Diet Nutrition and Inflammatory Bowel Disease Jason K

Diet, Nutrition and Inflammatory Bowel Disease Jason K. Hou, MD Baylor College of Medicine Houston, TX

Disclosures n None

Objectives n At the conclusion of the conference, participant should be able to: 1) Describe the possible role of diet in the development of IBD n 2) Identify the importance of nutritional deficiencies in IBD n 3) Describe the potential use of diet as therapy for IBD n

So doc, what can I eat? n “Intellectual divide” Physicians focus on nutritional deficiencies n Patients interested in diet as cause or cure of symptoms n

Malnutrition- then and now n 20 -85% of IBD patients with proteinenergy malnutrition n n Hospital based studies (1970 s) Most prevalent nutritional abnormality = excess body weight (2007) Sousa Guerreiro et al. Am J Gastroenterol. 2007 Nov; 102(11): 2551 -6

Got milk? n Food avoidance n n 65% of IBD patients report food avoidance 28% of IBD patients on dairy-free diet n Lactose intolerance no more common or even less common in UC than non-IBD controls. Gerasimidis et al. Aliment Pharmacol Ther. 2008 Jan 15; 27(2): 155 -65 Bernstein et al. Am J Gastroenterol. 1994 Jun; 89(6): 872 -7

Diet as Etiology
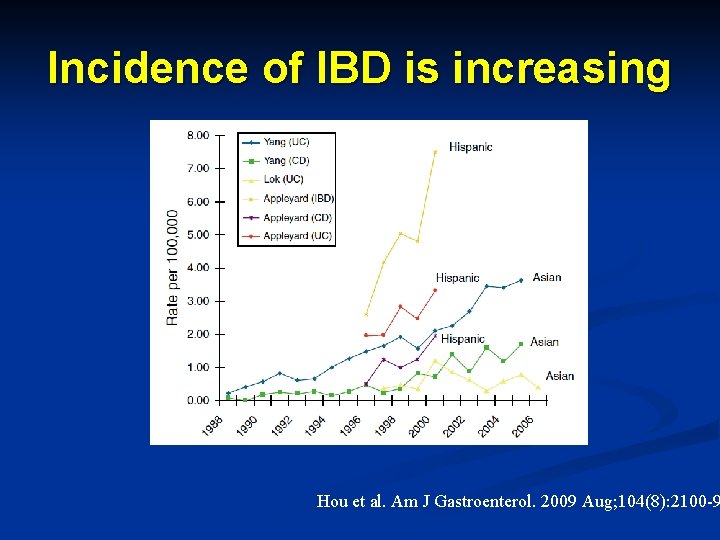
Incidence of IBD is increasing Hou et al. Am J Gastroenterol. 2009 Aug; 104(8): 2100 -9

Dietary fats n Omega 3 -fatty acids Docosahexonenoic acid (DHA) n Eicosapentaenoic acid (EPA) n Docosepentaenoic acid (DPA) n n Omega 6 -fatty acids n Linoleic acid

Dietary fats Hou et al. Therapy, Mar 2010, 7(2), 179 -189

Dietary fats n Food frequency questionnaire in newly diagnosed pediatric CD patients (130 patients) n Dose dependent protective effect of omega-3 FA (EPA, DHA) for CD n OR n 0. 44 (95% CI 0. 19 -1. 00) Ratio of omega-3 PUFA/ omega-6 PUFA n OR 0. 32 (95% CI 0. 14 -0. 71) Amre et al. Am J Gastroenterol. 2007 Sep; 102(9): 2016 -25

Dietary fats n Vegetable, fruit, nut, fish, dietary fiber intake protective in dose dependent manner n “Western diet” n n meat, fried food, fast food, snacks, dessert positive associated in development of CD in girls [OR 4. 7 (95% CI 1. 6 -14. 2)]

EPIC n Prospective cohort study 203, 193 persons n Case control of 126 incident cases of UC n Linoleic acid positively associated with development of UC in a dose dependent manner n OR 2. 49 (95% CI 1. 23 -5. 07 in highest quartile) n Dose dependent protective effect of DHA for UC n OR 0. 23 (95% CI 0. 06 -0. 97) Hart et al. Gut. 2009 Jul 23

EPIC-UK n UK subset of EPIC 25, 639 persons n Ages 40 -74 n 22 incident UC (median f/u 3. 9 years) n The highest tertile of dietary oleic acid protective for UC (OR 0. 11 (95% CI=0. 010. 87) n De Silva et al. Abstract DDW 2010

