DISORDERS CAUSING INFERTILITY IN COUPLES By Syed Tanveer


DISORDERS CAUSING INFERTILITY IN COUPLES By Syed Tanveer Abbas Gilani MBBS, FCPS, Classified Chemical Pathologist CMH Bahawalnagar

SEQUENCE OF PRESENTATION Introduction of infertility Causes, evaluation & diagnostic criteria of male infertility Causes, evaluation & diagnostic criteria of female infertility Clinical cases (10 to 20)
INTRODUCTION What was once an act of private “Love” is now a public act, a commercial transaction and a professionally managed procedure Sarah Franklin
INFERTILITY Infertility is inability to conceive after one year of unprotected intercourse Definition 25% of couples experience an episode of infertility Primary infertility Types Secondary infertility

INFERTILITY PRIMARY INFERTILITY • Refers to couples or patients who had no previous successful pregnancies SECONDARY INFERTILITY • Refers to couples who have previously conceived, but are currently unable to conceive Hormonal dysfunction of hypothalamic- pituitary-gonadal axis

PREVALENCE OF INFERTILITY Prevalence • World wide 10% to 15% • Pakistan 21. 9% Relative abnormalities • Female partner - 50% (42%) • Male partner - 40% (26%) • Both partners - 10% (32%) Unexplained infertility • Approximately 15% to 20% Ref. Sharlip I, Jarow J, Belker A, Lipshultz L, Sigman M, Thomas A, et al. Best practice policies for male infertility. Fertil Steril 2002; 77: 873– 82. , Turek PJ. Practical approaches to the diagnosis and management of male infertility. Nat Clin Pract Urol 2005; 2: 226– 38. 3. Mackay HT. Gynecology. In: Tierney LM, Mc. Phee SJ. Papadakis MA. Current medical diagnosis and treatment. 42 nd ed. New York: Mc Graw-Hill; 2003. p. 699– 733.
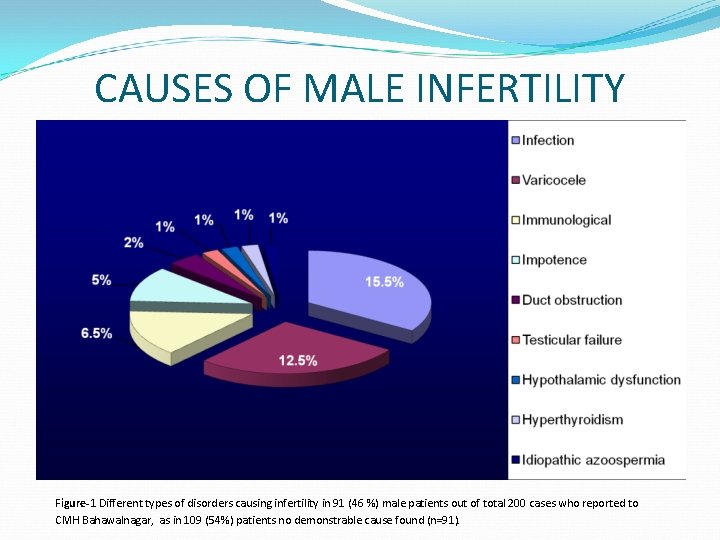
CAUSES OF MALE INFERTILITY Figure-1 Different types of disorders causing infertility in 91 (46 %) male patients out of total 200 cases who reported to CMH Bahawalnagar, as in 109 (54%) patients no demonstrable cause found (n=91).
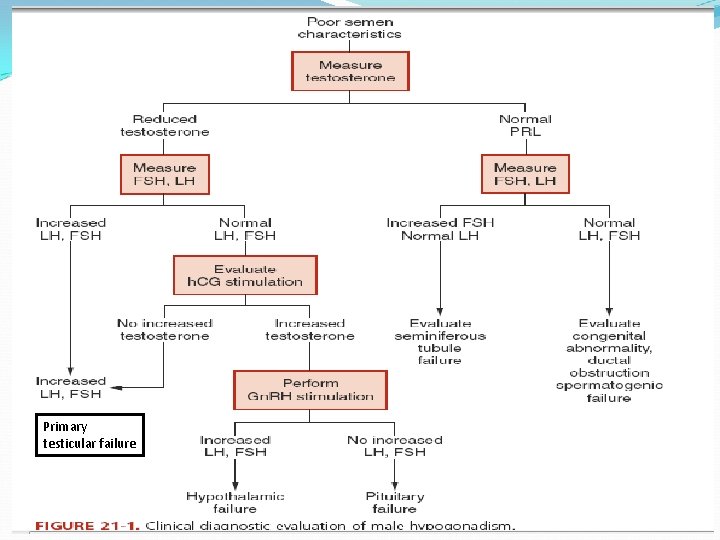
Primary testicular failure
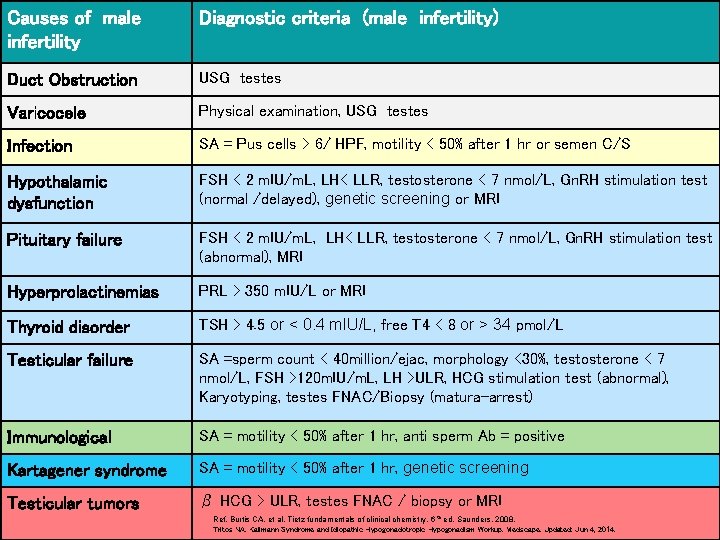
Causes of male infertility Diagnostic criteria (male infertility) Duct Obstruction USG testes Varicocele Physical examination, USG testes Infection SA = Pus cells > 6/ HPF, motility < 50% after 1 hr or semen C/S Hypothalamic dysfunction FSH < 2 m. IU/m. L, LH< LLR, testosterone < 7 nmol/L, Gn. RH stimulation test (normal /delayed), genetic screening or MRI Pituitary failure FSH < 2 m. IU/m. L, LH< LLR, testosterone < 7 nmol/L, Gn. RH stimulation test (abnormal), MRI Hyperprolactinemias PRL > 350 m. IU/L or MRI Thyroid disorder TSH > 4. 5 or < 0. 4 m. IU/L, free T 4 < 8 or > 34 pmol/L Testicular failure SA =sperm count < 40 million/ejac, morphology <30%, testosterone < 7 nmol/L, FSH >120 m. IU/m. L, LH >ULR, HCG stimulation test (abnormal), Karyotyping, testes FNAC/Biopsy (matura-arrest) Immunological SA = motility < 50% after 1 hr, anti sperm Ab = positive Kartagener syndrome SA = motility < 50% after 1 hr, genetic screening Testicular tumors β HCG > ULR, testes FNAC / biopsy or MRI Ref. Burtis CA, et al. Tietz fundamentals of clinical chemistry, 6 th ed. Saunders, 2008. Tritos NA. Kallmann Syndrome and Idiopathic Hypogonadotropic Hypogonadism Workup. Medscape. Updated: Jun 4, 2014.

