Dignity Health Plan Model of Care Training 1































- Slides: 34

Dignity Health Plan Model of Care Training 1

What if…? You were building Medicare from the ground up? Would you build a system that focuses on reacting to patient problems, or Would you build a system that focuses on preventing patient problems? What would you prefer as a patient? 2

Objectives • Understand an Institutional Special Needs Plan (ISNP) • Concepts • Benefits • Identify Key Personnel • Define and explain the Dignity Health Plan Model of Care (MOC) • Discuss clearly defined MOC roles and obligations • Understand concept of Skill in Place 3

Institutional-Equivalent Special Needs Plan Ne w • Types of Special Needs Plans (IE-SNP) For Medicare beneficiaries with conditions that would otherwise qualify them for I-SNP, but they don’t live in a Licensed LTC Facility A Special Needs Plan (SNP) is a Medicare Advantage (MA) coordinated care plan specifically designed to provide targeted care to special needs individuals. Each require a unique Model of Care. There are three types: Chronic Condition SNP (C-SNP) • For Medicare beneficiaries with a special medical condition (such as Diabetes) Dual Eligible SNP (D-SNP) • For Medicare beneficiaries who are also eligible for Medicaid Institutional SNP (I-SNP) • For Medicare beneficiaries who reside in a longterm care facility 4

Institutional Special Needs Plan (I-SNP) Concepts • Established by the Medicare Modernization Act of 2003 • Congress created a new type of Medicare Advantage Plan that focuses on beneficiaries that have special needs and would benefit from focused coordination of care • Replaces traditional Medicare and is an all-in-one plan covering inpatient and SNF care (Part A), outpatient and primary care (Part B), and prescription drugs (Part D). 5

Advantages of an ISNP • Preventive and proactive care vs traditional reactive, which results in: • Lower medical and drug costs • Improved patient satisfaction • Avoidance of unnecessary hospitalizations, ED visits, and costly specialty care Actively triage and manage patients by hospitalization (stratification) risk Improve member ability to determine Individual Care Goals via an Individualized Care Plan Leverage early detection in changes of condition and address problems sooner in the disease process Improve communication and coordination with the primary care physician, members, family, and the facility staff • Improve measurable quality of care metrics • Appropriately, completely, and accurately document the member’s medical conditions per HCC coding practices. • Achieve compliance with appropriate screenings/testing to meet CMS Quality Outcome Measures (HEDIS) and achieve a high Star Rating • • 6

Chapter 42 of the Code of Federal Regulations, Part 422 (42 CFR 422. 101 (f)(2)(ii)) mandates that Special Needs Plans (SNPs) conduct SNP Model of Care (MOC) training for all contracted providers. The Special Needs Plans Model of Care is the evidence-based process by which we integrate benefits and coordinate care for customers enrolled in Dignity’s Institutional Special Needs Plan. 7

Benefits of Dignity Health Plan • Dignity Health Plan offers all the benefits of traditional Medicare, including Part D prescription drug coverage + additional benefits to patients such as: • Dental: $500 allowance preventive and comprehensive • Vision Care: $300 allowance for frames/lenses • Hearing Exam and Hearing Aids: $1000 allowance • Nurse Practitioner on site to coordinate preventive and proactive medical care and advocate for member’s health • Coming in 2021 – Over the Counter Benefit Catalogue! 8

Model of Care • Every I-SNP must have a CMS approved Model of Care (MOC) • Provides basic framework under which the plan will meet the needs of its members • Serves as foundation for promoting quality, care management, and care coordination processes 9

Dignity Model of Care Components MOC 1: Description of the SNP Population • Description of Overall SNP Population • Sub-Population: Most Vulnerable Beneficiaries MOC 2: Care Coordination • SNF Staff Structure • Health Risk Assessment Tool (HRAT) • Individualized Care Plan (ICP) • Interdisciplinary Care Team (ICT) • Care Transition Protocols MOC 3: SNP Provider Network • Specialized Expertise • Use of Clinical Practice Guidelines & Care Transition Protocols • MOC Training for the Provider Network MOC 4: Quality Measurement & Performance Improvement • MOC Quality Performance Improvement Plan • Measurable Goals & Health Outcomes for the MOC • Measuring Patient Experience of Care (SNP Member Satisfaction) • Ongoing Performance Improvement Evaluation of the MOC • Dissemination of SNP Quality Performance Related to the MOC 10

