Dialectical Behavior Therapy An Adapted Approach Cindi Crew

Dialectical Behavior Therapy: An Adapted Approach Cindi Crew, LISW-S Director of Integrated Counseling Greater Cincinnati Behavioral Health Services

Dialectical Behavior Therapy • DBT was founded by Marsha Linehan, Ph. D. at the University of Washington in Seattle • It is an innovative method of treatment that was originally developed for treating Borderline Personality Disorder (BPD) • It is designed for the severe and chronic multi-diagnostic, difficult to treat client • It is a cognitive behavioral approach that combines therapeutic validation and acceptance of the person along with cognitive behavioral change strategies • It blends a matter-of-fact attitude about suicidal and other dysfunctional behaviors with therapists warmth, flexibility, responsiveness to client, and strategic selfdisclosure

Validation • Validation is: • A core DBT strategy to address the consequences of biological dysfunction interacting with an invalidating system • Finding the kernel of truth or wisdom in the client’s behavior • Seeing the world from the client's point of view, and saying so • Validation does not mean you have to: • Agree with the client • Approve of the behavior

How to Validate • • Stay Awake: Unbiased listening Accurately reflect back what was said Accurately reflect back what was not said Find how the behavior makes sense in the light of the individual’s history or biology • Find how the behavior makes sense in the light of normal functioning and current context • Radical genuineness: Be Yourself!

5 functions in DBT • Improve client skills • Increase motivation for change • Generalize skills to all relevant environments • Structure therapeutic environment to promote effectiveness • Enhance therapists capabilities and motivation to treat effectively

Why DBT for ID? • Empirically Based treatment • 7 -31% of individuals in the community with ID suffer from a personality disorder (2007, DM-ID, Fletcher) • Individuals with ID suffer abuse and neglect at rates 4 -10 times greater than the general population, further complicating personality development • People with ID have been difficult to treat, DBT offers treatment structure for difficult to treat populations • Delays in development of personality may lead to frustration and acting-out behaviors

• Addresses problems related to emotional, interpersonal, behavioral, cognitive and self dysregulation • Addresses skills deficits in Mindfulness, Emotion Regulation, Interpersonal Regulation, and Distress Tolerance • Expanded to other treatment populations (eating disorders, depression, substance abuse, sex offenders, bi-polar disorder) • Optimistic treatment for both clients and therapists • Preserves the morale of therapists

Standard Modes of DBT • • Weekly Individual Therapy Weekly Skills Group Telephone Consultation Weekly Therapist Consultation Meeting

Connection’s Adapted DBT Criteria Inclusions: • The individual has a co-occurring (or suspected) mental health and developmental disability diagnosis. • The individual exhibits symptoms of emotion dysregulation. • The individual has an established provider or family member that assists the individual with care coordination and is willing to participate in skills groups. • The individual has the ability to communicate in some form and at minimum level of moderate ID • The individual has agreed to make a commitment of at least 6 months of treatment. • The individual is at least 18 years of age or older. • The individual has active Medicaid. Exclusions: • The individual has a diagnosis of a primary psychotic disorder • The individual has a diagnosis of a primary substance abuse disorder

Individual Therapy Adaption's • • Shortened sessions to 45 minutes Diary card simplified Re-teaching the skills from the week Use of more sensory based activities

DBT DIARY CARD Name/Case#: Date: Target Behavior: _____________________________ Skill to Practice: ______________________________ Check a box when you practice it □ □ □ □ Rate the emotions you’ve felt today: Mad: Easy Going Furious Sad: Neutral Stressed: Sobbing Terrified Calm Happy: Neutral Thrilled Today, I had a hard time with: _____________________________________________________________

DBT DIARY CARD NAME: WEEK: GOAL I AM WORKING ON THIS WEEK: SKILL I AM PRACTICING: DATE: HOW DID I FEEL? WHAT SKILLS DID I USE? DID THEY WORK?

