DISORDERS OF THE DIAPHRAGM PROFESSOR HESHAM ATEF ABDELHALIM

DISORDERS OF THE DIAPHRAGM PROFESSOR HESHAM ATEF ABDELHALIM FACULTY OF MEDICINE, AIN SHAMS UNIVERSITY

OBJECTIVES • Normal anatomy, radiology and function of the diaphragm. • Abnormalities in function. • Involuntary movements of the diaphragm. • Infections related to the diaphragm. • Tumors of the diaphragm. • Disorders of the diaphragmatic structure.
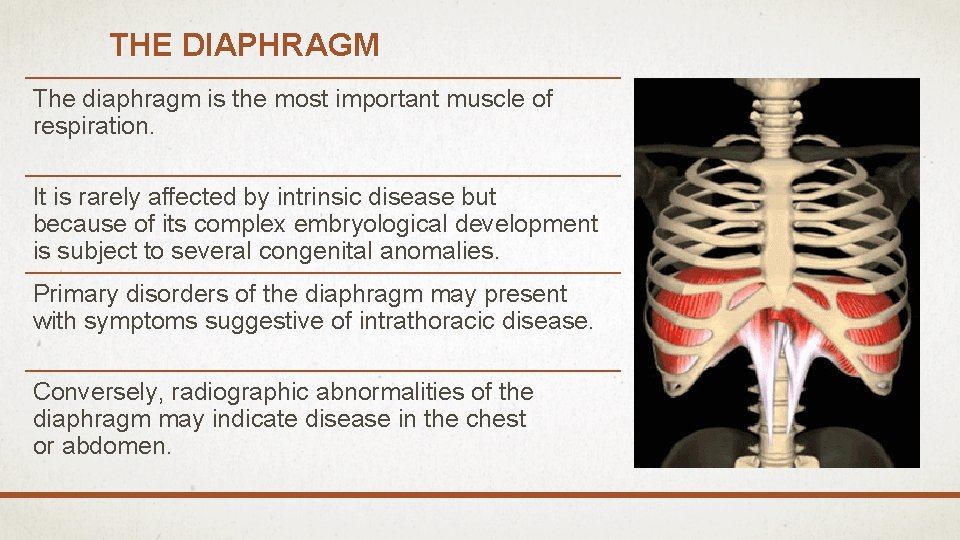
THE DIAPHRAGM The diaphragm is the most important muscle of respiration. It is rarely affected by intrinsic disease but because of its complex embryological development is subject to several congenital anomalies. Primary disorders of the diaphragm may present with symptoms suggestive of intrathoracic disease. Conversely, radiographic abnormalities of the diaphragm may indicate disease in the chest or abdomen.
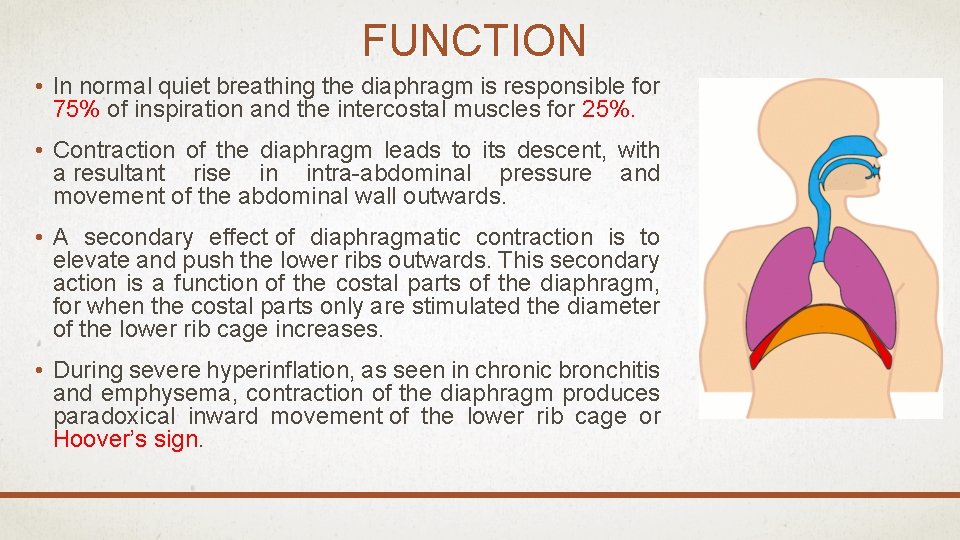
FUNCTION • In normal quiet breathing the diaphragm is responsible for 75% of inspiration and the intercostal muscles for 25%. • Contraction of the diaphragm leads to its descent, with a resultant rise in intra-abdominal pressure and movement of the abdominal wall outwards. • A secondary effect of diaphragmatic contraction is to elevate and push the lower ribs outwards. This secondary action is a function of the costal parts of the diaphragm, for when the costal parts only are stimulated the diameter of the lower rib cage increases. • During severe hyperinflation, as seen in chronic bronchitis and emphysema, contraction of the diaphragm produces paradoxical inward movement of the lower rib cage or Hoover’s sign.
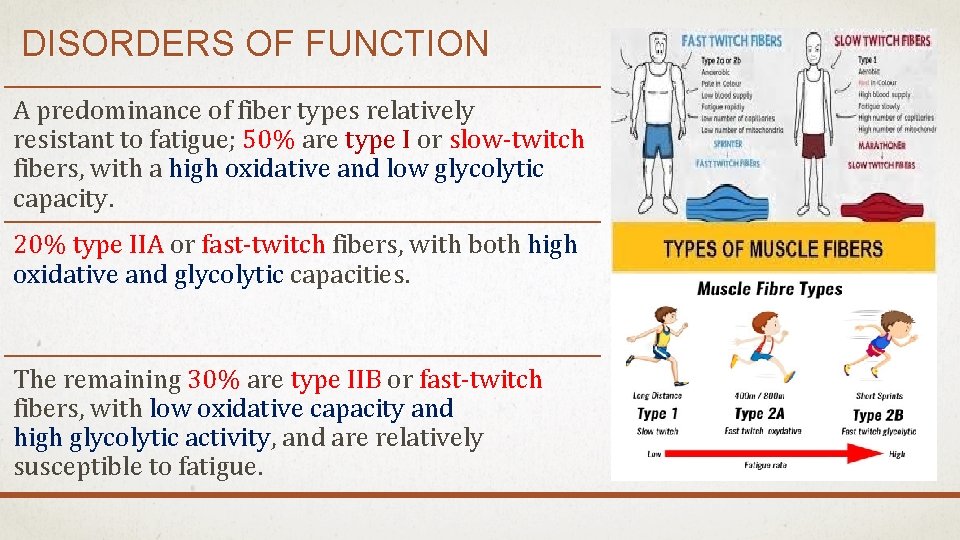
DISORDERS OF FUNCTION A predominance of fiber types relatively resistant to fatigue; 50% are type I or slow-twitch fibers, with a high oxidative and low glycolytic capacity. 20% type IIA or fast-twitch fibers, with both high oxidative and glycolytic capacities. The remaining 30% are type IIB or fast-twitch fibers, with low oxidative capacity and high glycolytic activity, and are relatively susceptible to fatigue.

