Disorders of Small and Large Bowel Jay Green

Disorders of Small and Large Bowel Jay Green October 26, 2006

Case 1 § § § 54 y. o. F, abdominal pain Started 2 days ago, shortly after Big Mac Hurts all over, comes and goes, crampy +D yesterday, bloated, +N today, ø V PMH: DMII, HTN, TAH/BSO (’ 04) Ideas?

DDx - Approach § Think anatomy Intraperitonaeal, retroperitoneal, other § Think VITAMIN D, VINDICATED, whatever… § Vascular § Ischemic gut, MI, AAA § Infection § Gastro, PUD, psoas abscess § Neoplastic § Intussusception § Inflammatory § Diverticulitis, Cholecystitis, Pancreatitis, Appendicitis § Traumatic § Obstruction § Pregnancy
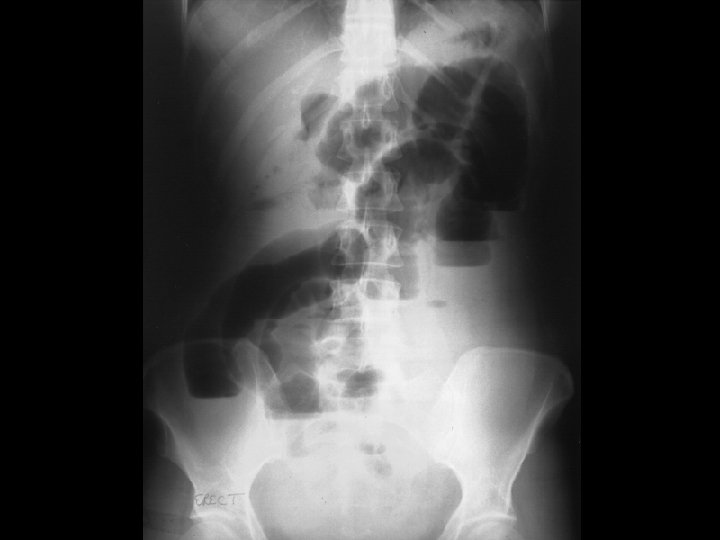

Small Bowel Obstruction § Top 3 causes? § Hernia § Adhesions § CA § Most likely to cause strangulation? § Hernia – often closed loop § Others to think about? § Gallstone ileus, volvulus, intussusception, abscess, hematoma, foreign body

§ More than half of SBO recurr § True § False § Bathing in tomato juice removes the smell of a skunk § True § False

SBO – Quick facts § 20% of acute abdo admissions § Mortality <5% (30% with strangulation, 60% in 1900) § >50% recur
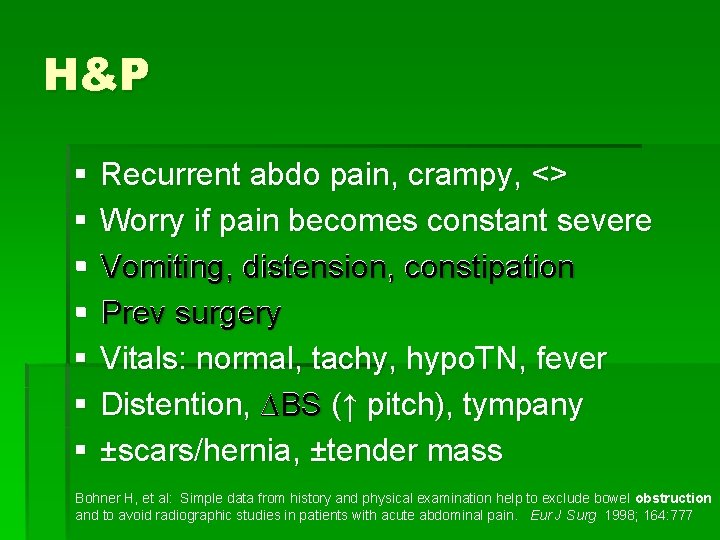
H&P § Recurrent abdo pain, crampy, <> § Worry if pain becomes constant severe § Vomiting, distension, constipation § Prev surgery § Vitals: normal, tachy, hypo. TN, fever § ∆ Distention, ∆BS ( BS ↑ pitch), tympany § ±scars/hernia, ±tender mass Bohner H, et al: Simple data from history and physical examination help to exclude bowel obstruction and to avoid radiographic studies in patients with acute abdominal pain. Eur J Surg 1998; 164: 777

