Diagnosing and Managing Ocular Emergencies and Urgencies Blair

Diagnosing and Managing Ocular Emergencies and Urgencies Blair Lonsberry, MS, OD, MEd. , FAAO Diplomate, American Board of Optometry Clinic Director and Professor of Optometry Pacific University College of Optometry blonsberry@pacificu. edu 1

Disclosures and Special Request Paid consultant for: – Alcon Pharmaceuticals, Bausch and Lomb, Carl Zeiss Meditec, Ni. Cox, Sucampo Special Request: Interactive remotes don’t work on your TV, so please don’t take them home! Commitment to change: - write down three things that you “learned” from this presentation that you can incorporate into your practice to improve patient care

What Classifies an Emergency? • Any condition in which the patient has the potential for: – vision loss, – currently experiencing vision loss, – permanent structural damage, – pain or discomfort, – or is an “emergency” for the patient. • It is important to be able to triage a walk-in patient and, more importantly, a call-in patient.
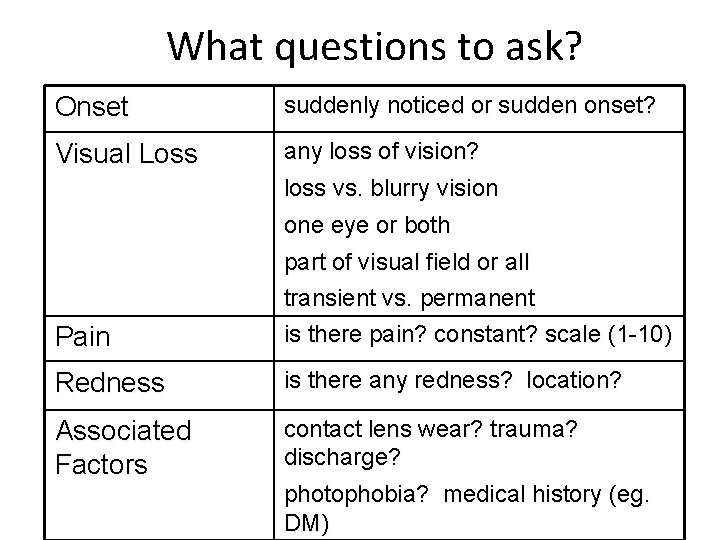
What questions to ask? Onset suddenly noticed or sudden onset? Visual Loss any loss of vision? loss vs. blurry vision one eye or both part of visual field or all Pain transient vs. permanent is there pain? constant? scale (1 -10) Redness is there any redness? location? Associated Factors contact lens wear? trauma? discharge? photophobia? medical history (eg. DM)

Common Types of Ocular Emergencies • Vision Loss: – Gradual vs. sudden onset – Vision loss with or without pain • Trauma • Red eyes

Visual Loss • Visual loss varies greatly in meaning from patient to patient – ranging from blur to complete blindness and may affect one or both eyes • Components include: – acuity, – visual field, – color and brightness may be affected jointly or separately • Detailed history and extent of vision loss crucial

Profound Loss of Vision • Referring to a complete or greatly diminished vision affecting the whole field • Common causes of severe vision loss: Vascular central retinal vein occlusion, central retinal artery occlusion, vitreous heme Inflammatory optic neuritis Infiltrative Mechanical optic neuropathy retinal detachment

Monocular vs. Binocular • Ocular or optic nerve pathology causes monocular vision loss • lesion at or posterior to chiasm causes binocular vision loss – VF defects become more congruous the further back in the visual pathway – Homonymous VF defects noted posterior to chiasm • Difference between mono vs. bino usually straightforward, keeping the following in mind: – Patients occasionally mistake homonymous hemianopsia (similar loss of visual field in both
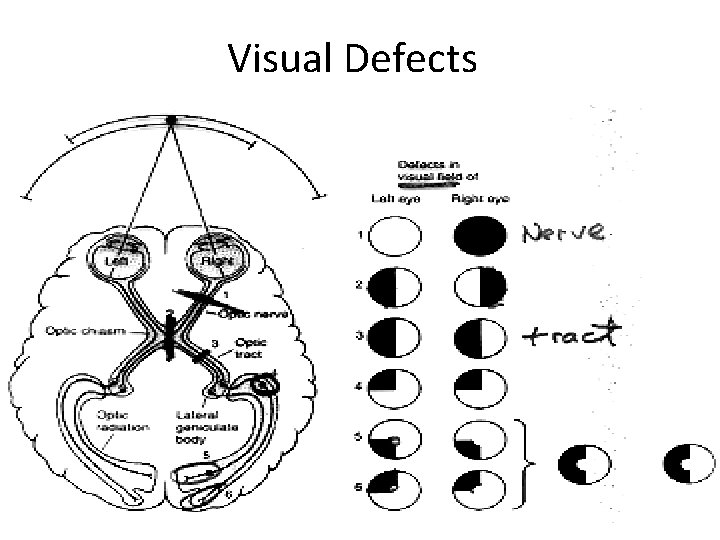
Visual Defects

Monocular • Differentiate between eyes that have lost all useful vision and those that have blurred vision • Blurring of vision is not localized and may be caused by pathology anywhere from cornea to optic nerve • Need to get anatomical diagnosis first before considering the cause

General Appearance • Level of consciousness – When introducing yourself be aware of the patient’s gross level of consciousness? • Is the patient awake, alert and responsive? • Personal Hygiene and Dress – Is it appropriate for the environment, temperature, age and social status of the patient? – Is the patient malodorous or disheveled?

General Appearance • Posture and Motor control – What posture does patient assume while sitting in the exam chair – Are there any signs of involuntary motor activity such as tremors • E. g. damage to the cerebellum may produce a tremor that usually worsens with movement of the affected limb

Case Example • 48 yr old white female presented for diabetic eye exam on referral from her PCP – She was scheduled 2 weeks previously but had fallen and was unable to make that appointment – She reports that her vision in her right eye seems to be getting worse over the past several weeks. – Was diagnosed with diabetes 1. 5 years ago • BS control has been erratic with range between 120 -240 • Last A 1 C: 9. 1

Blood Sugar • Throughout a 24 hour period blood sugar typically maintained between 3. 9 -7. 8 mmol/L (70 -140 mg/d. L) – Diabetes is diagnosed with a fasting BS of > 7. 0 mmol/L (126 mg/d. L) – or an A 1 c value of > 6. 5 • Hypoglycemia is typically defined as plasma glucose 3. 9 mmol/L (70 mg/d. L) or less – patients typically become symptomatic of hypoglycemia at 2. 8 mmol/L (50 mg/d. L) or less • [A 1 c (%) x 1. 59] – 2. 59 = average Blood Glucose (in mmol/L)
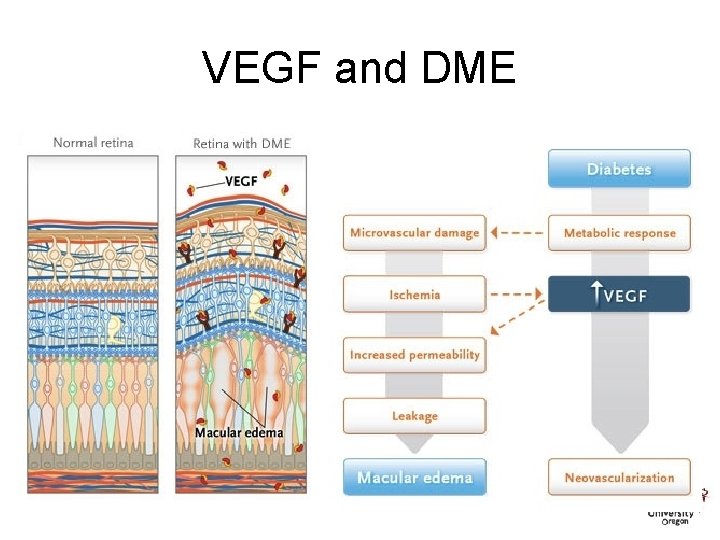
VEGF and DME
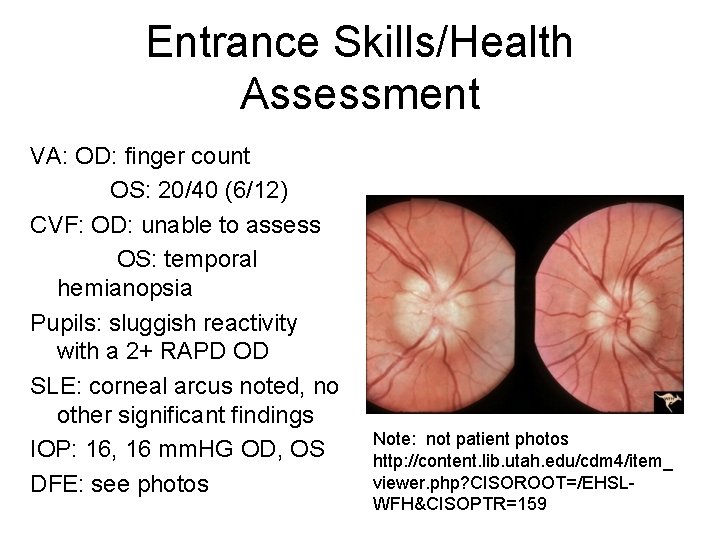
Entrance Skills/Health Assessment VA: OD: finger count OS: 20/40 (6/12) CVF: OD: unable to assess OS: temporal hemianopsia Pupils: sluggish reactivity with a 2+ RAPD OD SLE: corneal arcus noted, no other significant findings IOP: 16, 16 mm. HG OD, OS DFE: see photos Note: not patient photos http: //content. lib. utah. edu/cdm 4/item_ viewer. php? CISOROOT=/EHSLWFH&CISOPTR=159