• Two physical signs of diaphragmatic dysfunction are recognized. • Prominent rib cage movement in the supine position indicates recruitment of other respiratory muscles and is a feature of any disease or condition that leads to increase in the work of breathing. • More importantly, indrawing of the anterior abdominal wall during inspiration (when not due to abdominal muscle contraction) is a significant indication of diaphragmatic fatigue or paralysis. • Initial EMG evidence of fatigue either precedes or accompanies an increase in respiratory rate. This is followed by alternation between abdominal and rib cage breathing (respiratory alternans) and then by a paradoxical inward motion of the abdomen during inspiration (abdominal paradox). • Finally, minute ventilation and respiratory rate fall with a resultant increase in Paco 2. DIAPHRAGMATIC FATIGUE Clinical features

Ventilatory support with positive-pressure ventilation Ventilatory muscle training, which involves breathing against an inspiratory resistance for 30 min daily Pharmacological • Aminophylline • Caffeine MANAGEMENT

DIAPHRAGMATIC PARALYSIS Unilateral paralysis Aetiology: • The most common cause of unilateral diaphragmatic paralysis is involvement of the phrenic nerve by bronchogenic carcinoma. • Such involvement by tumors above the pulmonary hilum excludes surgical treatment, although when the lesion is below the hilum, resection of the tumor, nerve and pericardium may be attempted.
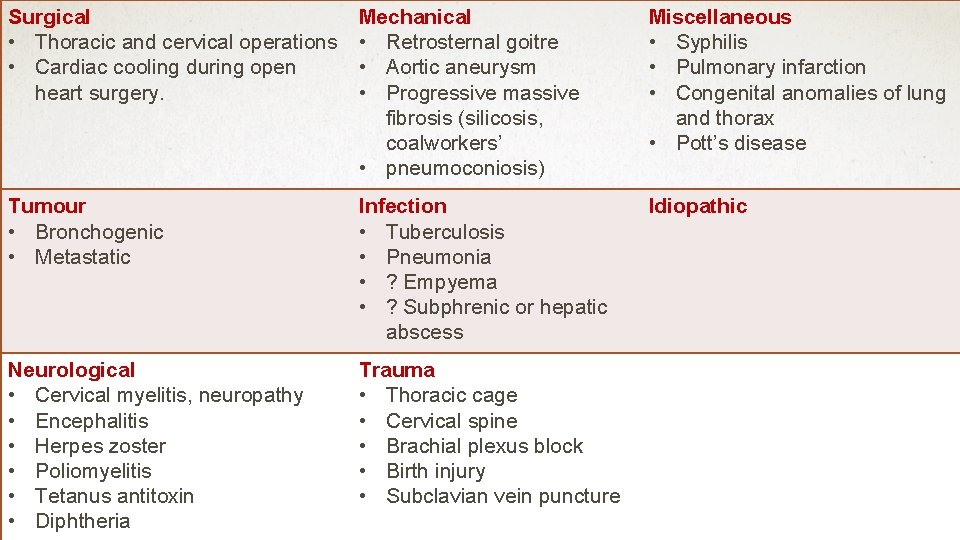
Surgical • Thoracic and cervical operations • Cardiac cooling during open heart surgery. Mechanical • Retrosternal goitre • Aortic aneurysm • Progressive massive fibrosis (silicosis, coalworkers’ • pneumoconiosis) Miscellaneous • Syphilis • Pulmonary infarction • Congenital anomalies of lung and thorax • Pott’s disease Tumour • Bronchogenic • Metastatic Infection • Tuberculosis • Pneumonia • ? Empyema • ? Subphrenic or hepatic abscess Idiopathic Neurological • Cervical myelitis, neuropathy • Encephalitis • Herpes zoster • Poliomyelitis • Tetanus antitoxin • Diphtheria Trauma • Thoracic cage • Cervical spine • Brachial plexus block • Birth injury • Subclavian vein puncture
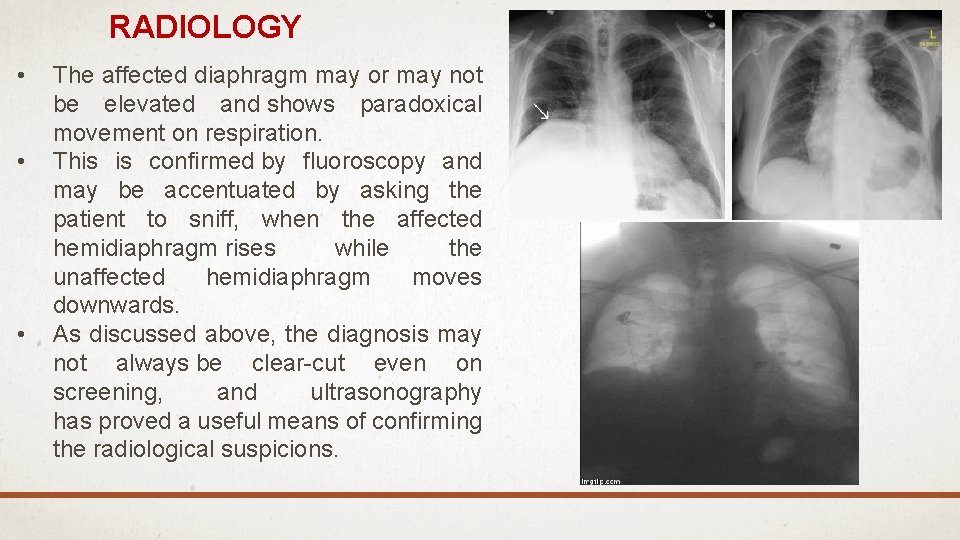
RADIOLOGY • • • The affected diaphragm may or may not be elevated and shows paradoxical movement on respiration. This is confirmed by fluoroscopy and may be accentuated by asking the patient to sniff, when the affected hemidiaphragm rises while the unaffected hemidiaphragm moves downwards. As discussed above, the diagnosis may not always be clear-cut even on screening, and ultrasonography has proved a useful means of confirming the radiological suspicions.

