Donor Case Studies Optimal Management HarborUCLA Critical Care

Donor Case Studies Optimal Management Harbor-UCLA Critical Care – Organ Donation Symposium April 12, 2010 Brant Putnam, MD FACS Trauma / Acute Care Surgery / Surgical Critical Care Harbor-UCLA Medical Center

What is OPTIMAL donor management? = GOOD CRITICAL CARE

OPTIMAL donor management begins PRIOR to proclamation of brain death. The ICU nurses and physicians are jointly responsible for optimal donor management, not just the OPO.

If the patient has not been formally pronounced brain dead, then the patient is alive. Who is not willing to provide good critical care to a live patient? NO ONE

Case #1 u 63 yo wall male found lying against a u. Possible fall vs. assault u. Large laceration to occipital area u. GCS 1 -4 -1 u. Pupils sluggish

Case #1 u Called as a “Tier II” (high acuity) trauma u. A - Patent, but not protected u. B - Spontaneous, clear bilaterally u. C - P = 86 BP – 150 u. D - Unresponsive GCS = 1 -4 -1 Pupils 3 2, sluggish Blood from left ear
Case #1 u Intubated in the ED for airway protection u Taken for CT scan for suspected severe traumatic brain injury
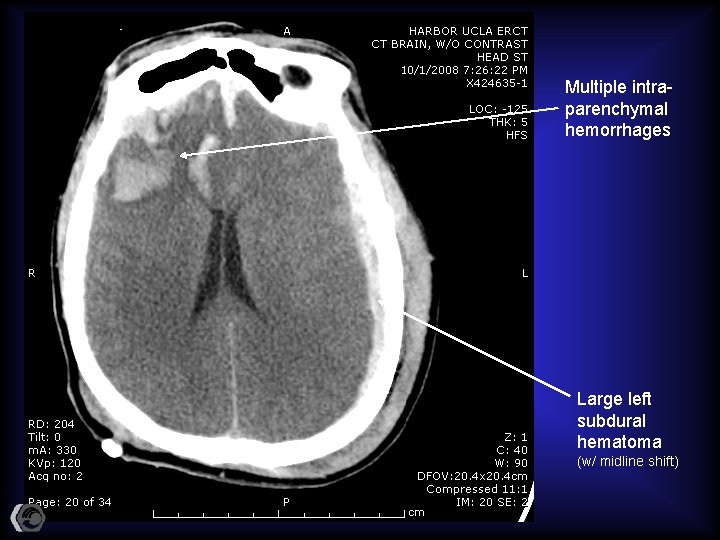
Multiple intraparenchymal hemorrhages Large left subdural hematoma (w/ midline shift)
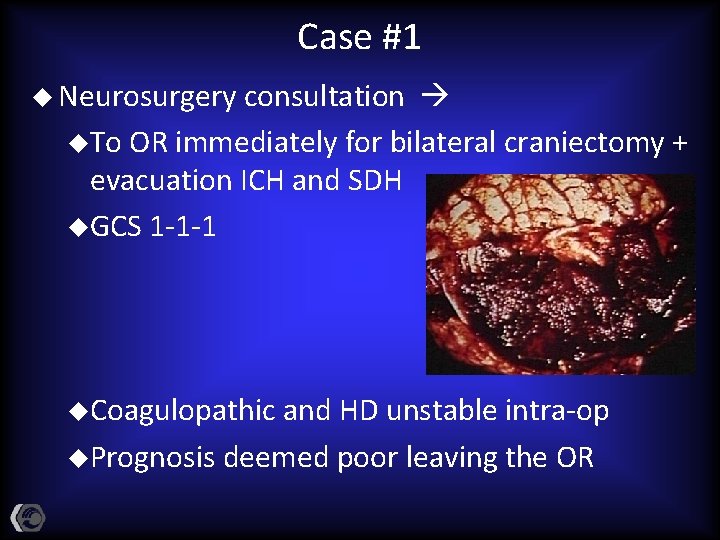
Case #1 u Neurosurgery consultation u. To OR immediately for bilateral craniectomy + evacuation ICH and SDH u. GCS 1 -1 -1 u. Coagulopathic and HD unstable intra-op u. Prognosis deemed poor leaving the OR