Physical Presentation • Upon entering the room I noted that her right hand was twitching – I asked her how long that had been going on and she said about 2 -3 weeks – I asked her if she experienced headaches, to which she said she had bad headaches that even woke her up at night

Referral • Contacted her PCP who reported that she had examined the patient 3 weeks prior and had noted any of these findings • Referred the patient for an immediate MRI – wasn’t able to be scheduled until the next day
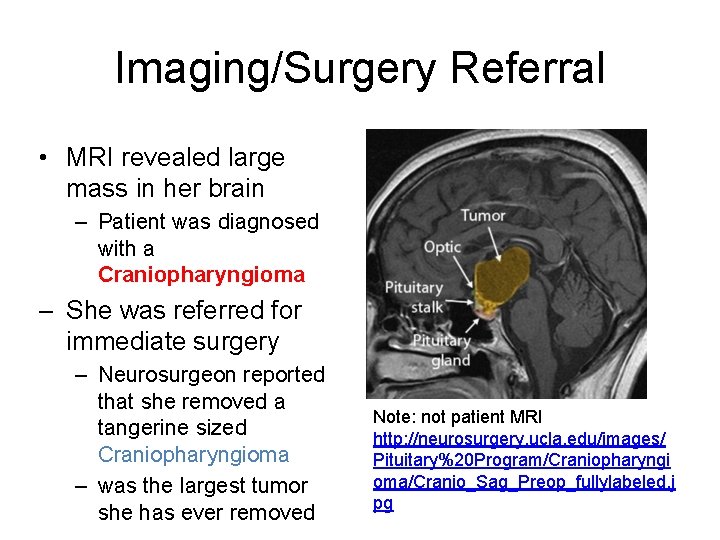
Imaging/Surgery Referral • MRI revealed large mass in her brain – Patient was diagnosed with a Craniopharyngioma – She was referred for immediate surgery – Neurosurgeon reported that she removed a tangerine sized Craniopharyngioma – was the largest tumor she has ever removed Note: not patient MRI http: //neurosurgery. ucla. edu/images/ Pituitary%20 Program/Craniopharyngi oma/Cranio_Sag_Preop_fullylabeled. j pg

Craniopharyngioma • Craniopharyngioma: – slow-growing, – epithelial-squamous origin, – calcified cystic tumor – arises from remnants of the craniopharyngeal duct • Craniopharyngiomas have a benign histology but malignant behavior – they have a tendency to invade surrounding structures and recur after what was thought to be total resection
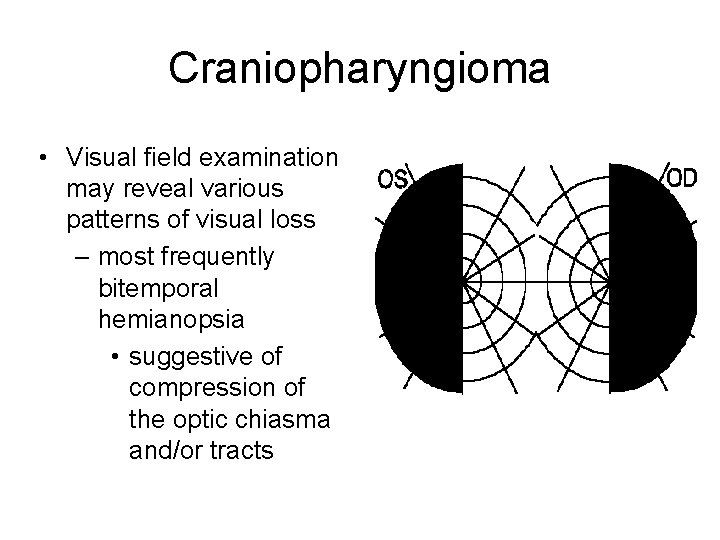
Craniopharyngioma • Visual field examination may reveal various patterns of visual loss – most frequently bitemporal hemianopsia • suggestive of compression of the optic chiasma and/or tracts
Our Patient • Patient had a complete resection of the tumor in addition to radiation therapy • She developed several significant perioperative complications: – Leakage of CSF which resulted in her having to have a shunt • She subsequently developed an infection post surgically – She is NLP in her right eye, but did regain 20/40 vision in her left eye • Retains a temporal hemianopsia OS – Diabetes control became erratic and was put on several hormone replacement medications
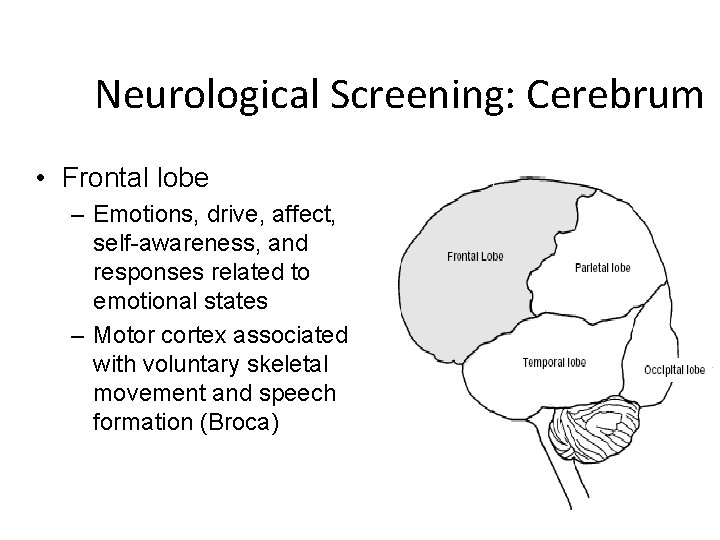
Neurological Screening: Cerebrum • Frontal lobe – Emotions, drive, affect, self-awareness, and responses related to emotional states – Motor cortex associated with voluntary skeletal movement and speech formation (Broca)

Right vs Left Brain Injury • So what happens if one side of the brain is injured? – People who have an injury to the right side of the brain "don't put things together" and fail to process important information. • As a result, they often develop a "denial syndrome" and say "there's nothing wrong with me. “

Right vs Left Brain Injury • The left side of the brain deals more with language and helps to analyze information given to the brain. – If you injure the left side of the brain, you're aware that things aren't working (the right hemisphere is doing its job) but are unable to solve complex problems or do a complex activity. – People with left hemisphere injuries tend to be more depressed, have more organizational problems, and have problems using language.

