Diseases of pleura Beatrix Blint MD SZTE Szeged

Diseases of pleura Beatrix Bálint MD. SZTE Szeged, 2017.
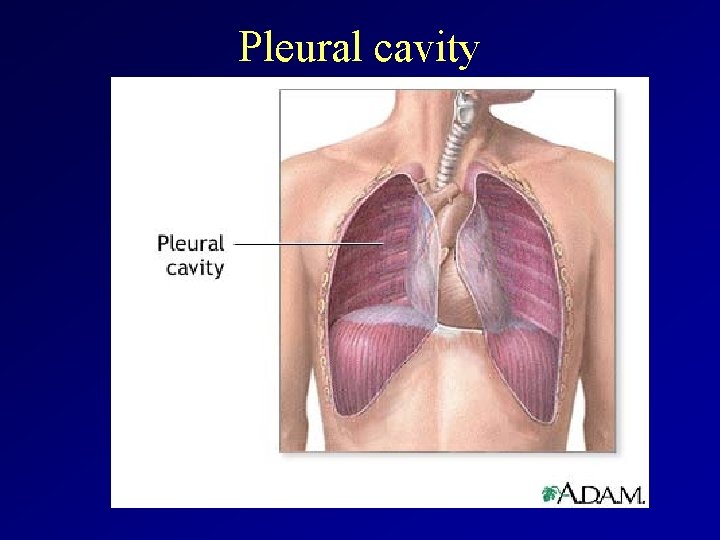
Pleural cavity
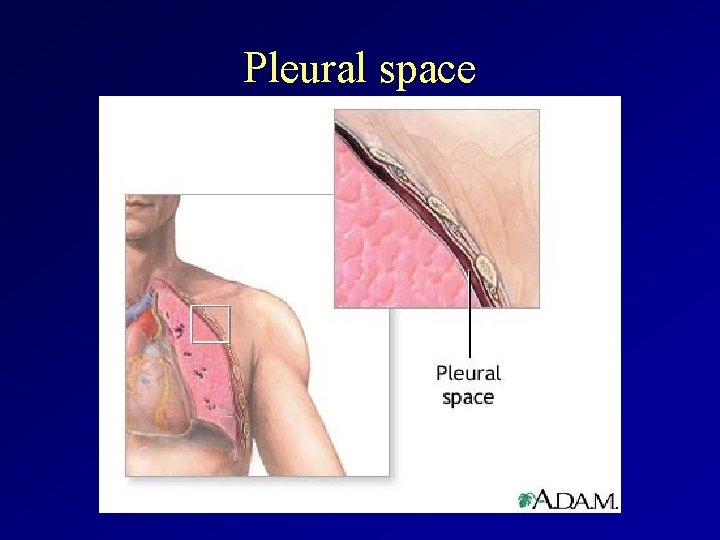
Pleural space

Diseases of pleura • Inflammation = pleurisy • Pneumothorax • Tumor

Inflammation of pleura • 1. Pleuritis sicca – Cause: viral infection • Bornholm’s disease (Coxsackie B) – Symptomes: • Pleuritic chest pain • Pleural friction rub – Therapy: • symptomatical

• 2. Pleural effusion: aetiology: multifactorial – Symptomes • Chest pain • Dyspnoe • Cough – Physical examination • Percussion note: dull • Auscultation: diminished/absent breath sounds – X-ray • Small fluid: blunting of costo-phrenic angle • Larger volume (>300 ml): homogenous shadow – Therapy • Thoracocentesis • To treat the cause of the pelural effusion

