Dr M H Jokar www doctorjokar com Objectives

Dr. M. H. Jokar www. doctorjokar. com

Objectives l l l l Etiology Epidemiology Pathogenesis Clinical manifestations & Laboratory findings Diagnosis & Differential diagnosis Treatment & Prevention Prognosis

DEFINITION Acute rheumatic fever (ARF) is a systemic autoimmune disease triggered by crossreactive immune responses between group A β-hemolytic streptococci (GAS) and host tissue epitopes.

“The most important consequence of rheumatic fever is chronic rheumatic heart disease”

Epidemiology l Ages 5 -15 yrs are most susceptible Rare <3 yrs Girls=boys Common in 3 rd world countries l Environmental factors-- over crowding, l l poor sanitation, poverty, Incidence more during fall , winter & early spring

Epidemiology l 3% of individuals with untreated group A streptococcal pharyngitis will develop rheumatic fever
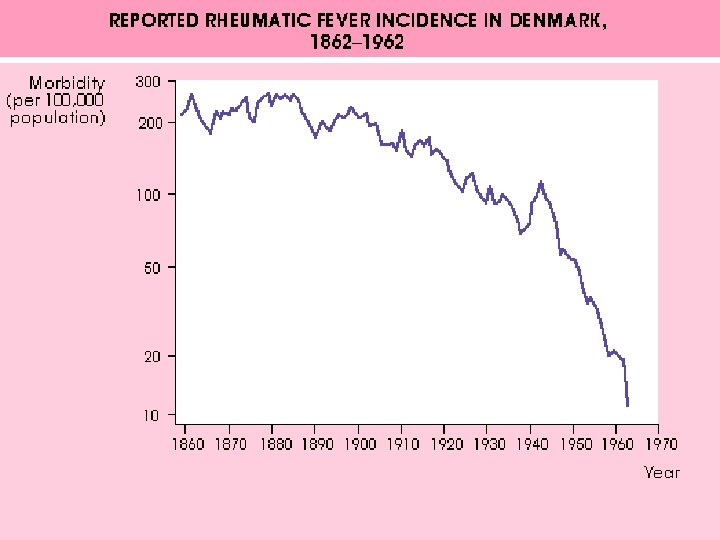
Epidemiology
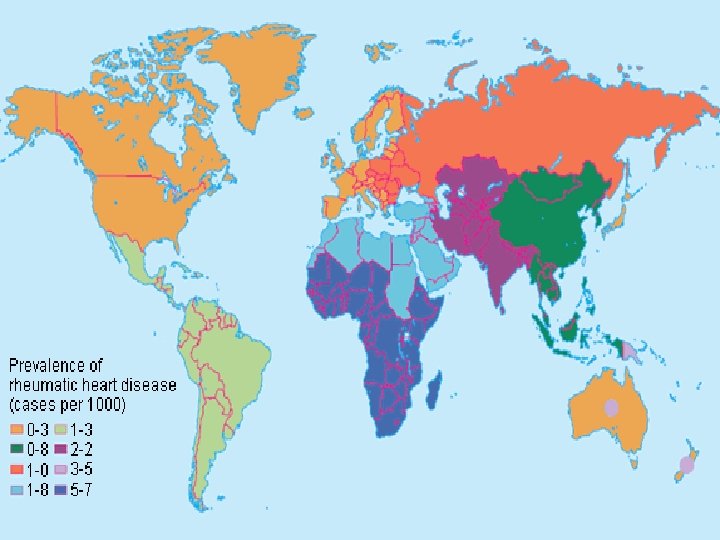

