Differential Diagnosis and Treatment of Excessive Daytime Sleepiness






























































- Slides: 63

Differential Diagnosis and Treatment of Excessive Daytime Sleepiness 1

What is EDS? n n Excessive daytime sleepiness u The tendency to fall asleep during normal waking hours 1 Contrast with “fatigue” u A desire to rest due to feelings of exhaustion 1 u Symptom of underlying disorder 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 2

EDS – a common complaint n n n Almost ½ of all Americans report a sleeprelated problem 1 EDS is the primary complaint of 1 in 8 people seen in sleep clinics 2 More than 1 in 4 patients complain of EDS in the primary care setting 3 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Roth T & Roehrs TA; Clin Ther. , 1996; 3. Kushida CA, et al. Sleep Breath; 2000. 3

EDS characteristics n n n Number of daily episodes vary Occurs during passive activities u TV watching, sitting on a plane Occurs during more active tasks u Driving, eating, speaking 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Bassetti C & Aldrich MS. Neuro Clin; 1996. 4

The Consequences of EDS 5

Consequences to Self n n n Productivity 1, 2 Motivation 2 Interpersonal relationship problems 2 Depression + anxiety 1, 3 Insomnia 1 Quality of life 1, 2 1. Hasler G, et al. J Clin Psychiatry; 2005; 2. Daniels E, et al. J Sleep Res; 2001; 3. Theorell-Haglow J, et al. Sleep; 2006. 6

Consequences to Health n Sleepiness vs. blood pressure 1 u EDS symptoms = t Sleep BP t Daytime systolic/diastolic variability t Anger, depression, anxiety t More likely to get a diagnosis of hypertension 1. Goldstein IB, et al. Am J Hypertens; 2004. 7

Consequences to Health n Sleepiness vs. CVD in older adults 1 u EDS symptoms = t CVD mortality • 200% in men; 40% in women t CVD morbidity • 35% more MI and CHF in men; 66% more in women 1. Newman AB, et al. J Am Geriatr Soc; 2000. 8

Consequences to Society n n n Crashes when driver falls asleep 1 u 100, 000 each year in U. S. u 1, 500 deaths u Death rate may exceed alcohol-related crashes ~1/2 of all work-related accidents 2 1 in 5 public accidents due to falls 2 1. Mahowald MW. Postgrad Med; 2000; 2. Leger D. Sleep; 1994. 9

Drivers beware: sleepiness vs. drunkenness n Study compared effects on performance of sleep deprivation and alcohol 1 n Drivers who went 17 -19 hours without sleep = drivers with 0. 05% BAC n Sleepy drivers responded ~50% more slowly/less accuracy than fully awake drivers n Sleepiness can compromise performance needed for road and job safety 1. Williamson AM & Feyer AM. Occup Environ Med; 2000. 10

Patient assessment 11

Is sleep the new vital sign? n n n Growing evidence shows that sleep is an important ingredient in good health 1 Few MDs address sleep quality in their practices u <10% of patient charts document sleep history 2 Sleep disorders are underdiagnosed, undertreated 1. Wilson JF. Am Coll Physicians; 2005; 2. Namen AM, et al. South Med J; 2001. 12

Pathophysiology of EDS n n EDS is not a disorder – but a symptom 1 Causes 2: u CNS abnormalities, e. g. narcolepsy u Sleep deficiency, e. g. sleep apnea u Circadian imbalances, e. g. jet lag u Drug side effects, e. g. marijuana 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Roth T & Roehrs TA. Clin Ther; 1996. 13

How does the patient report symptoms? ü I’m tired ü ü I feel lazy I have low energy I feel drowsy I feel sleepy 14

Assess for other psychiatric comorbidities n Symptoms of depression? n n n Mood or memory problems? Does patient fall asleep suddenly? Is the patient a “night owl”? Does the patient drink or take drugs? How many hours sleep per night, including weekends and weekdays? 15

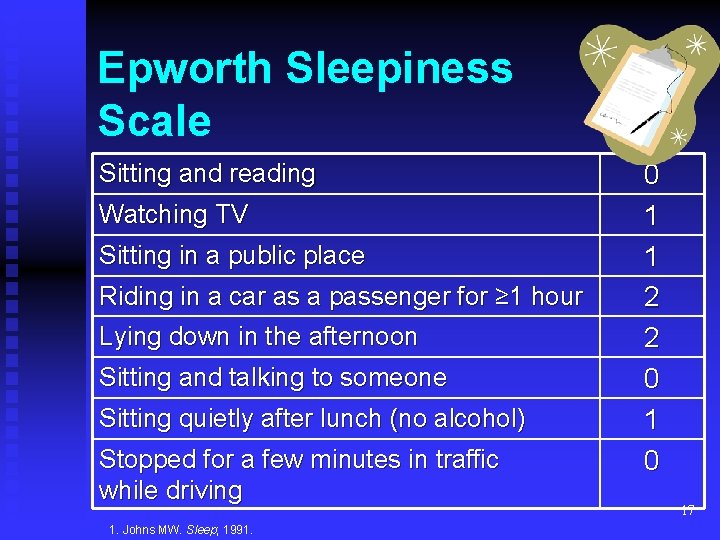
Epworth Sleepiness Scale n n n A quick, in-office test 1 Assesses whether a person will get sleepy in certain situations Use this scale for each situation: u 0 = would never doze or sleep u 1 = slight chance of dozing or sleeping u 2 = moderate chance of dozing or sleeping u 3 = high chance of dozing or sleeping 1. Johns MW. Sleep; 1991. 16