• Unilateral paralysis of the diaphragm reduces vital capacity by 20– 25% in the upright posture, with a further 10– 20% reduction in the supine position. • Pao 2 may fall in the supine position due to an increase in closing volume, and compression of basal lung segments on the affected side. • A 20% reduction in ventilation and perfusion to the lung on the affected side has also been shown. FUNCTIONAL EFFECTS

• • • In most cases, no treatment is necessary as the condition is symptomless. Occasionally, however, the development of unilateral paralysis in someone with severe pulmonary impairment precipitates ventilatory failure. This has been described particularly after lung or cardiac surgery. In such circumstance's recovery may take place with time, such as when the paralysis occurred because of phrenic stretching or hypothermia, and ventilatory support may be all that is necessary. If recovery does not occur, diaphragmatic plication has proved to be an effective method of improving lung mechanics and the patient’s condition. MANAGEMENT

CAUSES OF BILATERAL DIAPHRAGMATIC PARALYSIS Anterior horn cell disease • Poliomyelitis • Kugelberg–Welander disease • Motoneurone disease • Multiple sclerosis Peripheral nerve disease • Guillain–Barré syndrome • Charcot–Marie–Tooth Muscle disease • Acid maltase deficiency • Limb girdle dystrophy • Type II atrophy disease • Dystrophia myotonica • Idiopathic • Neuralgic amyotrophy
• Dyspnea is a usual feature of bilateral diaphragmatic paralysis • Paradoxical inward movement of the abdominal wall during inspiration, both particularly marked when the subject is in the supine position. • Respiratory rate is usually increased with a reduction in tidal volume. • Alveolar hypoventilation may occur during sleep with resultant carbon dioxide retention leading to disturbed sleep, morning headaches and daytime fatigue with hypersomnolence. There may be associated sleep apnoea. CLINICAL FEATURES

RADIOLOGY • Both diaphragms may be elevated on the chest film, move sluggishly or paradoxically with inspiration, and paradoxical movement should be (but is not always) seen during sniffing. • That fluoroscopy can be misleading is due to contraction of abdominal muscles during expiration, which pushes the diaphragm up passively and allows it to descend passively and apparently normally during inspiration.

• • • In complete bilateral diaphragmatic paralysis, Pdi does not change during tidal breathing or a maximum inspiration, while reduced changes in pressure are seen in patients with bilateral weakness. Vital capacity is reduced in the upright position and further decreased in the supine position. Pao 2 is reduced and falls further on lying down. Ventilation–perfusion ratio is substantially reduced in the dependent lung of patients with bilateral diaphragmatic paralysis, a phenomenon that must contribute to the postural hypoxia via shunting of blood. Decreases in both maximal transpulmonary pressure and static compliance. Reduced compliance. FUNCTIONAL CHANGES

• Although spontaneous improvement in diaphragm function has been seen, permanent paralysis is the rule. • Some patients have benefited from the use of a cuirass respirator at night to manage the associated respiratory failure. • Nasal CPAP. • Diaphragmatic pacing. MANAGEMENT

• Sudden inspiratory spasm of the diaphragm with associated closure of the glottis. • It is a familiar and harmless symptom in the normal subject, usually caused by gastric distension. • The usual cause is a reflex transmitted by vagal afferents, via vagal and respiratory nuclei in the medulla, and phrenic nerves to the diaphragm and by somatic nerves to other respiratory muscles. INVOLUNTARY MOVEMENTS OF THE DIAPHRAGM Hiccup

• Occasionally the symptom becomes persistent and distressing to the patient, especially in uraemia and neurological disease. • Some apparently idiopathic cases may be a vagal analogue of trigeminal neuralgia and hemifacial spasm, where the neural hyperactivity may be triggered by contact between nerve and blood vessel. HICCUP (Cont. )

Causes of hiccup Local causes, stimulating vagal afferents Gastric distension or inflammation Oesophageal reflux, achalasia Pericarditis Pleural effusion Mediastinial disease Chest and upper abdominal surgery Diaphragmatic irritation Subphrenic abscess Metabolic causes Anaesthesia Uraemia Addison’s disease Hypocalcaemia Central causes, affecting the brainstem Medullary infarction, tumour Multiple sclerosis Viral encephalitis, including HIV Meningitis

• Treatment depends on the cause and severity. • Empirical homely remedies recommended for transient hiccup that act via vagal stimulation. • More persistent episodes may respond to stimulation of the pharynx with a catheter introduced through the nose. This intervention is believed to initiate afferent vagal impulses that inhibit the hiccup reflex. • Prolonged or distressing hiccup requires investigation and removal of the cause. TREATMENT