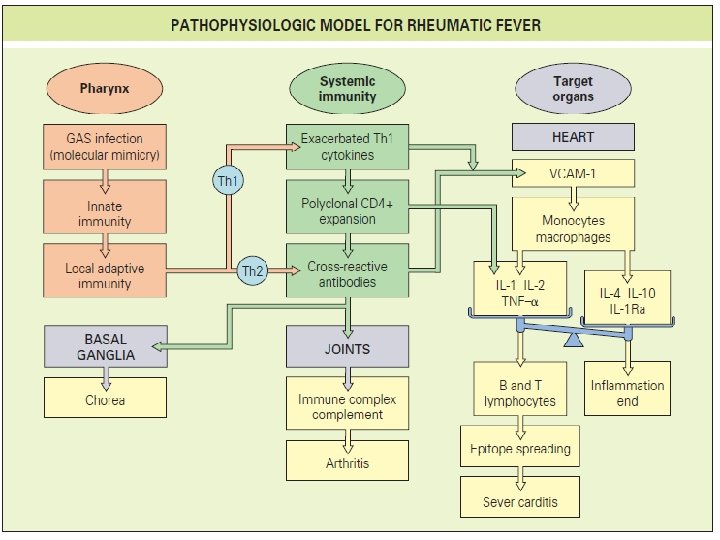
Pathophysiology

Etiology l l Follows group A beta hemolytic streptococcal pharyngitis It is a delayed non-suppurative sequelae to URTI with GABH streptococci.
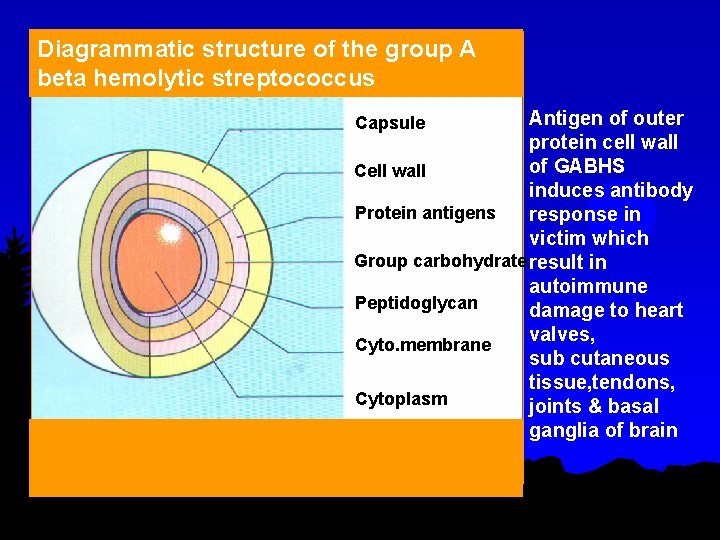
Diagrammatic structure of the group A beta hemolytic streptococcus Antigen of outer protein cell wall of GABHS Cell wall induces antibody Protein antigens response in victim which Group carbohydrate result in autoimmune Peptidoglycan damage to heart valves, Cyto. membrane sub cutaneous tissue, tendons, Cytoplasm joints & basal ganglia of brain Capsule ……………………… ……. . .

l l l Group A Beta Hemolytic Streptococcus Strains that produces rheumatic fever M types l, 3, 5, 6, 18 & 24 Pharyngitis- produced by GABHS can lead to- acute rheumatic fever , rheumatic heart disease & post strept. Glomerulonepritis Skin infection- produced by GABHS leads to post streptococcal glomerulo nephritis only. It will not result in Rh. Fever or carditis as skin lipid cholesterol inhibit antigenicity
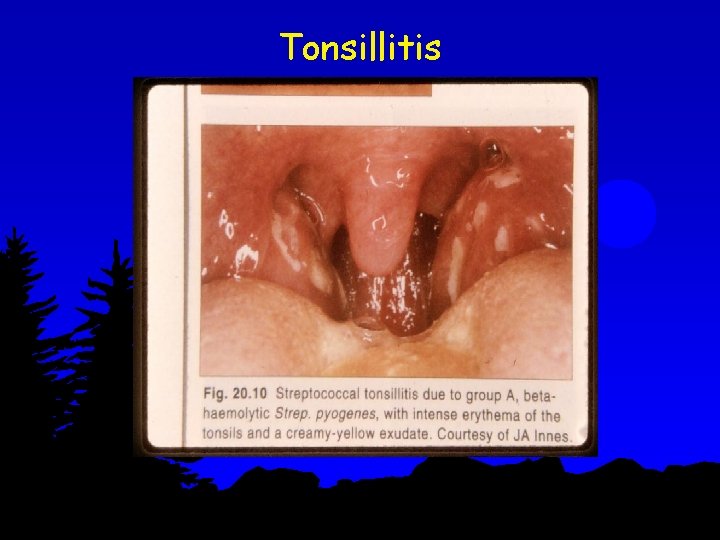
Tonsillitis