Epworth Sleepiness Scale Sitting and reading Watching TV Sitting in a public place Riding in a car as a passenger for ≥ 1 hour Lying down in the afternoon Sitting and talking to someone Sitting quietly after lunch (no alcohol) Stopped for a few minutes in traffic while driving 1. Johns MW. Sleep; 1991. 0 1 1 2 2 0 17

Rule out other medical conditions 1 n n n n Stroke Tumors/cysts Vascular malformations Head trauma CNS infections (sleeping sickness) Parkinsonism Alzheimer's, other dementias 1. Black JE, et al. Neurol Clin; 2005. 18

Differential Diagnosis 19

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 20

Insufficient sleep syndrome n Have patient keep a sleep log 1 u Bedtimes u Number/time of awakenings u Arising times u Frequency/duration of naps u Bedtime events (food, alcohol, physical activity) 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 21

Falling asleep vs. staying asleep n Difficulty falling asleep 1 u u n Suggests delayed sleep phase syndrome Chronic psychophysiologic insomnia Inadequate sleep hygiene Restless legs syndrome Difficulty staying asleep u u u Suggests advanced sleep phase syndrome Major depression Sleep apnea Limb movement disorder Aging 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 22

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 23

Obstructive sleep apnea n n Absence of breathing during sleep Obstruction of airways snoring, decrease in oxygen saturation of hemoglobin, arousal 1 Result is disturbed sleep and EDS Most common diagnosis of patients with complaint of EDS who seek care at US sleep centers 2 u Almost 7 out of 10 patients 1. Victor LD. Am Fam Physician; 1999; 2. Punjabi NM, et al. Sleep; 2000. 24

Obstructive sleep apnea n n Associated with: u Not only CVD and obesity, but also: u Metabolic syndrome 1 Untreated OSA Direct/deleterious effects on CV function and structure 3 u Sympathetic activation u Oxidative stress u Inflammation u Endothelial dysfunction 1. Vgontzas AN, et al. Sleep Med Rev; 2005; 2. Shamsuzzaman AS, et al. JAMA; 2003; 3. Narkiewicz K, et al. Curr Cardiol Rep; 2005. 25

Obstructive sleep apnea n n Systolic BP and heart rate 1 CRP concentrations 1 u n n May contribute to ischemia, CHF, arrhythmia, cerebrovascular disease, stroke Atrial fibrillation can predict OSA 2 u 49% vs. 32% who do not have OSA 1 in 15 has moderate to severe OSA 3 u 1 in 5 has mild OSA 1. Meier-Ewert HK, et al. J Am Coll Cardiol; 2004; 2. Gami AS, et al. Circulation; 2004; 3. Shamsuzzaman AD, et al. JAMA; 2003. 26

Physical exam for OSA n Check for: 1 u Obesity, especially at midriff & neck u Jaw and tongue abnormalities u Nasal obstruction; enlarged tonsils u Expiratory wheezing u Spinal curvature u Note signs of R ventricular failure t Edema, abdominal distention 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 27

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 28

Substance/medication use n EDS can be a sign of drug-dependent and drug-induced sleep disorders 1 u Chronic use of stimulants u Hypnotics, sedatives u Antimetabolite therapy u OCs; thyroid medications u Withdrawal from CNS depressants 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 29

Substance/medication use n n Review the patient’s Rx drug use u Check for interactions, high doses Inquire about OTC medications u Diphenhydramine, anticholinergics Take alcohol history u Interaction with Rx or OTCs? Ask about recreational drug use 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 30

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 31

Shift-work disorder n n n Circadian rhythm sleep disorder 1 u Internal/environmental sleep-wake cadence out of synch Insomnia, EDS, or both 1 ~10% of the night and rotating shift work population 2 n 4 -fold in sleepiness-related accidents, absenteeism, depression 2 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Drake CL, et al. Sleep; 2004. 32

