DNP CLINICAL SYSTEMS ADMINISTRATION CAPSTONE PROJECT Communication and





















- Slides: 27

DNP CLINICAL SYSTEMS ADMINISTRATION CAPSTONE PROJECT Communication and Civility Workshop in Healthcare and the Effects on Patient Satisfaction and the Work Environment By: Leah Lax RN-BSN CINDY COSTANZO PHD, RN, CNL PROJECT ADVISOR CREIGHTON UNIVERSITY JENNIFER BONAMER RN-BSN, PHD RESEARCH EDUCATION SPECIALIST MENTOR

FINANCIAL DISCLOSURE • Conflicts of Interest: The planners and presenters of this have not disclosed relevant financial relationships with any commercial companies pertaining to this activity as now such interests exist.

IRB AND ORGANIZATIONAL APPROVAL • Creighton IRB approval – exempt status • IRB at hospital was obtained – exempt status • Nursing Research and EBP council approval • Received organizational, leadership team on medical/surgical unit • Staff were offered 4 different workshop times and highly encouraged (not mandated) by their leadership team to attend.

LEARNING OBJECTIVES OF PROJECT • At the end of this presentation, participants will be able to: • Define effective communication • Distinguish between civil and uncivil behaviors • Identify issues of incivility in a work environment • Identify relationship between communication, civility, patient satisfaction, and healthy work environment • Identify sustainable measures

INTRODUCTION/BACKGROUND • The power of effective communication 13 • Miscommunication cost the US health care system 1. 7 billion dollars in malpractice costs alone and over 2, 000 lives • Miscommunication is number one reason for preventable deaths in the hospital setting 11 7, 18 • It has been discovered that health care professionals who have experienced a form of verbal abuse from colleagues or coworkers tend to miscommunicate information or not communicate it at all 2 • The Joint Commission estimates that 80% of medical errors in the health care setting occur due to poor communication 11 • Civil inter professional communication can be the difference between a healthy and non-healthy work environment and the safety outcomes for the patient 14 • 70% of nurses have experienced incivility in the workplace regularly in the form of condescending language 8 • When this behavior continues, nurses reported that they were less likely to inform those physicians about issues concerning the patient in a timely manner because they didn’t want to fall victim to the abuse 8 • This has led to medication errors, patient safety concerns, and overall unhealthy work environments 2

SIGNIFICANCE • Institute of Medicine printed To Err is Human; Building a Safer Health System that health care professionals understood the gravity of communication issues in the workforce situation 7 • The Joint Commission, an accreditation agency responsible for providing hospital organizations with quality and safety standards, released “The Sentinel Event Alert” in 2008 that addressed workplace behaviors that affect patient outcomes, such as the culture and incivilities in the workplace 8 • Joint Commission came out with an updated agenda for National Patient Safety Goals, the number 2 goal being to “improve effectiveness of communication among caregivers” 10 • HCAHPS survey, (Hospital Consumer Assessment of Healthcare Providers and Systems) 3 of the 11 domains listed for evaluation include the word communication; communication with doctors, communication with nurses, and communication about medications 9 • The American Association of Critical Care Nursing states that communication is one of the six essential standards needed to create a healthy work environment 1

COMMUNICATION AND CIVILITY – A COMPLEX PROBLEM • 800 bed, Magnet Hospital in Southern FL has identified the need for civility in communication to be taught and intentionally identified as a standard of practice • Previous results from baseline survey at this hospital in October 2016 found that over half of respondents had experienced incivility regularly on the job, 43% considered incivility to be a “part of their job”; and, 54% experience incivility from coworkers 19

PURPOSE STATEMENT • The purpose of this project was to improve communication and the experience of civility between Interprofessional staff (registered nurses, technicians, and unit secretaries) who work on a medical surgical unit

AIMS • Conducted a baseline survey to assess the use of civility in communications and patient satisfaction within the workplace environment using the AACN’s Healthy Work Environment Assessment communication subscale tool, Civility and Communication Class Evaluation Tool, the Nursing Incivility Scale (NIS), and HCAHPS scores. • Conducted an educational intervention on civility (1. 5 hour workshop). • Evaluated the effectiveness of the educational intervention. The evaluation included a post workshop survey, the Civility and Communication Class Evaluation Tool and AACN’s Healthy Work Environment subscale of communication, the Nursing Incivility Scale (NIS) and HCAHPS, was completed immediately post educational intervention, at 1 -month, and 2 -month mark.


