DISCUSSION ON SPORTS CONCUSSION Dr Isstelle Joubert Sports

DISCUSSION ON. . . SPORTS CONCUSSION Dr Isstelle Joubert Sports Meds, UFS 1 st year, 2011

SURFACE ANATOMY: q Cerebrum: ü largest + developmentally advanced portion ü controls higher functions • speech, emotion, integration of sensory stimuli, • initiation of final common pathways for movement • fine control of movement ü left hemisphere • controls the majority of functions on right side of the body ü right hemisphere • controls most of functions on left side of the body • injury to left: sensory and motor deficits on right side, vice versa
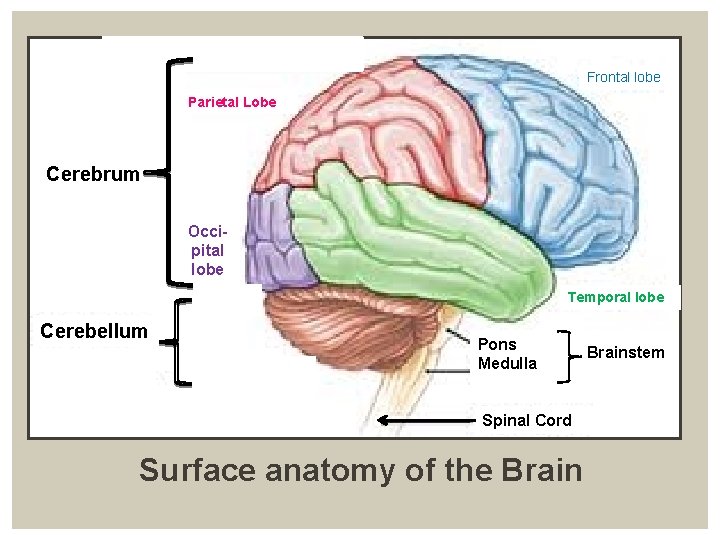
Frontal lobe Parietal Lobe Cerebrum Occipital lobe Temporal lobe Cerebellum Pons Medulla Spinal Cord Surface anatomy of the Brainstem

SURFACE ANATOMY: o frontal: planning, organizing, problem solving and selective attention • prefrontal cortex: personality, behaviour and emotions • back of frontal lobe: pre-motor, motor areas - produce / modify movement o parietal: primary sensory cortex controls sensation (touch and pressure) + fine sensation (judgment of texture, weight, size, and shape) • damage to R: visuo-spacial deficits, difficult in new / familiar places • damage to L: inability to understand spoken / written language