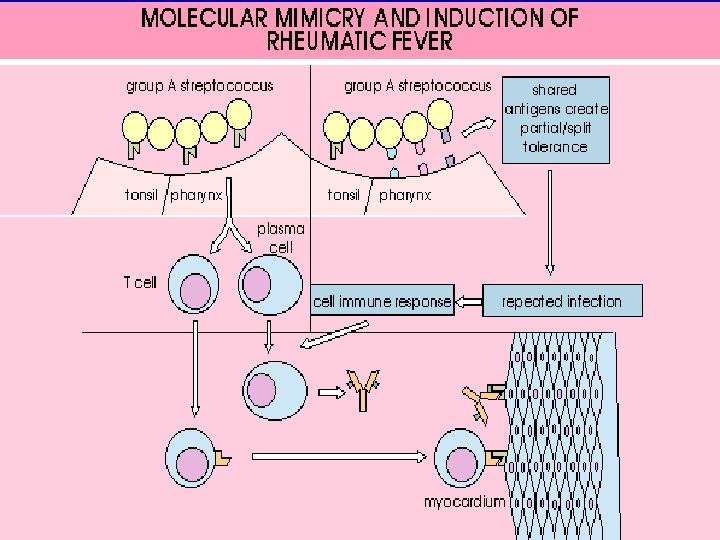
Pathogenesis Abnormal immune response to one or more as yet unidentified somatic or extracellular antigens produced by all (or perhaps only by some) group A streptococci.

Pathogenesis l l Delayed immune response to infection with group. A beta hemolytic streptococci. After a latent period of 1 -3 weeks, antibody induced immunological damage occur to heart valves, joints, subcutaneous tissue & basal ganglia of brain

Pathogenesis l l Antigenic mimicry Predisposing genetic influence

Arthritis l l l Migratory polyarthritis, involving large joints: knee, ankle, elbow & wrist Occur in 80% Involved joints are exquisitely tender In children below 5 yrs arthritis usually mild but carditis more prominent Arthritis do not progress to chronic disease

l It usually does not affect the small joints of the hands or feet and seldom involves the hip joints

Carditis

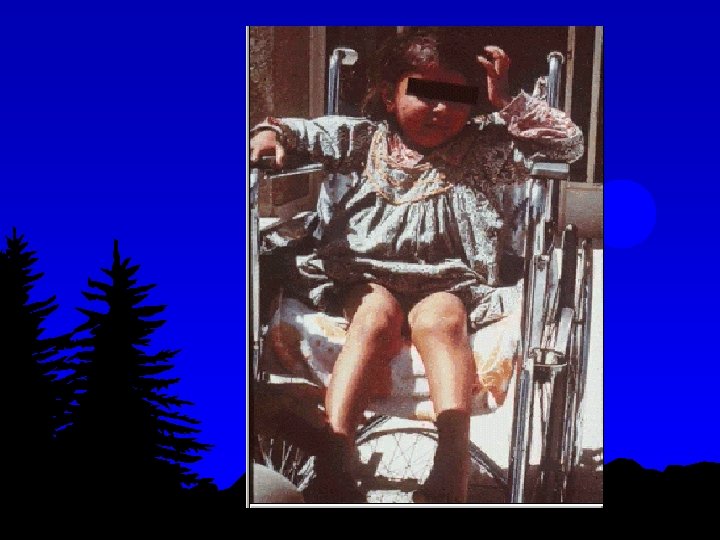
Sydenham Chorea l l l Occur in 5 -10% of cases Mainly in girls of 5 -15 yrs age May appear even 6/12 month after the attack of rheumatic fever Clinically manifest as deterioration of handwriting, emotional lability or grimacing of face Clinical signs- milking sign of hands