Dignity Enrollment Eligibility • CMS restricts ISNP enrollment to eligible individuals who: • • • Reside in a long-term care facility for 90 days or longer No plan for discharge Enrolled in Medicare Part A and Part B No End Stage Renal Disease Geography: Qualifying parishes in Louisiana 11

Dignity Model of Care Components MOC 1: Description of the SNP Population • Description of Overall SNP Population • Sub-Population: Most Vulnerable Beneficiaries MOC 2: Care Coordination • SNF Staff Structure • Health Risk Assessment Tool (HRAT) • Individualized Care Plan (ICP) • Interdisciplinary Care Team (ICT) • Care Transition Protocols MOC 3: SNP Provider Network • Specialized Expertise • Use of Clinical Practice Guidelines & Care Transition Protocols • MOC Training for the Provider Network MOC 4: Quality Measurement & Performance Improvement • MOC Quality Performance Improvement Plan • Measurable Goals & Health Outcomes for the MOC • Measuring Patient Experience of Care (SNP Member Satisfaction) • Ongoing Performance Improvement Evaluation of the MOC • Dissemination of SNP Quality Performance Related to the MOC 12

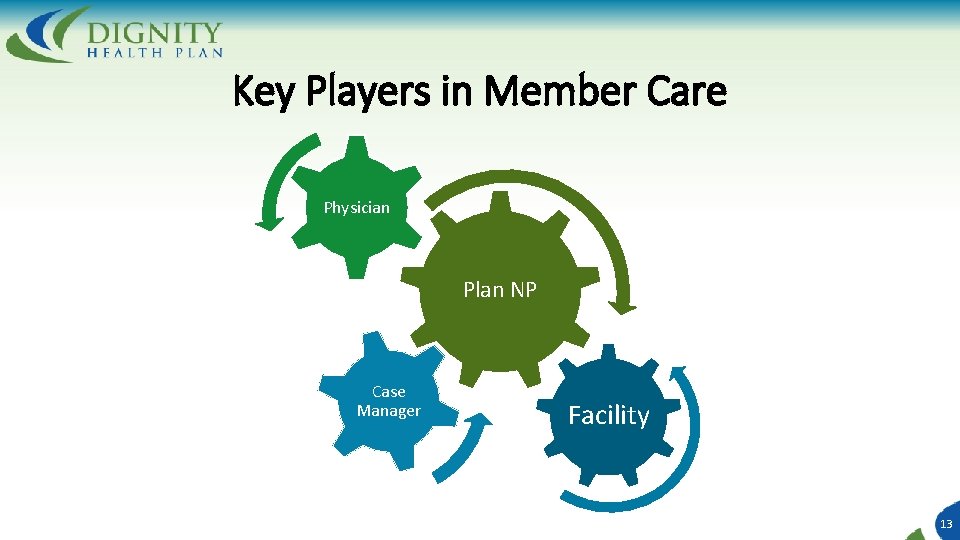
Key Players in Member Care Physician Plan NP Case Manager Facility 13

Physician (PCP) Provide oversight and primary care services to plan members Participate in care coordination efforts Performs usual regulatory visits When available, participates in Interdisciplinary Care Team (ICT) meetings to identify a change in beneficiary status and services needs/issues • Collaborates with Plan NP in Individualized Care Plan (ICP) development • • 14

Plan Nurse Practitioner (NP) • Serves as the cornerstone and the center of care management for the member • Performs complete member assessments, including Heath Risk Assessments (HRAs) • Conducts clinical assessments on an ongoing basis based on risk of hospitalization and episodic changes in conditions • Determines when a higher level of skilled care is necessary for a member • Facilitates early diagnosis, intervention, communication, and delivery of the appropriate quality medical services in a cost-effective manner • When needed, interfaces with other practitioners to help facilitate access to all service 15

RN Case Manager • Partners with Plan NP in coordinating care management for plan members • Assists Plan NP with Utilization Management – Prior Authorization Process • As the Plan grows in size and scope: • Identifies changes in condition each morning from facility – reporting mechanism • Ensures the implementation of the Individualized Care Plan (ICP), as well as monitoring and updating ICP as needed • Collaborates with Interdisciplinary Care Team (ICT) in assessment, planning, facilitation, and advocacy for an individual’s health needs • Facilitates discharge planning and transition of care activities • Provides education to members, facilities, and nursing home staff 16