• If this is not possible, it may respond to intravenous injection of 50 mg chlorpromazine. • Other drugs used have included haloperidol, metoclopramide, baclofen, antiepileptics and antidepressants. • In exceptional cases, phrenic nerve block by local anaesthetic or phrenic nerve crush has been used but is not recommended since it impairs lung function and is usually only partially successful. • In one rather dramatic instance, neurosurgical separation of the vagus from contact with the posterior inferior cerebellar artery appears to have relieved the condition. TREATMENT

Tonic spasm may complicate rabies, tetanus and strychnine poisoning and less commonly pregnancy toxemia, encephalitis and epilepsy. It results in upper abdominal pain and dyspnea and assisted ventilation. may necessitate TONIC SPASM OF THE DIAPHRAGM

• Diaphragmatic or respiratory myoclonus was first diagnosed and described by van Leeuwenhoek, the inventor of the microscope, who himself suffered from the condition. • It can occur at any age and in most cases the etiology is unknown, • Encephalitis and assorted causes of phrenic nerve irritation have been implicated in some. • The diaphragm or one hemidiaphragm contracts irregularly, with an average frequency of 150/min (range 35– 480); the EMG shows bursts of electrical activity during inspiration and expiration. DIAPHRAGMATIC OR FLUTTER

Episodes may be precipitated by emotion, eating, exercise or assorted respiratory manoeuvres. May last only a few seconds or persist for months. Attacks are usually associated with upper abdominal or lower chest pain that may mimic angina. Respiratory distress may occur. Stridor and apneustic respiration (a prolonged breathhold in inspiration) Other symptoms include belching, hiccups and retching. In some subjects, epigastric pulsations may be seen, and if the stomach is full a rhythmic splashing sound may be heard. Fluoroscopy demonstrates the abnormal movement of the diaphragm, which may also distort an ECG tracing. . The diagnosis may be confirmed if necessary, by diaphragmatic EMG. CLINICAL FEATURES

• Treatment with phenytoin 400 mg daily or carbamazepine has been successful in some cases. • Others have required phrenic paralysis by crush or injection of local anaesthetic. TREATMENT

Clinical features Subphrenic abscess may occur spontaneously due to perforation of a viscus, amoebic liver abscess or pancreatitis, or may follow abdominal surgery. Such abscesses may occur on either or both sides. Features include local costal or subcostal pain and tenderness, unexplained fever, tachycardia and leukocytosis. If antibiotics have been taken, the course may be more chronic with vague pains, chronic illhealth, unexplained fever and anaemia. Its importance for the chest physician lies in the associated changes that may be seen on a chest film or on fluoroscopy. INFECTIONS RELATED TO THE DIAPHRAGM Subphrenic abscess
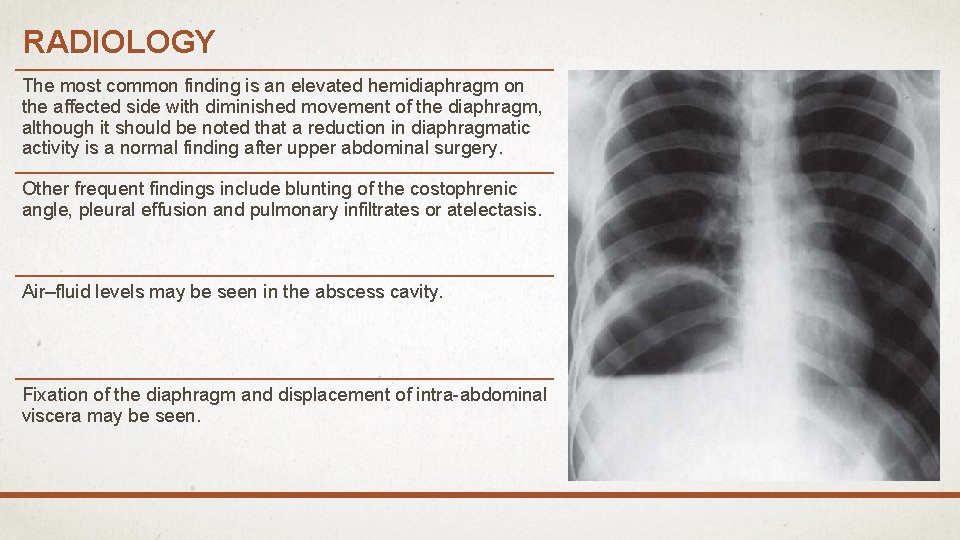
RADIOLOGY The most common finding is an elevated hemidiaphragm on the affected side with diminished movement of the diaphragm, although it should be noted that a reduction in diaphragmatic activity is a normal finding after upper abdominal surgery. Other frequent findings include blunting of the costophrenic angle, pleural effusion and pulmonary infiltrates or atelectasis. Air–fluid levels may be seen in the abscess cavity. Fixation of the diaphragm and displacement of intra-abdominal viscera may be seen.
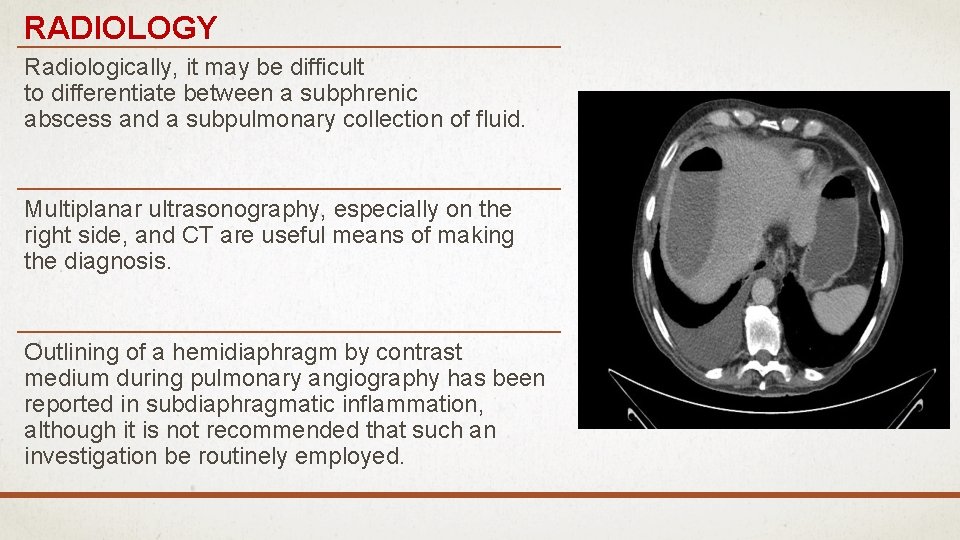
RADIOLOGY Radiologically, it may be difficult to differentiate between a subphrenic abscess and a subpulmonary collection of fluid. Multiplanar ultrasonography, especially on the right side, and CT are useful means of making the diagnosis. Outlining of a hemidiaphragm by contrast medium during pulmonary angiography has been reported in subdiaphragmatic inflammation, although it is not recommended that such an investigation be routinely employed.

