Diet PCOS presented by Martha Mc Kittrick RD

Diet & PCOS presented by Martha Mc. Kittrick RD, CDE Website: Martha. Mc. Kittrick. Nutrition. com Blog: City. Girl. Bites. com Contact: mmckittnyc@gmail. com Twitter: @citygirlbites

Goals of Discussion Provide background information on PCOS Discuss the role of insulin resistance in PCOS Diagnosing & treating PCOS Provide the RD with guidance for lifestyle education for the patient with PCOS


Part One: Background Information on PCOS

PCOS was first identified by Stein & Leventhal in 1935 They described a group of women who were obese and infertile, with enlarged ovaries and multiple cysts Few of these original features are now considered consistent findings in PCOS

More Common Than You Think PCOS is possibly the most common hormone abnormality that exists! Up to 10% of all females have PCOS 6 million American women have PCOS #1 cause of anovulatory infertility

What is PCOS ? ? ?

What is PCOS? PCOS is a complex hormonal disturbance that affects the entire body It has numerous implications for general health and well being It can affect all females – from adolescence to post menopause Accounts for ~ $40 billion yearly in the U. S. Dr. Azziz

Statistics 80%+ show PCO on ultrasound (but having PCO does not mean PCOS!) 40 – 80% will have a fertility problem 60 - 80% hirsuitism 40 - 70% scalp hair thinning (alopecia)

Statistics 75 - 90% irregular menstrual periods 40 - 60% acne 70% - hyperlipidemia (often low HDL, high LDL)* 10% - acanthosis nigricans * Legro RS, et al, Am. J. Med. 111, 607 -613 (2001).
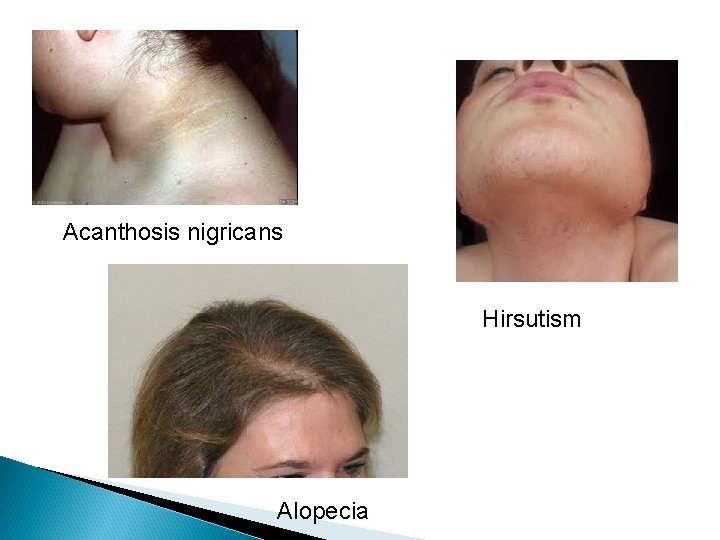
Acanthosis nigricans Hirsutism Alopecia

Health Risks That May Be Associated with PCOS Insulin resistance (up to 80% of women with PCOS) Metabolic syndrome (~ 1 in 3 women with PCOS) Increased risk of diabetes/prediabetes (> 50% will get this by age 40) Obesity (~ 50% of women with PCOS)

Health Risks That May Be Associated with PCOS Endometrial Cancer Obstructive sleep apnea HTN Mood disorders

Mood Disorders and PCOS Increased incidence of mood disorders (i. e. depression or anxiety, or to engage in bingeing). Certain features of PCOS may contribute to the increased risk of mood disorders. For example: Abnormal levels of androgens and other hormones are related to mood disorders Obesity is linked to mood disorders as well as to abnormal hormone levels. Studies show that the risk of mood disorders is even greater among women with PCOS who are also obese http: //www. nichd. nih. gov/health/topics/PCOS/conditioninfo/Pages/default. a spx

Health Risks That May Be Associated with PCOS Heart disease Inflammation Pregnancy complications

