Diagnosis of Microbial Infection Patient Clinical diagnosis Nonmicrobiological

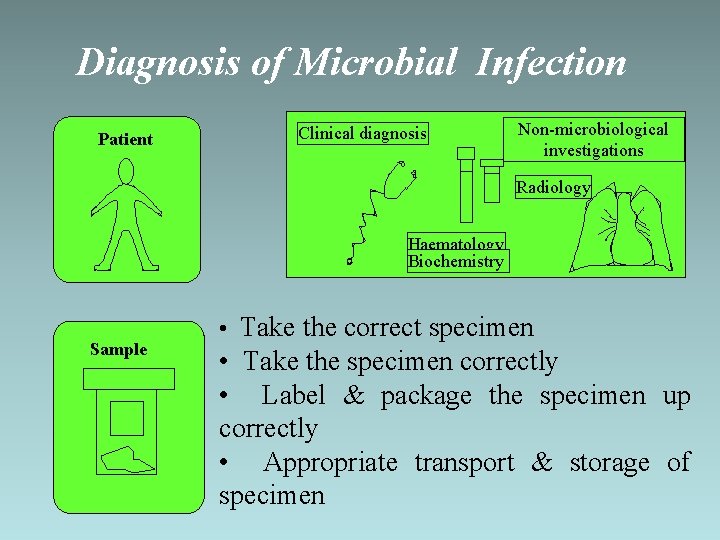
Diagnosis of Microbial Infection Patient Clinical diagnosis Non-microbiological investigations Radiology Haematology Biochemistry Sample • Take the correct specimen • Take the specimen correctly • Label & package the specimen up correctly • Appropriate transport & storage of specimen

Specimen processing • • Receiving Recording Culturing Staining Isolation Identification Sensitivity test

Getting the specimen to the lab • Problems in delay or inappropriate storage. • Delay in diagnosis & treatment lead to: üPathogens die. üContaminants overgrow. • Blood cultures directly into incubator not refrigerator!? ? • CSF straight to lab. • Don't put an entire surgical specimen into formalin !? ? But: Send a portion to microbiology in a sterile container.

Collecting the specimen correctly • Take an mid-stream urine to: ü avoids contamination with normal flora. • Blood cultures ü Avoid contamination with skin organisms • CSF ü Avoid contamination. ü Avoid bloody tap. • Throat swab ü Make the patient gag!

Patient Details • • Name and age Hospital number Sex, for female: if she pregnant or lactating Address Presenting signs/symptoms Suspected diagnosis Travel history? ? Immunization

Identification of specimens • • Patient details. Type of specimen. Collection date and time. Laboratory number. Test requested. Name of ordering physician. Note: ALL specimens must be properly labeled with the patient's full name, date and time of collection, and specimen source.

Normal microbiota • All body surfaces possess a rich normal bacterial flora, especially the mouth, nose and skin. • This can be a nuisance – disturbance- in that üIt can contaminate specimens. üIt can cause disease. • This is beneficial in that üIt can protect against infection by preventing pathogens colonising epithelial surfaces (colonisation resistance). NOT: Removal of the normal flora with antibiotics can cause super infection, usually with resistant microbes.

Microbiota and humans Disease can come about in several overlapping ways 1. Some bacteria are entirely adapted to the pathogenic way of life in humans. They are never part of the normal flora but may cause subclinical infection, e. g. M. Tuberculosis. 2. Some bacteria which are part of the normal flora acquire extra virulence factors making them pathogenic, e. g. E. coli. 3. Some bacteria which are part of the normal flora can cause disease if they gain access to deep tissues by trauma, surgery, lines, e. g. S. epidermidis. 4. In immunocompromised patients many free-living bacteria and components of the normal flora can cause disease, especially if introduced into deep tissues, e. g. Acinetobacter.

Specimens & Infection Control • Please be considerate to lab staff!! üLabel hazardous specimens • Don't send specimens to the lab without proper packing. üLeaking or blood-stained specimens are not acceptable!!!

Factors limiting usefulness of bacteriological investigations • • Wrong sample for example saliva mixed with sputum. Delay in transport / inappropriate storage e. g. CSF. Overgrowth by contaminants e. g. blood cultures. Insufficient sample / sampling error e. g. in mycobacterial diseases. • Patient has received antibiotics.