Facility • Continues to house, care for, and maintain health of member population • Communicates changes in condition to Plan NP and/or RN Case Manager quickly • Works with NP and Case Manager to prevent unnecessary ED visits and hospitalizations • Works with NP and RNCM on cost-effective care and medication/therapy options • Understands concepts of ISNP Model of Care and managing residents with aggressive care in place strategies • Participates in Interdisciplinary Care Team (ICT) meetings and discussions 17

Managing Sick in Place “Skilling in Place” • Goal: Reduce hospitalizations by utilizing facility and facility staff proactively and effectively to provide comfortable, convenient, and costeffective nursing care instead of sending the patient to the hospital • Promotes a proactive approach to treatment. • Treat early • Treat aggressively and effectively 18

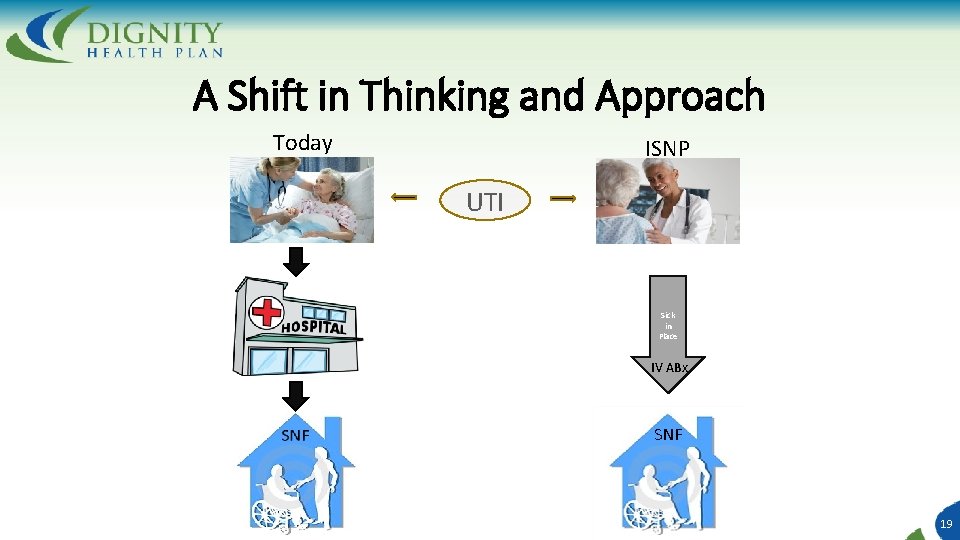
A Shift in Thinking and Approach Today ISNP UTI Sick in Place IV ABx SNF 19

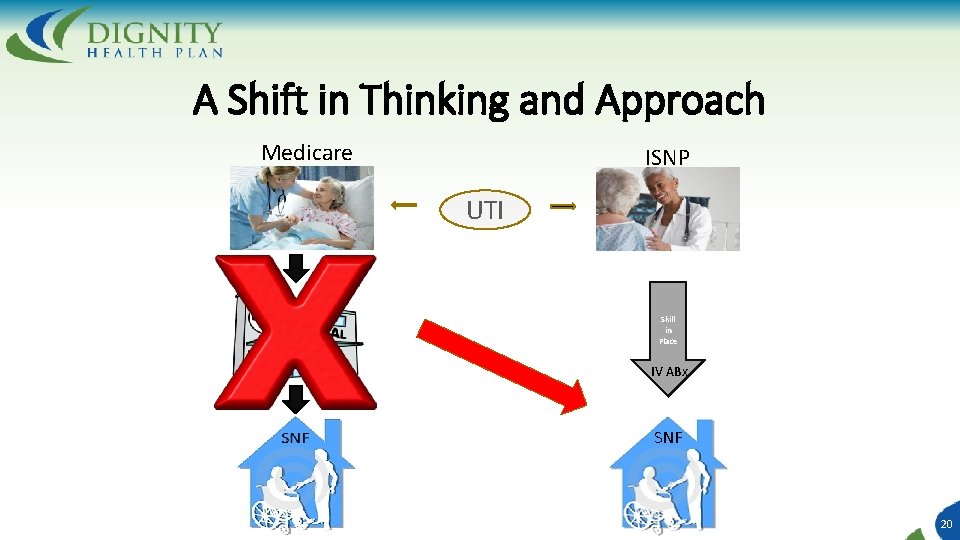
A Shift in Thinking and Approach Medicare ISNP UTI Skill in Place IV ABx SNF 20

