Differentiation between cancer and inflammation in lung cancer

Differentiation between cancer and inflammation in lung cancer imaging Chumy Nwogu, MD, Ph. D, FACS Associate Professor of Oncology & Surgery Roswell Park Cancer Institute University at Buffalo MEDAMI September 7 th, 2014

Outline n Background n Clinical Applications of Molecular Imaging in Lung Cancer n Evolution of Radioguided Lung Cancer Imaging n Limitations n Future Prospects

Background n Lung Ca – most frequent cause of cancer death worldwide n 15% SCLC ; 85% NSCLC n LN metastasis – most important prognostic factor in locoregional NSCLC n Current staging methods are suboptimal n 40% of Stage I (node negative) patients will recur within 2 years n Understaging – unrecognized micrometastases
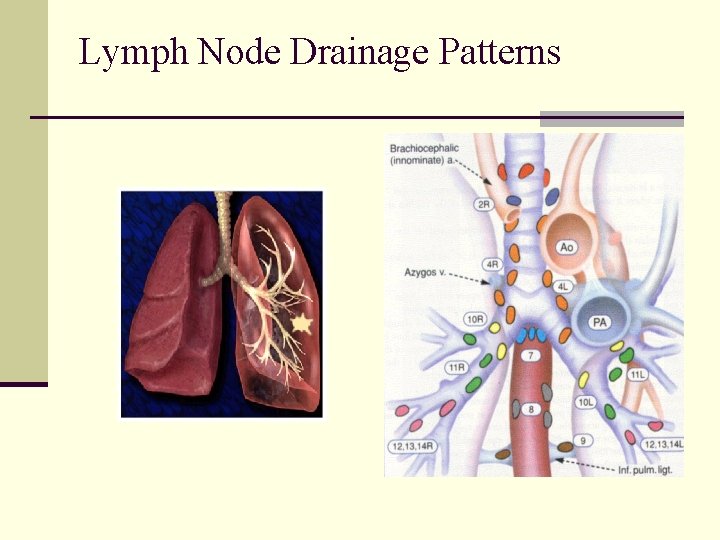
Lymph Node Drainage Patterns

Background n PET-CT is currently the imaging modality of choice for NSCLC clinical staging n All resected LNs undergo bisection and H&E staining n Conventional pathologic techniques can miss micrometastases n Defined as 0. 2 -2. 0 mm sized tumor deposits in LNs n IHC and RT-PCR (ultra-staging) are much more sensitive but labor intensive & expensive n Need for a tool to select most suspicious LNs for ultra-staging
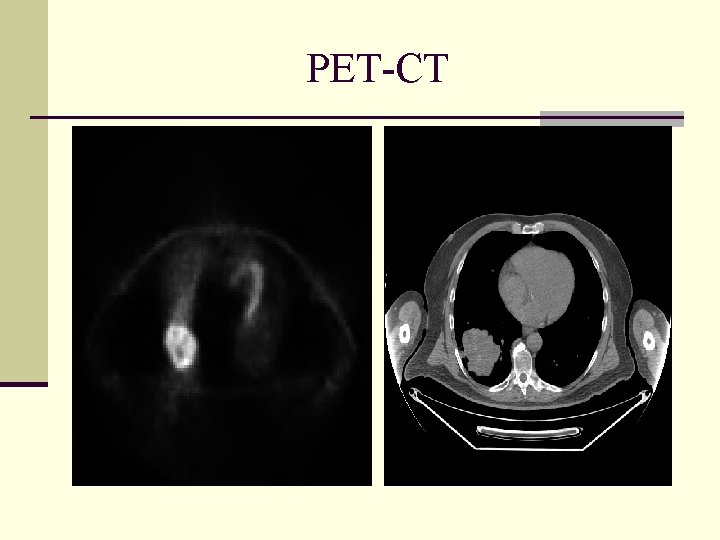
PET-CT

Background n Incidence of micromets is about 19 - 26% n Can be detected by multiple step sections, IHC, RT-PCR n Skip metastases also occur n There is great value in assessing ALL the regional lymph nodes in patients n Higher # of lymph nodes examined and lower lymph node ratio are both associated with better disease specific and overall survival Kim AW. Sem in Thorac & Cardiovasc Surg 2009; 21(4): 298 -308 Nwogu C, et al. Number of Lymph Nodes and Metastatic Lymph Node Ratio are Associated with Survival in Lung Cancer. Ann Thor Surg 2012; 93(5): 1614 -1619