Consensus Statement by the Androgen Excess PCOS Society re: Cardiovascular Risk & Prevention of Cardiovascular Dz in Women with PCOS: Conclusions: Women with PCOS Obesity, Cig. Smoking, Dyslipidemia, HTN, IGT, Subclinical Vascular Dz = At risk Whereas those with metabolic syndrome and/or type 2 DM = High risk http: //www. pcoschallenge. org/symposium/2014 -presentations/pcospreventing-cardiovascular-disease-gregorry-pokrywka. pdf

Lean PCOS and Heart Disease Risk? The absence of the important cardiometabolic risk factor represented by obesity often misguides clinicians when lean PCOS patients are evaluated Actually, IR even in lean women represents an important risk factor for glycometabolic and cardiovascular sequelae http: //www. sciencedirect. com/science/article/pii/S 001502821400315 X

Inflammation and PCOS Research suggests that PCOS associated with long-term, low-grade inflammation polycystic ovaries to produce androgens Inflammation is associated with hardened arteries major risk factor for heart attack & stroke. ? inflammation results from obesity and metabolic dysfunction or whether it’s an independent symptom of the disorder

PCOS & Pregnancy Complications Spontaneous Abortions - increased in high BMI/PCOS pts Impaired Glucose Tolerance Gestational Diabetes HTN Small for Gestational Age http: //www. pcoschallenge. org/symposium/2014 presentations/pcos-improving-feritliy-mark-perloe. pdf

Etiology – not 100% Clear Likely a Genetic & Environmental component

Etiology Genetic. Research has found subtle changes in insulin receptor gene which may alter its function in the ovaries. It is known that insulin is capable of stimulating the ovaries to produce testosterone which causes many of the symptoms of PCOS Combination effect of pituitary lutenizing hormone (LH) & insulin on stimulating the ovary to produce excessive male hormone (androgens). Obesity magnifies this. Intrinsic enzymatic abnormalities have been demonstrated in the ovaries as well as the adrenal glands

Part Two: Role of Insulin Resistance in PCOS

What is Insulin Resistance? IR is a condition where cells do not adequately respond to insulin IR appears to result from several defects in the relationships among insulin, its receptor, and the genome IR increases with age and is aggravated by obesity IR is exacerbated at puberty and in pregnancy
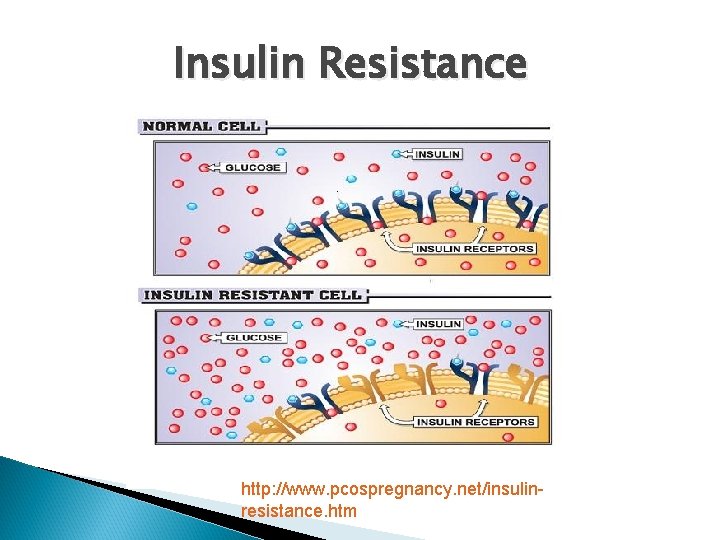
Insulin Resistance http: //www. pcospregnancy. net/insulinresistance. htm

Effects of IR & Hyperinsulinemia and/or Visceral Obesity Stimulation of ovarian and adrenal androgen production Stimulation of pituitary luteinizing hormone (LH) secretion Inhibition of hepatic sex hormone binding globulin (SHBG) production, leading to a reduced total testosterone in men and increased free testosterone in women Increased risk of miscarriage

Effects… continued Increased BP Low HDL, high TG Increased apolipoprotein B levels Small dense LDL cholesterol particles Increased fibrinogen levels Increased C reactive protein and other inflammatory markers Increased thickening and pigmentation of skin (acanthosis nigricans) Premature atherosclerosis

Insulin Resistance in PCOS Can also lead to Increased food cravings Weight gain and/or difficulty losing weight