FEMALE INFERTILITY Female infertility factors are 1. OVARIAN OR HORMONAL FACTORS a. METABOLIC DISEASE Ø Polycystic ovarian syndrome Ø Thyroid Ø Liver Ø Obesity Ø Androgen excess

FEMALE INFERTILITY FACTORS b. HYPERGONADOTROPIC HYPOGONADISM Ø Premature ovarian failure (autoimmune, cytotoxic chemotherapy, tumor) Ø Menopause Ø Luteal phase deficiency Ø Gonadal dysgenesis Ø Resistant ovary syndrome c. HYPOGONADOTROPIC HYPOGONADISM Ø Hyperprolactinemia (tumor, drugs) Ø Hypothalamic insufficiency (Kallmann syndrome) Ø Pituitary insufficiency (tumor, necrosis, stress, anorexia)

FEMALE INFERTILITY FACTORS d. OVULATORY DYSFUNCTION Ø Ovulatory dysfunction manifests itself in presence or absence of normal menses Ø Metabolic diseases affect ovulatory function Ø PCOS is the most common cause of anovulation Ø CAH should be considered (21 -hydroxylase deficiency or 3ßhydroxysteroid deficiency may be present in 26% cases)
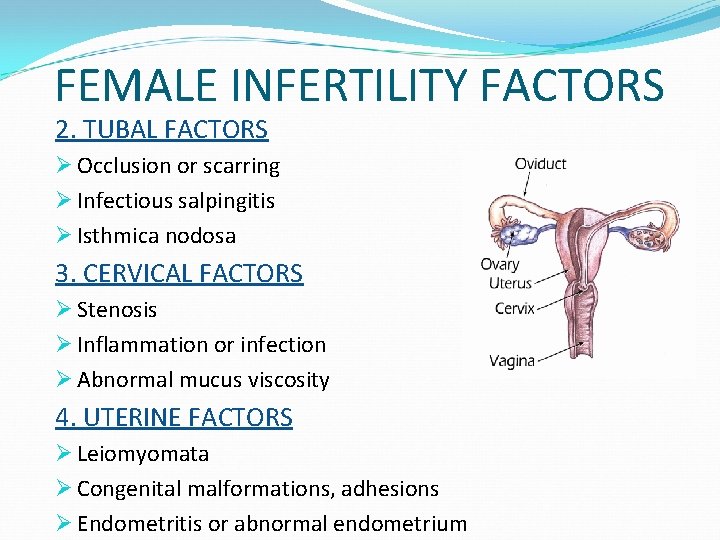
FEMALE INFERTILITY FACTORS 2. TUBAL FACTORS Ø Occlusion or scarring Ø Infectious salpingitis Ø Isthmica nodosa 3. CERVICAL FACTORS Ø Stenosis Ø Inflammation or infection Ø Abnormal mucus viscosity 4. UTERINE FACTORS Ø Leiomyomata Ø Congenital malformations, adhesions Ø Endometritis or abnormal endometrium

