Diseases of Esophagus Dysphagia Dr Vishal Sharma Diseases






























































- Slides: 146

Diseases of Esophagus & Dysphagia Dr. Vishal Sharma

Diseases of esophagus

Contents • Esophagitis, Barret’s esophagus & GERD • Esophageal tear & perforation • Esophageal web, ring, stricture, atresia • Achalasia cardia • Esophageal hiatus hernia • Esophageal hypermotility disorder • Esophageal vascular impression • Esophageal neoplasm

Esophagitis

Etiology • Gastro-esophageal reflux disease (commonest) • Infective: candidiasis, cytomegalovirus, HIV, herpes simplex, tuberculosis, Crohn’s disease, actinomycosis • Caustic ingestion • Medication: Iron, vitamin C, doxycycline, NSAID • Iatrogenic: nasogastric tube, radiation • Others: graft vs. host disease, uremia, eosinophilic esophagitis, benign pemphigoid, epidermolysis bullosa

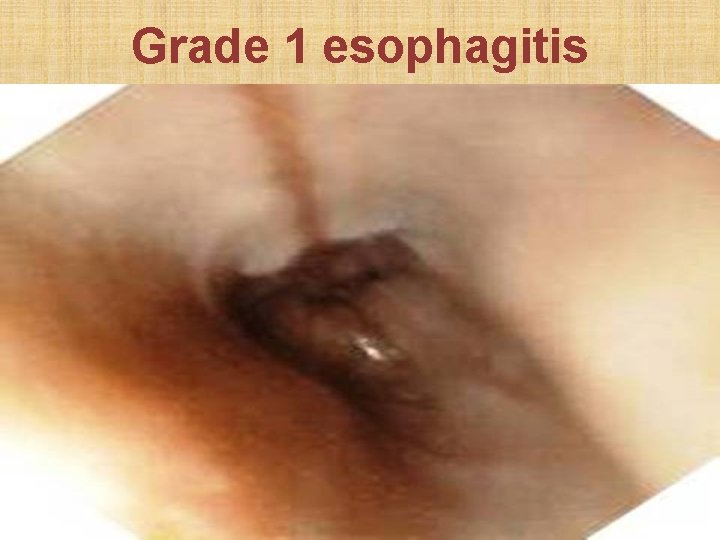
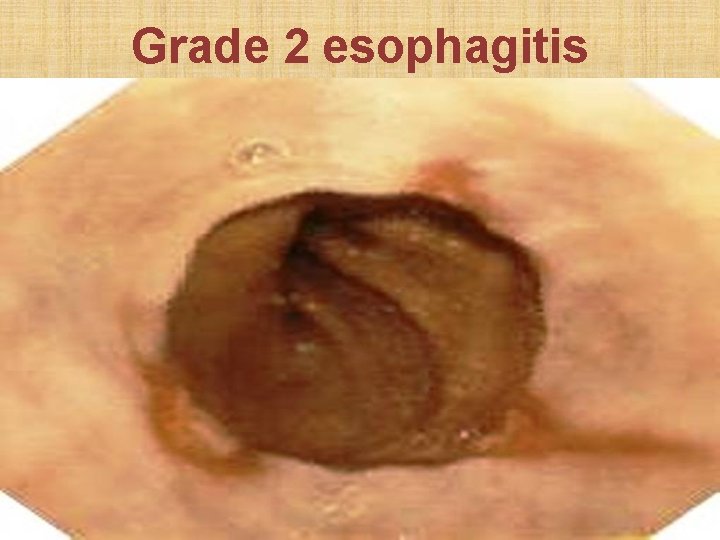
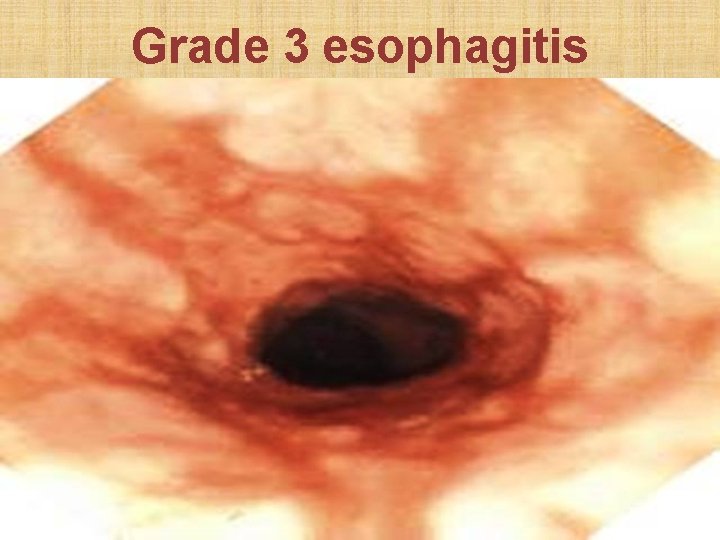
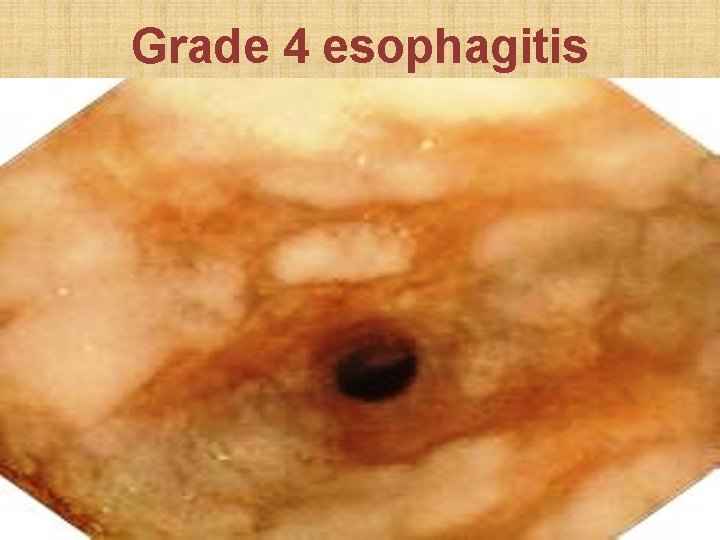
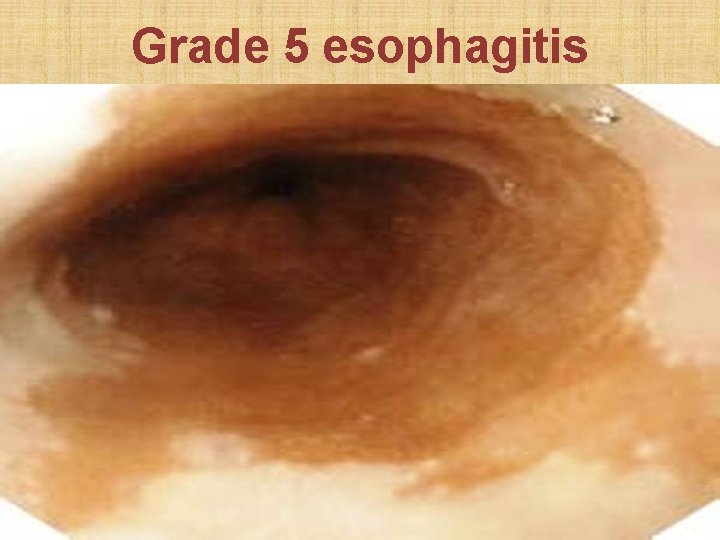
Savary Monnier classification of esophageal erosion • Grade 1: Single erosion over single mucosal fold • Grade 2: Erosions over multiple folds • Grade 3: Circumferential mucosal erosions • Grade 4: Erosion with definitive ulcer or stricture • Grade 5: Columnar metaplasia (Barret’s esophagus)

Grade 1 esophagitis

Grade 2 esophagitis

Grade 3 esophagitis

Grade 4 esophagitis

Grade 5 esophagitis

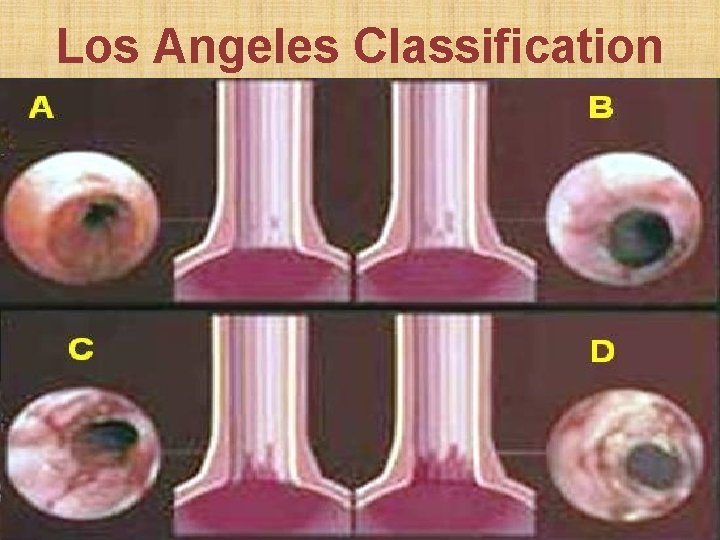
Los Angeles Classification • Grade A: Mucosal break < 5 mm in length over single mucosal fold • Grade B: Mucosal break > 5 mm over single mucosal fold • Grade C: Continuous mucosal break b/w > 2 mucosal folds but < 75% of esophageal circumference • Grade D: Mucosal break >75% of esophageal circumference

Los Angeles Classification

Gastro- Esophageal Reflux Disease

Predisposing factors Inefficient lower esophageal sphincter due to: Pregnancy Obesity Fatty food, large meals Coffee, chocolate Cigarette smoking Alcohol ingestion Reflux promoting drugs (see under treatment) Scleroderma Hiatus hernia

Clinical features • Retro-sternal burning pain (heartburn / pyrosis) • Dysphagia • Chest pain • Hoarseness, choking (laryngospasm), • Bronchospasm / asthma • Hematemesis & melaena • Chronic cough due to aspiration pneumonia • Symptomatic relief with trial of Pantoprazole

GERD • Burning pain Angina pectoris • Gripping / crushing pain • Pain seldom radiates to • Pain radiates into neck, arms • Produced by bending, drinking hot liquids shoulders & both arms • Pain produced by exercise • Relieved by antacids • Relieved by rest • Dyspnea absent • Dyspnea present

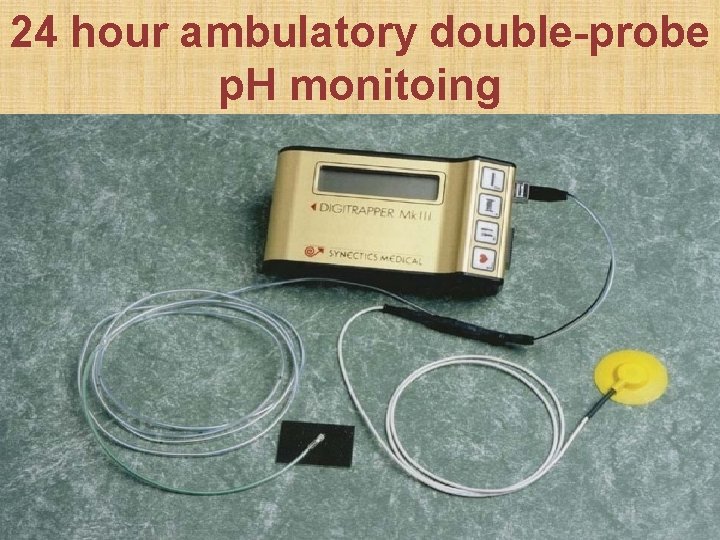
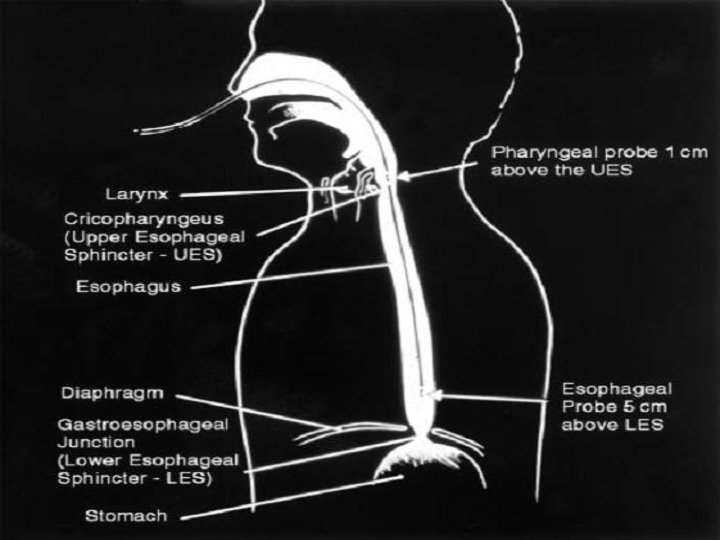
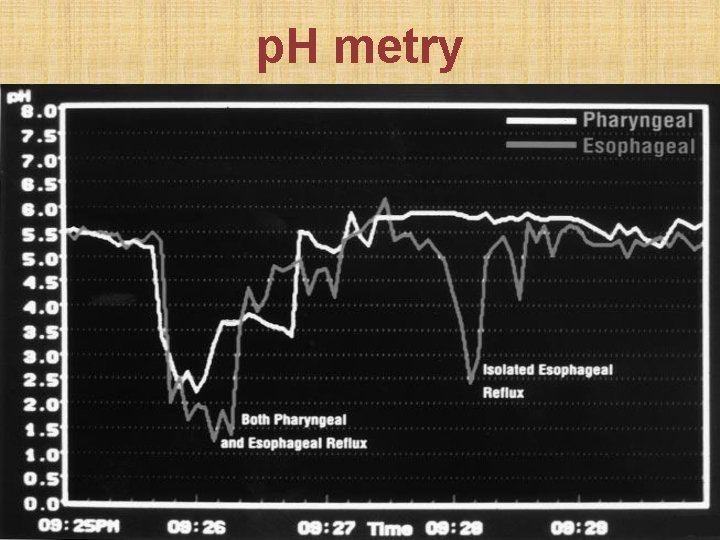
Investigations 1. Flexible upper GI endoscopy 2. Ambulatory 24 -hour double-probe (esophageal & pharyngeal) p. H metry = gold standard • Distal probe = 5 cm above lower esophageal sphincter • Proximal probe = 1 cm above upper esophageal sphincter, in hypopharynx behind laryngeal inlet • Laryngo-pharyngeal reflux = acidic p. H in both probes • Gastro-esophageal reflux = acidic p. H in distal probe only

