Disorders of the Pancreas Nrsg 407 PANCREAS Exocrine





















- Slides: 47

Disorders of the Pancreas Nrsg 407

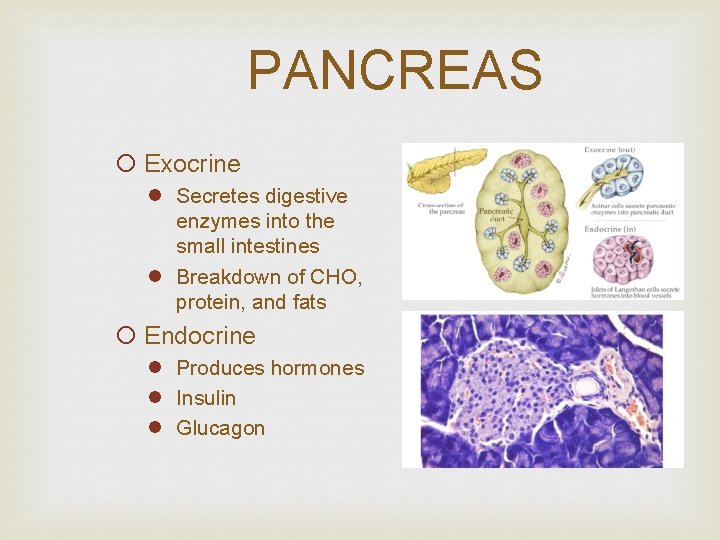
PANCREAS ¡ Exocrine l Secretes digestive enzymes into the small intestines l Breakdown of CHO, protein, and fats ¡ Endocrine l Produces hormones l Insulin l Glucagon

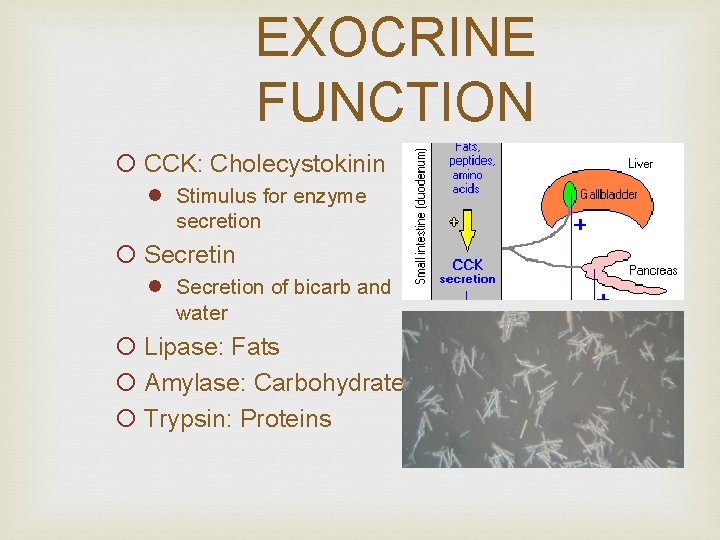
EXOCRINE FUNCTION ¡ CCK: Cholecystokinin l Stimulus for enzyme secretion ¡ Secretin l Secretion of bicarb and water ¡ Lipase: Fats ¡ Amylase: Carbohydrates ¡ Trypsin: Proteins

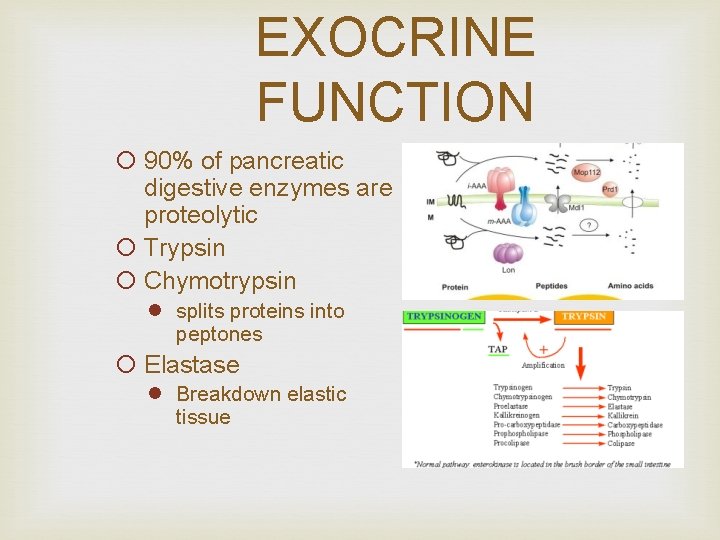
EXOCRINE FUNCTION ¡ 90% of pancreatic digestive enzymes are proteolytic ¡ Trypsin ¡ Chymotrypsin l splits proteins into peptones ¡ Elastase l Breakdown elastic tissue