Shift-work disorder n n n Resolves as body clock realigns 1 Fixed-shift work is preferable u Full-time night or evening Rotating shifts should go clockwise u Day Evening Night Helpful: Bright light, masks, white noise Short t 1/2 hypnotics, wake-promoting drugs used judiciously 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 33

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 34

Delayed-sleep phase syndrome n n Sleep cycle out of synch with desired wake times 1 Problem: Going to sleep and awakening late (3 AM and 10 AM) If earlier wake times are necessary, then EDS can result u Poor performance in work/school Improved sleep hygiene is key 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 35

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 36

Narcolepsy n n Pathologic sleepiness, sudden loss of muscle tone (cataplexy), fragmented sleep, sleep paralysis 1 Affects 1 out of 2, 000 people 2 u 140, 000 Americans 2 Delay of 10 yr from onset to diagnosis is common 1 The cause is unknown 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Ohayon MM, et al. Neurology; 2002. 37

Narcolepsy Pathophysiology n n n Cause? – hypocretin-secreting neurons 1, 2 u Regulate arousal state in hypothalamus Marker – REM sleep during ≥ 2 daytime naps 3 Dysfunctional switching to REM sleep wakefulness during sleep 3 u Patients are mentally awake but physically in REM sleep – sleep paralysis syndrome. 1. Thannickal TC, et al. Neuron; 2000; 2. Sutcliffe JG & de Lecea. Nat Rev Neurosci; 2002; 3. Scammell T. Ann Neurol; 2003. 38

Narcolepsy Pathophysiology n n Genetic predisposition 1 u Familial clustering u 10 - to 40 -fold vs. general population Hallmark symptom – cataplexy u Bilateral weakness 2 u Prevalence ~ 75%2 1. Nishino S, et al. Sleep Med Rev; 2000; 2. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 39

Narcolepsy – Diagnosis n n n Diagnostic for narcolepsy 1 u History of cataplexy u Nocturnal polysomnography u MSLT Differential diagnosis 1 u Lesions of brain stem, hypothalamus u Encephalitis, metabolic disorders Urine and blood exams can confirm nonnarcoleptic EDS 1 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 40

Most frequent causes of EDS Insufficient sleep syndrome n Obstructive sleep apnea n Substance/medication use n Shift-work sleep disorder n Delayed sleep-phase syndrome n Narcolepsy n Periodic limb movement disorders n 41

Periodic limb movement disorders n n Abnormal twitching/kicking of legs during sleep 1 u Interferes with nocturnal sleep EDS u ~10% of adults 2 u Restless legs syndrome t More common in middle/later years t Creeping/crawling sensations Abnormalities in dopamine transmission 2 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Hornyak M, et al. Sleep Med Rev; 2006. 42

Periodic limb movement disorders n Often occurs in narcolepsy and OSA 1 n Seen in pregnancy, renal/hepatic failure, anemia and other disorders n Sleep history/partner’s testimony n Test: Iron, anemia, kidney/liver function n Dopamine agonists can be helpful 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Hornyak M, et al. Sleep Med Rev; 2006. 43

When to refer? 44

Know when to treat and when to refer n n Can condition be treated via sleep hygiene? u Insufficient sleep syndrome u Substance/medication use u Delayed sleep-phase syndrome u Shift-work sleep disorder Counsel on sleep architecture Do blood work, RFTs/LFTs Prescribe sedatives prudently 45

Know when to treat and when to refer n Refer when diagnosis appears to be: u Obstructive sleep apnea Pulmonologist, sleep clinic, surgeon u Narcolepsy Neurologist, sleep clinic u Periodic limb movement disorders Internist, endocrinologist, sleep clinic 46

The sleep clinic n n Sleep studies evaluate EDS as well as OSA, narcolepsy, periodic limb movement disorders Polysomnography 1 u Data accumulated from patient as s/he sleeps u Quantifies sleep adequacy u Determines what causes EDS 1. AARC-APT. Respir Care; 1995. 47

The sleep clinic Polysomnography n n Measures 1: u EEG u Eye movements u Heart rate u O 2 saturation u Muscle tone & activity All-night test 1. AARC-APT. Respir Care; 1995; 2. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 48

The sleep clinic – MSLT n Multiple Sleep Latency Test u Complimentary test for narcolepsy 1 u Assesses speed of sleep onset u REM sleep is monitored u All-day test: 8 -10 hours u High ESS scores ~ Low MSLT scores 2 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006; 2. Chervin RD, et al. J Psychosom Res; 1997. 49

Treatment 50

Non-pharmacologic treatment n n Rationale – To improve natural sleep Counsel patients on good sleep hygiene 1 u Regular sleep schedule u Restrict time in bed u Sleep-conductive environment u Exercise u Avoid stimulants u Incorporate relaxation techniques 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006 51

