Does Feeding Tube Insertion and Its Timing Improve

Does Feeding Tube Insertion and Its Timing Improve Survival? Ryan Zitnay MD Journal Club December 14, 2012

Patient Case • 87 year old veteran male NH resident with multiple medical problems including advanced dementia (MMSE<10), systolic heart failure (EF 10%), Afib, CVA with residual deficits now with worsening eating problems • Multiple episodes of aspiration pneumonia leading to transfers to acute care facilities

Patient Case • Evaluated by speech: – Signs and symptoms consistent with ongoing aspiration with all consistencies • Recurrent aspiration events likely – “All routes: prandial, secretions, reflux possible”

Patient Case • On dysphagia mechanically altered and nectar thick liquids diet • Requires full assist with feeds • Strict aspiration precautions – HOB > 30 degrees – Thorough oral hygiene – Small amounts per mouthful

The Dilemma • Resident no longer felt “safe” to take in food orally • Continued aspiration episodes despite aggressive precautions by staff • Generally declining health: dementia, CHF • Family meeting with wife, daughter – Questioned possibility of tube feeding? – Main motivation to prolong survival

If you were the provider… • Based on your knowledge of the current evidence, what would you recommend to this family?

Despite our common practice here at BUGS… • PEG tubes are still being placed frequently in older adult patients nearing the end of their life • Prevalence thought to be 18 -34% nationally – Varies significantly state by state – 56/1000 demented NH residents had PEGs placed
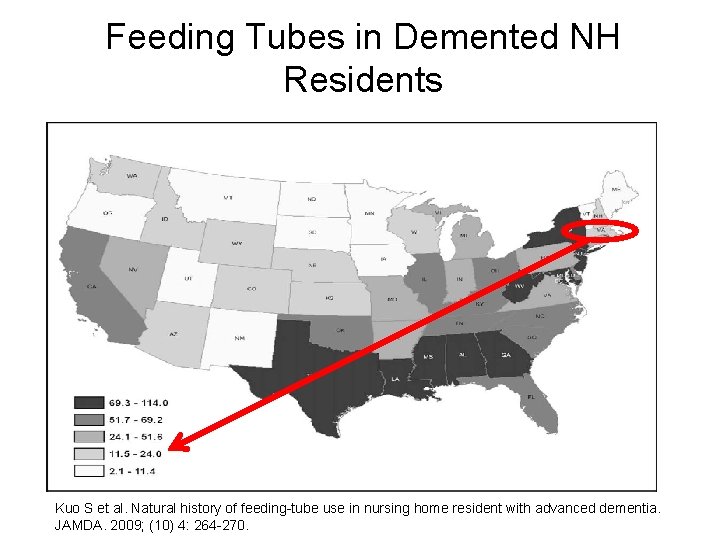
Feeding Tubes in Demented NH Residents • Figure 1 Kuo et al 2009 Kuo S et al. Natural history of feeding-tube use in nursing home resident with advanced dementia. JAMDA. 2009; (10) 4: 264 -270.

Why is this happening? • Dementia is one of leading causes of death in US • Eating problems develop in 90% of those with advanced dementia – Loved ones concerned will “starve to death” • Many families & providers see as only option

Perceived Benefits of Tube Feeding • By healthcare providers, patients, & surrogates: – Better nutritional status – Reduced risks of complications such as aspiration PNA, pressure ulcers, infection – Improved functional status and quality of life – Safe, effective, easily-obtained, inexpensive procedure – Prolonged survival • But are these supported by the evidence? Kuo S et al. Natural history of feeding-tube use in nursing home resident with advanced dementia. JAMDA. 2009; (10) 4: 264 -270.

Perceived Benefits of PEG Tubes • Prolonged Survival – 2 observational studies concluded against – BUT • 6 -mo survival varied tremendously among those with PEGs placed: 10 -85% • 5 studies performed at same institution • 2 studies used MDS data solely: no differentiation between NGT & PEG = limited generalizability – Are patients being referred too late to receive benefits?

Background • Editorial ’ 08 AJG questioned interpretation that feeding tubes do not effect survival – Most evidence retrospective – Called for prospective research to further examine Delegge MH. Percutaneous Endoscopic Gastrostomy in the Dementia Patient: Helpful or Hindering? Am J Gastroenter 2008; 103: 1018 -1020


Aims of Study • Does feeding tube insertion affect survival in NH residents with advanced dementia? • Is the timing of insertion after development of eating problems associated with different patterns of survival?