24 hour ambulatory double-probe p. H monitoing


p. H metry

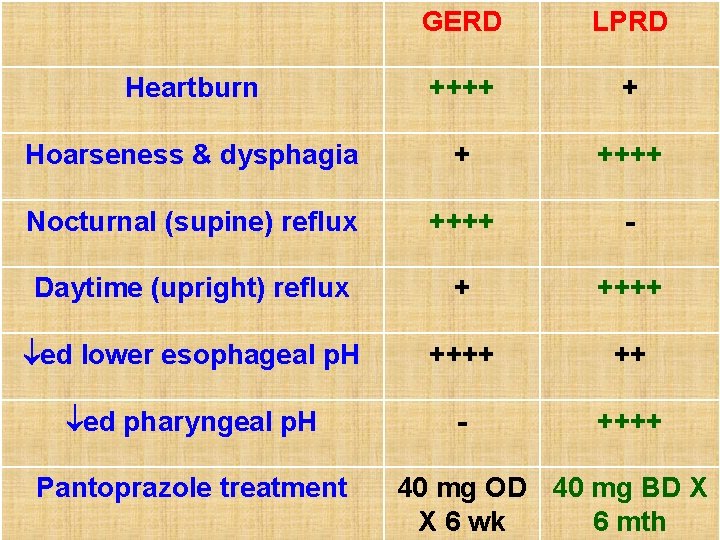
GERD LPRD Heartburn ++++ + Hoarseness & dysphagia + ++++ Nocturnal (supine) reflux ++++ - Daytime (upright) reflux + ++++ ed lower esophageal p. H ++++ ++ ed pharyngeal p. H - ++++ Pantoprazole treatment 40 mg OD 40 mg BD X X 6 wk 6 mth

Treatment of GERD A. Life style modifications: 1. Raise head end of bed by 6 inches. Sleep in left lateral position. Maintain optimum weight. 2. Avoid the following: • Tight fitting clothes & belts • Lifting of heavy weight / straining / stooping • Smoking

B. Dietary modifications: 1. Take 6 small meals. Eat slowly & chew thoroughly. 2. Take high protein diet. 3. Avoid the following: • Eating / drinking within 3 hours of reclining • Fried food / excess fat / large meals • Taking large amount of fluids with meals • Aerated drinks / alcohol (especially in evening) • Coffee / tea / chocolate / mint / citrus fruit juice

C. Avoid following medicines: • Tranquilizers & sedatives • Muscle relaxants • Calcium channel blockers • Anti-cholinergic drugs • Theophylline • N. S. A. I. Ds • Doxycycline

Dietary + Life style modifications + avoid reflux producing medicines + Liquid antacid (2 tsp 1 hour before meals & at bed time) no relief after 4 weeks Ranitidine 150 mg BD + Cisapride 10 mg TID before meals no relief after 4 weeks Pantoprazole 40 mg OD before breakfast no relief after 4 weeks Nissen’s fundoplication + Hill’s posterior gastropexy

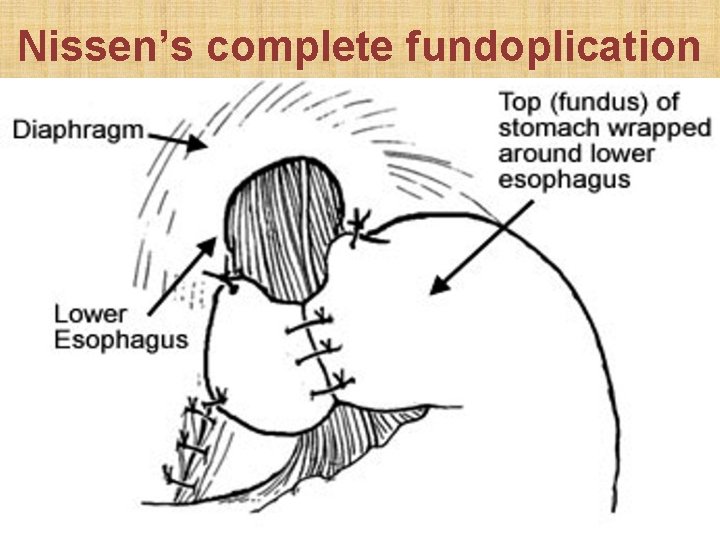
Nissen’s complete fundoplication

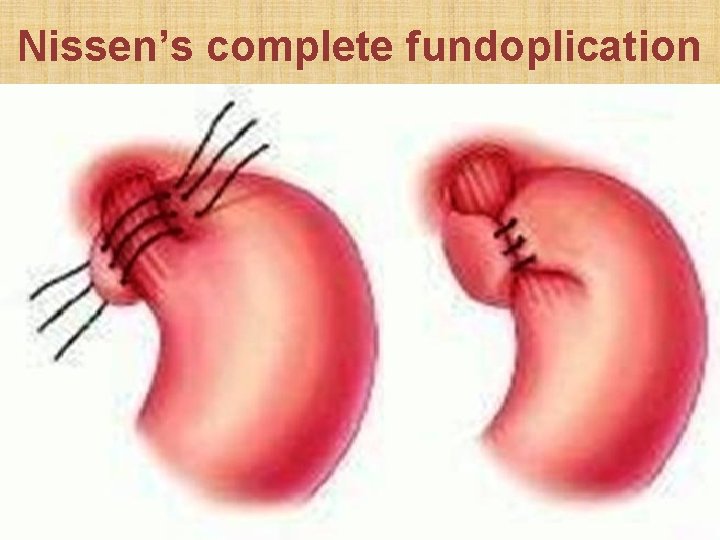
Nissen’s complete fundoplication

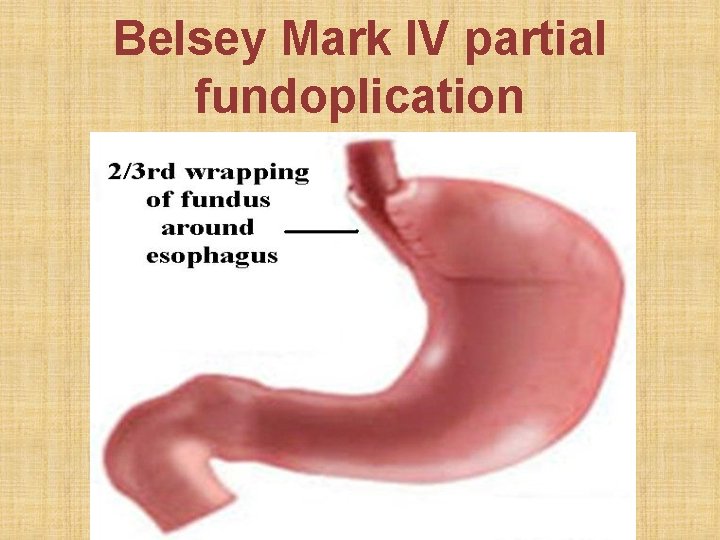
Belsey Mark IV partial fundoplication

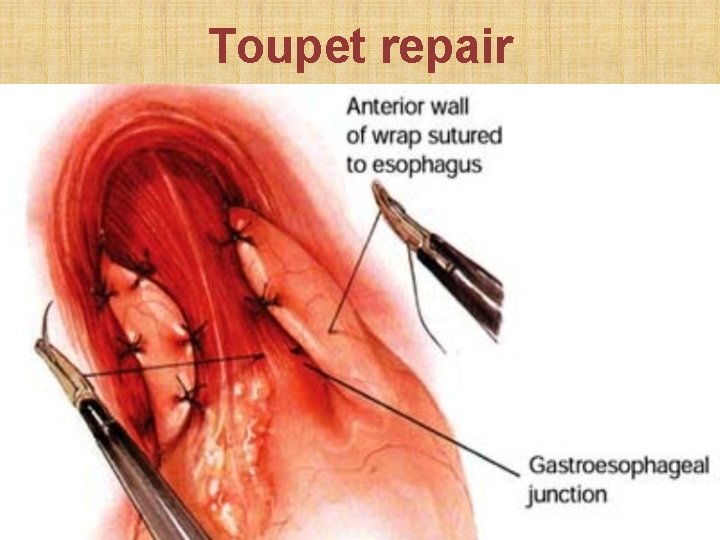
Toupet repair

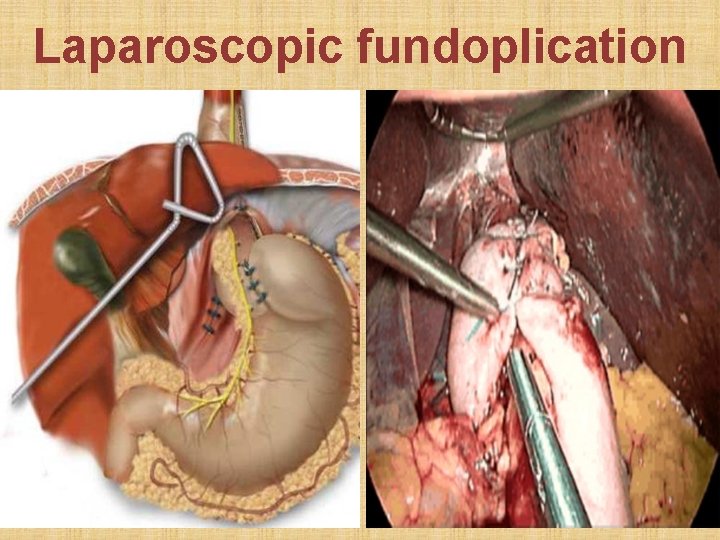
Laparoscopic fundoplication

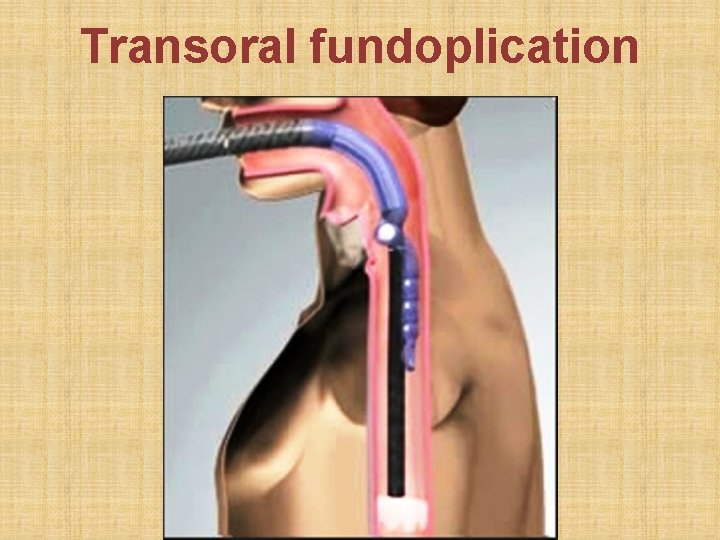
Transoral fundoplication

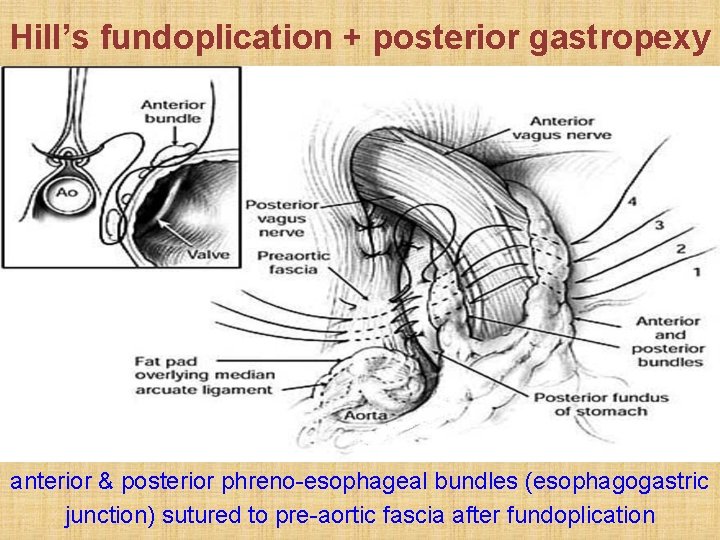
Hill’s fundoplication + posterior gastropexy anterior & posterior phreno-esophageal bundles (esophagogastric junction) sutured to pre-aortic fascia after fundoplication

Complications of GERD • Esophageal ulceration • Esophageal stricture • Iron-deficiency anemia • Barrett's esophagus • Laryngitis, laryngeal ulcers • Bronchial asthma • Aspiration pneumonia

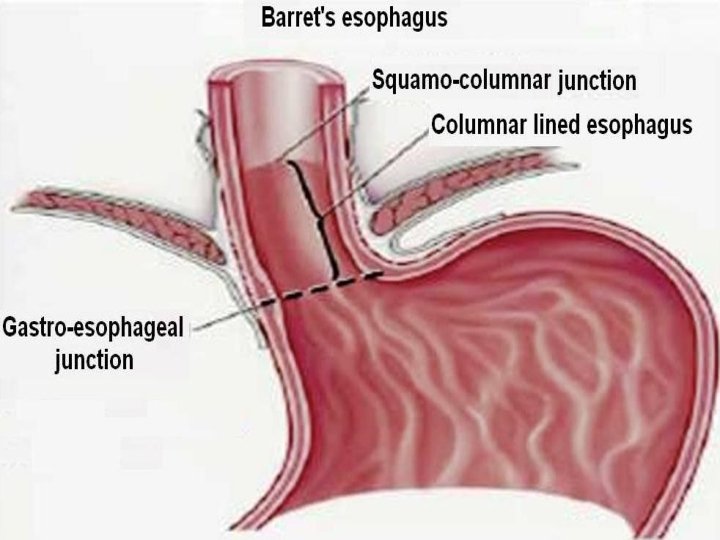
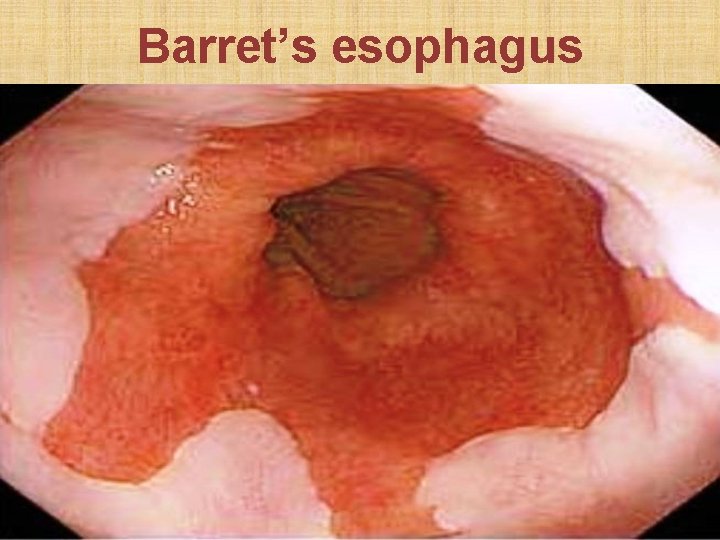
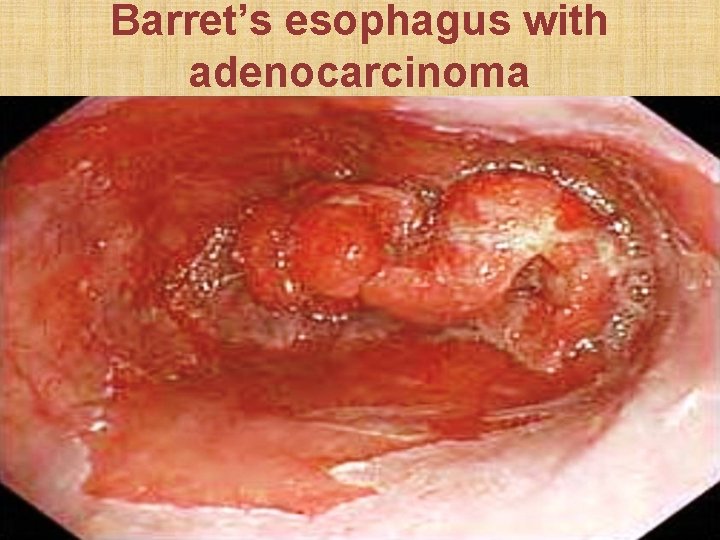
Barret’s esophagus • Presence of gastric epithelium more than 3 cm above gastro-esophageal junction caused by columnar metaplasia of squamous epithelium due to chronic acid exposure • Pre-malignant condition for adenocarcinoma • Rx: Pantoprazole + periodic esophagoscopy every 2 years to rule out dysplasia / malignancy



