DIZZINESS VERTIGO IMBALANCE DR AGBONIFO M CONSULTANT E

DIZZINESS, VERTIGO & IMBALANCE DR AGBONIFO M CONSULTANT E. N. T SURGEON ISTH, IRRUA. EDO STATE.

PRETEST ABOUT VERTIGO �IT IS ALSO REFFERED TO AS DIZZINESS �IT IS AN INNER EAR DISEASE �IT IS DEFINED AS HALLUCINATION OF MOVEMENT �A VERY IMPORTANT COMPONENT OF IT IS NYSTAGMUS
�BPPV: �MEANS BENIGH PAROXYSMAL POSITIONAL VERTIGO �IT IS THE COMMONEST CAUSE OF PERIPHERAL VERTIGO �IT IS ASSOCIATED WITH HEARING LOSS �TREATMENT IS SURGICAL

�DIX HALLPIKE TEST IS AN OFFICE PROCEDURE TO DIAGNOSE MENIERE’S DX �MEDICAL TREATMENT FOR VERTIGO INCLUDE THE USE OF BETAHISTINE �CAUSE OF PERIPHERAL VERTIGO INCLUDE MENIERE’S DX �CENTRAL VERTIGO COULD BE CAUSED BY C. V. A �SURGICAL TREATMENT IS THE FIRST LINE OF TREATMENT FOR BPPV �CAUSES OF VERTIGO IS VERTIGO

OUTLINE �INTRODUCTION �ANATOMY &PATHOPHYSIOLOGY (VESTIBULAR APPARATUS) �AETIOLOGY �CLINICAL FEATURES �INVESTIGATION �TREATMENT �REHABILITATION �CONCLUSION

INTRODUCTION �For the otolaryngologist the dizzy Pt often presents a diagnostic challenge, therefore the clinical evaluation has the following basic objectives: � It aims to present the basic knowledge and concept of symptom of dizziness �It presents the clinical approach to evaluating the dizzy patient. To differentiate different causes of dizziness, vertigo and imbalance �It explains the skills needed in primary care and secondary care settings of managing a dizzy patient �It aims to bring about positive attitudinal changes in the management of dizzy patients

Introduction cont… It is a common symptom especially with increasing age We have to distinguish between �VERTIGO and �NONVERTIGO �A critical distinction is differentiating vertigo from nonvertigo �Central and peripheral vertigo

Definitions �Vertigo is the true rotational movement of self or the surroundings. �Nonvertigo includes light-headedness, unsteadiness, motion intolerance, imbalance, floating, or a tilting sensation. �This dichotomy is helpful because true vertigo is often due to inner-ear disease, whereas symptoms of nonvertigo may be due to CNS, cardiovascular, or systemic diseases. �Nystagmus is involuntary rapid movt of the eyes.

Definitions cont �It can be horizontal (back & forth ; left & right), vertical (up & down) or rotatory. It has 2 phases ; slow & fast. The slow phase originates from the vestibular system and fast corrective phase from the brain.

ANATOMY/ PATHOPHYSIOLOGY 10 � MAITENANCE OF BALANCE RELIES UPON INPUTS FROM � VISUAL(70%) � VESTIBULAR(15%) � PROPRIOCEPTIVE(15%) � PATHOLOGY IN A WIDE VARIETY OF SYSTEMS MAY GIVE RISE TO DYSEQUILIBRIUM.

