Dr Muhammad Shoaib MBBS MPH Senior Lecturer Department

Dr. Muhammad Shoaib MBBS, MPH Senior Lecturer Department of community Medicine MBBS MC

INTRODUCTION Family planning is the term given for pre-pregnancy planning and action to delay, prevent or actualize a pregnancy. DEFINITION: Family planning is a way of thinking and living that is adopted voluntarily, upon the bases of knowledge, attitude and responsible decision by individuals and couples in order to promote the health and welfare of family group and thus contribute effectively to the social development of country.

OBJECTIVES ( WHO ) “the use of a range of methods of a fertility regulation to help individuals or couples attain certain objectives: avoid unwanted birth. bring about wanted birth. Produce a change in the no. of children born. Regulate the intervals between pregnancies. Control time at which birth occur. ”
Elements of family planning 3 important elements in family planning: Proper spacing Proper tim ing No. of pregnanci es

Benefits to Mother � Reduce the health risk. � Below 20 years, and above 35 years are at risk of developing complications during pregnancy. Physical strain of child bearing. � Reduce number of maternal death. � Reduce the risk of ovarian cysts.

Health Benefits to Children: Ensures better chance of survival at birth. Promote better childhood nutrition. Promote physical growth and development. Prevent birth defects.

Health Benefits to Father Allows father to keep a constant balance between their physical, mental, social well –being. Increase father sense of respect because he is able to provide the type of education and home environment.

Benefits to Whole Family Health - help the family to enjoy the better kind of life.
TYPES OF FAMILY PLANNING Natural family planning Barrier family planning Permanent/surgical family planning

INTRODUCTION OF NATURAL FAMILY PLANNING No introduction of chemical of foreign material into the body. Practice may be due to religious belief, “natural” way is best for them. Effectiveness varies greatly, depends on couples ability to refrain from having intercourse on fertile days. Failure Rates: about 25% Poses no risk to fetus.

NATURAL FAMILY PLANNING Rhythm (Calendar) method Basal Body Temperature (BBT) Ovulation or Cervical Mucus Method Symptothermal method Coitus Interruptus Lactation amennorhea

RHYTHM (Calendar) METHOD �The rhythm method, also called the fertility awareness method, is a form of pregnancy prevention where couples calculate a woman's fertile time using a calendar. �Abstaining from coitus on the days of menstrual cycle when a woman is most likely to conceive (3 or 4 days before until 3 or 4 days after ovulation). Woman keeps a diary of 6 menstrual cycles.
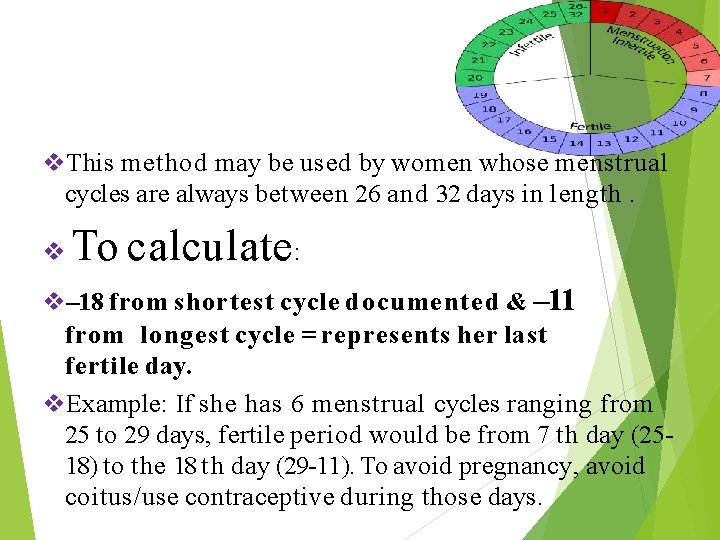
This method may be used by women whose menstrual cycles are always between 26 and 32 days in length. To calculate : --18 from shortest cycle documented & --11 from longest cycle = represents her last fertile day. Example: If she has 6 menstrual cycles ranging from 25 to 29 days, fertile period would be from 7 th day (2518) to the 18 th day (29 -11). To avoid pregnancy, avoid coitus/use contraceptive during those days.
Disadvantages Lifespan of Sperm Failure of method Reliability