FEMALE INFERTILITY FACTORS 5. PSYCHOSOCIAL FACTORS Ø Decreased libido Ø Anorgasmia 6. IATROGENIC 7. IMMUNOLOGICAL Ø Anti sperm antibodies
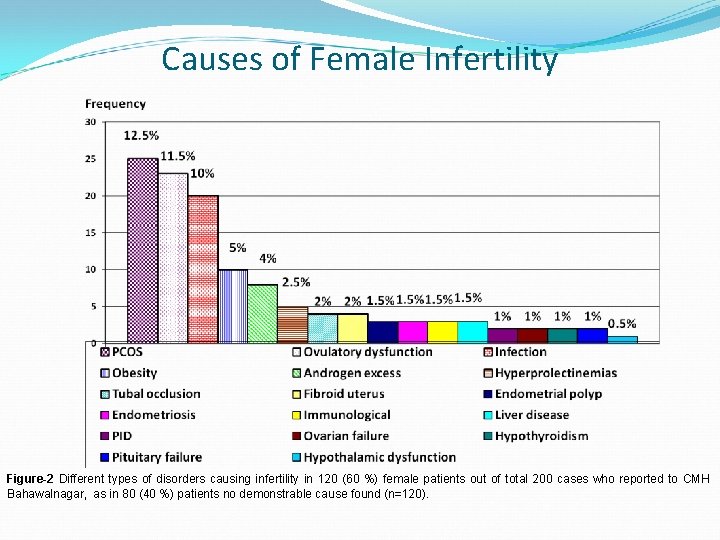
Causes of Female Infertility Figure-2 Different types of disorders causing infertility in 120 (60 %) female patients out of total 200 cases who reported to CMH Bahawalnagar, as in 80 (40 %) patients no demonstrable cause found (n=120).

EVALUATION OF FEMALE INFERTILITY 1) 2) 3) 4) 5) 6) Detailed history Physical examination PAP smear Search for tubal patency, endometriosis or adhesions Assessment of ovulation & adequate luteal function Endocrine parameters (serum FSH, LH, estradiol, progesterone, prolactin, TSH, free T 4, testosterone, DHEAS and 17 -OH -progesterone) 7) Immunological parameters (anti sperm antibody) 8) Genetic screening 9) Karyotyping

EVALUATION OF FEMALE INFERTILITY STEPS OF EVALUATION 1 DETAILED HISTORY • Irregular periods or no menstrual periods • Very painful periods • Endometriosis • Pelvic inflammatory disease • More than one miscarriage

1 DETAILED HISTORY (CONT) Many things can affect a woman's ability to have a baby. These include: • Age • Stress • Poor diet • Athletic training • Overweight or underweight • Smoking • Alcohol • STDs
2. PHYSICAL EXAMINATION • Body mass index (BMI): kg/m 2 • Weight change >10% within past year • Blood pressure • Body shape and stature • Abdominal scars • Abnormalities in body systems • Assessment of hirsutism • Assess secondary sex characteristics • Record Tanner stage for women not mature • Examine nipple discharge microscopically • Examine external genitalia for inflammation • Clitoral enlargement • Intact hymen • Pubic hair distribution

3. PAP SMEAR A papanicolaou cervical and vaginal smear (tumor of squamocoloumnar junction) Along with appropriate cervical and endocervical cultures (infections) 4. USG / HYSTEROSALPANGIOGRAM / LAPROSCOPY Ø If ovulation is normal, these tests are needed to search for tubal patency, endometriosis or adhesions Ø Performed between the 7 th and 11 th day of the cycle (hysterosalpangiogram)

5. ASSESMENT OF MENSTRUAL STATUS No amenorrhea or amenorrhea If no amenorrhea EVALUATION OF OVULATION Serum progesterone levels Measurement of midluteal (21 day of menses) serum progesterone If< 15 nmol/l anovulation or leuteal defect • If >30 nmol/l indicates normal ovulation Basal body temperature (rapid rise in body temperature by 0. 5ºF, persists through luteal phase) Evaluation of LH surge (LH appears in urine just after serum LH surge & 24 to 36 hrs before ovulation)