Review of the basics § Types? § Mechanical & functional § Simple & closed loop (±strangulation) § Common causes of ileus? § Trauma, infection, sx, meds, metabolic, renal colic

§ Physicians reliably can distinguish bowel strangulation from simple obstruction § True § False § Cracking knuckles leads to arthritis § True § False

Simple vs Strangulated How good are we? § Confident diagnosis of “non-strangulating obstruction” wrong 31% of the time. § No parameter is sensitive, specific, or predictive for strangulation § Not very good! Sarr et al. Preoperative recognition of intestinal strangulation obstruction: Prospective evaluation of diagnostic capability. Am J Surg 145: 176 -182, 1983.

Pathophysiology § Mechanical SBO → prox dilation → ↑ local peristalsis → ↑ secretory activity → ↓ reabsorption fluid/lytes → capillary/lymphatic obstruction → edema → perforation or strangulation

Investigations § Labs: § ↑WBC, ±↑CPK, ±↑lactate § Imaging: § 3 views (60% +SBO, 25% suggestive) § Five places to look for air? § How many A/F levels? § Dilated?
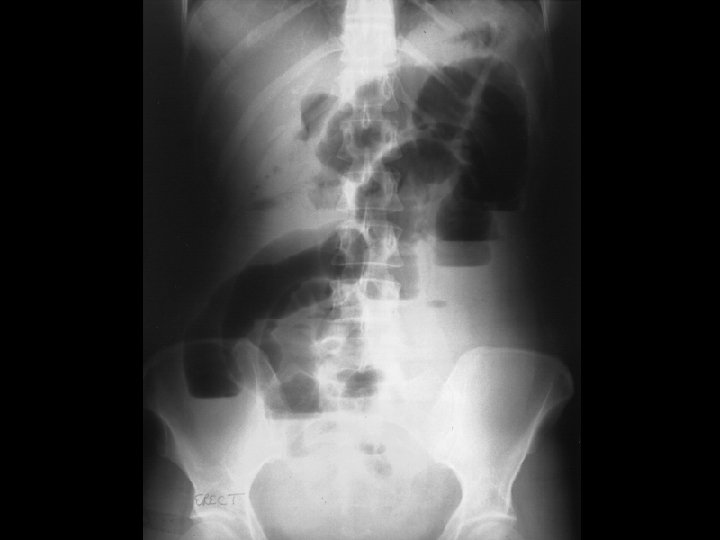
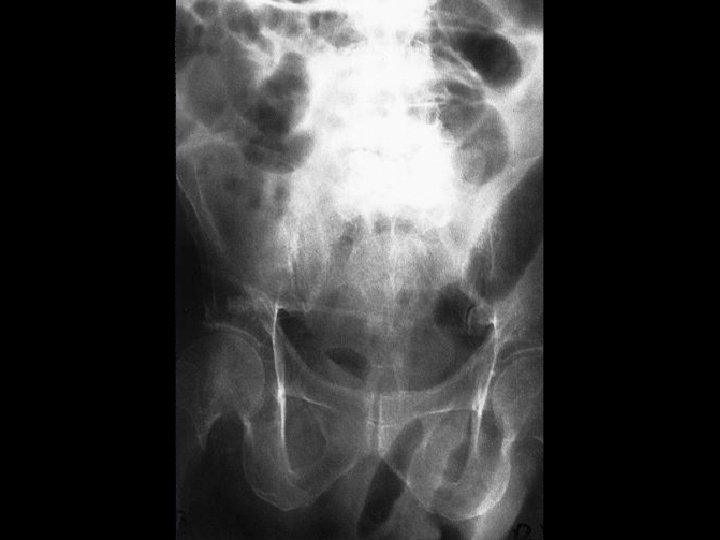
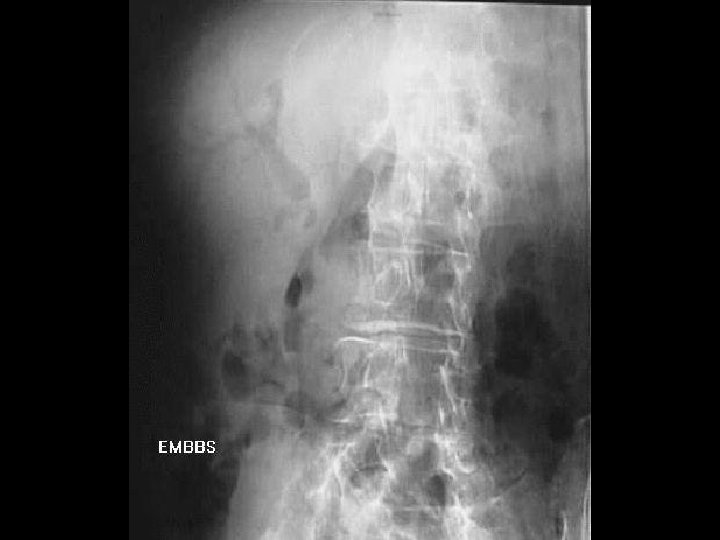
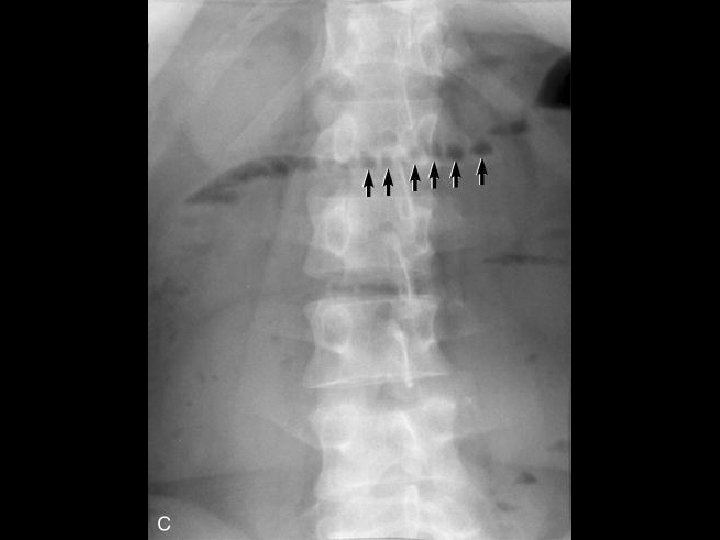

CT Scan? § Not required for diagnosis § Can help define site/cause § Other imaging? § Small bowel series, U/S
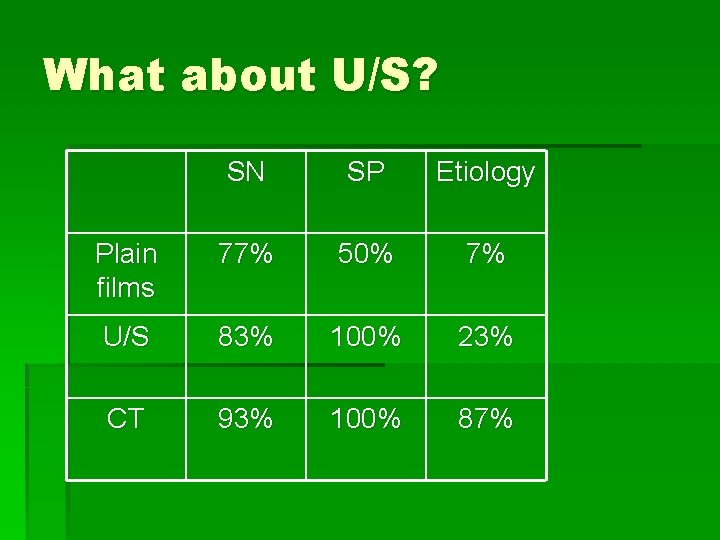

