Diseases of the Periradicular Tissues 1 Acute alveolar































































- Slides: 71


Diseases of the Periradicular Tissues: 1. Acute alveolar abscess 2. Acute apical periodontitis - Vital - Nonvital 3. Acute exacerberation of a chronic lesion

4. Chronic periradicular diseases with areas of rarefaction a. Chronic alveolar abscess b. Granuloma c. Cyst 5. Condensing osteitis 6. External root resorption 7. Diseases of the periradicular tissue of non endodontic origin

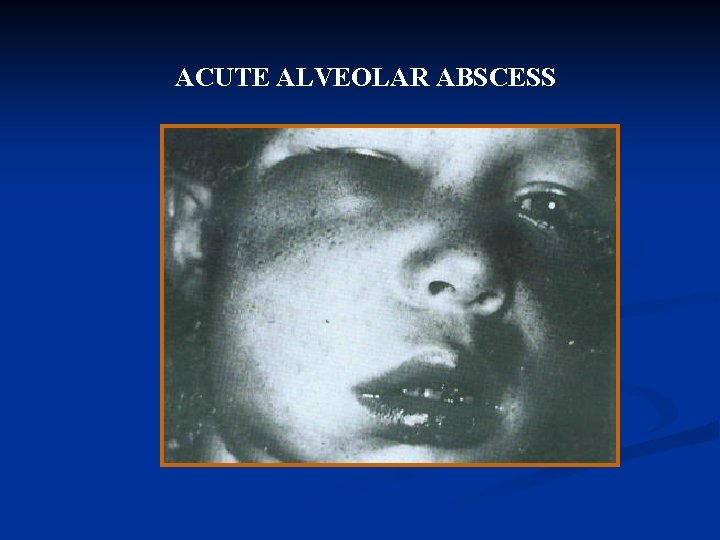
ACUTE ALVEOLAR ABSCESS

Definition: An acute alveolar abscess is a localized collection of pus in the alveolar bone at the root apex of a tooth following death of pulp

Symptoms: Initially slight tenderness of the tooth. Later - severe throbbing pain, swelling of the overlying soft tissues.

As the infection progresses- and extends beyond the original site. painful, becomes more tooth The elongated, and mobile. while the adjacent tissue continuous to swell.

osteitis, periostitis, cellulitis, or osteomyelitis. The contained pus may break through to form a sinus tract, usually opening in the labial or buccal mucosa. such as the skin of the patient’s face or neck, or even the antrum or nasal cavity.

ulting becomes swelling extensive, the When cellulitis may distort the patient’s appearance grotesquely.

The patient may appear pale, irritable and weakened from pain and loss of sleep. Patients with mild cases may have only a slight rise in temperature (90 to 1000 F).


Diagnosis: In the early stages, it may be difficult to locate the tooth because of the absence of clinical signs and the presence of diffuse, annoying pain.

1. Diagnosis by EPT and by thermal tests – No response 2. The tooth may be tender to percussion in late stages, 3. Pain during mastication 4. The apical mucosa is tender to palpation, 5. The tooth may be mobile and extruded. 6. A radiograph may help one to determine the tooth affected by showing a cavity, a defective restoration, thickened periodontal ligament space,

Differential Diagnosis: Acute alveolar abscess should be differentiated from periodontal abscess and from irreversible pulpitis. A periodontal abscess is an accumulation of pus along the root surface of a tooth that originates from infection in the supporting structures of the tooth.

