Diastolic Heart Failure Carmen B Gomez MD Eugene

Diastolic Heart Failure Carmen B. Gomez MD Eugene Yevstratov MD “The very essence of cardiovascular medicine is recognition of early heart failure. ” Sir Thomas Lewis 1933

Introduction Diastolic heart failure has emerged over the last 10 years as a separate clinical entity. Diastolic heart failure accounts for approximately one third of all heart failure cases, especially in an elderly population, and its natural history, with an annual mortality rate of 8%, is more benign than other forms of heart failure with an annual mortality of 19%. A need has therefore grown to establish precise criteria for the iagnosis of diastolic heart failure.

Requirments for Diagnostic of the DHF u Presence of sighs or symptoms of congestive heart failure u Presence of normal or only midly abnormal left ventricular systolic function u Evidence of abnormal left ventricular relaxation(filling, diastolic
Pathophysiology u. Impaired relaxation u. Increase passive stiffness u. Endocardial and pericardial disordersw u. Microvascular flow. Myocardial turgor u. Neurohormonal regulation
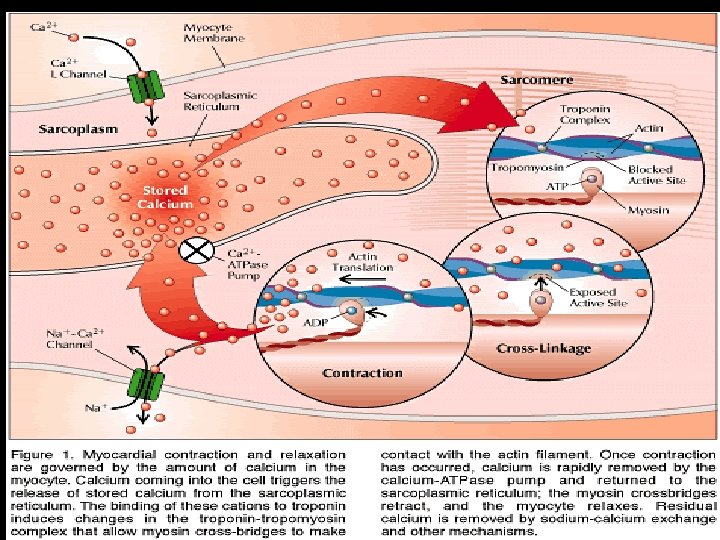
Pathophysiology Impaired Relaxation u. Epicardial or microvascular ischemia u. Myocite hypertrophy u. Cardiomyopathies u. Aging u. Hypothyroidism
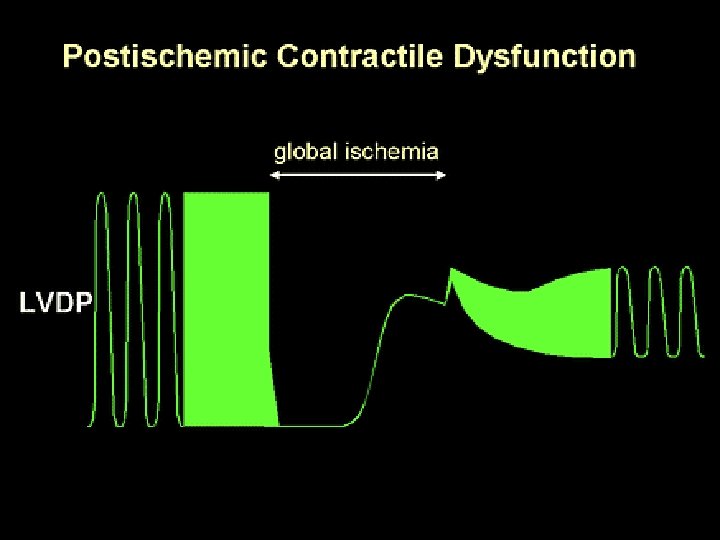
Pathophysiology Increase Passive Stiffness Diffuse fibrosis u Post-infarct scarring u Myocyte hypertrophy u Infiltrative (amyloidosis, hemochromatosis, Fabry´s disease) u
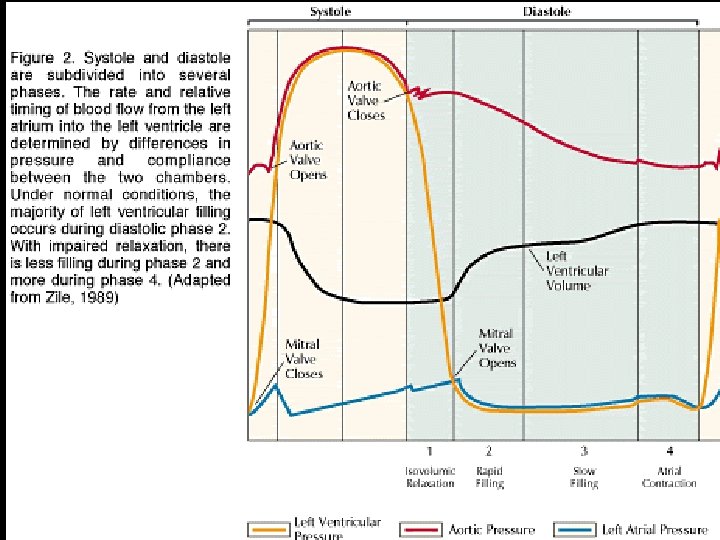