Treatment • The management of subphrenic abscess is by surgical drainage and appropriate antibiotic therapy. • Percutaneous drainage under ultrasonic or fluoroscopic guidance using wide-bore catheters has been used with some success by those with special expertise.

One of the few primary diseases of the diaphragm. When ingested in undercooked pork, or much less commonly bear meat, the larvae of the nematode Trichinella spiralis may be freed in the intestines where mating of male and female produces new larvae that can penetrate the intestinal wall and enter the bloodstream. Their subsequent fate is variable: some settle in organs where they die out; others reside in the muscles, including the diaphragm, where they may remain alive for years, subsequently becoming encysted. TRICHINIASIS

The phases of intestinal invasion and encystment are usually symptomless but may be accompanied by diarrhoea and vomiting. The main symptoms usually occur 1 or 2 weeks after ingestion. These include fever, oedema that may affect the face only or be more widespread, muscle aches, skin rashes, chest pain (usually attributed to involvement of the intercostal muscles and diaphragm), hiccup, cough and haemoptysis (due probably to parasites in the lung). Respiratory failure secondary to weakness of the diaphragm and intercostal muscles has been described. CLINICAL FEATURES

Eosinophilia is a constant and early feature. The parasite may be recovered from the blood in the early stages. Other diagnostic procedures in a suspected case are muscle biopsy (after the third week) and skin and precipitin tests with Trichinella antigen. In long-standing cases the calcified larvae are visible in muscles on the chest radiograph. INVESTIGATIONS

The condition is usually self-limiting, and no treatment is required. In severe cases treatment with corticosteroids and tiabendazole (thiabendazole) 25 mg/kg daily may be required. Prevention is the most important aspect of management of trichiniasis and the disease can be eradicated by making it known that the longer pork is cooked, the safer it is. TREATMENT

TUMOURS Primary tumours of the diaphragm are exceedingly rare, Secondary tumours usually only occur as a direct extension from lung, liver or pleura.

Metastatic tumours • Are more common than primary tumours. • Few are blood-borne, the majority occurring by seeding across serous membranes, infiltration from lung through pleura or direct spread, for example from the stomach. • The most common extrapleural primary sources are breast, ovary and stomach, • Local involvement by bronchogenic carcinoma and mesothelioma is also seen. Benign tumours • Benign primary tumours occur more frequently than malignant ones. • The most common is the lipoma, which presents radiologically as a smooth rounded mass with a lower border continuous with the diaphragm. • The mass, which may appear less dense than would be expected based on its size, usually arises from the • posterolateral portion of the hemidiaphragm, more commonly on the left. • Other benign tumours include fibroma, angiofibroma, neurilemmomas and haemangiopericytomas. Angiofibromas may be calcified. • Mesothelial cysts may arise in relation to the pleuroperitoneal canal. Malignant tumours • Most malignant tumours are of mesenchymal origin • fibrosarcoma is the most common.

Clinical presentation • Malignant diaphragmatic tumors may present with severe lower chest or hypochondrial pain that radiates along intercostal nerves or to the shoulder. • The pain is usually exacerbated by respiration and may be associated with cough, dyspnea or upper gastrointestinal symptoms. • A hemorrhagic pleural effusion may be present. • A bulging of the hypochondrium that moves with respiration may occur. A palpable mass is found in 10%. • Hypertrophic pulmonary osteoarthropathy has been described in a 10% of cases. • The tumour may metastasize or invade lung locally.

Diagnosis • On radiography a mass is seen in the lower thorax that is difficult to separate from surrounding structures. • On fluoroscopy the mass is seen to move with the diaphragm. • Pneumoperitoneum and pneumothorax may be needed to confirm that the mass arises from the diaphragm. • CT may be helpful in diagnosis and may identify lipomas by their decreased radiodensity. Management • If possible, surgical excision is indicated, with local repair using fascia lata or prosthetic material

Eventration of the diaphragm • Eventration of the diaphragm is a condition in which all or part of the diaphragm is largely composed of fibrous tissue with only a few or no interspersed muscle fibers. • It is usually congenital but may be acquired. DISORDERS OF STRUCTURE

COMPLETE EVENTRATION Complete eventration almost invariably occurs on the left side and is characterized by elevation of the left hemidiaphragm, which on screening is virtually immobile and which moves paradoxically on sniffing. The condition is usually asymptomatic in adults but occasionally upper gastrointestinal symptoms such as undue flatulence may occur. In many patients, barium examination shows the stomach to be inverted beneath the hemidiaphragm. Plication of the diaphragm, has occasionally been undertaken because of the severity of dyspeptic symptoms.