Barret’s esophagus

Barret’s esophagus with adenocarcinoma

Esophageal ring, web, stricture & atresia

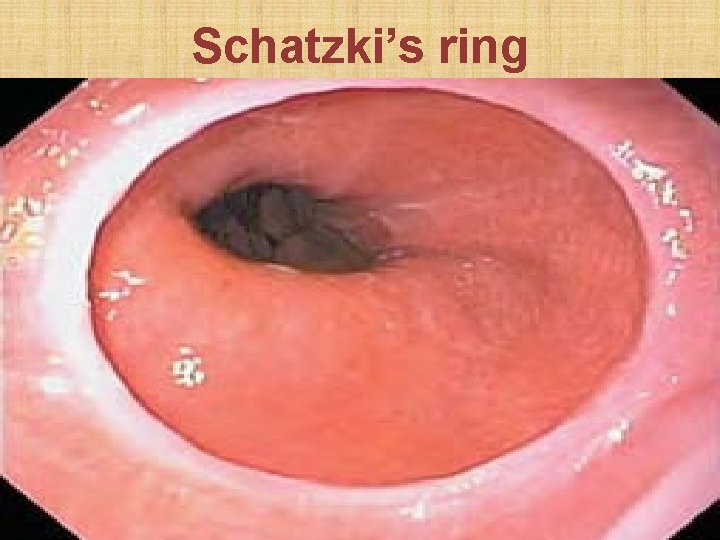
Web Ring • Only part of lumen • Circumferential • Consists of mucosa • Consist of mucosa + only • Involves proximal esophagus • E. g. web of Plummer Vinson Syndrome muscle • Involves distal esophagus • E. g. Schatzki's ring of lower esophagus

Schatzki’s ring

Plummer Vinson Syndrome • Synonym: 1. Patterson Brown Kelly syndrome 2. Sideropenic dysphagia • Seen in middle-aged females due to iron deficiency caused by atrophic gastritis or vitamin B 12 deficiency (pernicious anemia) • Classical Triad: upper esophageal web iron deficiency anemia (sideropenia) cheilitis / glossitis

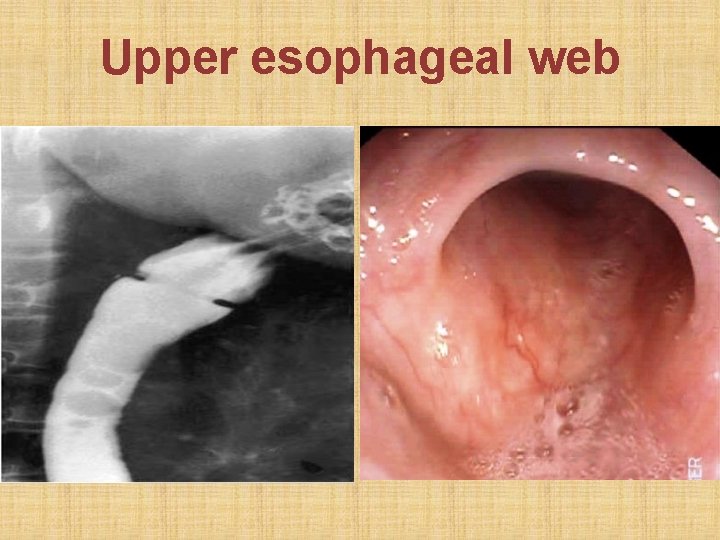
Clinical features • Dysphagia: more to solids than liquids. Due to upper esophageal web caused by sub-epithelial fibrosis. • Pallor: iron deficiency anemia • Koilonychia (spoon nails): iron deficiency anemia • Cheilitis + glossitis: vitamin B 12 deficiency

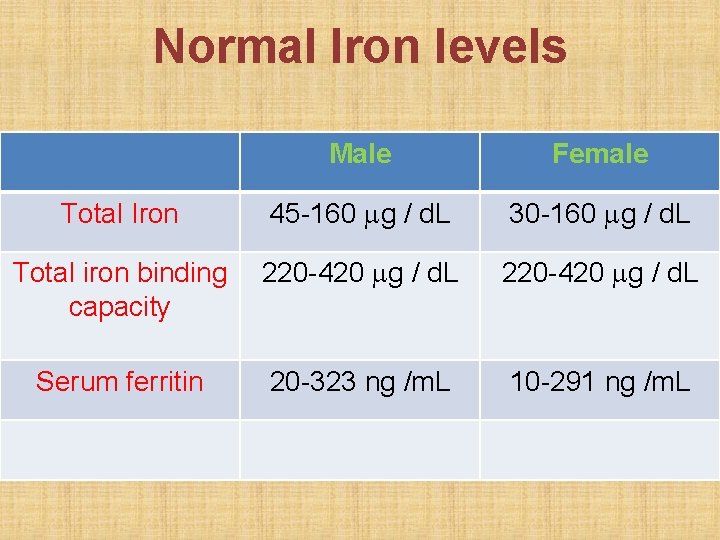
Investigations • Barium swallow anterior wall web in • Esophagoscopy upper esophagus • Blood smear: microcytic, hypochromic anemia • Serum iron: decreased • Total iron binding capacity: increased • Gastric juice analysis: achlorhydria

Normal Iron levels Male Female Total Iron 45 -160 g / d. L 30 -160 g / d. L Total iron binding capacity 220 -420 g / d. L Serum ferritin 20 -323 ng /m. L 10 -291 ng /m. L

Upper esophageal web

Treatment • Supplementation: iron + vitamin B 12 + vitamin B 6 + folic acid • Endoscopic dilatation of web with elastic bougie or Hurst mercury pneumatic dilator • Electrosurgical incision or surgical resection of web for refractory cases • Regular check endoscopy to rule out post-cricoid malignancy (seen in 10% cases)

Esophageal strictures • Definition: narrowing of esophageal lumen (normal diameter = 20 mm • Dysphagia is main symptom (Solids > liquids) • Etiology for multiple esophageal strictures: benign pemphigoid, epidermolysis bullosa, caustic ingestion, candidiasis, graft vs. host disease

Causes of single stricture • GERD, esophagitis, Barret’s esophagus • Caustic ingestion: corrosives, hot fluid • Trauma: foreign body, external injury • Medication capsules & tablets • Radiotherapy, sclerotherapy • Surgical anastomosis of esophagus • Malignancy • Congenital: involves lower 1/3 rd

Benign stricture Malignant stricture • Multiple • Single • Regular mucosa • Irregular mucosa • Proximal esophageal • Proximal dilation absent dilation present • At sites of normal constrictions due to cancer invasion • Involves any site in esophagus

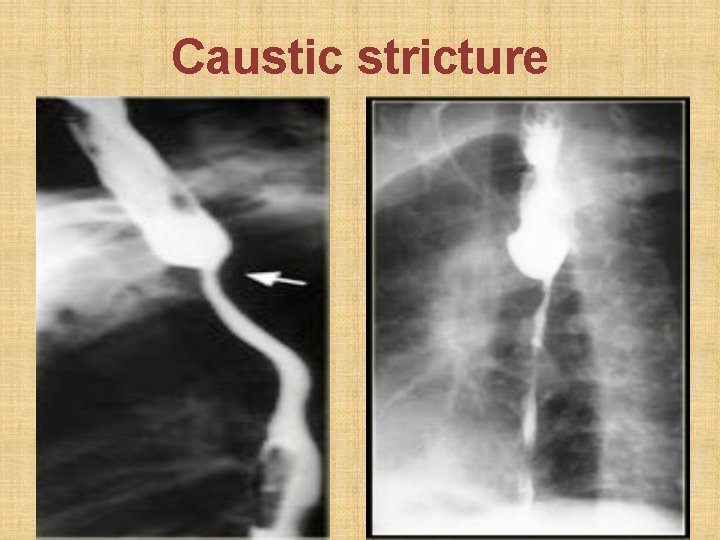
Caustic stricture

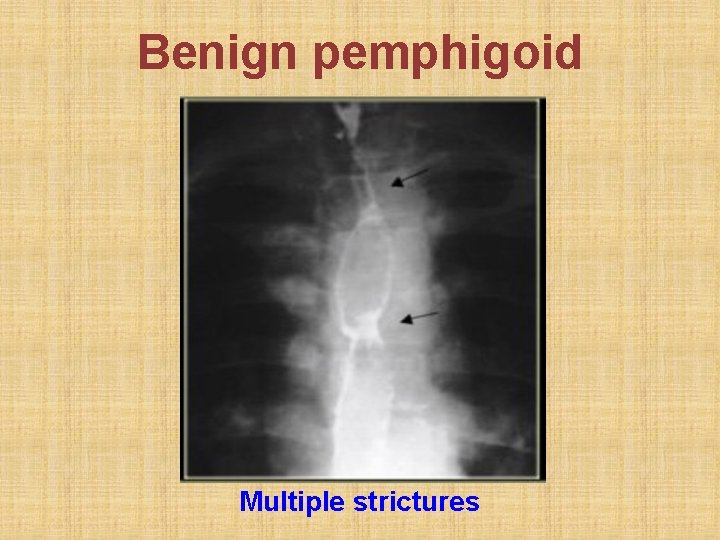
Benign pemphigoid Multiple strictures

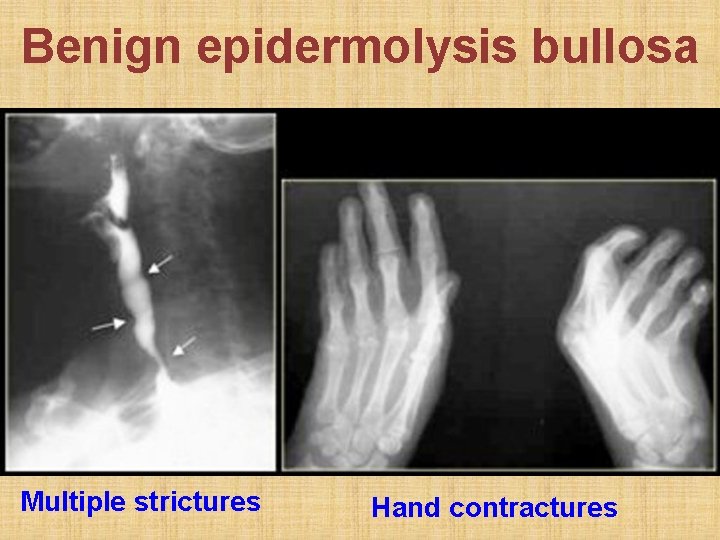
Benign epidermolysis bullosa Multiple strictures Hand contractures

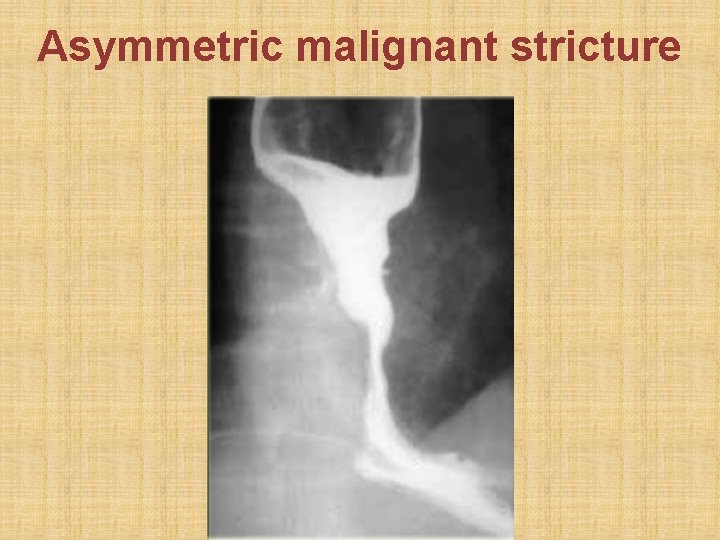
Asymmetric malignant stricture

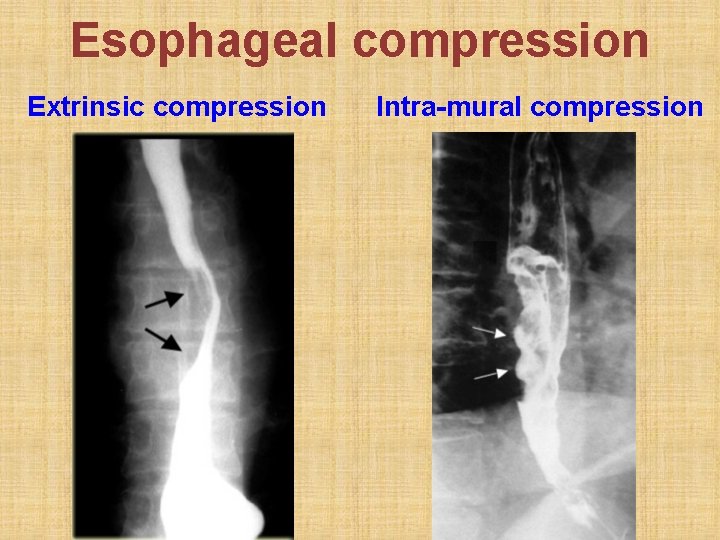
Esophageal compression Extrinsic compression Intra-mural compression

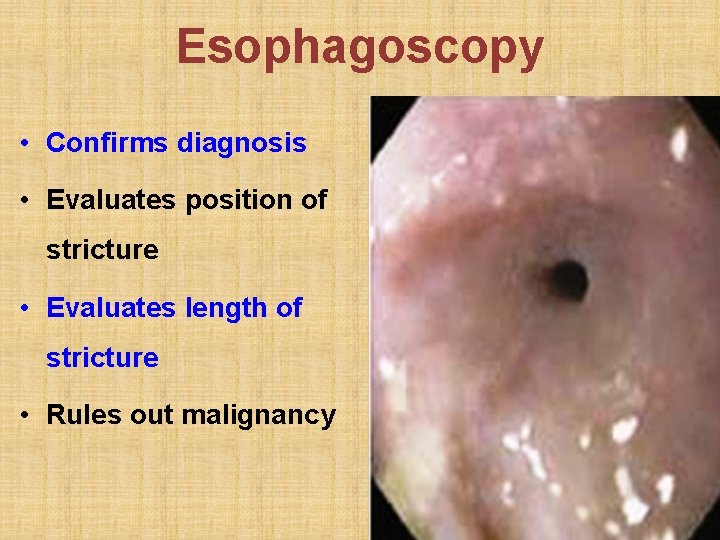
Esophagoscopy • Confirms diagnosis • Evaluates position of stricture • Evaluates length of stricture • Rules out malignancy

