Disseminated Intravascular Coagulation Presented by Ri Jan 29

Disseminated Intravascular Coagulation Presented by Ri 蕭雅澤 Jan. 29, 2007

What is DIC? • • • An acquired syndrome characterized by systemic intravascular coagulation Secondary to an underlying serious illness Alternative names: • Generalized intravascular coagulation • Defibrination syndrome • Consumption coagulopathy • Complications: thrombosis and bleeding, but bleeding is far more common
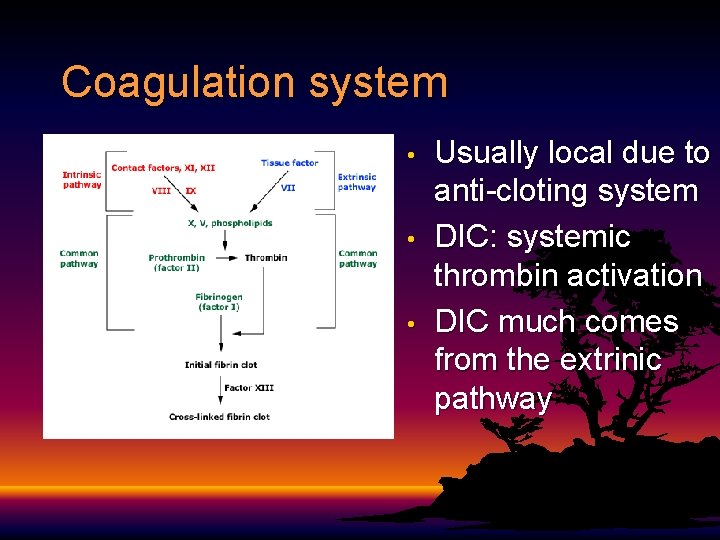
Coagulation system • • • Usually local due to anti-cloting system DIC: systemic thrombin activation DIC much comes from the extrinic pathway

Anti-cloting system • • Antithrombin III (AT-III) is most important since it could inactivate thrombin, XIIa, Xa, IXa and Kallekrein The action of AT-III is enhanced by heparin

Cause of DIC (1) • • Systemic inflammatory response, leading to activation of cytokine • Release or exposure of procoagulant material into the bloodstream • • Sepsis (any microorgansim) Trauma (polytrauma, neurotrama, fat embolism) Cancer (Both solid tumor and hema) Obst. problems Vascular abnormality

Cause of DIC (2) • Less common cause • • • severe hepatic failure Snake bites Transfusion reactions Transplant rejection Deficiency of protein C and protein S ※ Although the coagulation system is activated in pre-eclampsia and HELLP syndrome, DIC only occurs in a small percentage of these P’t

Complications of DIC • Acute DIC • PLT↓, clotting factors ↓, frbrinogen ↓ Bleeding into organs Microvascular thrombosis Digital ischemic, gangrene Renal cortical necrosis, adrenal infarction • Etiology: infection, trauma, obst. Problems, … • Subacute DIC • • • Venous thromboembolism (SVT, DVT, PE) Abnormal bleeding is uncommon Etiology: cancer Trousseau’s syndrome

Diagnosis of DIC • • S/S: (spontaneous) bleeding, ozzing at venipuncture site, digital ischemic, gangrene Lab • Decrease: PLT, PT, AT-III*, fibrinogen* (H=4 days) • Increase: FDPs, D-dimer* (most sensitive) • PB smear: fragmented RBC if microangiopathic hemolytic anemia present (about 25% of P’t) • Scoring system • ISTH scoring system (Taylor et al, 2000) • ISTH: International Society on Thrombosis and Haemostasis

Differential Diagnosis • • • Liver disease: fibrinogen(-), PLT(-, ↓) Vit. K deficiency: fibrinogen(-), PLT(-) Sepsis: fibrinogen(-) Thrombotic thrombocytopenic purpura: fibrinogen(-), PT/PTT(-) HELLP syndrome: fibrinogen(-)

Treatment • • • Treat underlying disease!!! No specific therapy is acquired if only lab abnormality with mild clinical S/S Replacement therapy alone If etiology is rapidly reversible (obstetric cases)

Treatment (1) • Cryoprecipitate • • Factor 8+13, v. WF, fibrinogen, fibronectin Aim: Plasma fibrinogen > 150 mg/d. L 1 U may increase fibrinogen 6 -8 mg/d. L FFP • Coagulation factor and fibrinogen • 1 U may increase cloting factors 4% and fibrinogen 6 -8 mg/d. L • • SFP: FFP without fibrinogen p. RBC, platelet conc.

Treatment (2) • Heparin therapy • Indication: (1) Acral cyanosis (2) Serious clinical sequence and the cause is not rapidly reversible • In other situation is controversial • Antithrombin III dependent, so must check before administration • Low dose: 500 -750 units per hour • Goal: Fibrinogen↑ and FDP↓, not PTT↑

Treatment (3) • Gabexate mesilate (Foy®) • • • Drotrecogin alfa (Xigris®) • • • Serine protease inhibitor Didn’t need antithrombin III Dosage: 1 -2 mg/kg/hr Clinical effect similar to heparin Recombinant human activated protein C Beneficial for DIC with sepsis EACA (with heparin) • Indication: excess fibrinolysis • Antithrombin III • Didn’t reduce the mortality rate


Thanks for your attention!!!
- Slides: 15