• In infants, diaphragmatic eventration may occur on either side. • May give rise to severe respiratory symptoms such as cough, dyspnea and wheeze. • Recurrent bronchopneumonia with associated dyspnea and cyanosis may be seen. • Anorexia and vomiting are less common. • On examination there may be bulging of the affected hemithorax and a scaphoid abdomen. • Fluoroscopy may show a ‘dicrotic-like’ pattern of diaphragmatic movement, with the lax portion of diaphragm moving initially in a paradoxical manner followed by normal contraction of the periphery. Treatment • Diaphragmatic plication usually gives excellent clinical and radiographic results. • However, a proportion of these patients have other congenital anomalies, including neurological and bowel disorders, that may influence their clinical outcome.
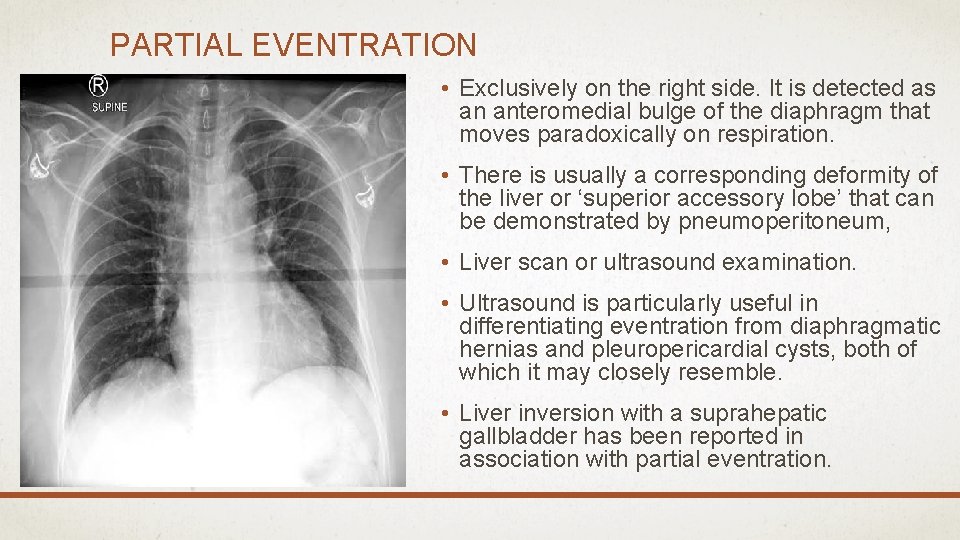
PARTIAL EVENTRATION • Exclusively on the right side. It is detected as an anteromedial bulge of the diaphragm that moves paradoxically on respiration. • There is usually a corresponding deformity of the liver or ‘superior accessory lobe’ that can be demonstrated by pneumoperitoneum, • Liver scan or ultrasound examination. • Ultrasound is particularly useful in differentiating eventration from diaphragmatic hernias and pleuropericardial cysts, both of which it may closely resemble. • Liver inversion with a suprahepatic gallbladder has been reported in association with partial eventration.
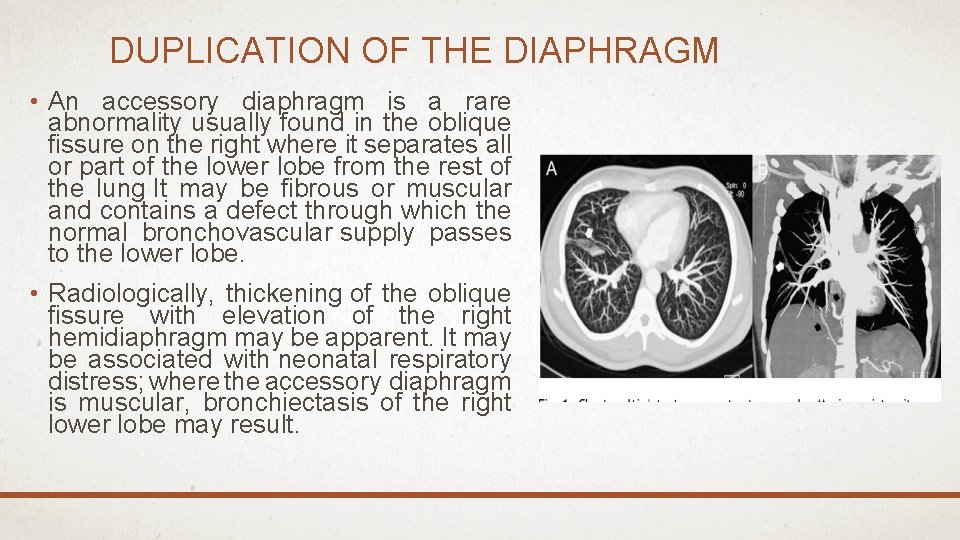
DUPLICATION OF THE DIAPHRAGM • An accessory diaphragm is a rare abnormality usually found in the oblique fissure on the right where it separates all or part of the lower lobe from the rest of the lung It may be fibrous or muscular and contains a defect through which the normal bronchovascular supply passes to the lower lobe. • Radiologically, thickening of the oblique fissure with elevation of the right hemidiaphragm may be apparent. It may be associated with neonatal respiratory distress; where the accessory diaphragm is muscular, bronchiectasis of the right lower lobe may result.
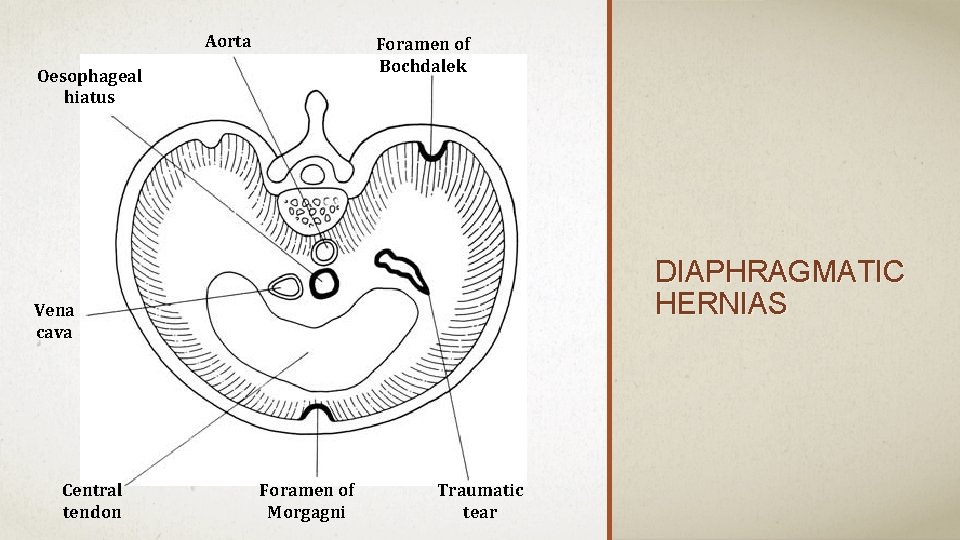
Aorta Foramen of Bochdalek Oesophageal hiatus DIAPHRAGMATIC HERNIAS Vena cava Central tendon Foramen of Morgagni Traumatic tear
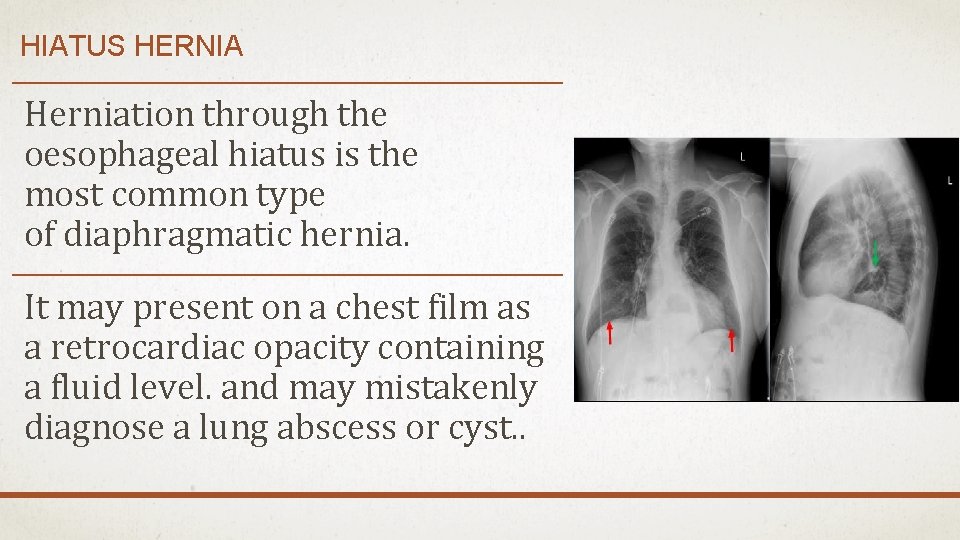
HIATUS HERNIA Herniation through the oesophageal hiatus is the most common type of diaphragmatic hernia. It may present on a chest film as a retrocardiac opacity containing a fluid level. and may mistakenly diagnose a lung abscess or cyst. .