Clinical Applications of Molecular Imaging in Lung Cancer n Risk stratification of CT screening detected lung nodules n Sentinel lymph node mapping n Identification of all malignant thoracic lymphadenopathy n Localization of small lung nodules n Cytotoxic therapy for lymph node metastases

Sentinel Lymph Node Mapping n Sentinel LNs – 1 st echelon of LNs draining a tumor n Initial reported technique: Isosulfan blue n SLN identified in 17 of 36 pts (47%) n The other pts showed diffuse staining of the lung n Difficulty differentiating blue nodes from anthracotic nodes n 5 cases of unexpected N 2 were identified Little A. G. , et al. J Thorac Cardiovasc Surg 1999; 117: 220 -224

Use of Tc-99 m n Successful migration on Tc-99 m in 120 of 148 pts (81%) n Lack of Tc-99 m migration in 19% n SLN identified in 104 of 120 pts (87%) n 104 of all 148 pts (70%) n n SLN harbored cancer in 32% of pts n Upstaging occurred in 8 of 104 pts (5. 5%) Liptay MJ, et al. Ann Thorac Surg 2000; 70: 384 -389

RPCI Preclinical Study n Pulmonary Lymphatic Mapping in Dogs n Technetium 99 m sulfur colloid & Isosulfan blue dye n Isosulfan blue dye detected SLN in 50% within 5 minutes n Tc 99 m detected SLN in 83% within 20 minutes n Tc 99 m technically easier to use Nwogu CE, Kanter PM, Anderson TM Cancer Invest 2002; 20(7 -8): 944 -947

Multicenter Phase II CALGB Study n 46 pts accrued in 2 yrs (150 planned) n SLN detected in 24 of 39 pts (61. 5%) n SLN accurate in 20 of 24 pts (83. 3%) n Overall accuracy of 51. 2% (20 of 39 pts) n Closed early due to poor accrual, low accuracy and loss of funding. Liptay MJ, D’Amico TA, Nwogu CE, et al. J Thorac Oncol 2009; 4: 198 -202

Multicenter Phase II CALGB Study n Collaboration challenges b/w some nuclear medicine, surgery & pathology depts n State radiation safety obstacles n Some surgeons possibly still in their learning curve: 8 surgeons performed an average of 5 cases (1 -13)

Limited adoption of SLN mapping in NSCLC n Perceived difficulty of technique n Surgical delay after intra-op isotope injection n Extra procedure for injection of Tc 99 m-tin colloid pre-op n Controversial clinical benefit n Low morbidity of thoracic lymphadenectomy Nwogu CE. Sem in Thorac & Cardiovasc Surg 2009; 21(4): 323 -326

Pilot Gamma Probe Study n Radioguided Detection of NSCLC lymph node mets Assessment of all lymph nodes (not just the sentinel LNs) n Use of 18 F-FDG instead of Tc or blue dye n Nwogu C, Fischer G, Tan D, et al. Ann Thorac Surg 2006; 82: 1815 -1820

Objectives n Measure the feasibility of a hand-held gamma probe to detect FDG in malignant tissue Primary tumor n Lymph nodes n n Explore the ability of this technique to improve lymph node staging in NSCLC

Gamma Probe

Methods n 10 pts enrolled – all had pre-op PET scans n Pts had tumors >3 cm or enlarged thoracic LNs on CT n 10 -15 m. Ci FDG injected on the day of surgery n Handheld probe used intraop to assess Primary tumor n Regional lymph nodes n Lung resection with lymphadenectomy n Pathologic assessment n H&E n Serial sections & IHC of probe +, H&E - LNs n

Results n The intra-op handheld gamma probe detected All PET positive lesions n 2 cases with FDG avid LNs not seen on PET scan n n Only the ex-vivo counts were useful n 9/55 (16%) of all lymph nodes ultrastaged n 4 of 10 cases with micrometastases n 3 cases (30%) were upstaged n 37% false positive rate

Conclusions from Pilot Study n Detection of occult LN metastases with an FDG-sensitive intra-op gamma probe is feasible n This can improve NSCLC staging n Larger study required to determine the accuracy and predictive value of this technique

Follow-up Gamma Probe Trial n 100 patient trial n Stage I and II NSCLC patients n Specific Aim 1: Assess the utility of an intra-operative gamma probe in detecting FDG avid LNs n Specific Aim 2: Assess the clinical relevance of the gamma probe detected lymph node metastases Supported by an NCI K-23 grant (K 23 CA 122182)