Gradual Onset: Cataracts • The decreased acuity must correlate with the severity of the cataract… – ie if cataract doesn’t correlate with the amount of vision loss (or afferent pupillary defect present) then you need to find another reason for the vision (or other test results)
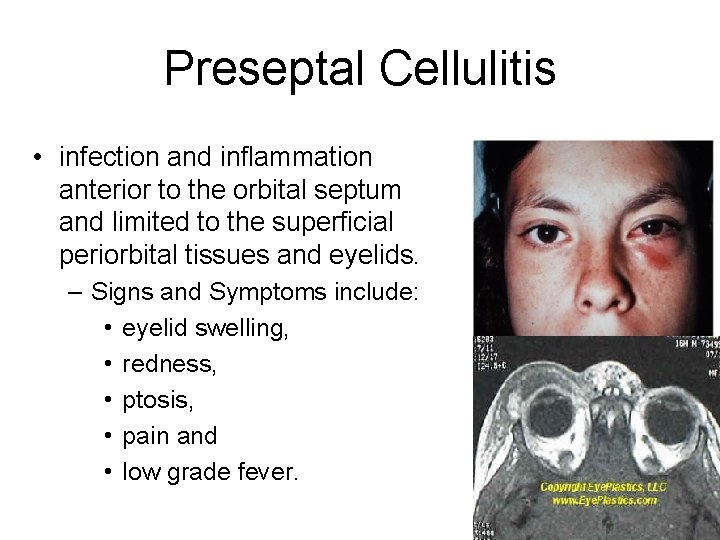
Preseptal Cellulitis • infection and inflammation anterior to the orbital septum and limited to the superficial periorbital tissues and eyelids. – Signs and Symptoms include: • eyelid swelling, • redness, • ptosis, • pain and • low grade fever.
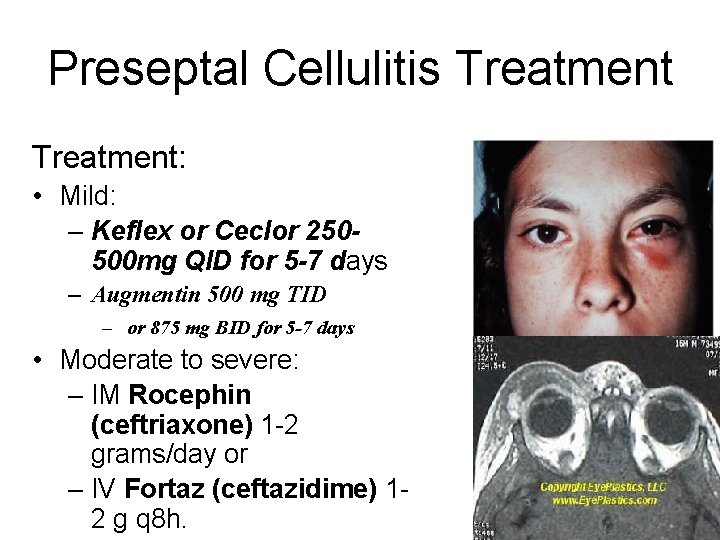
Preseptal Cellulitis Treatment: • Mild: – Keflex or Ceclor 250500 mg QID for 5 -7 days – Augmentin 500 mg TID – or 875 mg BID for 5 -7 days • Moderate to severe: – IM Rocephin (ceftriaxone) 1 -2 grams/day or – IV Fortaz (ceftazidime) 12 g q 8 h.
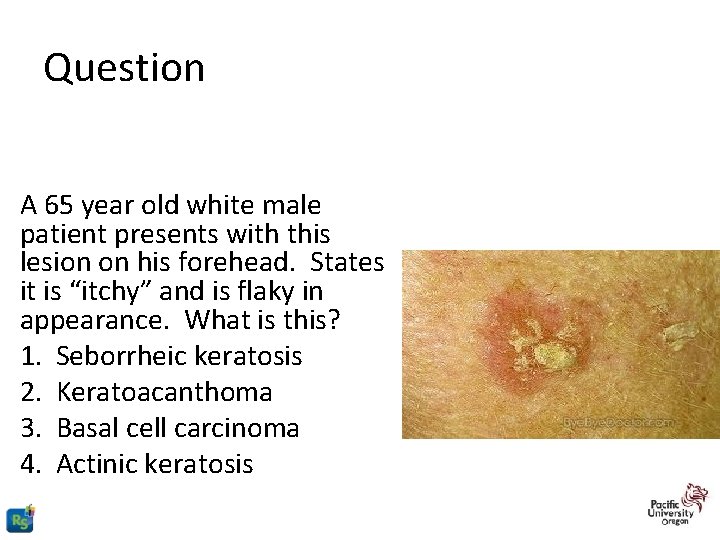
Question A 65 year old white male patient presents with this lesion on his forehead. States it is “itchy” and is flaky in appearance. What is this? 1. Seborrheic keratosis 2. Keratoacanthoma 3. Basal cell carcinoma 4. Actinic keratosis
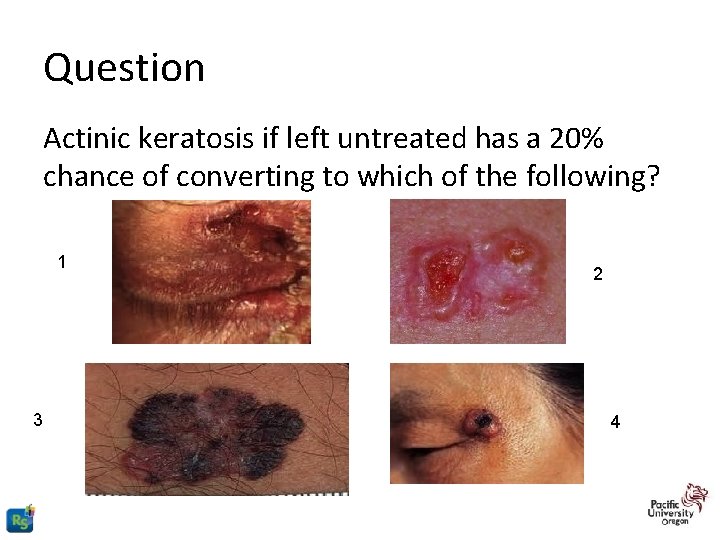
Question Actinic keratosis if left untreated has a 20% chance of converting to which of the following? 1 3 2 4
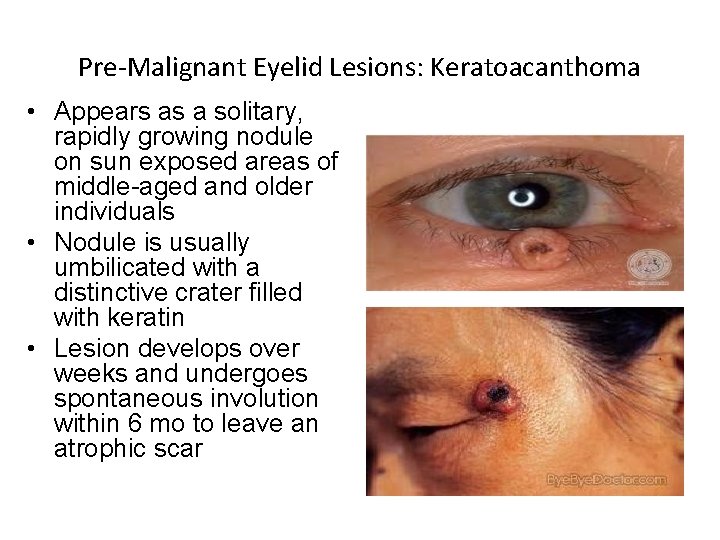
Pre-Malignant Eyelid Lesions: Keratoacanthoma • Appears as a solitary, rapidly growing nodule on sun exposed areas of middle-aged and older individuals • Nodule is usually umbilicated with a distinctive crater filled with keratin • Lesion develops over weeks and undergoes spontaneous involution within 6 mo to leave an atrophic scar
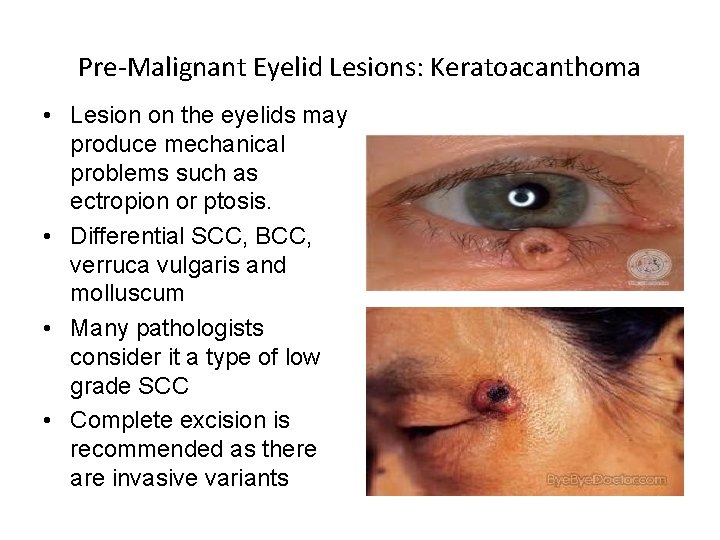
Pre-Malignant Eyelid Lesions: Keratoacanthoma • Lesion on the eyelids may produce mechanical problems such as ectropion or ptosis. • Differential SCC, BCC, verruca vulgaris and molluscum • Many pathologists consider it a type of low grade SCC • Complete excision is recommended as there are invasive variants
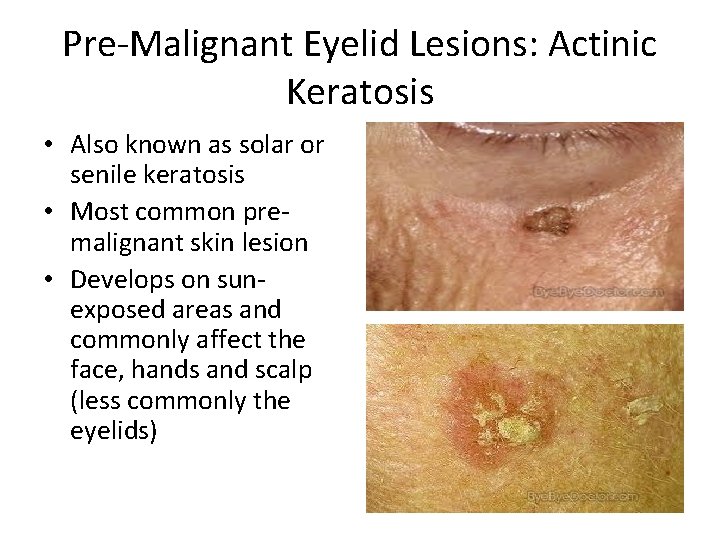
Pre-Malignant Eyelid Lesions: Actinic Keratosis • Also known as solar or senile keratosis • Most common premalignant skin lesion • Develops on sunexposed areas and commonly affect the face, hands and scalp (less commonly the eyelids)
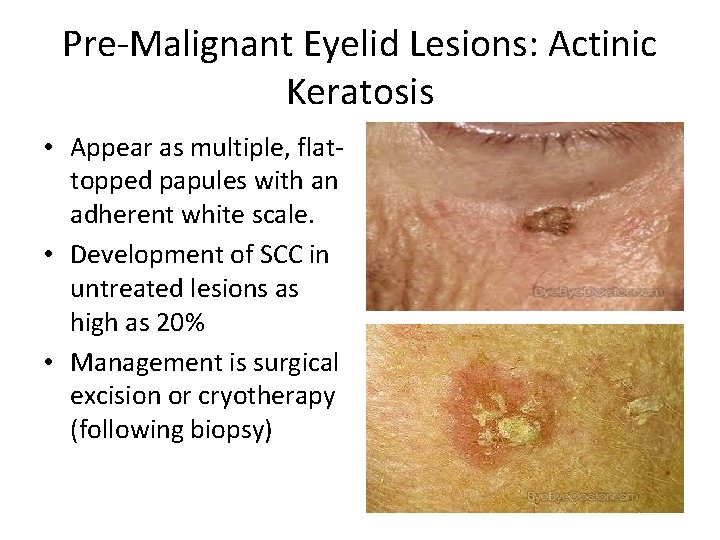
Pre-Malignant Eyelid Lesions: Actinic Keratosis • Appear as multiple, flattopped papules with an adherent white scale. • Development of SCC in untreated lesions as high as 20% • Management is surgical excision or cryotherapy (following biopsy)
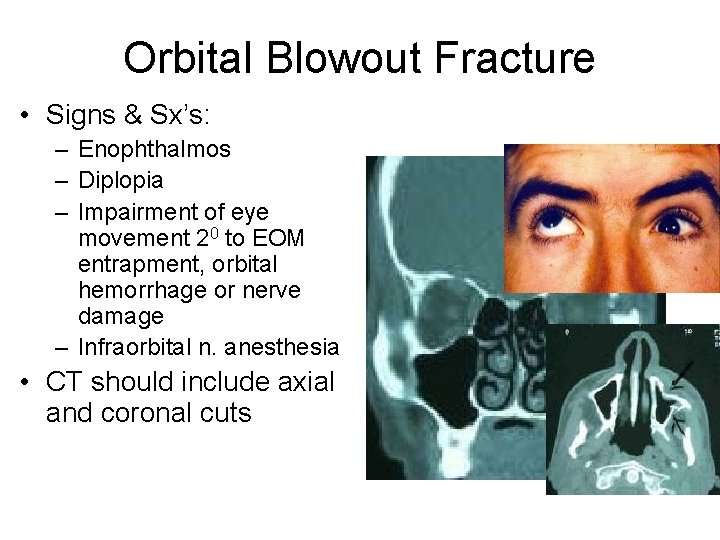
Orbital Blowout Fracture • Signs & Sx’s: – Enophthalmos – Diplopia – Impairment of eye movement 20 to EOM entrapment, orbital hemorrhage or nerve damage – Infraorbital n. anesthesia • CT should include axial and coronal cuts