Specimen rejection criteria • • Mismatch information Improper container or temperature Insufficient specimen Leaking specimen Formalin specimen Dried out swap Late specimen Physician must be informed about rejection
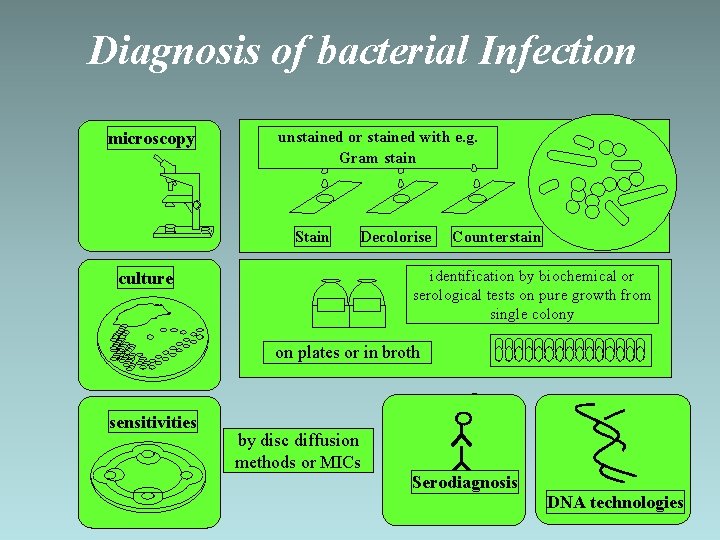
Diagnosis of bacterial Infection microscopy unstained or stained with e. g. Gram stain Stain Decolorise Counterstain identification by biochemical or serological tests on pure growth from single colony culture on plates or in broth sensitivities by disc diffusion methods or MICs Serodiagnosis DNA technologies
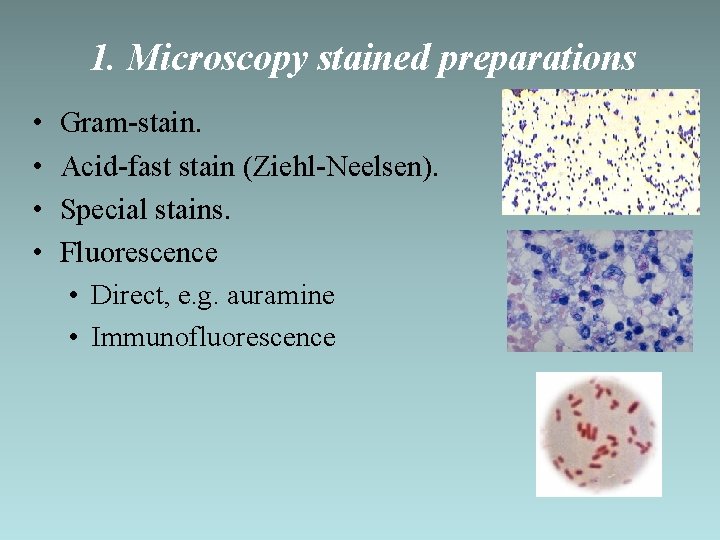
1. Microscopy stained preparations • • Gram-stain. Acid-fast stain (Ziehl-Neelsen). Special stains. Fluorescence • Direct, e. g. auramine • Immunofluorescence
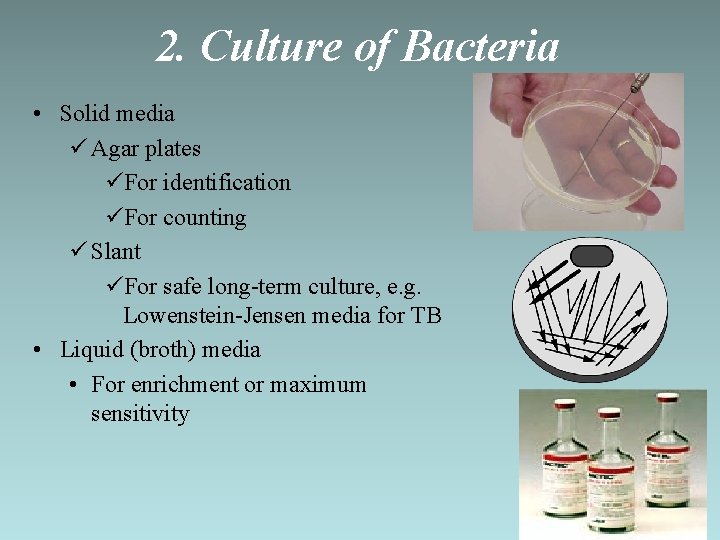
2. Culture of Bacteria • Solid media ü Agar plates üFor identification üFor counting ü Slant üFor safe long-term culture, e. g. Lowenstein-Jensen media for TB • Liquid (broth) media • For enrichment or maximum sensitivity