LITERATURE REVIEW SUBGROUPS • Communication • crucial conversations 6 • Patient Outcomes 16 • Healthy Work Environment and Communication 1, 13 • Education and Communication 3 • Civility • Workplace 12 • Impact of Patient Outcomes 5 • Teaching 17

METHODS – PRE-WORKSHOP • pre and post intervention design • Educational workshop related to civility and communication in healthcare • Nurses, techs, and unit clerks were asked to attend a 1. 5 hour workshop related to civility and communication in health care • Measures were obtained pre-workshop, immediate post workshop, 1 month, and 2 month post workshop

METHODS - SAMPLE AND SETTING • 800 bed hospital, non-profit community, Magnet accredited trauma hospital in southern Florida • Sample consisted of nurses, technicians, and unit clerks members and 36/90 staff members attended the workshop • 30 were registered nurses • 4 were PCTs (personal care techs) • 2 were HUCs (unit clerks)

MEASUREMENT • AACN’s Healthy Work Environment Assessment Tool 1 • Civility and Communication Class Evaluation Tool • HCAHPS scores 9 • Nursing Incivility Scale (NIS) 12 • Personal Interviews – open dialogue and informal

METHODS – DURING WORKSHOP • Participants • signed consents on arrival • given surveys to complete before workshop began • Given consent form to sign stating they are voluntarily participating • First 15 min on definitions – done by Project Lead • Next 45 min on applying concepts and how to address incivility/communication issues – as done by Licensed Mental Health Counselor • Final 30 min on case studies

METHODS – POST WORKSHOP • Participants given survey immediately after class to complete • NIS • AACN Healthy Work Environment Assessment tool – communication questions • Confidence scale/Communication Class Evaluation Tool • Participants given 1 month and 2 month survey via email to complete • Data was pulled from HCAHPS scores for October, November, and December 2018 and compared them to HCAHPS scores in July, August, and September.

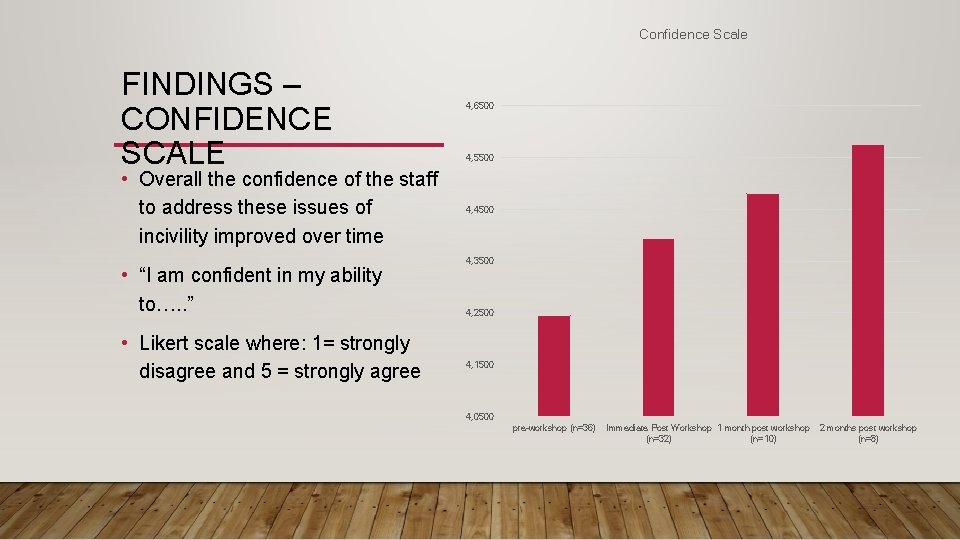
Confidence Scale FINDINGS – CONFIDENCE SCALE • Overall the confidence of the staff to address these issues of incivility improved over time • “I am confident in my ability to…. . ” • Likert scale where: 1= strongly disagree and 5 = strongly agree 4, 6500 4, 5500 4, 4500 4, 3500 4, 2500 4, 1500 4, 0500 pre-workshop (n=36) Immediate Post Workshop 1 month post workshop (n=32) (n=10) 2 months post workshop (n=8)