What about U/S? SN SP Etiology Plain films 77% 50% 7% U/S 83% 100% 23% CT 93% 100% 87%

§ ½ of complete SBO resolve spontaneously § True § False § Eating 3 poppy seed bagels may result in positive urine drug screen for opiates § True § False

Management § Fluid resuscitation § Decompression § NG tube § ? Antibiotics § Observation vs. surgery § “never let the sun rise or set on an SBO” § 75% of partial/30 -50% complete resolve

Take home points § You are not good at dx strangulation § AXR - >2 A/F levels, >2. 5 cm, air x 5 § ½ of SBO resolve spontaneously

Case 2 § 28 M central/RLQ crampy abdominal pain, N § Last BM this am, no fever/chills/V § Best guess? § 28 F same hx? § 25% signs initially suggestive of appe = gyne § 84 F type II DM same hx? § 4 M same hx?

Case 2 § Vitals – 37. 3, 85, 126/85, 18 § RLQ tenderness, +guarding § Investigations?

Appendicitis – Quick facts § § § 7% lifetime incidence 250 000 cases/yr in the USA First appendectomy – 1735

What the heck is this?

The Appendix § "Its major importance would appear to be financial support of the surgical profession. " - Alfred Sherwood Romer Leonardo da Vinci (1492)

Pathophysiology § § § Obstruction ↑ pressure distension ischemia + bacteria/PMN invasion swells, irritates necrosis and rupture

History § Three most common symptoms? § abdo pain, anorexia, nausea § Rule out based on pain location? § no, can even have LUQ pain

Physical exam § § § Vitals – 37. 3, 85, 126/85, 18 Do normal vitals r/o appendicitis? What if T = 38. 1? § Low grade fever in 15% (40% if ruptured) § Eponyms § Mc. Burney’s, Rovsing’s, Obturator, Psoas, Dunphy

H&P § Three important signs/symptoms? § RLQ pain, rigidity, migration of pain § Four to help rule out appendicitis? § Pain > 48 h, similar pain, lack of migration, lack of ↑ pain with movement/cough

§ CMT is uncommon in women with acute appendicitis § True § False § The air expelled in a sneeze can travel up to 100 mph § True § False

Classic Appendicitis § § § § Peri-umbilical pain RLQ migration N, anorexia, V No history of similar pain in past Pain < 48 hrs at presentation Pain ↑ with movement/cough Low grade fever Rigidity & guarding Local RLQ tenderness

Serial exams § § § Review of 30 years of publications “active observation” = reassess pt q 2 -3 h Pain resolved in 1/3 of patients No change in perforation rate Negative appendectomy rate 6% § vs 20 -30% (? lower with CT or U/S) Jones PF. Suspected acute appendicitis: Trends in management over 30 years. Br J Surg 2001; 88: 1570 -77.

What labs? § Commonly ordered § CBC, β-hcg, U/A § ±LFT’s/lipase, ±CRP § Findings § ↑ WBC, U/A – pyuria, microscopic hematuria § Necessary? § β-hcg!