. Basal Body Temperature (BBT) Identifying fertile and infertile period of a woman’s cycle by daily taking and recording of the rise in body temperature during and after ovulation. Just before ovulation, a woman’s BBT falls about 0. 5ºF At time of ovulation, her BBT rises a full degree (influence of progesterone). This higher level is maintained the rest of menstrual cycle.

DISADVATAGES NOT reliable method: of birth control, especially for women with irregular cycles. Plus, outside factors, Woman’s body temperature can be altered due to disturbance in sleep.

Cervical Mucus/Ovulation �Cervical mucus is a fluid produced by small glands near the cervix � This fluid changes throughout her cycle, from scant and sticky, to cloudy and thick, to slick and stringy. �Each of these types of mucus is related to the hormonal shifts that naturally occur during the menstrual cycle as her body prepares for and achieves ovulation.

Right before ovulation, the mucus from the cervix changes from being cloudy and scanty to being clear and slippery. The consistency of ovulation mucus is like that of an egg white and it can be stretched between the fingers. It is the peak of her fertility. After the ovulation, the mucus tends to dry up again. These are also safe days. Ideal Failure rate: 3%

DISADVANTAGES � It is not a particularly reliable method of birth control, especially for women with irregular cycles. �Remember that cervical mucus does not let you know when you will soon be ovulating, but sperm can live up to seven days inside the vagina. Any sperm deposited ahead of time can still impregnate the woman.

Symptothermal Method Combines the cervical mucus and BBT methods Watches temp. daily and analyzes cervical mucus daily. Watch for mid-cycle abdominal pain, couple must abstain from intercourse until 3 days after rise in temp. or 4 t h day after peak of mucus change. More effective than BBT or CM method alone Ideal Failure rate: 2%

COITUS INTERRUPTUS One of oldest known methods of contraception Couple proceeds with coitus until the moment of ejaculation which Offers little protection.

LACTATION AMENNORRHEA The lactation amenorrhea method (LAM) is a natural birth control technique based on the fact that lactation (breast milk production) causes amenorrhea (lack of menstruation).

How it works: Breastfeeding interferes with the release of the hormones needed to trigger ovulation. ADVANTAGES: Breastfeeding on demand improves health for mother and baby. Nothing to buy or use.

DISADVANTAGES an use this method only for the first six months after birth or until the first menstrual period. LAM does not provide protection against SEXUALLY TRANSMITTED INFECTIONS.
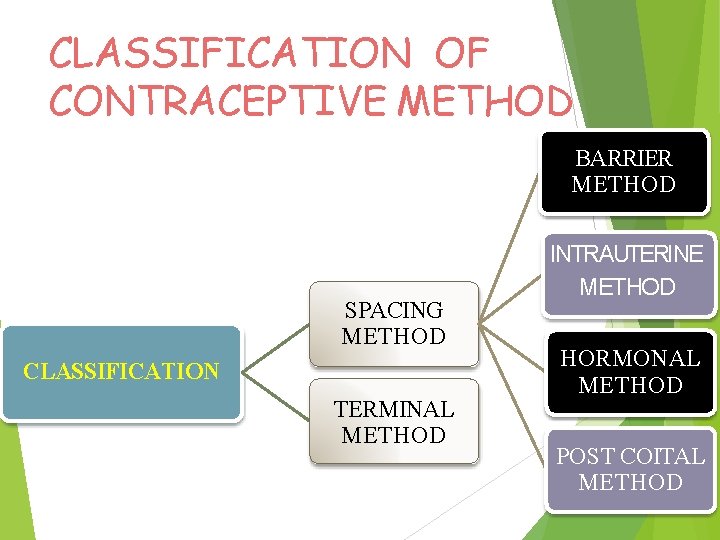
CLASSIFICATION OF CONTRACEPTIVE METHOD BARRIER METHOD SPACING METHOD CLASSIFICATION TERMINAL METHOD INTRAUTERINE METHOD HORMONAL METHOD POST COITAL METHOD