Pharmacotherapy – Hypnotics n n n Rationale – To treat insomnia Sleep-onset insomnia u Use drugs with shorter t 1/2 t Zalepon, zolpidem, triazolam Sleep-maintenance insomnia u Use drugs with longer t 1/2 t Temazepam, eszopiclone 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006 52

Pharmacotherapy – Hypnotics n n Use with caution in elderly, pulmonary insufficiency To tolerance, use lower doses for brief periods; taper off slowly In patients who continue to have EDS, stop or switch the drug Monitor for amnesia, hallucinations, incoordination, falls 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006 53

Pharmacotherapy – Stimulants n n n Rationale – To improve alertness Methylphenidate, amphetamines Indirect-acting sympathomimetics 1 u Produce behavioral activation and increased arousal, motor activity, alertness Used mostly for EDS; ineffective for cataplexy 1, 2 Immediate- or extended-release forms 1 1. Mitler MM & Hayduk R. Drug Saf; 2002; 2. Littner M, et al. Sleep; 2001. 54

Pharmacotherapy – Stimulants n n MPH and the amphetamines are Schedule II u Carry the risk of substance abuse/illicit use Rebound hypersomnia or tolerance to alerting agent can occur 1 u Switch to a different drug class or provide drug holiday 1. Black JE, et al. Neuro Clin; 2005. 55

Pharmacotherapy – Modafanil n n Rationale – To promote wakefulness Approved for narcolepsy-associated EDS Ill-defined MOA (not a stimulant)1 u Activates hypocretin-secreting neurons 1, 2 u Does not control cataplexy 1 Long-acting – once-daily dosing u Peak plasma concentrations – 2 -4 hr 3 u Small afternoon booster dose can be used 4 1. US Modafinil. Ann Neurol; 1998; 2. Willie JT, et al. Neuroscience; 2005; 3. Provigil PI; 2004; 4. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006. 56

Pharmacotherapy – Modafanil isomer n n n Isomer formulation – r-modafanil or armodafanil – also being evaluated Once daily for EDS 2 u r-isomer T 1/2 = 10 -14 hr vs. 3 -4 hr for sisomer u Higher peak concentrations vs. racemic mixture No efficacy/safety advantage over modafainil 2 1. Harsh JR, et al. Curr Med Res Opin; 2006; 2. Dinges DF, et al. Curr Med Res Opin; 2006. 57

Pharmacotherapy – Sodium oxybate n n n Rationale – To treat EDS, narcolepsy FDA-approved for treatment of EDS and cataplexy in narcolepsy 1 MOA largely unknown 2 Rapidly acting hypnotic (Tmax 0. 5 -1. 25 hr)2 Short t½ (0. 5 -1 hr)2 duration of stages 3, 4 sleep u First REM sleep , then with continued use, REM sleep 1. FDA Talk Paper; 2002; 2006; 2. Xyrem PI; 2005. 58

Pharmacotherapy – Sodium oxybate n n n Studies show efficacy in cataplexy and EDS 1, 2, 3 u cataplexy attacks, ESS scores Can be used with modafinil 4 u nightly awakenings Dosing: twice nightly u Taken HS, then at 2. 5 -4 hrs after the sleep begins 1. Xyrem. Sleep Med. 2005; 2. Xyrem. Sleep; 2003; 3. Xyrem. Sleep; 2002; 4. Xyrem. Sleep Med; 2004; 5. Bogan RK. Sleep. 2005; 6. Xyrem PI, 2005. 59

Pharmacotherapy – Sodium oxybate n n Potential drug of abuse (CIII)1 u Enforced as Schedule I Special distribution requirements 2 u Use of a central pharmacy u Registration of prescribing MD u Pharmacy verification of MD’s eligibility to prescribe u Registration/required reading of materials by patient 1. FDA Talk Paper; 2002; 2006; 2. Xyrem PI; 2005. 60

Continuous positive airway pressure n n Rationale – To correct OSA Reverses EEG slowing for both REM sleep and wakefulness 1 Improves symptoms of EDS 1 u MSLT scores u Persistent EDS 2° to obesity Used at home but pressure is set in sleep clinic first 1. Morisson F, et al. Chest; 2001. 61

Surgery n n n Rationale – To correct anatomical flaws UPPP is the most common procedure u Enlarges airways u Submucosal tissue resection from tonsillar pillars; adenoid resection u Not suitable for obese patients Trachestomy – last resort u May take ≥ 1 year to heal 1. Beers MH, et al. Merck Manual of Diagnosis and Therapy; 2006 62

Conclusions n n EDS quality of life; can cause serious consequences EDS may be a sign of sleep apnea, narcolepsy or a symptom of another condition Patients who complain of EDS should be assessed in a step-wise manner to rule out the various conditions that can cause it Know when to treat and when to refer 63