U/S vs CT § SN 94%, SP 95%, LR+ 13. 3, LR- 0. 09 § + usually visualize appendix, not operator dependent, ID other pathology § - radiation § Contrast? § Rectal – best but not practical § Oral – delay, ? tolerated, esp. helpful in thin/kids § IV – not recommended

U/S vs CT § U/S § SN 86%, SP 81%, LR+ 5. 8, LR- 0. 19 § + pregnant, kids, female, thin pts § - obese, strictures, retrocecal, normal § MRI? § Very sensitive but not available

? Change Management? § 2 studies of CT in pts w/ suspected appendicitis comparing Tx plan before & after access to results of scans § § CT changed disposition in 27 – 59% of pts Prevented d/c of ~3% pts w/ appendicitis Prevented negative laparotomy in 3 -13% Alternate Dx in 11 -20% § Frank et al. Unenhanced helical CT scanning of the abdomen and pelvis changes disposition of patients presenting to the emergency department with possible acute appendicitis. J Emerg Med 2002; 23: 1 -7 § Rao et al. Effect of computed tomography of the appendix on treatment of patients and use of hospital resources. N Eng J Med. 1998; 338: 141 -6 Thanks Moritz!

To image or not? § Imaging based on risk-stratification § Don’t image: § Low risk – minimal physical findings, hungry, alternative dx, hx similar pain, sympt > 3 days § First few hours of pain § Image § Intermediate risk – lack classic appendicitis finding § ? Image § High risk – classic presentation § Will go to OR anyway

Wake the surgeon? § Time from onset of symptoms to rupture? § 24 -36 hours § Average time to seek medical care § 17 hours § Complication rate § 3% vs 12% with rupture § Mortality § <0. 1% vs 3 -4% with rupture

Take home points § Normal vitals do not rule out appendicitis § Think about U/S over CT in skinny/kids § Image pts with equivocal presentation § Single most important lab test β-hcg

Mesenteric adenitis? § Most common associated condition § 5 -10% admissions for appendicitis § § § ? More common than appendicitis Mostly children Non-specific infl. of mesenteric LN § Can follow viral illness § Yersinia species (Y. enterocolitica)

Mesenteric adenitis? § O/E: § ±Mild fever § Diffuse tenderness, RLQ, no peritonitis § 20% other lymphadenopathy § Ix: § ±↑WBC § U/S or CT may be helpful § Tx: § none, self-limited

Case 3 § 65 M § Suprapubic and LLQ pain x days, similar bouts of pain in past § Anorexia, nausea § O/E: Vitals normal, LLQ tender, no peritoneal signs, ? distended § #1 in DDx? § Initial investigations?