Pleural effusion Definition: An accumulation of fluid between the layers of the membrane lining the lung and the chest cavity. Alternative names: Fluid in the chest; Transudative pleural effusion; Exudative pleural effusion Causes: Pleural fluid is normally formed in small amounts to lubricate the surfaces of the "pleura, " the thin membrane that lines the chest cavity and surrounds the lungs. A "pleural effusion" is an abnormal collection of this fluid.
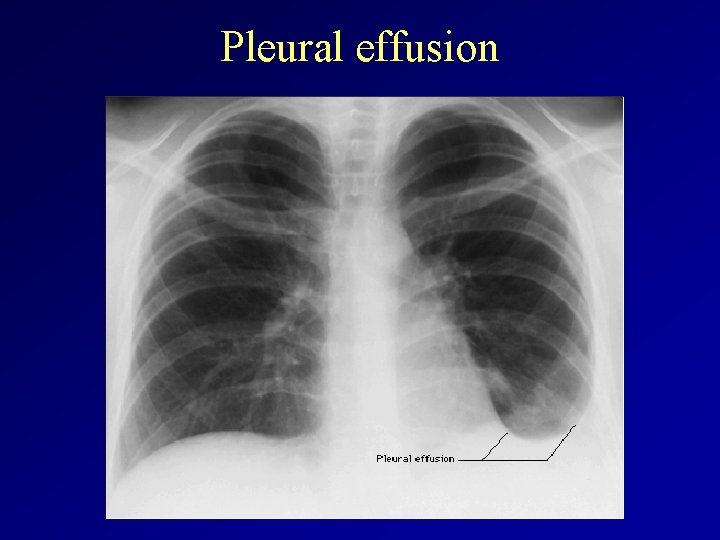
Pleural effusion
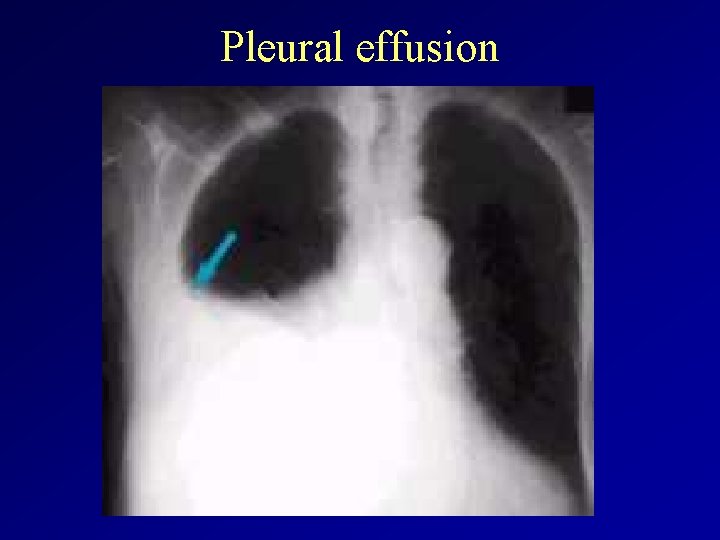
Pleural effusion
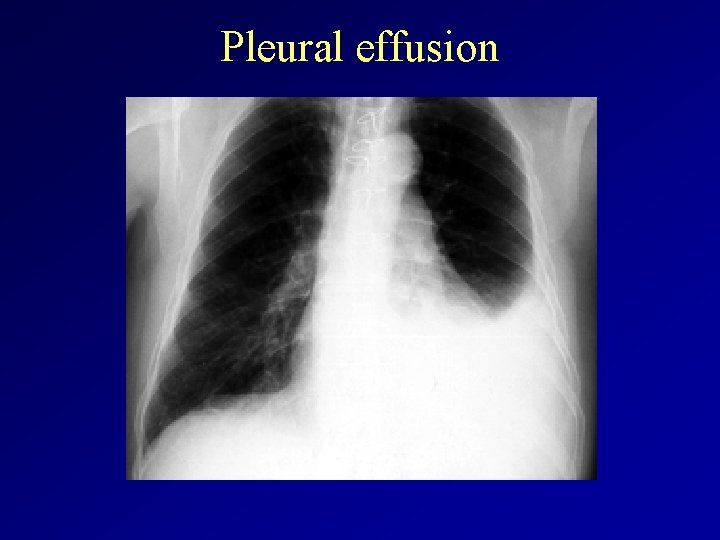
Pleural effusion
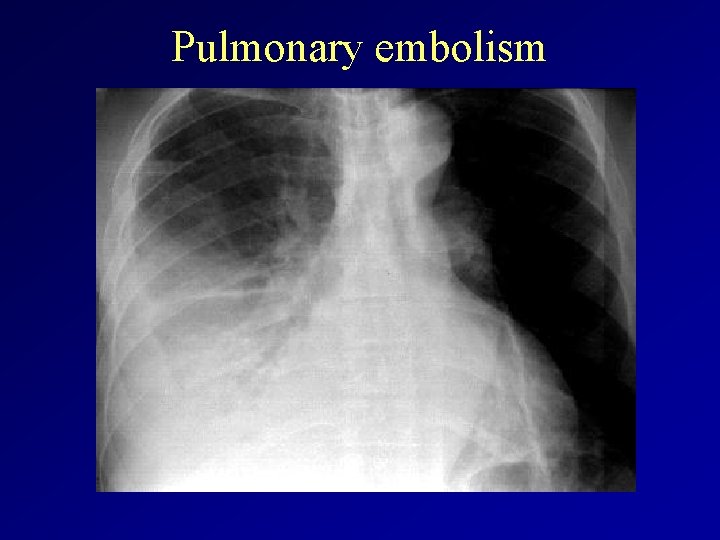
Pulmonary embolism