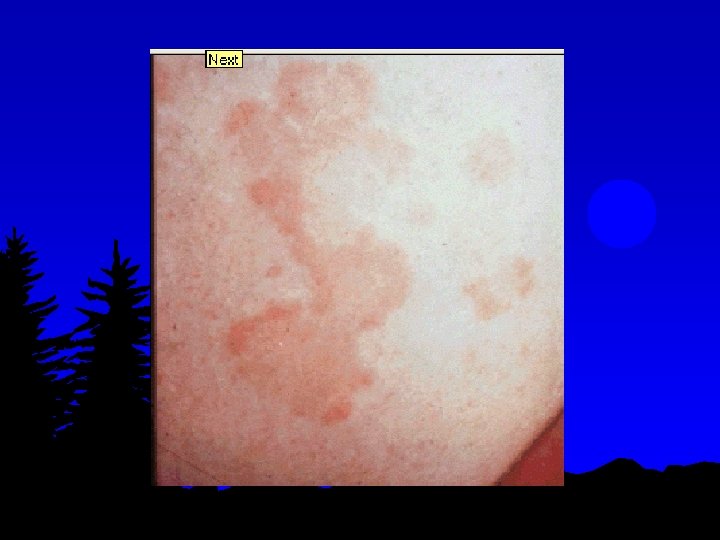
4. Erythema Marginatum l l l Occur in <5%. Unique, transient, serpiginous-looking lesions of 1 -2 inches in size Pale center with red irregular margin More on trunks & limbs & non-itchy Worsens with application of heat Often associated with chronic carditis
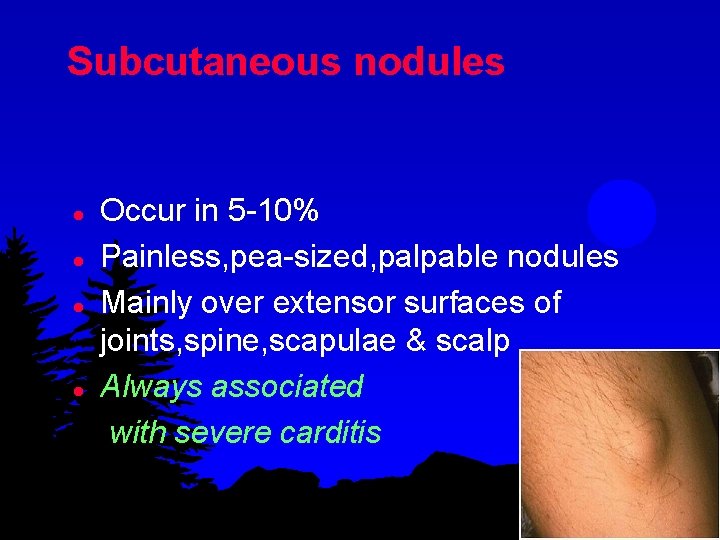
Subcutaneous nodules l l Occur in 5 -10% Painless, pea-sized, palpable nodules Mainly over extensor surfaces of joints, spine, scapulae & scalp Always associated with severe carditis
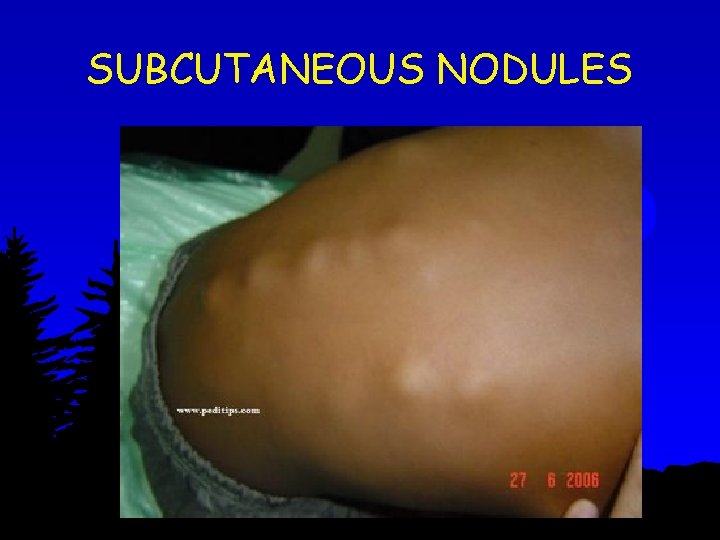
SUBCUTANEOUS NODULES