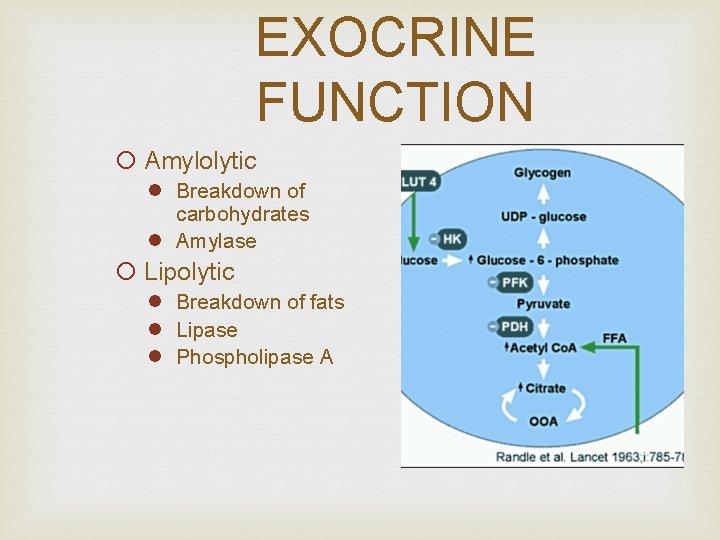
EXOCRINE FUNCTION ¡ Amylolytic l Breakdown of carbohydrates l Amylase ¡ Lipolytic l Breakdown of fats l Lipase l Phospholipase A

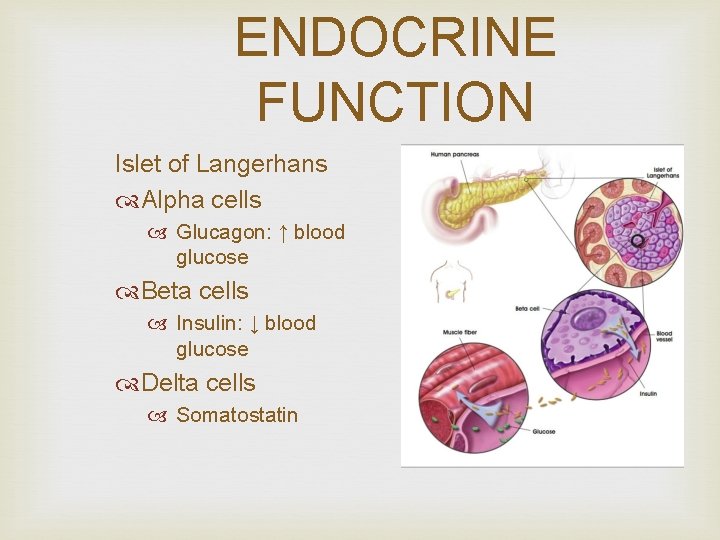
ENDOCRINE FUNCTION Islet of Langerhans Alpha cells Glucagon: ↑ blood glucose Beta cells Insulin: ↓ blood glucose Delta cells Somatostatin

PANCREATITIS ¡ Inflammation of the pancreas ¡ Autodigestion of the pancreas by pancreatic enzymes ¡ Cellular destruction and organ damage

ACUTE PANCREATITS ¡ Acute l Mild or Nonhemorrhagic l Severe or Hemorrhagic l Fulminant

EPIDEMIOLOGY 185, 000 cases each year 150, 000 cholelithiasis or sustained alcohol abuse African-Americans are at ↑ risk

CAUSES ¡ Alcohol consumption ¡ Gallstones ¡ Pancreatic obstruction ¡ Drugs and toxins ¡ Hyperlipidemia ¡ Family history ¡ Trauma and iatrogenic factors

SIGNS and SYMPTOMS ¡ Severe abdominal pain l Epigastrium radiating to midback l Not relieved by vomiting ¡ Fever, malaise ¡ Nausea, vomiting ¡ Rigid and distended ¡ Rebound tenderness ¡ Absent or diminished bowel sounds

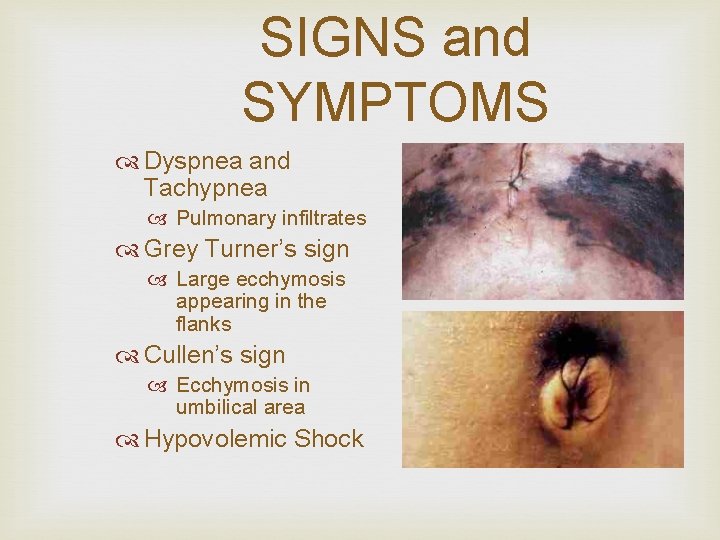
SIGNS and SYMPTOMS Dyspnea and Tachypnea Pulmonary infiltrates Grey Turner’s sign Large ecchymosis appearing in the flanks Cullen’s sign Ecchymosis in umbilical area Hypovolemic Shock