5. ASSESMENT OF MENSTRUAL STATUS (cont) If amenorrhea Rule out pregnancy by β - HCG For primary amenorrhea Asses karyotyping For secondary amenorrhea Perform estrogen / progesterone challenge test Abnormal result shows uterine disease
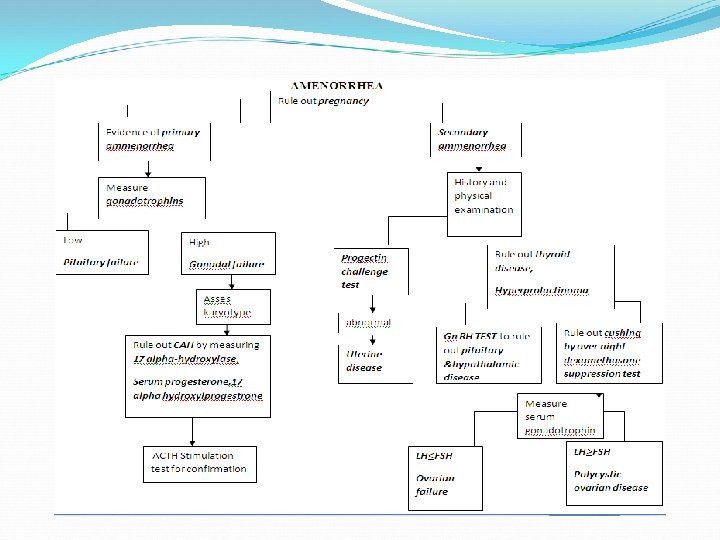

6. ENDOCRINE PARAMETERS Ø Female fertility profile (serum) FSH LH Estradiol (2 nd day of menses) Progesterone (21 day of menses) Prolactin Ø Gn. RH stimulation test Ø Other endocrine tests are TSH, f T 4 Testosterone & DHEAS (hirsutism) 17 -OH-progesterone (CAH) Ø Misc (plasma glucose )
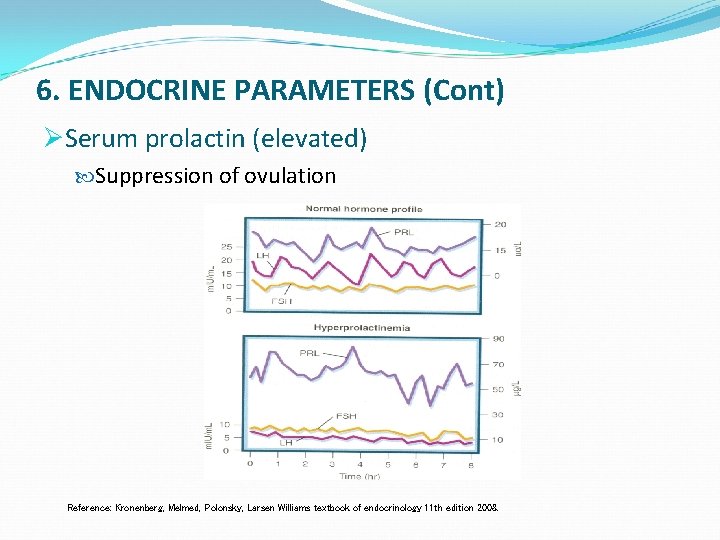
6. ENDOCRINE PARAMETERS (Cont) ØSerum prolactin (elevated) Suppression of ovulation Reference: Kronenberg, Melmed, Polonsky, Larsen Williams textbook of endocrinology 11 th edition 2008.

6. ENDOCRINE PARAMETERS (Cont) Ø If Serum estradiol is low (2 nd day of menses) a. HYPERGONADOTROPIC HYPOGONADISM Premature ovarian failure FSH > 20 m. IU/ml, estradiol < 73 pmol/L Relative ovarian age Ø Serum FSH (rise) Ø As FSH increases rate of successful pregnancies decreases Ø b. HYPOGONADOTROPIC HYPOGONADISM Serum FSH < 2 m. IU/m. L, LH < 2 m. IU/m. L, estradiol < 110 pmol/L (hypothalamic or pituitary insufficiency) Serum prolectin elevated TSH increase, f T 4 decrease (hypothyroidism)
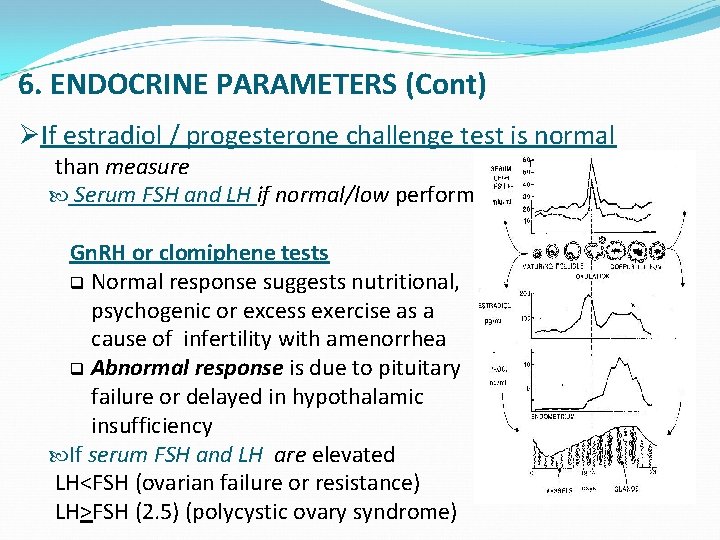
6. ENDOCRINE PARAMETERS (Cont) ØIf estradiol / progesterone challenge test is normal than measure Serum FSH and LH if normal/low perform Gn. RH or clomiphene tests q Normal response suggests nutritional, psychogenic or excess exercise as a cause of infertility with amenorrhea q Abnormal response is due to pituitary failure or delayed in hypothalamic insufficiency If serum FSH and LH are elevated LH<FSH (ovarian failure or resistance) LH>FSH (2. 5) (polycystic ovary syndrome)

