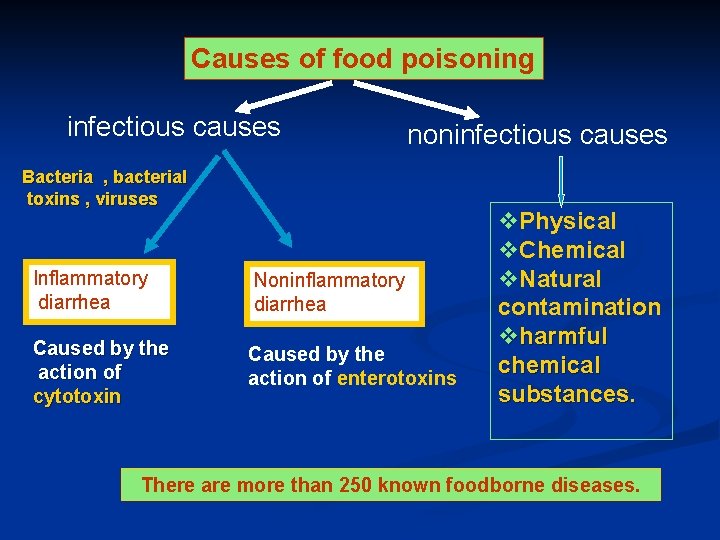
Causes of food poisoning infectious causes noninfectious causes Bacteria , bacterial toxins , viruses Inflammatory diarrhea Noninflammatory diarrhea Caused by the action of cytotoxin Caused by the action of enterotoxins v. Physical v. Chemical v. Natural contamination vharmful chemical substances. There are more than 250 known foodborne diseases.
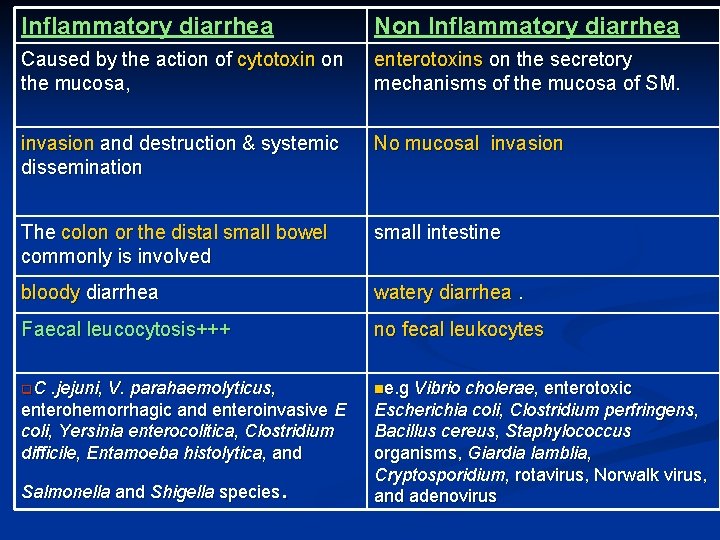
Inflammatory diarrhea Non Inflammatory diarrhea Caused by the action of cytotoxin on the mucosa, enterotoxins on the secretory mechanisms of the mucosa of SM. invasion and destruction & systemic dissemination No mucosal invasion The colon or the distal small bowel commonly is involved small intestine bloody diarrhea watery diarrhea. Faecal leucocytosis+++ no fecal leukocytes q. C ne. g . jejuni, V. parahaemolyticus, enterohemorrhagic and enteroinvasive E coli, Yersinia enterocolitica, Clostridium difficile, Entamoeba histolytica, and . Salmonella and Shigella species Vibrio cholerae, enterotoxic Escherichia coli, Clostridium perfringens, Bacillus cereus, Staphylococcus organisms, Giardia lamblia, Cryptosporidium, rotavirus, Norwalk virus, and adenovirus

n Non Infectious causes n n Physical contamination: - objects falling in to food – metal, glass, packaging materials etc. Chemical contamination: - Bleach, cleaning chemicals getting in to food , heavy metals [eg, arsenic, mercury, lead]) Natural contamination: Poisonous plants and berries, undercooked red kidney beans, mushrooms mycotoxins (poisonous chemicals produced by some moulds)

Toxins n Released by bacteria & cause food poisoning. n exotoxins multiply in food. n n not easily destroyed by cooking and may remain in food once they have developed. endotoxins n Other bacteria produce toxins inside the human body only after the food has been eaten.

