Diagnostic Laboratory Blood Tests Complete Blood Count and

Diagnostic Laboratory Blood Tests Complete Blood Count and Blood Chemistry Profiles

Blood Counts

Complete Blood Count n Evaluations of cellular parameters n Types of cells n Numbers of cells n Size and volume of cells

CBC n Provides a “snap shot “ of the hematopoietic system at a specific point in time.

CBC Components n n n White blood cell count n Mean corpuscular volume Differential count n Mean corpuscular Red blood cell count hemoglobin Hematocrit n Mean corpuscular Hemoglobin hemoglobin concentration

White Blood Count (WBC) n White blood cells (leukocytes) are the disease fighting cells of the immune system. n Only about 1% of blood cells are WBCs n Large numbers of WBCs can be produced rapidly if needed

White Blood Count (WBC) The WBC tells the total number of white cells present in a specified volume of blood n Different disease states affect the WBC in different ways n

WBC Methods n Hemocytometer n Automated cell counters n Quantitative Buffy Coat Analysis

Manual Hemocytometer n Manual counting is the oldest and most time consuming method of determining cell counts n Special slides and diluting fluids are required n Method can be used for counting cells in other body fluids and effusions

Advantages of Manual Counts n Manual counting is the least expensive in terms of equipment and supplies n Can be performed in a mobile clinic

Limitations of Manual Counts n Time consuming (staff expense) n Inherent staff n Requires error (20%), even with skilled well trained and meticulous personnel

Manual Counts n WBC count is the most frequently performed hemocytometer count n RBC counts are very inaccurate n Meticulous attention to detail is necessary to achieve consistent cell count results when using manual methods
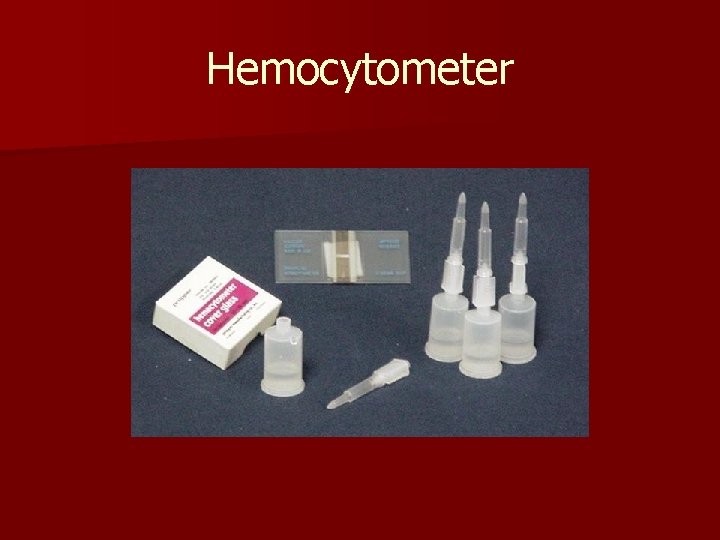
Hemocytometer



Automated Cell Counter n Several types now available for use in vet settings n All types are more accurate than manual methods n Results are obtained rapidly

Types n Semi-automated requires some sample preparation by technical staff n Fully automated performs all steps itself

Automated Cell Counter

Impedance methods n All make use of Coulter principle


Advantages n Faster and more effective use of staff time n Newer models store calibrations for multiple species n Can perform most of components of a complete blood count

Limitations n Cannot perform differential counts n Cannot recognize reticulocytes n Cannot reliably differentiate between WBCs and nucleated RBCs n Several artifacts can create false counts

Quantitative Buffy Coat Analysis n QBC is based on differential centrifugation n Uses special tubes that contain a float that has the same density as the buffy coat n When spun under high speed, the buffy coat components are separated out by density (weight) n Automated reader scans buffy coat and records percentages of aggregates


Advantages of QBC Analysis n Efficient and economical method n Simple to operate n Good for rapid screening in office n The system flags abnormal or unexpected results

Limitations of QBC Analysis n Cannot produce a complete differential count n Cannot distinguish between lymphocytes and monocytes n Does not distinguish between segs and bands

Increased WBCs n Bacterial infections generally increase the numbers of white cells present n Pyometra n Bacterial pneumonia n Peritonitis

Decreased WBCs n Viral infections tend to reduce numbers of WBCs n Parvovirus n Canine Distemper n Feline panleukopenia

Decreased WBCs n Immune system inadequacy n Bone marrow disease n Overwhelming bacterial infection

Differential Counts n Important in order to interpret the WBC results n Gives much of the information needed to interpret WBCs n To date, no machine is able to perform this task adequately and completely

Red Blood Cell Count n The measurement of RBCs is a way of evaluating the blood’s ability to deliver oxygen to tissues and to carry carbon dioxide away n Changes in the morphology of RBCs can give information about bone marrow function n Some infectious agents or parasites may be seen on the RBC surface

Hematocrit n Measures the percentage of RBCs in the total blood n Can give information about the animal’s state of hydration n May show evidence of RBC destruction in the spleen

Hemoglobin n Hemoglobin is the oxygen carrying protein in the RBC n Low levels of Hgb indicate genetic problems, inadequate iron, inadequate B vitamins n High levels of Hgb may indicate abnormalities such as high iron intake, a toxin, or internal organ malfunction

Mean Corpuscular Volume n MCV n Measures the size of the RBCs

Mean Corpuscular Hemoglobin n MCH n Reflects the average weight of the hemoglobin in the RBCs

