Disorders of the Stomach and Duodenum J B

Disorders of the Stomach and Duodenum J. B. Handler, M. D. Physician Assistant Program University of New England 1

Abbreviations n n n R/O- rule out ETOH- alcohol UGI- upper GI bid- twice daily qid- 4 x daily Dx- diagnosis Rx- treatment Sx- symptoms DDx- differential diagnosis Abd- abdomen ZE- Zollinger-Ellison n n PUD- peptic ulcer disease PPI- proton pump inhibitor H 2 - histamine 2 receptor EGD- esophago-gastroduodenoscopy COX- cyclooxygenase ARF- acute renal failure DU- duodenal ulcer GU- gastric ulcer CNS- central nervous system ETOH- alcohol 2

Case 1 n n n A 44 y/o man presents with several wk hx of mid -epigastric burning pain that improves with eating or antacids. No other medical problems. Meds: Ibuprofen 3 -4 x wk for HA’s. Smokes 1 ppd. ETOH: 1 -2 glasses of wine daily. PE- VS normal; Resp and CV examsunremarkable; Abd- Nl BS; no tenderness, masses or guarding. Rectal- no masses; stoolhemmocult neg. DDx? 3

Peptic Ulcer Disease n Definition: A break in the gastric or duodenal mucosa as a result of: n n Impaired normal mucosal defense factors (e. g. NSAIDS) Defensive factors overwhelmed by aggressive luminal factors (acid, pepsin, infection) >5 mm in diameter- extend through muscularis mucosa Location: duodenal bulb, pyloris, stomach 4
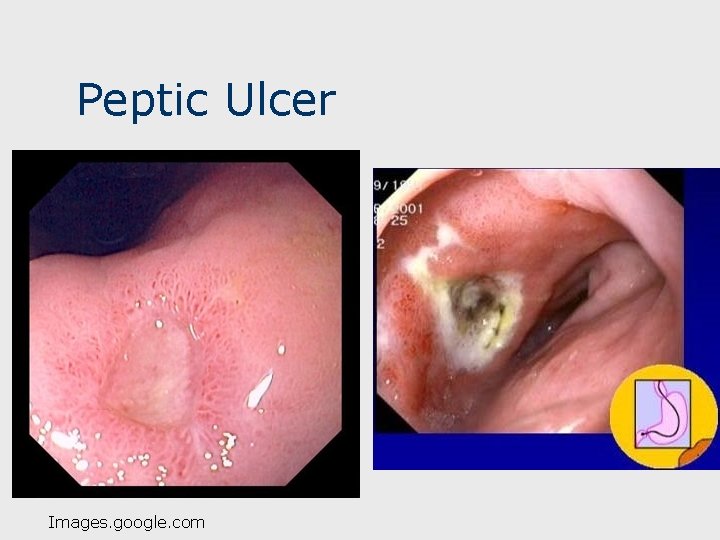
Peptic Ulcer Images. google. com

Epidemiology n n n 500, 000 new cases/year/USA. 10 -20% lifetime incidence in adults. Decreasing incidence since ’ 70’s: death rates, provider visits; need for surgery has decreased by 50%. n n Decrease correlates with H pylori infection/successful treatment and development of anti-secretory drugs. Duodenal ulcers 5 x more common than gastric: gastric antrum (60%), lesser curvature (25%); Benign vs malignant. 6

Case 1 DDx n Peptic ulcer disease associated with: n n Gastritis from: n n n H pylori NSAIDS Idiopathic NSAIDS Alcohol Stress (unlikely in absence of major medical problems) H pylori GERD 7

Ulcer Pathology n n NSAIDS: ulcers and/or gastritis-usually associated with long term use. Helicobacter pylori infection n n Duodenal and gastric ulcers Idiopathic- H pylori negative and not taking NSAIDs (5 -10% of all ulcers) Hypersecretory States (Z-E syndromesee below) Smoking is a risk factor for all ulcers. 8

Ulcer Pathology Hypotheses n n n DU: H pylori infection (gastric antrum) acid gastric metaplasia in duodenal bulb further H pylori infection duodenitis mucosal breakdown duodenal ulcer. GU: H pylori infection of stomach (body) gastritis with chronic inflammation overwhelms defenses mucosal breakdown gastric ulcer. NSAIDS impaired defenses mucosal breakdown gastric ulcer. 9