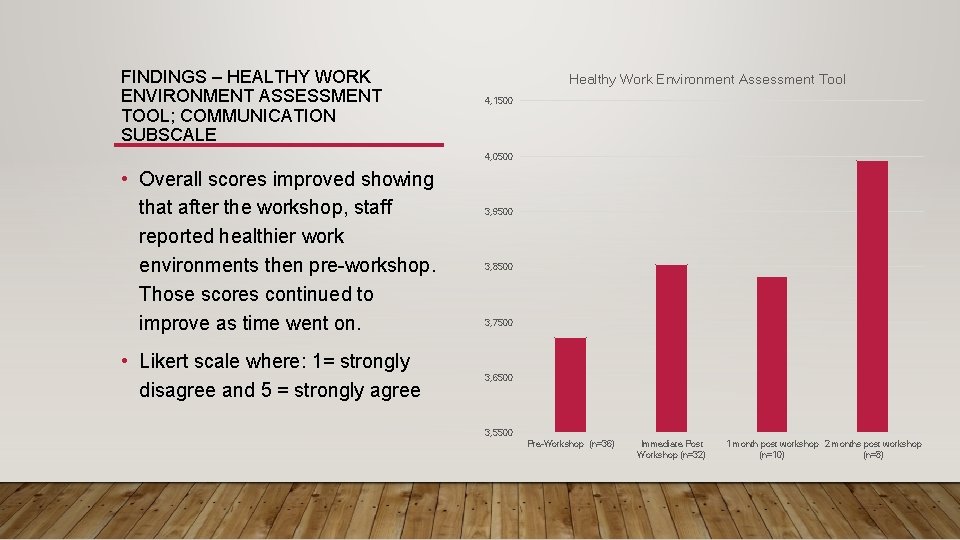
FINDINGS – HEALTHY WORK ENVIRONMENT ASSESSMENT TOOL; COMMUNICATION SUBSCALE Healthy Work Environment Assessment Tool 4, 1500 4, 0500 • Overall scores improved showing that after the workshop, staff reported healthier work environments then pre-workshop. Those scores continued to improve as time went on. • Likert scale where: 1= strongly disagree and 5 = strongly agree 3, 9500 3, 8500 3, 7500 3, 6500 3, 5500 Pre-Workshop (n=36) Immediate Post Workshop (n=32) 1 month post workshop 2 months post workshop (n=10) (n=8)