Diverticular disease facts § § § 10% > 45 yrs, 80% > 80 yrs ? Dietary deficiency in fibre 85% L-sided (opposite in Japan)
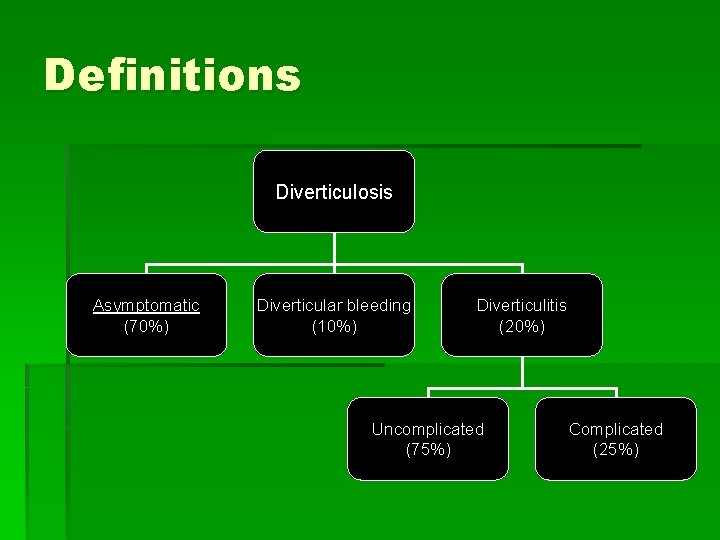
Definitions Diverticulosis Asymptomatic (70%) Diverticular bleeding (10%) Diverticulitis (20%) Uncomplicated (75%) Complicated (25%)
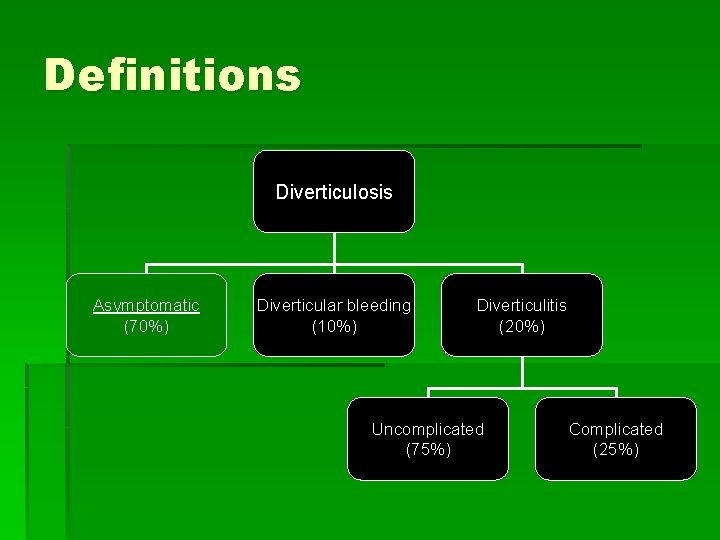
Definitions Diverticulosis Asymptomatic (70%) Diverticular bleeding (10%) Diverticulitis (20%) Uncomplicated (75%) Complicated (25%)

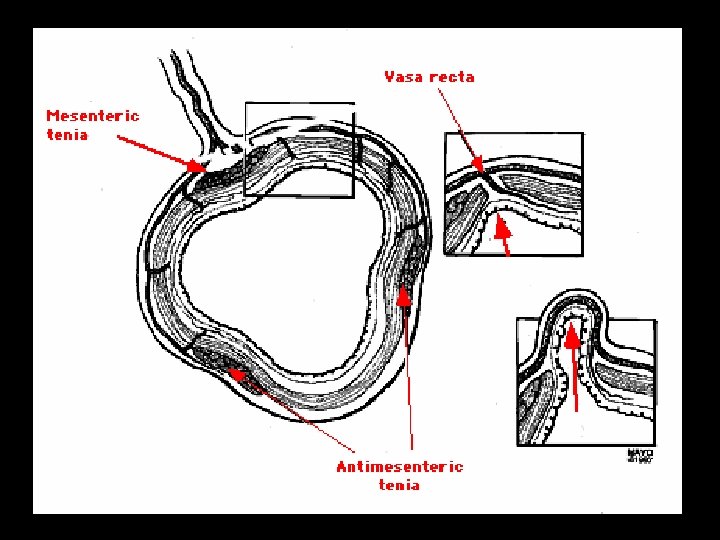
Anatomy/Pathogenesis § Vasa recta penetrate colonic wall § Forms weak points § Small (low fibre) stool ↑ pressure herniation of mucosa at vasa recta
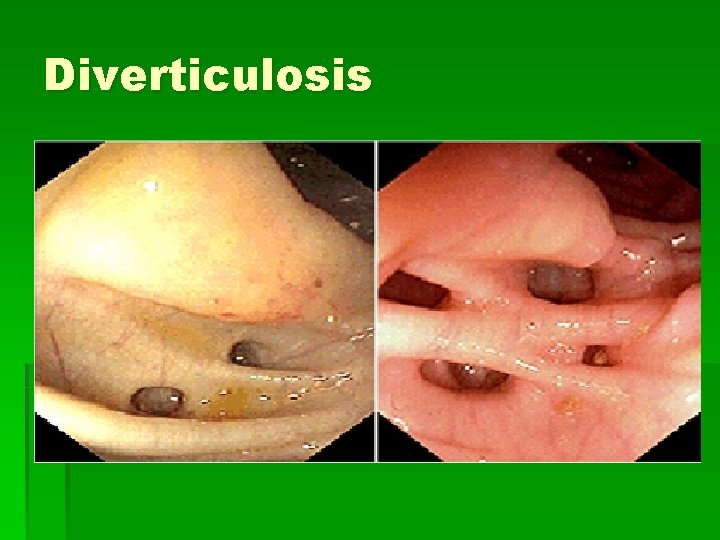
Diverticulosis