ANATOMY/PATHOPHYSIOLOGY CONT �Vestibular apparatus is made up of �Membranous and bony labyrinth embedded in petrous part of the temporal bone � 5 distinct end organs 3 semicircular canals: superior, lateral, posterior 2 otolith organs: utricle and saccule
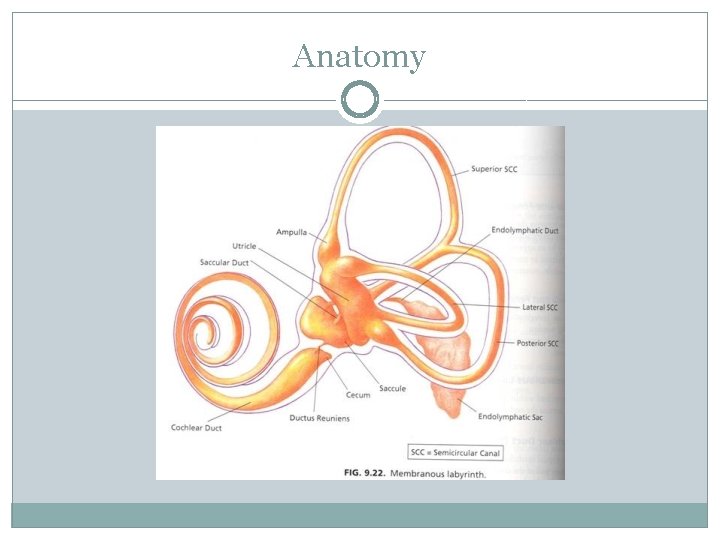
Anatomy
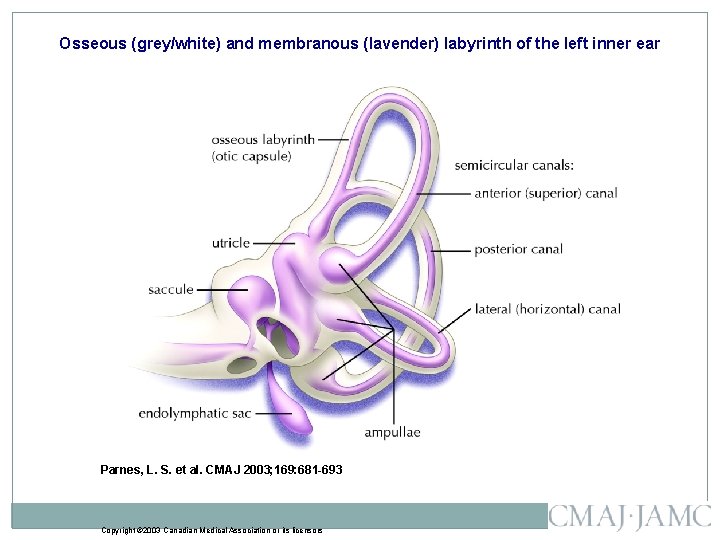
Osseous (grey/white) and membranous (lavender) labyrinth of the left inner ear Parnes, L. S. et al. CMAJ 2003; 169: 681 -693 Copyright © 2003 Canadian Medical Association or its licensors
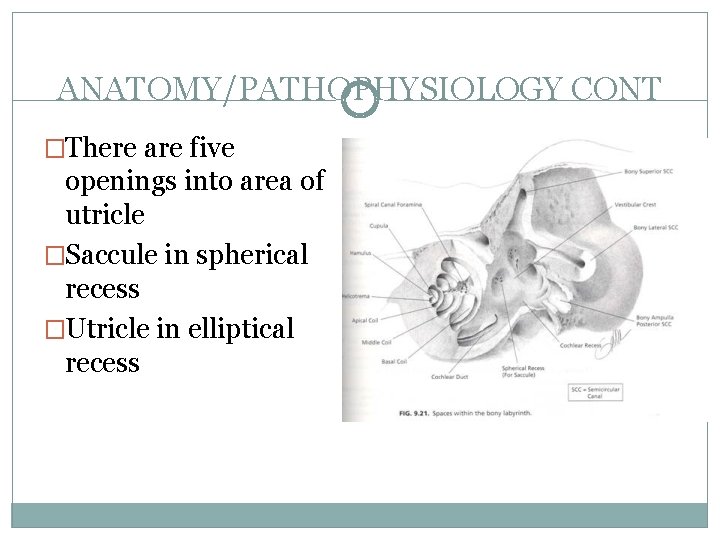
ANATOMY/PATHOPHYSIOLOGY CONT �There are five openings into area of utricle �Saccule in spherical recess �Utricle in elliptical recess
ANATOMY/PATHOPHYSIOLOGY CONT 15 �Vestibular labyrinth - detects linear and angular head movements �Semicircular canals - angular Hair cells organized under cupula �Otolithic organs (utricle, sacule) - linear Hair cells attached to a layer of otoconia �Vestibular nerve - superior, inferior branch �Afferent nerve fibers are bipolar - cell bodies lie within Scarpa’s ganglion

ANATOMY/PATHOPHYSIOLOGY CONT �Afferent fibers terminate in the vestibular nuclei in floor of fourth ventricle Superior vestibular nucleus Lateral vestibular nucleus Medial vestibular nucleus Descending vestibular nucleus