Pathophysiology Endocadial, Pericardial Disorders Fibroelastosis u Mitral or tricuspid stenosis u Pericardial constriction u Pericardial tamponade u
Pathophysiology Endocadial, Pericardial Disorders

Pathophysiology Microvascular Flow, Myocardial Turgor Capillary compression u Venouse engorgement u
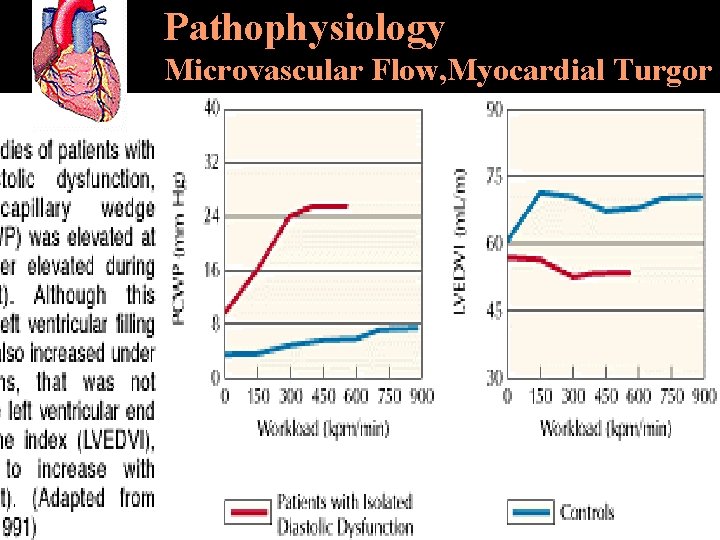
Pathophysiology Microvascular Flow, Myocardial Turgor
Pathophysiology Neurohormonal Regulation, Other Upregulated reninangiotensin system u Volume overload of the contralatetal ventricle u Extrinsic compression by tumor u
Diagnosis Increased ventricular filling pressure with normal systolic function. u Incresed ventricular pressure with preserved systolic function and normal ventricular volumes. u Increased left atrial and pulmonary capillary wedge pressure. u