Carbohydrates n FODMAPs Fermentable n Oligon Din Mono-saccharides n And n Polyols n

FODMAPs n May increase bacterial overgrowth in distal small bowel n n Increase intestinal permeability Trigger CD in susceptible host No data Gibson et al. Aliment Pharmacol Ther. 2005 Jun 15; 21(12): 1399 -40

Nutritional Deficiencies

Nutritional deficiencies n CD n n 32% overweight 8% obese 2. 6% underweight 5. 3 % considered malnourished by SGA Sousa Guerreiro et al. Am J Gastroenterol. 2007 Nov; 102(11): 2551 -6

Nutritional deficiencies n Food avoidance 29% excluded grains n 28% excluded milk n 18% excluded vegetables n 11% excluded fruits n Sousa Guerreiro et al. Am J Gastroenterol. 2007 Nov; 102(11): 2551 -6

Nutritional deficiencies n Percentage of patients who reached daily recommended intake Sousa Guerreiro et al. Am J Gastroenterol. 2007 Nov; 102(11): 2551 -6

Calcium and Vitamin D n 21 -40% increased risk of fractures n n Increased risk even after adjusting for steroid use Management n Bisphonate Bernstein et al. Gastroenterology. 2003 Mar; 124(3): 795 -841 Siffledeen et al. Clin Gastroenterol Hepatol. 2005 Feb; 3(2): 122 -32 von Tirpitz et al. Eur J Gastroenterol Hepatol. 2000 Jan; 12(1): 19 -24

AGA guidelines (2003) n Who to Screen n n n > 3 months steroids Low trauma fracture Postmenopausal female Male > 50 Hypogonadism Management n n DEXA T score < -2. 5 OR history of compression fracture n n Bisphonate -2. 5 <T score < -1 n Bisphonate if need to continue steroids Bernstein et al. Gastroenterology. 2003 Mar; 124(3): 795 -84

Folate/B 12 n Decreased intestinal transportsulfasalazine n Deficiency may result in hyperhomocystinemia n n Hypercoagulable state Folate supplementation- possible Lashner et al. Gastroenterology. 1989 Aug; 97(2): 255 -9 protective against colorectal Lashner et al. Gastroenterology. 1997 Jan; 112(1): 29 -32 cancer/dysplasia

Micronutrients n Zinc n n Selenium n n wound healing possible anti-inflammatory and anti-neoplastic properties Antioxident vitamins

Diet as Therapy

Possible pathways n Remove toxin/antigenic stimulus (elemental diet) n Alter bacteria flora (prebiotic) n Alter intestinal fluid transport/gas production

Enteral therapy n Elemental and non-elemental diet n n No differences in efficacy Limitations n Palatability n May require nasogastric feeding

Enteral Therapy- Cochrane review (2007) Induction of remission: 20 -84% n Beneficial but inferior to corticosteroids n n Open label RCT n 37 pediatric new diagnosed CD n Remission (10 wk) n n ET: 79%; 95% confidence interval (CI), 56%-92% Steroid 67%; 95% CI, 44%-84% P =. 4 n Endoscopic healing seen only in ET group Zachos et al. Cochrane Database Syst Rev. 2007 Jan 24; (1): CD 000542 Borrelli et al. Clin Gastroenterol Hepatol. 2006 Jun; 4(6): 744 -53

Nutritional supplements n Omega-3 - PUFA (Fish oil) and CD EPIC-1 (quiescent disease) n EPIC-2 (flare, remission induction by steroids) n 4 grams daily n Control- MCT n Feagan et al. JAMA. 2008 Apr 9; 299(14): 1690 -

Nutritional supplements n Omega-3 - PUFA n EPIC-1 n At 1 year 31. 6 % vs. 35. 7% relapse n HR 0. 82, 95% CI 0. 57 - 1. 19 n EPIC-2 n At 1 year 47. 8% vs. 48. 8% relapse n HR 0. 90, 95% CI 0. 67 - 1. 21 Feagan et al. JAMA. 2008 Apr 9; 299(14): 1690 -

Nutritional supplements n Omega-3 - PUFA n Cochrane review (2009) n Small n pooled benefit RR 0. 77, 95% CI 0. 61 -0. 98 n Authors conclude likely no benefit based on EPIC Turner et al. Cochrane Database Syst Rev. 2009 Jan 21; (1): CD 00632