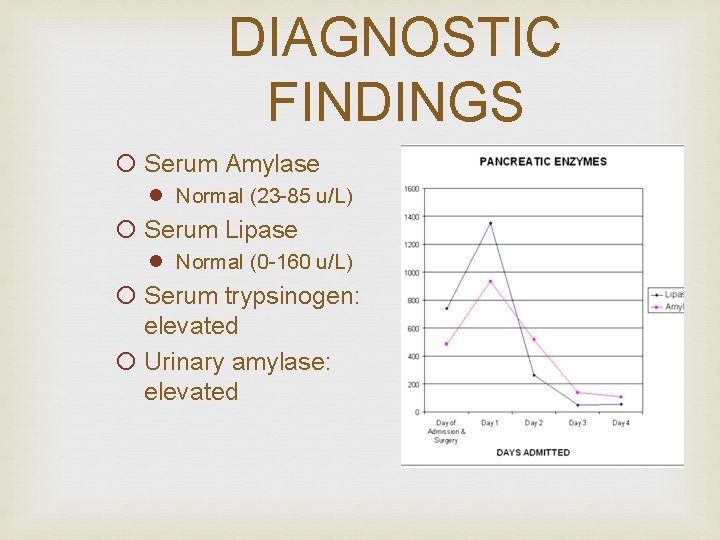
DIAGNOSTIC FINDINGS ¡ Serum Amylase l Normal (23 -85 u/L) ¡ Serum Lipase l Normal (0 -160 u/L) ¡ Serum trypsinogen: elevated ¡ Urinary amylase: elevated

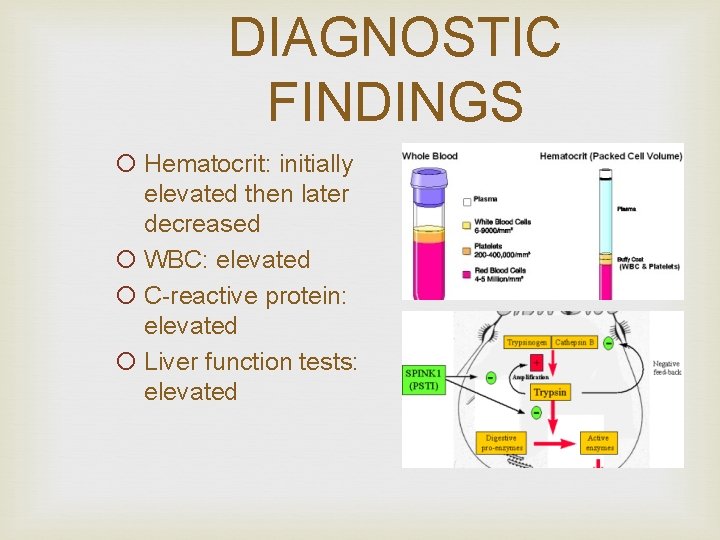
DIAGNOSTIC FINDINGS ¡ Hematocrit: initially elevated then later decreased ¡ WBC: elevated ¡ C-reactive protein: elevated ¡ Liver function tests: elevated

DIAGNOSTIC FINDINGS ¡ Sodium and Potassium: decreased ¡ Blood glucose: elevated ¡ Serum Calcium: decreased ¡ Albumin and Magnesium: decreased