Examples of Qualifying Skill in Place (SIP) Conditions • Conditions, with appropriate qualifying diagnostic criteria, that may qualify for SIP include: • • Pneumonia Congestive Heart Failure exacerbation/decompensation COPD/Asthma exacerbation Skin Infection such as Cellulitis or acutely worsening wound Severe Dehydration/Volume Depletion Urinary Tract Infection Other similarly acute qualifying conditions 21

Prior Authorizations PA • The following services require Prior Authorization from Dignity: • • • • Inpatient Hospitalization – Acute Inpatient Hospitalization – Psychiatric Skilled Nursing Facility Care (i. e. , return to facility from hospital) Skill in Place Home Health Services Occupational Therapy Services Physical Therapy Services Speech Pathology Services Outpatient Diagnostic and Therapeutic Radiology Services Ambulatory Surgery Center Services Durable Medical Equipment Prosthetics/Medical Supplies in excess of $500 Dialysis Services Medicare Part B Prescription Drugs if over $500 22

Health Risk Assessment - HRA • The Health Risk Assessment (HRA) is a comprehensive questionnaire and assessment of the Member’s current health status that estimates their level of health risk and facilitates their Individual Care Plan (ICP) • Components: • • • Medical History Functional Status Cognitive screening Psychosocial screening Mental Health screening 23

Health Risk Assessment (cont. ) • Requirements: • Complete within 90 days of the effective start date for each newly enrolled member • Subsequent assessment performed in response to significant events and/or changes in member condition and at least annually • Outcomes: • • • Questions use algorithms to weigh responses and determine risk level Calculates High, Medium, or Low Acuity Risk Score determines member’s stratification for proactive medical management Acuity Risk Score should be updated with each HRA completed Essential to risk adjustment factor (RAF), payment, and monitoring 24

Individualized Care Plan - ICP Measurable goals reflecting clinical, behavioral, and/or social needs • The ICP addresses issues the member may be facing within these areas: • • • Medical Psychosocial Behavioral Cognitive Functional Pharmaceutical • ICP developed by: • Low and Medium Risk members: RN Case Manager in consultation with the Plan NP as needed. • High Risk members: RN Case Manager in coordination with the Plan NP. Both are co-owners of the ICP. 25

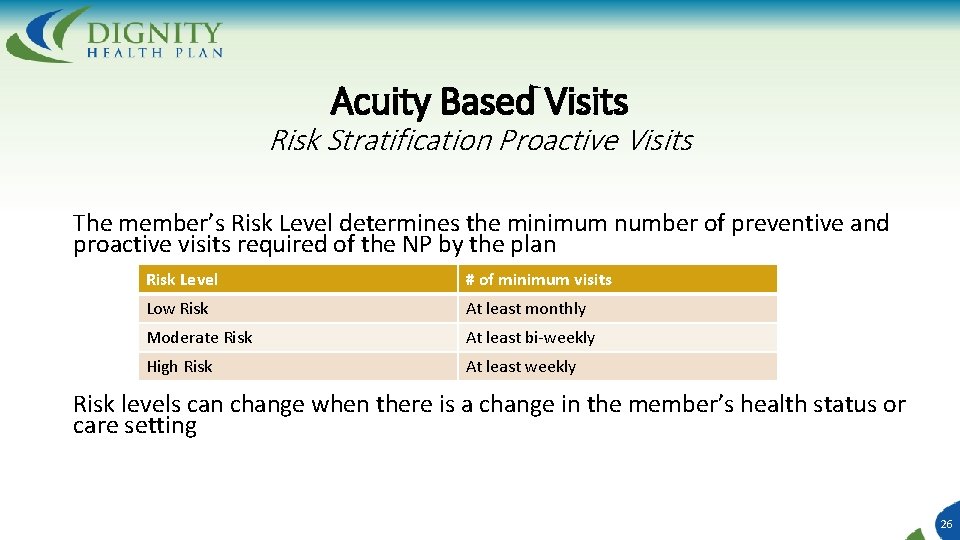
Acuity Based Visits Risk Stratification Proactive Visits The member’s Risk Level determines the minimum number of preventive and proactive visits required of the NP by the plan Risk Level # of minimum visits Low Risk At least monthly Moderate Risk At least bi-weekly High Risk At least weekly Risk levels can change when there is a change in the member’s health status or care setting 26

