DIFFERENTIAL DIAGNOSIS AND TREATMENT OF LOW BACK AND

DIFFERENTIAL DIAGNOSIS AND TREATMENT OF LOW BACK AND LOWER EXTREMITY PAIN Prof. Dr. Ece Aydoğ PMR

Learning objectives • 1. be able to differentiate mechanical and non- • • mechanical pain 2. be able to enumerate the risk factors for low back pain 3. be able to define spondylosis, spondylolysis, spondylolisthesis and spondylitis 4. be able to describe clinical presentation and treatment for acute muscular strain, lumbar discopathy, spinal stenosis and spondylolisthesis and spondylolysis. 5. be able to enumerate non-mechanic causes of low back pain and describe differential diagnosis.

Learning objectives • 6. be able to enumerate the red flags of serious low back pain • 7. be able to enumerate the reasons which cause pain in the lower extremity and make the differential diagnosis. • 8. be able to enumerate situations that require emergency surgery for lumbar back pain and surgical indications in lumbar discopathy. • 9. be able to enumerate diagnostic methods, treatment approaches, pharmacological and non pharmacological methods for low back pain.

Who gets back pain ? • Almost Everybody – Estimates run as high as 80% of the population. – Only 1 -2 % need surgery. – 5 -10 % develop chronic pain. – 75 % of patients have relapses. – Peak occurrence is between age 30 and 45.
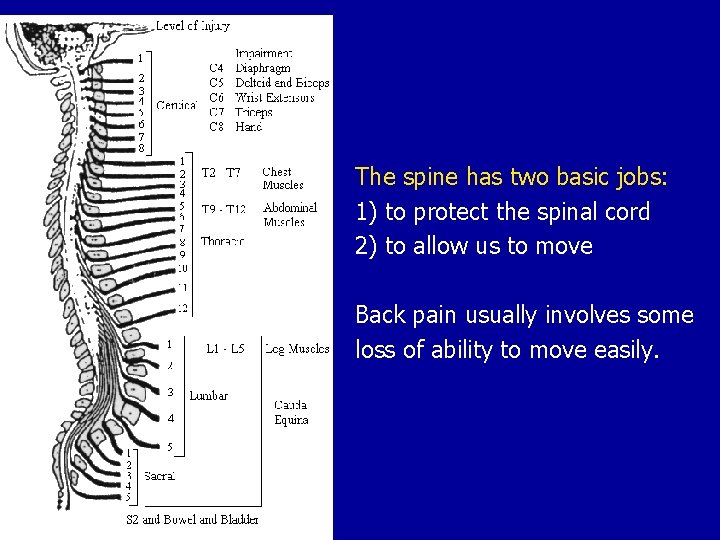
The spine has two basic jobs: 1) to protect the spinal cord 2) to allow us to move Back pain usually involves some loss of ability to move easily.
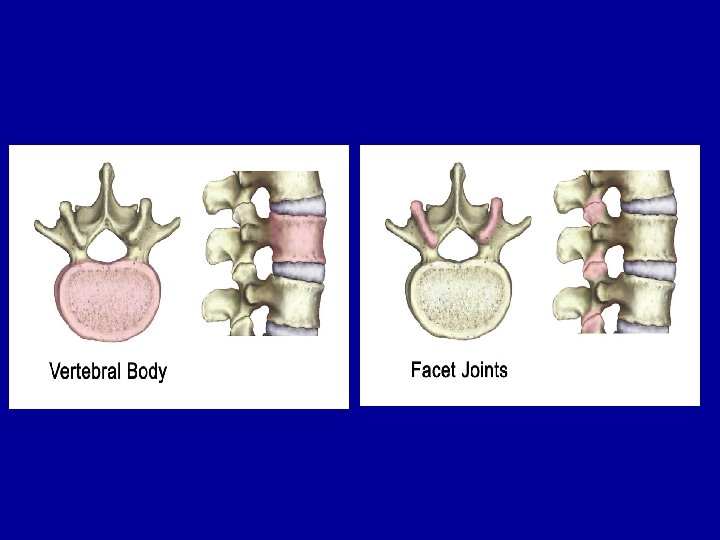
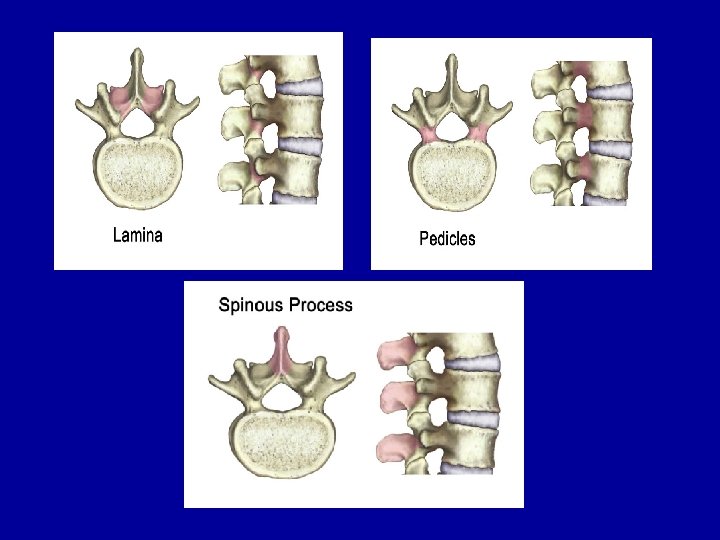
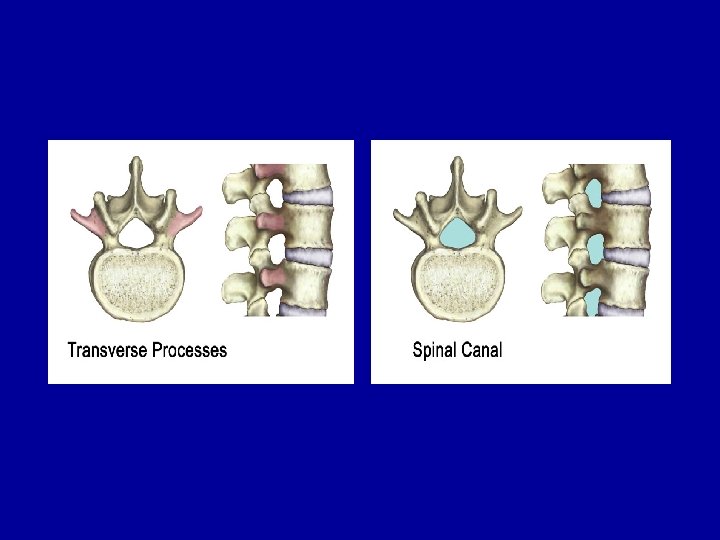
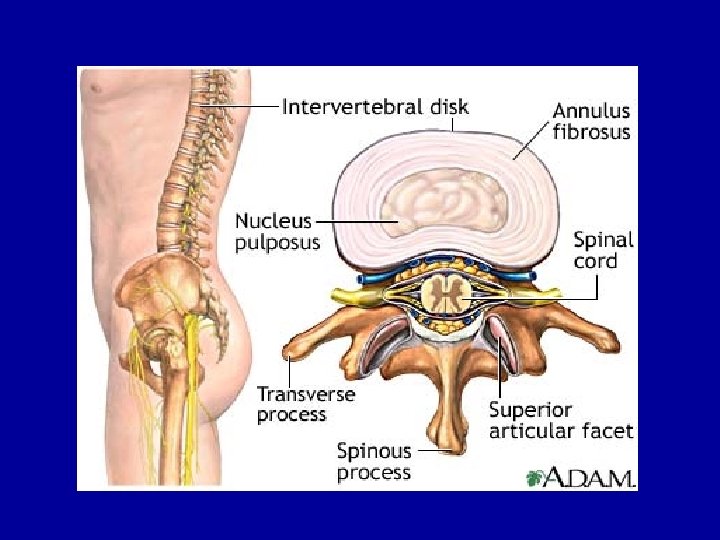
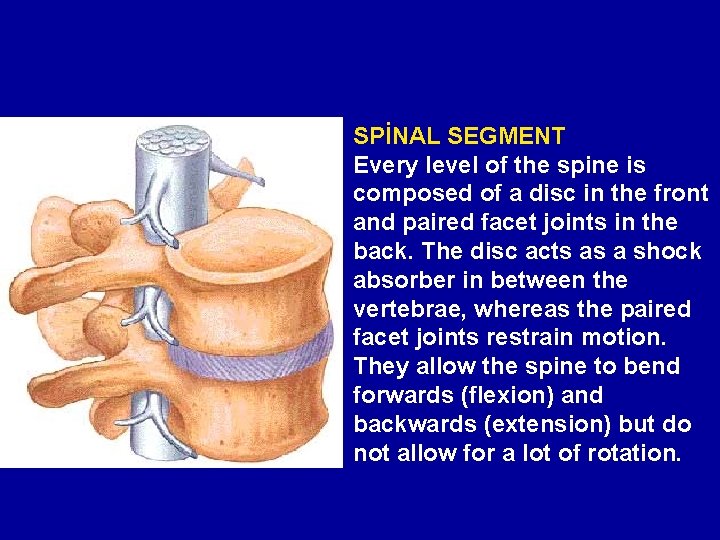
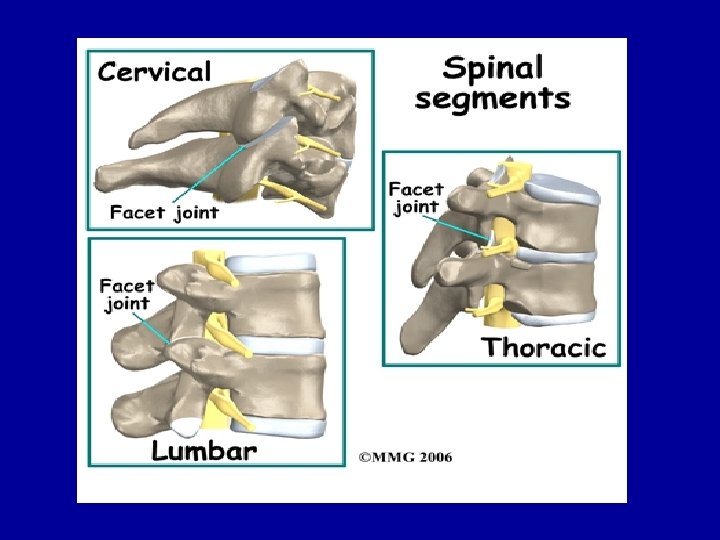
SPİNAL SEGMENT Every level of the spine is composed of a disc in the front and paired facet joints in the back. The disc acts as a shock absorber in between the vertebrae, whereas the paired facet joints restrain motion. They allow the spine to bend forwards (flexion) and backwards (extension) but do not allow for a lot of rotation.