Treatment of corrosive ingestion Acid = superficial coagulative necrosis (better) Alkali = penetrating liquefaction necrosis (worse) 1. Hospitalize + treatment of shock & acid-base balance 2. Stricture prevention by: • Steroid given within 48 hours for 6 weeks • Careful nasogastric tube insertion for 3 weeks • N-acetyl cysteine / Penicillamine: es collagen bonding 3. IV antibiotics + antacids + analgesics 4. Neutralize corrosive with weak acid / alkali within 6 hr 5. Discharge after 6 wk; life long follow up to r/o cancer

Surgical treatment of stricture 1. Progressive stricture dilatation over months a. Prograde: oral route with elastic bougie b. Retrograde: gastrostomy route 2. Stent insertion 3. Stricture excision + reconstruction with colon 4. Esophageal bypass with jejunum / colon segment

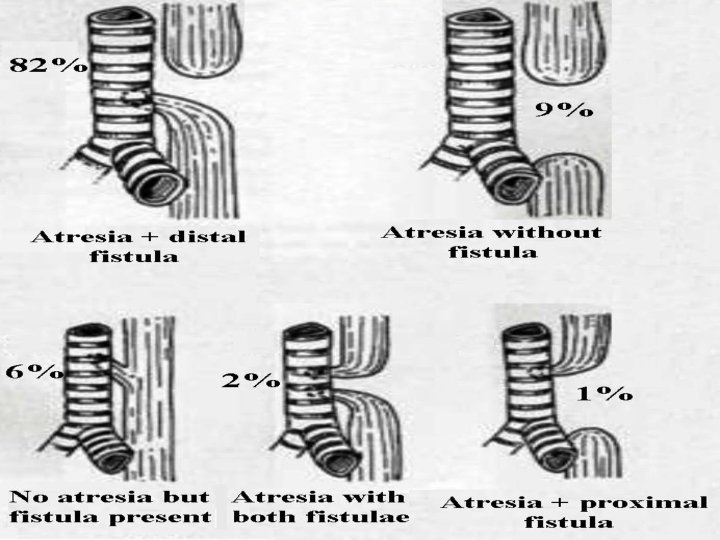
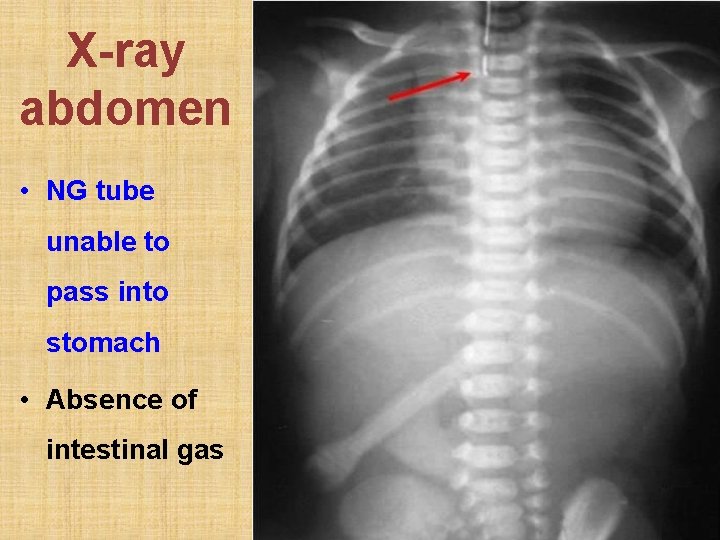
Esophageal atresia 1. Usually occurs with tracheo-esophageal fistula 2. Diagnosed at birth due to: a. failure to pass nasogastric tube b. absence of intestinal gas in X-ray abdomen 3. VACTERL: anomalies of Vertebra, Ano-genital, Cardiac, Trachea, Esophagus, Renal, Limb 4. Rx: immediate repair of esophagus


X-ray abdomen • NG tube unable to pass into stomach • Absence of intestinal gas

Esophageal tear & perforation

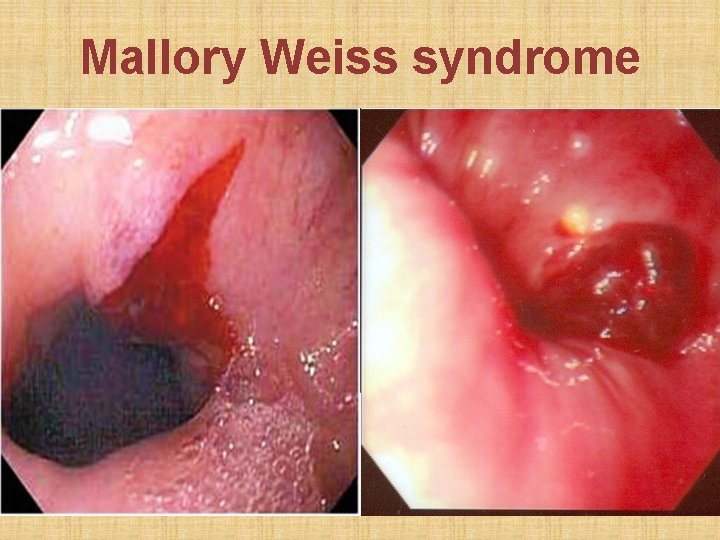
Etiology 1. Instrumentation: involves upper esophagus a. Esophagoscopy b. Dilatation of esophageal stricture 2. Severe vomiting (alcoholic): lower esophagus a. Superficial mucosal tear = Mallory Weiss tear b. esophageal perforation = Boerhaave syndrome 3. ed esophageal lumen pressure: childbirth, forced cough, defecation, seizure, weight lifting

Clinical Features Esophageal tear: painless hematemesis Esophageal perforation: life threatening condition • Severe pain in neck, chest, intra-scapular area • Odynophagia, fever, prostration • Tachypnea, tachycardia & hypotension • Subcutaneous emphysema of neck • Pneumo-mediastinum: Hamman’s mediastinal crunch on auscultation

Mallory Weiss syndrome

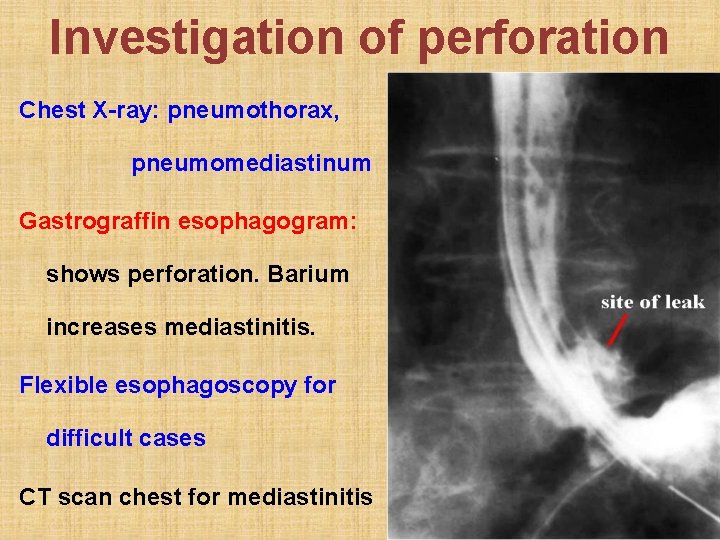
Investigation of perforation Chest X-ray: pneumothorax, pneumomediastinum Gastrograffin esophagogram: shows perforation. Barium increases mediastinitis. Flexible esophagoscopy for difficult cases CT scan chest for mediastinitis

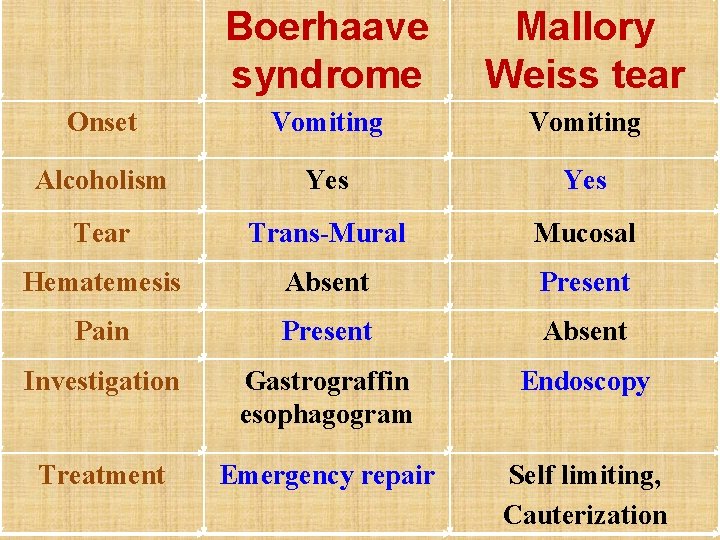
Boerhaave syndrome Mallory Weiss tear Onset Vomiting Alcoholism Yes Tear Trans-Mural Mucosal Hematemesis Absent Present Pain Present Absent Investigation Gastrograffin esophagogram Endoscopy Treatment Emergency repair Self limiting, Cauterization

Treatment • Conservative: for upper esophageal rupture detected within 12 hours & peptic stricture ruptures • Thoracotomy & urgent repair of perforation: for lower esophageal rupture detected within 12 hours • Esophageal bypass / resection & anastomosis / indwelling Celestin feeding tube: for perforation detected after 12 hours & stricture perforations of malignancy, caustic ingestion & post-radiotherapy

Conservative treatment 1. Nil by mouth 2. Parenteral nutrition 3. IV high dose broad-spectrum antibiotics 4. Endoscopic insertion of nasogastric tube 5. Continuous nasogastric tube suction for 1 week • Most perforations heal within 2 weeks

Achalasia Cardia (Cardiospasm)

Etiology: 1. degeneration of ganglion cells of inhibitory neurons in Auerbach’s myenteric plexus 2. Chagas disease (American trypanosomiasis) Pathogenesis: failure of lower esophageal sphincter relaxation + uncoordinated peristalsis food retention dilated + tortuous lower esophagus Clinical features: – Dysphagia more to liquids than solids – Regurgitation of undigested food – Weight loss, aspiration pneumonia

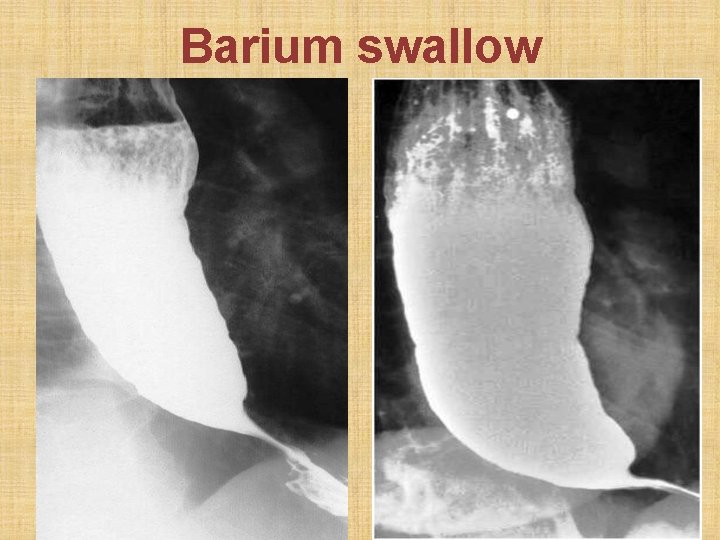
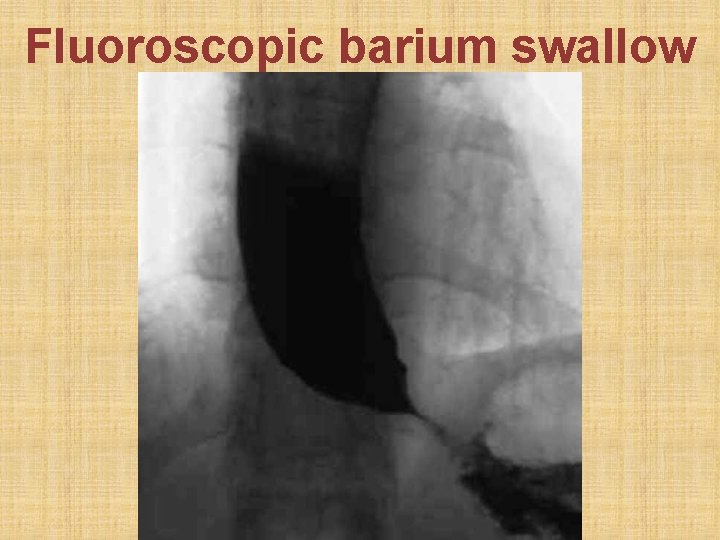
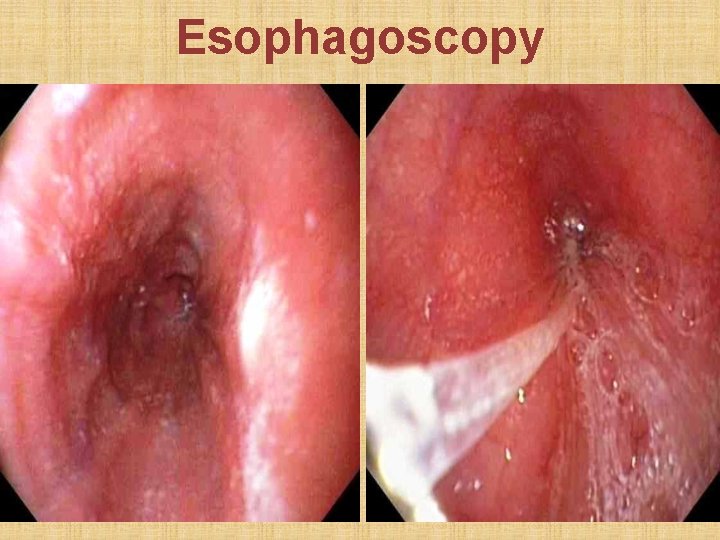
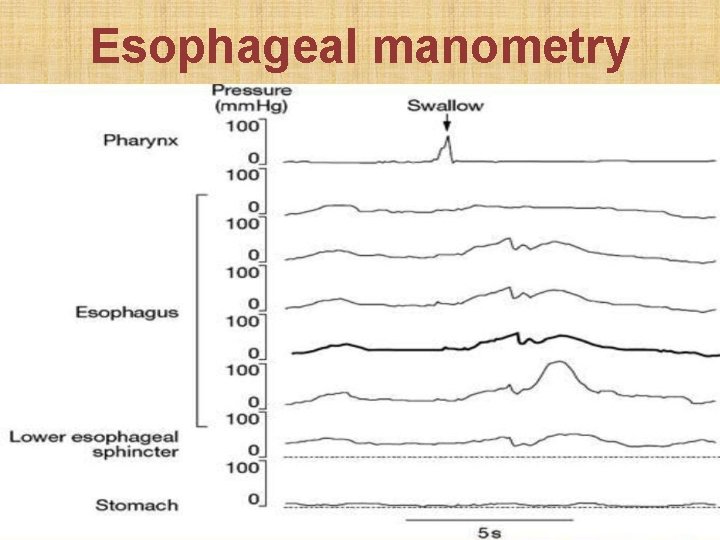
• Chest X-ray: mediastinal widening + air-fluid level • Barium swallow: Smooth fusiform lower esophageal dilation (mega-esophagus) with abrupt tapering of lower end (bird's beak appearance). Absence of fundic gas shadow. Absence of peristalsis. • Esophagoscopy: sudden dilatation of lower esophageal lumen (like entering a dirty cave). Rule out malignancy (0. 15% ) causing pseudo-achalasia. • Esophageal manometry: pressure in esophageal body; pressure at lower esophageal sphincter