Pathophysiology of pleural effusion • of pulm. capill. wedge pressure: cong. heart failure • onc. pressure in microvas. circulation: low Se albumin • in pressure in the pelural space: lung collapse due to ptx • permeability of microvasc. circ. : due to inflam. mediators • Impaired lymphatic drainage from pl. space: due to tu / fibrosis • Occlusion of pariet. pleura stomata with fibrin, debris and mesoth. swellings: due to pneumonia • Movement of fluid from peritoneal space through diaphr. lymph. / diaphr. defect

Thoracocentesis Definition: A procedure to remove fluid from the space between the lungs and the wall of the chest. How to prepare for the test: No special preparation is needed before the procedure. A chest X-ray is may be performed before and after the test. Do not cough, breathe deeply, or move during the test to avoid injury to the lung. Risks: pneumothorax (collapse of the lung), fluid re-accumulation, pulmonary edema, bleeding, infection, and respiratory distress.
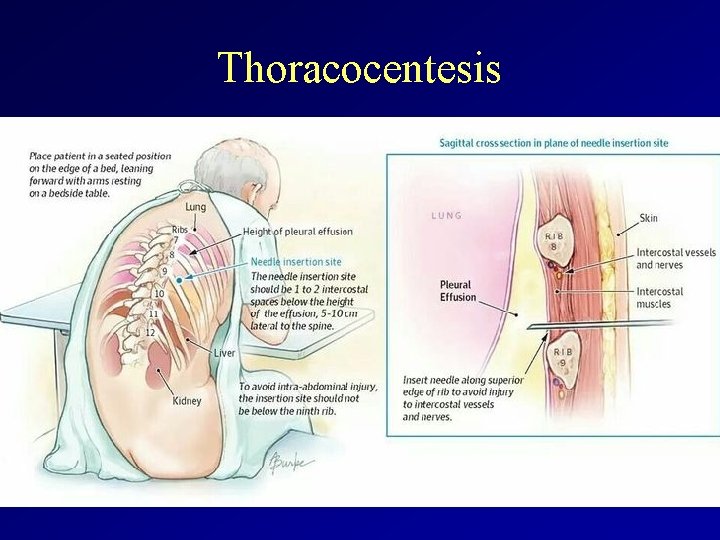
Thoracocentesis
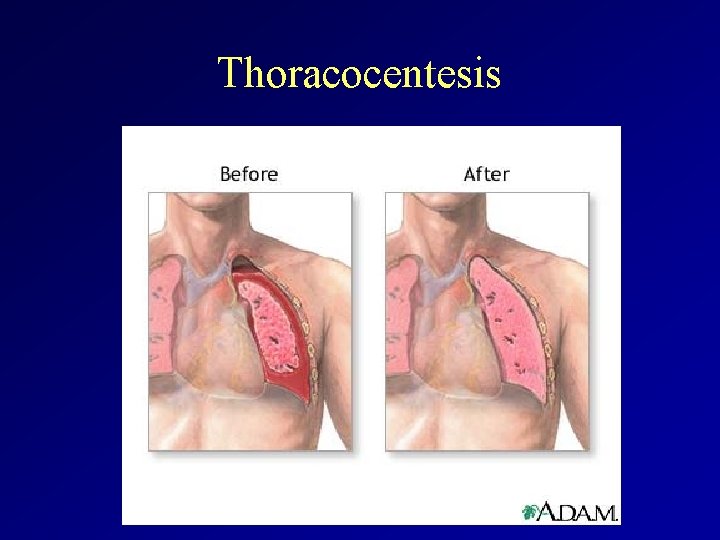
Thoracocentesis

