Diagnosis and Treatment of Acute Otitis Media Authors



















- Slides: 21

Diagnosis and Treatment of Acute Otitis Media Author(s): Anna Dolgner, MD Level: Basic Academic Affiliation : Duke University School of Medicine Version No: 1. 2 Submitted: March 2012 Editors’ Review: April 2013

2 Disclaimer/Liability • The information provided in the VAP is made available in good faith and is derived from sources believed to be reliable and accurate at the time of release. • The materials presented on the VAP may include links to external Internet sites. These external information sources are outside the control of Duke-NUS. The user of the Internet links is responsible for making his or her own decision about the accuracy, reliability and correctness of the information found. • In no event shall Duke-NUS be liable for any indirect, special, incidental, or consequential damages arising out of any use of reliance of any information contained in the VAP. Nor does Duke-NUS assume any responsibility for failure or delay in updating or removing the information contained in the VAP. • Moreover, information provided on the VAP does not constitute medical advice or treatment nor should it be considered as a replacement of the patient/physician relationship or a physician’s professional judgment. Duke-NUS expressly disclaims all liability for treatment, diagnosis, decisions and actions taken or not taken in reliance upon information contained in the VAP. This work is licensed under a Creative Commons Attribution-Non. Commercial-No. Derivs 3. 0 Unported License To view a copy of this license, visit [http: //creativecommons. org/licenses/by-nc-nd/3. 0/]

3 Financial Disclosures (past 3 years) • No Disclosures

4 Learning Objectives • Learn the symptoms of AOM • Be able to diagnose AOM by exam • Understand treatment and antibiotic choices

5 Outline • Epidemiology • Pathophysiology • Microbiology • Signs and Symptoms • Treatment

6 Epidemiology of AOM • Most commonly occurs ages 6 -18 months – 60 -80% of pts have AOM by 1 year – 80 -90% of pts have AOM by 3 years • Most common reason for antibiotic use in children • Responsible for 16 million office visits in 2000 – About 80% of these visits led to antibiotic prescription • Risk factors include daycare, lack of breastfeeding, tobacco smoke exposure, being member of indigenous (American Indian) population, and + FH

7 Pathophysiology • Definition: Presence of fluid in inner ear associated with signs of illness and middle ear inflammation • Antecedent URI+colonization by pathogenic bacteria inflammation of Eustachian tubes, blocking isthmus secretions accumulate microbial migration and growth AOM

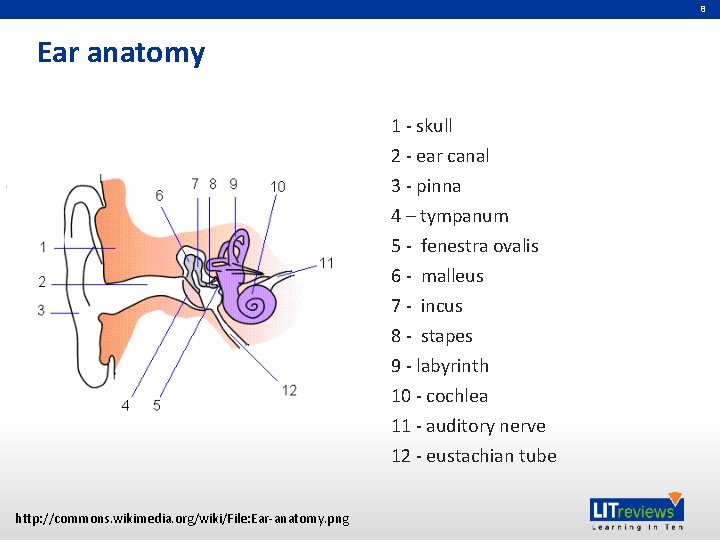
8 Ear anatomy 1 - skull 2 - ear canal 3 - pinna 4 – tympanum 5 - fenestra ovalis 6 - malleus 7 - incus 8 - stapes 9 - labyrinth 10 - cochlea 11 - auditory nerve 12 - eustachian tube http: //commons. wikimedia. org/wiki/File: Ear-anatomy. png

9 Microbiology • Bacteria: the big 3 – Streptococcus pneumoniae (~50%) – Moraxella catarrhalis (~20%) – non-typeable Haemophilus influenzae (~30%) • Special considerations – ~100% Moraxella and ~50% Haemophilus colonies are betalactamase + – 50% S. pneumoniae isolates moderately or highly PCNresistant via PCN-binding proteins

10 Signs and Symptoms • Fever, otalgia, irritability, otorrhea – Fever present in 30 -60% of patients Rare to be >40 degrees C – Otalgia present in about 80% of patients • Can also have non-specific symptoms such as headache, nausea, vomiting, diarrhea • Antecedent/concurrent URI symptoms present in many patients