Classifications • Transient—duration is hours to days, only brought to medical attention when episodic • Acute—duration is days to weeks; most recover spontaneously • Persistent—lasts more than 3 -6 months; does not improve with time; no psychological co-morbidities (often associated with spondylotic disease) • Chronic—lasts more than 6 months; worsens with time, associated with major psychological comorbidities

• 90% of low back pain is “mechanical” • Injury to muscles, ligaments, bones, disks Spontaneous resolution is the rule • Nonmechanical causes uncommon but don’t • • • miss them! Spondyloarthropathy Spinal infection Osteoporosis Cancer Referred visceral pain

Risk Factors • • Age Sendentary lifestyle Pregnancy Obesity Smoking Injury Preexisting back injury due to: – Lifting a heavy object – Improper lifting – Sudden movement, bending, or twisting – Prolonged sitting or standing – Bad posture – Vibration from vehicles or heavy equipment • Prior back surgery • Other factors which may negatively influence back pain include: – Psychological factors, such as low job satisfaction – Fatigue or sleep deficit – Drug or alcohol abuse – Stress

Congenital bone conditions Congenital causes (existing from birth) of low back pain include scoliosis and spina bifida. Scoliosis is a sideways (lateral) curvature of the spine that can be caused when one lower extremity is shorter than the other (functional scoliosis) or because of an abnormal design of the spine (structural scoliosis). Children who are significantly affected by structural scoliosis may require treatment with bracing and/or surgery to the spine. Adults infrequently are treated surgically but often benefit by support bracing.
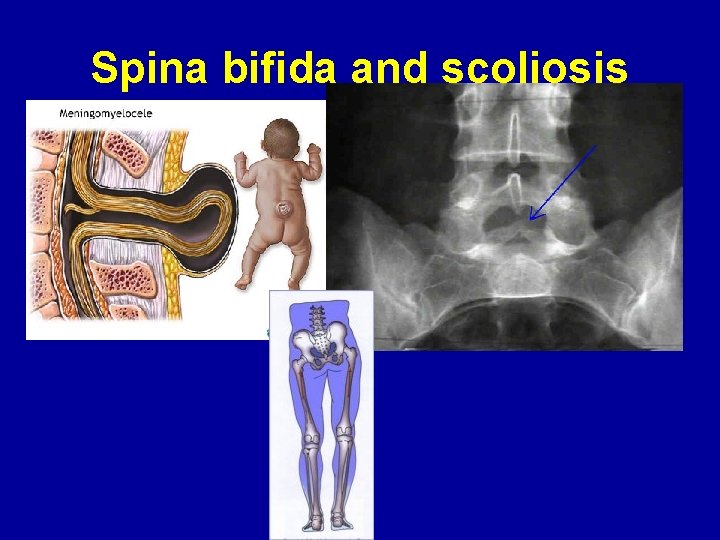
Spina bifida and scoliosis
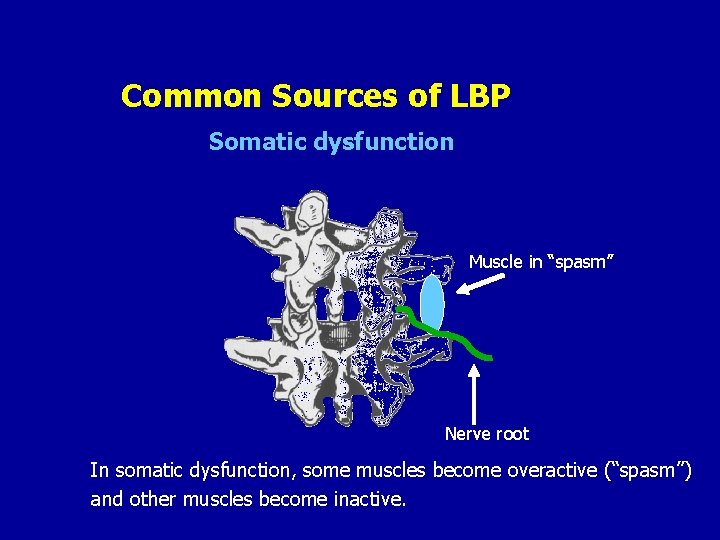
Common Sources of LBP Somatic dysfunction Muscle in “spasm” Nerve root In somatic dysfunction, some muscles become overactive (“spasm”) and other muscles become inactive.
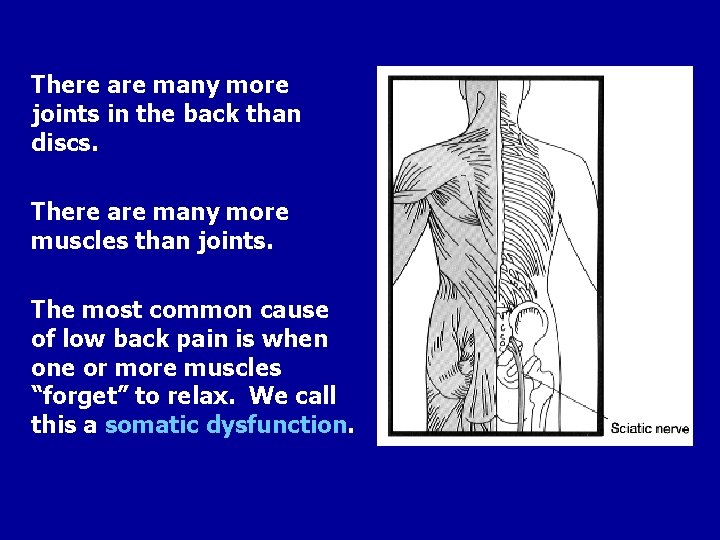
There are many more joints in the back than discs. There are many more muscles than joints. The most common cause of low back pain is when one or more muscles “forget” to relax. We call this a somatic dysfunction.
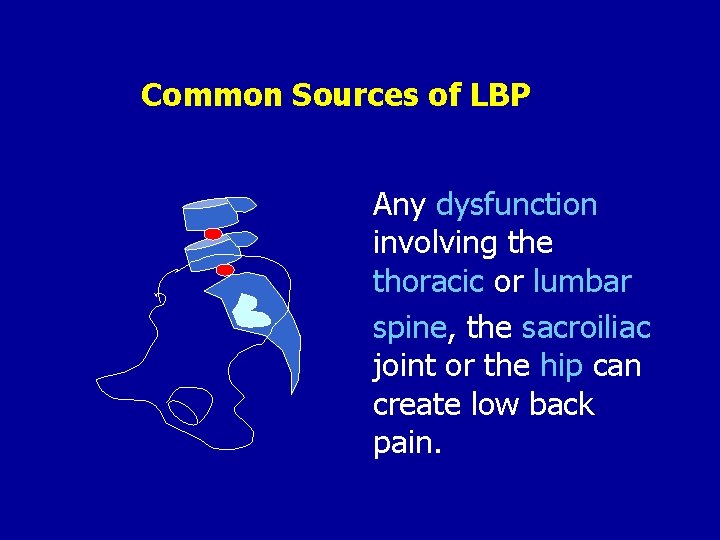
Common Sources of LBP Any dysfunction involving the thoracic or lumbar spine, the sacroiliac joint or the hip can create low back pain.
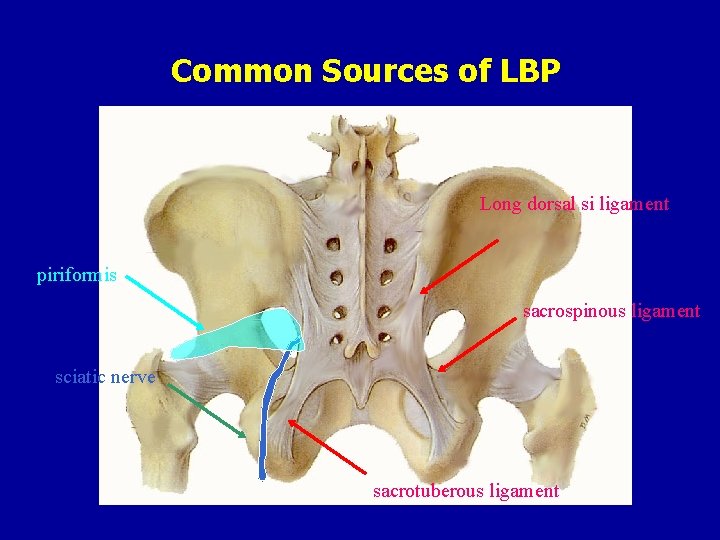
Common Sources of LBP Long dorsal si ligament piriformis sacrospinous ligament sciatic nerve sacrotuberous ligament
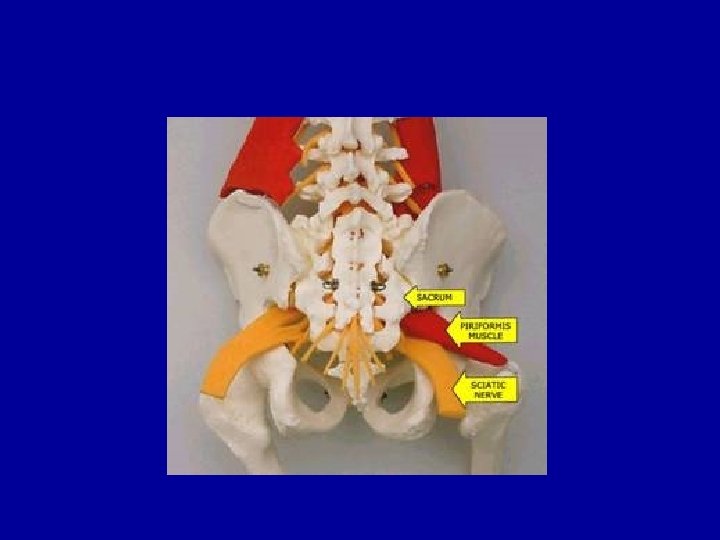
Role of the sacroiliac joint 1 3 2 The sacroiliac joint requires muscle activity to keep it stable. If muscles can’t work correctly, perhaps because of a somatic dysfunction, the joint becomes unstable and painful.