BARRIER METHODS Condoms (male and female) Spermicidal �Sponge �Diaphragm Cervical cap

Male condoms: These are made up of polyurethane or latex. Silicon used now a days to produce semi dry prelubricated forms. In Pakistan one particularly brand is widely marketed as ‘Durex’. Spermicidal – coated with nonoxynol on inner and outer surfaces.

MALE CONDOM

ADVANTAGES: Simple spacing method No side effects Easily available, safe & inexpensive Protects against STDs DISADVANTAGES; Chances of slip off and tear off Allergic reaction to latex Failure rate: 16%

Female condoms: �It is a pouch made up of polyurethane which lines the vagina and also external genitalia. �It is 17 cm in length with one flexible polyurethane ring at each end. ADVANTAGES: Prevents STDs including HIV/AIDS Not damaged by oils and other chemicals.


DISADVANTAGES: High motivation Only women who can use diaphragms can use female condom Slippage occurs Expensive Failure rate 21% with typical use and 5% with correct and consistent use.

Diaphragm Most common and easiest to fit and use. Thin, nearly hemispherical dome made of rubber or latex material, with circular, covered metal spring at periphery (flat type and coil type) External diameter of rim is size of diaphragm – 45 mm diameter rising in steps of 5 mm to 105 mm (most common 60, 65, 70, 75, 80)

The device is introduced up to 3 hours before intercourse and is to be kept for at least 6 hrs after intercourse. ADVANTAGES: cheap No gross medical side effects Control of pregnancy in hands of woman Reasonably safe when properly used Prevent spread of STDs though less effective than condom
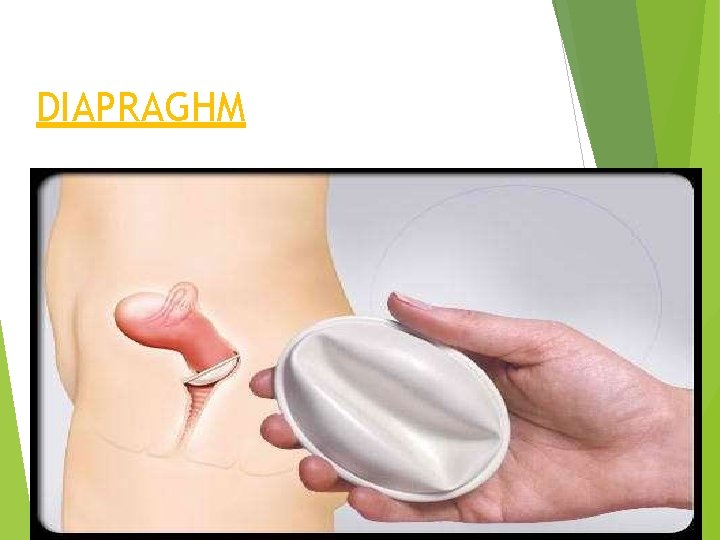
DIAPRAGHM

DISADVANTAGES: �Requires help of doctor to measure the size required. �Need high motivation �Allergic reaction to rubber �Erosion �UTI’s

SPERMICIDES �Available as vaginal foams , gels , creams , tablets and suppositories. �Contain surfactant like nonoxynol-9, benzalkonium chloride. �Alter the sperm surface membrane permeability resulting in killing of sperm.