Orbital blowout fracture Disposition - If no diplopia, minimal displacement, and no muscle entrapment, discharge with follow up within a week. Consider Surgery - For enophthalmos, muscle entrapment, or visual loss. Management: – Ice packs beginning in clinic and for 48 hrs will help decrease swelling associated with injury. – Elevate head of bed (decrease swelling). – If sinuses have been injured, give prophylactic antibiotics and instruct patient not to blow nose. – Treat nausea/vomiting with antiemetics.
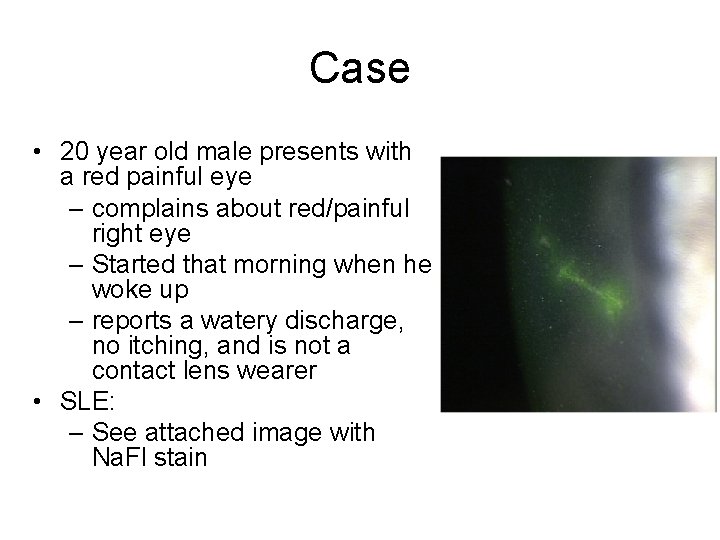
Case • 20 year old male presents with a red painful eye – complains about red/painful right eye – Started that morning when he woke up – reports a watery discharge, no itching, and is not a contact lens wearer • SLE: – See attached image with Na. Fl stain

Herpes Simplex Keratitis: Clinical Features • Characterized by primary outbreak and subsequent reactivation • Primary outbreak is typically mild or subclinical • After primary infection, the virus becomes latent in the trigeminal ganglion or cornea • Stress, UV radiation, and hormonal changes can reactivate the virus • Lesions are common in the immunocompromised (i. e. recent organ transplant or HIV patients)
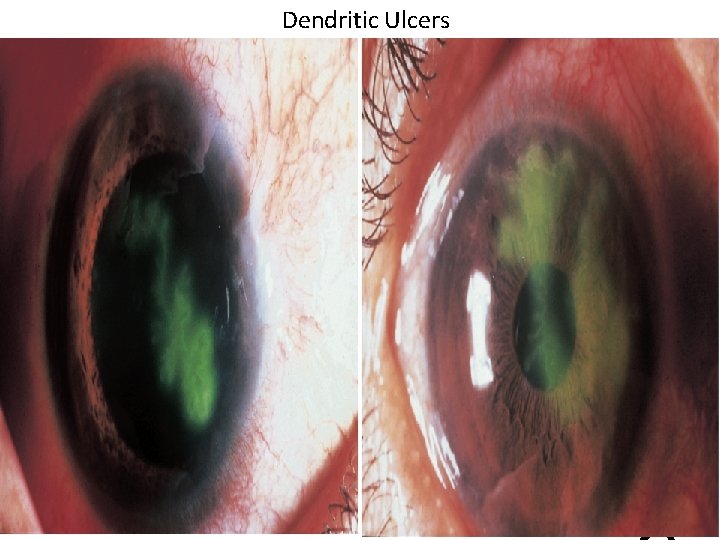
Dendritic Ulcers 3
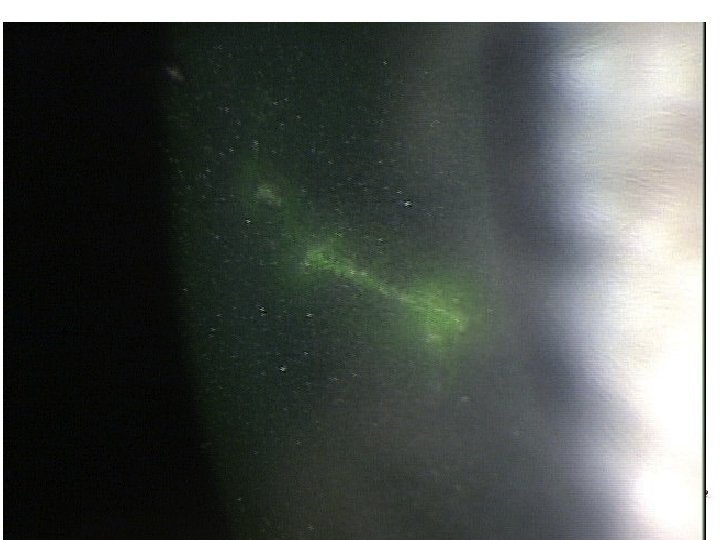


Herpes Simplex Keratitis • Topical: – Viroptic (trifluridine) q 2 h until epi healed then taper down for 10 -14 days. • Viroptic is toxic to the cornea. – Zirgan (ganciclovir) available in USA, use 5 times a day until epi healed then 3 times for a week • Oral acyclovir (2 g/day) has been reported to be as effective as topical antivirals without the toxicity – Valtrex (valcyclovir)) 500 mg TID for 7 -10 days – Famvir (famciclovir) 250 mg TID for 7 -10 days • If stomal keratitis present, after epi defect has healed, add Pred Forte QID until inflammation reduced and then slowly taper

Prophylaxis? ? • Prophylaxis of 400 mg acyclovir BID vs placebo for 1 year resulted in a lower recurrence in the treatment arm (19% vs 32%) – Valtrex 500 mg qd was found to be equivalent to acyclovir BID • Pitfalls to Prophylaxis: – Reduction of recurrence does not persist once drug stopped – Resistance? ? • van Velzen, et. al. , (2013) demonstrated that longterm ACV prophylaxis predisposes to ACV-refractory disease due to the emergence of corneal ACVR HSV-1.