Diagnosing Insulin Resistance is tricky!! Insulin levels vary throughout the day Normal range is up to 18, however many experts feel any number over 8 is high

Labs: IR / Glucose Intolerance Test Interpretation Fasting insulin (not very accurate test!) 8 -14 m. U/L mild IR > 14 -18 moderate – severe Fasting glucose/insulin ratio < 4. 5 (< 7. 0 in adolescents) Oral glucose tolerance Normal: 2 hr < 140 test Impaired: 2 hr 140 -199 Diabetes: 2 hour glucose ≥ 200

Labs: IR / Glucose Intolerance HOMA (Homeostasis Model Assessment) < 2 = normal, 2. 2 - 3 = moderate, > 3 = severe Hyperinsulinaemic glucose clamp “gold standard” – but rarely used Other clues of IR: Elevated LH/FSH ratio Low SHBG Low HDL and/or TG Upper-body obesity Acanthosis nigricans BMI > 25 (or waist circumference > 35” in women) Fam hx of type 2 diabetes or glucose intolerance Age > 40

Do Lean Women with PCOS Have Insulin Resistance?

Insulin Resistance in Lean PCOS Study: 72% of overweight/obese pts with PCOS were IR compared to 26% lean Hypothesized that lean PCOS pts could be affected by an “intrinsic” form of IR whereas obese patients have a combined form of IR due in part to the syndrome itself and in part to the weight excess. In fact, lean PCOS patients could be considered to be a “unique model” to study the natural history of IR per se, because the IR occurs in the presence of normal glucose http: //www. sciencedirect. com/science/article/pii/S 001502821400315 X

Non-Obese PCOS Patients 10. 3% of lean PCOS have IGT and 1. 5% have diabetes. In long -term f/u, 16% of women who had been treated for PCOS 20– 30 yrs. earlier had developed DM by menopause. The etiology of the insulin resistance is unclear, but suppression of the excess androgens does not alter the insulin resistance Even in lean PCOS, a higher waist-to-hip ratio is seen in those with PCOS compared to those without PCOS. This is supported by the higher proportion of visceral adiposity measured by ultrasound in lean PCOS patients compared to weight-matched control subjects Obese women with PCOS have greater insulin resistance than weight -matched control subjects or lean PCOS subjects http: //clinical. diabetesjournals. org/content/21/4/154. full

Part Three : Diagnosing and Treating PCOS

Diagnosing PCOS Symptoms and physical exam Hormonal testing Ultrasound

Diagnosing PCOS Much controversy on what the proper diagnostic criteria are! Using the Rotterdam criteria, a woman with 2 of the 3 cardinal features that characterize PCOS may have the condition: Hyperandrogenism (androgen excess) based on: -sx: acne, excessive hirsutism or male-pattern hair loss -elevated circulating levels of androgens (usually testosterone) Ovulatory dysfunction – can be manifested as oligomenorrhea or infrequent menstruation Small cysts on the ovaries as seen on ultrasound. Legro BMC Medicine (2015) 13: 64
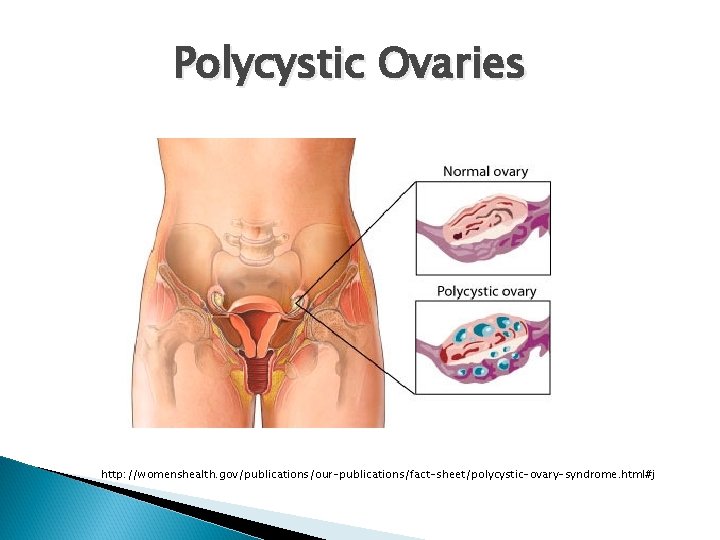
Polycystic Ovaries http: //womenshealth. gov/publications/our-publications/fact-sheet/polycystic-ovary-syndrome. html#j

