DIFFUSE ALVEOLAR HEMORRHAGE SYNDROM Katarina Osolnik University Clinic














- Slides: 17

DIFFUSE ALVEOLAR HEMORRHAGE SYNDROM Katarina Osolnik University Clinic of Respiratory and Allergic Diseases, Golnik, Slovenia Portorož, May 8 th 2009

DIFFUSE ALVEOLAR HEMORRHAGE • • • acute, life-threatening event repeated episodes can lead to: organizing pneumonia collagen deposition in small airways fibrosis

DIFFUSE ALVEOLAR HEMORRHAGE • • Wegener granulomatosis microscopic polyangiitis Goodpasture syndrome connective tissue disorders antiphospholipid antibody sy infectious or toxic exposures neoplastic conditions

CAUSES OF DIFFUSE ALVEOLAR HEMORRHAGE • vasculitis or capillaritis • pulmonary haemorrhage without capillaritis or vasculitis (» bland « pulmonary haemorrhage) • alveolar bleeding associated with another process or condition

CLINICAL MANIFESTATIONS Acute or subacute (present for less than a week) • dyspnea, • cough, • fever, • haemoptysis are the most common clinical manifestations of DAH. *Haemoptysis may be absent at time of presentation in up to a third of patients.

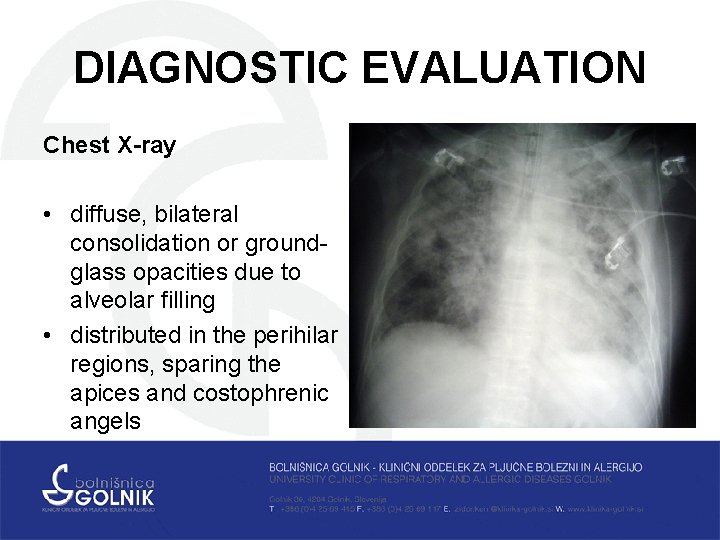
DIAGNOSTIC EVALUATION Chest X-ray • diffuse, bilateral consolidation or groundglass opacities due to alveolar filling • distributed in the perihilar regions, sparing the apices and costophrenic angels

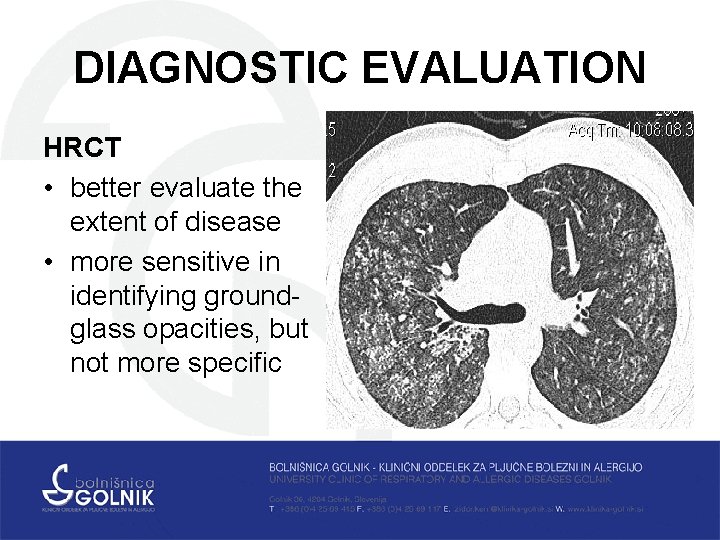
DIAGNOSTIC EVALUATION HRCT • better evaluate the extent of disease • more sensitive in identifying groundglass opacities, but not more specific

DIAGNOSTIC EVALUATION Laboratory tests • anemia, leukocytosis • ESR, CRP • blood urea and serum creatinine, abnormal findings of urin analysis in pulmonary-renal sy • anti-GBM, ANCA, C 3 and C 4, anti-ds-DNA, antiphospholipid Ab Pulmonary function test • increased diffusing capacity • restrictive changes • obstructive changes

DIAGNOSTIC EVALUATION Bronchoscopy • to document alveolar hemorrhage by BAL • to exclude airway sources of bleeding • to exclude an associated infection Within the first 48 hours of symptoms the diagnostic yield is higher!

BAL • is the method of choice • by showing free red blood cells and hemosiderin-laden, iron-positive macrophages

BAL WITH IRON +AM GOLNIK 2004 -2009 (64+/84 staining samples) • vasculitis or capillaritis 29% • pulmonary haemorrhage without capillaritis or vasculitis (» bland « pulmonary haemorrhage) 18% • alveolar bleeding associated with another process or condition 39%. . . . . • pneumoconiosis 14%

BAL WITH IRON +AM GOLNIK 2004 -2009 vasculitis or capillaritis: pulmonary haemorrhage without capillaritis or vasculitis: • 58% sistemic vasculitis • 42% connective tissue • 66% drugs disorders • 17% infective endocarditis

BAL WITH IRON +AM GOLNIK 2004 -2009 alveolar bleeding associated with another process or condition: • 48% infections • 32% sarcoidosis • 20% malignant conditions

TREATMENT OF DAH • combination of treatment autoimmune destruction of the alveolare capillary membrane and the underlaying condition • immunosupresive agents are the mainstay of therapy, especially if DAH is associated with systemic or pulmonary vasculitis, Goodpasture syndrome or conective tissue disorders • treatment of small vessel vasculitis of the lung is largely the same, regardless of aetiology or whether it is isolated to the lung or a component of a systemic disease

TREATMENT OF DAH Immunosupresive agents • Methylprednisolone and • Cyclophosphamide are the mainstay of therapy. • Plasmapheresis - clinical benefit in Goodpasture syndrome • Recombinant activated human factor VIIsuccessful in several case reports of treating alveolar hemorrhage due to allogenic hematopoietic stem cell transplantation, ANCA associated vascullitis, SLE or antiphospholipid syndrome.

TREATMENT OF DAH-other possible management measures: • supplemental oxygen, • bronchodilators, • reversal of any coagulopathy, • intubation with bronchial tamponade, • protective strategies for the less involved lung, • mechanical ventilation should be done in the course of the disease if they are needed.

CONCLUSION • DAH can be a catastrophic illness if recognition and treatment are delayed. • Diagnosis is often aided by other systemic findings, associated illnes and serological results. • Patients with unexplained isolated DAH should undergo a lung biopsy with immunofluorescent studies and routine histological tests. • During therapy close monitoring, due to potential complications of treatment and the possibility to relapses, is needed.