Skills Training Adaption's • The skills book was modified to simplify language and pictures were added to help explain concepts • Family and/or providers attend the skills groups with the individual • Use of concrete and sensory- based experiential learning was added • Additional time allotted for practicing skills in group

• The skills group facilitator is a Connection’s therapist and the co-leader is a DDS staff member • Providers or family members attend skills classes with clients – 5 -7 clients per group • Training is offered for provider agencies of clients attending DBT

MINDFULNESS HANDOUT 1 Taking Hold of Your Mind: Reasonable Mind Wise Mind States of Mind Emotional Mind

INTERPERSONAL EFFECTIVENESS HANDOUT 11 Making Repairs This skill is about having healthy relationships that last. Part of this skill is being able to make and accept apologies as well as having the ability to let go sometimes. While not an easy process, being able to admit when you’ve made mistakes and were wrong can be very useful. Effectively apologizing will increase trust and safety. Being able to effectively accept apologies is useful in relationships because it is respectful and compassionate. Occasionally, letting things go enhances relationships by allowing you to be in the present without bringing in baggage from the past.
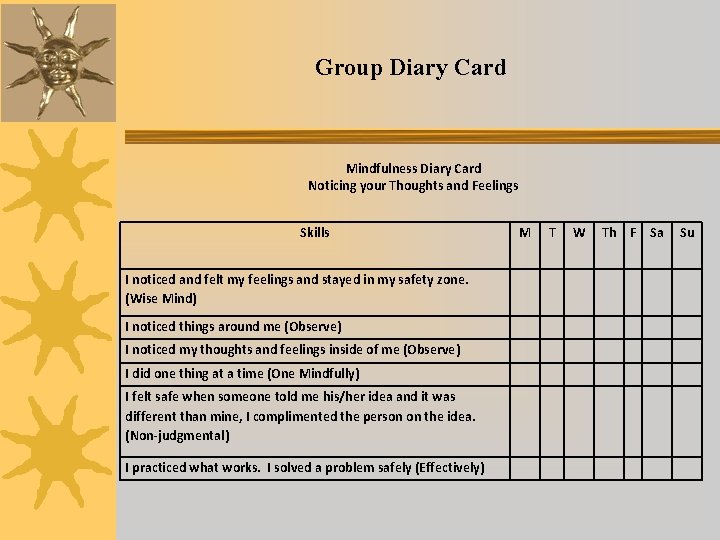
Group Diary Card Mindfulness Diary Card Noticing your Thoughts and Feelings Skills I noticed and felt my feelings and stayed in my safety zone. (Wise Mind) I noticed things around me (Observe) I noticed my thoughts and feelings inside of me (Observe) I did one thing at a time (One Mindfully) I felt safe when someone told me his/her idea and it was different than mine, I complimented the person on the idea. (Non-judgmental) I practiced what works. I solved a problem safely (Effectively) M T W Th F Sa Su

Telephone Consultation • Offered by therapist between sessions to the client and the provider • After hours contact • Each therapist set their own limits for the time of contact and the purpose of contact • Telephone contact is not for the purpose of extra therapy, but to give the client help and support in applying the skills that are being learned in skills group to real life situations, between sessions and to help find ways of avoiding self-injury and/or other targeted behaviors

Team Consultation • Weekly group supervision • Team consists of: Individual therapist, Group skills leader, co-leader, DDS Liaison • Therapist should receive DBT from each other on a regular basis…this keeps things in a DBT mode • These meetings help to avoid burn out, help us respect our limits, and allow us to share ideas