Helicobacter pylori n n n Necessary cofactor for majority (7590%) of duodenal/gastric ulcers; not associated with NSAID ulcers. A “hearty” bacteria: spiral, gram (–) rod Urease production Transmission: Unknown; likely oral-oral, fecal-oral, gastro-oral (via vomitus, NG/endo tube). Incidence correlates with socioeconomic status; 25 -30% adults in US, varies with age. 10

Helicobacter pylori n n May be associated with acute infectious syndrome: “gastroenteritis”, nausea, abd pain. Chronic local infection: diffuse superficial mucosal inflammation with polys, lymphocytes; majority of patients asymptomatic (see H pylori gastritis below). n n 15% of infected individuals develop PUD. Eradication crucial to prevent ulcer recurrence (85% recurrence if not). 11

Signs and Symptoms: PUD n n n Epigastric pain common (80 -90% pts with PUD); burning, gnawing, aching, “hungerlike”. Not sensitive/specific enough to serve alone as a reliable diagnostic marker of PUD. Pain relief with eating (50%), antacids, with subsequent return in 2 -4 hrs. Nocturnal awakening with pain common. 12

Signs and Symptoms Caution: change in patternpenetration or perforation. n Gastric ulcers: nausea/anorexia may be associated symptoms. n Physical Exam more often unremarkable; rectal for occult blood is important. n 13

Case 1 Based on the history and PE, you decide that his presentation is most consistent with PUD although gastritis remains a possibility. n Which diagnostic tests are indicated to further sort this out? n 14

Investigative Findings: PUD n n n Hgb/Hct for anemia; +/-amylase. Endoscopy- EGD- best diagnostic tool: visualize ulcer, biopsy (GU); can test for H pylori via histology and/or rapid urease biopsy testing if not yet done noninvasively (below). Imaging: Barium UGI: screening tool for dyspepsia; helpful but limited- cannot identify malignant vs benign gastric ulcers; may be unable to identify some ulcers. 15
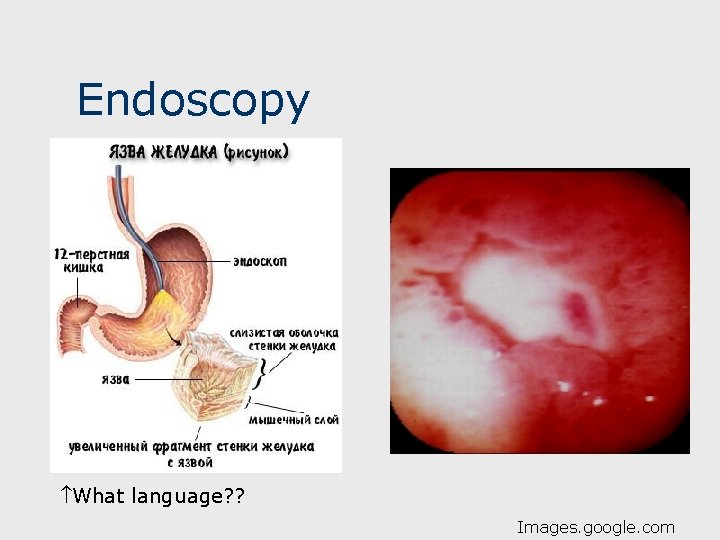
Endoscopy What language? ? Images. google. com

Non-Invasive H pylori Testing *Fecal antigen test- indicates active infection, >90% S/S. n *13 C-urea breath test- indicates active infection, >90% S/S. n Serologic blood tests no longer recommended- lack S/S. n *Tests of choice for active PUD, recurrent PUD, proof of eradication Must D/C PPI 7 -14 days before test or can have false (-) 17

Gastric vs Duodenal Ulcer n n Major difference is gastric ulcers may be malignant (3 -5% incidence). Essential to biopsy at time of endoscopy. Gastric ulcers often take longer to heal than duodenal ulcers, require length of Rx. Non-healing (ongoing or recurrent Sx) GU warrants repeat endoscopy and biopsy for malignancy. 18

Case 1 His EGD reveals an oval shaped (2. 5 x 3 cm) duodenal ulcer without evidence of bleeding. n H pylori breath test is positive. n How should this man be managed? n Is there any indication to repeat the above tests following treatment? n 19

PUD Treatment Acid-antisecretory agents n H pylori eradication n Enhanced mucosal defense agents n What happens if H pylori not eradicated? n 20