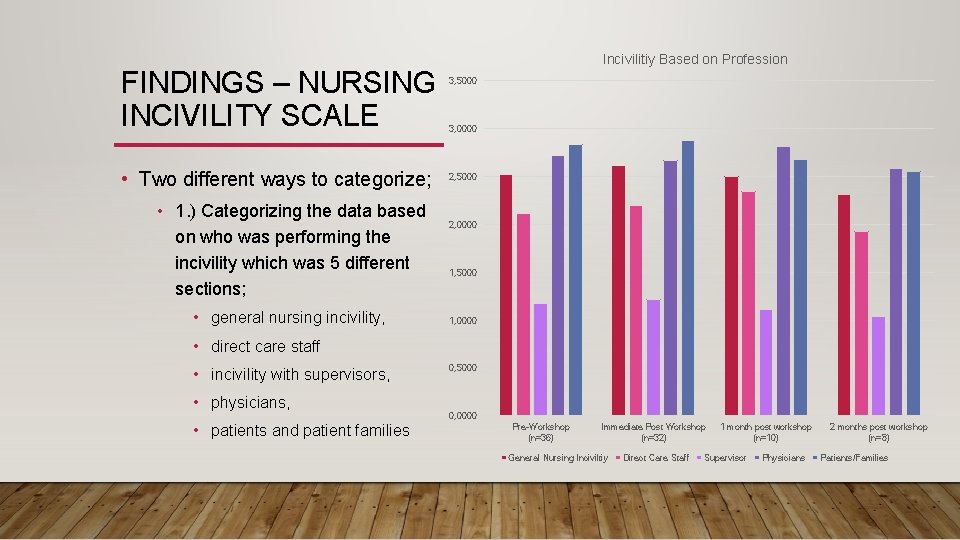
FINDINGS – NURSING INCIVILITY SCALE • Two different ways to categorize; • 1. ) Categorizing the data based on who was performing the incivility which was 5 different sections; • general nursing incivility, Incivilitiy Based on Profession 3, 5000 3, 0000 2, 5000 2, 0000 1, 5000 1, 0000 • direct care staff • incivility with supervisors, 0, 5000 • physicians, • patients and patient families 0, 0000 Pre-Workshop (n=36) Immediate Post Workshop (n=32) General Nursing Inciviltiy Direct Care Staff 1 month post workshop (n=10) Supervisor Physicians 2 months post workshop (n=8) Patients/Families

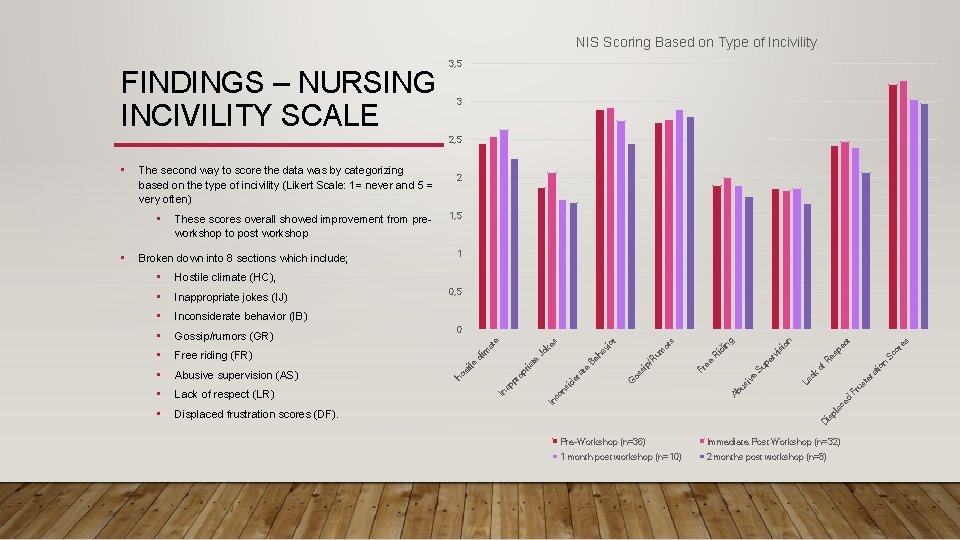
NIS Scoring Based on Type of Incivility FINDINGS – NURSING INCIVILITY SCALE 3, 5 3 2, 5 es or Sc n tio ra of te ck Fr us La Su ed Ab us iv e R pe es rv i si pe ct on g ee Fr R si p/ os G R um id in or s or ha vi Be e ac pl is D Displaced frustration scores (DF). at • id er Lack of respect (LR) s • ke Abusive supervision (AS) ns • co Free riding (FR) Jo • 0 In Gossip/rumors (GR) te • ria Inconsiderate behavior (IB) op • 0, 5 e Inappropriate jokes (IJ) ap pr • at Hostile climate (HC), In • 1 im Broken down into 8 sections which include; 1, 5 cl • These scores overall showed improvement from preworkshop to post workshop ile • 2 st The second way to score the data was by categorizing based on the type of incivility (Likert Scale: 1= never and 5 = very often) ho • Pre-Workshop (n=36) Immediate Post Workshop (n=32) 1 month post workshop (n=10) 2 months post workshop (n=8)