SPERMICIDE

ADVANTAGES: � No instructions by doctors or nurses � Easily available and easy to use � No gross medical side effects DISADVANTAGES Failure rate high when used alone Can increase spread of HIV infection by irritating vaginal and cervical mucosa Failure rate – 21% with typical use

Vaginal contraceptive sponge The sponge is a doughnut-shaped device made of soft foam coated with spermicide. Made up of polyurethane with 1 gm of nonoxynol-9 as a spermicide. It releases spermicide during coitus, absorbs ejaculate and blocks the entrance of cervical canal. To use the sponge, it must be moistened with water. Once inserted in the vagina, it covers the cervix and blocks sperm from entering the uterus.

DISADVANTAGES May get broken difficult removal High pregnancy rate Allergic reactions Vaginal dryness, soreness May damage vaginal epithelium increase risk of HIV transmission
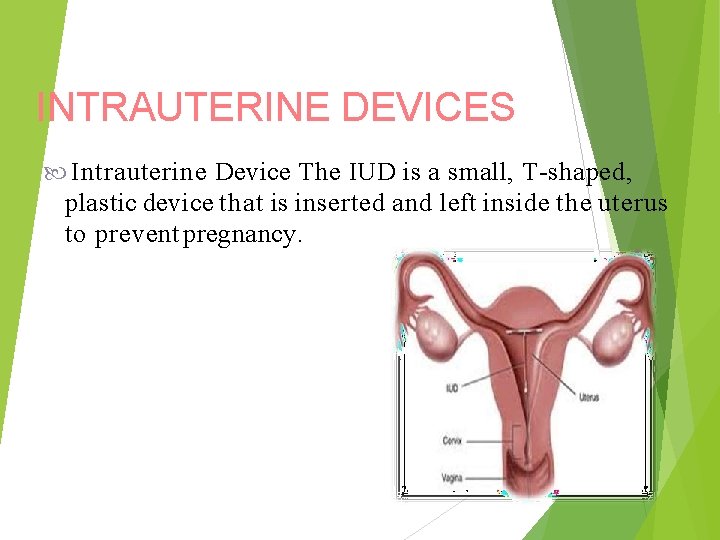
INTRAUTERINE DEVICES Intrauterine Device The IUD is a small, T-shaped, plastic device that is inserted and left inside the uterus to prevent pregnancy.
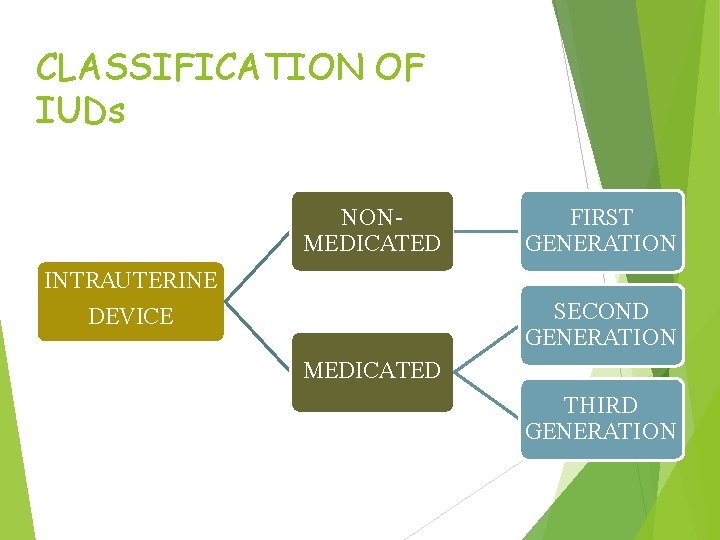
CLASSIFICATION OF IUDs NONMEDICATED FIRST GENERATION INTRAUTERINE SECOND GENERATION DEVICE MEDICATED THIRD GENERATION

First generation Non-medicated made up of polyethylene. Different shapes and sizes LIPPE’S LOOP Double ‘s’ shaped device , made up of polyethylene material. Non- toxic, non-tissue reactive and extremely durable. Small amount of barium sulphate is also added for radiological examination Available in 4 sizes A, B, C, D

Second generation Made up of metal Cu Earlier devices Cu-7 , Cu-T 200 Newer devices T copper 220 C , T copper 380 C , nova T multiload devices: ML-Cu 250 ML-Cu 375
Third generation Hormones releasing IUD PROGESTASTERT : Most commonly used T shaped device filled with 38 mg progesterone Effective for 1 year LNG- mirena Mirena (levonorgestrel-releasing intrauterine device) is a form of birth control that is indicated for intrauterine contraception for up to 5 years and Releases 20 µg of levonorgestrol. Effective for 5 years.