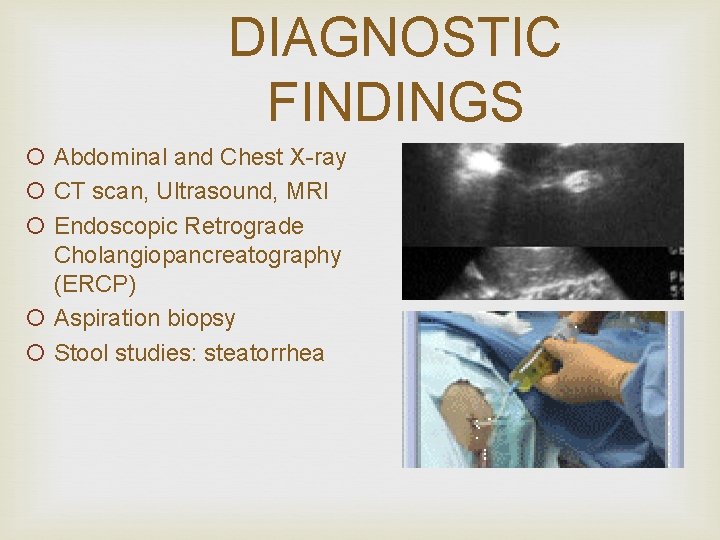
DIAGNOSTIC FINDINGS ¡ Abdominal and Chest X-ray ¡ CT scan, Ultrasound, MRI ¡ Endoscopic Retrograde Cholangiopancreatography (ERCP) ¡ Aspiration biopsy ¡ Stool studies: steatorrhea

COMPLICATIONS ¡ Hypovolemic shock l l 3 rd spacing Hemorrhage Vomiting Decreased protein intake

COMPLICATIONS ¡ Pulmonary complications l l Atelectasis Acute lung injury Pleural effusion ARDS

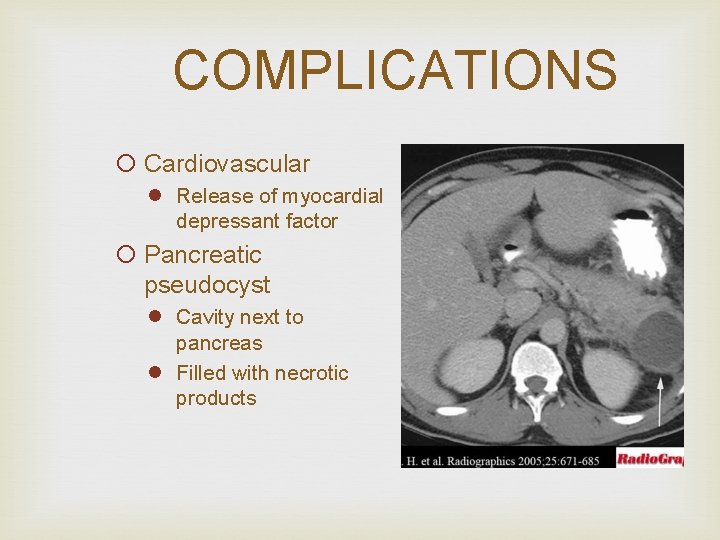
COMPLICATIONS ¡ Cardiovascular l Release of myocardial depressant factor ¡ Pancreatic pseudocyst l Cavity next to pancreas l Filled with necrotic products

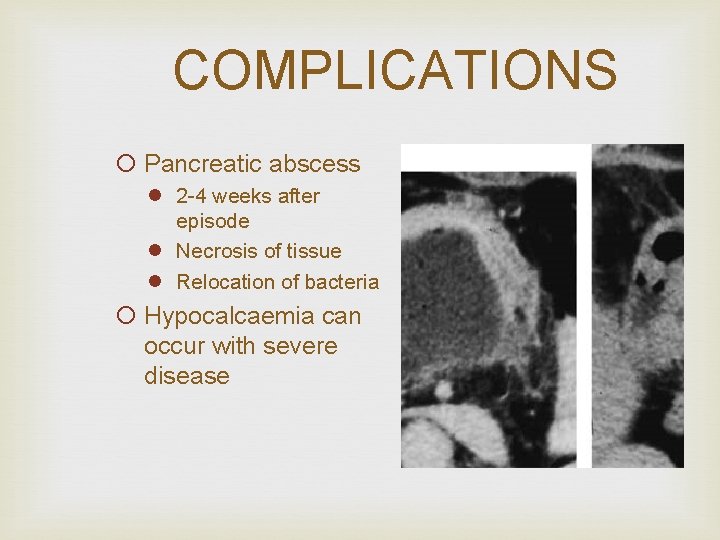
COMPLICATIONS ¡ Pancreatic abscess l 2 -4 weeks after episode l Necrosis of tissue l Relocation of bacteria ¡ Hypocalcaemia can occur with severe disease