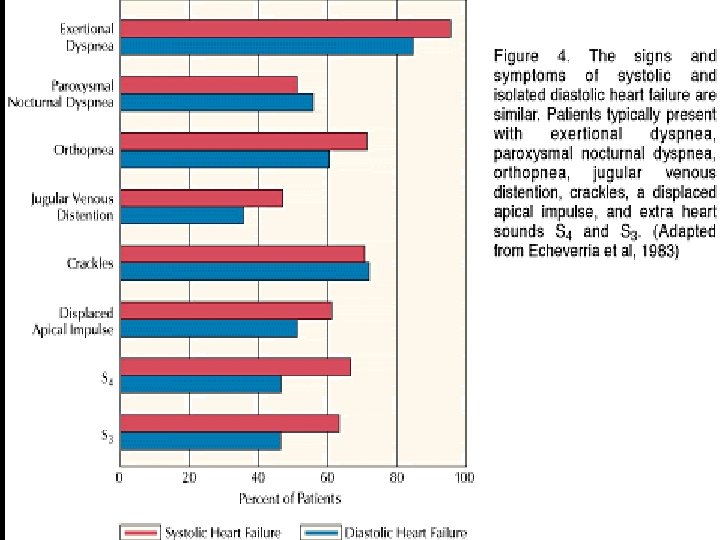
Clinical Signs and Symptoms Evidence of raised left atrial pressure u Exertional dyspnoea u Orthopnoea u Gallop sounds u Lung crepitations u Pulmonary oedema u Exercise intolerance u
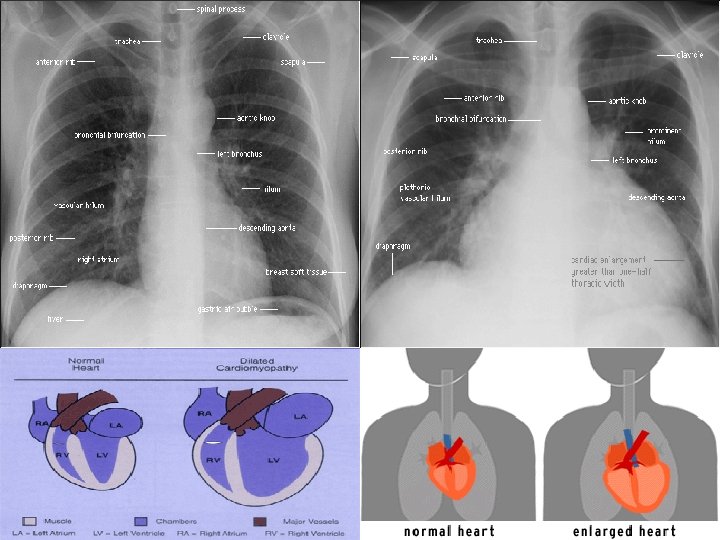
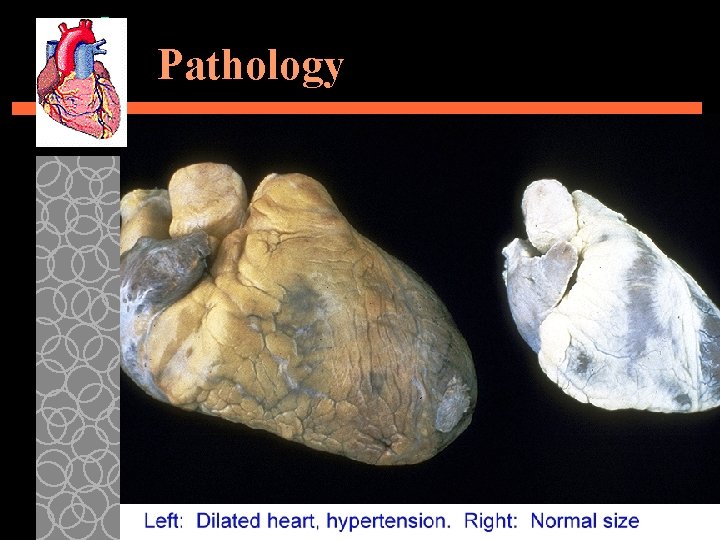
Pathology
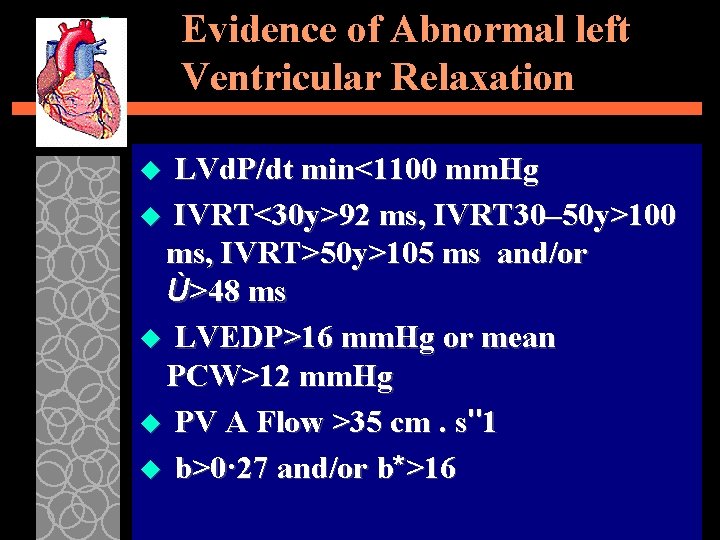
Evidence of Abnormal left Ventricular Relaxation LVd. P/dt min<1100 mm. Hg u IVRT<30 y>92 ms, IVRT 30– 50 y>100 ms, IVRT>50 y>105 ms and/or Ù>48 ms u LVEDP>16 mm. Hg or mean PCW>12 mm. Hg u PV A Flow >35 cm. s"1 u b>0· 27 and/or b*>16 u