SURFACE ANATOMY: o temporal: differentiate smells + sounds help in sorting new information / short-term memory • right lobe: visual memory (i. e. , memory for faces and pictures) • left lobe: verbal memory (i. e. , memory for words and names) o occipital: • visual information - reception, recognition of shapes, colours damage: visual deficits
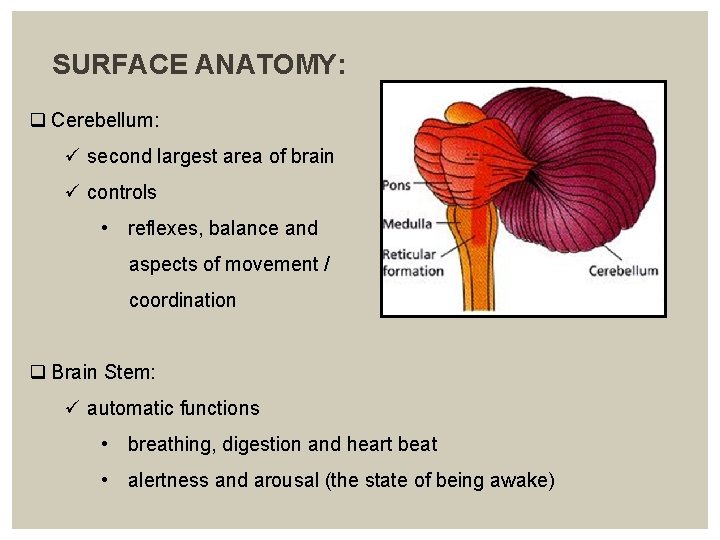
SURFACE ANATOMY: q Cerebellum: ü second largest area of brain ü controls • reflexes, balance and aspects of movement / coordination q Brain Stem: ü automatic functions • breathing, digestion and heart beat • alertness and arousal (the state of being awake)
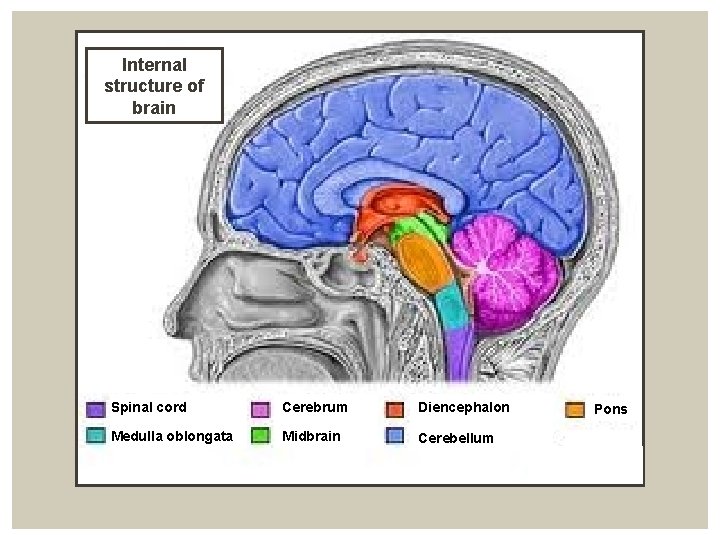
Internal structure of brain Spinal cord Cerebrum Diencephalon Medulla oblongata Midbrain Cerebellum Pons
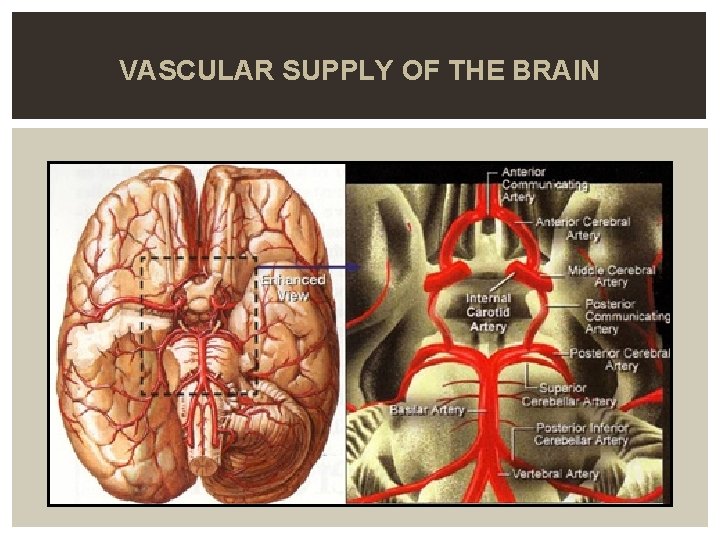
VASCULAR SUPPLY OF THE BRAIN

DEFINITION – SPORTS CONCUSSION: ü type of minor head injury ü complex patho-physiological process affecting the brain ü process is induced by traumatic bio-mechanical forces (brukner and khan 2009) ü trauma-induced change in mental state ü a mild form of brain injury ü with or without loss of consciousness (Patricios & Kohler et al, 2010)

DEFINITION: Consensus statement on Concussion in Sport (Zurich Nov 2008) common features: ü direct blow being a causative factor; ü rapid onset of neurologic impairment of short duration ü neuropathological changes - functional > structural ü graded set of clinical symptoms with / without LOC ü structurally normal neuro-imaging studies
SYNONYMS: ü brain concussion ü mild head injury ü minor head injury ü mild or minimal traumatic brain injury (Signoretti et al, 2010)

INCIDENCE: ü varies - level of play / different management protocols ü reported in all sports ü studied most widely in American football ü mostly ice hockey + American football (Meehan, Bachur, 2009) ü 1. 74 million concussions annually USA (2010) CDC ü football: 10% in US College athletes 20% in US high school athletes each season

INCIDENCE: q sex of athlete (soccer) ü 2 – 4 % concussions in male ü 3 – 5% in female players q non-reporting of concussions ü American football, only 47%, reported the injury (Meehan, Bachur, 2009)

INCIDENCE: q level of play ü 4 – 14% in sport at school level ü 3 – 23% at adult level (Shuttleworth-Edwards & Noakes et al, 2008) q level of play ü higher level of play – associated: ü increased strength and body size ü increased impact and momentum ü increased competitiveness ü longer seasons

PATHOPHYSIOLOGY: ü precise mechanism - not clear ü neurological deficit due to biomechanical injury • shearing forces • external forces transferred • to intracranial contents ü usually transient in character (brukner and khan 2009)