SIDE EFFECTS Amenorrhea Intermenstrual bleeding and spotting Abdominal/pelvic pain Ovarian cysts Headache/migraine Acne depressed/altered mood.

ADVANTAGES OF IUD Safe effective , Reversible Long action , Inexpensive DISADVANTAGES Heavy bleeding and pain Pelvic inflammatory diseases Ectopic pregnancy May come out accidently if not properly inserted.

CONTRAINDICATION History of PID Abnormal shaped uterus Ectopic pregnancy Menorrhagia
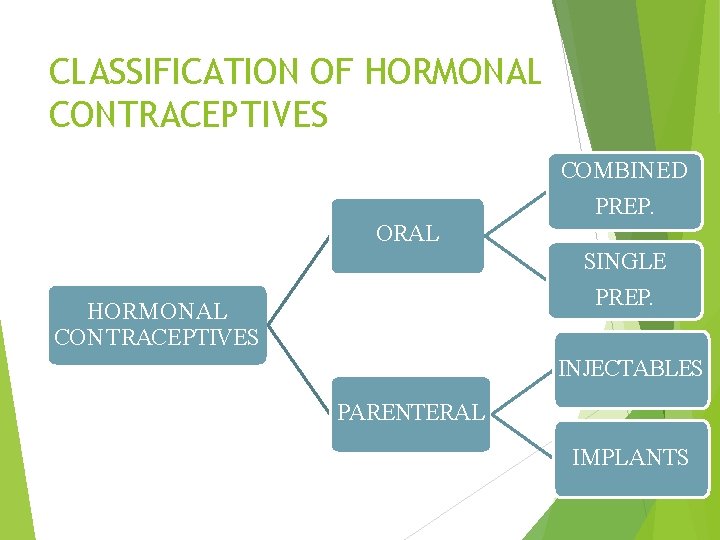
CLASSIFICATION OF HORMONAL CONTRACEPTIVES COMBINED PREP. ORAL SINGLE PREP. HORMONAL CONTRACEPTIVES INJECTABLES PARENTERAL IMPLANTS

HORMONAL CONTRACEPTIVES �With hormonal birth control , a women takes hormones similar to those her body makes naturally. �Hormonal contraceptives are mostly for female sex steroids.

Oral contraceptives �Combined oral contraceptive pills �Commonly used progestin are either levonorgestrol or norethisterone and estrogens are ethiyl estradiol or menstranol �COMMERCIAL NAMES NO. OF TABLETS �Famila-28 21+7 iron tab. �Meliane 21 tab. �Desofam 21 tab. (Ethinyloestradio & desogestrel )
TYPES Monophasic biphasic triphasic Monophasic: fixed doses of both estrogen and progesterone throughout 21 day cycle.

Biphasic: Constant amount of estrogen throughout cycle BUT increased amount of progestin during the last 11 days. Triphasic: Varies level of estrogen and progesterone. Closely mimic natural cycle, reducing breakthrough bleeding (bleeding outside the normal menstrual flow)

Contraindications ABSOLUTE: Circulatory diseases Severe HTN Angina, ischemic heart diseases. Liver disease Tumors Pregnancy Breast cancer, breast feeding.

RELATIVE: �Age>40 yrs. �Smoker, history of jaundice �Diabetes

Benefits Contraceptive benefits: �Protection against unwanted pregnancy �Convenient to use. Non-contraceptives benefits: �Regulation of menstrual cycle �Reduction of dysmenorrhea �Protection against PID, fibroids, ovarian cysts, chances of cancer.