Goals of Treatment Individualization is essential Regulation of cycle Promote weight loss Correction of metabolic abnormalities - Cholesterol, glucose, insulin resistance, blood sugar, HTN Decrease androgens - Skin, hair Improve Fertility Improve overall well-being

Treatment Traditional: the individual symptoms were treated ◦ BCP, anti-androgens, fertility treatments More recent: targets insulin resistance as well as the individual symptoms ◦ Traditional treatments as above as well as weight loss/exercise and insulin sensitizing agents (ISA)

Metformin: Insulin Sensitizer Brand names Glucophage, Glucophage XR, Fortamet, Riomet, Glumetza, and others Lowers blood glucose Slows release of glucose from liver Decreases insulin resistance in muscle Lowers androgen and insulin levels May lower LDL May aid in weight loss Off label usage in PCOS Helps overweight and normal weight women achieve ovulation

Metformin Dosing & Safety Info Gastrointestinal intolerance in 30% Contraindications: (take with meal) - Creatinine ≥ 1. 4 mg/d. L (for women) - Liver disease (or risk thereof: alcohol abuse/binge drinking) - Other risks for lactic acidosis: pulmonary disease, congestive heart failure Dosages range from 500 -1000 mg bid. Start slow!! May need B 12 supplement

Efffects of Metformin on Fertility Has been shown to restore regular menstruation in > 90% amenorrheic adolescents, restoring ovulation in 80% More effective at restoring ovulation than clomiphene Potentiates the effect of clomiphene Taken during the 1 st trimester, reduces miscarriage rate by 80% However – not every women needs Metformin!

First Step in Treatment… Diet & Exercise!!! Benefits Include: Increased regularity of menstrual cycles Decreased levels of androgens Improvement in lipid levels Decreased risk of diabetes Improves insulin sensitivity

Part Four: Lifestyle Counseling Tips - exercise nutrition counseling session practical tips

Which is best? We igh t tra inin g? o? i rd Ca Mo vem en t? HIIT ?

How Exercise Improves Insulin Sensitivity - Enhances both GLUT 4 -dependent and hypoxiadependent glucose transport in skeletal muscle - Increases skeletal muscle vascularization, mitochondrial neobiogenesis and eventually tissue mass - Repartitions intracellular fat, thereby improving its utilization - Fat mass loss Physical Activity and Insulin Sensitivity The RISC Study Diabetes. 2008 Oct; 57(10): http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 2551669/
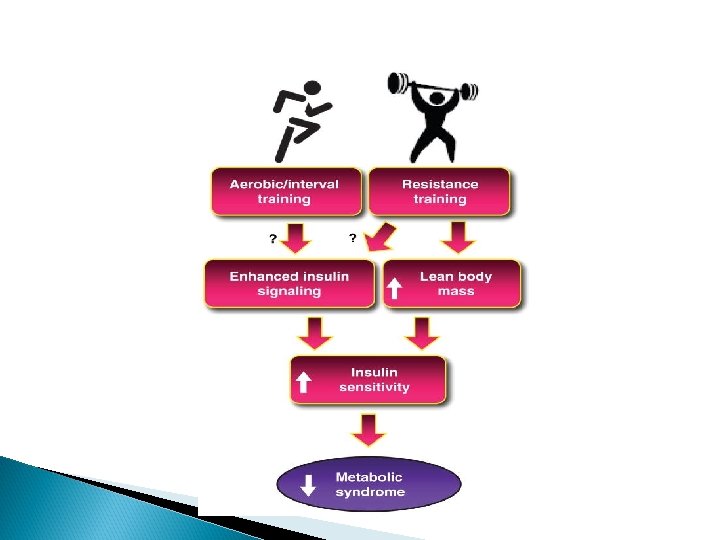

Aerobic Exercise Aerobic exercise increases insulin sensitivity (especially in skeletal muscle) from ~ 25 -50% in all ages, gender, body weights

Resistance Training A systemic review of 20 studies found that supervised resistance training improved glycemic control and insulin sensitivity in a wide variety of study groups *however this review showed that RT compliance and glycemic control are generally less without supervision http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 4129661/#R 278