ANATOMY/PATHOPHYSIOLOGY CONT �Vestibular nuclei project to Cerebellum Extraocular Spinal nuclei cord Contralateral vestibular nuclei
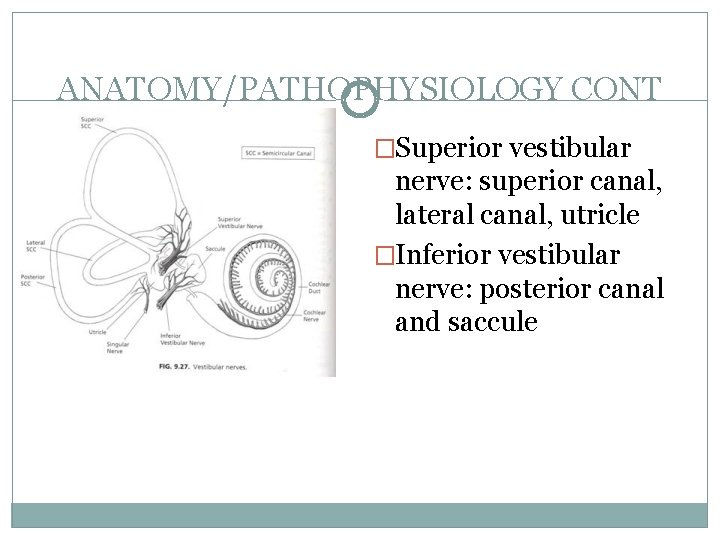
ANATOMY/PATHOPHYSIOLOGY CONT �Superior vestibular nerve: superior canal, lateral canal, utricle �Inferior vestibular nerve: posterior canal and saccule

Pathophysiology 19 �Balance requires – Normal functioning vestibular system Input from visual system (vestibulo-ocular) Input from proprioceptive system (vestibulo-spinal) �Central causes compromise central circuits that mediate vestibular influences on posture, gaze control, autonomic fx �Disruption of balance between inputs results in vertigo �Goal of treatment: restore balance between different inputs

Pathophysiology 20 �Vestibular system influences autonomic system �Intimate linkage in brainstem pathways between vestibular and visceral inputs �Alteration of vestibular inputs results in: nausea, vomiting Pallor Respiratory/circulatory changes

VERTIGO �CAUSES: �Vascular �Endocrine/Epilepsy �℞eceived (℞) �Trauma �Infection/Inflammatory �Growth (Tumour) �Others (Ophthalmologic, Miscellaneous)
CAUSES OF VERTIGO �VASCULAR Hypertension Orthostatic hypotension Subclavian steal syndrome Carotid-artery disease Vertebral-basilar artery insufficiency Arrhythmia Aortic stenosis Bradycardia

CAUSES OF VERTIGO � ENDOCRINE Diabetis mellitus Hypoglcaemia Thyromegaly Hyperthyroidism/Hypothyroidism Salt losing syndrome � EPILEPSY Temporal lobe epilepsy � HAEMATOLOGIC Anemia Polycythemia Leukemia

CAUSES OF VERTIGO � RECEIVED DRUGS Streptomycin Kanamycine Diazepam Sedatives Opiates Alcohol Neuroleptics Aspirin Nicotine Caffeine Prochlorperazine
CAUSES OF VERTIGO �TRAUMA Head injury Neck injury Fracture semicircular canal

CAUSES OF VERTIGO �INFECTIONS/INFLAMMATORY Influenza Herpes zoster oticus Measles Mumps Syphilis , neurosyphilis Encephalitis Meningitis �( see more under otologic causes)

CAUSES OF VERTIGO �GROWTHS (TUMOURS) Posterior fossa tumours Metastatic tumours to brain Acoustic neuroma (intracranial) Primary intracranial tumors �GLIAL Multiple sclerosis

CAUSES OF VERTIGO �OTHERS Heat stroke Temporomandibular joint syndrome Osteoarthritis Stroke Transient ischemic attacks �OTOLOGIC

CAUSES OF VERTIGO � OTOLOGIC Bening paroxysmal positional vertigo Vestibular neuronitis Acute serous otitis media Acute labyrinthitis Choleasteatoma Purulent otitis media Petrositis Poststapedectomy syndrome Perilymph fistula Meniere’s syndrome Acoustic neuroma (intracranial) Ototoxic drugs Auto-immune ear diseases

TYPES OF VERTIGO � Peripheral Vertigo: BPPV Vestibular neuronitis Ménière disease Auto-immune inner ear disease Labyrinthitis Acoustic neuroma syphilis � Central Vertigo: Migraine Cerebropontine angle tumours Multiple sclerosis Falls Cerebrovascular disease

CLINICAL FEATURES �HISTORY: �A patient who presents with dizziness should be questioned to distinguish true vertigo and nonvertigo. Ask patient to use other words other than dizziness in describing symptom �The rationale for using other words is that patients may use word dizzy nonspecifically to describe vertigo, unsteadiness, generalized weakness, syncope, presyncope, or falling.