Side effects � Dizziness �Nausea � Weight gain � Headache � Breast tenderness �Vaginal infection �Mild hypertension �Depression �Increase blood clotting

Progesterone only pills �Also known as “Minipill”. �Contains just progesterone or progesterone hormone. �Causing plug of mucus in the neck of cervix block the entry of the sperm. Example: levonorgesrol 75 µg, desogestrel 75 µg

Advantages �No side effect on breast feeding or lactation �May be prescribed in patient having diabetes, HTN , smoking etc. �Reduce risk of PID DISADVANTAGES �Acne, mastalgia, headache

Long acting contraceptives �These are more suitable for women who do not want to be pregnant again or few years. THESE ARE: �CONTRACEPTIVE INJECTIONS �IMPLANTS �PATCHES

CONTRACEPTIVE INJECTIONS ( DEPO-PROVERA & NORISTERAT) �Contain progesterone hormone. �Prevents ovulation. �Commonly used as Depomedroxyl progesterone acetate (DMPA) administered on deltoid muscle within 5 days of cycle. �DOSE: 150 mg �Provide protection for 3 months.

Contraceptive implants �It is a small device placed under the skin �Contains progesterone hormone. �Works in a similar way to injection �Contains 3 ketodesogestrel �Releases hormone about 60 mcg, gradually reduced to 30 mcg per day over year. �Inhibts ovulation. �Lasts for 3 years. �NORPLANT – II

�NORPLANT- II �Two rods of 4 cm long. Each rod containing 75 mg of levonorgestrel releases 50 mcg per day.

Emergency contraceptives �Used whithin 72 hrs , ovulation is either prevented or delayed. It may be in form of : hormones, IUD, antiprogesterone INDICATIONS �Unprotected intercourse �Condom rupture �Sexual assault