Pleural effusion: analysis • Quantity • Quality: color, density, opacity • Lab. analysis – Chemical – Cytological – Bacteriological: culture • Spec • Aspec.
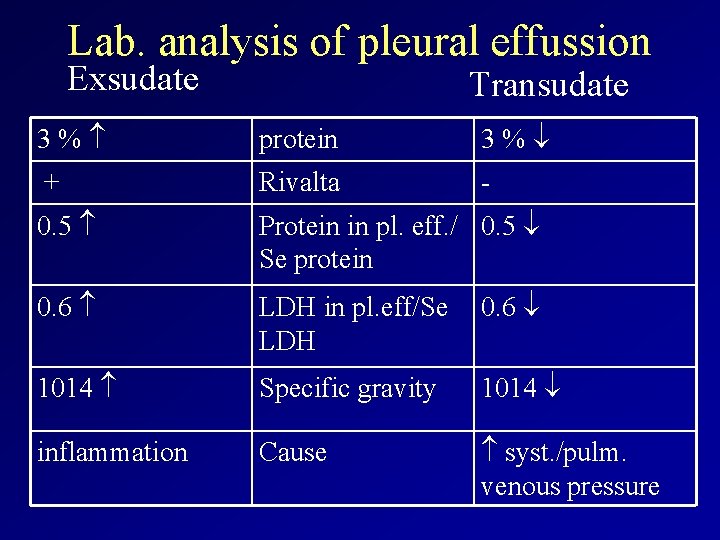

Lab. analysis of pleural effussion Exsudate Transudate 3 % protein 3 % + Rivalta - 0. 5 Protein in pl. eff. / 0. 5 Se protein 0. 6 LDH in pl. eff/Se 0. 6 LDH 1014 Specific gravity 1014 inflammation Cause syst. /pulm. venous pressure

Common Causes of Exudative Effusion Tuberculosis Lung cc Pneumonia Pulm. Infarction Lymphoma Metastatic tumor Mesothelioma Trauma Unilateral Bloody, large, parenchymal lesion on the X-ray, rapid. Reprod. X-ray: infiltr. Bloody, pleural pain E. g. : Hodgkin disease, +mediast. Lg. Large, rapid. Reprod. Bloody, Large, rapid. Reprod. Bloody

Common Causes of Transudative Effusion Congestive heart failure Bilateral Cirrhosis Ascites, Se protein low, usually on the right side Nephrotic syndrome Hypoproteinaemia, Generalized oedema, ascites
• Empyema = pus in the pleural space – Causes: bacteria: Streptococcus pneumoniae, Staphylococcus aureus, Klebsiella pn, E. Coli, Mycobact. Tb, anaerobic bact. – Risk factors: alcoholism, drug use, HIV infection, neoplasm, pre-existent pulmonary disease – Appear: as the complication of bacterial pneumonia, subdiaphragmatic abscess, oesophageal perforation, following thoracic surgery – Symptomes: • • • Chest pain Dyspnoe Cough Fever Night sweats Weight loss