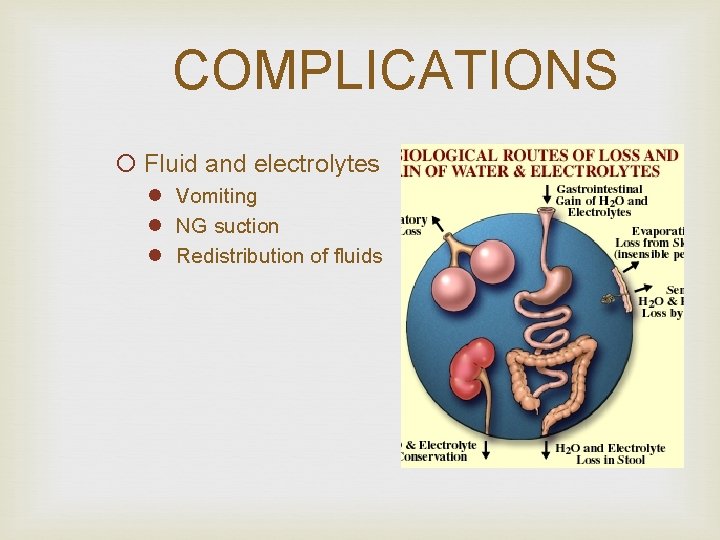
COMPLICATIONS ¡ Fluid and electrolytes l Vomiting l NG suction l Redistribution of fluids

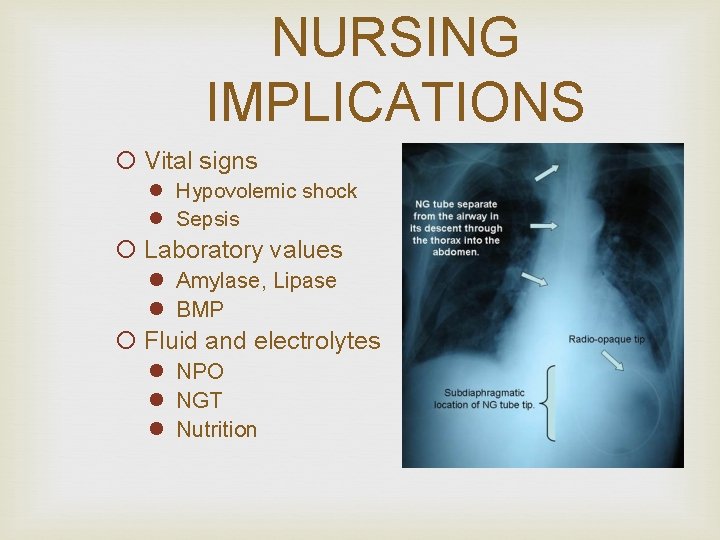
NURSING IMPLICATIONS ¡ Vital signs l Hypovolemic shock l Sepsis ¡ Laboratory values l Amylase, Lipase l BMP ¡ Fluid and electrolytes l NPO l NGT l Nutrition

NURSING IMPLICATIONS ¡ Administer pain medication ¡ Monitor blood glucose ¡ Monitor intake and output ¡ Daily weight

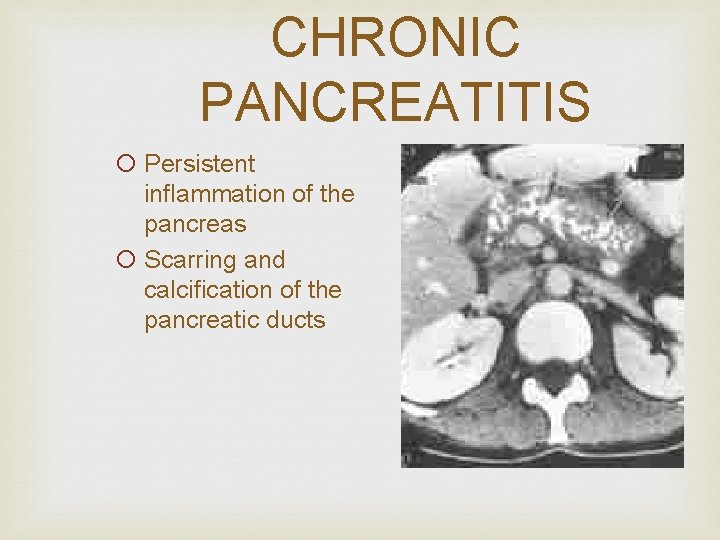
CHRONIC PANCREATITIS ¡ Persistent inflammation of the pancreas ¡ Scarring and calcification of the pancreatic ducts

CAUSES ¡ 70% is caused by alcohol abuse ¡ 20% is caused by obstruction, trauma, metabolic disturbances

SIGNS & SYMPTOMS ¡ 80% of pancreatic destruction causes l Malabsorption resulting in nutritional deficits l Diarrhea and steatorrhea l Impaired glucose regulation