Barium swallow

Fluoroscopic barium swallow

Esophagoscopy

Esophageal manometry

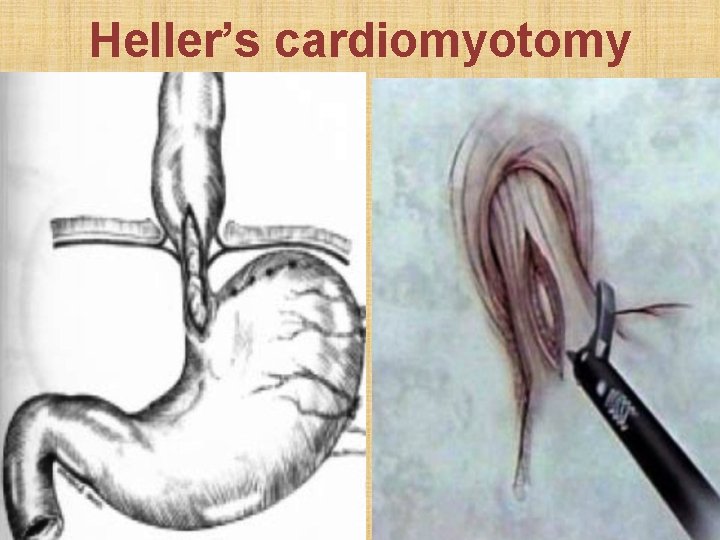
Treatment • Smooth muscle relaxants (nitrates or calcium channel blockers): afford short-lived relief • Endoscopic Botulinum toxin injection into lower esophageal sphincter: gives relief for many weeks • Endoscopic dilatation of lower esophageal sphincter: with elastic bougie / pneumatic dilator • Heller’s laparoscopic cardio-myotomy: surgical division of lower esophageal sphincter + Nissen’s complete fundoplication to prevent post-op reflux

Heller’s cardiomyotomy

Laparoscopic cardiomyotomy

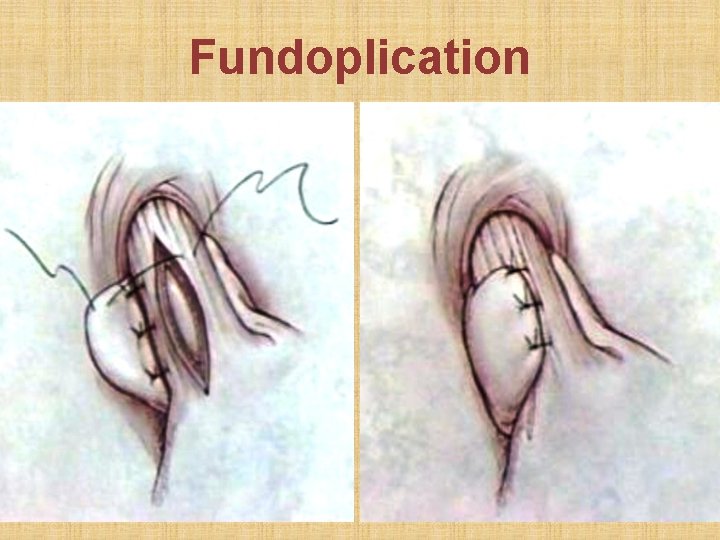
Fundoplication

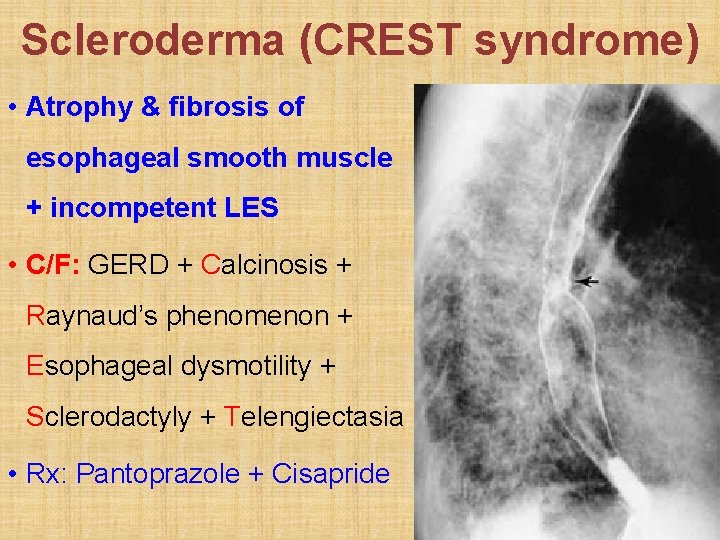
Scleroderma (CREST syndrome) • Atrophy & fibrosis of esophageal smooth muscle + incompetent LES • C/F: GERD + Calcinosis + Raynaud’s phenomenon + Esophageal dysmotility + Sclerodactyly + Telengiectasia • Rx: Pantoprazole + Cisapride

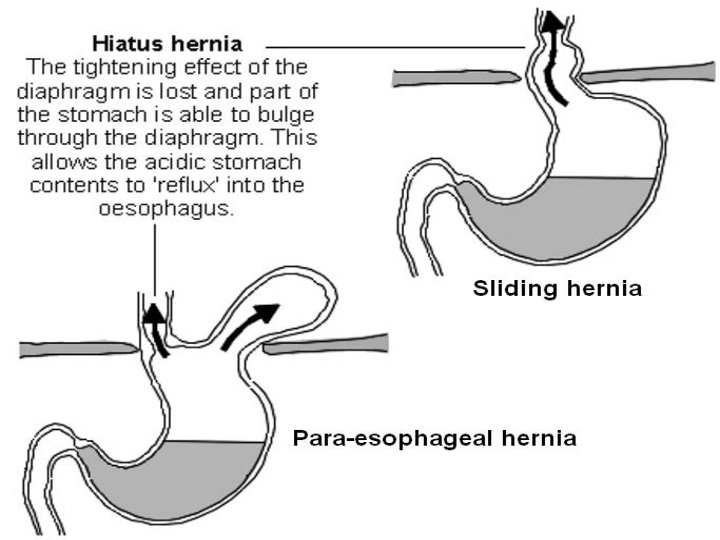
Esophageal hiatus hernia

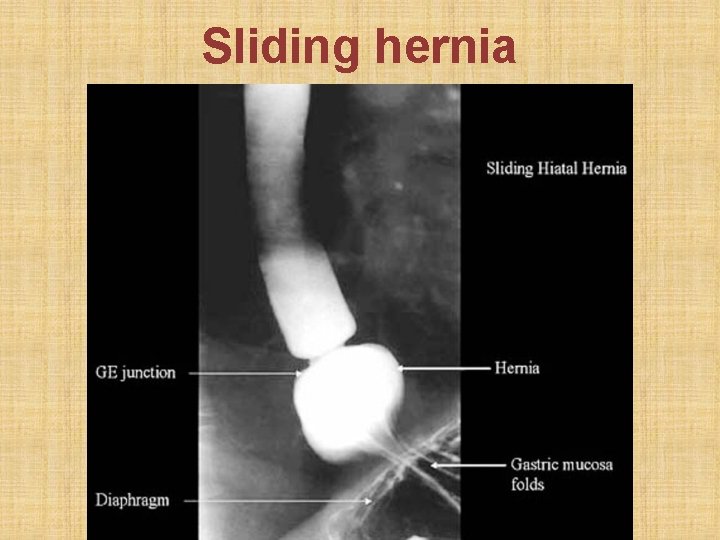
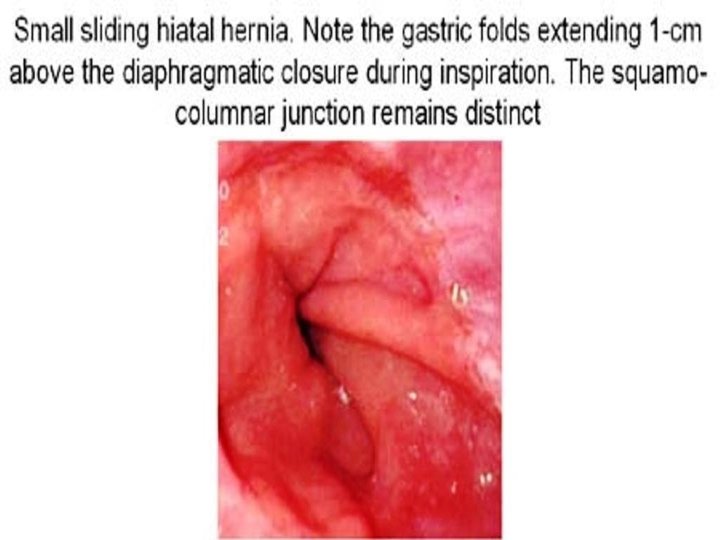
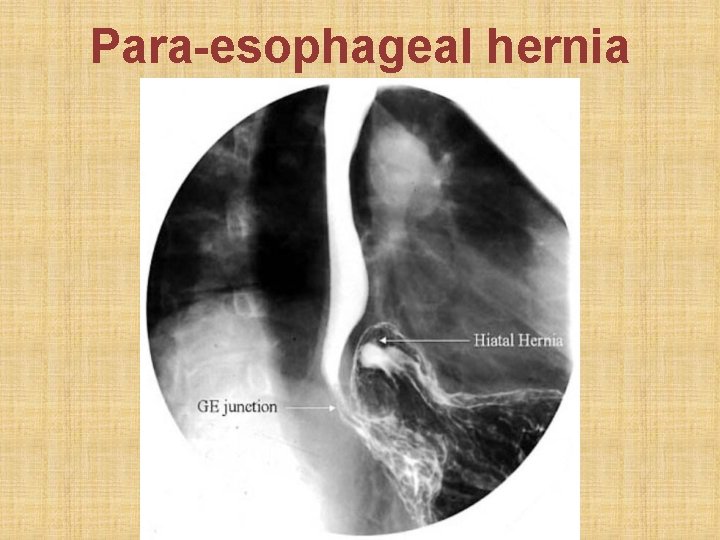
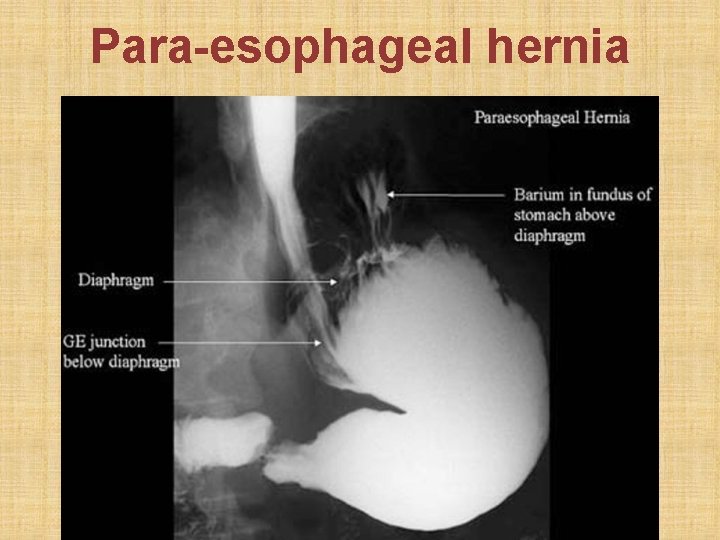
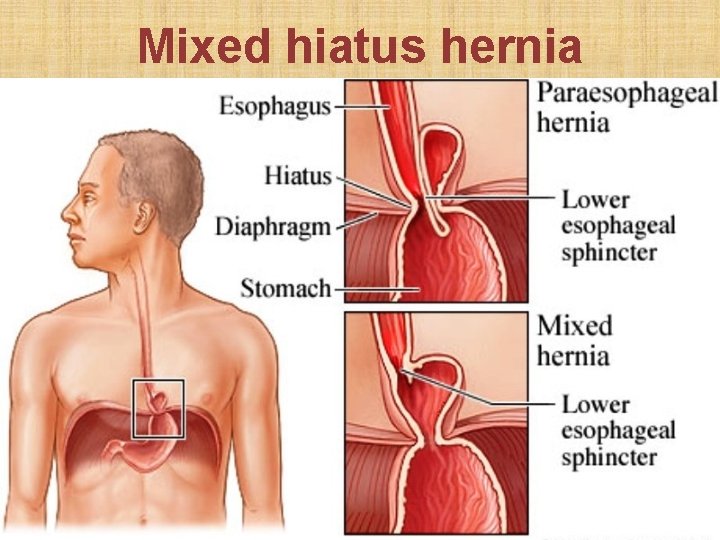
• Definition: herniation of part of stomach above esophageal hiatus in diaphragm • Sliding hiatus hernia: gastro-esophageal junction slides > 2 cm above esophageal hiatus in diaphragm. Esophagoscopy is diagnostic. • Para-esophageal or rolling hernia: part of gastric fundus rolls up via esophageal hiatus in diaphragm, alongside esophagus. Gastro-esophageal sphincter remains below diaphragm & is competent. Esophagogram is diagnostic. • Rx: Reduction of hernia + Nissen’s fundoplication


Sliding hernia


Para-esophageal hernia

Para-esophageal hernia

Mixed hiatus hernia

Esophageal Hypermotility disorders

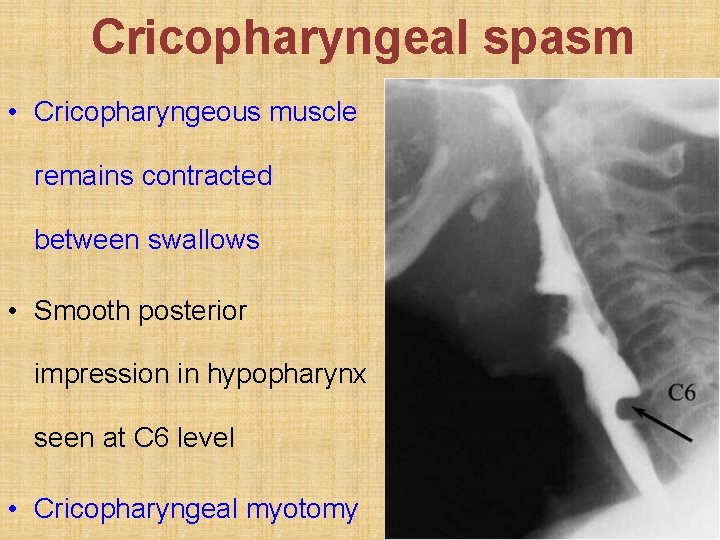
Cricopharyngeal spasm • Cricopharyngeous muscle remains contracted between swallows • Smooth posterior impression in hypopharynx seen at C 6 level • Cricopharyngeal myotomy

