Dignity risk and choice in the care of
































- Slides: 34

Dignity, risk, and choice in the care of the elderly Whose Choice Is It? Ethics and Living at Risk NSHEN Annual Conference October 22, 2015 Best Western Burnside, Dartmouth NS

Hello! CATHERINE-ANNE MURRAY, OT(Reg NS) KATHRYN HOMINICK, MSW Senior’s Health Team Central Zone Nova Scotia Health Authority

Health care ethics at its simplest, is a set of moral principles, beliefs and values that guide us in making choices about medical care. At the core of health care ethics is our sense of right and wrong and our beliefs about rights we possess and duties we others. “

What “living at risk” looks like within our practice. “

Beginnings ◉In 2011 a quality assurance study was performed by a group from Geriatric Medicine Research at Capital Health in Halifax, Nova Scotia, examining care needs of patients classified as “sub-acute”. ◉An unexpected finding of this work was how frequently staff recommended “ 24 hr care” for older patients who were deemed to be somehow at risk if they were to return home.

Staff Workshop Themes Safety Oriented Culture – Focused on Physical Harm

Medical paternalism

50% ageism most tolerated social prejudice 79% agree that seniors 75 > are seen as less important and more ignored than younger generations Ageism

Professional and Personal Values

Practice Setting

Fear of liability

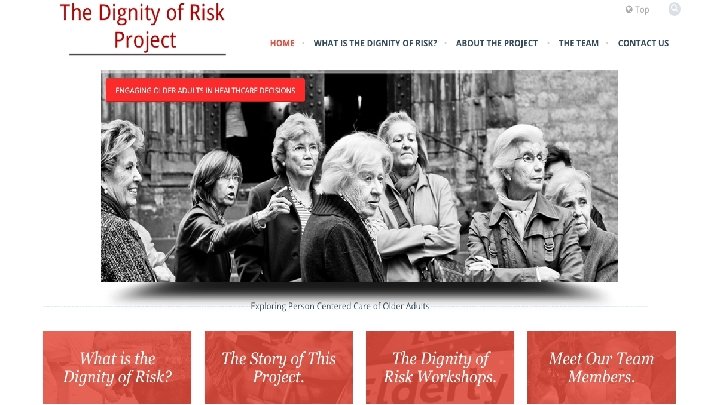
The Dignity of Risk “THE RIGHT OF PEOPLE TO TAKE RISKS WHEN ENGAGING IN LIFE EXPERIENCES AND THE RIGHT TO FAIL IN TAKING THESE. ”

Dignity of Risk Principles ◉1. Adults have the right to make their own decisions, and to be assumed to have capacity to do so unless shown otherwise – and capacity should be viewed as decision-specific. ◉2. A person should be offered all reasonable support and assistance in making and following through on their decisions before others step in to make decisions for them. ◉3. People have the right to make decisions that others feel are unwise or disagree with, the right to have a different tolerance for the risks associated with a decision, and the right to fail after making a decision. ◉4. When others are involved in decision making with person, any decisions must be made with the person’s best interest and preferences at the forefront, and must strive to infringe the least upon their basic rights and freedoms.

Duty of Care What does this mean to us as health care professionals? Do we need to view the Do. R and the Do. C in opposition? “Is the patient safe to go home” Or “You want to go/stay home? Let’s see how we can help you get there” “You want to go to the bathroom yourself, you’re a bit unsteady, but let’s explore ways or strategies to minimize the risks and still be able to go yourself.

Consider our Duty of Care to include… Valuing and working with older adults’ values, preferences, and wishes, Even in the presence of cognitive impairment, and facing the challenges in care planning, that go hand in hand with this approach

How does our perception of risk change if…?

So then how does the Dignity of Risk translate into practice? ◉Start small and go from there ◉Have open and supportive conversations with co-workers, allow ourselves to be challenged re ageism ◉Be aware of language ◉Balanced conversations about risk

See Risk as a Positive Value ◉Enhanced quality of life ◉True patient-centered care? ◉Autonomous/Relational Autonomy - Decision making ◉Creating a system that supports our risks when we are older.

Why caring for individuals living at risk can be so challenging: The Ethical Issues “

Dementia and it’s complexity ◉Lack of insight 2/3 of people with dementia ◉Relational autonomy/Collateral ◉Dementia diagnosis can initiate ageism/paternalism and stigma ◉Progressive disease ◉Changing care plans ◉Capacity

Relational autonomy

Risk to self and others

Capacity

Discussion/Thoughts?

Share an example of a time when the Dignity of Risk principle was well supported, or challenged, with an older adult. What did this look like?

Thank You Any questions ? You can find us at catherine-anne. murray@nshealth. ca kathryn. hominick@nshealth. ca


How can we support families’ comfort level with risk? Consider within the settings of hospital, long term care, or at home.

Let’s dive in – Hospital scenario ◉Mrs. D is 83 and was admitted to hospital after falling at home and fracturing her pelvis. She was started on pain meds in the ED, however this has contributed to a delirium ◉Mrs D has a dementia that is undiagnosed. She re-wears clothing at times, has difficulty using the stove, has missed her medications at times, 3 falls in the past 3 months, and thinks she’s managing fine at home. ◉Her daughter “loses sleep at night” worrying about her and helps her with pre-made meals 3 -4 x/week. She does not think her mom is safe to return home. ◉She’s now on an acute care floor for discharge planning

And what about at home? ◉Mr and Mrs T both have dementia, Mrs T later stages, but physically well and is exit seeking, Mr T moderate stages and wants to place indoor locks on the doors to keep her from leaving. Home care and VON are involved. ◉Mr. W has Lewy Body and leaves their downtown apt at least once a day ◉Mr D’s son wants his capacity assessed, or a health care professional has asked

Medical Ethics ◉Autonomy ◉Confidentiality ◉Beneficence ◉Disclosure ◉Non-maleficence ◉Informed Consent ◉Justice

What do we do when… ◉Mrs. D wants to go home, but she still has resolving delirium ◉Mrs. D has undiagnosed dementia and some team members are worried about her returning home? ◉Mrs. D is incontinent at home, and her bed sheets are often soiled ◉Mrs. D is driving and she likely has mild-moderate dementia ◉Mrs. D’s dtr is so stressed, she has voiced her desire to withdrawal from situation if she goes home. ◉Mrs. D. dtr is stressed about how repetitive and forgetful she is becoming. ◉Mrs. D has fallen once on the way to the bathroom in hospital, but still wants to get up on her own. ◉Mrs. E has wandered into another patient’s room and shook her cane at another patient.

Slides. Carnival icons are editable shapes. This means that you can: ● Resize them without losing quality. ● Change line color, width and style. Isn’t that nice? : ) Examples:

Instructions for use Open this document in Google Slides (if you are at slidescarnival. com use the button below this presentation) You have to be signed in to your Google account EDIT IN GOOGLE SLIDES EDIT IN POWERPOINT® Go to the File menu and select Make a copy. Go to the File menu and select Download as Microsoft Power. Point. You will get a. pptx file that you can edit in Power. Point. You will get a copy of this document on your Google Drive and will be able to edit, add or delete slides. Remember to download and install the fonts used in this presentation (you’ll find the links to the font files needed in the Presentation design slide) More info on how to use this template at www. slidescarnival. com/help-use-presentation-template This template is free to use under Creative Commons Attribution license. If you use the graphic assets (photos, icons and typographies) provided with this presentation you must keep the Credits slide.