Case • 27 year old pharmacy student presents to the clinic on emergent basis – complains about red/painful eyes for the past 2 days – started OD then transferred to OS – reports a watery discharge, no itching, and is not a contact lens wearer – reports that others in his class have had a similar red eye – no seasonal, food or drug allergies – has taken Visine 4 -5 times/day since eyes became red but hasn’t helped much
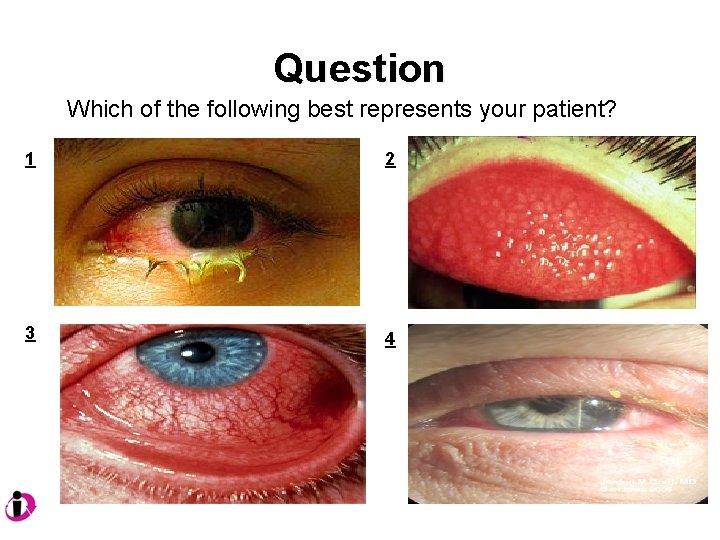
Question Which of the following best represents your patient? 1 2 3 4
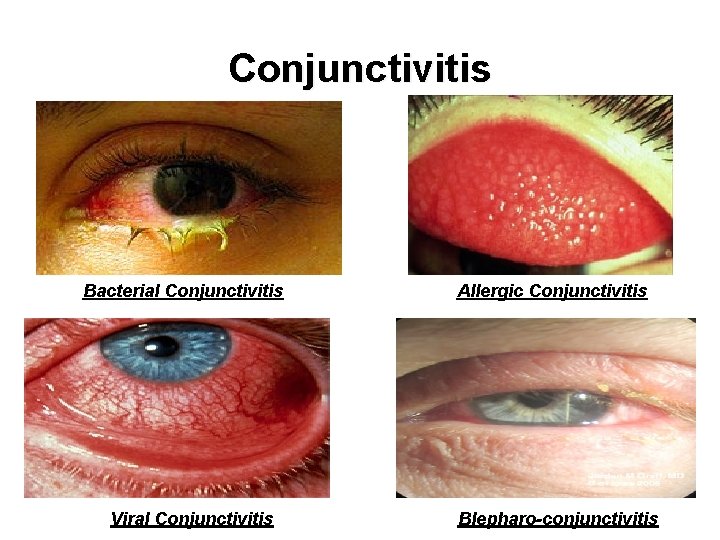
Conjunctivitis Bacterial Conjunctivitis Viral Conjunctivitis Allergic Conjunctivitis Blepharo-conjunctivitis
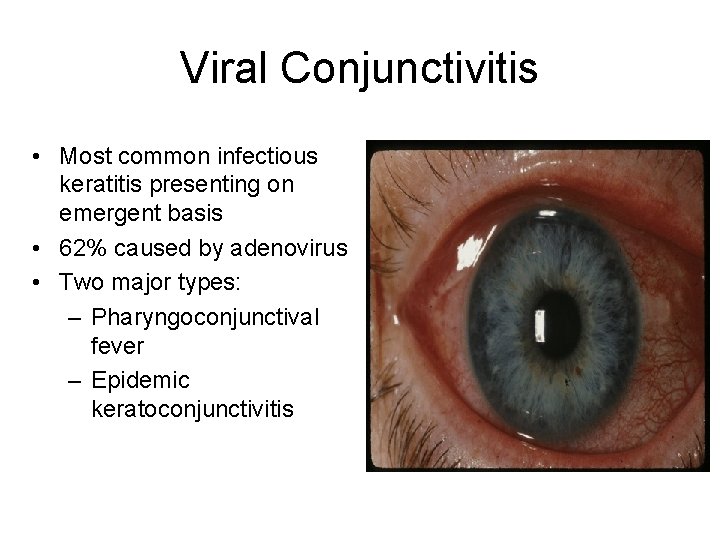
Viral Conjunctivitis • Most common infectious keratitis presenting on emergent basis • 62% caused by adenovirus • Two major types: – Pharyngoconjunctival fever – Epidemic keratoconjunctivitis

Viral Conjunctivitis • PCF: history of recent/current upper respiratory infection • EKC: highly contagious with a history of coming in contact with someone having a red eye. – Adenovirus 8 common variant leading to “rule of 8’s” • First 8 days red eye with fine SPK • Next 8 days deeper focal epithelial lesions • Following 8 potential development of infiltrates • Resolution • RPS Adeno Detector available to use for adenoviral confirmation – Adeno. Plus is currently being marketed and distributed by Ni. Cox

Adeno. Plus • Have you heard about this? www. nicox. com

Interpreting the results NEGATIVE RESULT • Only a BLUE line appears in the control zone. – A negative result is indicative of an absence of Adenovirus Antigens. POSITIVE RESULT • The presence of both a BLUE line in the control zone and a RED line in the result zone indicates a positive result. • Even if the RED line is faint in color, incomplete over the width of the test strip, or uneven in color, it must be interpreted as positive. • A positive result indicates the presence of Adenovirus antigens. www. rpsdetectors. com

Interpreting the results Invalid Result • If a BLUE line does not appear, the test may be invalid. – Reimmerse the absorbent tip into the buffer vial for an additional 10 seconds. – If a BLUE line still does not appear after 10 minutes, the test must be discarded and the subject retested by resampling the eye using a new Adeno. Plus test kit www. rpsdetectors. com
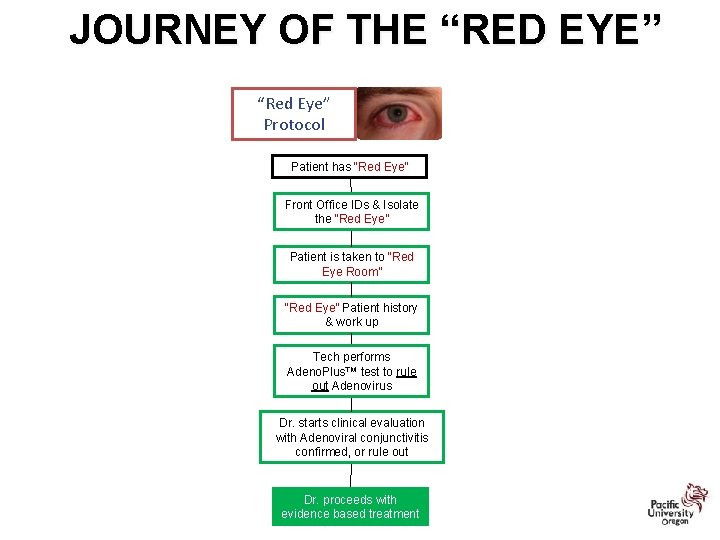
JOURNEY OF THE “RED EYE” “Red Eye” Protocol Patient has “Red Eye” Front Office IDs & Isolate the “Red Eye” Patient is taken to “Red Eye Room” “Red Eye” Patient history & work up Tech performs Adeno. Plus™ test to rule out Adenovirus Dr. starts clinical evaluation with Adenoviral conjunctivitis confirmed, or rule out Dr. proceeds with evidence based treatment
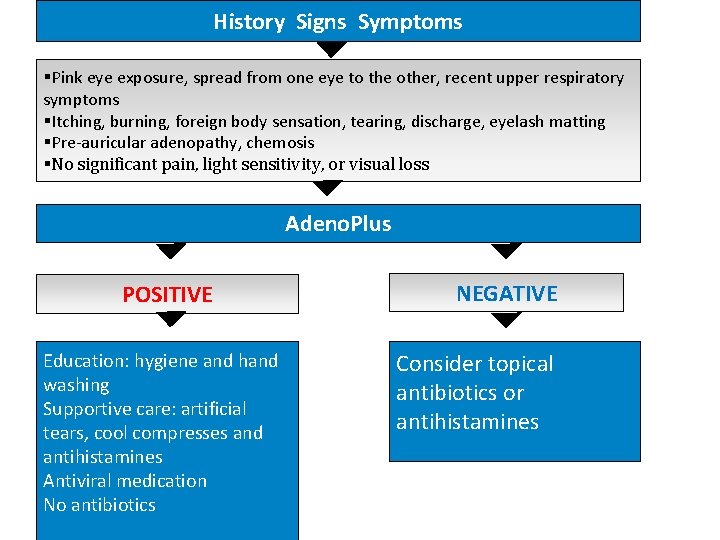
History Signs Symptoms Pink eye exposure, spread from one eye to the other, recent upper respiratory symptoms Itching, burning, foreign body sensation, tearing, discharge, eyelash matting Pre-auricular adenopathy, chemosis No significant pain, light sensitivity, or visual loss Adeno. Plus POSITIVE Education: hygiene and hand washing Supportive care: artificial tears, cool compresses and antihistamines Antiviral medication No antibiotics NEGATIVE Consider topical antibiotics or antihistamines
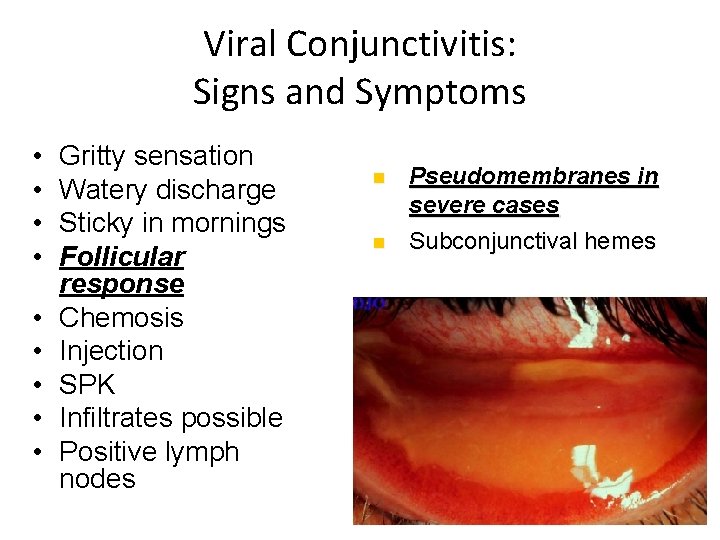
Viral Conjunctivitis: Signs and Symptoms • • • Gritty sensation Watery discharge Sticky in mornings Follicular response Chemosis Injection SPK Infiltrates possible Positive lymph nodes n n Pseudomembranes in severe cases Subconjunctival hemes