Case #1 u Patient Time BP P transported to ICU 0400 2200 140/70 90 85 2300 160/80 110 0000 80/60 60 0100 100/70 100 Labetalol given Levophed started What do you think happened here?
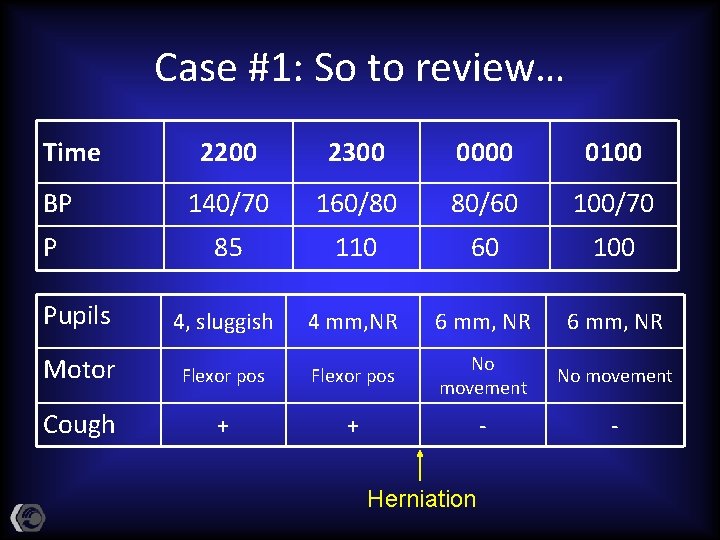
Case #1: So to review… Time 2200 2300 0000 0100 BP 140/70 160/80 80/60 100/70 P 85 110 60 100 Pupils 4, sluggish 4 mm, NR 6 mm, NR Motor Flexor pos No movement Cough + + - - Herniation
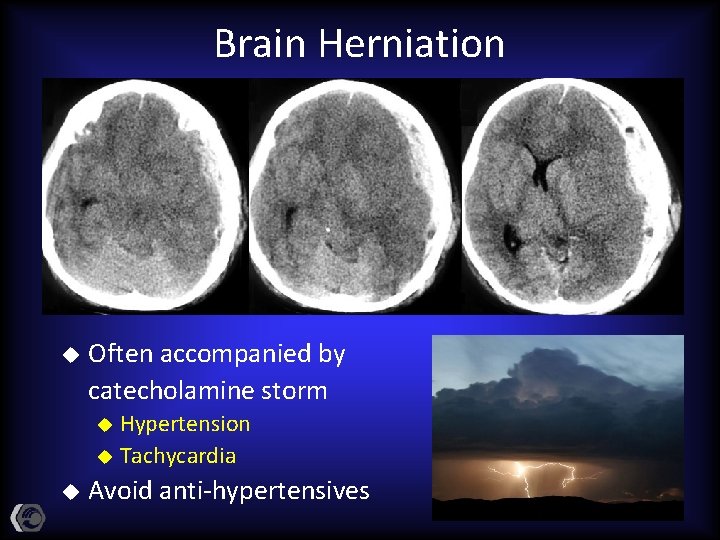
Brain Herniation u Often accompanied by catecholamine storm Hypertension u Tachycardia u u Avoid anti-hypertensives
Management Goal #1 u Appropriate hemodynamic resuscitation to maintain perfusion to potential organs for donation u Maintain MAP 65 -100 mm. Hg u Place central venous line; fluid resuscitation to CVP 4 -10 cm H 20 u Use of < 1 vasopressor u Dopamine < 10 mcg/kg/min u Levophed < 10 mcg/min u Neosynephrine < 60 mcg/min u Consider hormonal resuscitation with T 4 protocol

What should happen next? ? u Begin testing for brain death u One Legacy notification (actually should have already been notified!!!) u Clinical optimization

When to notify One Legacy…

Case #1: What did happen…. u Next u One morning… 1200 noon Legacy notified u Physician to hold family conference to discuss poor prognosis u No new orders written…

No new orders written… Time 0800 1200 1800 24 hr total UOP 300 250 300 100 - 1000 cc Na 153 158 164 165 What do you think is going on here? Management?
Diabetes Insipidus u Excretion of large amounts of severely dilute urine u “Central” – no ADH release from brain u Kidney can not concentrate urine u Therapy u DDAVP (desmopressin acetate) u Synthetic u Free analogue of ADH water replacement u Frequent monitoring of serum Na

What was done… u DDAVP given at 1900 Time UOP Na 0800 300 153 1200 250 158 1800 300 164 2400 165 Free water replacement started next morning (POD #2)… u M. D. “brain death evaluation when electrolytes correct” u