Clinical features § Usually nil § Can present like IBS § Abdo pain/cramping § Bloating § Constipation/diarrhea

Management § If necessary § Analgesia § Anti-spasmodics § Modify natural history of disease § High-fibre diet § ±stool softeners

Case 3 b § § 65 M Hematochezia No pain O/E: Vitals normal, abdo benign, FOB+ § Top 3 in DDx?
Definitions Diverticulosis Asymptomatic (70%) Diverticular bleeding (10%) Diverticulitis (20%) Uncomplicated (75%) Complicated (25%)

Diverticular bleeding § § § 40% of all LGIB 5% severe bleed Typically painless hematochezia

Management § Resuscitation § Localization of bleeding site § r/o UGIB, colonoscopy § ± angiography or radionuclide scan § Treatment § Surgery
Definitions Diverticulosis Asymptomatic (70%) Diverticular bleeding (10%) Diverticulitis (20%) Uncomplicated (75%) Complicated (25%)

Diverticulitis Diverticulum obstructed inflammation microperforation pericolic inflammation pain

Diagnosis – H&P, Labs § History § LLQ pain, several days, prev. pain § O/E § Fever, LLQ tenderness, ±distension, ±mass § Labs § ↑WBC
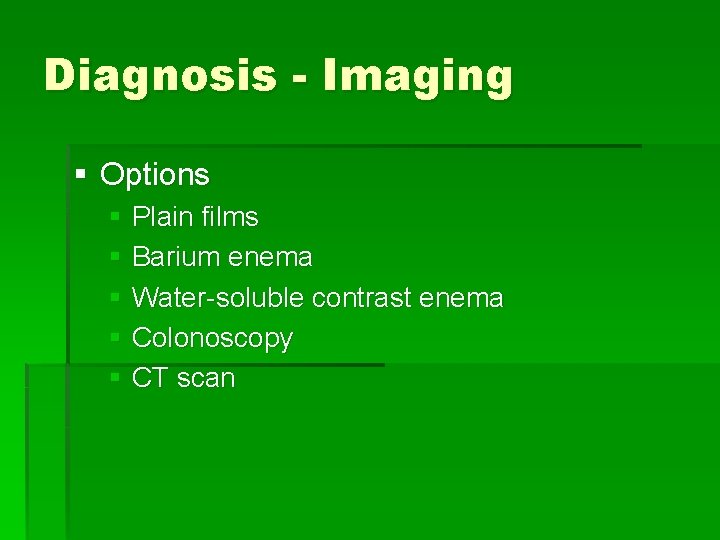
Diagnosis - Imaging § Options § Plain films § Barium enema § Water-soluble contrast enema § Colonoscopy § CT scan

§ Barium enema is an appropriate investigation in acute diverticulitis § True § False § Spicy food can cause ulcers § True § False

Plain films § Not useful in diagnosis of diverticulitis § Utility lies in ruling out obstruction/ perforation