7. ENDOCRINE PARAMETERS (Cont) Gn. RH stimulation test Ø Indication: To diagnose hypothalamic pituitary disease in precocious and delayed puberty in both sexes in children with low basal gonadotrophins Ø Procedure: 0 min: Take 3 ml blood for LH and FSH Inj Gn. RH 100 ug IV (child 2. 5 ug/kg body weight to max 100 ug) After 30 & 60 min : Take 3 ml blood for LH and FSH

7. ENDOCRINE PARAMETERS (Cont) Interpretation: In follicular phase; LH increases 2 fold over baseline or a net change of at least 10 m. IU/ml and FSH 1. 5 fold over baseline or a change of at least 2 m. IU/ml In luteal phase; LH increases 8 fold over baseline or a net change of 20 m. IU/ml and FSH 1. 5 fold over baseline or a net change of 2 m. IU/ml Reference: (Lufkin et al, 1983)

7. ENDOCRINE PARAMETERS (Cont) Clomiphene stimulation test Clomiphene acts by interrupting the negative feedback loop and thereby stimulating release of gonadotropin from pituitary Indication To diagnose hypothalamic pituitary disease in precocious and delayed puberty in both sexes in children with low basal gonadotrophins Procedure 100 mg of clomiphene citrate is given for 5 to 7 days Result A doubling of LH and a 20 to 50% increase in FSH are normal, indicative of an intact hypothalamic-pituitary response Santen RJ, Leonard JM, Sherins RJ, Gandy HM, Paulsen CA. Short- and long-term effects of clomiphene citrate on the pituitary-testicular axis. J Clin Endocrinol Metab. 1971; 33: 970 -979.
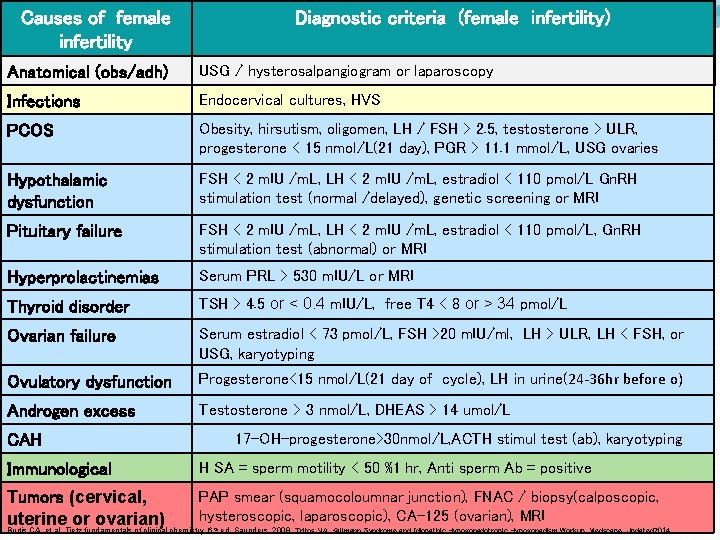
Causes of female infertility Diagnostic criteria (female infertility) Diagnostic criteria (Female Infertility) Diagnostic criteria (Fem Anatomical (obs/adh) USG / hysterosalpangiogram or laparoscopy Infections Endocervical cultures, HVS PCOS Obesity, hirsutism, oligomen, LH / FSH > 2. 5, testosterone > ULR, progesterone < 15 nmol/L(21 day), PGR > 11. 1 mmol/L, USG ovaries Hypothalamic dysfunction FSH < 2 m. IU /m. L, LH < 2 m. IU /m. L, estradiol < 110 pmol/L Gn. RH stimulation test (normal /delayed), genetic screening or MRI Pituitary failure FSH < 2 m. IU /m. L, LH < 2 m. IU /m. L, estradiol < 110 pmol/L, Gn. RH stimulation test (abnormal) or MRI Hyperprolactinemias Serum PRL > 530 m. IU/L or MRI Thyroid disorder TSH > 4. 5 or < 0. 4 m. IU/L, free T 4 < 8 or > 34 pmol/L Ovarian failure Serum estradiol < 73 pmol/L, FSH >20 m. IU/ml, LH > ULR, LH < FSH, or USG, karyotyping Ovulatory dysfunction Progesterone<15 nmol/L(21 day of cycle), LH in urine(24 -36 hr before o) Androgen excess Testosterone > 3 nmol/L, DHEAS > 14 umol/L 17 -OH-progesterone>30 nmol/L, ACTH stimul test (ab), karyotyping CAH Immunological H SA = sperm motility < 50 %1 hr, Anti sperm Ab = positive PAP smear (squamocoloumnar junction), FNAC / biopsy(calposcopic, Tumors (cervical, hysteroscopic, laparoscopic), CA-125 (ovarian), MRI uterine or ovarian) Burtis CA, et al. Tietz fundamentals of clinical chemistry, 6 ed. Saunders, 2008. Tritos NA. Kallmann Syndrome and Idiopathic Hypogonadotropic Hypogonadism Workup. Medscape. Updated 2014. th
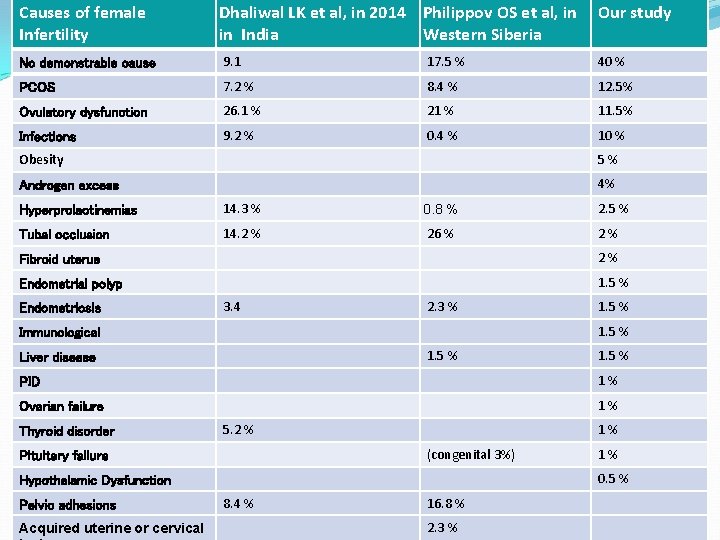
Causes of female Dhaliwal LK et al, in 2014 Philippov OS et al, in Our study Frequency of disorders leading to female infertility in literature Infertility in India Western Siberia No demonstrable cause 9. 1 17. 5 % 40 % PCOS 7. 2 % 8. 4 % 12. 5% Ovulatory dysfunction 26. 1 % 21 % 11. 5% Infections 9. 2 % 0. 4 % 10 % Obesity 5 % Androgen excess 4% Hyperprolactinemias 14. 3 % 0. 8 % 2. 5 % Tubal occlusion 14. 2 % 26 % 2 % Fibroid uterus 2 % Endometrial polyp 1. 5 % Endometriosis 3. 4 2. 3 % 1. 5 % Immunological 1. 5 % Liver disease 1. 5 % PID 1 % Ovarian failure 1 % Thyroid disorder 5. 2 % 1 % (congenital 3%) Pituitary failure 0. 5 % Hypothalamic Dysfunction Pelvic adhesions Acquired uterine or cervical 1 % 8. 4 % 16. 8 % 2. 3 %