§ manifested by swelling and mild pain. § Aperiodontalabscessisgenerallyassociatedwith vital rather than with pulp less teeth,

Treatment: Treatment consists of establishing drainage and controlling the systemic reaction. When symptoms have subsided, the tooth has been left open for drainage, one must perform careful and through debridement by instrumentation and irrigation before medicating and sealing the root canal. Once the root canal is sealed, endodontic treatment is completed

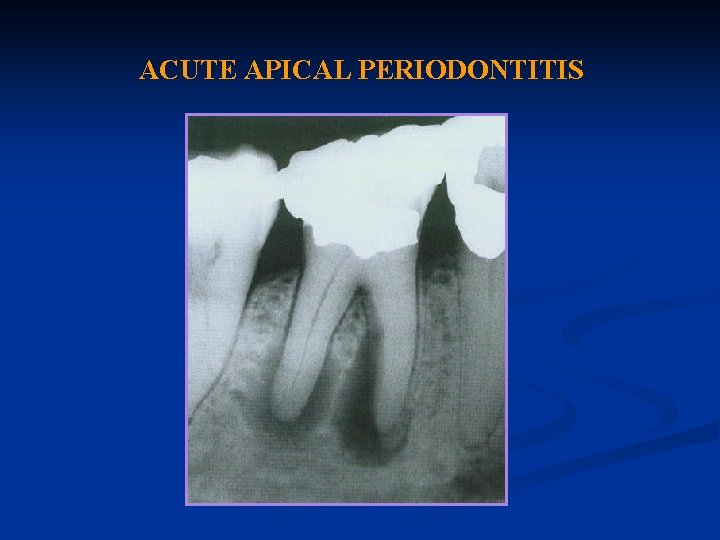
ACUTE APICAL PERIODONTITIS

Acute Apical Periodontitis: Definition Acute apical periodontitis is a painful inflammation of the periodontium as result of trauma, irritation, or infection through the root canal, regardless of whether the pulp is vital or nonvital.

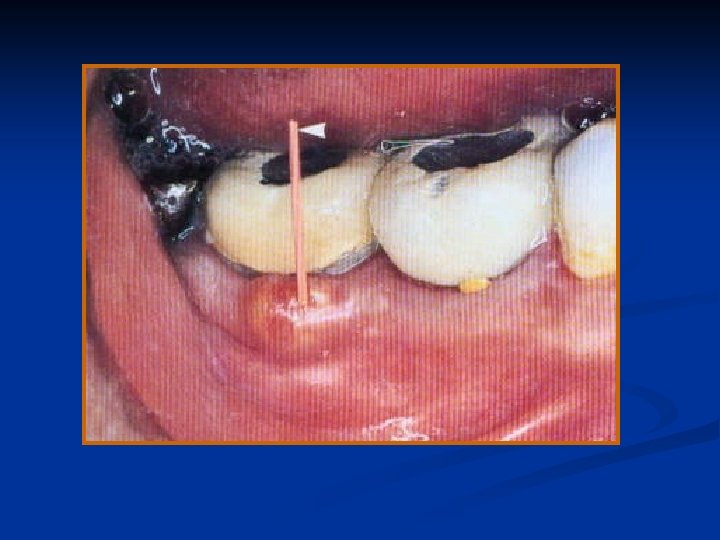
Cause: Cause A. Vital tooth ØThat has experienced occlusal trauma caused by abnormal occlusal contacts, Ø the occlusal plane, ect ween gn ahe hwedging Ø of By such as a toothpick,

B. Nonvital Ø diseases. the diffusion of bacteria and noxious products from an inflamed or Ø Or may be iatrogenic necrotic pulp,

Symptoms: 1. Pain and tenderness of the tooth. slightly some sore, be when times 2. tooth only may The it is percussed in a certain direction, or the soreness may be severe. 3. The tooth may be extruded, making closure painful.

Diagnosis: The diagnosis is frequently made from a known history of a tooth under treatment. The tooth is tender to percussion or slight pressure, whereas the mucosa overlying the root apex may or may not be tender to palpation.

Differential Diagnosis: A differential diagnosis should be made between acute apical periodontitis and acute alveolar abscess. at times, the difference is only of degree because acute alveolar abscess represents a further stage in development,

Treatment: Treatment of acute apical periodontitis consists of determining the cause and relieving the symptoms. When the acute phase has subsided, the tooth is treated by conservative means.