The most common causes of low back pain; • Injury or overuse of muscles, ligaments, facet joints, and the sacroiliac joints.

Lumbar Strain • stretching injury to the ligaments, tendons, and/or muscles of the low back • microscopic tears of varying degrees in these tissues • one of the most common causes of low back pain • occur because of overuse, improper use, or trauma • "acute" if it has been present for days to weeks • "chronic" lasts longer than three months

Symptoms • Pain, mostly in the back and buttocks. • Muscle spasms, cramping, and stiffness. • It is aggravated by weight-bearing or specific movements and is relieved by rest. • The most severe pain usually lasts 48 to 72 hours and may be followed by days or weeks of less severe pain. • The back is easily reinjured during this time.

Spondylolysis • Spondylolysis (spondylo = spine; lysis=dissolved) refers to the defect (black arrows) present when the pars interarticularis is fractured. This results is the lamina and inferior facet joints being disconnected from the vertebral body.

Spondylolysis • Spondylolysis isn't something that people are born with, but develop in childhood /adolescence. • It is thought to be a stress fracture that doesn't heal. • It is seen most often in football linemen and in gymnasts

Spondylolisthesis • Spondylolisthesis (spondylo=spine; listhesis=to slip) occurs in the presence of a spondylolysis when the intervertebral disc stretches and allows the vertebral body to slide forward on the vertebra below. This results in widening of the pars defect. This is known as an isthmic spondylolisthesis.

Spondylolisthesis • Displastic (congenital dysplasia between the L 5 -S 1) • Degenerative (elderly people) • Traumatic (fracture in the posterior stractures except isthmus) • Patologic (metabolic bone disease, metastatic Ca. . )
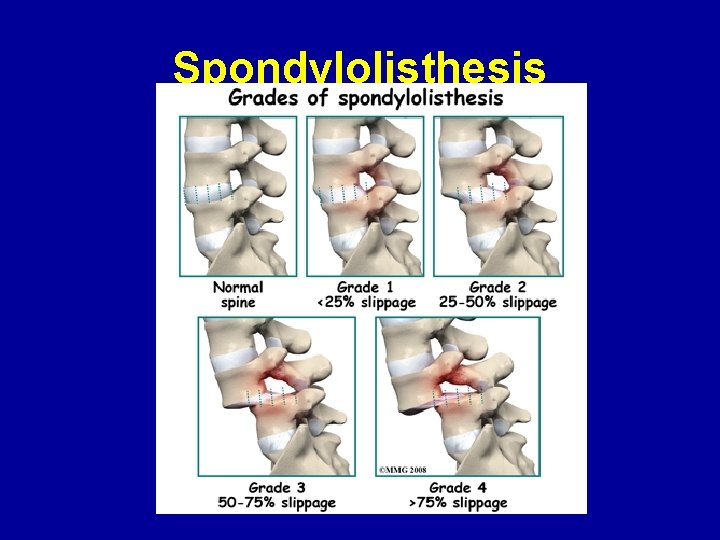
Spondylolisthesis

Spinal Stenosis • Spinal stenosis is a medical condition in which the spinal canal narrows and compresses the spinal cord and nerves. • This is usually due to the common occurrence of spinal degeneration that occurs with aging. • It can also sometimes be caused by spinal disc herniation, osteoporosis or a tumor. • In the cervical and lumbar region it can be a congenital condition to varying degrees.

Spinal Stenosis • Spinal-nerve compression in these conditions can lead to sciatica pain that radiates down the lower extremities. • Spinal stenosis can cause lowerextremity pains that worsen with walking and are relieved by resting (mimicking poor circulation) (Neurogenic claudication)
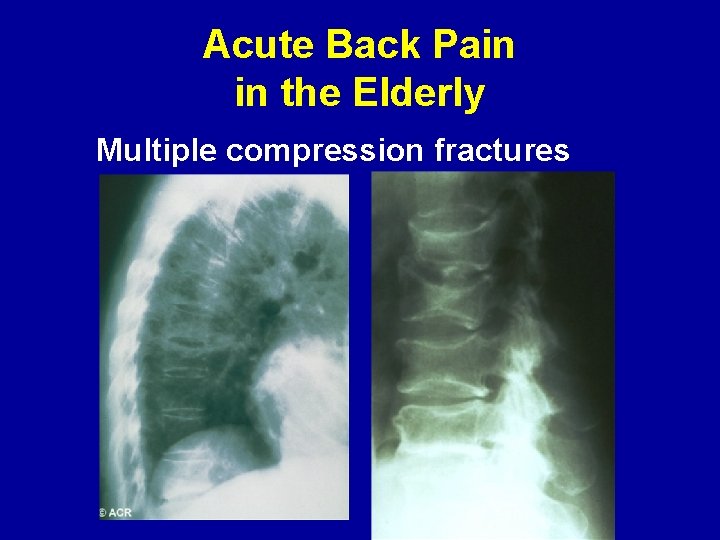
Acute Back Pain in the Elderly Multiple compression fractures