11 Physical Examination-suggestive findings • Middle ear effusion – Fullness/bulging of TM Best indicator – Reduced/absent TM mobility on insufflation • Erythematous or cloudy TM • Bullae on TM • Pus behind TM • TM perforation

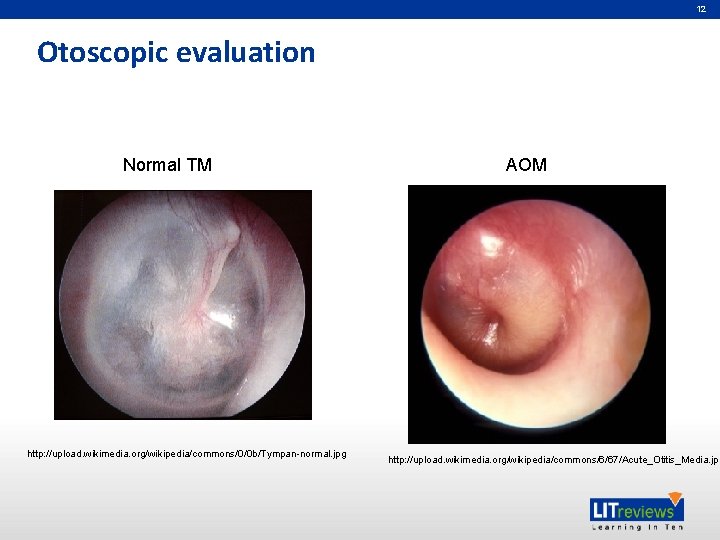
12 Otoscopic evaluation Normal TM http: //upload. wikimedia. org/wikipedia/commons/0/0 b/Tympan-normal. jpg AOM http: //upload. wikimedia. org/wikipedia/commons/6/67/Acute_Otitis_Media. jpg

13 Treatment-symptomatic • Treat fever – acetaminophen or ibuprofen • Treat otalgia – acetaminophen or ibuprofen – Intra-otic therapy Antipyrine-benzocaine (Auralgan) drops

14 Antibiotics-who to treat? • Immediate therapy – <6 months if diagnosis suspected or certain – 6 -24 months if diagnosis certain – Felt to be “severely ill” • Delayed therapy (48 -72 h symptomatic tx) – 6 -24 months if diagnosis uncertain and not “severely ill” and otherwise healthy child – >24 months if diagnosis uncertain or not “severely ill” and otherwise healthy child

15 Antibiotics-preferred • Amoxicillin – First-line for uncomplicated AOM – 80 -90 mg/kg/d to overcome penicillin binding proteins • Amoxicillin-clavulanate – If systemically ill (temp >39 C, severe otalgia) – If suspect beta-lactamase producing organism – 80 -90 mg/kg/d of amoxicillin component to overcome penicillin binding proteins

16 Antibiotics-other considerations If pt PCN-allergic • If mild allergy – 2 nd or 3 rd generation cephalosporin Cefdinir, cefpodoxime, cefuroxime, single dose IM ceftriaxone • If severe allergy (type I) – Macrolides Azithromycin, clarithromycin, erythromycin-sulfisoxazole – Clindamycin – TMP-SMX (less preferred)

17 Duration of Antimicrobial Therapy • Standard duration is 10 days – Except azithromycin (5 days) • Reasonable to consider 5 -7 day course in children >6 with mild to moderate AOM

18 Antibiotic Failure If symptoms do not resolve in 48 -72 hours, suspect resistant infection • Usually beta-lactamase producing organism, but could be unusual organism • Change medication to amoxicillin-clavulanate or aforementioned cephalosporins

19 Summary • Most common ages 6 -18 months • Fever, otalgia, otorrhea +/- concurrent URI are common • See erythematous, bulging TM +/- purulence on exam • Antibiotics can be delayed in lower risk groups – >24 months – 6 -24 months if diagnosis uncertain and child clinically well • Antibiotic choices should target S. pneumo, M. catarrhalis, and H. influenzae and consider illness severity and resistance mechanisms – Common choices are high dose amoxicillin or amoxicillin-clavulanate, 2 nd -3 rd generation cephalosporins, and macrolides

20 Key References • AAP Practice Guideline: Diagnosis and Management of Acute Otitis Media. Pediatrics Vol. 113 No. 5 May 1, 2004 pp. 1451 -1465 • http: //commons. wikimedia. org/wiki/File: Ear-anatomy. png • Klein JO et al. Acute otitis media in children: Epidemiology, microbiology, clinical manifestations, and complications. Up. To. Date Online. Accessed 3/17/12. • Wald ER. Acute otitis media in children: Diagnosis. Up. To. Date Online. Accessed 3/17/12. • http: //upload. wikimedia. org/wikipedia/commons/6/67/Acute_Otitis_Media. jpg • http: //upload. wikimedia. org/wikipedia/commons/0/0 b/Tympan-normal. jpg

Partners in Academic Medicine