• Bochdalek first described the embryology and the congenital absence of the posterolateral part of the diaphragm in 1848. • This is the most common site for congenital diaphragmatic hernia and an incidence of 0. 8 per 1000 live births has been reported. • The foramen of Bochdalek is normally closed by the eighth week of fetal life. Failure of the pleuroperitoneal membrane to fuse with the septum transversum allows herniation of the abdominal contents into the hemithorax; 75% occur on the left BOCHDALEK HERNIA

• There may be other associated malformations, most commonly of the central nervous system. • A 13 th pair of ribs is a reported association. • The lung on the side of hernia is usually hypoplastic with a reduction in the number of airway generations, although normal numbers of alveoli are found in the segments that are present. • The contralateral lung may also be hypoplastic and this heralds a poor prognosis. In an extreme form, • Bochdalek hernia merges with congenital diaphragmatic agenesis, a condition more readily diagnosed by antenatal ultrasound, but which causes even more severe postnatal respiratory problems. BOCHDALEK HERNIA
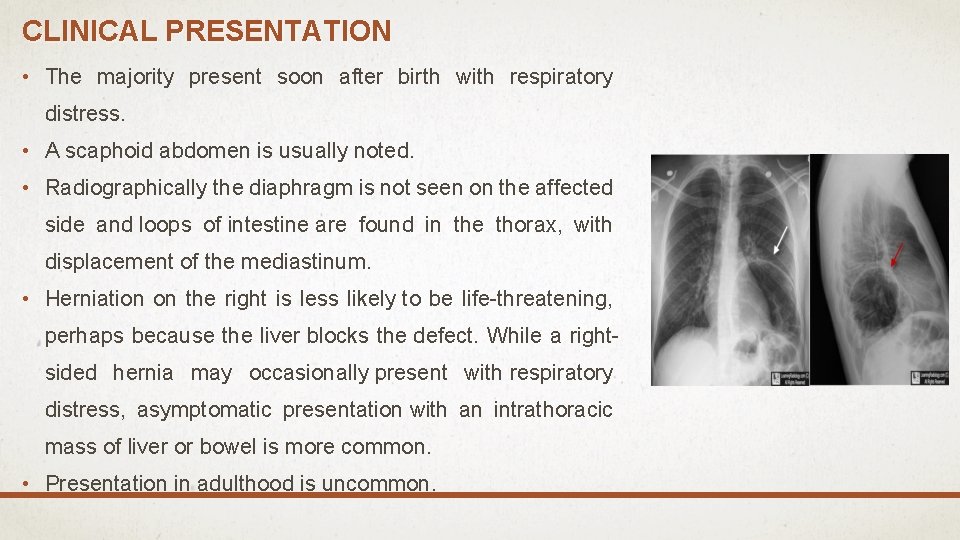
CLINICAL PRESENTATION • The majority present soon after birth with respiratory distress. • A scaphoid abdomen is usually noted. • Radiographically the diaphragm is not seen on the affected side and loops of intestine are found in the thorax, with displacement of the mediastinum. • Herniation on the right is less likely to be life-threatening, perhaps because the liver blocks the defect. While a rightsided hernia may occasionally present with respiratory distress, asymptomatic presentation with an intrathoracic mass of liver or bowel is more common. • Presentation in adulthood is uncommon.