High-Intensity Interval Training HIIT demonstrates improved insulin sensitivity http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 4129661/#R 278

Total Accumulated Activity More Important Than Intensity RISC Study: activity has beneficial effects on insulin sensitivity Total accumulated activity was the important factor rather than intensity of the activity. More movement during the day as well as from exercise, accumulated to exert a beneficial effect on insulin sensitivity http: //www. ncbi. nlm. nih. gov/pmc/articles/PMC 4129661/#R 278

Benefits of Exercise Increases insulin sensitivity Decreases blood pressure Raises HDL, decreases TG Burns calories Increases lean mass Aids in stress management Lowers fasting glucose

My Recommendations for Exercise Anything is better than nothing Get a baseline and increase from there Ideally 3 aerobic and 2 weight training sessions a week (but not many can do this!) Suggest some HIIT sessions in motivated fit patients Increase everyday movement Consider activity tracker Beware of “over-exercisers”

Additional Benefits of Exercise in PCOS In PCOS, women who self-reported 8 hours of sports activities per week had improvement in acne and menstrual irregularities Exercise as the primary intervention without attendant weight loss (< 5% weight loss) improved insulin sensitivity and free testosterone index and induced ovulation in 9 of 18 obese PCOS patients Julie L. Sharpless, MD http: //clinical. diabetesjournals. org/content/21/4/154. full

Nutrition Counseling for PCOS

5 Nutrition Tips for PCOS No one eating plan works for everyone Realistic, livable eating plan Long term healthy diet to decrease health risks If overweight, lose 5 -10% of body weight Low glycemic seems to work best

Obtain Medical Info • PMH • Symptoms (menstrual history, skin, hair, weight) • Labs (full lipid profile, glucose, insulin, GTT) • Meds (BCP, anti-androgen, insulin sensitizer, etc. ) • Family hx of PCOS, diabetes, heart disease

Tips for Counseling Sessions Obtain medical history (including fam. hx), as well as labs, meds, supplements Ask about symptoms Obtain weight, diet history Ask about “food/mood/energy level” link Provide education on PCOS Discuss exercise Address sleep, mood, sitting time Develop individually tailored meal plans Set realistic goals Maintain supportive demeanor Develop referral network

Initiate Education on PCOS Hormonal imbalance Explain insulin resistance How food affects insulin & glucose levels Importance of weight loss (even 5 -10% of body weight Role of exercise in lowering insulin levels

Tips to Improve Insulin Resistance Lose weight if overweight Exercise Do not smoke Low glycemic index diet Medications (insulin sensitizing agents)

What Kind of Plan Will Work Best for You? Do you feel tired soon after eating a high carb meal and / or does this meal trigger sugar cravings? Do meals higher in protein and fat make you feel more energetic? Do you feel very tired or irritable if you go for more than 4 hours without eating? Do you constantly crave carbs? Is your LDL cholesterol high? Are your triglycerides high?

Summary of Lifestyle Recs for PCOS Calorie control if weight management needed Low glycemic Ideally combine “healthy” carb + protein + fat at meals. Promotes satiety and may help prevent insulin spikes Anti-inflammatory foods Heart healthy diet Consume adequate omega 3 fats (supplement if needed)

Summary of Lifestyle Recs for PCOS Magnesium rich foods Adequate sleep Stress management Exercise: cardio & weight train & movement Pay attention to how foods make you feel Supplement if needed (Vit B 12, Vit D, ? Omega 3, others? )

One step further: Environmental chemical exposures Endocrine disruptors BPA Phthalates (some) Pesticides Perchlorate Cosmetics, Fragrances Arsenic Hormones Antibiotics I don’t really address these – just food for thought! Be Fruitful Victoria Maizes MD Integrative Healthcare Symposium, NYC

Supplements & PCOS

Inositol and PCOS • Inositols are C 6 sugar alcohols of cyclohexane • There are 9 stereoisomers of inositol, including myo-inositol and D-chiro-inositol • Inositol is a component of the inositolphosphoglycans (IPGs) which are “secondary messengers” in insulin signaling • Insulin resistance appears to be a main underlying metabolic derangement in PCOS, possibly due to a defect in IPG signaling • Published studies confirm that inositol supplementation can improve insulin sensitivity, reduce serum levels of insulin, testosterone, and LH, and induce ovulation in women with PCOS