Acute Exacerbation of a chronic Lesion: Phoenix abscess

Acute Exacerbation of a chronic Lesion: Synonyms: Phoenix Abscess. Definition: Definition This condition is an acute inflammatory reaction superimposed on an existing chronic lesion, such as a cyst or granuloma.

Cause: Chronic periradicular diseases, such as granulomas and cysts, are in a state of equilibrium, so these apical reactions are completely asymptomatic.

At times, because of bacteria and their toxins, these apparently dormant lesions may react and may cause an acute inflammatory response.

Symptoms : At the onset, the tooth may be tender to the touch. As inflammation progresses, the tooth may be elevated in its socket and may become sensitive. The mucosa over the radicular area may be sensitive to palpation and may appear red and swollen.

Diagnosis: The exacerbation of a chronic lesion is most commonly associated with the initiation of root canal therapy in a completely asymptomatic tooth. In such a tooth, radiographs show well-defined periradicular lesions.

Lack of response to vitality tests points to a diagnosis of necrotic pulp, although, on rare occasions, a tooth may respond to the electric pulp test because of fluid in the root canal; or in a multirooted tooth.

DIFFERENTIAL DIAGNOSIS

Differential Diagnosis: An acute exacerbation of a chronic lesion causes symptoms similar to those of an acute alveolar abscess. Because the treatment of both lesions is the same, no differential diagnosis is needed.

Treatment: The treatment of acute exacerbation of a chronic lesion, which is an emergency, is the same as that of an acute alveolar abscess. Prognosis: The prognosis for the tooth is good once the symptoms have subsided.

CHRONIC PERIRADICULAR DISEASES WITH AREAS OF RAREFACTION These diseases are - Chronic alveolar abscess. - Granuloma, and - Radicular cyst.

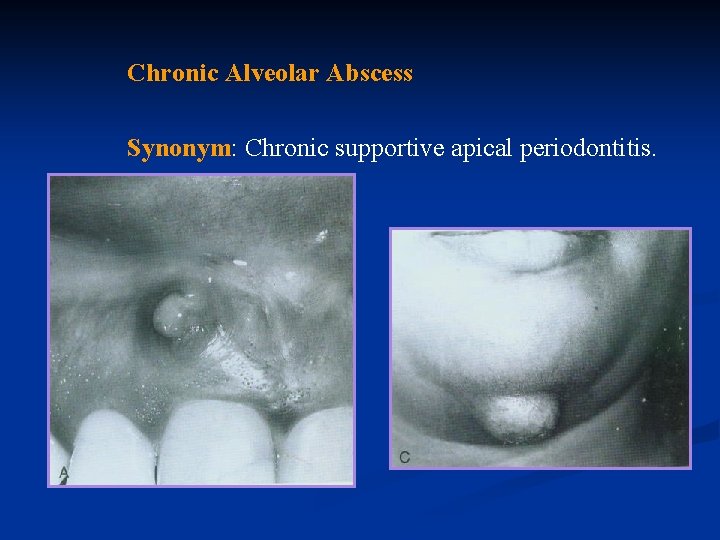
Chronic Alveolar Abscess Synonym: Chronic supportive apical periodontitis.

Definition: A chronic alveolar abscess is a long-standing, low –grade infection periradicular alveolar bone. The source of the infection is in the root canal.

Cause: Chronic alveolar abscess is a natural sequela of a death of the pulp with extension of the infective process periapically, or it may result from a pre-existing acute abscess.

Symptoms: A tooth with chronic alveolar abscess is generally asymptomatic; at times, such an abscess is detected only during routine radiographic examination or because of the presence of a sinus tract.


Diagnosis: A chronic abscess may be painless or only mildly painful. At times, the first sign of osseous breakdown is radiographic evidence seen during routine examination or discoloration of the crown of the tooth.

When asked, the patient may remember a sudden, sharp pain that subsided and has not recurred, or he may relate a history of traumatic injury. The tooth does not react to the electric pulp test or to thermal tests.