Compression fractures • More common among postmenopausal women with osteoporosis, or in men or women after long-term corticosteroid use. • No early warning, often occurs with forward flexion during normal activity or with trivial trauma • Severe spinal pain • Marked muscle spasm • Some relief with recumbency
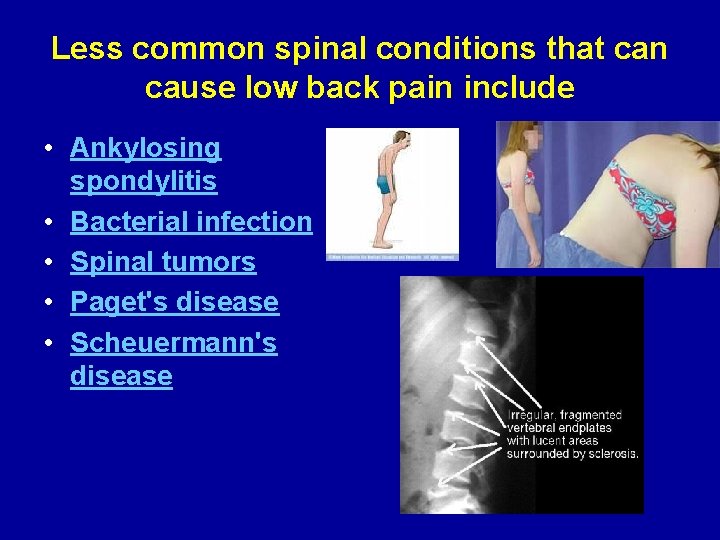
Less common spinal conditions that can cause low back pain include • Ankylosing spondylitis • Bacterial infection • Spinal tumors • Paget's disease • Scheuermann's disease

Spinal Infections • Acute infection • • Bacterial Fungal • Sites of spinal infection • • Chronic infection • • Bacterial Fungal Tuberculosis Brucellosis • • Vertebral osteomyelitis Disk space infection Septic sacroiliitis
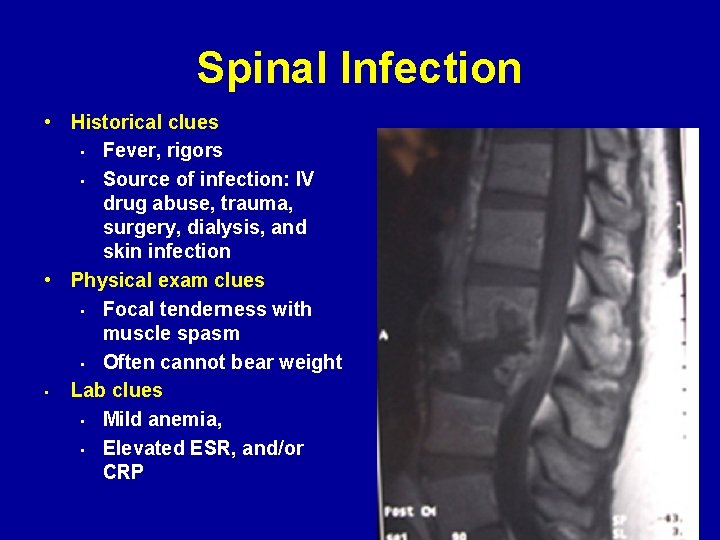
Spinal Infection • Historical clues • Fever, rigors • Source of infection: IV drug abuse, trauma, surgery, dialysis, and skin infection • Physical exam clues • Focal tenderness with muscle spasm • Often cannot bear weight • Lab clues • Mild anemia, • Elevated ESR, and/or CRP
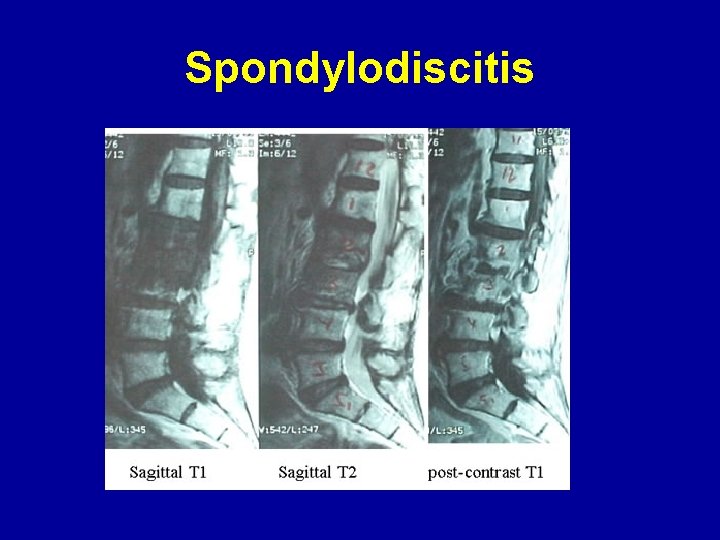
Spondylodiscitis
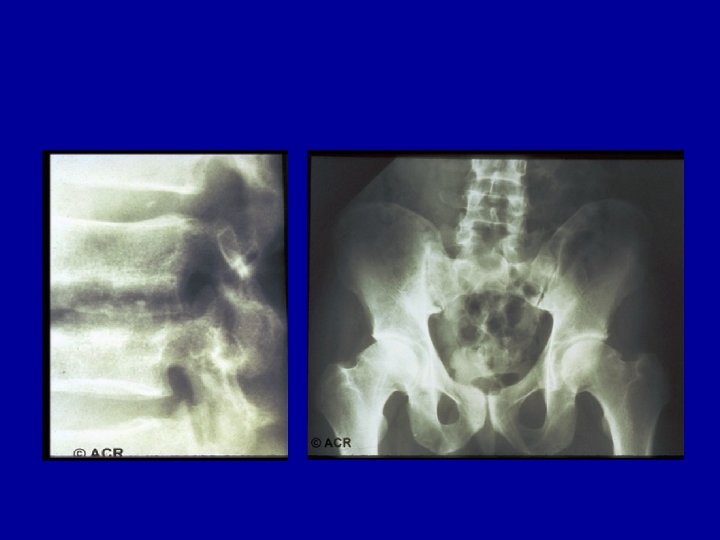
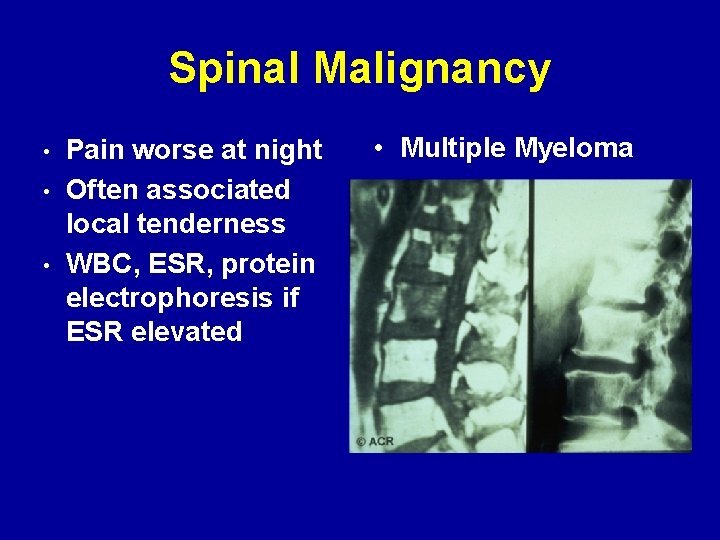
Spinal Malignancy • • • Pain worse at night Often associated local tenderness WBC, ESR, protein electrophoresis if ESR elevated • Multiple Myeloma
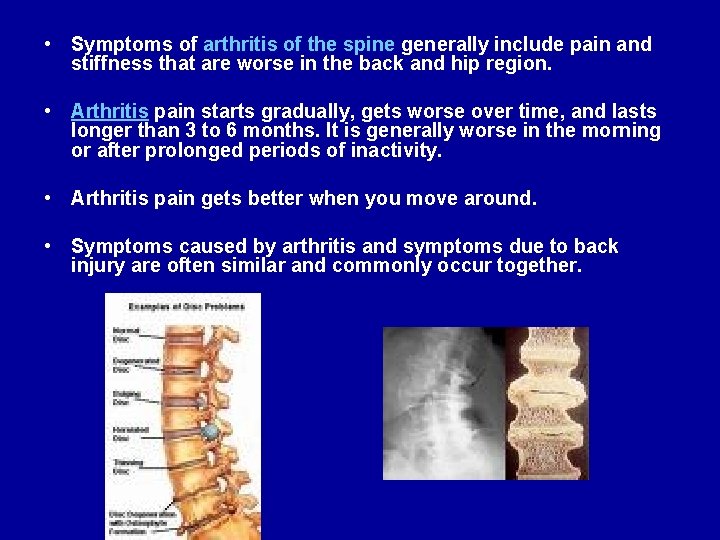
• Symptoms of arthritis of the spine generally include pain and stiffness that are worse in the back and hip region. • Arthritis pain starts gradually, gets worse over time, and lasts longer than 3 to 6 months. It is generally worse in the morning or after prolonged periods of inactivity. • Arthritis pain gets better when you move around. • Symptoms caused by arthritis and symptoms due to back injury are often similar and commonly occur together.