Results n Median additional operative time for LN mapping was 5 minutes (Range 0 -20) n Detection of FDG avid (hot) lymph nodes PET-CT: 6 patients n Gamma Probe: 86 patients n n Median # of LNs harvested/patient – 10 (Range 1 -21)
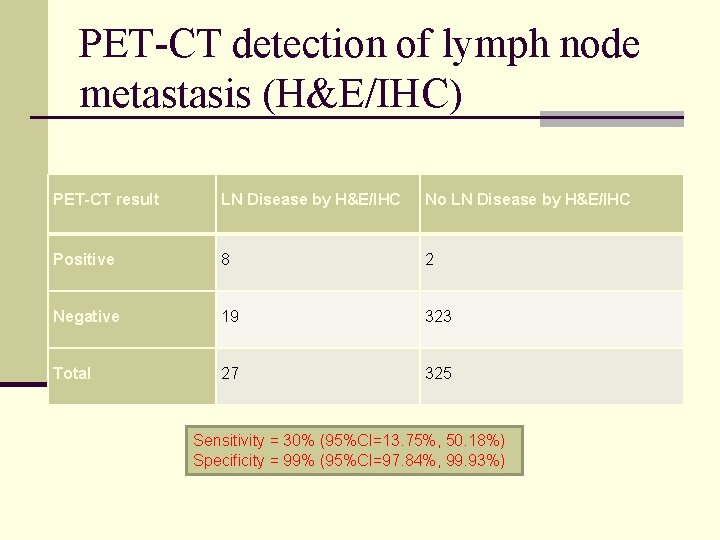

PET-CT detection of lymph node metastasis (H&E/IHC) PET-CT result LN Disease by H&E/IHC No LN Disease by H&E/IHC Positive 8 2 Negative 19 323 Total 27 325 Sensitivity = 30% (95%CI=13. 75%, 50. 18%) Specificity = 99% (95%CI=97. 84%, 99. 93%)
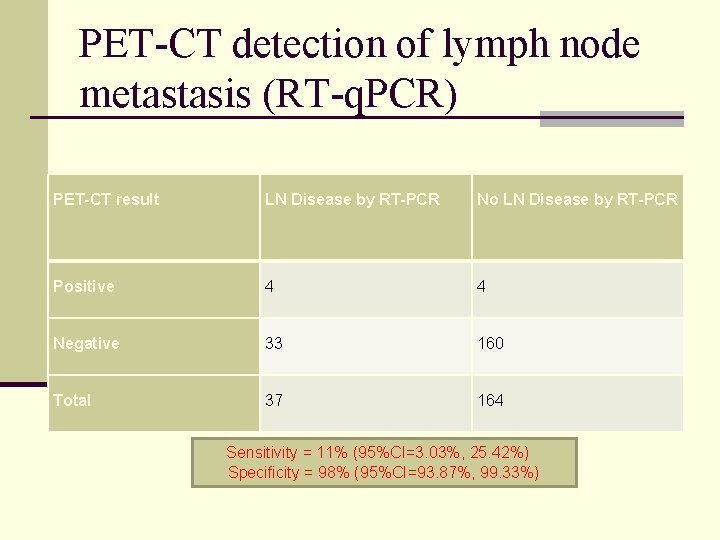
PET-CT detection of lymph node metastasis (RT-q. PCR) PET-CT result LN Disease by RT-PCR No LN Disease by RT-PCR Positive 4 4 Negative 33 160 Total 37 164 Sensitivity = 11% (95%CI=3. 03%, 25. 42%) Specificity = 98% (95%CI=93. 87%, 99. 33%)

Gamma probe detection of lymph node metastasis (H&E/IHC) Gamma probe result LN Disease by H&E/IHC No LN Disease by H&E/IHC Positive (Hot) 20 155 Negative (Cold) 7 170 Total 27 325 Sensitivity = 74% (95%CI=53. 72%, 88. 89%) Specificity = 52% (95%CI=46. 59%, 57. 59%)