Interdisciplinary Care Team - ICT Comprehensive and integrated communications network that discusses the care plan, health status, and current/possible interventions for the member The ICT is responsible for addressing the entire spectrum of care for the member • The ICT is comprised of: • • • The Member’s family, caregiver, or legal representative The Nurse Practitioner The RN Care/Case Manager The member’s PCP Specialists Ancillary healthcare providers The Plan’s Chief Medical Officer (as needed only) The Plan’s Clinical Pharmacist (as needed only) Any other entity/persons involved in the member’s 27

Interdisciplinary Care Team (cont. ) • NP and RN Case Manager can be the primary contact for the member and supports the ICT to coordinate care for the members across care settings and providers. • The ICT meetings will be conducted on a scheduled frequency based on the member’s risk level • All meetings and communications are documented in Apropos, the Care Management System. • ICT approach ensures that each beneficiary has timely access to care, to the opportunity for improved health outcomes that eliminate barriers to accessing services, and to ensure the appropriate use of health care services. 28

Care Transitions Continuity of Care of Members Avoiding unnecessary, costly, and disabling hospitalizations is an important goal of Member continuity of care Members do occasionally require and experience transitions in care, which require close coordination and constant, directionally-focused communications throughout the entire spectrum of services 29

Care Transition Components • Timely data sharing between settings • Safe, timely, and effective transitions • Education for the Member and/or their caregiver on the reason(s) for the transition • Updates provided to all parties throughout the care transition • Follow-up with Member and Family during inpatient admission, throughout the stay, and discharge • Completion of an initial follow-up assessment, medication reconciliation, and abbreviated HRA within 3 business days of inpatient discharge • Reviewal and revision of ICP, engaging Member, Caregivers, and all other involved parties, as appropriate 30

Dignity Model of Care Components MOC 1: Description of the SNP Population • Description of Overall SNP Population • Sub-Population: Most Vulnerable Beneficiaries MOC 2: Care Coordination • SNF Staff Structure • Health Risk Assessment Tool (HRAT) • Individualized Care Plan (ICP) • Interdisciplinary Care Team (ICT) • Care Transition Protocols MOC 3: SNP Provider Network • Specialized Expertise • Use of Clinical Practice Guidelines & Care Transition Protocols • MOC Training for the Provider Network MOC 4: Quality Measurement & Performance Improvement • MOC Quality Performance Improvement Plan • Measurable Goals & Health Outcomes for the MOC • Measuring Patient Experience of Care (SNP Member Satisfaction) • Ongoing Performance Improvement Evaluation of the MOC • Dissemination of SNP Quality Performance Related to the MOC 31

Provider Network • The Plan is building a Provider network that includes all Provider types, such as: • • Facilities Primary Care Physicians Specialists Behavioral and Mental Health Specialists Labs, X-Rays, Specialized Imaging Nursing Professionals Allied Health Professionals (pharmacy, therapists, etc. ) • The provider network is reviewed on an ongoing basis for adequacy and gaps in the types of specialty care needed to provide services for beneficiaries 32

Dignity Model of Care Components MOC 1: Description of the SNP Population • Description of Overall SNP Population • Sub-Population: Most Vulnerable Beneficiaries MOC 2: Care Coordination • SNF Staff Structure • Health Risk Assessment Tool (HRAT) • Individualized Care Plan (ICP) • Interdisciplinary Care Team (ICT) • Care Transition Protocols MOC 3: SNP Provider Network • Specialized Expertise • Use of Clinical Practice Guidelines & Care Transition Protocols • MOC Training for the Provider Network MOC 4: Quality Measurement & Performance Improvement • MOC Quality Performance Improvement Plan • Measurable Goals & Health Outcomes for the MOC • Measuring Patient Experience of Care (SNP Member Satisfaction) • Ongoing Performance Improvement Evaluation of the MOC • Dissemination of SNP Quality Performance Related to the MOC 33

Quality Measurement and Performance Improvement • The Plan is committed to improving the quality of health for its beneficiaries • Monitoring and evaluation of health outcomes and implementation of the Model of Care is performed on an ongoing basis • Examples include: • • Timely completion of proactive, preventive visits, Hospital Admissions per thousand, HEDIS measures, Member satisfaction 34