Associated symptoms �Sudden onset and vivid memory of vertiginous episodes are often due to innerear disease, especially if hearing loss, ear pressure, or tinnitus is also present. �Gradual and ill-defined symptoms are most common in CNS, cardiac, and systemic diseases.

The time course of vertigo is also important. �Episodic true vertigo that lasts for seconds and is associated with head or body position changes is probably due to benign paroxysmal positional vertigo (BPPV). �Vertigo that lasts for hours or days is probably caused by Ménière disease or vestibular neuronitis. �Vertigo of sudden onset that lasts for minutes can be due to brain or vascular disease, especially if cerebrovascular risk factors are present.

The history should include �review of systems (especially head trauma and/or ear diseases) and screening for anxiety and/or depression. �History of prescription medicines, over-thecounter medications, herbal medicines, and recreational drugs (including smoking and alcohol) can help to identify pharmacologically induced syndromes.

Physical examination General examination should emphasize �vital signs, �supine and standing blood-pressure measurement, �evaluation of the cardiovascular and �neurologic systems.
Ear and Neck examinations �Examine the ears for visible external- and/or middle-ear infection and/or inflammation. �Test hearing by using a tuning fork or by whispering. �( Audiometric tests) �Examine the neck for range of motion.

Other Tests �Specific examination of the vestibular system, beyond the ears, nose, throat and neurologic examination, is fundamental to the evaluation of the patient with dizziness.

Clinical assessment of the Vestibular system �The Romberg and single leg standing tests �Assessment of gait with eyes open and closed �A search for past pointing �Evidence of spontaneous nystagmus �Evidence of positional nystagmus �The fistula tests

Office Examination of the Dizzy Patient �Dix-Hallpike Maneuver Used to provoke nystagmus and vertigo commonly associated with BPPV Head turned 45 degrees to maximally stimulate posterior semicircular canal Head supported and rapidly placed into head hanging position Frenzel glasses eliminate visual fixation suppression of response

Dix-Hallpike Maneuver

Dix-Hallpike Maneuver �Positive test Up-beating nystagmus Nystagmus to the stimulated side Rotary component to the affected ear Lasts 15 -45 seconds Latency of 2 -15 seconds Fatigues easily

Pneumatic Otoscopy �Positive and negative pressure applied to middle ear �Hennebert’s sign/symptom – nystagmus and vertigo with pressure, alternates with positive and negative pressure �Can be present in patients with perilymphatic fistula, syphilis, Meninere’s disease, SCC dehiscence syndrome
Dynamic Visual Acuity �Used for bilateral vestibular weakness �Visual acuity checked on Snellen chart �Rechecked while rotating head back and forth at 1 -2 Hz. �Loss of 2 -3 lines considered abnormal

Romberg Test �Patient asked to stand with feet together and eyes closed �Fall or step is positive test �Equal sway with eyes open and closed suggests proprioceptive or cerebellar site �More sway with eyes closed suggests vestibular weakness

Romberg Test

Dysdiadochokinesia Testing �Most commonly tested with the hand slapping test �Abnormalities seen in patients with cerebellar dysfunction �Poor sensitivity and specificity

Tandem Gait Test �Patients are asked to walk heal to toe in a straight line or in a circle �Complex function evaluates many aspects of balance �Poor performance seen in cerebellar lesions, but can be seen in many disorders �Poor sensitivity and specificity

Quantitative Vestibular Testing �Diagnosis unclear �Prolonged symptoms unresponsive to conservative treatment �Screen for central disorders �Evaluate prior to surgical ablation procedures �Documentation of vestibular deficits

Electronystagmography (ENG) �Divided into oculomotor tests, positional and positioning tests, and caloric tests �Only vestibular test with the ability to test individual labyrinths separately �Relies on the vestibulo-ocular reflex (VOR) to test the peripheral vestibular function �Mostly a test of HSCC function

Electronystagmography (ENG) �Oculomotor tests All test eye movements that originate in the cerebellum Saccadic tracking Smooth pursuit tracking Optokinetic testing

Oculomotor Tests �Saccadic tracking Patients concentrates on a randomly moving target Latency – difference in time between movement of object and eye (150 -250 ms) Velocity – speed of saccade 200 -400 degrees/second low end of normal Accuracy – amount of undershoot/overshoot of target (75 -120%)