Culture characteristics • • • Shape Margin Optical properties Elevation Color Odor Animation
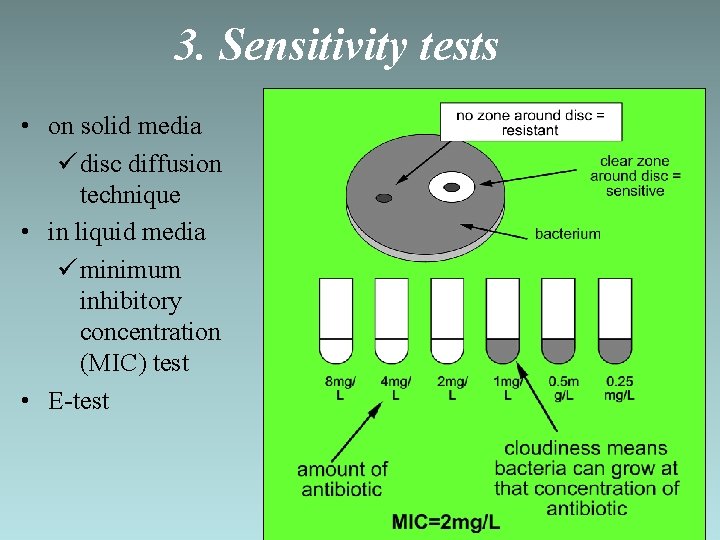
3. Sensitivity tests • on solid media ü disc diffusion technique • in liquid media ü minimum inhibitory concentration (MIC) test • E-test

4. Serology tests • Antigen detection ü e. g. latex agglutination • Antibody detection ü e. g. agglutination tests, complement fixation tests, indirect immunofluorescence 5. Molecular methods ü Polymerase Chain Reaction (PCR)

Diagnosis of Viral Infection • Electron microscopy • Serology: Antigen detection or antibody detection • Virus culture • Molecular methods üPolymerase Chain Reaction üSequencing (e. g. for sensitivities)

How do we know that a given pathogen causes a specific disease? • Koch's postulates ü The pathogen must be present in every case of the disease. ü The pathogen must be isolated from the diseased host & grown in pure culture. ü The specific disease must be reproduced when a pure culture of the pathogen is inoculated into a healthy susceptible host. ü The pathogen must be recoverable from the experimentally infected host. • Exceptions? ?

Report of bacteriology result • CSF, body fluid, blood, and wound: üpositive gram stain üCulture and isolation üIdentification • Ear: üPotential pathogens; S. aureus, G –ve • Eye: üReport identification of any organism

Report of bacteriology result • Gastrointestinal: ü Stool culture for Salmonella, shigella, campylobacter, Vibrio, and E. coli O 157: H 7 ü Negative culture will be reported as “No enteric pathogens isolated” • Lower respiratory and sputum: ü Report identification of any organism

• Nasal / nasopharyngeal: üReport identification of any Gram –ve rod, S. aureus, S. pneumonia, H. influenza, N. meningitides, group A streptococci. • Skin: üPredominant organism • Throat: ü group A streptococci, Sensitivity test

• Urine: üReport identification and antimicrobial sensitivity on colony count greater than 10. 000 CFU üMixed flora of less than 10. 000 will be reported as normal skin flora. • Vaginal / cervical: üReport predominant organisms üMixed culture of lactobacillus, diptheroids, staphylococcus, alpha streptococcus, and yeast will be reported as normal vaginal flora.


- Slides: 27