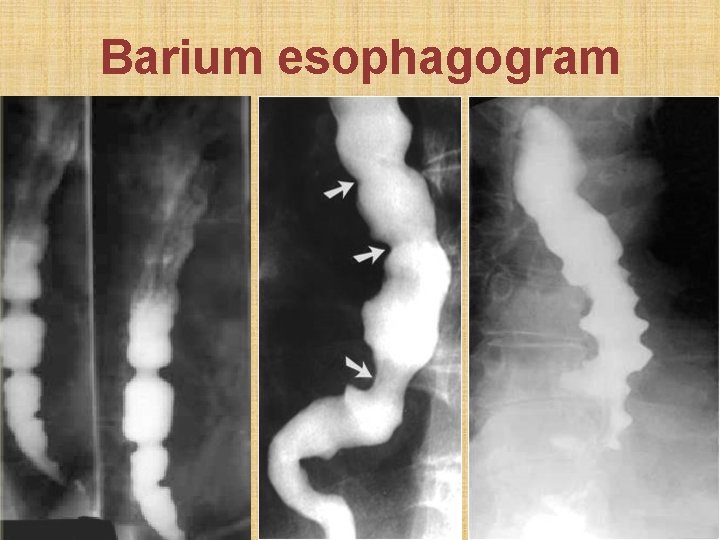
Diffuse esophageal spasm • Dysphagia & chest pain mimicking myocardial infarction especially on drinking cold liquids • Barium swallow: simultaneous, uncoordinated, non-peristaltic contractions in esophagus body (cork-screw esophagus). Normal LES relaxation. • Esophageal manometry: simultaneous repetitive contractions in esophageal body • Treatment: Nitrates, Nifedipine, Amytriptilline

Barium esophagogram

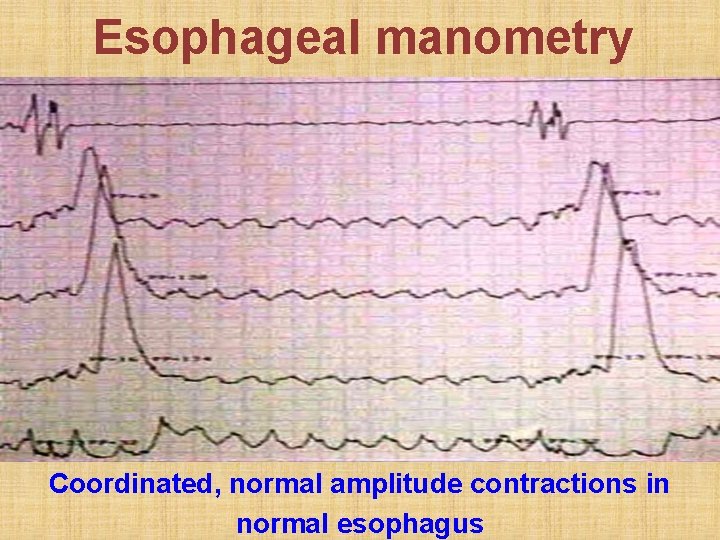
Esophageal manometry Coordinated, normal amplitude contractions in normal esophagus

Esophageal manometry simultaneous, uncoordinated, non-peristaltic contractions in esophagus body in diffuse esophageal spasm

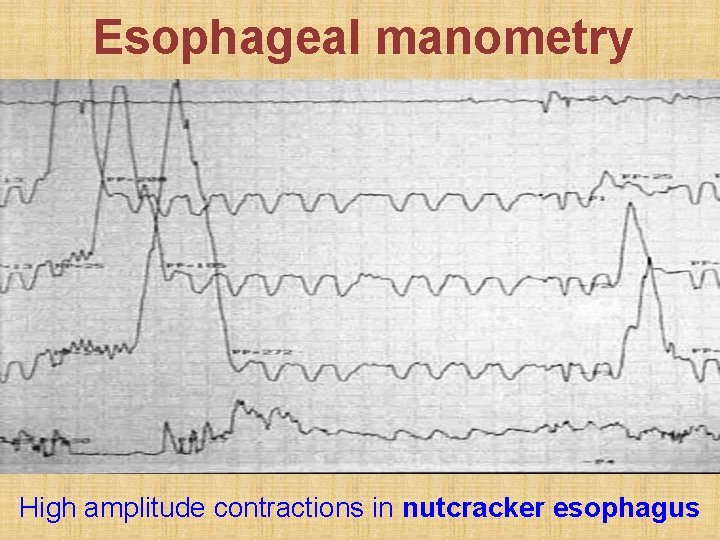
Esophageal manometry High amplitude contractions in nutcracker esophagus

Esophageal vascular impressions

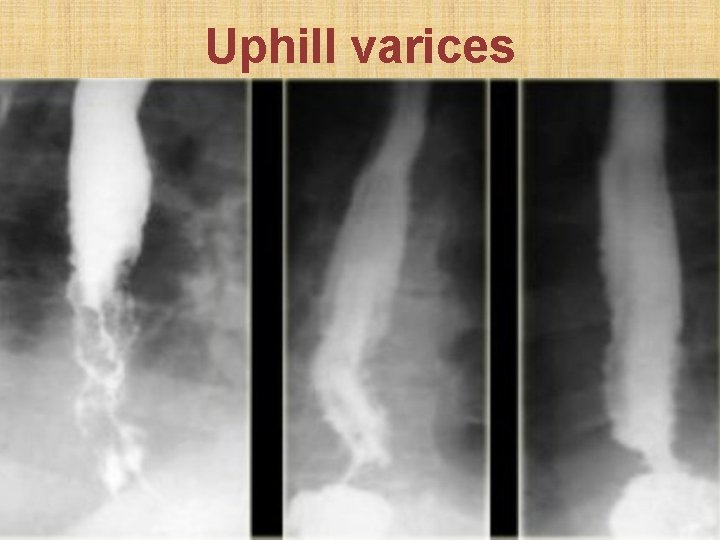
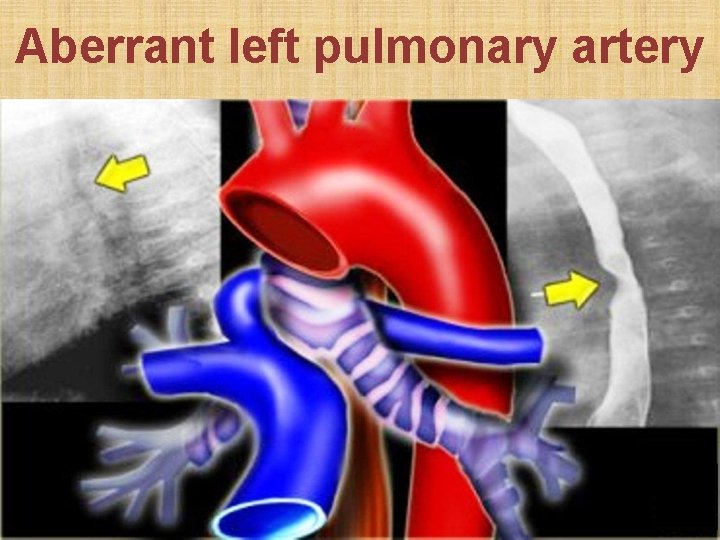
Vascular impressions A. Intrinsic esophageal varices • Uphill: in portal hypertension • Downhill: in superior vena cava obstruction B. Extrinsic (dysphagia lusoria) • Aberrant right subclavian artery • Right aortic arch • Double aortic arch • Aberrant left pulmonary artery

Esophageal varices

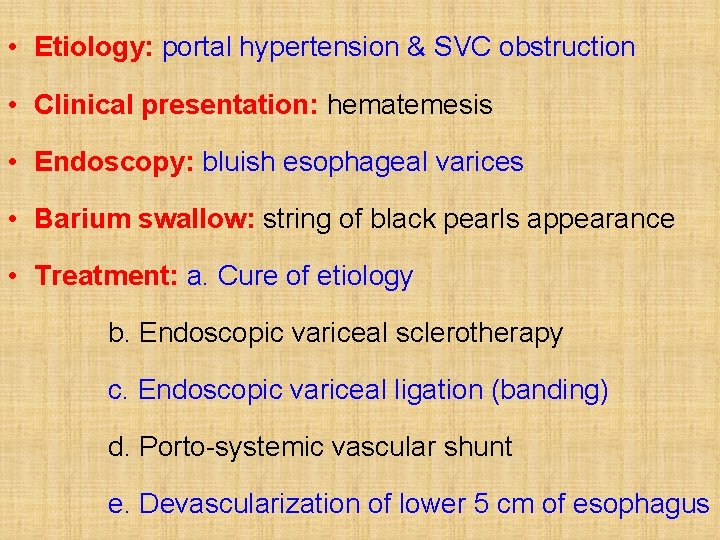
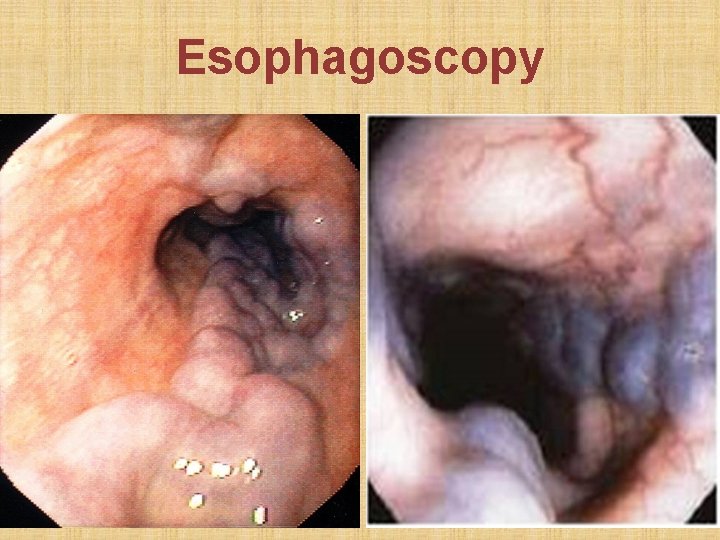
• Etiology: portal hypertension & SVC obstruction • Clinical presentation: hematemesis • Endoscopy: bluish esophageal varices • Barium swallow: string of black pearls appearance • Treatment: a. Cure of etiology b. Endoscopic variceal sclerotherapy c. Endoscopic variceal ligation (banding) d. Porto-systemic vascular shunt e. Devascularization of lower 5 cm of esophagus

Esophagoscopy

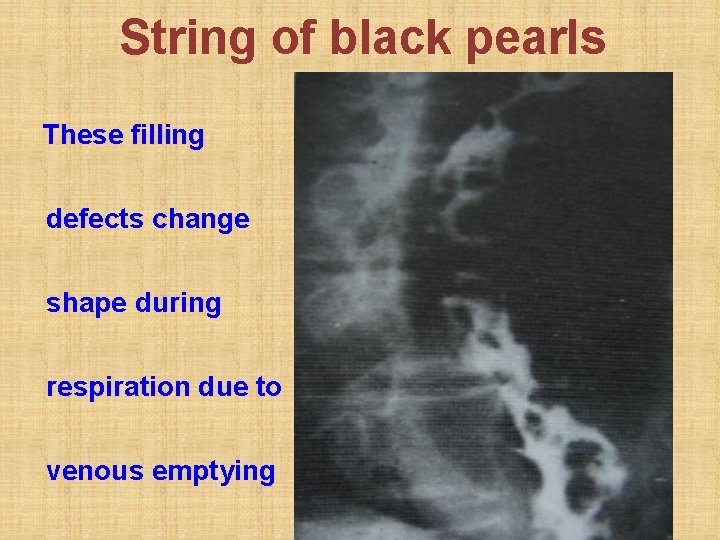
String of black pearls These filling defects change shape during respiration due to venous emptying

Uphill varices

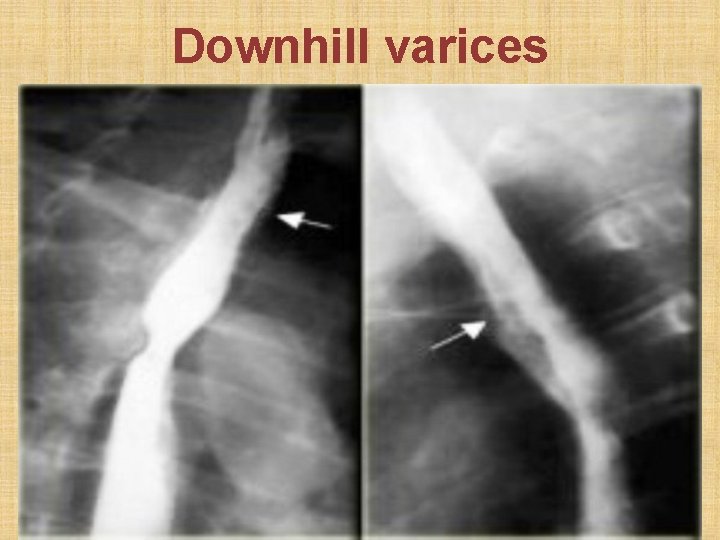
Downhill varices

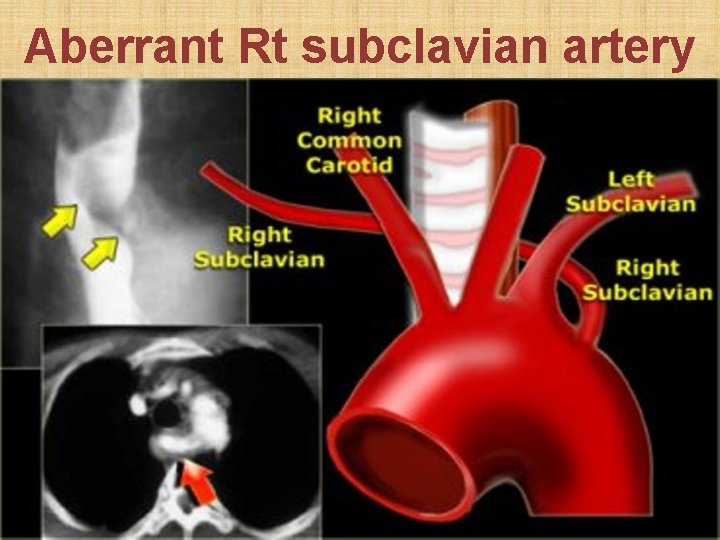
Aberrant Rt subclavian artery

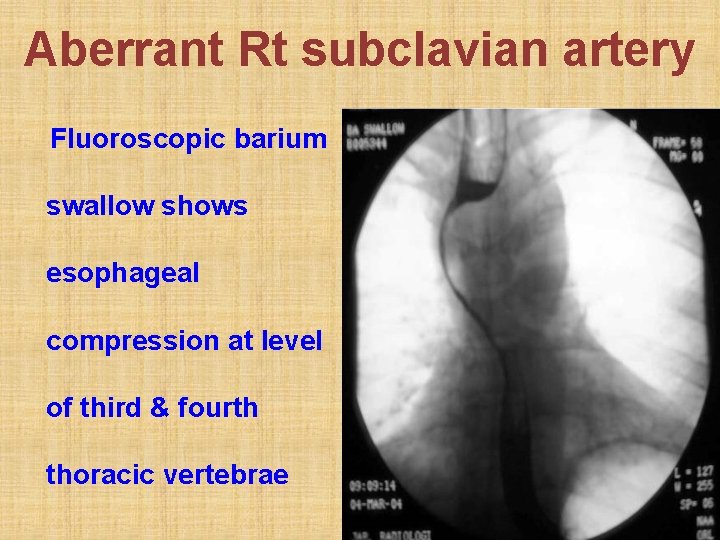
Aberrant Rt subclavian artery Fluoroscopic barium swallow shows esophageal compression at level of third & fourth thoracic vertebrae