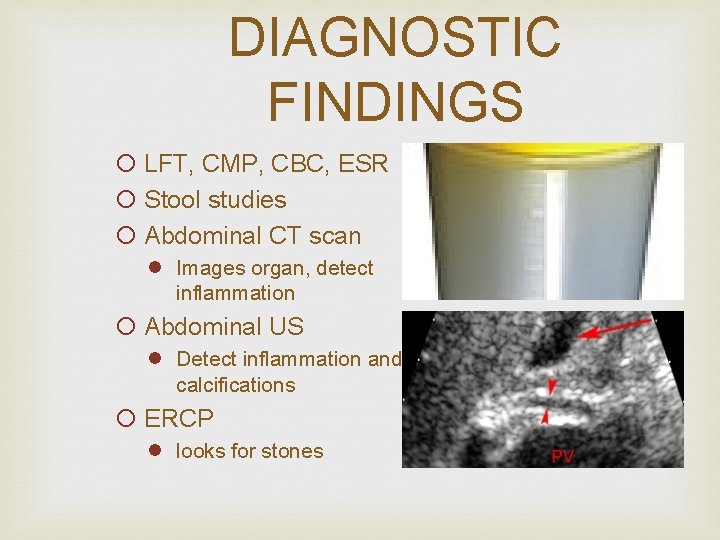
DIAGNOSTIC FINDINGS ¡ LFT, CMP, CBC, ESR ¡ Stool studies ¡ Abdominal CT scan l Images organ, detect inflammation ¡ Abdominal US l Detect inflammation and calcifications ¡ ERCP l looks for stones

Pancreas Islets of Langerhans Glucagon – alpha cells Insulin – beta cells Hormones secreted directly into blood capillaries Readily available for use

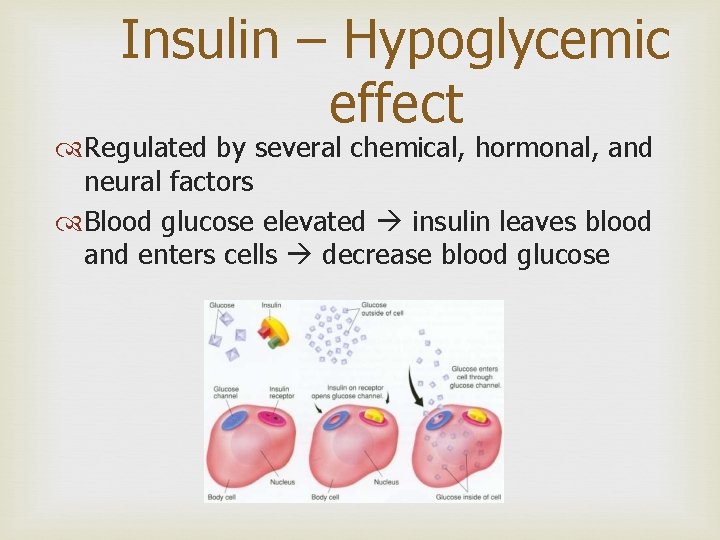
Insulin – Hypoglycemic effect Regulated by several chemical, hormonal, and neural factors Blood glucose elevated insulin leaves blood and enters cells decrease blood glucose

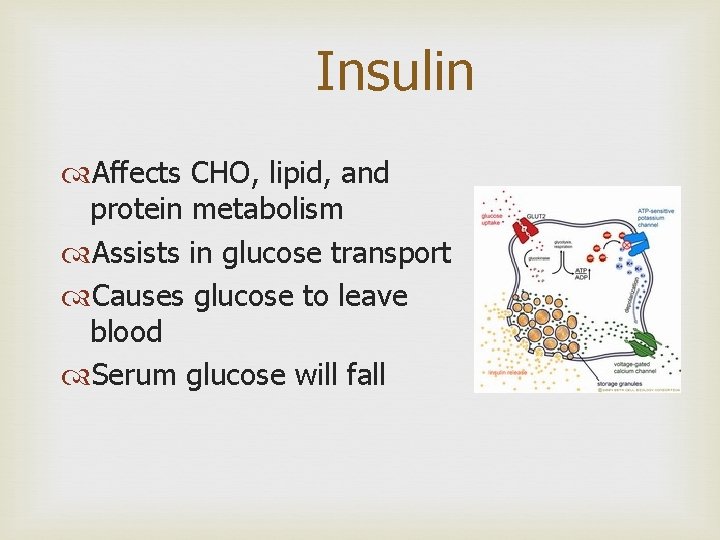
Insulin Affects CHO, lipid, and protein metabolism Assists in glucose transport Causes glucose to leave blood Serum glucose will fall