Acid-Antisecretory Agents n n n Proton Pump Inhibitors (PPI): inactivate the H+ K+ ATPase or “proton pump” in stomach. Short T 1/2 but 24 hr pump inactivation allows 1 -2 x daily Rx (see below); mostly oral agents; inhibit >90% acid secretion. >90% of duodenal ulcers heal in 4 wks >90 of gastric ulcers heal in 8 weeks 21

Acid-Antisecretory Agents n n Safe, low side effect profile; minor GI, CNS side effects. Omeprazole (Prilosec), lansoprazole (Protonix), others. n n n Esomeprazole & pantoprazole available IV 2 x daily dosing while eradicating H pylori, then once daily (e. g. Omeprazole 20 mg). Ulcers likely to recur unless H pylori eradicated. 22

Acid-Antisecretory Agents H 2 receptor antagonists: inhibit histamine mediated gastric acid secretion. n Suppress nocturnal> waking/post meal acid secretion. n Less effective than PPI, but most ulcers heal (85 -90% efficacy) over 6 -8 weeks. n 23

Acid-Antisecretory Agents Ranitidine (Zantac), famotidine (Pepcid), others, all over-the counter. n Safe, usually taken as single large oral dose in the PM (e. g. ranitidine 300 mg) n Available in IV forms (see belowstress gastritis). n 24

Mucosal Defense Agents n n n These are 2 nd line or adjunct therapy for Rx of PUD. Antisecretory agents are drugs of choice. Antacids- buffer acid; rapid symptom relief; useful for supplemental Rx. Sucralfate- (Carafate)- adheres to ulcer craters and protects cells from acid and pepsin; allows healing- 2 nd line to PPI or H 2 -blockers. 25

Mucosal Defense Agents n n Bismuth- anti-bacterial vs H pylori; enhances mucosal defenses. Misoprostol (Cytotec)- for prophylaxis vs. NSAID induced ulcer or gastritis; prostaglandin analog, stimulates gastroduodenal mucus and HCO 3 secretion; side effect is diarrhea. Infrequently used. n Preferred Rx for prophylaxis is a PPI (see below). 26

H pylori Eradication n n Difficult to eradicate; requires “triple” therapy- 2 antibiotics plus PPI bismuth. 10 -14 day course: n n n PPI 2 x daily Clarithromycin* 500 mg 2 x daily Amoxicillin 1 gram 2 x daily Alternative antibiotics include metronidazole*, tetracycline. *Resistant strains common. See CMDT for other regimens 27

Ulcer Treatment H pylori assoc ulcers: goal is symptoms, promote healing, eradicate H pylori. n Antibiotic regimen + PPI (2 x/d) for 10 -14 days. n PPI continued 1 x/d: Duodenal ulcer- additional 2 -4 wks Gastric ulcer– additional 4 -6 wks n 28

Ulcer Treatment n n n H 2 blockers as alternative if cost a concern; may require longer treatment. Most will heal; key to preventing recurrence is eradication of H pylori (>85% success rate). Proof of H pylori eradication not needed unless: ulcer complication, recurrent or refractory ulcers. 29

Ulcer Recurrence n For recurrent ulcers: essential to R/O ongoing H pylori infection and/or NSAID use. n n NSAID use can promote recurrence. <20% incidence if H pylori eradicated. Once gone, H pylori reinfection rates are very low (<. 5%/year). Multiple recurrences suggest alternative pathology, i. e hypersecretory states. 30

NSAID Ulcers n n n Selective Cox-2 vs. non-selective (N-S) NSAIDs. Long term use of N-S NSAIDS can cause both gastritis and ulcers; inhibit gastric COX-1, prostaglandin synthesis impair gastric mucus/HCO 3 secretion and other protective mechanisms. NSAID anti-inflammatory effects via inhibition of COX-2. Selective COX-2 agents (Celecoxib) risk of ulcers/gastritis, but associated with risk of coronary events in susceptible patients (see below). 31

NSAID Ulcers n Complications: bleeding & perforation occur in 1 -2% patients with NSAID ulcers. n n n Risk factors for complications: hx PUD or complications; corticosteroids; anticoagulants; age> 60; also on ASA; underlying medical illness. Treatment once present: PPI or H 2 blocker 4 -8 wks, plus D/C NSAID; rapid vs delayed healing if NSAID continued. H pylori not a cofactor but often presentmust eradicate if present. 32