Management of DHF Reduce symptoms u Control hypertension u Prevent myocardial ischemia u There is no specific therapy for DHF
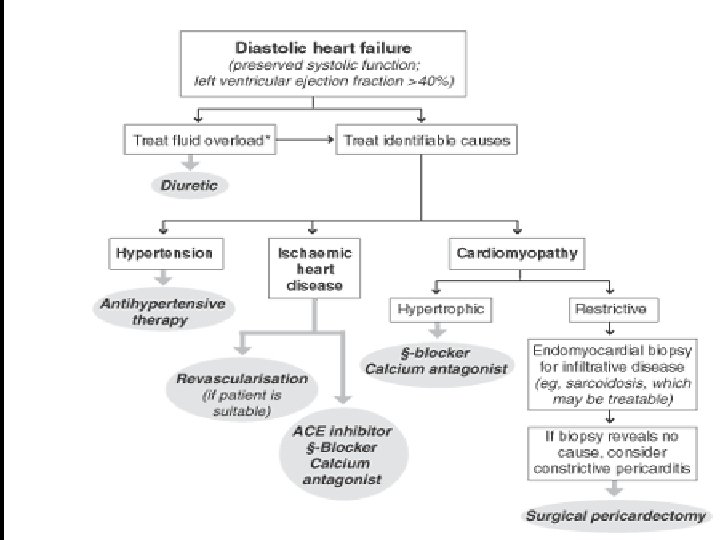

Management of DHF u Diuretics – provide the most symptoms relief if fluid retentionn is a future ACE inhibitors and β Blockers – complement diuretics well u Central sympatholytics – u hypertensive episodes Nitrates – preventing ischemia u Trimetazidine – as a metabolic u support

Conclusion Until further evidence is available from randomized therapeutic trials, clinicians should focus on a few general principles in the treatment of DHF: Reduce volume overload Slow the heart rate Control hypertension, Relieve myocardial ischemia.

http: //myprofile. cos. com/eugenefox FUNDACION FAVALORO INSTITUTO DE CARDIOLOGIA Y CIRUGIA CARDIOVASCULAR Carmen B. Gomez MD Eugene Yevstratov MD
- Slides: 25