Vulnerable Groups v. Food poisoning is more likely to affect people with lowered resistance to disease than healthy people who might show mild symptoms or none at all. v. The following are particularly vulnerable to food poisoning: v Elderly or sick people v Babies v Young children v Pregnant women

The inoculum of infection agent required for illness Infectious agent v. Shigella dyseteriae v. Echerichia coli 0157: H 7: v. Nontyphoidal v. Salmonella v. Vibrio salmonella: typhi cholera v. Listeria monocytogens v-Botulimum toxin Dose n 10 -100 n 50 organisms n 1000 organisms v 100, 000 n 1 organisms. million organisms. billion organisms vmedian lethal dose: 0. 001 microgram/kg

Staphylococcus aureus n n n It elaborates heat- stable toxins which are responsible for the illness. Sudden onset of vomiting followed by diarrhea and occasionally fever. Symptoms usually resolve within 12 hr. Outbreaks occur predominantly in summer time in association with hum, poultry, egg, salads and pastries. Food handlers are usually responsible of contamination.

Clostridium perfringens n n n n anaerobic gram + ve spore -forming rod. It is a common cause of bacterial food borne illness. IP : 8 -16 hr diarrhea & abdominal cramps & resolve within 24 hr. The organism is found in the GIT of animal (including human) & contaminate beef , poultery. Roasting meat fail to kill spores Thespores germinate in meat at room temp. organism elaborates enterotoxin following sporulaion in the stomach

Clostridium difficile Is a gram-positive anaerobic spore-forming bacillus. n The organism produce a syndrome ranging from mild diarrhea to pseudomembranous colitis & is often associated with antibiotic. n symptoms may begin from 24 hr after starting antibiotic therapy to 6 week after finishing but commonly occur 4 -9 days after starting antibiotic. n

n n n Profuse watery diarrhea with abdominal tenderness , fever & a raised peripheral WBCS. The condition can progress to toxic megacolon & colonic perforation & death Treatment should stop antibiotics. n In severe colitis, specific therapy with oral Vancomycin should be commenced. n Metronidazole is also currently in progress n anti-toxin antibodies is given by mouth for patients with multiple relapses who require continued antibiotics.

Campylobacter n n Campylobacter jejuni is the most common cause of gastroenteritis in the most developed countries. Infection is usually associated with ingestion of contaminated food or water or n consumption of undercooked meat particularly poultry. n n The incidence peaks in the summer months.

n n n IP: 3 -5 days C/O : malaise, abdominal cramps with frequent loose watery stools which may become bloody. Resolution generally occurs in a few days, through prolonged symptomatic infection & relapses may occur. Stool culture is diagnostic to campylobacter infection. Treatment: n Most cases require only fluid replacement n in prolonged or severe infection, Erythromycin can reduce the duration of symptoms. Alternatively, Ciprofloxacin may be given.

Salmonella gastroenteritis n n n Many serotypes cause gastroenteritis in humans e. g. S. enteritidis, S. typhimurium & S. virchow ). Food products are the principle source of the organisms, hen’s egg have been implicated in outbreaks. Infection neutrophil infiltration of the mucosa , local , & systemic release of inflammatory mediators, inflammation & tissue damage.

n n These events lead to fluid secretion & a marked enteric inflammatory response. IP: 16 -48 hr n n vomiting & diarrhoea. +/- Fever , though this usually resolves in 48 hr. Diarrhoea usually settles by 10 days. Diagnosis : n n by presence of WBCs in stool and stool culture. Blood culture may be positive in a few of patients

Treatment Ø Ø fluid replacement. Antibiotics are recommended for the following groups: Ø Ø Ø Neonates. Patients with valvular heart disease or prosthetic implants. Immunosuppressed patients. Ciprofloxacin is the drug of choice if antibiotic is required. Convalescent carriage of the organism usually clears in 4 -6 weeks. It may be prolonged particularly in the elderly & the young.

Shigella

Shigella n n Shigella dysentery predominantly affects children under 5 years of age, It rarely occurs in infants ( absence of specific receptors on enterocytes. ) In developing countries --- sh. dysenteriae , sh. Flexneri & sh. Boydii may cause epidemics & may be associated with fatal infection. Sh sonnei - ------ common in USA ( mildest) Shigella spp has been implicated as a cause of ( gay bowel ) syndrome in homosexual men.