Nutritional supplements n Fiber and UC n Converted to short chain fatty acids (SCFA) n Energy source for colonocytes n Modulate local immune response n (attenuate IL-6, IL-8, TNF-α, leukocyte adhesion) n Modify microbiota (prebiotic) Menzel et al. Inflamm Bowel Dis. 2004 Mar; 10(2): 122 Galvez et al. Mol Nutr Food Res. 2005 Jun; 49(6): 601 -8

Nutritional supplements n Butyrate (SCFA) Increase in dietary fiber can increase fecal butyrate n Germinated barley foodstuff (GBF) n n Alter n colonic bacterial concentrations Increase in Bifidobacterium sp. and Eubacterium limosum Hallert et al. Inflamm Bowel Dis. 2003 Mar; 9(2): 116 -21 Kanauchi et al. J Gastroenterol. 2002 Nov; 37 Suppl 14: 67 -72

Nutritional supplements n Butyrate (SCFA) n n Butyrate enemas n Benefit in UC (pilot study) n Did not reach statistical significance in RCT Plantago ovata seeds n Open label randomized trial (105 pts) n Mesalamine 500 TID vs. fiber 10 gm BID n Increased fecal butyrate in fiber group n No difference @ 1 year n Relapse 40% in fiber n Relapse 35% in mesalamine Scheppach et al. Gastroenterology. 1992 Jul; 103(1): 51 -6 Fernández-Bañares et al. Am J Gastroenterol. 1999 Feb; 94(2): 427 -33

Nutritional supplements n Defined diets- No data n Specific Carbohydrate Diet n “Breaking the Viscious Cycle” n Maker’s diet n “juicing” diets
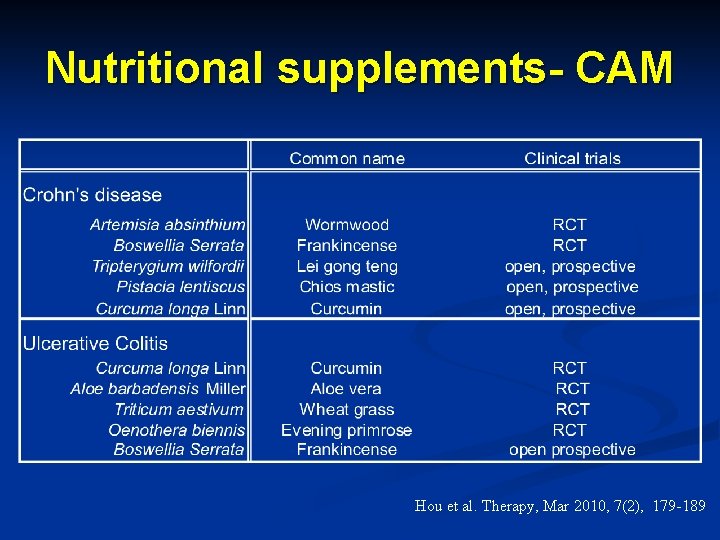

Nutritional supplements- CAM Hou et al. Therapy, Mar 2010, 7(2), 179 -189

Ongoing research BCM

BCM Food aversion study n Hypothesis: Food aversion in IBD is common. n Food aversion in IBD may be related to several factors n n Physician n Patient directed education n Patient symptom correlation

BCM Food aversion study n Primary aim: To define the frequency and character of dietary alterations that occur in patients with IBD n Secondary aims: Identify the reason IBD patients initiate dietary modifications n Identify if IBD patients feel dietary modifications are effective n

Methods n Prospective, controlled data acquisition n 100 IBD patients n 50 CD n 50 UC n 100 healthy controls n Non-IBS n Matched for age, sex

BCM Food aversion study n Goals Establish food aversion patterns in IBD n Identify etiology of food aversion patterns in IBD n Create pilot data for further studies regarding dietary habits and IBD n n Establish if unnecessary food aversion result in nutritional deficiency n Apply educational tools to correct nutritional deficiencies

Conclusions n Diet as Etiology n n Nutritional deficiencies n n Fatty acids composition may play a role in pathogenesis Protein-calorie malnutrition becoming less common, but Micronutrient deficiencies common Diet as Therapy n Fiber, enteral therapy, CAM

Thank you for listening Special thanks to Drs. Hashem El-Serag, Joseph Sellin, and Selvi Thirumuthi
- Slides: 43