As a result, a proper and accurate diagnosis can be made only when tissue specimen has been examined microscopically Differential Diagnosis: A chronic abscess should be differentiated from cementoma or ossifying fibroma, which is associated treatment. with a vital tooth and requires no endodontic

Treatment: Treatment consists of elimination of infection in the root canal.

GRANULOMA: Definition: A dental granuloma is a growth of granulomatous tissue continuous with the periodontal ligament resulting from death of the pulp and the diffusion of bacteria and bacterial toxins from the root canal in to the surrounding periradicular tissues through the apical and lateral foramina.

A granuloma may be seen as a chronic, low-grade defensive reaction of the alveolar bone to irritation from the root canal.

Cause: The cause of the development of a granuloma is death of the pulp, followed by a mild infection or irritation of the periapical tissues that stimulates a productive cellular reaction. A granuloma develops only some time after the pulp has died.

Symptoms: A granuloma may not produce any subjective reaction, except in rare cases when it breaks down and undergoes supuration. Usually, a granuloma is asymptomatic

Diagnosis: The presence of a granuloma, which is symptomless, is generally discovered by routine radiographic examination. The area of rarefaction is well defined, with lack of continuity of the lamina dura

Differential Diagnosis: A granuloma cannot be differentiated from other periradicular diseases unless the tissue is examined microscopically.

Treatment: Root canal therapy may suffice for the treatment of a granuloma.

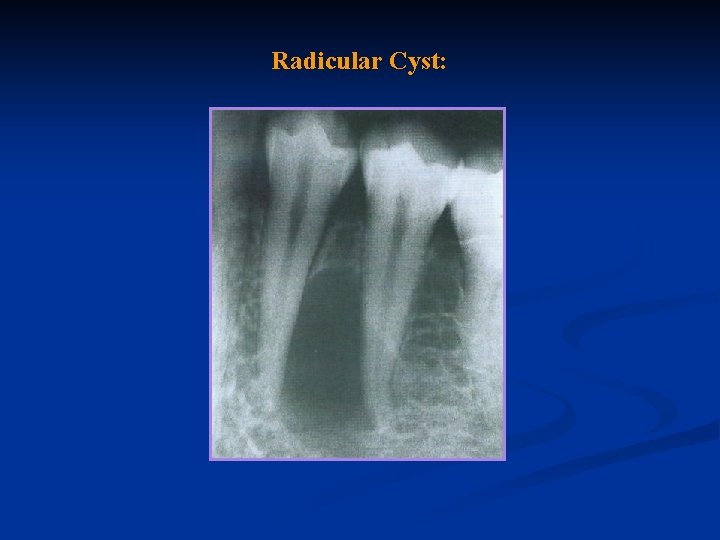
Radicular Cyst:

Definition: A cyst is a closed or sac internally lined with epithelium, the center of which is filled with fluid or semisolid material. A radicular or alveolar cyst is a slowly growing sac at the apex of a tooth that lines a pathologic cavity in the alveolar bone.

Cause: A radicular cyst presupposes physical, chemical, or bacterial injury resulting in death of the pulp, followed by stimulation of the epithelial rests of Malassez, which are normally present in the periodontal ligament: Symptoms: No symptoms are associated with the development of a cyst,

A cyst may become large enough, however, to become obvious as a swelling. The presence of the cyst may be sufficient to cause movement of the affected teeth, owing to accumulation of cystic fluid. In such cases, the root apices of the involved teeth become spread apart, so the crowns are forced out of alignment. The teeth may also become mobile. If left untreated, a cyst may continue to grow at the expense of the maxilla or the mandible.