Management • Consider the use of anti-inflammatory treatment to relieve patient symptoms and improve comfort – Alrex QID OU – Lotemax QID OU – FML QID OU • EKC patients are typically very uncomfortable and would benefit from anti-inflammatory treatment – especially if infiltrates or pseudomembrane present

Management • Betadine (Melton-Thomas Protocol): – Proparacaine – 4 -5 drops of Betadine 5% • Get patient to close eye and gently roll them around – After one minute, lavage the eye – Lotemax/FML 4 times a day for 4 days • Alternative: Betadine swabsticks. – 5% Betadine solution only comes in 30 ml bottles cost $14. 00. – Case of 200 Betadine swabsticks apprx. 45 dollars.

Management • Antivirals used in HSV keratitis are ineffective in treatment of viral conjunctivitis – New Update: in conversation with several colleagues, Zirgan 4 -5 times/day has shown significant improvement in patients over a 710 time period. • Important to stress limited contact with others, frequent hand washing, not sharing of towels, etc.

Sinusitis Red Eye • With a sinus infection or inflammation – the sinuses swell and mucus cannot properly drain. • The increase in mucus and the narrow passage through which it tries to escape creates pressure in the sinuses that leads to pain. • The sinuses surround the ocular region – pressure from sinuses may feel like eye pressure. – swollen sinuses and nasal membranes can push against ocular nerves resulting in pain. • Pooled mucus can result in infection that increases the pain in the sinus and ocular region even

Sinusitis Treatment • The infection is likely bacterial and should be treated with antibiotics if: – symptoms last for 10 days without improvement, or – include fever of 102 degrees or higher, – nasal discharge and facial pain lasting three to four days • Because of increasing resistance to the antibiotic amoxicillin — the current standard of care — the ISDA recommends Augmentin • Augmentin 250/500 TID for 5 -7 days for adults, 10 -14 days for children – Alternative is Keflex 500 mg QID

Flashes and Floaters • Patients often present complaining of “spots” or “cobwebs” in front of their eyes • Causes of floaters include: posterior vitreous detachment (PVD), retinal tear, vitreous heme, uveitis. • Since PVD and retinal tears present the same way, a RT has to be eliminated • Ask the patient whether spots move with eye and continue to move after the eye has stopped • Large spots could be blood clots
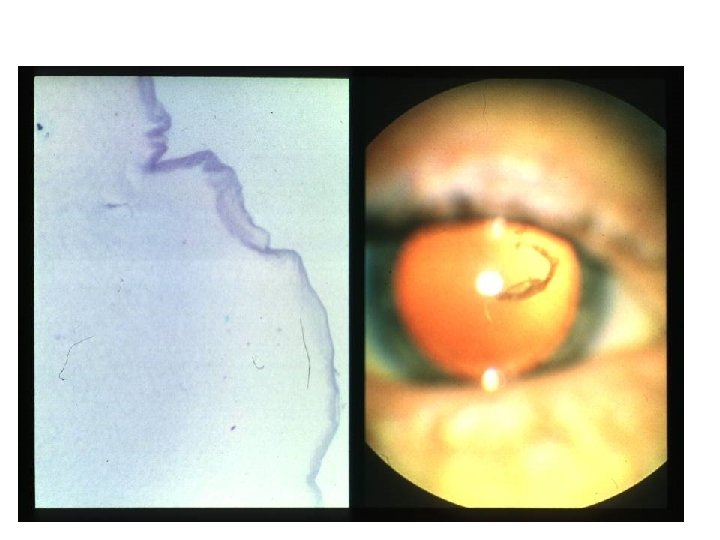
Posterior Vitreous Detachment (PVD)
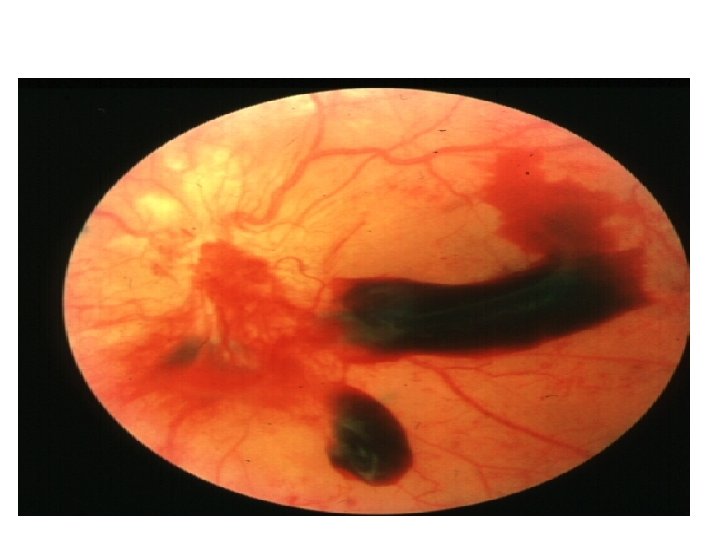
Vitreous Heme
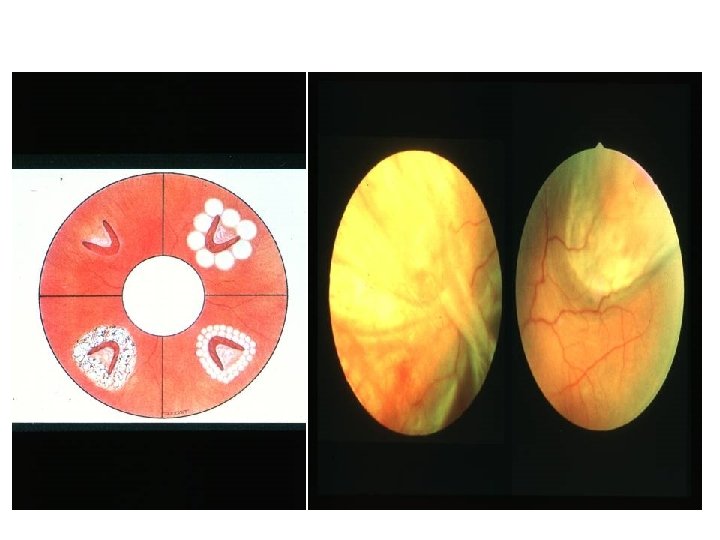
Retinal Tear

Flashes and Floaters • Sudden onset typically means a PVD, retinal tear or heme • If the spots appear after flashing light, then retinal tear must be eliminated • Myopes tend to have floaters and will notice them for a long time • Key is to rule out potentially sight threatening condition for the floaters, ie retinal tear. • Patients with retinal condition such as lattice degeneration and myopes need to be educated about S&S of RD (flashes and floaters) – 5 -10% population has lattice – Risk of RD with lattice is approx 1% – 30 -50% of patients with a RD have lattice