Management Goal #2 u Maintain perfusion to all organs u Goal urine output 1 -3 cc/kg/hr u Suspect DI if U/O > 200 cc/hr x 2 hrs u Treat with DDAVP and fluid (free H 2 O) u Keep serum Na 135 -155
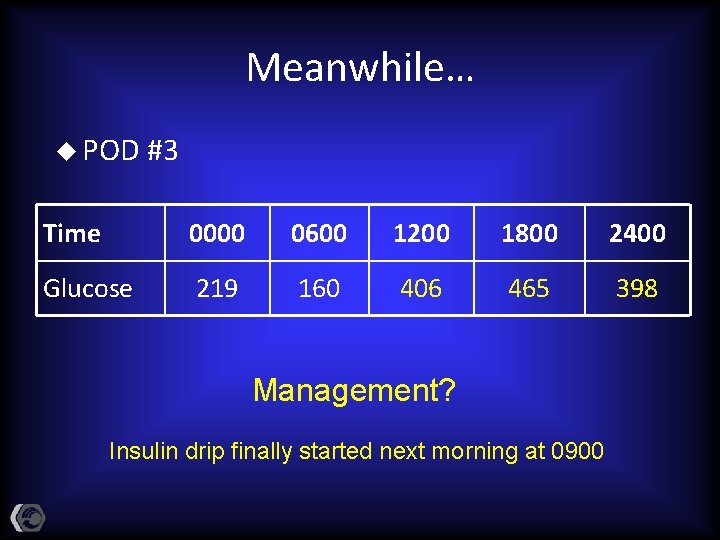
Meanwhile… u POD #3 Time 0000 0600 1200 1800 2400 Glucose 219 160 406 465 398 Management? Insulin drip finally started next morning at 0900

Management Goal #3 u Potential donors are critically ill patients u Tight glucose control applies u. Increase frequency of Accu-checks u. Increase sliding scale u. Insulin drip as needed u Goal is to keep serum glucose < 150

As time passes. . . u Multiple ventilator alarms u PIPs 45 -50 u Low exhaled tidal volumes u O 2 sats 85% u Increase TVs to 1 L to maintain sats 88 -90% Is this the best ventilator management?

Management Goal #4 u Maintain good oxygenation u Pa. O 2/Fi. O 2 ratio > 300 u Reduce Fi. O 2 to reduce oxygen toxicity u Avoid high PEEP effects on hemodynamics u Maintain u ABG u Avoid u PIPs adequate ventilation p. H 7. 30 -7. 45 barotrauma to lungs < 32 cm H 20
Case #1: POD #4 0300 1 st Brain Death Note written (Note: 75 hours after herniation event) 1000 2 nd Brain Death Note written 1455 One Legacy obtains consent for all organs and tissue

Case #1: Outcome u HD deterioration to near-code u Poor organ function u Crashed donor to OR because of instability u Kidneys recovered u Kidney biopsy results poor u No organs suitable for transplant

Case #2 – Getting it right. . . u 22 yo male S/P pedestrian struck by auto x 2 u GCS 1 -1 -1 u Lost pulses on arrival; CPR x 12 min u Devastating brain injury u One Legacy notified within 4 hours of arrival
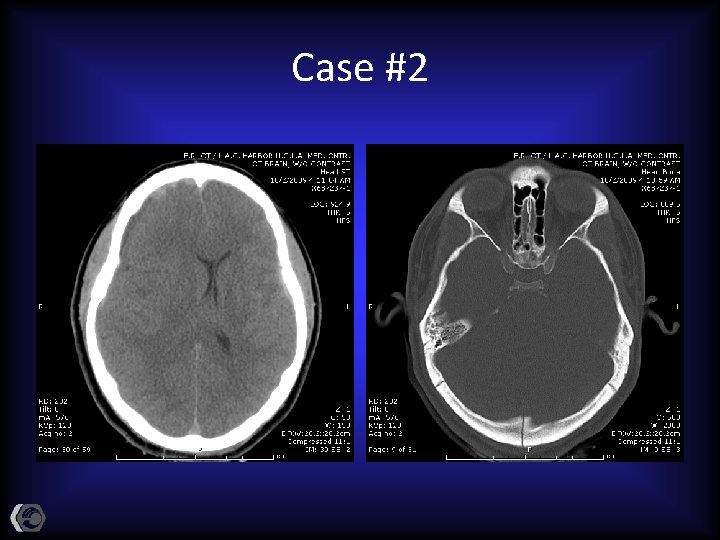
Case #2
Case #2 u Ongoing resuscitation u IV fluid to CVP 8 u Blood products to keep Hb near 10 u Correction of coagulopathy u Use of Levophed to maintain MAP > 65 u Addition of T 4 within 4 hours u Adequate u ABG oxygenation / ventilation 7. 39 / 40 / 118 / 24 / -2 / 99% u Pa. O 2 / Fi. O 2 = 350 u PIPs 22 -24
Case #2 u Early treatment of DI u DDAVP u Free water replacement u Na 150 -154 u Tight u Loss glycemic control with insulin drip of brainstem functions u First BD note < 12 hours after arrival
Case #2 u Outcome centers: u Right - 7 organs transplanted at local lung u Left lung u Heart u Liver u Right kidney u Left kidney u Pancreas