Empyema diagnosis and therapy – Physical examination: Signs of pleural fluid • Percussion note: dull • Auscultation: diminished/absent breath sounds – X-ray: Signs of pleural fluid – Ultrasonography – CT, MRI – Thoracocentesis: pus! – Therapy • prompt chest tube drainage (drainage of pleural space) – Video-assisted thoracoscopic surgery (VATS) is used as a first-line therapy in many hospitals, although open thoracic drainage remains a frequently used alternative technique. • Antibiotics iv. based on Gram stain or culture • In case of uneffective th or recurrent empyema and pleural thickening, which may lead to functional lung impairment: surgical decortication.
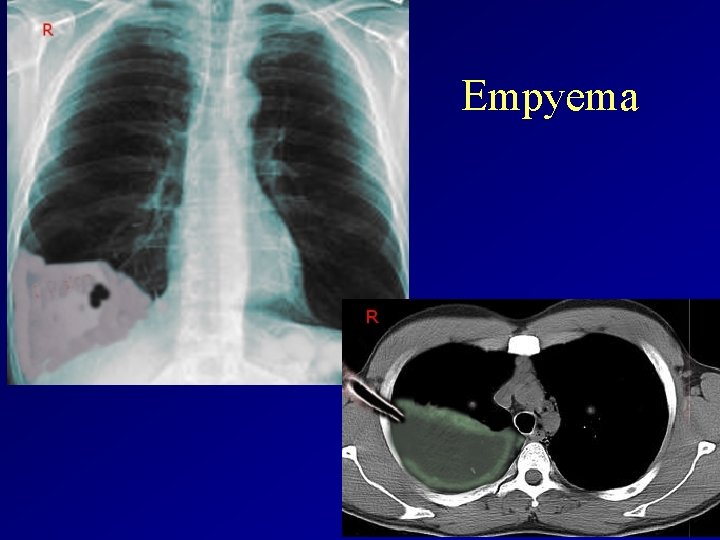
Empyema
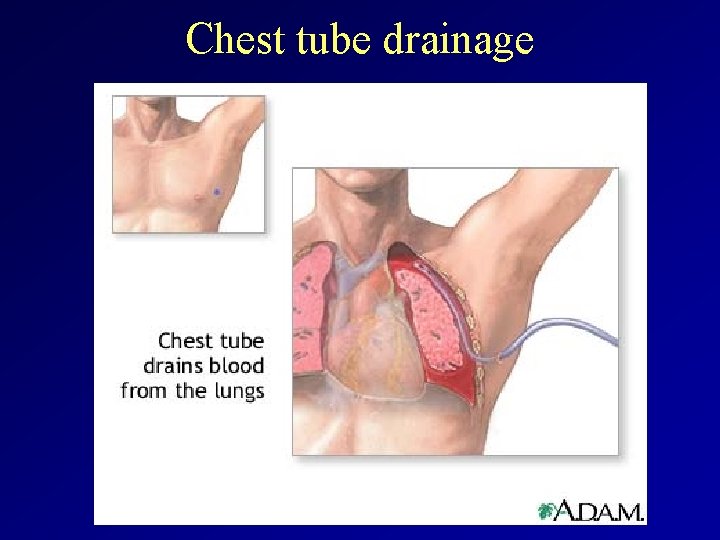
Chest tube drainage
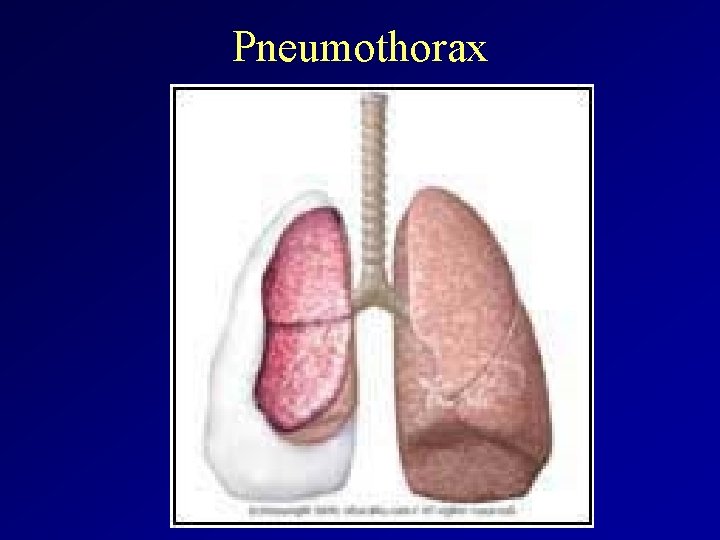
Pneumothorax