Diagnosis: The pulp of a tooth with a radicular cyst does not react to electrical or thermal stimuli, and results of other clinical tests are negative, except the radiograph. The radiolucent area is generally round in outline, except where it approximates adjacent teeth, in which case it may be flattened and may have an oval shape. Neither the size nor the shape of the rarefied area is a definitive indication of a cyst

Differential Diagnosis: A cyst is usually larger than granuloma and may cause the roots of adjacent teeth to spread apart because of continuous pressure from accumulation of cystic fluid.

Treatment: Resolution of these areas of rarefaction occurs following root canal therapy in 80 to 98% of cases. Prognosis: The prognosis depends on the particular tooth, the extent of bone destroyed, and the accessibility for treatment

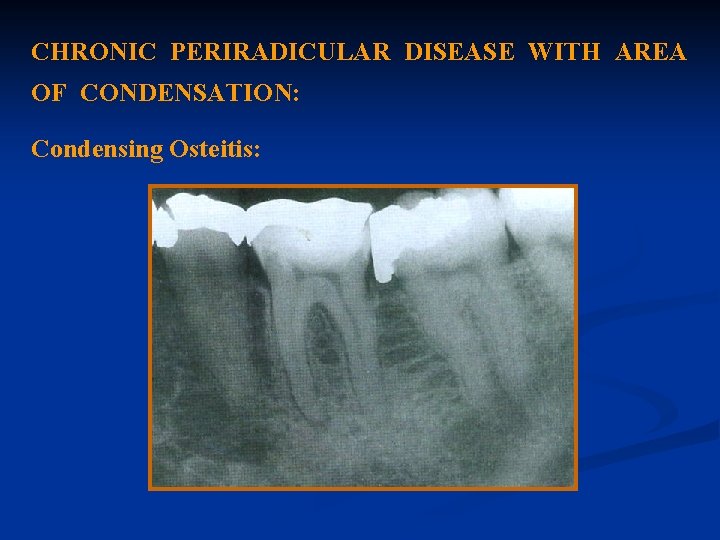
CHRONIC PERIRADICULAR DISEASE WITH AREA OF CONDENSATION: Condensing Osteitis:

Definition: Condensing osteitis is the response to a low-grade, chronic inflammation of the periradicular area as a result of a mild irritation through the root canal.

Cause: Condensing osteitis is a mild irritation from pulpal disease that stimulates osteoblastic activity in the alveolar bone. Symptoms: This disorder is usually asymptomatic. It is discovered during routine radiographic examination.

Diagnosis: The diagnosis is made from radiographs. Condensing osteitis appears in radiographs as a localized area of radiopacity surrounding the affected root.

Treatment: Endodontic treatment is indicated. Prognosis: The prognosis for long-term retention of the tooth is excellent if root canal therapy is performed and if the tooth is restored satisfactorily.

External Root Resorption: Definition: External resorption is a lytic process occurring in the cementum or cementum and dentin of the roots of teeth. Cause: Although unknown, the suspected cause of external resorption is periradicular inflammation due to trauma.

Symptoms: Throughout its development, external root resorption is asymptomatic. When the root is completely resorbed, the tooth may become mobile. If the external root resorption extends into the crown. It will give the appearance of “pink tooth” seen in internal resorption

Diagnosis: External resorption is usually diagnosed by radiographs.

Differential Diagnosis: External resorption needs to be differentiated from internal resorption. In external resorption, the radiograph shows a blunting of the apex, a ragged area, a “scooped – out” area on the side of the root, or, if the area is superimposed on the root canal, the root canal clearly traverses the area of resorption.

Treatment: Internal resorption ceases when the pulp is removed or becomes necrotic Prognosis: The prognosis of a tooth with external resorption is guarded. If the etiologic factor is known and it is removed, the resorptive process will stop, but it may leave a weak tooth unable to sustain functional forces.

Diseases of the Periradicular Tissues of Nonendodontic Origin: Periradicular lesions not only arise as extensions of pulpal diseases, but they may also originate in the remnants of odontogenic epithelium. Such lesions may be manifestations of systemic diseases, such as multiple neurofibromatosis or they may have other causes, such as periodontal diseases.