Barium enema § Useful to diagnose asymptomatic diverticulosis § CONTRAINDICATED in acute diverticulitis § Potential for barium peritonitis
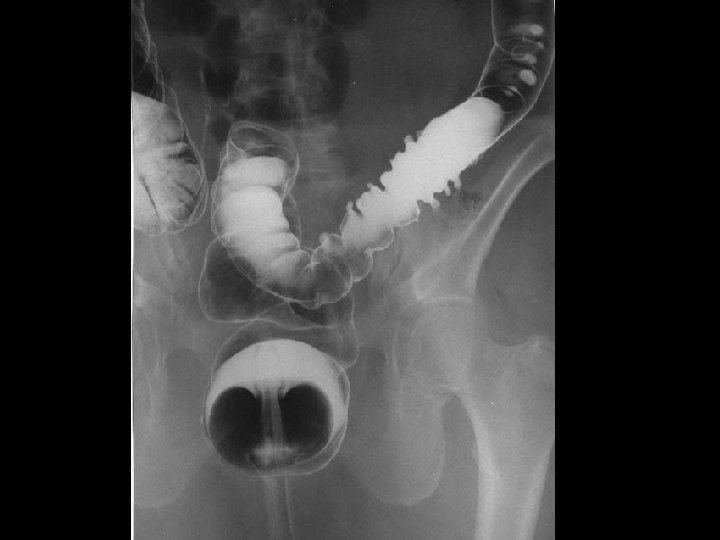
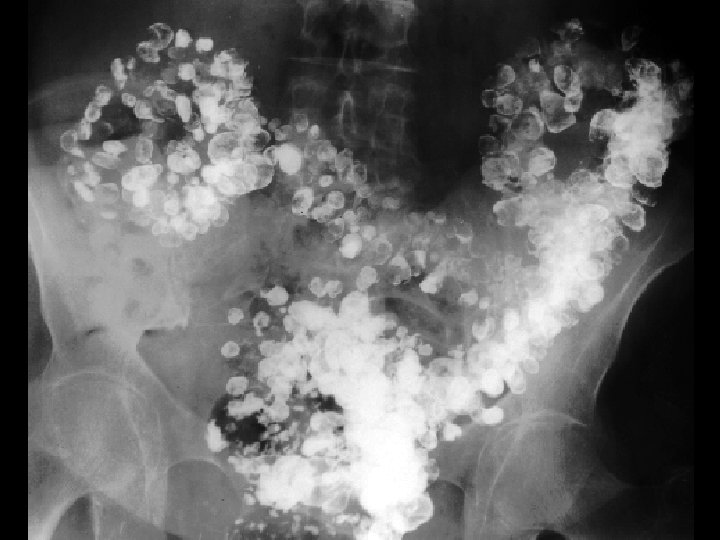

Water-soluble contrast enema § Less detail than barium § Can see contrast collect in abscess cavity, peritoneum, along fistulae § Less info than CT about disease extent

Colonoscopy § Not for acute setting

CT scan § § § Investigation of choice SN 69 -95%, SP 75 -100% Evaluate extent of disease Exclude other pathology If known uncomplicated diverticulitis – not necessary

Management § Uncomplicated § Outpatient § Analgesia § Oral Abx § Septra/Flagyl, Cipro/Flagyl, Clavulin § Fibre § F/U

Management § Complicated § Inpatient § Analgesia § IV Abx § Surgery vs. medical management

Surgery or not? § First episode § Usually medical management § 3 -30% recurr § Subsequent episodes, immunocompromised § More likely to require surgery or precutaneous abscess drainage

Take home points § Diverticulosis asympt vs. IBS-like bleeding inflammation § Imaging of choice in diverticulitis is CT § Most uncomplicated pts can go home

Questions?

References § Ferri: Ferri's Clinical Advisor: Instant Diagnosis and Treatment, 8 th ed. , 2006 Mosby § Leyner, Goldberg. Why Do Men Have Nipples? 2005 Three Rivers Press § Mandell, Bennett, & Dolin: Principles and Practice of Infectious Diseases, 6 th ed. , 2005 Churchill Livingstone § Marx, Hockberger & Walls. Rosen’s Emergency Medicine, 6 th ed. , 2006 Mosby § Up. To. Date
- Slides: 74