II. Pneumothorax • Air in the pleural space causing partial or complete lung collapse. • It can occur spontaneously or result from trauma or medical procedures. • Diagnosis is based on clinical criteria and chest x-ray. • Symptomes: chest pain, dyspnoe depending on the size of pneumothorax • Physical signs – Percussion note: Hyperresonance – Breath sounds: diminished/absent

Potential causes of pneumothorax • Air: from the airways – Idiopathic – Rupture of oesophagus – COPD – Pos. pressure ventillation – Infection, tumor, foreign body • Air: outside the chest wall – Trauma – Thoracocentesis, pleural biopsy, TTB – Insertion of venous catheter

Pneumothorax diagnosis and therapy • X-ray: upright inspiratory chest x-ray. – visible pleural edge with no lung markings between this edge and the chest wall – shrunken lobe or lung and the parietal pleura are diagnostic of pneumothorax. – Tracheal deviation and mediastinal shift occur with large pneumothoraces. • Therapy: depends on the size of the ptx – small: supplemental oxigen th, close observation, suction of the air by needle – large: consant tube drainage – Recurrent ptx: • Pleurodesis, • VATS (Video-assisted thoracoscopic surgery), • surgery
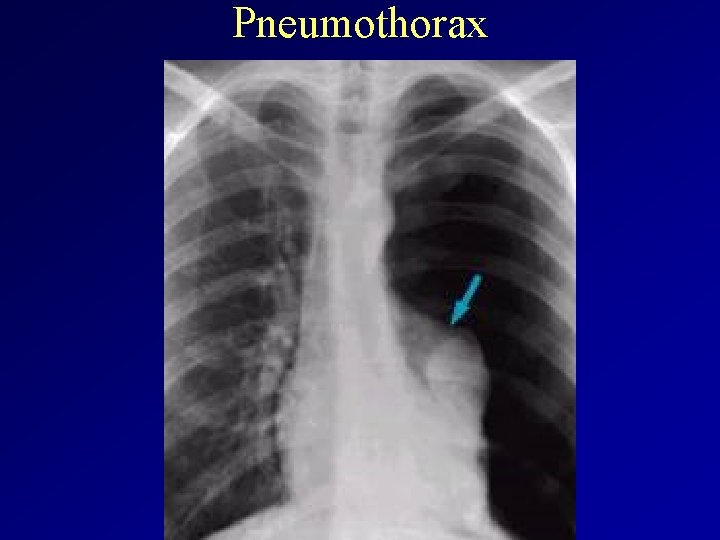
Pneumothorax
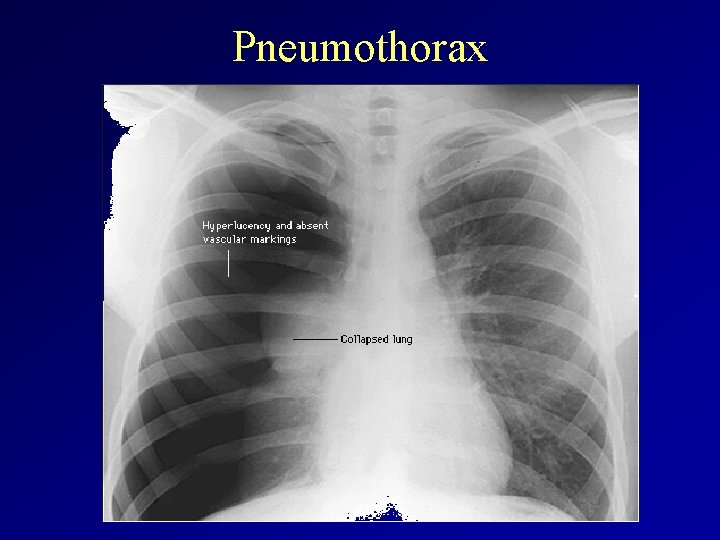
Pneumothorax
Ptx tube drainage