Other medical conditions that can cause pain that may be similar to low back pain include: • Pelvic inflammatory disease • Aortic aneurysm • Peptic ulcers • Gallbladder disease • Pancreatitis • Urinary disorders such as kidney stones or urinary tract infections. • Prostate disease

What Are the Red Flags for Serious Low Back Pain? • Fever, weight loss • Intractable pain—no improvement in 4 to 6 weeks • Nocturnal pain or increasing pain severity • Morning back stiffness with pain onset before age 40 • Neurologic deficits

Lower extremity pain Causes • MUSCLE CRAMP 1. Dehydration or low amounts of potassium, sodium, calcium, or magnesium in the blood. 2. Medications 1. Diuretics, 2. Statins, which lower cholesterol and can cause muscle injury 3. Muscle fatigue or strain from overuse, too much exercise, or holding a muscle in the same position for a long time
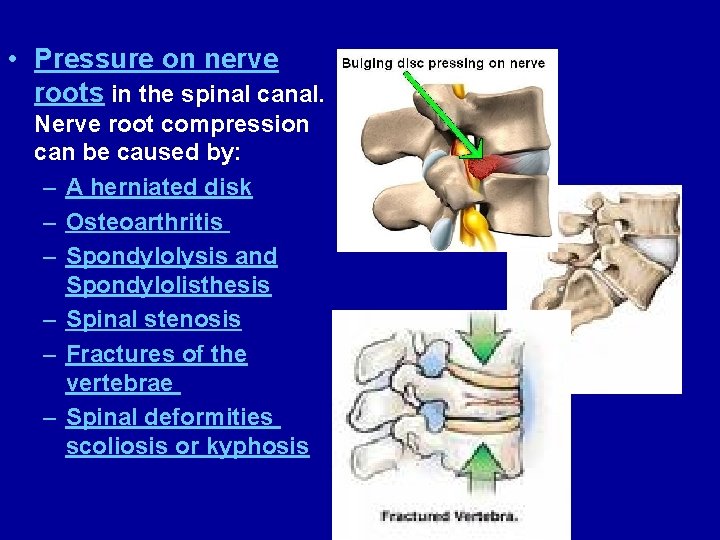
• Pressure on nerve roots in the spinal canal. Nerve root compression can be caused by: – A herniated disk – Osteoarthritis – Spondylolysis and Spondylolisthesis – Spinal stenosis – Fractures of the vertebrae – Spinal deformities scoliosis or kyphosis
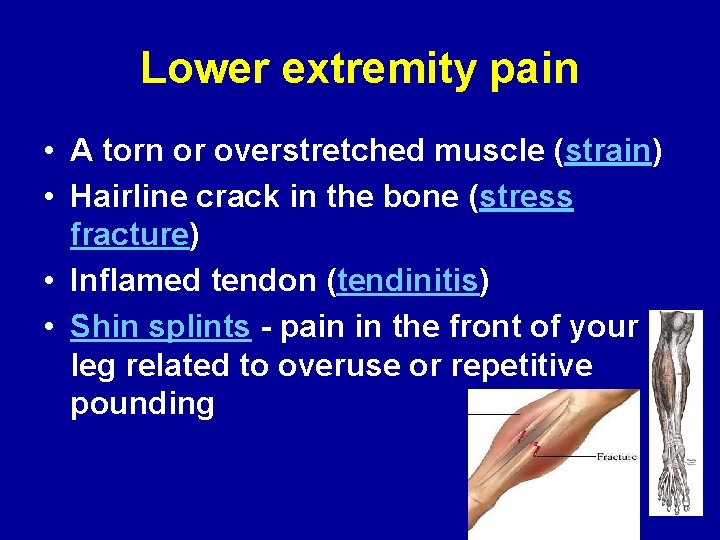
Lower extremity pain • A torn or overstretched muscle (strain) • Hairline crack in the bone (stress fracture) • Inflamed tendon (tendinitis) • Shin splints - pain in the front of your leg related to overuse or repetitive pounding