Management and prognosis • Management of patients in respiratory distress is with ventilatory support and correction of acidosis, followed immediately by surgical repair, either by direct suture or with insertion of synthetic patches. • Overall survival rates of 70– 80% have been reported in neonates, with lower rates in those requiring operation within the first 24 h of life. • Most deaths are due to the presence of severely hypoplastic lungs that are incapable of sustaining life. • In those with unilateral hypoplasia, compensatory emphysema may develop in the other lung.

• The foramen of Morgagni lies anteromedially and is bounded anteriorly by the sternum, medially by the sternal portion of the diaphragm and laterally by the costal portion of the diaphragm in the region of the attachment to the seventh costal cartilage. • It is usually filled with loose connective tissue but omentum, colon, liver or other infradiaphragmatic structures, including gallbladder, may herniate through the foramen, • More commonly on the right. MORGAGNI HERNIA
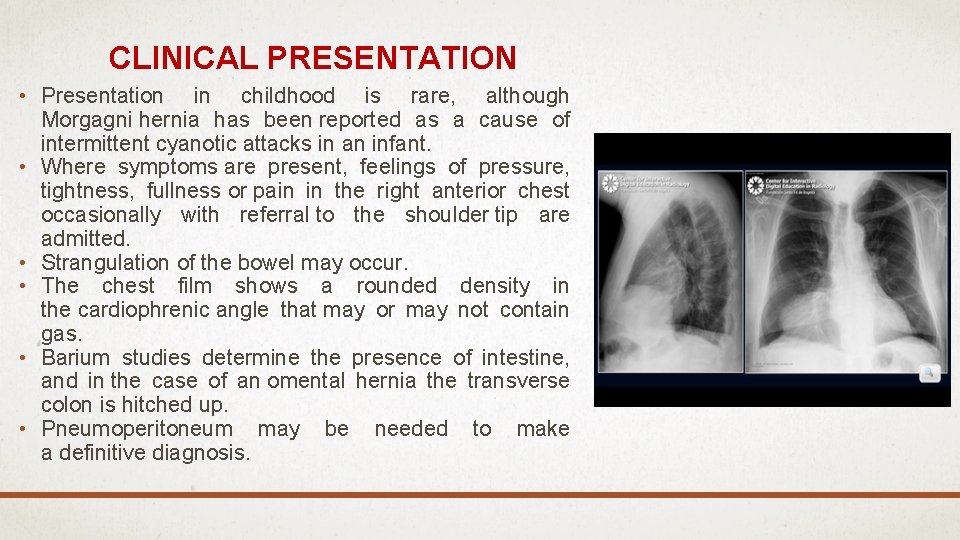
CLINICAL PRESENTATION • Presentation in childhood is rare, although Morgagni hernia has been reported as a cause of intermittent cyanotic attacks in an infant. • Where symptoms are present, feelings of pressure, tightness, fullness or pain in the right anterior chest occasionally with referral to the shoulder tip are admitted. • Strangulation of the bowel may occur. • The chest film shows a rounded density in the cardiophrenic angle that may or may not contain gas. • Barium studies determine the presence of intestine, and in the case of an omental hernia the transverse colon is hitched up. • Pneumoperitoneum may be needed to make a definitive diagnosis.

Management • Surgical repair by suture after reduction of the hernia is normally enough.

• Traumatic diaphragmatic hernias are most seen following blunt non-penetrating trauma to the chest in road traffic accidents or falls from a height. Many are detected at the time of the initial injury although a substantial number present later, even up to 15 years after the initial injury. It has been estimated that 90% of traumatic diaphragmatic hernias are overlooked at the time of injury. • Traumatic hernias represent only 5% of all diaphragmatic hernias, but 90% of all strangulated hernias result from trauma; 90% of tears occur in the left leaf of the diaphragm, most commonly in the central and posterior portion. The most common hernial contents are omentum, stomach or colon, although any abdominal organ including kidney may be found. Rarely, herniation into the pericardium occurs. TRAUMATIC HERNIA

Clinical presentation • The most common complaints are of upper abdominal or lower chest pain with dyspnea, which may be worse after eating. • Bowel sounds may be audible in the chest. If strangulation occurs, sudden and progressive severe lower chest or upper abdominal pain is experienced, with dyspnea, vomiting or retching. • Upper abdominal guarding is found and progression to shock occurs. • On one occasion, the author has seen perforation of colon into the pleura following traumatic rupture of the diaphragm, causing pyopneumothorax. • A rare complication of traumatic rupture is bronchopancreatic fistula following acute pancreatitis; this can be diagnosed by finding high levels of amylase in the profuse frothy sputum.

Radiology • Radiologically, the only evidence may be an elevated hemidiaphragm; • at the other extreme multiple air–fluid levels may be present. • Barium studies demonstrate obstruction or constriction of the stomach or colon as it passes through the tear. • With herniation of the liver on the right side, pneumoperitoneum (which results in pneumothorax) may be needed to confirm the diagnosis. • CT may enable the discontinuity in the diaphragm to be seen.

Management Surgical repair may be achieved by the abdominal, thoracic or combined routes. In view of the common concurrence of injury to abdominal viscera, the abdominal route is usually preferred.

- Slides: 57