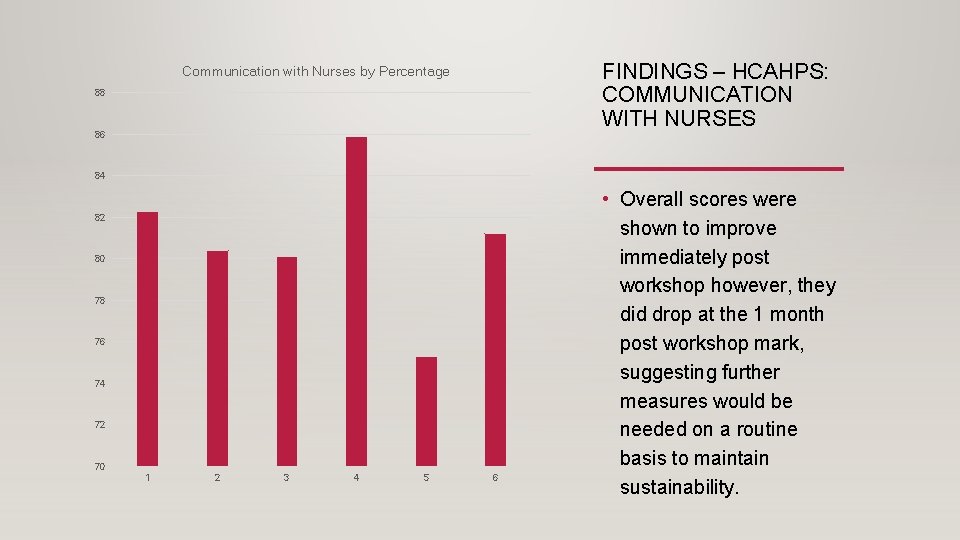
FINDINGS – HCAHPS: COMMUNICATION WITH NURSES Communication with Nurses by Percentage 88 86 84 82 80 78 76 74 72 70 1 2 3 4 5 6 • Overall scores were shown to improve immediately post workshop however, they did drop at the 1 month post workshop mark, suggesting further measures would be needed on a routine basis to maintain sustainability.

EVALUATION PLAN • Create “civility specialists” on each unit – use as resource for staff when addressing issues on unit between staff, patients, families, etc. • Support staff with “nurse rounders” • Yearly Health. Stream on importance of communication and civility in working environment and during orientation • Quarterly civility training classes/meetings for those who are “civility specialists” and those who want to gain more skills/knowledge

STRENGTHS AND LIMITATIONS STRENGTHS LIMITATIONS • Great feedback from staff • Sample size: 36 initial – final survey only had 8 • Overall success in workshop • Staff requested more courses/training • Supported by Leadership team • Workshop was well received • NIS discrepancies – 2 versions of survey • Sign up time – only given 2 weeks notice

DNP IMPLICATIONS Scholarship Leadership Policy Clinical Review of literature helps improve knowledge of topic and gain stakeholder support Ability to take initiative; start pilot program Work Place Violence Policy – needs additional focus on civility and prevention/escalation at bedside Gather support from leadership teams Encourage initiation of program to support staff when these issue arise Financial support Workshop provided a learning atmosphere for participants Teaching the class Taking lead on the topic Provide staff with incentives – how do we market to bedside staff?