HORMONES: MORNING AFTER PILLS: It prevent conception in case of accidental intercourse. drugs used ethinyl oestradiol 2. 5 mg, premarin(conjugated oestrogen) 15 mg. Drug is taken orally twice daily for 5 days.
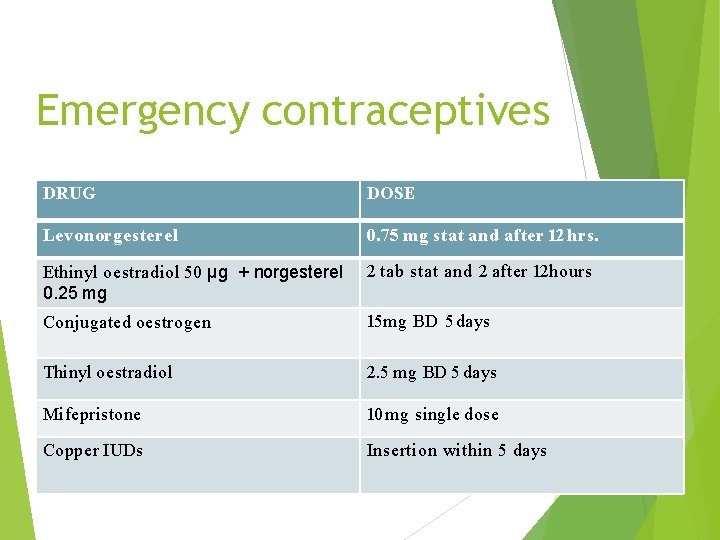
Emergency contraceptives DRUG DOSE Levonorgesterel 0. 75 mg stat and after 12 hrs. Ethinyl oestradiol 50 µg + norgesterel 0. 25 mg 2 tab stat and 2 after 12 hours Conjugated oestrogen 15 mg BD 5 days Thinyl oestradiol 2. 5 mg BD 5 days Mifepristone 10 mg single dose Copper IUDs Insertion within 5 days
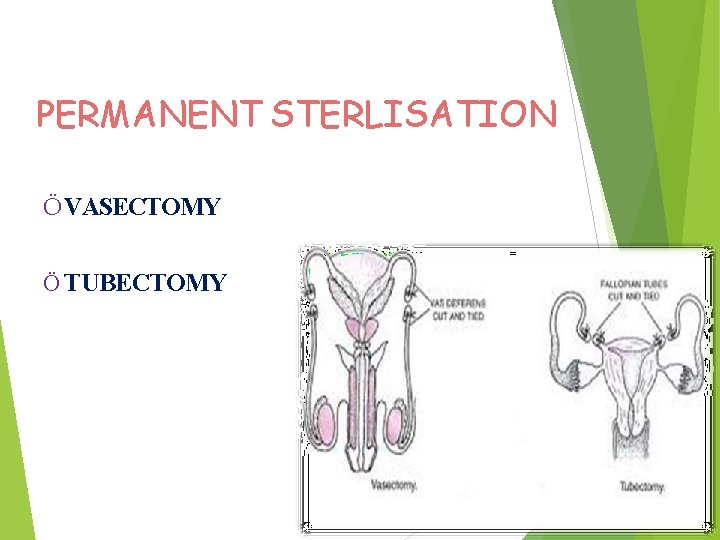
PERMANENT STERLISATION Ö VASECTOMY Ö TUBECTOMY
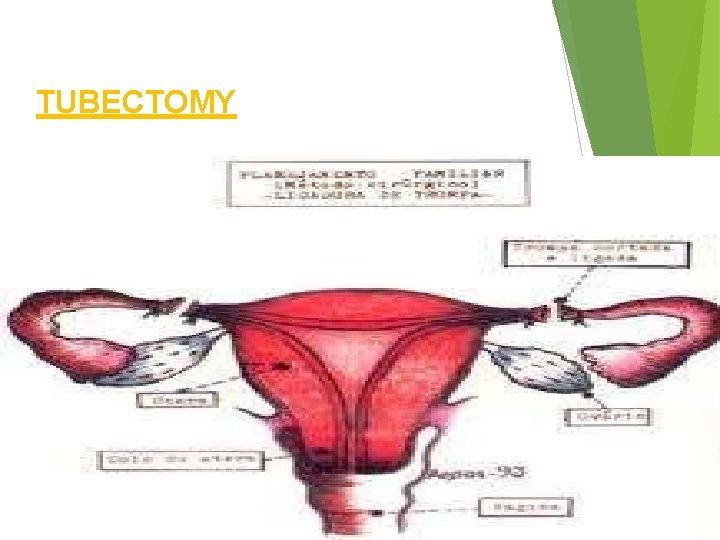
TUBECTOMY

STERILIZATION It is most effective method its failure rate is 1/2000 so in this there is permanent termination. VASECTOMY : Small incision made on each side of scrotum vas deferens is then cut and tied , cauterized or plugged. Blocking the passage of spermatozoa. Does not interfere with production of sperms but does not pass beyond vas deferens.

Very effective after 3 months of procedure Permanent and safe No apparent long term risks. DISADVANTAGES: Slightly uncomfortable due slightly pain and swelling after 2 -3 days of the procedure. Bleeding may result in the hematoma in scrotum.

TUBECTOMY : It is one of the operative procedure where resection of a both segment of both fallopian tubes is done to achieve permanent sterilization The approach may be : Abdominally Vaginally
ABDOMINAL Ω CONVENTIONAL MINILAPROTOMY Ω CONVENTIONAL: In which a loop is made by holding the tube by Allis forceps in such a way that the major part of loop consists mainly of isthmus and ampullary part of tube. The loop is ligated with catgut and is cut.

MINILAPROTOMY: When the tubectomy is done through small abdominal incision along with some device. VAGINAL LIGATION : Tubectomy through vaginal route may be done along with vaginal plastic operation or on isolation.

COMPLICATION : Ectopic pregnancy Menstrual irregularities Loss of libido Infection

Thank You
- Slides: 76