Prevention/Prophylaxis n n Reserved for high risk patients prevent ulcer complications (see above). PPI prophylaxis (omeprazole 20 mgs daily) while taking NSAID. n n Alternative is Misoprostol (see above). COX-2 NSAIDS as alternative to nonselective NSAID cardiac events/MI in patients with underlying CHD. n If dose of celecoxib is low ( 200 mg/d) and duration short (<3 mos. ), there is very low risk. 33

Refractory Ulcers n n n Uncommon; non-compliance is major cause. Cigarettes retard healing. NSAIDS (including low dose ASA). Failure to eradicate H pylori. Malignancy (non-healing gastric ulcer). 34

Ulcer Complications Bleeding n Penetration/Perforation n Gastric outlet obstruction n 35

Bleeding Ulcers Common; seen in 10 -20% patients with active PUD; 6 -10% mortality; 50% of UGI bleeding is from ulcers. n May be first sign/symptom vs antecedant ulcer symptoms. n Hematemesis and/or melena vs hematochezia dependent on amount. n 36
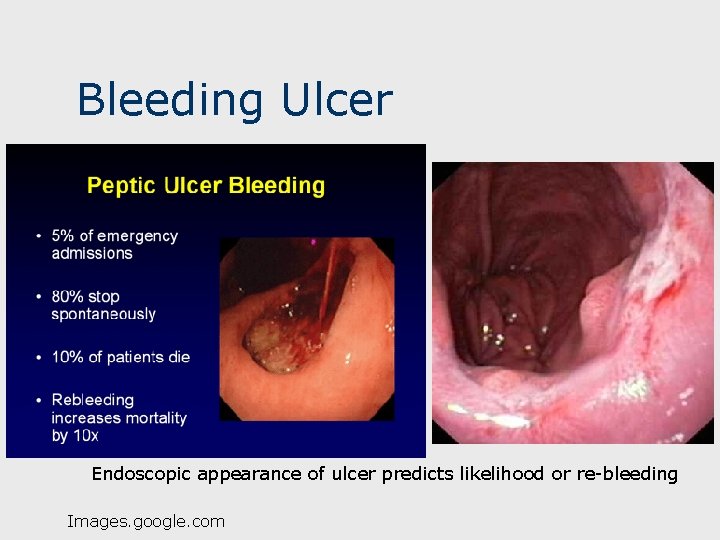
Bleeding Ulcer Endoscopic appearance of ulcer predicts likelihood or re-bleeding Images. google. com

Bleeding Ulcers n n n Gastric lavage/emesis: BRB vs “coffee grounds”. PE: vital signs, postural changes, palor etc. dependent on amount of blood loss. Lab: decrease Hgb, Hct (will drop further with volume expansion); check PTT, INR and platelets; BUN may be increased from digested blood. 38

Treatment: Bleeding Ulcer n n Volume expansion (isotonic fluids); transfuse when needed. Bleeding stops spontaneously in 80%. Endoscopy identifies site, stability of bleeding site; also used to stop bleeding when necessary (theromocoag, vasoconstricters, clips/staples, etc. ). IV PPI or high dose oral PPI- decrease rebleeding, need for transfusion or repeat interventions, including surgery. 39

Treatment: Bleeding Ulcer H pylori eradication if present (most) essential in preventing rebleeding. n Surgery for re-bleeding/refractory bleeding in selected patients. n 40

Ulcer Perforation n n 5% incidence in ulcer patients. Anterior wall of stomach or duodenum. Results in chemical peritonitis- severe, generalized abdominal pain, rigid abd, rebound, WBC, free air on KUB/upright. Laparoscopic perforation closure carries morbidity compared to laparotomy with vagotomy, antrectomy. Intensive medical Rx also required. 41

Other Complications (IO) n n Ulcer Penetration of posterior wall of stomach/duodenum into pancreas, liver or biliary tract. Symptoms: increase in pain, radiates to back, unresponsive to antacids and other meds; amylase may be elevated. Rx is intensive PPI regimen or IV H 2 blocker. IO- interest only 42