Tension PTX A tension PTX is a life-threatening condition that requires immediate intervention. Causes: penetrating chest injuries, fractures of the trachea or bronchi, a ruptured esophagus, the presence of an occlusive dressing over an open PTX, and PPV. Progressive build-up of pressure in the pleural space pushes the mediastinum to the opposite hemithorax, and obstructs venous return to the heart. This leads to circulatory instability and may result in traumatic arrest. Symptomes: patient is tachycardic and tachypnoeic, and may be hypoxic. These signs are followed by circulatory collapse with hypotension and subsequent traumatic arrest with pulseless electrical activity (PEA). Breath sounds and percussion note may be very difficult to appreciate and misleading in the trauma room. .
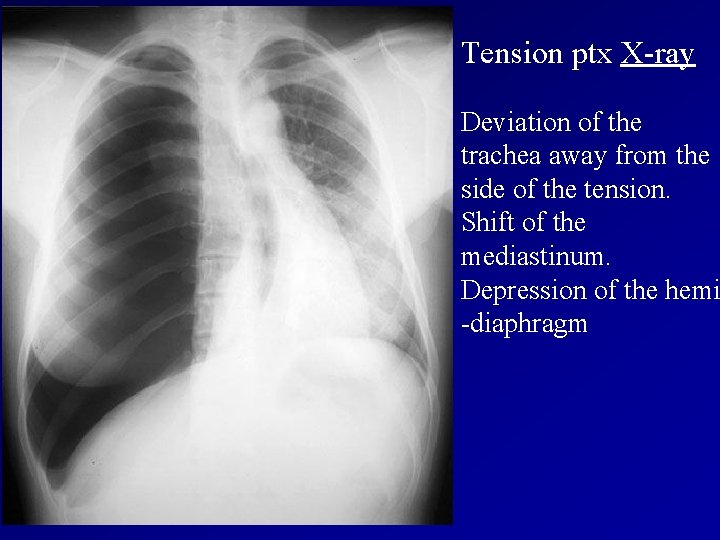
Tension ptx X-ray Deviation of the trachea away from the side of the tension. Shift of the mediastinum. Depression of the hemi -diaphragm
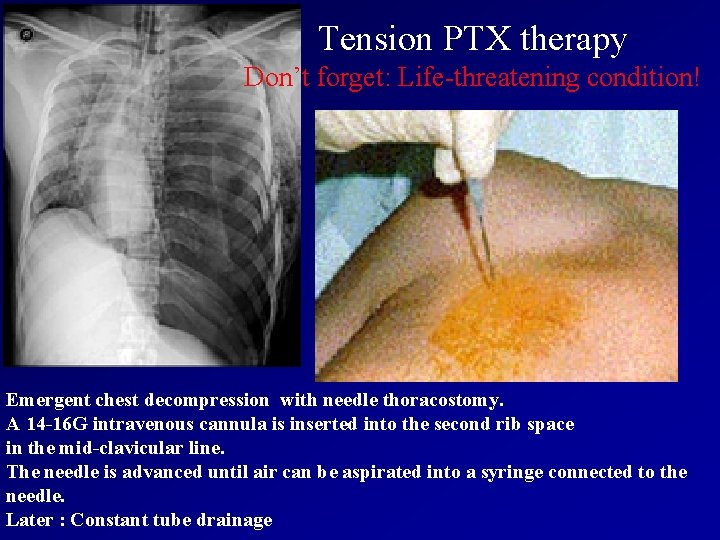
Tension PTX therapy Don’t forget: Life-threatening condition! Emergent chest decompression with needle thoracostomy. A 14 -16 G intravenous cannula is inserted into the second rib space in the mid-clavicular line. The needle is advanced until air can be aspirated into a syringe connected to the needle. Later : Constant tube drainage
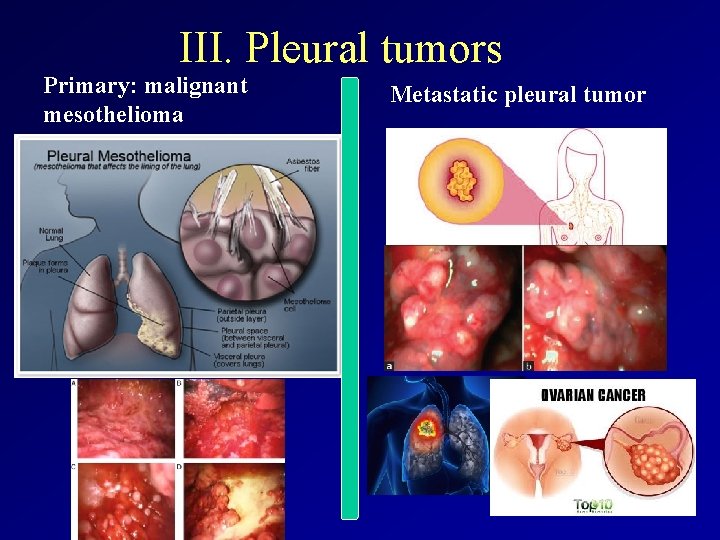
III. Pleural tumors Primary: malignant mesothelioma Metastatic pleural tumor