Transmission is known to be associated with : n poor sanitation n food contamination by flies also contributes to spread. n disease control provision of clean drinking water & proper sewage disposal n

Pathological Features Shigella toxins local ulceration & pseudomembrane formation diarrhea

The clinical features n n n IP: 2 -3 days High fever, headache, malaise & anorexia Frequent small- volume stools progressing to passage of pus an blood & severe abdominal cramps, tenesmus Clinical resolution occurs within a few days. Young children may continue to excrete organisms for many weeks continuing risk of cross-infection.

n The mainstay of diagnosis is stool culture & specific serological testing.

Treatment n Fluid replacement is the principal treatment, using oral rehydration glucose electrolyte solution & I. V replacement for severe cases. n Antibiotics should be used only in severe cases of shigellosis. n in most adult-----Ciprofloxacin is preferred n in children------- co-trimoxazole or ampicillin are alternative.

Escherichia coli

Escherichia coli E-coli is a major cause of foodborne illness n Harmless strains of E. coli exist in the GIT of humans and warm-blooded animals n A dangerous type ; enterohemorrhagic E. coli ( EHEC ) bloody diarrhea and can n lead to kidney failure in children or elderly people.

Transmission Of E COLI n n Sources : Cattle are the main of E. coli O 157: H 7. low infecting dose (10 -100 organisms) n E. coli bacteria and its toxins have been found in: n Undercooked or raw hamburgers n Salami n Alfalfa sprouts n Lettuce n Unpasteurized milk, apple juice n Contaminated well water n swimming in sewagecontaminated water.

The pathogenesis of diarrhea n The pathogenesis of diarrhea & the inflammatory response is through basic mechanisms involving combinations of q adherence of cells, q invasion q toxin n n production The type of harmful E. coli most commonly found is named O 157: H 7 It produces powerful toxins severely damage the intestinal mucosa.

n Many different serotypes are involved. n Pathogenic mechanisms of E-coli are : n Verotoxin-producing E-coli. n Entero- invasive E-coli. n Enterotoxicogenic E-coli. n Enteropathogenic E-coli. n Enterohaemorrhagic E. coli (EHEC)

Pathological features & CP n n IP: 1 - 7 days The infection is classically with haemorrhagic colitis. n Typically there is watery diarrhoea with severe abdominal cramps, preceding blood diarrhoea. n Enterotoxins have: n local effect on the bowel n distant effect --- glomerular apparatus, heart and brain.

n The illness often lasts for up to 12 days & usually resolves spontaneously but may be fatal. n Fever or rising BC may indicate the onset of complications such as: haemolytic uraemic syndrome (10 -15% ) & ischaemic colitis.

Many different serotypes are involved. q. Enterotoxigenic E. coli (ETEC) q. Entero-invasive E. coli (EIEC) q. Enteropathogenic E. coli (EPEC) q. Entero-aggregative E. coli (EAEC ) q. Enterohaemorrhagic E. coli (EHEC)

Enterotoxigenic E. coli (ETEC) Causes most cases of travellers' diarrhoea in developing countries n Produce either a heat-labile or a heatstable enterotoxin secretory diarrhoea and vomiting after 1 -2 days' incubation. n mild and self-limiting after 3 -4 days. n Antibiotics limit the duration of symptoms and prophylaxis. n

Entero-invasive E. coli (EIEC) n n Caused by invasion and destruction of colonic mucosal cells. No enterotoxin is produced. Acute watery diarrhoea, abdominal cramps and some scanty blood-staining of the stool are common. Rarely severe and are usually self-limiting.

Enteropathogenic E. coli (EPEC) n These are very important in infant diarrhea. n They attach to the gut mucosa destruction of microvilli and disruption of normal absorptive capacity. n The symptoms vary from mild non-bloody diarrhoea to quite severe illness.

Entero-aggregative E. coli (EAEC) n They adhere to the mucosa produce a locally active enterotoxin prolonged diarrhea in children

Enterohaemorrhagic E. coli (EHEC ) n n A number of distinct 'O' serotypes of E. coli possess both the genetic codes for Attachment & Plasmids encoding for two distinct enterotoxins (verocytotoxin) --- identical Shigella toxins E. coli O 157: H 7 is perhaps the best known of these verocytotoxigenic E. coli) VTEC), but others, including types O 126 and O 11, are also implicated.

n n n The identification of E-coli 0157: H 7 from stool culture can be confirmed by a latex agglutination test with specific antiserum. Fluid replacement is essential. Antibiotic don’t reduce the severity of the illness or reduce the risk of haemolytic uraemic syndrome

MOST COMMON CAUSES OF TRAVELLERS' DIARRHOEA

CAUSES OF BLOODY DIARRHOEA

- Slides: 41