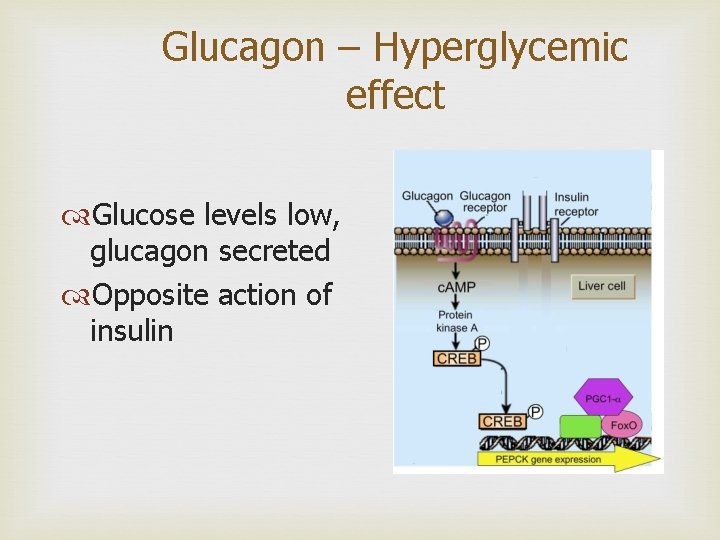
Glucagon – Hyperglycemic effect Glucose levels low, glucagon secreted Opposite action of insulin

DIABETES Disorder of insulin action or secretion (usually both) Results in high blood glucose Two different types of diabetes: Type I Autoimmune disorder Type II Multifactorial disease

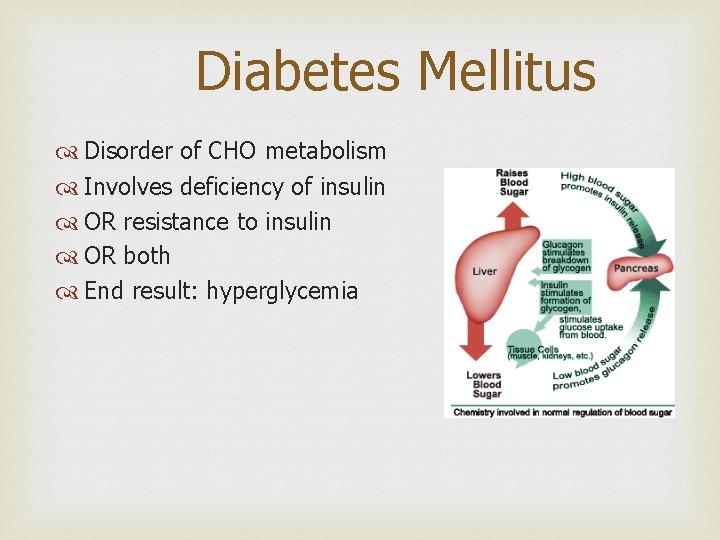
Diabetes Mellitus Disorder of CHO metabolism Involves deficiency of insulin OR resistance to insulin OR both End result: hyperglycemia

Diabetes Mellitus Related to destruction of beta cells in pancreas Insulin can neither be produced or secreted Can also have insulin receptor defects Will need mandatory dietary modifications

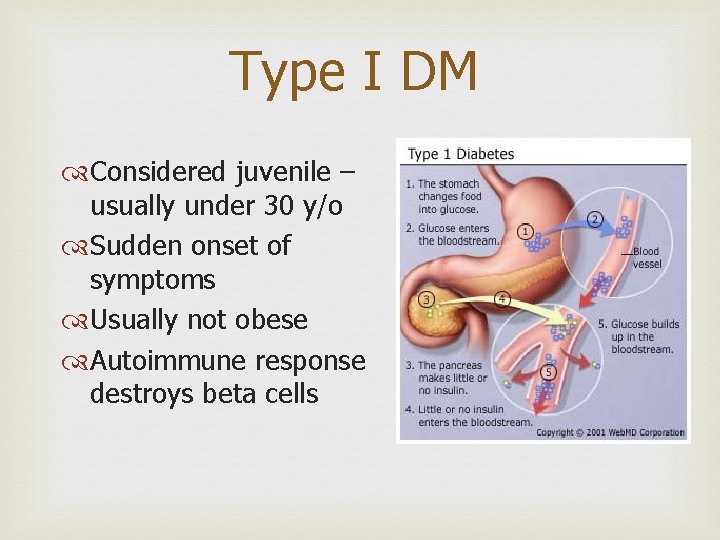
Type I DM Considered juvenile – usually under 30 y/o Sudden onset of symptoms Usually not obese Autoimmune response destroys beta cells

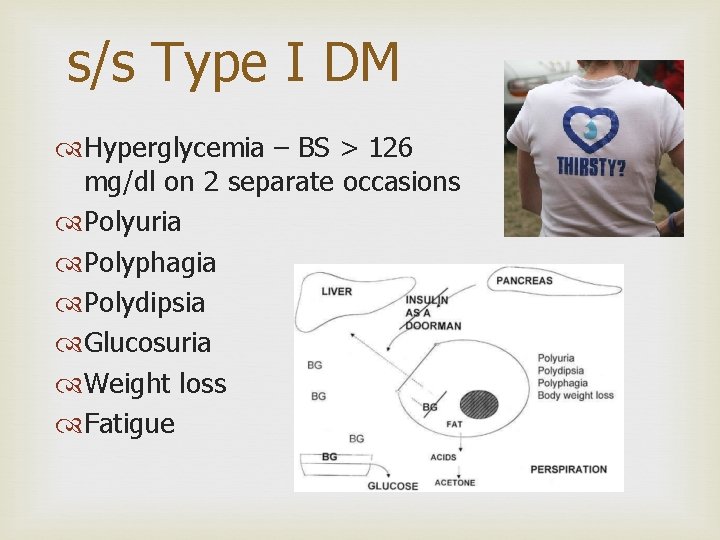
s/s Type I DM Hyperglycemia – BS > 126 mg/dl on 2 separate occasions Polyuria Polyphagia Polydipsia Glucosuria Weight loss Fatigue