Smooth Pursuit Test �Tests ability to accurately and smoothly pursue a target �Gain of eyes compared to movement of target �Saccade movements eliminated from calculations �Asymmetrical pursuit highly suggestive of central disorders

Optokinetic Tests �Vestibular system and optokinetic nystagmus allow steady focus on objects �Target is rapidly passed in front of subject in one direction, then the other �Eye movements are recorded and compared in each direction �Asymmetry suggestive of CNS lesion �High rate of false positive results

Caloric Testing �Established and widely accepted method of vestibular testing �Most sensitive test of unilateral vestibular weakness �Patient positioned 30 degrees from prone (HSCC vertical allowing max stim) �Cold and warm water/air flushed into EAC

Caloric Testing �COWS (cold opposite, warm same) – direction of the nystagmus �Stimulation in 0. 002 -0. 004 Hz range (Head movements in 1 -6 Hz range) �Visual fixation should reduce strength of caloric responses 50 -70% �% caloric paresis = 100 * [(LC + LW) – (RC + RW)/(LC + LW + RC + RW)]

Posturography �Used to tests integration of balance systems �Useful in quantification of fall risk �Most useful in following conditions: Chronic disequilibrium and normal exams Suspected malingering Suspected multifactorial disequilibrium Poorly compensated vestibular injuries

INVESTIGATIONS Audiogram is routinely needed Electronystagmography Caloric testing Radiological Investigation Blood examination Gadolinium-enhance MRI – pinpoints site of lesion. Dynamic posturography - quantifies balancing response to induced sways.

TREATMENT 58 � TREAT THE CAUSE IF KNOWN � MEDICAL � SURGICAL � PHYSICAL THERAPY

Medical Treatment 59 �Symptomatic �Specific therapy �Vestibular rehabilitation

Medical Treatment �Medications are most useful for treating acute vertigo that lasts a few hours to several days �They have limited benefit in patients with benign paroxysmal positional vertigo, because the vertiginous episodes usually last less than one minute. �Vertigo lasting more than a few days is suggestive of permanent vestibular injury (e. g. , stroke), and medications should be stopped to allow the brain to adapt to new vestibular input.

Categories of Drugs commonly used in treatment of dizziness �Antihistamines: eg meclizine, stugerone, • Betahistidine (serc) �Anticholinergics: e. g. Scopolamine (Isopto), glycopyrrolate (Robinul) �Phenothiazines : eg Promethazine, prochlorperazine �Benzodiazepines: eg diazepam (Valium) �Monoaminergics: eg ephedrine

Vestibular rehabilitation exercises �Semont manoeuvre �Particle repositioning manoeuvre (Epley) �Dix-Hallpike manoevre �Cawthorne exercises �Brandt-Daroff exercises (dispersing otolithic debris in the semicircular canals) �Lempert, and Hamid maneuvers, among others.
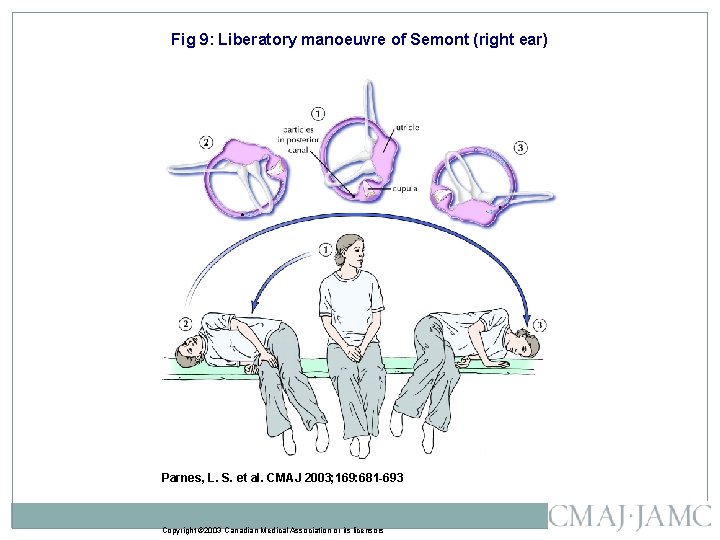
Fig 9: Liberatory manoeuvre of Semont (right ear) Parnes, L. S. et al. CMAJ 2003; 169: 681 -693 Copyright © 2003 Canadian Medical Association or its licensors