Case #3: Steven u 17 yo male S/P skateboarding accident u. GCS 1 -1 -1 u. Severe DAI, small SDH on CT scan u. Devastating brain injury

Case #3: Steven
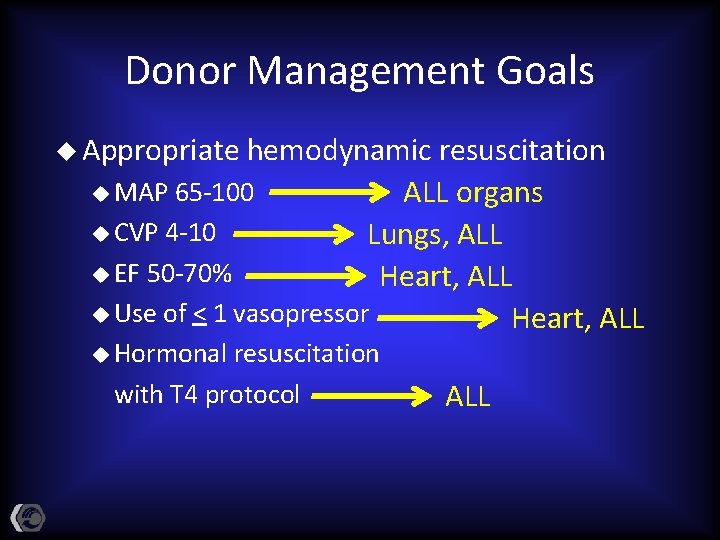
Donor Management Goals u Appropriate hemodynamic resuscitation u MAP 65 -100 ALL organs u CVP 4 -10 Lungs, ALL u EF 50 -70% Heart, ALL u Use of < 1 vasopressor Heart, ALL u Hormonal resuscitation with T 4 protocol ALL
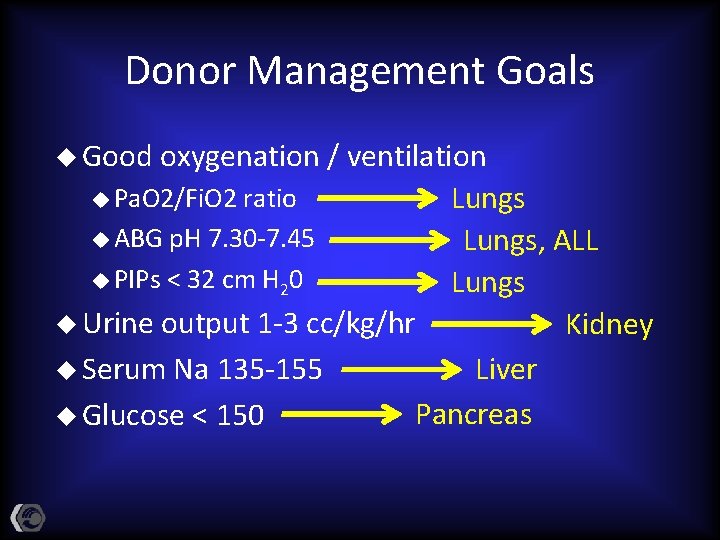
Donor Management Goals u Good oxygenation / ventilation u Pa. O 2/Fi. O 2 ratio Lungs u ABG p. H 7. 30 -7. 45 Lungs, ALL u PIPs < 32 cm H 20 Lungs u Urine output 1 -3 cc/kg/hr Kidney u Serum Na 135 -155 Liver Pancreas u Glucose < 150
- Slides: 35