Type I DM – Insulin dependent Usually not insulin resistant Normal insulin receptors Decreased plasma insulin Most common complication – Diabetic ketoacidosis (DKA) [blood sugars >600 mg/dl

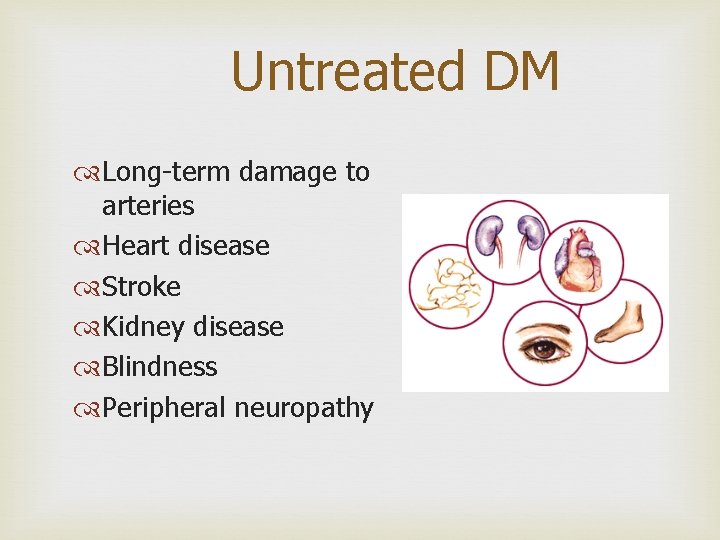
Untreated DM Long-term damage to arteries Heart disease Stroke Kidney disease Blindness Peripheral neuropathy

Diagnosis Classic symptoms: Increased urination, increased thirst, and unexplained weight loss plus random blood glucose ≥ 200 mg/d. L OR Fasting (8 hours+) ≥ 126 mg/d. L OR Blood glucose ≥ 200 mg/d. L two hours after a standard carbohydrate load Oral Glucose tolerance (OGTT) Any glucose ≥ 200 mg/d. L Exception: someone receiving IV infusion of glucose

Type I Autoimmune destruction of beta cells causes a decrease in or absence of insulin production by islets of Langerhans Islets are infiltrated by T lymphocytes Has genetic component Environmental factors also play a role

Type II Mixture of genetic and environmental factors Obesity is the underlying cause of most type II diabetes Also lifestyle factors play an important role Is characterized by: Decreased sensitivity of peripheral cells to the effect of insulin (insulin resistance) Beta-cell dysfunction that prevents adequate insulin response to decreased peripheral cell sensitivity and high blood glucose

Secondary Type II Due to causes other than obesity Pregnancy Drug therapy (steroids, Cushing disease) Diabetes usually will disappear when underlying condition is corrected

Diabetic Complications Excessive glucose binds to extracellular proteins to form abnormal glycoproteins that negatively impact vascular endothelium Increases inflammation Promotes thrombosis Loosens endothelial cells Stimulates proliferation of vascular smooth muscle cells (atherosclerosis) Promotes vascular disease

Complications cont’d High intracellular glucose results in increased oxidative stress (diabetic neuropathy) Also stimulates production of mediators that: Stimulate growth of new blood vessels (diabetic retinal disease) Promote thrombosis Promotes vascular inflammation Promotes vasoconstriction

Diabetic Ketoacidosis Acidosis occurs due to absence of insulin because in the absence of glucose, body must burn fat for fuel Fat is broken down into fatty acids-transported to liver and converted into ketones to be burned for fuel Lowers blood p. H Present mainly with Type I diabetes

Long-Term Complications of DM Usually seen 15 -20 years after onset of hyperglycemia Infections: due to impaired neutrophil & macrophage function and impaired delivery of circulating cells and molecules necessary for host defense Vascular disease relating complications: Atherosclerosis (increases risk of MI, stroke, lower extremity gangrene) Diabetic retinopathy Diabetic nephropathy Diabetic neuropathy

Treatment Lifestyle changes Type I: insulin replacement Type II: oral hypoglycemic drug to increase insulin secretion, insulin or both