Methods • Prospective cohort study • 1999 – 2007 • Nationwide data – All US nursing homes – Merged Medicare claims & Minimum Data Set (MDS) NH resident assessments • NH residents with advanced cognitive impairment & new eating problems
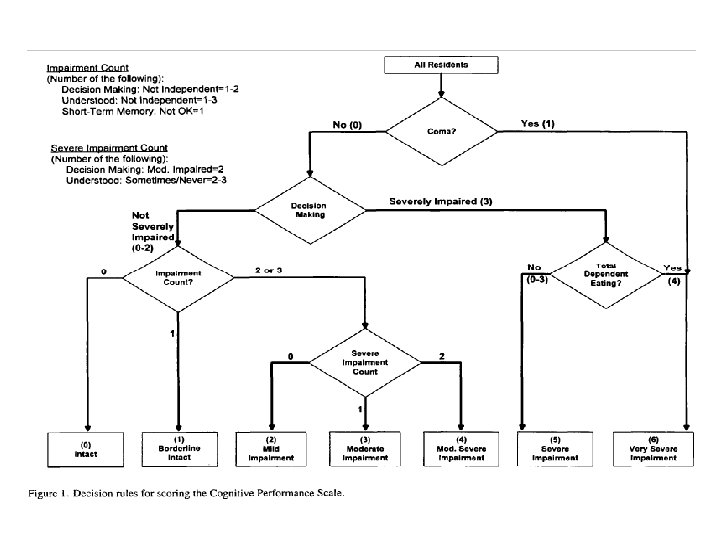
Inclusion Criteria • MDS assessment with – New Cognitive Performance Score (CPS) of 6 • Indicates patient needs assist with eating • Had to have increased from 4 or 5 previously – Diagnosis of Dementia

Exclusion Criteria • Based on review of MDS & Medicare claims: – Comatose – Died within 2 weeks of MDS assessment – Any evidence of PEG feeding in prior 6 months • Based on designated procedural codes identified in previous research

Methods • Survival determined by: # of days Baseline MDS Assessment CPS score of 6 Death determined by Medicare Denominator File • Potential confounding variables were chosen based on prior research

Statistical Analysis • Descriptive analysis of baseline characteristics of pts +/- feeding tubes – Chi-square test for categorical variables – t-test for continuous variables • 1 year survival after PEG insertion AND timing of insertion analyses – Multivariate survival models – Accounted for potential selection bias

Results • n = 36, 492 participants – 1, 956 patients in the cohort had feeding tubes inserted (5. 4%) – 34, 536 without feeding tubes
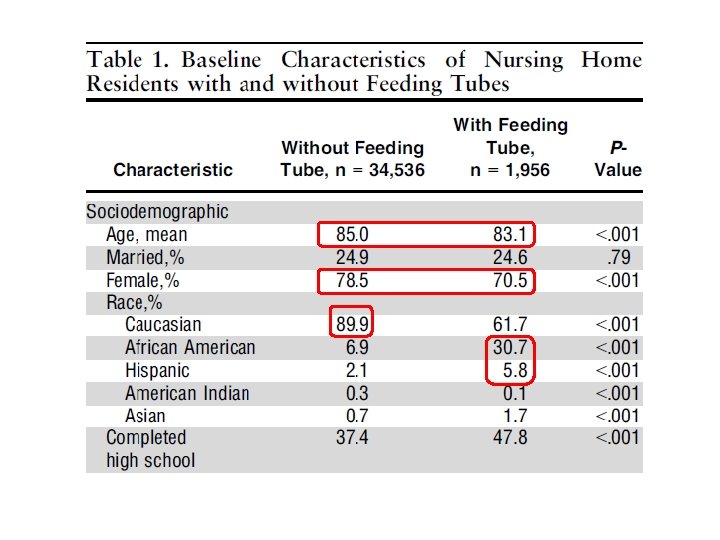
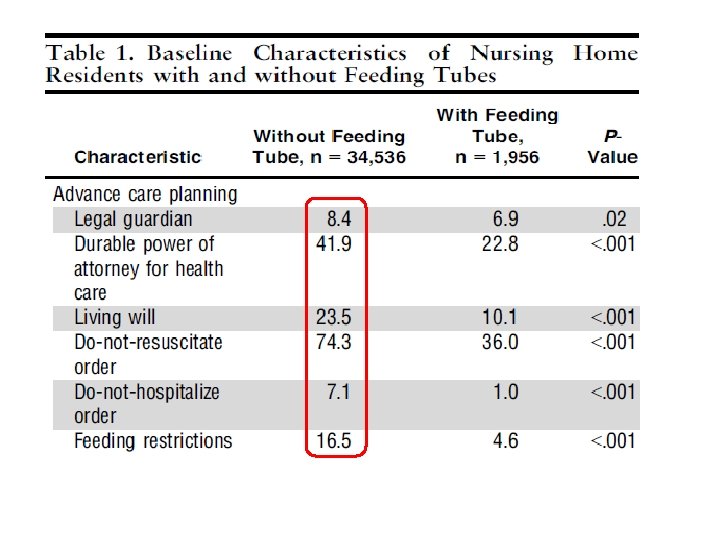
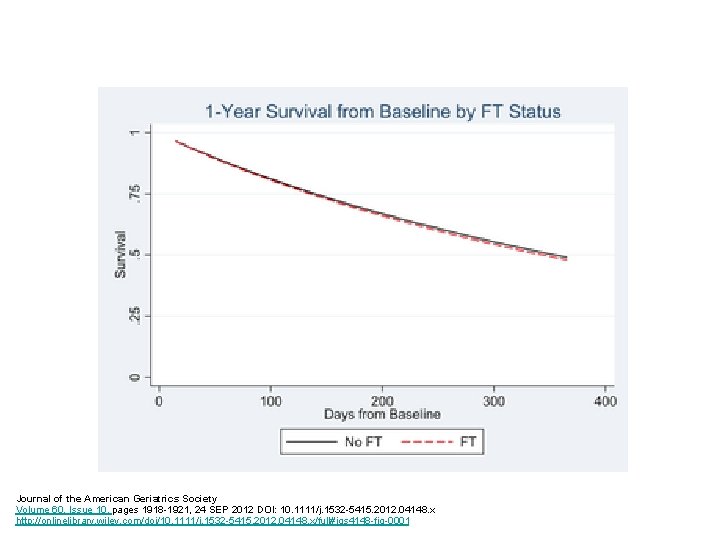
Journal of the American Geriatrics Society Volume 60, Issue 10, pages 1918 -1921, 24 SEP 2012 DOI: 10. 1111/j. 1532 -5415. 2012. 04148. x http: //onlinelibrary. wiley. com/doi/10. 1111/j. 1532 -5415. 2012. 04148. x/full#jgs 4148 -fig-0001