ACKNOWLEDGEMENTS • Miriam Lacher MA, MRC, LMHC – Presenter at workshop • 6 ET leadership staff: Kariann Harris (manager), Lauren Linde (clinical coordinator), Kelly Lulofs (educator) • Jean Lucas ARNP, MBA, RN – Associate Chief Nursing Officer SMH • Cindy Costanzo Ph. D, RN, CNL – Creighton University Project Advisor • Jennifer Bonamer Ph. D, RN-BC, AHN-BC – Research Specialist

QUESTIONS

1. ) American Association of Critical Care Nurses. 2016. AACN healthy work environment assessment tool. 2. ) American Association of Critical Care Nurses. 2005. Nurse to physician communication. 3. ) Baker, M. J. , & Durham, C. F. (2013). Interprofessional Education: A Survey of Students' Collaborative Competency Outcomes. Journal Of Nursing Education, 52(12), 713 -718. doi: 10. 3928/01484834 -20131118 -04 REFERENCE S 4. ) Bylund, C. , Peterson, E. , & Cameron, K. (2012). A practitioner’s guide to interpersonal communication theory: An overview and exploration of selected theories. Patient Education and Counseling, 87(3), 261 -267. Doi: 10. 1016/j. pec. 2011. 10. 006 Retrieved from: https: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 3297682/ 5. ) Dang, D. , Bae, S. H. , Karlowicz, K. A. , & Kim, M. T. (2016). Do clinician disruptive behaviors make an unsafe environment for patients? . Journal of nursing care quality, 31(2), 115 -123. 6. ) De. Voe, J. E. , Wallace, L. S. , & Fryer Jr, G. E. (2009). Measuring patients’ perceptions of communication with healthcare providers: do differences in demographic and socioeconomic characteristics matter? . Health Expectations, 12(1), 70 -80 7. ) Ellison, Deborah. 2015. Communication skills. Elsevier 8. ) Felblinger, D. M. (2009). Bullying, incivility, and disruptive behaviors in the healthcare setting: identification, impact, and intervention. Frontiers of health services management, 25(4), 13 -23. 9. ) HCAHPS. 2017. Technical notes for HCAHPS star ratings report. Retrieved from: http: //www. hcahpsonline. org/Files/April_2017_Star%20 Ratings_Tech%20 Notes. pdf 10. ) Joint Commission. 2015. National patient safety goals effective January 1, 2015. Retrieved from: http: //www. jointcommission. org/assets/1/6/2015_NPSG_HAP. pdf 11. ) Kern, Christine. 2016. Healthcare miscommunication costs. Health-it Outcomes 12. ) Laschinger, H. K. S. (2014). Impact of workplace mistreatment on patient safety risk and nurse-assessed patient outcomes. Journal of Nursing Administration, 44(5), 284 -290. 13. ) Makary, M. A. , & Daniel, M. (2016). Medical error—the third leading cause of death in the US. Bmj, 353, i 2139. 14. ) Manojlovich, M. , & De. Cicco, B. (2007). Healthy work environments, nurse-physician communication, and patients’ outcomes. American Journal of Critical Care, 16(6), 536 - 543. 15. ) Pirnejad, H. , Niazkhani, Z. , Berg, M. , & Bal, R. (2008). Intra-organizational communication in healthcare. Methods of Information in Medicine , 47(4), 336 -45. 16. ) Propp, K. M. , Apker, J. , Zabava Ford, W. S. , Wallace, N. , Serbenski, M. , & Hofmeister, N. (2010). Meeting the complex needs of the health care team: identification of nurse—team communication practices perceived to enhance patient outcomes. Qualitative Health Research, 20(1), 15 -28. 17. ) Skarbek, A. J. , Johnson, S. , & Dawson, C. M. (2015). A phenomenological study of nurse manager interventions related to workplace bullying. Journal of nursing administration, 45(10), 492 -497. 18. ) Vertino, Kathleen. 2014. Effective interpersonal communication: a practical guide to improve your life. The Online Journal of Issues in Nursing 19. ) Wilks, Kristin. 2016. Civility and bullying.