Flashes and Floaters: Management • A patient who presents with a sudden onset PVD without retinal breaks or hemorrhage requires repeat peripheral examination in six weeks, as the risk of retinal complications is highest within the six weeks following vitreous detachment. • If no retinal breaks are seen at that point, routine yearly examination is all that is needed
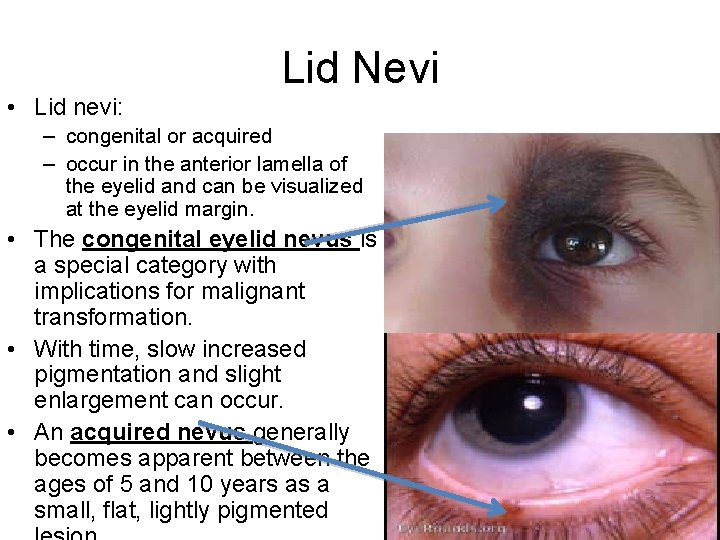
Lid Nevi • Lid nevi: – congenital or acquired – occur in the anterior lamella of the eyelid and can be visualized at the eyelid margin. • The congenital eyelid nevus is a special category with implications for malignant transformation. • With time, slow increased pigmentation and slight enlargement can occur. • An acquired nevus generally becomes apparent between the ages of 5 and 10 years as a small, flat, lightly pigmented
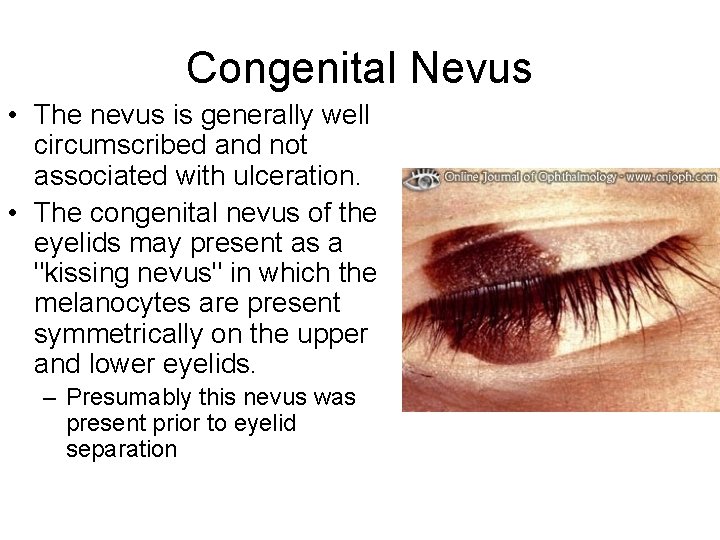
Congenital Nevus • The nevus is generally well circumscribed and not associated with ulceration. • The congenital nevus of the eyelids may present as a "kissing nevus" in which the melanocytes are present symmetrically on the upper and lower eyelids. – Presumably this nevus was present prior to eyelid separation

Congenital Nevus • Most nevi of the skin are not considered to be at increased risk of malignancy. – However, the large congenital melanocytic nevus appears to have an increased risk of malignant transformation of 4. 6% during a 30 year period
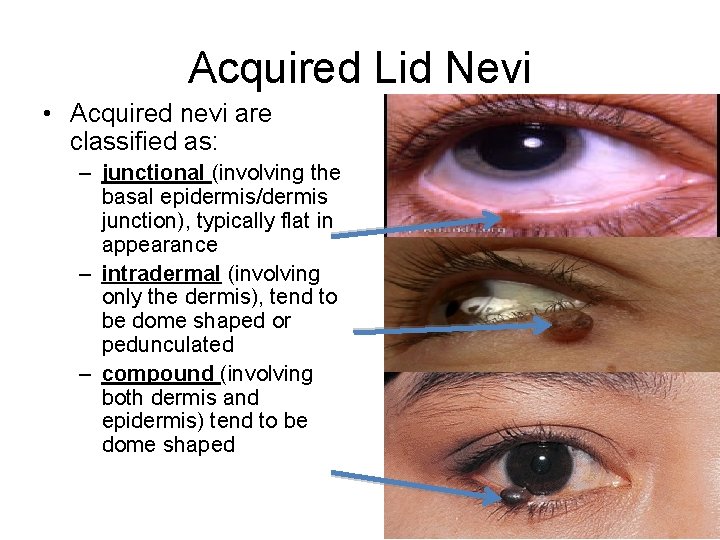
Acquired Lid Nevi • Acquired nevi are classified as: – junctional (involving the basal epidermis/dermis junction), typically flat in appearance – intradermal (involving only the dermis), tend to be dome shaped or pedunculated – compound (involving both dermis and epidermis) tend to be dome shaped

Corneal Ulcers • • Infective bacterial and fungal corneal lesions cause severe pain and loss of vision Signs and Symptoms: – Pain, photophobia, tearing – Mucopurulent discharge with generalized conjunctival injection – Decreased VA (esp if on visual axis) – Possible AC reaction and hypopyon – Dense infiltrate – Satellite lesions around main lesion may indicate fungal infection

Sterile vs Infectious Infiltrates
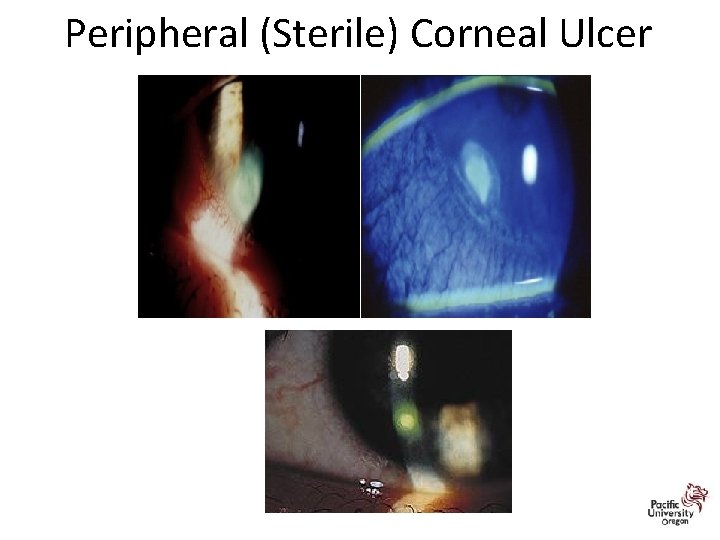
Peripheral (Sterile) Corneal Ulcer
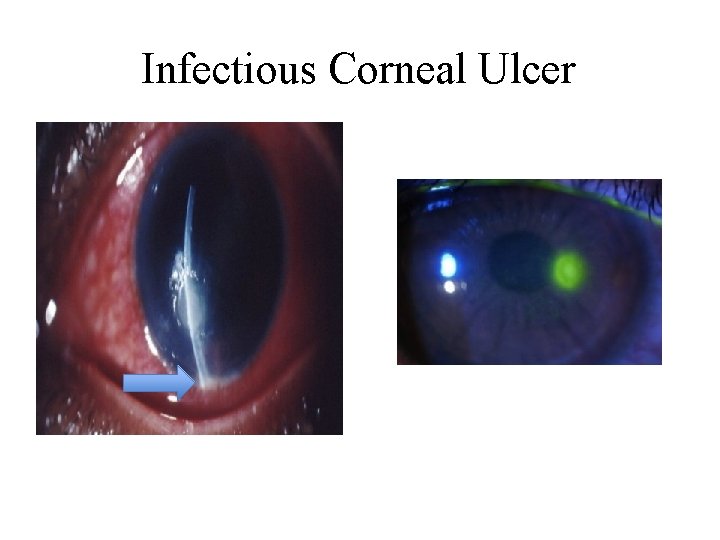
Infectious Corneal Ulcer

Corneal Ulcers • The Steroids for Corneal Ulcers Trial (SCUT) • Conclusions: – no overall difference in 3 -month BSCVA and no safety concerns with adjunctive corticosteroid therapy for bacterial corneal ulcers – researchers did find significant vision improvement for one specific subgroup of the study by using steroid therapy on patients with severe ulcers • Application to Clinical Practice: – Adjunctive topical corticosteroid use does not improve 3 -month vision in patients with bacterial corneal ulcers unless in the severe category

Corneal Ulcers • • Infective bacterial and fungal corneal lesions cause severe pain and loss of vision S and S: – Pain, photophobia, tearing – Mucopurulent discharge with generalized conjunctival injection – Decreased VA (esp if on visual axis) – Possible AC reaction and hypopyon – Dense infiltrate – Satellite lesions around main lesion may indicate fungal infection

Associated Factors • Contact lens wear, especially soft and extended wear lens • Recent history of corneal trauma • Topical steroid use • History of exposure to vegetative matter (fungal etiology)

Protein Synthesis Inhibitors • These antibiotics work by targeting the bacterial ribosome. – they are structurally different from mammalian ribosomes, – in higher concentrations many of these antibiotics can cause toxic effects. • This group includes: – (a) tetracyclines, (b) aminoglycosides, (c) macrolides, – (d) chloramphenicol, (e) clindamycin, (f) quinupristin/dalfopristin and (g) linezolid

Tetracyclines • Nonresistant strains concentrate this antibiotic intracellularly resulting in inhibition of protein synthesis. • Broad spectrum, bacteriostatic, – effective against gram (+) and (-) bacteria and against non-bacterial organisms – widespread resistance has limited their use. • Drug of choice for Rocky Mountain Spotted Fever, Cholera, Lyme disease, mycoplasma pneumonia, and chlamydial infections. • Side effects include gastric discomfort, phototoxicity, effects on calcified tissues, vestibular problems, pseudotumor.