Other features (Minor features) l l l Fever Arthralgia Pallor Anorexia Loss of weight

Laboratory Findings l l l High ESR Anemia, leucocytosis Elevated C-reactive protien ASO titre >200 Todd units. 80% (Peak value attained at 3 weeks, then comes down to normal by 6 weeks) Anti-DNAse Throat culture-GABHstreptococci 20 -40%

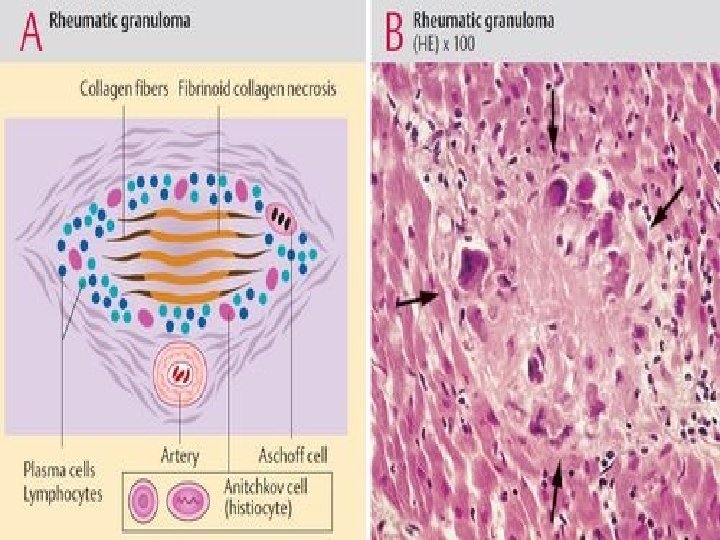
Pathology Aschoff nodule (body)

Diagnosis l l Rheumatic fever is mainly a clinical diagnosis No single diagnostic sign or specific laboratory test available for diagnosis

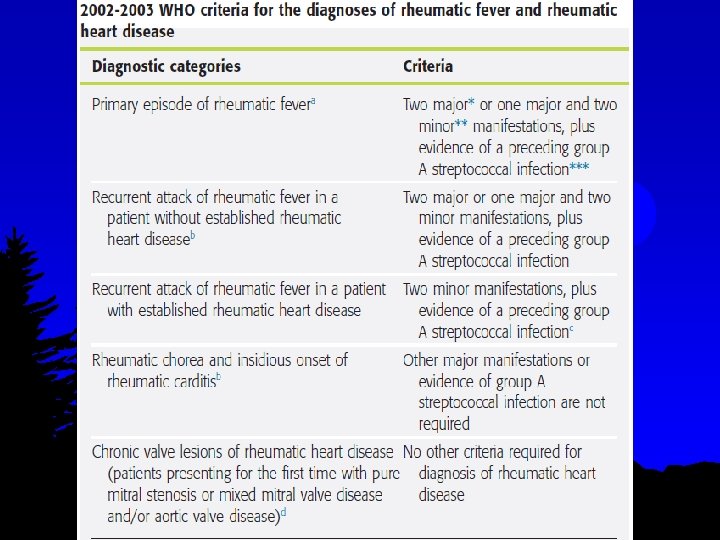
Major & Minor manifestations Major Minor l Carditis l Polyarthritis l Chorea l Erythema marginatum, (erythrocyte sedimentation l Subcutaneous nodules. rate or leukocyte count). l Fever l Polyarthralgia l Acute-phase reactants