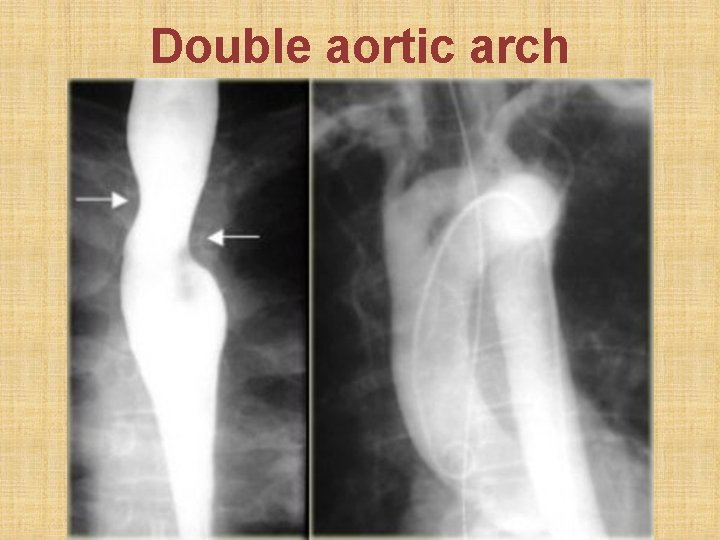
Double aortic arch

Aberrant left pulmonary artery

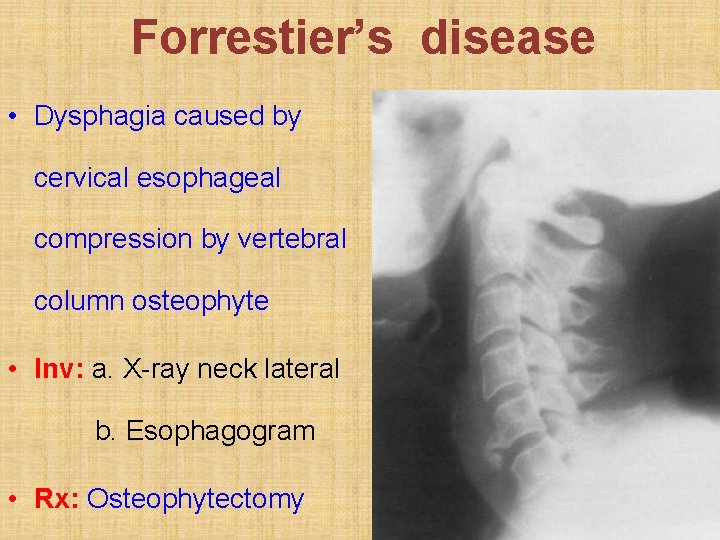
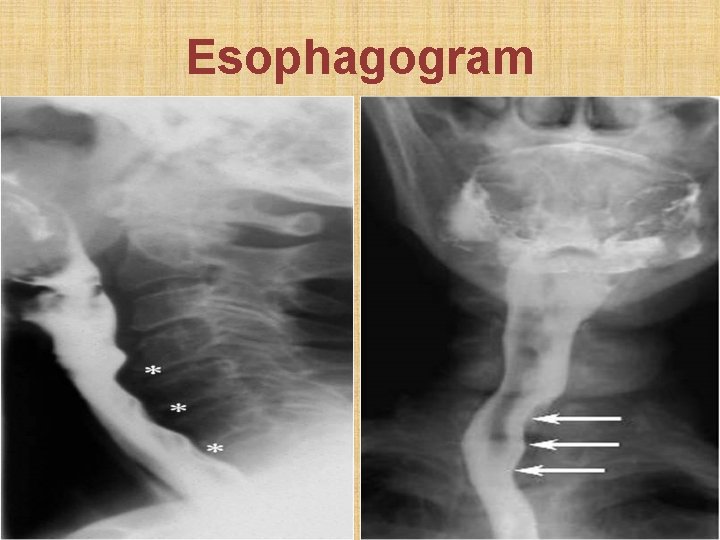
Forrestier’s disease • Dysphagia caused by cervical esophageal compression by vertebral column osteophyte • Inv: a. X-ray neck lateral b. Esophagogram • Rx: Osteophytectomy

Esophagogram

Esophageal neoplasm

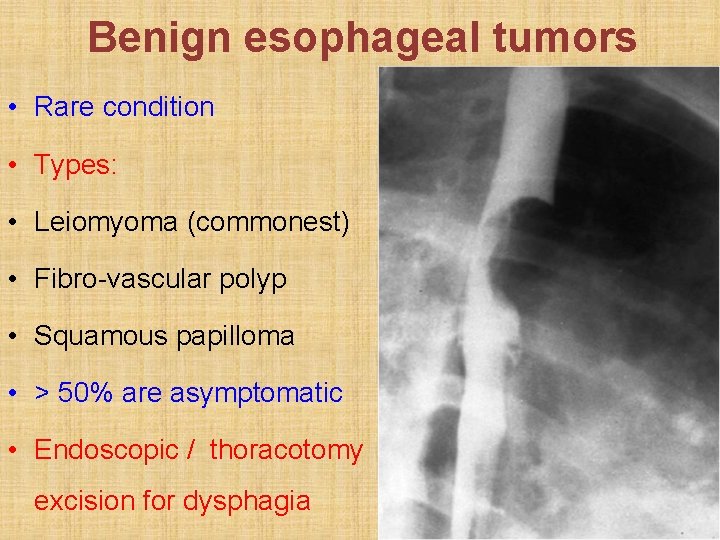
Benign esophageal tumors • Rare condition • Types: • Leiomyoma (commonest) • Fibro-vascular polyp • Squamous papilloma • > 50% are asymptomatic • Endoscopic / thoracotomy excision for dysphagia

Esophageal malignancy • Squamous cell carcinoma (upper 2/3 rd) • Adenocarcinoma (lower 1/3 rd) • Spindle cell carcinoma • Leiomyosarcoma • Lymphoma • Metastasis

Clinical features • progressive, painless dysphagia for solid foods • acute food bolus obstruction • weight loss in late stages • chest pain or hoarseness: mediastinal invasion • coughing after swallowing, pneumonia & pleural effusion: tracheo-esophageal fistula • cervical lymphadenopathy: node metastasis

Risk factors Smoking Alcohol consumption Betel nut chewing Tobacco chewing Vitamin A deficiency Vitamin C deficiency Barret’s esophagus Achalasia cardia Corrosive stricture Human Papilloma Virus Plummer Vinson syndrome Tylosis (familial hyperkeratosis of palms & soles)

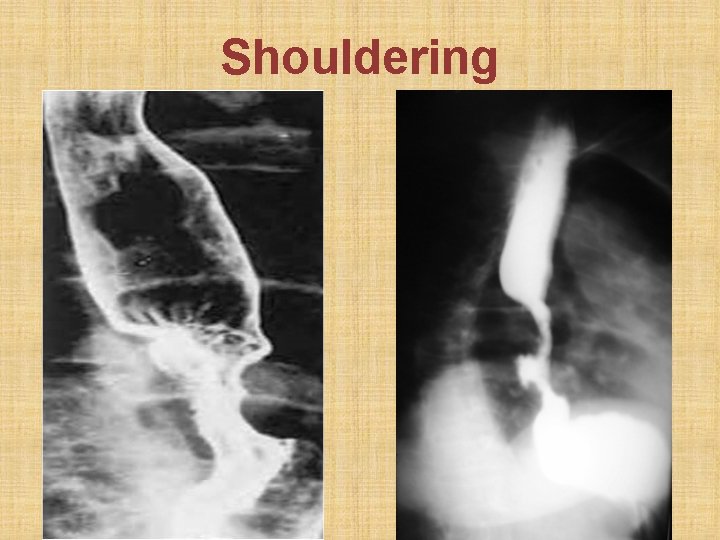
Investigations 1. Barium swallow: a. shouldering: malignant ulcer with everted margin b. rat tail appearance: narrow lower 1/3 rd with no proximal dilatation c. apple core appearance: narrow middle 1/3 rd only 2. Esophagoscopy & biopsy from growth 3. CT scan chest: for staging of malignancy

Shouldering

Rat tail appearance Also seen in advanced cases of achalasia cardia

Palliative treatment 70% patients have advanced disease at presentation & require palliative treatment 1. Endoscopic tumour ablation using laser 2. Low dose intra-cavitary radiotherapy 3. Indwelling feeding tube (Mousseau-Barbin, Celestin) 4. Feeding jejunostomy 5. Chemotherapy (5 Fluorouracil) 6. Nutritional support & analgesia with morphine

Definitive Treatment Upper 1/3 rd: early: radical radiotherapy (5500 c. Gy) advanced: chemo-radiation Middle 1/3 rd: early: radical RT or radical surgery advanced: radical surgery + CT Lower 1/3 rd: early: radical surgery advanced: radical surgery + CT Radical surgery: esophagectomy + gastrectomy + reconstruction with gastric / jejunal flap Chemotherapy (CT): Cisplatin + 5 -fluorouracil

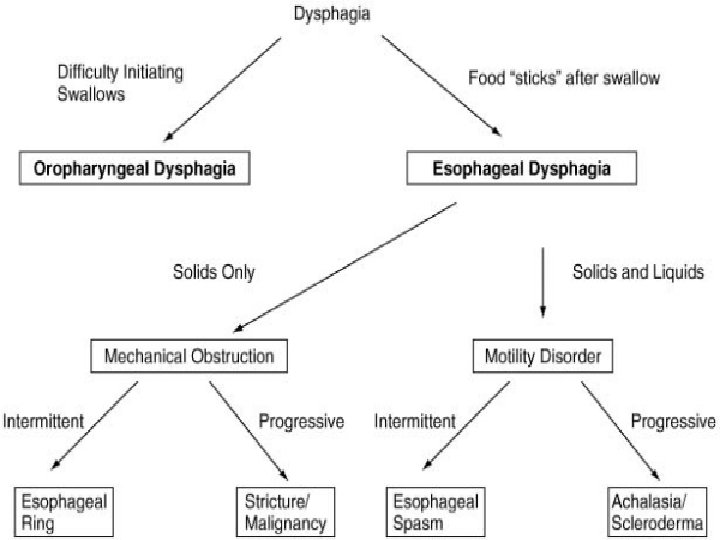
Evaluation of dysphagia

Extra-esophageal causes • Neoplasm: jaw / oral cavity / oropharynx / hypopharynx / supraglottis • Inflammation: TM joint arthritis / aphthous ulcer / Ludwig’s angina / tonsillitis / quinsy / epiglottitis / retropharyngeal abscess / parapharyngeal abscess • Paralysis: tongue / soft palate

Esophageal intra-luminal causes • Impacted foreign body / food bolus • Esophageal atresia • Esophageal web (Plummer Vinson Syndrome) • Esophageal ring (Schatzki’s ring) • Esophageal stricture: benign / malignant • Esophageal neoplasm: benign / malignant

Esophageal intra-mural causes • Inflammation: esophagitis (GERD commonest) • Hypomotility disorders: Achalasia / scleroderma • Hypermotility disorders: cricopharyngeal spasm / diffuse esophageal spasm / nutcracker esophagus • Other neuro-muscular disorders: Myasthenia gravis / Multiple sclerosis / Motor neuron disease

Esophageal extra-mural causes • Pharyngeal pouch • Hiatus hernia • Thyroid enlargement: benign / malignant • Mediastinal: Ca left bronchus / lymphadenopathy / cardiomegaly / aortic aneurysm / neoplasm • Vascular ring: dysphagia lusoria • Cervical spine osteophyte: Forrestier’s disease

History taking • Level of dyphagia: oral cavity / pharynx / esophagus • Acute onset: foreign body / trauma / inflammation • Intermittent: hypermotility disorder • Progressive: malignancy / stricture • More for liquids: neuromuscular disorder • Difficulty in initiation of swallow or after swallow • Fever + odynophagia: inflammation • Esophageal trauma / caustic ingestion

History taking • Hoarseness / stridor: laryngo-tracheal invasion • Hemoptysis: Ca bronchus • Heartburn: GERD • Hematemesis: esophageal varices • Regurgitation: pharyngo-esophageal obstruction • Neck mass: metastatic lymph node / goitre • Neurological disorder • Smoking & alcohol consumption


Examination • General: pallor + koilonychia = Plummer Vinson synd • Oral cavity, oropharynx • Indirect laryngoscopy: larynx, pyriform sinus, posterior pharyngeal wall, post cricoid area • Laryngeal crepitus: absent in post-cricoid malignancy, retropharyngeal abscess • Neck node & cranial nerve examination

Investigations • Barium swallow with or without air contrast • Video-fluoroscopic (modified) Barium swallow • Esophagoscopy: flexible & rigid • Esophageal manometry: achalasia, esophageal spasm • 24 hour double probe ambulatory p. H monitoring • Fibreoptic Endoscopic Evaluation of Swallowing with Sensory Testing (FEESST)

Investigations Bolus scintigraphy Chest X-ray: mediastinal mass / cardiomegaly CT scan chest: mediastinal or pulmonary tumor Bronchoscopy: Ca bronchus Thyroid scan: thyroid malignancy Angiography: vascular rings (dysphagia lusoria) Peripheral blood smear: Plummer Vinson syndrome