Myo-inositol and hormone, metabolic, and ovulation induction effects in women with PCOS • Myo-inositol increased ovulation rates and improved metabolic factors. Gerli, 2007 • Myo-inositol decreased insulin and testosterone levels and improved metabolic factors. Costantino, 2009 • Myo-inositol improved insulin sensitivity and decreased LH and LH/FSH ratio. Artini, 2013 • Myo-inositol improves insulin resistance and hormonal parameters in non-obese women. Genazzani, 2014

Myo-inositol and Egg Quality in Women with PCOS • Myo-inositol decreased the number of days of stimulation, reduced E(2) levels at h. GC administration, and decreased degenerated oocytes without compromising total number of oocytes retrieved. Papaleo, 2009 • Myo-inositol increased number of oocytes retrieved and embryos transferred, and improved embryo scores. Ciotta, 2011 • Myo-inositol, but not D-chiro-inositol, improved egg and embryo quality during ovarian stimulation. Unfer, 2011 • In women without PCOS, myo-inositol significantly reduced number of ooctyes retrieved, with no change in clinical pregnancy rate. Lisi, 2012

Myo-inositol + D-chiro-inositol • Research indicates that a combination of myo- and D-chiro-inositol, in the body’s physiological ratio of 40: 1, is more beneficial than either alone. • This combination improved metabolic parameters more than myoinositol alone after 3 months of treatment in overweight women with PCOS. Nordio and Proietti, 2012 • This combination improved lipid profile in obese women with PCOS. Minozzi, 2013 • This combination (vs. D-chiro-inositol alone) improved egg and embryo quality, and pregnancy rates, in women with PCOS undergoing IVF. Colazingari, 2013

Inositol: Treatment considerations • Inositol is safe and relatively inexpensive • Reasonable evidence of benefit in PCOS, but may be counterproductive in non-PCOS patients • Available from multiple sources online or in retail outlets • Typical recommended daily dose: 2 grams, bid • Typical treatment regimen of 3 -6 months • Myo-inositol vs. Metformin- in one study, women taking 4 g myoinositol had higher pregnancy rates and percentage restored ovulation than women on 1500 mg Metformin (Raffone, 2010)

N-acetyl cysteine (NAC) NAC is an antioxidant & amino acid Derivative of the amino acid L-cysteine, an essential precursor used by the body to produce glutathione Glutathione is an antioxidant produced by the body to help protect against free radical damage, and is a critical factor in supporting a healthy immune system. NAC has also been found to reduce inflammation, heart disease and most recently, insulin http: //www. pcosnutrition. com/links/blogs/nac-and-pcos. html

N-acetylcysteine and PCOS Improved menstrual regularity but has not been shown to help improve fertility in women with PCOS. NAC may help improve insulin resistance in women with PCOS who have high insulin levels and could be used with metformin or if metformin isn't an option. NAC also seems to have a favorable effect of lowering cholesterol, TG and testosterone http: //www. pcosnutrition. com/links/blogs/nac-and-pcos. html

N-acetylcysteine and PCOS Systematic review and meta-analysis of randomized controlled clinical trials 8 studies with a total of 910 women with PCOS were randomized to NAC or other treatments/placebo. RESULTS: NAC showed significant improvement in pregnancy and ovulation rate as compared to placebo No significant difference in rates of the miscarriage, menstrual regulation, acne, hirsutism, and adverse events, or change in body mass index, testosterone, and insulin levels with NAC as compared to placebo. More studies are needed Obstet Gynecol Int. http: //www. ncbi. nlm. nih. gov/pubmed/25653680 2015

Co. Q 10 and PCOS Combination of Co. Q 10 and clomiphene citrate in the treatment of clomiphene-citrate -resistant PCOS patients improves ovulation and clinical pregnancy rates. It is an effective and safe option and can be considered before gonadotrophin therapy or laparosc http: //www. ncbi. nlm. nih. gov/pubmed/? term=Coenzyme+Q 10+and+pcos opic ovarian drilling
- Slides: 75