Supporting evidence for a preceding GAS l Prolonged PR interval l Elevated or rising aso or antibody l Positive throat culture l Positive rapid antigen test l Recent scarlet fever.
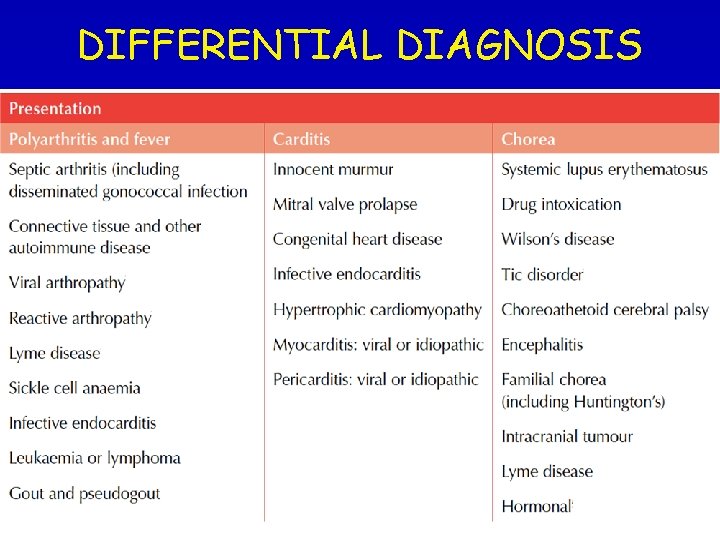
DIFFERENTIAL DIAGNOSIS

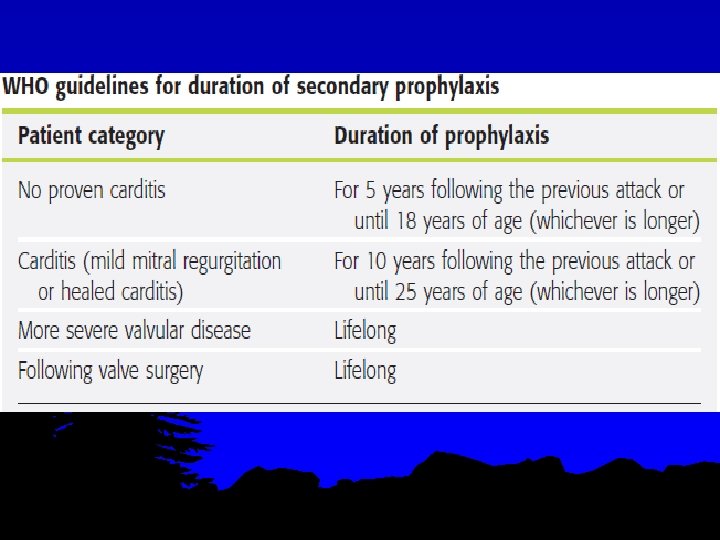
Treatment l l l Step I - primary prevention (eradication of streptococci) Step II - anti inflammatory treatment (aspirin, steroids) Step III- secondary prevention (prevention of recurrent attacks)

ANTI-INFLAMMATORY AGENTS l l Aspirin 4 -8 grams/day for adults Continue anti-inflammatory therapy until ESR or CRP are normal May need steroids if there is cardiac involvement to help prevent sequelae such as mitral stenosis Corticosteroids, if indicated, are given at prednisone 2 mg/kg/day for 2 weeks and then tapered


Prognosis l l l Rheumatic fever can recur whenever the individual experience new GABH streptococcal infection, if not on prophylactic medicines Good prognosis for older age group & if no carditis during the initial attack Bad prognosis for younger children & those with carditis with valvar lesions
- Slides: 41