RECOMMENDATIONS The prevalence of different conditions leading to infertility differ in various regions, and management depends on the cause It is vital to know the frequency of different causes of infertility in our setup

CONCLUSION Genital tract infection is the commonest cause of infertility, followed by varicocele and immunological causes in males PCOS is the commonest problem causing infertility, followed by ovulatory dysfunction, infection, obesity, androgen excess, endometriosis and hyperprolactinemias in females Estimation of semen analysis in male and fertility hormonal profile in female provides the basis for early diagnosis and better management of effected patients

Case - 1 A 19 yr old female. H/O amenorrhea, menarche at age 13 yr, regular menses till age 18 yr. O/E tense, anxious, thin, low weight 38 kg. Lab tests HCG < 5 m. Iu/m. L (Negative = <5) LH 1 m. IU/m. L (1. 7 – 15) FSH 2. 5 m. IU/m. L (1. 4 – 9. 9) E 2 95 pmol/l (73 – 550) PRL 450 m. IU/L (40 -530) MRI pituitary fossa (Normal)

Case - 1 Give Diagnosis? A. B. C. D. Prolectinoma Premature ovarian failure PCOS Hypogonadotropic hypogonadism (anorexia nervosa)

Case -1 Answer D Hypogonadotropic hypogonadism (anorexia nervosa)

Case - 2 A 27 yr old women. H/O amenorrhea, hirsutism, obesity, menarche at age 13 yr, regular menses till age 20 yr, over last 7 yr irregular menses (oligomen--). O/E overweight, acne. On USG bil cystic ovaries Lab tests LH 24 m. IU/m. L (1. 7 – 15) FSH 5. 5 m. IU/m. L (1. 4 – 9. 9) E 2 140 pmol/L (73 – 550) PRL 375 m. IU/L (40 - 530) Testosterone 3. 7 nmol/L (0. 7 – 2. 8)