Other common causes of leg pain • Atherosclerosis that blocks blood flow in the arteries (this type of pain, called claudication, is generally felt when exercising or walking and relieved by rest) • Blood clot (deep vein thrombosis) from prolonged bed rest • Infection of the bone (osteomyelitis) or skin and soft tissue (cellulitis) • Inflammation of the leg joints by arthritis or gout • Nerve damage - common in diabetics, smokers, and alcoholics (symptoms include numbness, tingling, or a sensation of pins-and-needles) • Varicose veins

Less common causes • Benign tumors or cysts of the femur or tibia (osteoid osteoma) • Legg-Calve-Perthes disease - poor blood flow to the hip that may stop or slow the normal growth of the leg • Malignant bone tumors (Osteosarcoma, Ewing sarcoma) • Sciatic nerve pain (radiating pain down the leg) caused by a slipped disk in the back. • Slipped capital femoral epiphysis - usually seen in boys and overweight children between 11 and 15 years old

Differential diagnosis • Arteriogram to check blood flow • Blood tests for specific diseases • Bone biopsy if tumor is seen on MRI which may be malignant • Bone scan • Duplex Doppler/ultrasound exam to look for a blood clot • MRI if a malignant tumor is suspected • X-ray of your back or legs
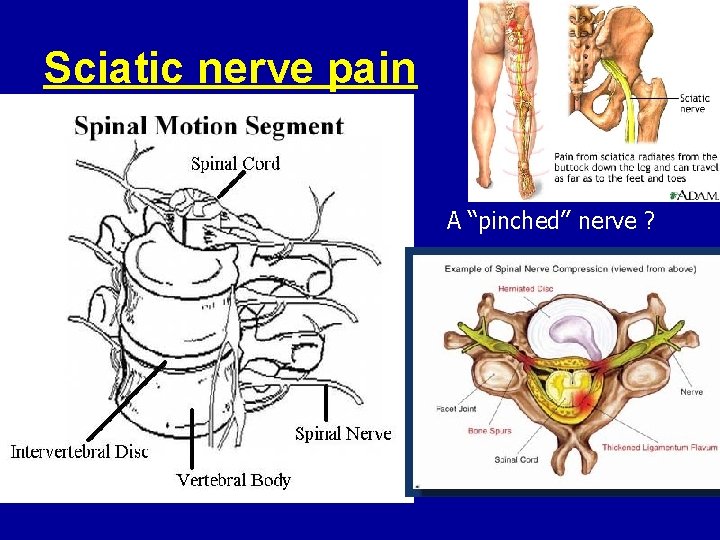
Sciatic nerve pain A “pinched” nerve ?
Symptoms of nerve-root pressure • LEG PAİN: If pain extends below the knee, it is more likely to be due to pressure on a nerve than to a muscle problem. The pain starts in the buttock and travels down the back of the leg as far as the ankle or foot. The pain usually affects only one leg.

Symptoms of nerve-root pressure – Pain can be made worse by activities that cause you to forcefully contract the core muscles of your trunk, such as a cough, sneeze, or a difficult bowel movement, or if you hold your breath during an activity (Valsalva maneuver) – Nerve-related problems, such as tingling, numbness, or weakness in one leg or in the foot, lower leg, or both legs
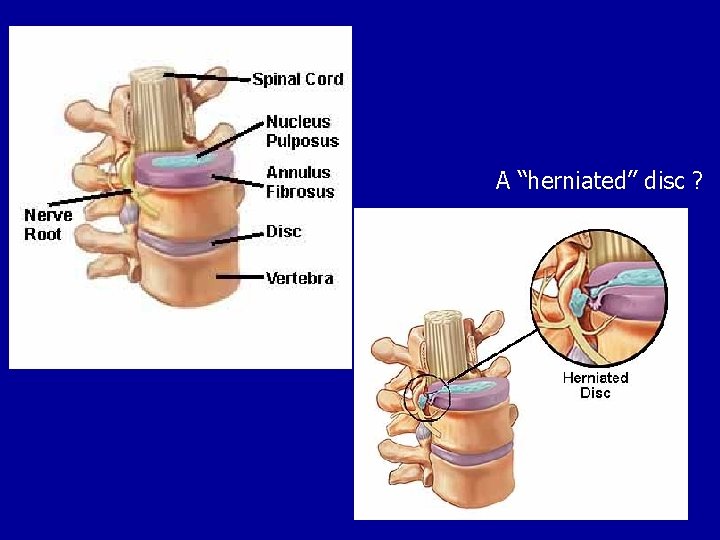
A “herniated” disc ?
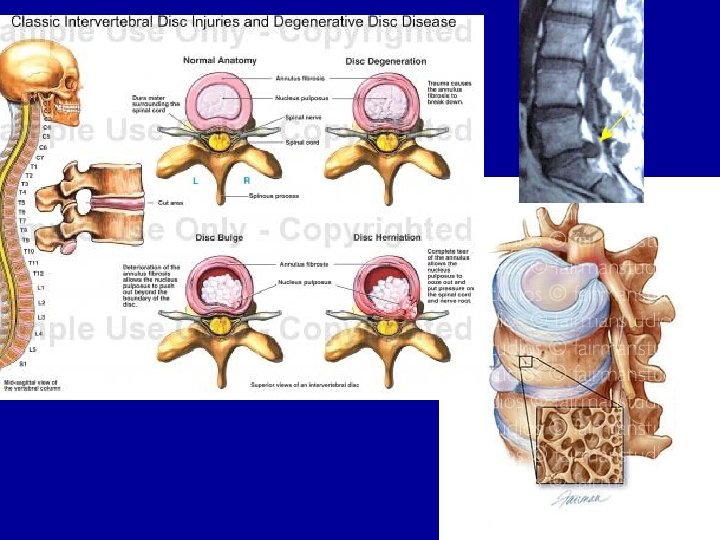
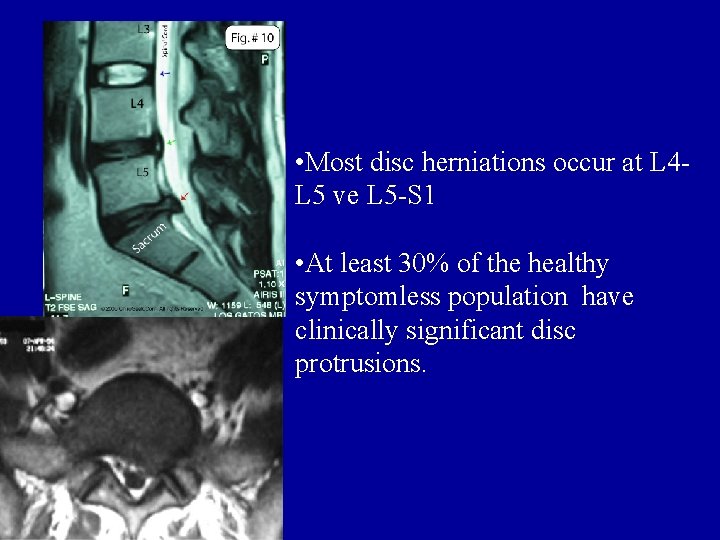
• Most disc herniations occur at L 4 L 5 ve L 5 -S 1 • At least 30% of the healthy symptomless population have clinically significant disc protrusions.