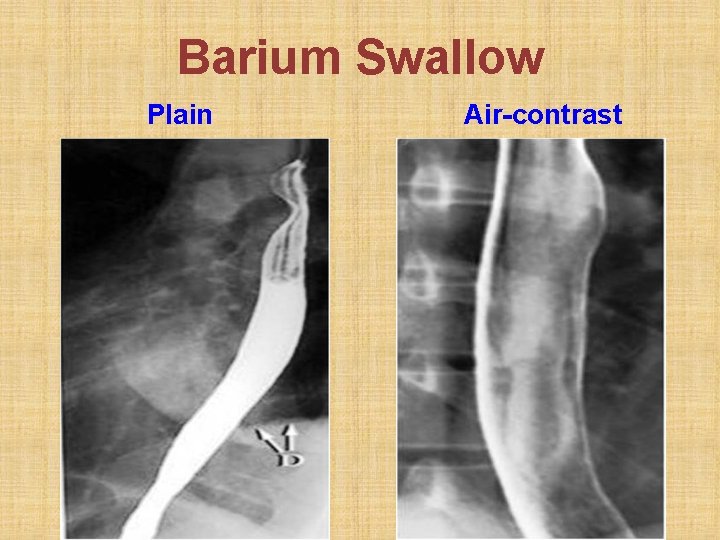
Barium Swallow Plain Air-contrast

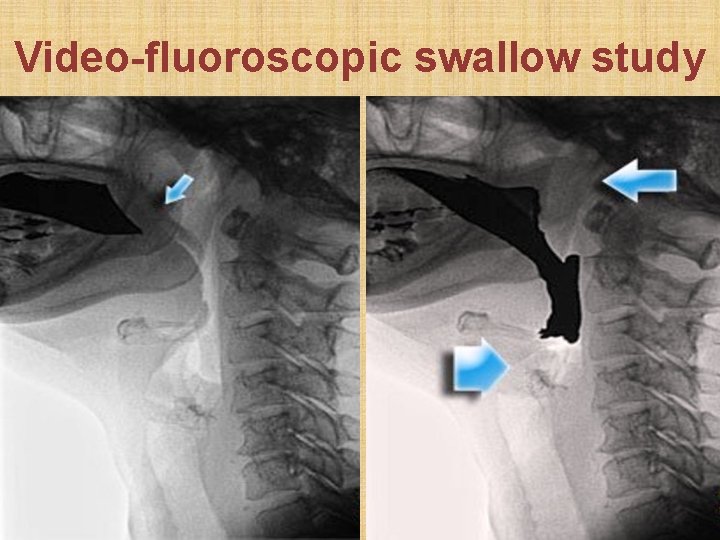
Video-fluoroscopic swallow study

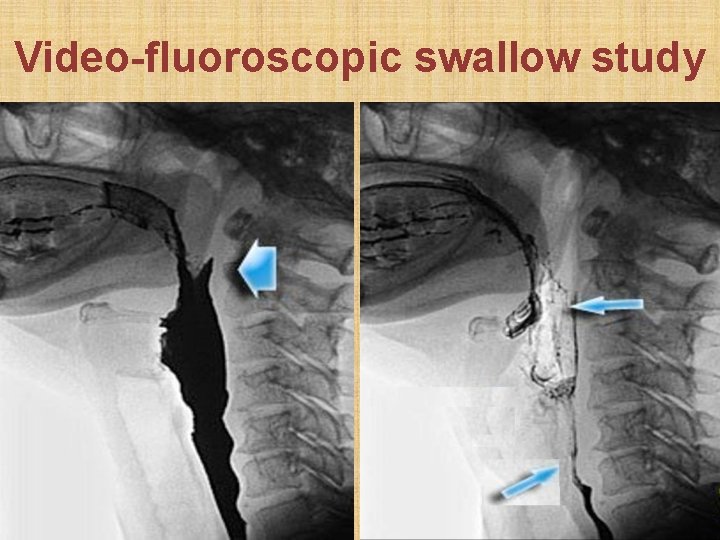
Video-fluoroscopic swallow study

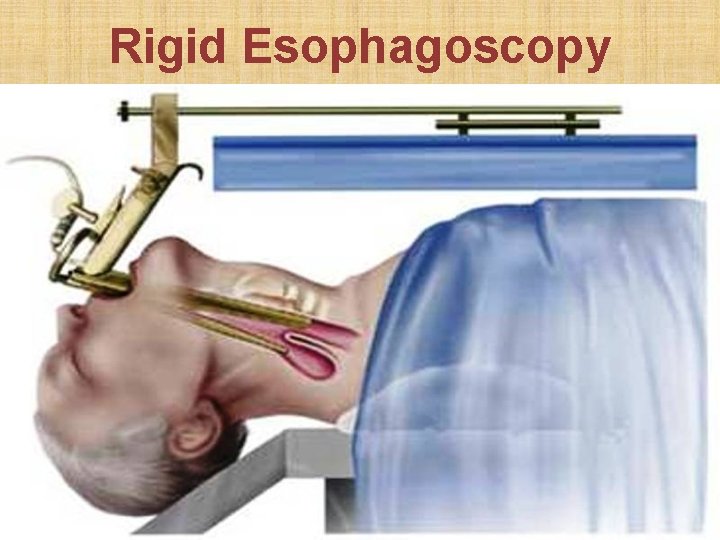
Rigid Esophagoscopy

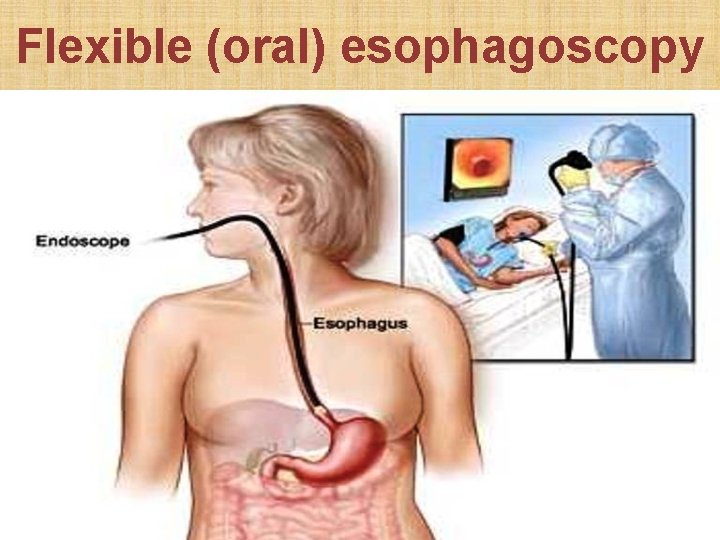
Flexible (oral) esophagoscopy

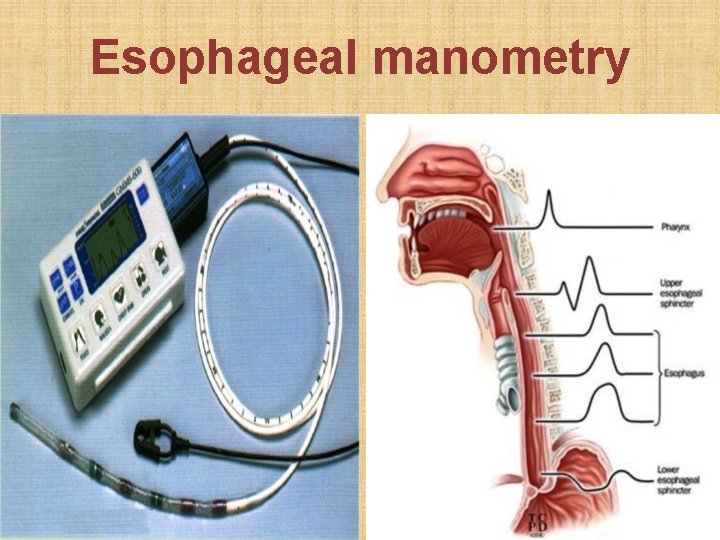
Esophageal manometry

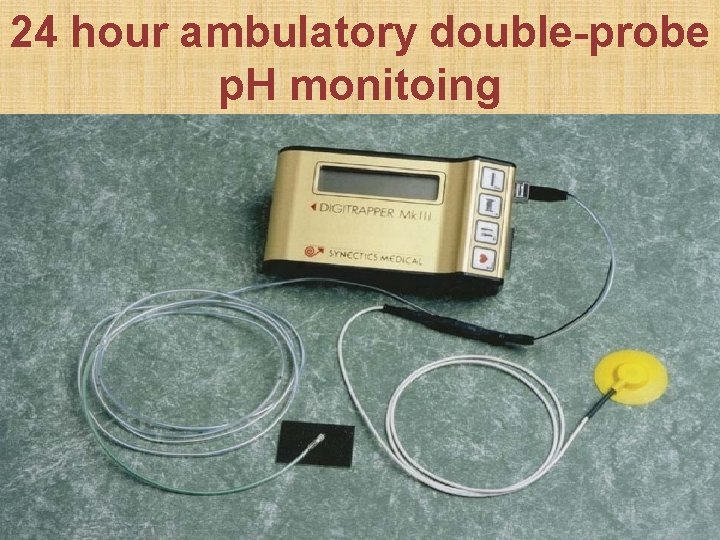
24 hour ambulatory double-probe p. H monitoing

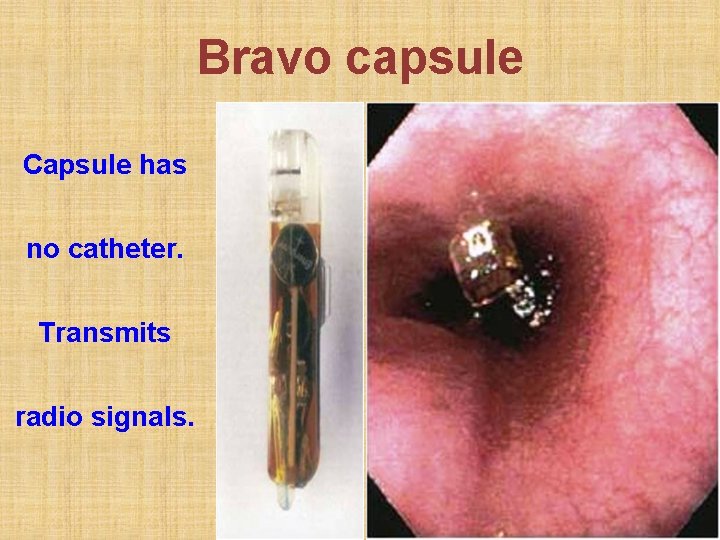
Bravo capsule Capsule has no catheter. Transmits radio signals.

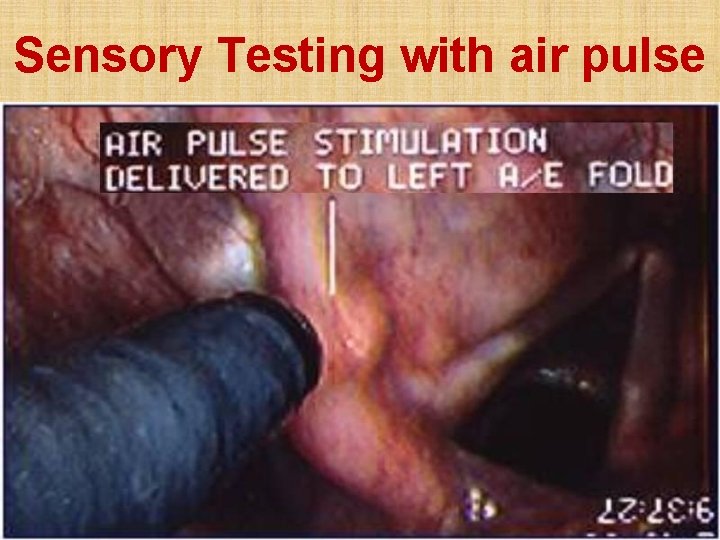
Fibreoptic Endoscopic Evaluation of Swallowing with Sensory Testing • Air-pulse stimuli delivered to ary-epiglottic fold mucosa innervated by superior laryngeal nerve to elicit laryngeal adductor reflex for airway protection • Swallowing evaluation performed with variety of food consistencies containing green food dye • Look for aspiration into larynx

Sensory Testing with air pulse

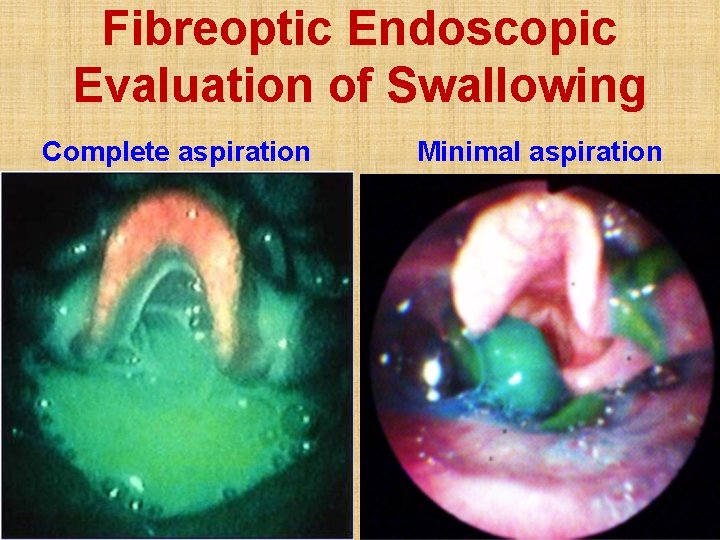
Fibreoptic Endoscopic Evaluation of Swallowing Complete aspiration Minimal aspiration

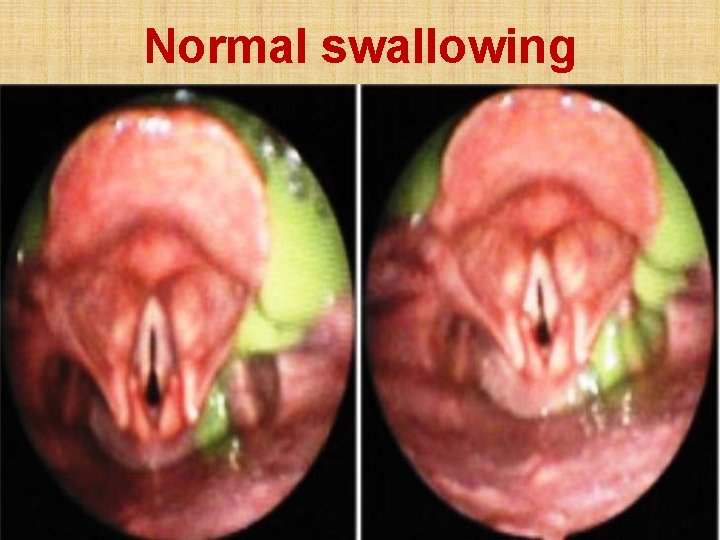
Normal swallowing

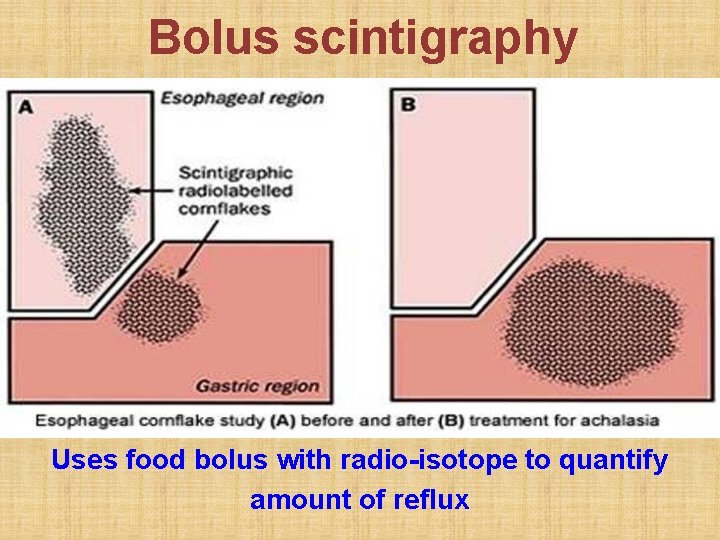
Bolus scintigraphy Uses food bolus with radio-isotope to quantify amount of reflux

Thank You