Results: 1 Year Survival • Median Survival 177 days • No association found between insertion of PEG tube & survival time – From “baseline” = development of need for assistance in eating • Adjusted Hazard Ratio 1. 03
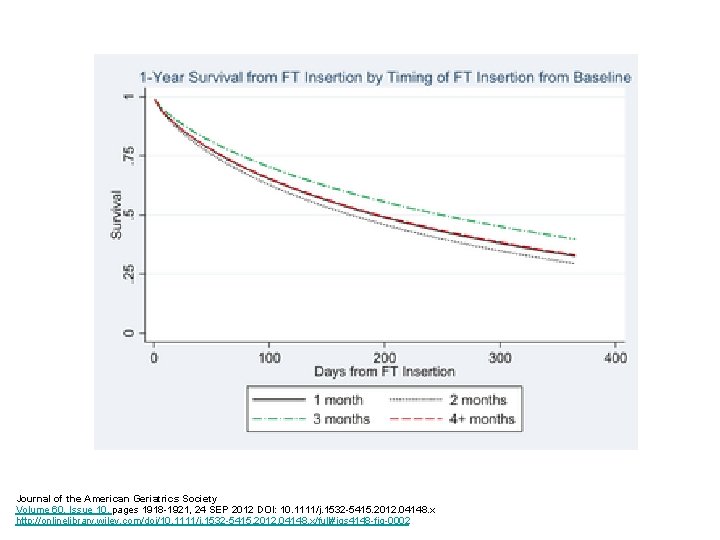
Journal of the American Geriatrics Society Volume 60, Issue 10, pages 1918 -1921, 24 SEP 2012 DOI: 10. 1111/j. 1532 -5415. 2012. 04148. x http: //onlinelibrary. wiley. com/doi/10. 1111/j. 1532 -5415. 2012. 04148. x/full#jgs 4148 -fig-0002

Results: Survival by Timing of Insertion from Baseline • Adjusted Hazard Ratios comparing survival from PEG insertion in Months 1 -3 with those 4+ months: – 1 (n=569): 1. 01 – 2 (n=310): 1. 12 – 3 (n=205): 0. 82 – 4+ (n=872)

Discussion • Study confirms lack of treatment effect on survival • First to show earlier insertion of PEG tube not associated with improved survival – 1 month with similar post-treatment survival as 4+ months

Strengths • • • Prospective! National database Large cohort Distinguished between PEG & NGT Used statistical techniques to control for potential selection bias • Focused on timing of insertion

Limitations • Largely white, female population • Did not incorporate: – Physiological measures of nutrition (other than BMI) – Pt or family member preferences for feeding tube placement • Medical diagnoses were based on MDS • Only focused on NH setting Generalizable?

Conclusions • Supports current literature that there is no survival benefit in PEG tube insertion in advanced dementia – ? Prolonging dying process without meaningful gains in quality of life • The early bird does not get the worm! • Can use to strengthen argument against insertion in inappropriate patients

Back to the Patient • NH team recommended against PEG tube placement • Additional hospitalization for aspiration PNA – Pt intubated; wife pushed for PEG tube while in hospital – Communication between team & inpatient providers prevented placement • Shifted goals to comfort care/hospice – Comfort feeding pursued • Patient died a few months later in NH comfortably

Thank you!
- Slides: 32