Erosive & Hemorrhagic Gastritis n n Etiologies: ETOH, NSAIDS; stress from underlying severe medical/surgical disease (common in ICU patients). Symptoms: Often asymptomatic; anorexia, N&V, “dyspepsia”; initial presentation may be GI bleeding. n n UGI bleeding: hematemesis, “coffee ground” emesis, melena as above; usually self-limited. Dx often requires endoscopy: DDx: bleeding peptic ulcer, esophageal varices, mallory-weiss tear. 43
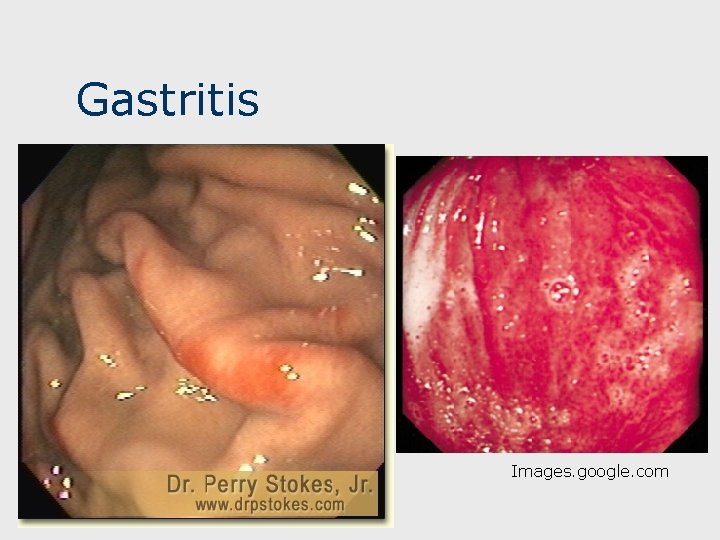
Gastritis Images. google. com

Stress Gastritis/Ulcers n n n Superficial erosions common and develop quickly in critically ill/ICU patients; bleeding in up to 6% with associated mortality. Pathophys: gastric mucosal blood flow. Risk factors for bleeding: trauma, burns, sepsis, shock, hypotension, respiratory failure/mechanical ventilation, coagulation problem, ARF, CNS injury. 45

Prophylaxis: High Risk Patient n IV H 2 blockers bleeding incidence by 50% or more in high risk patients. n n n PPI- Oral/NG* (omeprazole suspension) or IV (expensive) may be better than H 2 blocker, but controlled comparison trials are lacking. Goal: gastric p. H>4 Sucralfate not as effective: alternative if patient intolerant to antisecretory agents. Improve hemodynamics where possible. Enteral feedings when indicated; risk of bleeding. *NG- nasogastric or nasoenteric tube 46

NSAID Gastritis n n Very common in patients on chronic NSAIDs; most unrecognized because no Sx. Dyspepsia in 25% of patients with NSAID gastritis. If on NSAIDS with Sx, empiric Rx is reasonable: D/C NSAID; PPI for 2 wks. Persistent or worsening symptoms endoscopy (EGD) PPI 2 -4 wks. 47

Alcohol Gastritis n n n Excessive ETOH intake nausea, dyspepsia, emesis, hematemesis (usually minor UGI bleeding. ) Responds to H 2 receptor blocker, PPI or sucralfate therapy- 4 week course. DDX of UGI bleeding in alcoholics includes PUD and esophageal varices from portal hypertension more significant bleeding. 48

H pylori Gastritis n n Non-erosive, non-specific picture. Usually asymptomatic; unlikely cause of dyspepsia. Co-factor for PUD Associations: 1. Gastric adenocarcinoma 2. B-cell gastric lymphoma (mucosa associated lymphoid tissue lymphoma or MALToma). 49

Zollinger-Ellison Syndrome n n n Hypersecretory state from a gastrin secreting tumor (gastrinoma). Tumor found in pancreas, duodenum, lymph nodes; 2/3 malignant, metastasize to liver; slow growth. Excess acid secretion leads to recurrent or refractory duodenal ulcers. n n Associated Sx: GERD, diarrhea. Can lead to malabsorbtion, weight loss. 50

Zollinger-Ellison Syndrome n n Testing: Increased serum gastrin (often >500 pg/ml) levels (nl< 100 pg/ml), + document gastric p. H <3 (to r/o hypochlorhydria which can also raise gastrin levels) Special imaging required to find primary tumor and/or metastasis: somatostatin receptor scintigraphy endoscopic ultrasonography 51

Treatment of Z-E If isolated primary tumor: PPI + resection. n If metastasis: PPI in high dose to decrease basal acid output. n Prognosis: good for isolated tumor. n 52
- Slides: 52