PATHOPHYSIOLOGY: ü shearing force -> diffuse axonal injury ü functional > structural injury ü molecular level: • in-flux of Ca 2+ , out-flux of K+ • due to depolarization • caused by excitatory neurotransmitters such as glutamate, acetylcholine and aspartate ü mitochondrial dysfunction ü inflammatory responses ü therefore changes in cellular physiology (Hayes & Dixon, 1994)
PATHOPHYSIOLOGY: ü restore pre-injury cell physiology + metabolism ü cell metabolism increase drastically: ü “hyper-metabolism” ü sodium-potassium-pump is in overdrive ü to increase the glucose metabolism ü to restore neuronal membrane potential ü ↑ cell metabolism + ↓ blood flow + ü disrupted glucose-supply-and-demand ü = energy crisis (cellular level) ü concussion symptoms and signs (Patricios & Kohler et al, 2010)
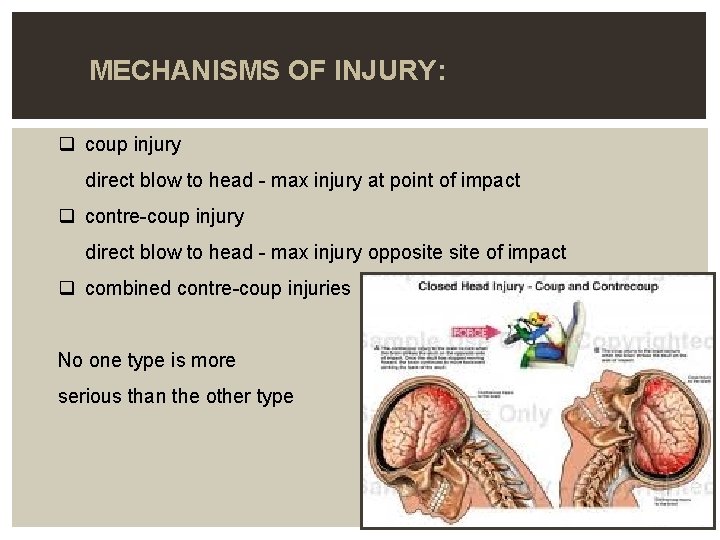
MECHANISMS OF INJURY: q coup injury direct blow to head - max injury at point of impact q contre-coup injury direct blow to head - max injury opposite of impact q combined contre-coup injuries No one type is more serious than the other type
MECHANISMS OF INJURY: 3 types of stresses : q compressive or crushing force q shearing force across parallel organization of brain tissue q tensile stress pulling / stretching of brain tissue Uniform compressive stress – fairly well tolerated by neural tissue

POSSIBLE COMPLICATIONS OF CONCUSSION: q Early complications ü intracranial space occupying lesion ↑ ICP due to damage to veins / arteries with bleeding - epidural / subdural / intracerebral ü second impact syndrome ü impact convulsions q Late complications ü post-concussion syndrome ü chronic traumatic encephalopathy ü risk of 2 nd concussion

Early complications ü intracranial space occupying lesion ü second impact syndrome (1 st in 1984) • athlete suffers another blow to head • before the previous concussion resolved completely • increased brain oedema from first injury didn’t disappear • 2 nd injury increases the oedema + ICP further • existence of syndrome questioned (Ropper 2009) • current literature recommend: concussed athletes do not RTP until / after all Sx and neuro-ab. N have resolved

Early complications ü impact convulsions • seizures not common • not associated with structural damage • good outcome • anti-convulsant - not indicated

Late complications ü post-concussion syndrome • Sx / Tx persist : few days to weeks • patient feels disturbed and debilitated • mostly in young concussed athletes • should rest completely from cognitive (thinking processes) and physical stress ü chronic traumatic encephalopathy • boxing - repeated concussions • eventually cognitive dysfunction • ? genetic factors could play a role (Apo E 4 genes)

Late complications ü risk of 2 nd concussion • very controversial statement • risk factors not clear • athlete’s style of play predispose him to concussion • age and level of play - expose athletes to greater forces • ? one brain injury - ↑ susceptibility for another injury (Schulz and Marshall, 2004)

SYMPTOMS AND SIGNS ASSOCIATED WITH CONCUSSION ü reported in the concussed athlete ü by the athlete self ü observed by family members, coaches or teammates
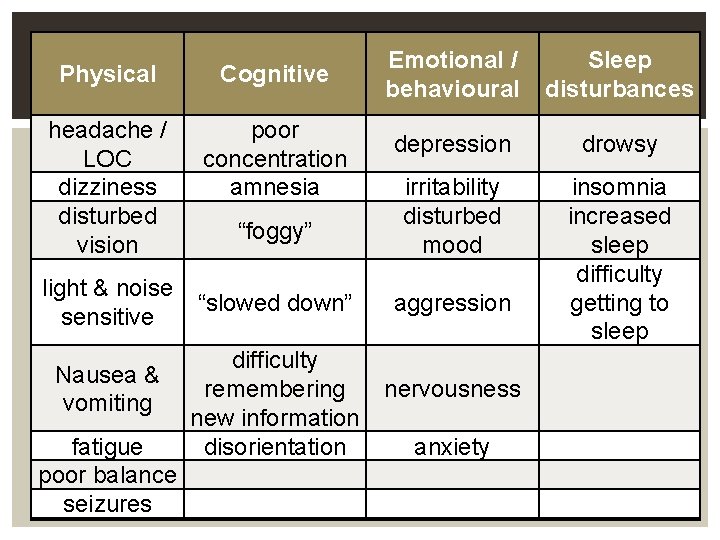
Physical Cognitive headache / LOC dizziness disturbed vision poor concentration amnesia “foggy” light & noise “slowed down” sensitive difficulty remembering new information fatigue disorientation poor balance seizures Nausea & vomiting Emotional / Sleep behavioural disturbances depression drowsy irritability disturbed mood insomnia increased sleep difficulty getting to sleep aggression nervousness anxiety