III. Pleural tumors • 1. Primary tumor = mesothelioma – Localised form: solitary growth on pleural surface • Th: surgical resection – Diffuse mesothelioma: Malignant , aggressive tumour originating in the serosal membranes that line thoracic and abdominal cavities. More than 90% of mesothelioma cases occur in the pleura. The occurrence of it typically related to exposure to mineral fibres such as asbestos and erionite. • Symptomes: Chest pain, especially when taking a deep breath, Cough, General discomfort, uneasiness, or ill feeling (malaise), Shortness of breath, Weight loss • Diagnosis: – Chest X-ray: rapidly reproducated pleural effusion – CT scan of the chest – Thoracentesis: Pleural fluid analysis: cytology, histology, immunhistochemistry – Open pleural biopsy – Pleural needle biopsy

Mesothelioma therapy • Surgery: Depending on the location and stage of the cancer, and the health of the patient, tumors may be able to be removed through surgery. • Chemotherapy: pemetrexed • Radiation therapy: One of the oldest mesothelioma treatments, radiation techniques can target and shrink tumors to make other treatments more effective. • Experimental Treatment: Clinical trials that test newer therapies like immunotherapy can prove effective if other options are exhausted. • Palliative Treatment: Additional techniques and therapies can treat the symptoms of mesothelioma to help ease patient pain and suffering. : painkiller, thoracocentesis, pleurodesis, tube drainage

Metastatic pleural tumor • Metastatic tumor: malignant pleural effusion caused by primery tumor of the body: breast c. , lung c. , ovarian cancer, kidney c, • Symptomes: symptomes of pleural effusion+symptomes of primary tumor • Pleural fluid reproduction is rapid • Diagnosis: Anamnesis! X-ray, ultrasonography, CT, lab. – Thoracocentesis: cytology, histology, immunhistochemistry • Therapy: therapy of primary tumor + palliative care (thoracocentesis, pleurodesis, painkiller)

- Slides: 38