Case - 2 What is diagnosis? A. POF B. PCOS C. CAH D. Liver disease

Case - 2 Answer B PCOS (LH/FSH ratio >2. 5, USG bil cystic ovaries, hyperandrogenism)

Case - 3 A 35 -year-old woman. H/O amenorrhea in the previous 6 months, menarche at age 12, two successful pregnancies. Provera (10 mg× 5 days) challenge with no subsequent withdrawal bleeding. She denied visual changes, hot flashes, or night sweats. No acne, hirsutism, or alopecia. She did describe galactorrhea, migraine headaches, which increased in frequency and intensity. Laboratory evaluation included HCG negative Prolactin 1050 m. IU/L (40– 530) FSH 3 m. IU/m. L (1. 4 – 9. 9) TSH 3 m. IU/L (0. 5– 5)

Case- 3 MRI of the pituitary fossa-- 2. 7 cm suprasellar mass, mild compression of the optic chiasm was noted The patient had transphenoidal surgery and subsequently received hormone replacement therapy but her menses did not resume. What is the best choice? A. Pituitary insufficiency B. Hypothalamic failure C. Amenorrhea was secondary effect of prolactin on ovaries D. Pituitary tumors within the pituitary gland can interfere directly with gonadotrope function by a mass effect

Case - 3 Answer D Pituitary masses can cause amenorrhea via a mass effect on the hypothalamus or pituitary stalk as in this case, via elevated prolactin levels, which result in decreased Gn. RH secretion, or through a mass effect on pituitary gonadotropes

Case - 4 Which of the following lab tests should you order when a patient presents with secondary amenorrhea? A. HCG B. Prolactin C. TSH D. FSH E. All of the above

Case - 4 Answer: E Pregnancy should always be a consideration in the workup of secondary amenorrhea, and it is important to rule out premature ovarian failure. Thyroid dysfunction (either hypo- or hyper-) can cause menstrual cycle abnormalities. Prolactin-secreting microadenomas frequently present in this age group in association with menstrual cycle abnormalities

Case-5 In a patient with amenorrhea and an elevated prolactin which of the following would be the next appropriate step? A. Treat with a dopamine against B. Perform a pituitary MRI C. Treat with an oral contraceptive pill D. Perform a mammogram E. Treat with hormone replacement therapy

Case - 5 Answer: B It is essential that a patient with a persistently elevated prolactin level have a neuroimaging study to rule out a large hypothalamic or pituitary tumor. Treatment with a dopamine agonist will mask the symptoms and needs to be reserved for use after the cause of the elevated prolactin has been ascertained. Oral contraceptives and hormone replacement will likewise obscure the problem and may mask the appropriate diagnosis

Case-6 How does hyperprolactinemia cause amenorrhea? A. Increases Gn. RH pulse frequency B. Decreases Gn. RH pulse frequency C. Blocks estrogen binding to estrogen receptor D. Accelerates estrogen metabolism

Case - 6 Answer: B Hyperprolactinemia can interfere with normal LH and FSH secretion by decreasing Gn. RH pulse frequency

Case-7 Which of the following hypothalamic-pituitary disorders can cause secondary amenorrhea? A. Hemochromatosis B. Lymphocytic hypophysitis C. Sheehan’s syndrome D. Sarcoidosis E. All of the above

Case - 7 Answer: E All of the options presented can cause hypothalamic or pituitary dysfunction and result in secondary amenorrhea

Case - 8 A 31 -year-old woman. H/O infertility for 2 -year, menarche at age of 12 years and regular cycles with intermittent development of ovarian cysts. The cysts were treated with oral contraceptive pills (OCPs) from age 24 to 26 yrs. She became amenorrheic after discontinuing the OCPs 5 years ago. She noted very occasional hot flashes. Her past medical history was remarkable for hypothyroidism, diagnosed at age 11 years, for which she took thyroid hormone replacement O/E no vitiligo, hirsutism, acne or acanthosis, normal peripheral visual fields, a 10 -g thyroid, no galactorrhea, and slightly enlarged ovaries

Case - 8 Laboratory evaluation TSH 2. 27 m. IU/L (0. 5– 5) Prolactin 320 m. IU/L (40– 530) HCG negative FSH 19. 9 m. IU/m. L ( 1. 4 – 9. 9) Estradiol < 73 pmol/L (73 – 550) Inhibin B level was very high at 1000 pg/m. L (follicular phase average 173 pg/m. L). An ultrasound demonstrated multiple ovarian cysts bilaterally (1 of 10 mm, 3 of 12 mm, and one each at 17, 20, 22, and 30 mm)

Case - 8 MRI demonstrated a normal pituitary gland The patient underwent several cycles of ovulation induction using a combination of purified LH and FSH, also treated with estradiol and cyclic progesterone for hormone replacement. The patient subsequently developed achy joints and a positive antinuclear antibody. Ten years later, the patient developed darkening of the skin and extreme fatigue. ACTH stimulation test demonstrated baseline cortisol 108 nmol/L, which was unchanged 1 hour after 250 ug ACTH analogue. Adrenocorticotropin (ACTH) was elevated at 176 pmol/L. She was treated with prednisone and fludrocortisone