Gamma probe detection of lymph node metastasis (RT-PCR) Gamma probe result LN Disease by RT-PCR No LN Disease by RT-PCR Positive 14 82 Negative 23 82 Total 37 164 Sensitivity = 38% (95%CI=22. 46%, 55. 24%) Specificity = 50% (95%CI=42. 10%, 57. 90%)
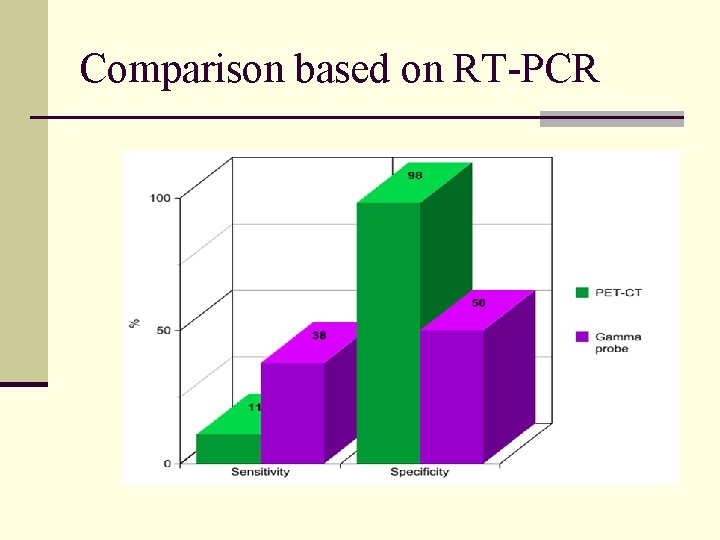
Comparison based on RT-PCR
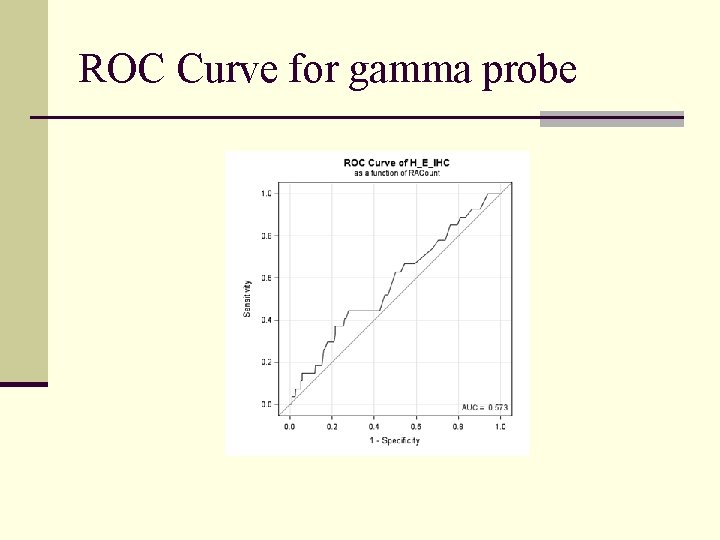
ROC Curve for gamma probe

Results n 18 patients had malignant LNs by H&E n IHC detected additional metastatic LNs in 4% of patients n RT-PCR detected additional metastatic LNs in 47% of patients n Median patient follow-up is 24 months n Worse disease free survival in patients with positive LNs by H&E/IHC but not by RT-PCR

Discussion n 90% of patients were in clinical stage I with relatively small tumors n Lower probability of occult LN mets compared to pilot study or the literature n Upstaging of 4% of pts by IHC and 47% by RT-PCR n Need for adjuvant chemotherapy trial on patients with occult LN metastases

Discussion n The gamma probe was more sensitive but less specific than PET-CT in predicting malignant LN disease n The poor specificity of the gamma probe limits clinical utility n Inability to differentiate between malignancy and inflammation n Strong need for better radioisotopes (other than FDG)

Thoracic Radioguided Node Mapping Challenges n High background radioactivity n Aerosolization of Tc-99 m n Cardiac FDG uptake n Primary tumor ‘shine-through’ effect n Intrapulmonary lymph nodes n Need for minimally invasive probes n Mediastinoscopy n Thoracoscopy n Robotic surgery

Non-radioactive Tracers n Peritumoral injection of various non- radioactive tracers for SLN mapping have been investigated Ferumoxides (magnetite) detected with a sterilizable magnetometer n Near-Infrared Fluorescent Quantum Dots or Indocyanine Green (ICG) n Oncolytic herpes virus with a green fluorescent protein (GFP) transgene n