Acute LBP: Red Flags for Emergent Surgical Consultation • Cauda equina syndrome • Bilateral sciatica, saddle anesthesia, bowel/bladder incontinence • Abdominal aortic aneurysm • • • Pain pattern is variable Bruits +/- pulsatile abdominal mass • Significant neurologic deficit • If they can’t walk, they can’t be sent home

Other symptoms or conditions that may occur with low back pain and require additional evaluation and treatment • Depression • Drug or alcohol abuse. Use of intravenous illegal drugs is especially risky • Use of steroids over a long period of time. • Unexplained weight loss • Fever • A history of cancer • Bladder or bowel problems • An illness or condition that affects the immune system, such as diabetes, chemotherapy for cancer treatment, HIV (AIDS), or an organ transplant.

Diagnosis






Treatment Approaches • Adequate treatment must address all the factors involved in producing pain. • Adequate treatment starts with a good evaluation. • A good evaluation must include an examination of muscle function.


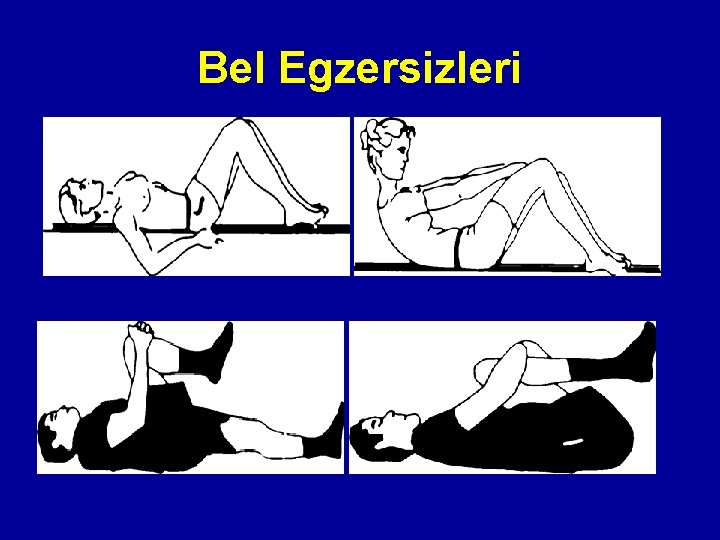
Bel Egzersizleri •
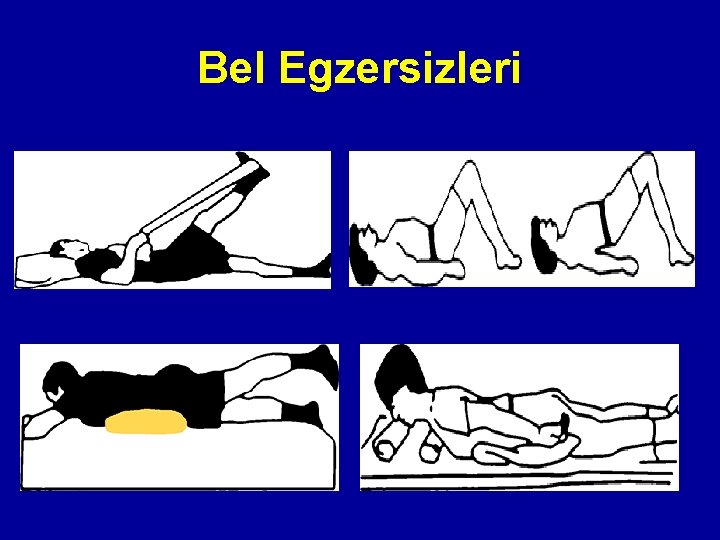
Bel Egzersizleri
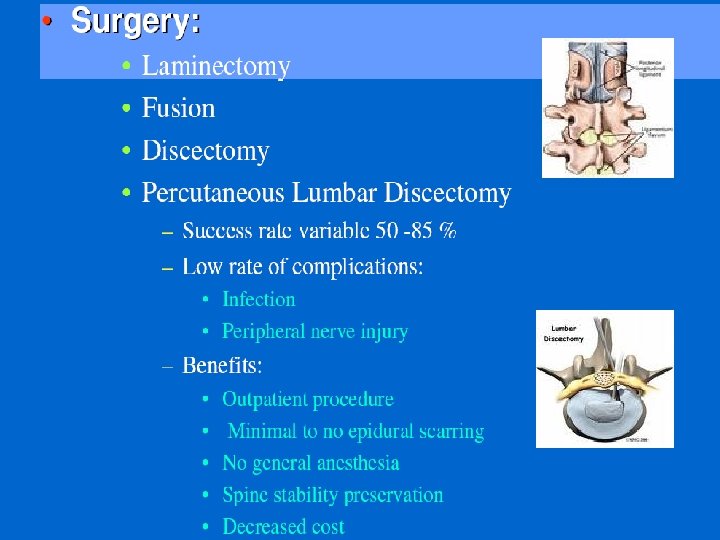

Why Not Get an Operation for a Herniated Disk? • Spontaneous recovery is the rule: 90% resolve over 6 weeks • Long-term outcome of pain relief no different with or without surgery

How Can You Stay Pain-free ? Have good genes – studies of identical twins show a reasonably strong genetic component to disabling low back pain. Avoid sudden unintended movements. This is the presumed cause of most cases of somatic dysfunction. Maintain good posture. A spine that is too flat or too curved increases stress on all the joints and the discs. Exercise regularly and moderately. Have regular check-ups by your physician, to find and fix somatic dysfunctions before they cause bigger problems.
- Slides: 74