Case - 8 What is the most likely cause of infertility? A. Hypothyroidism B. PCOS C. Addison disease D. Pituitary adenoma E. Autoimmune ovarian failure

Case - 8 Answer E The patient has polyglandular failure type II with autoimmune ovarian failure

Case-9 Which test results are consistent with premature ovarian failure? A. FSH 3. 2 m. IU/m. L, LH 0. 6 m. IU/m. L, estradiol <73 pmol/L B. FSH 68 m. IU/m. L, LH 57 m. IU/m. L, estradiol < 73 pmol/L C. FSH 9 m. IU/m. L, LH 56 m. IU/m. L, estradiol 164 pmol/L D. FSH 25 m. IU/m. L, LH 80 m. IU/m. L, estradiol 1095 pmol/L

Case - 9 Answer: B Results in A are consistent with hypothalamic amenorrhea, results in C are consistent with polycystic ovary syndrome, and results in D are typical day of the LH surge in a normal menstrual cycle

Case - 10 When the diagnosis of premature ovarian failure is made, which additional tests should be ordered? A. Karyotyping B. Fragile X premutation screen C. Adrenal autoantibodies D. Thyroid autoantibodies E. All of the above

Case - 10 Answer: E All of these tests are important after an initial diagnosis has been made

Case -11 A 56 -year-old postmenopausal woman presents with a history of mild hypertension and a 6 -month history of significant frontal alopecia, hirsutism (Ferriman- Gallwey score 22) and deepening of her voice. What are the most important initial test(s)? A. Total testosterone and urinary 17 -ketosteroids B. Free testosterone C. Dexamethasone suppression test D. Total testosterone and insulin-like growth factor I (IGF-I)

Case - 11 Answer: A The development of hyperandrogenic symptoms in a postmenopausal woman raises concerns for an androgensecreting tumor of the ovary or, less commonly, the adrenal. In this woman other concerning signs for significant hyperandrogenism include deepening of the voice and the rapid progression of symptoms. The most useful initial tests in this instance are a total testosterone and urinary 17 -ketosteroids. Ovarian tumors or other pathologic processes cause secretion of testosterone, while adrenal tumors often secrete androgen precursors that are detected as 17 -ketosteroids. Some adrenal tumors make only testosterone

Case - 12 A 36 -year-old woman with a 5 -year history of oligomenorrhea, 15 -lb centripetal weight gain, treated hypertension, impaired glucose tolerance, polycystic ovary morphology on ultrasound, complains of hirsutism, increased edema and bruising. What is the most appropriate diagnostic test to perform? A. DHEAS B. 24 -hour urine free cortisol C. 17 -hydroxyprogesterone D. TSH

Case - 12 Answer: B In this patient with hirsutism, the signs and symptoms suggest the presence of Cushing’s syndrome. An overnight dexamethasone test or a 24 -hour urine free cortisol are the best screening tests

Case - 13 A 22 -year-old college student (BMI 24) is diagnosed with PCOS based on a history of amenorrhea and biochemical hyperandrogenemia. Clinically she has mild acne on her face. She is not currently interested in pregnancy and is sexually active. What is the most appropriate first-line treatment option? A. Lifestyle changes B. Metformin 500 mg t. i. d. C. Oral contraceptives D. Medroxyprogesterone 5 mg daily for 14 days per month E. Spironolactone 100 mg daily

Case - 13 Answer: C In this hyperandrogenic patient who is sexually active, management of cycle irregularity and acne can most easily be accomplished using oral contraceptives. Oral contraceptives both suppress gonadotropin stimulation of ovarian androgen secretion and increase sex hormone– binding globulin, therefore decreasing circulating free testosterone

Case-14 A 49 -year-old woman, increased hair growth for the past 6 months that started abruptly; she has male pattern hair loss, as well. O/E, she has temporal loss of hair and clitorimegaly. Lab tests: Testosterone 12. 5 nmol/L (0. 7 – 2. 8) FSH 12 m. IU/m. L (1. 4 – 9. 9) LH 9 m. IU/m. L (1. 7 – 15) Normal prolactin level

Case - 14 The next step in the evaluation is one of the following? A. DHEAS level B. Repeat FSH and LH levels C. Fasting blood sugar level D. Fasting lipid level E. Computed tomography of adrenal and ovaries

Case - 14 Answer E Computed tomography of adrenal and ovaries (as testosterone is > 7 nmol/L)

Case - 15 A 37 yr old women with a history of gonococcal salpingitis presents with her spouse for evaluation of infertility. What study is most indicated on the initial evaluation? A. Basal body temperature record B. Semen analysis C. Hysterosalpingogram D. Endometrial Biopsy E. A, B & C

Case - 15 Answer E Without evidence of anovulation the endometrial bx is not indicated. The couple should have A, B, and C

THANK YOU Dr. Sarma 100
- Slides: 74