Mean Corpuscular Hemoglobin concentration n MCHC n Measures the amount of hemoglobin in a given volume of packed red cells

Blood Chemistry

Blood Chemistry Values n Blood chemistry panels measure a variety of substances dissolved in the plasma of blood § Nutrients § Carrying agents § Catalysts § Waste matter

Blood Chemistry n Substances are present in minute amounts n Each substance contributes to the overall health of the patient n Increases or decreases of chemicals can be good indicators of the patient’s condition n Can give valuable aid in making a diagnosis



Aspartate Aminotransferase n AST n Formerly called serum glutamic oxaloacetic transaminase (SGOT) n Enzyme n Levels increase with liver or severe muscle injury

Alanine Aminotransferase n ALT n Formerly known as serum glutamic pyruvate transaminase n Enzyme n Levels increase in general liver injury

Total Bilirubin n. T Bili n Measures the total amount of all bilirubin in the serum n Bilirubin is a pigment released in the destruction of RBCs n Increased levels: § Intravascular hemolysis § Primary liver or bile duct disease

Direct Bilirubin n. D Bili n Conjugated bilirubin n Bilirubin that has been combined with other compounds by the liver n Increases levels often associated with primary liver disease

Indirect Bilirubin n. I Bili n Unconjugated bilirubin n Bilirubin that has not yet been combined with other substances n Increased levels usually associated with abnormal hemolysis

Alkaline Phosphatase n Alk Phos n Enzyme n Related to bone, liver, bile duct system n Increased levels: § Young, growing animals § Bone disease § Liver disease § Bile duct blockage § Steroids and anticonvulsants

Total Protein n. T Prot or TP n Measure both albumin and globulin n Gives very general information n Further division of proteins needed for meaningful interpretation

Albumin ALB n Decreases: § Reduced production by n Major plasma protein liver n Transports substances § Malnutrition § Chronic liver disease throughout body § Kidney disease n Increases: § Tissue fluid loss from n § Dehydration § Tissue fluid loss from wounds, burns

Globulin n GLOB n Blood protein n Antibodies n Indicator of immune function

Cholesterol n Chol n Increases due to § Liver disease § Diet § Thyroid disease § Genetic abnormalities

Blood Urea Nitrogen n BUN n Associated with kidney function n Levels increase with: § Dehydration § High dietary protein § Small Bowel hemorrhage § Kidney disease

Creatinine n Creat n Breakdown metabolism product of skeletal muscle – Creatinine is filtered out by the kidneys – Used with BUN to determine kidney function § Not influenced by diet or GI bleeding

Phosphorus n Phos n Mineral n Levels are regulated by the kidneys n Linked with calcium , vitamin D, parathormone n Increased in young, growing animals n Increases occur with aging kidneys and kidney failure

Calcium n Ca+ n Mineral n Important for skeletal strength n Needed for nervous system function n Regulated by parathyroid glands n Linked to Vit D, calcitonin, and others

Glucose n Gluc n Essential source of energy for all cells n Reacts to: § Insulin levels § Diet § Glucagon § Liver function

Glucose increases n Hyperglycemia n After eating n Stress n Exercise n Acute pancreatitis n Some drugs

Glucose decreases n Hypoglycemia n Malnutrition n Parasitism n Increased insulin § Administration of overdose § insulin producing tumor

Amylase n Pancreatic enzyme n Levels increase in § Acute pancreatitis § Kidney disease

Lipase n Pancreatic enzyme n Levels increase in § Acute pancreatitis § Kidney disease

Sodium n Na+ n Major blood electrolyte n Filtered by renal glomerulus, reabsorbed by renal tubules

Sodium n Increased levels: – – Dehydration Increased salt intake Diabetes insipidus Kidney failure n Decreased levels: – Vomiting and Diarrhea (can lead to metabolic acidosis) – CHF – Adrenal malfunction (Addison’s disease) – Diabetes mellitus

Chloride n CHL n An electrolyte that balances sodium and potassium n Increased levels indicate changes in overall electrolyte balance

Potassium n K+ n Levels linked to Na+ n Controlled by hormone aldosterone

Potassium Hyperkalemia n Increases: n – – – Very serious Kidney failure Adrenal malfunction Hypoklalemia n Decreases: n – – Decreased intake Excessive loss Vomiting, diarrhea Kidney disease

Creatine Kinase n CK § Formerly called creatine phosphokinase, or CPK n Associated with skeletal muscle or heart muscle damage n Increases with: § Myositis § Trauma § Heart damage

Uric Acid n Blood uric acid reflects the end product of purine metabolism n Increases in: § General liver disease § Genetic abnormalities in metabolism (Dalmatians)

T 3 n Triiodothyronine n Three iodine atoms attached to thyroxine n Thyroid hormone n Regulates metabolism of all body cells

T 3 n Increase – Hyperthyroidism due to increased thyroid gland activity – Tumors – Rare in dogs – Common in cats n Decrease – In cases of reduced thyroid function – In any generalized illness – Very low if animal is gravely ill

T 4 n Tetraiodothyronine (4 iodine molecules) n Converted to T 3 by the liver n Free T 4 (FT 4) less than 0. 1 percent of all T 4, not bound to protein § When measured accurately, most predictive of true thyroxine concentrations
T 4 n Increase – Tumors – Thyroid gland hyperplasia n Decrease – Reduced thyroid gland function
- Slides: 71