Fig. 9: Liberatory manoeuvre of Semont (right ear). �The top panel shows the effect of the manoeuvre on the labyrinth as viewed from the front and the induced movement of the canaliths (from blue to black). This manoeuvre relies on inertia, so that the transition from position 2 to 3 must be made very quickly. � Photo: Christine Kenney

Epley maneuver � The patient sits on the examination table, with eyes open and head turned 45 degrees to the right (A). � The physician supports the patient's head as the patient lies back quickly from a sitting to supine position, ending with the head hanging 20 degrees off the end of the examination table (B). � The physician turns the patient's head 90 degrees to the left side. The patient remains in this position for 30 seconds (C). � The physician turns the patient's head an additional 90 degrees to the left while the patient rotates his or her body 90 degrees in the same direction. The patient remains in this position for 30 seconds (D). � The patient sits up on the left side of the examination table. (E) � The procedure may be repeated on either side until the patient experiences relief of symptoms.
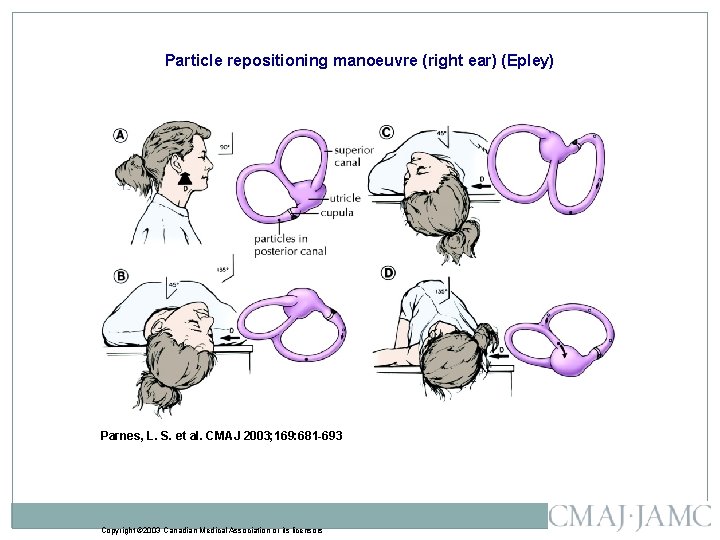
Particle repositioning manoeuvre (right ear) (Epley) Parnes, L. S. et al. CMAJ 2003; 169: 681 -693 Copyright © 2003 Canadian Medical Association or its licensors

Particle repositioning manoeuvre (right ear). � Schema of patient and concurrent movement of posterior/ superior semicircular canals and utricle. The patient is seated on a table as viewed from the right side (A). The remaining parts show the sequential head and body positions of a patient lying down as viewed from the top. Before moving the patient into position B, turn the head 45° to the side being treated (in this case it would be the right side). Patient in normal Dix–Hallpike head-hanging position (B). Particles gravitate in an ampullofugal direction and induce utriculofugal cupular displacement and subsequent counter-clockwise rotatory nystagmus. This position is maintained for 1– 2 minutes. The patient's head is then rotated toward the opposite side with the neck in full extension through position C and into position D in a steady motion by rolling the patient onto the opposite lateral side. The change from position B to D should take no longer than 3– 5 seconds. Particles continue gravitating in an ampullofugal direction through the common crus into the utricle. The patient's eyes are immediately observed for nystagmus. Position D is maintained for another 1– 2 minutes, and then the patient sits back up to position A. D = DIRECTION OF VIEW OF LABYRINTH, DARK CIRCLE = POSITION OF PARTICLE CONGLOMERATE, OPEN CIRCLE = PREVIOUS POSITION. ADAPTED FROM PARNES AND ROBICHAUD (Otolaryngol Head Neck Surg 1997; 116: 238 -43). 45 Photo: Christine Kenney

Surgical Care: �Surgery is usually reserved for those in whom CRP fails. It is not a first-line treatment because it is invasive and holds the possibility of complications such as hearing loss and facial nerve damage.

Surgical Care: �Options include labyrinthectomy, posterior canal occlusion, singular neurectomy, Vestibular nerve section, and transtympanic aminoglycoside application. �All have a high chance of vertigo control.

Conclusions 70 �Vestibular complaints common to ENT �Thorough evaluation and understanding �Dx and treat acute symptoms �Wean vestibular suppressants �Specific pharmacotherapy instituted �Chronic, uncompensated disease benefits from early VRT
- Slides: 70