Near Infrared Fluorescence Imaging n NIR light is invisible n Wavelength 700 -1000 nm n Special imaging system required n Contrast Agents n Indocyanine Green (ICG) n Quantum Dots (QDs) – fluorescent semiconductor nanocrystals
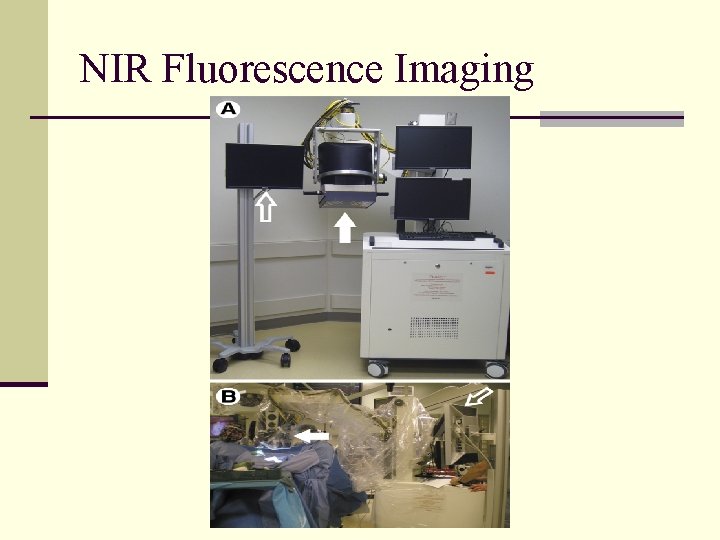
NIR Fluorescence Imaging

NIR Fluorescence Imaging Soltez EG, et al. Ann Thorac Surg 2005; 79: 269 -277

18 F-FDG Versus 18 F-fluoro-Ltyrosine PET n Protein synthesis and amino acid transport are enhanced in most tumor cells but affected less in inflammatory conditions n 22 patients: 11 NSCLC, 10 lymphomas, 2 head & neck carcinomas n 18 F-TYR PET only visualized 67% of the lesions identified by 18 F-FDG PET n Tumor SUV 5. 2 vs. 2. 5; tumor: muscle ratio 7. 4 vs. 2. 7; tumor: mediastinum activity ratio 3 vs. 1. 4 - all favored 18 F-FDG PET n Conclusion: 18 F-TYR PET not superior to 18 F-FDG PET Hustin R. , et al. J Nucl Med 2003; 44(4): 533 -9
![18 F-FLT PET n 3’-deoxy-3’-[18 F]fluorothymidine PET n Most promising nucleoside metabolic tracer n 18 F-FLT PET n 3’-deoxy-3’-[18 F]fluorothymidine PET n Most promising nucleoside metabolic tracer n](http://slidetodoc.com/presentation_image/4baccb242cfadea734b78094abd9d624/image-38.jpg)
18 F-FLT PET n 3’-deoxy-3’-[18 F]fluorothymidine PET n Most promising nucleoside metabolic tracer n 28 women with suspicious breast findings on conventional imaging (mammography & ultrasonography) n Whole body and regional breast PET performed n Same Sensitivity (92. 3%) but better specificity (66. 7% vs. 52. 4%) with the regional PET Wang J. , et al Ann Nucl Med 2014 Aug 20 [Epub ahead of print]

18 F-FLT PET/CT imaging in inflammation n Wister rabbit inflammation model n 8 rabbits with tibial Staph aureus abscesses n 8 rabbits with tibial sterile granulomas n After 4 weeks, 18 F-FLT PET/CT - SUVMAX 5. 76± 0. 25 vs. 1. 15± 0. 32 (P<0. 01) n Conclusion: 18 F-FLT is not a tumor specific tracer Tan Y. , et al Exp Ther Med 2014; 8(1): 69 -72
Therapeutic SLN Imaging n Targeted SLN Imaging n Liposomes n Dendrimers n Quantum Dots n Chemical & biologic cytotoxic agents n Attenuated viruses n Genetically modified bacteria

Future Prospects n Reliable, reproducible lymph node mapping techniques n Sensitive, affordable path methods for micrometastasis detection n Elimination of interference from the heart, major blood vessels or central airway n More specific PET radioisotopes in preclinical studies n Heptamethine cyanine based 64 Cu-PET Probe PC 1001 n 124 I

Future Prospects n Easy detection of peri-tumoral LN radioactivity n Integration with other molecular lung cancer staging techniques n Coupling therapeutic with diagnostic agents n 124 I used for both PET imaging & Photodynamic therapy (PDT) n Improvement in NSCLC staging, therapy and outcomes

Collaborators n n n Todd Demmy, MD Sai Yendamuri, MD Mary Reid, Ph. D Alex Adjei, MD, Ph. D Alan Hutson, Ph. D n n n Ravi Pandey, Ph. D Gal Shafirstein, Ph. D Richard Cheney, MD Dominic Lamonica, MD Paul Bogner, MD Elizabeth Repasky, Ph. D

Thanks Questions?
- Slides: 44