MANAGEMENT OF CONCUSSION: q Before the game: ü Pre participation evaluations ü Preparedness before onset of the game q Immediate management of the injured player: ü Exclude serious head and spinal injury, ü ATLS approach ü Remove player from field of play ü Assess severity of head injury

MANAGEMENT OF CONCUSSION: q Early management: ü Decide on : • urgent referral or not • return to play or not • baseline symptom analysis ü Hospital management ü Post-injury discharge information ü Follow-up consultations ü Neuropsychological evaluations q Late management ü Return to play indications

MANAGEMENT OF CONCUSSION: q neuro-psychological evaluations: v traditional DSST - digit symbol substitution testing v newer computerised testing like Im. PACT • assess degree of recovery – baseline / data • serial evaluations by an experienced • clinical assessment of brain’s ability to process information ü SCAT 2 assessment forms ü Acute Concussion Evaluation Forms (Gioia & Collins of CDC) ü Cog. State Sport as used by SA Rugby Union • neuropsychologist part of holistic management team • not via internet or telephone conversations

q neuro-psychological evaluations: ü Im. PACT (Immediate Post concussion assessment and cognitive testing) software program - University of Pitsburgh Medical Centre ü baseline test: brain processing, speed, memory, visual and motor skills ü some schools request baseline ü does not prevent concussion - detect subtle cognitive impairment ü aid to clinical decision - aid in determining safe return to play ü measure performance variability ü baseline data not affected by disease, medication, practice effects or malingering

WHAT IS NEW IN CONCUSSIONS. . . ? q Prevention possibilities q Evaluation possibilities q Medication possibilities q Management possibilities q Fighting the Ghosts

Prevention possibilities. . . ü ethical values - address violence, fair play and respect for other players ü muscle conditioning: • appropriate level of exercise tolerance • reduction of adiposity • increased flexibility, strength and aerobic capacity ü prevention of fatigue: • earlier substituting of fatigued player • attention to recovery of previous head injuries • attention to fitness, nutrition and hydration ü mouth guard /helmets: ↓ severity of concussion, doesn’t prevent • fit snugly, not move easily on head during the game • secured with neck + chin strap; tested to safety standards ü rules: • prevent front-on tackling / techniques of going to ground during a tackle

Evaluation possibilities. . . ü Cog. State ü Impact ü SCAT Medication possibilities. . . ü steroids ü anti-oxidants ü glutamate receptor antagonists ü hyperbaric oxygen ü hypothermia ü calcium channel blockers

Management possibilities. . . ü education of athletes, trainers or coaches and parents ü implementing the baseline testing that is available Fighting the Ghosts. . . ü “winna-mania” – player, coach, parent, media ü “winning isn’t everything, it’s the only thing” ü “play the man, leave the ball”

THE TAKE HOME MESSAGE IS. . . Concussion is real and not always preventable, but with the correct knowledge and management tools applied – the outcome is not necessarily poor. . .

REFERENCES: Brukner & Khan. Clinical sports medicine 3 rd revised ed. 2009(13)201 -206 Hayes RL, Dixon CE. Neurochemical changes in mild head injury. Semin Neurol 1994; 14: 25 Meehan WP & Bachur RG. Sport-Related Concussion. Pediatrics 2009; 123: 114 -123 Patricios JS, Kohler RMN, Collins RM. Sports-related concussion relevant to the South African rugby environment - A review. SAJSM 2010; 22(4): 88 -94

Ropper A, Gorson H. Concussion. N Engl J Med. 2007; 356: 166– 172 Schulz MR, Marshall SW et al. Bowling Incidence and risk factors for concussion in high school athletes, North Carolina, 1996 -1999. American Journal of Epidemiology. 2004; 160(10): 937 -944 Shuttleworth-Edwards AB, Noakes TD, Radloff S et al. The Comparative Incidence of Reported concussions presenting for Follow-up management in SA Rugby Union. Clinical Journal of Sport Medicine. Sept 2008; 18(5): 403 -409 Signoretti S, Vagnozzi R, Tavazzi B et al. Biochemical and Neurochemical Sequelae following mild traumatic brain injury: summary of experimental data and clinical implications. Neurosurg focus. 2010; 29(5): e 1
- Slides: 37