Outcomes • Mindfulness-Based Self Efficacy Scale-Revised • This client rated questionnaire that measures the change in levels of perceived self-efficacy before and after mindfulness-based therapy programs. • It has sub scores that measures emotion regulation, distress tolerance, equanimity, taking responsibility, social skills, and interpersonal effectiveness. • We added data collection by self report of hospitalizations and incident reports
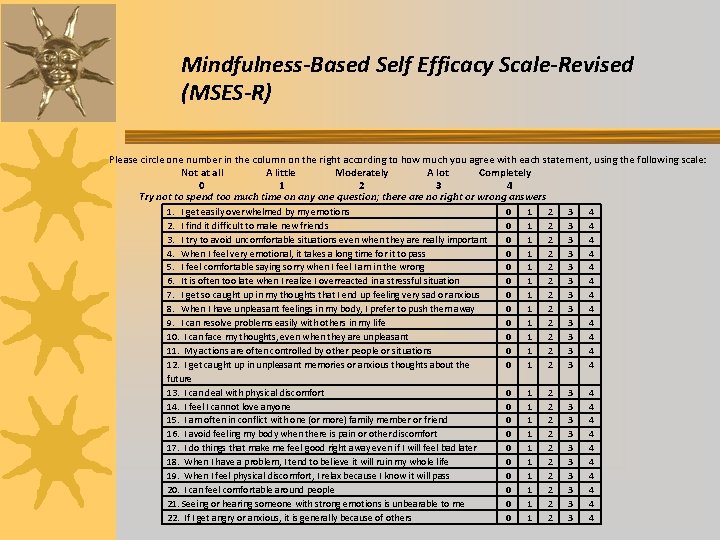
Mindfulness-Based Self Efficacy Scale-Revised (MSES-R) Please circle one number in the column on the right according to how much you agree with each statement, using the following scale: Not at all A little Moderately A lot Completely 0 1 2 3 4 Try not to spend too much time on any one question; there are no right or wrong answers 1. I get easily overwhelmed by my emotions 2. I find it difficult to make new friends 3. I try to avoid uncomfortable situations even when they are really important 4. When I feel very emotional, it takes a long time for it to pass 5. I feel comfortable saying sorry when I feel I am in the wrong 6. It is often too late when I realize I overreacted in a stressful situation 7. I get so caught up in my thoughts that I end up feeling very sad or anxious 8. When I have unpleasant feelings in my body, I prefer to push them away 9. I can resolve problems easily with others in my life 10. I can face my thoughts, even when they are unpleasant 11. My actions are often controlled by other people or situations 12. I get caught up in unpleasant memories or anxious thoughts about the future 13. I can deal with physical discomfort 14. I feel I cannot love anyone 15. I am often in conflict with one (or more) family member or friend 16. I avoid feeling my body when there is pain or other discomfort 17. I do things that make me feel good right away even if I will feel bad later 18. When I have a problem, I tend to believe it will ruin my whole life 19. When I feel physical discomfort, I relax because I know it will pass 20. I can feel comfortable around people 21. Seeing or hearing someone with strong emotions is unbearable to me 22. If I get angry or anxious, it is generally because of others 0 0 0 1 1 1 2 2 2 3 3 3 4 4 4 0 0 0 0 0 1 1 1 1 1 2 2 2 2 2 3 3 3 3 3 4 4 4 4 4

Matt’s Scores
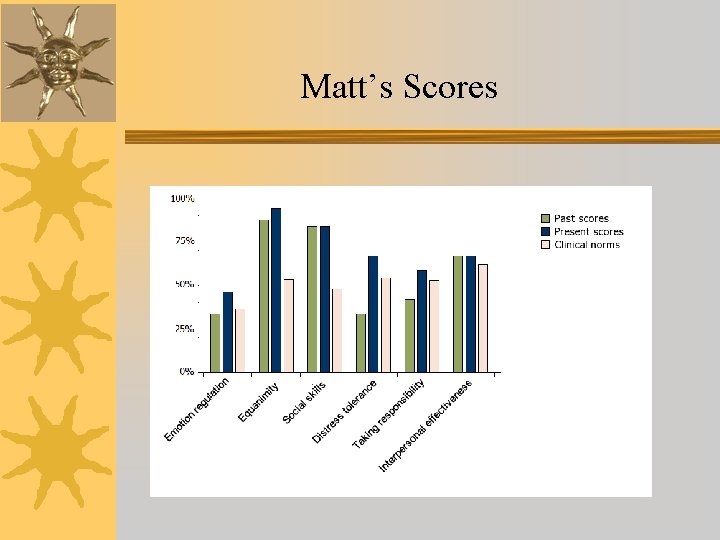
Matt’s Scores

Current Outcomes Data • • 8 graduates in FY 15 80% increase in overall MSES-R scores 90% decrease in incident reports 100% decrease in psychiatric hospitalizations

- Slides: 25