Tetracyclines • This group includes: – Tetracycline (250 mg - 500 mg cap BID-QID) needs to be taken 1 hour before or 2 hours after a meal. – Minocycline (100 mg cap BID) – Doxycycline (20 mg - 100 mg cap or tab BID)
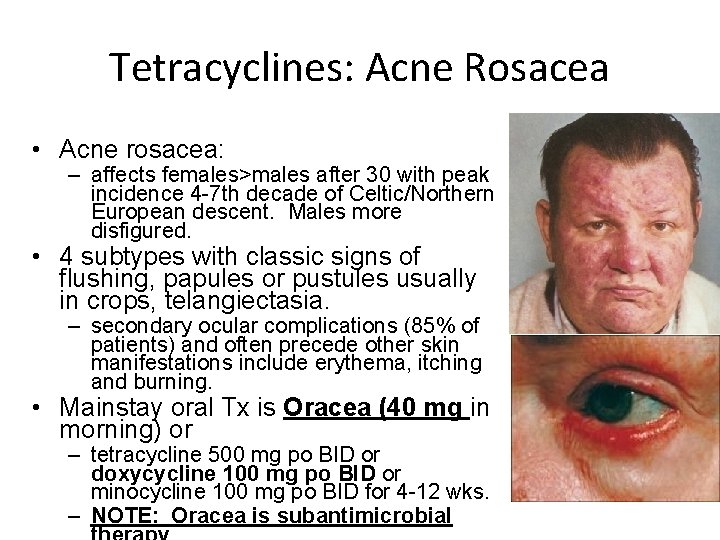
Tetracyclines: Acne Rosacea • Acne rosacea: – affects females>males after 30 with peak incidence 4 -7 th decade of Celtic/Northern European descent. Males more disfigured. • 4 subtypes with classic signs of flushing, papules or pustules usually in crops, telangiectasia. – secondary ocular complications (85% of patients) and often precede other skin manifestations include erythema, itching and burning. • Mainstay oral Tx is Oracea (40 mg in morning) or – tetracycline 500 mg po BID or doxycycline 100 mg po BID or minocycline 100 mg po BID for 4 -12 wks. – NOTE: Oracea is subantimicrobial
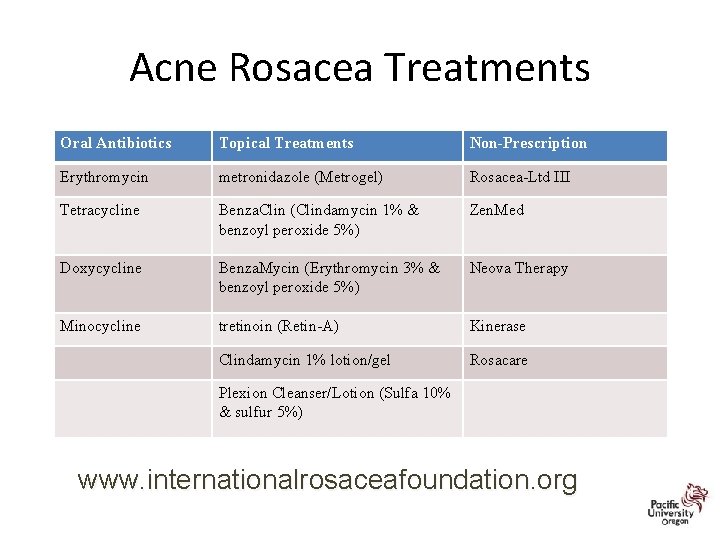
Acne Rosacea Treatments Oral Antibiotics Topical Treatments Non-Prescription Erythromycin metronidazole (Metrogel) Rosacea-Ltd III Tetracycline Benza. Clin (Clindamycin 1% & benzoyl peroxide 5%) Zen. Med Doxycycline Benza. Mycin (Erythromycin 3% & benzoyl peroxide 5%) Neova Therapy Minocycline tretinoin (Retin-A) Kinerase Clindamycin 1% lotion/gel Rosacare Plexion Cleanser/Lotion (Sulfa 10% & sulfur 5%) www. internationalrosaceafoundation. org

Anti-inflammatory effects • • • Degrade extracellular proteins Tetracyclines inhibit MMPs Anti-inflammatory
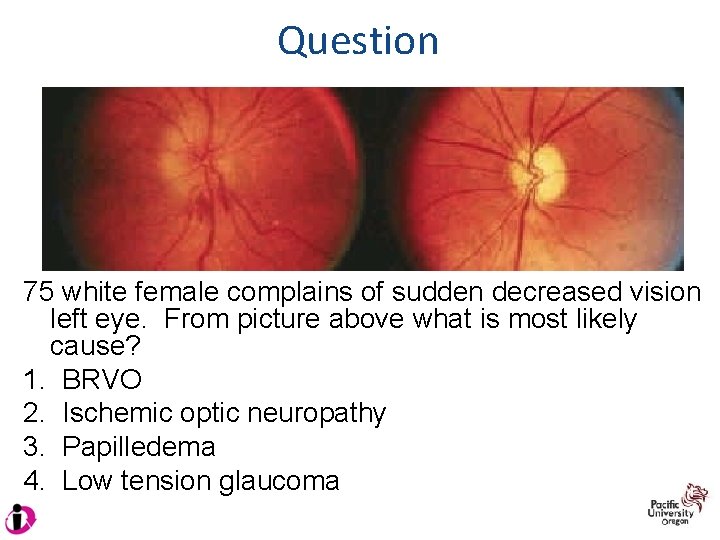
Question 75 white female complains of sudden decreased vision left eye. From picture above what is most likely cause? 1. BRVO 2. Ischemic optic neuropathy 3. Papilledema 4. Low tension glaucoma
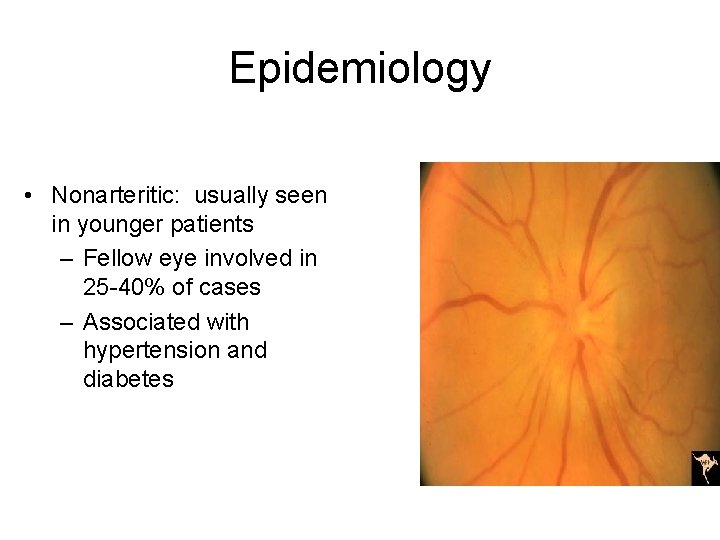
Epidemiology • Nonarteritic: usually seen in younger patients – Fellow eye involved in 25 -40% of cases – Associated with hypertension and diabetes
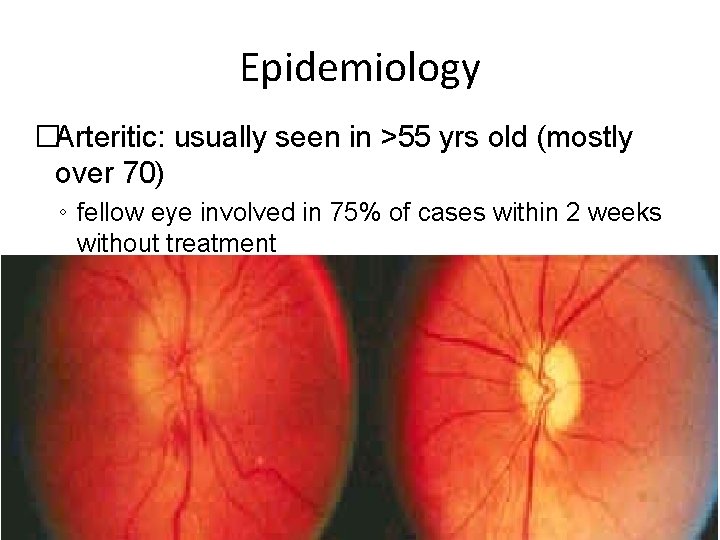
Epidemiology �Arteritic: usually seen in >55 yrs old (mostly over 70) ◦ fellow eye involved in 75% of cases within 2 weeks without treatment

Symptoms • Acute visual loss (arteritic>non) • dyschromatopsia • Arteritic may also have associated: – Headache, fever, malaise, – weight loss, scalp tenderness, jaw claudication, – amaurosis fugax, diplopia, and eye pain.
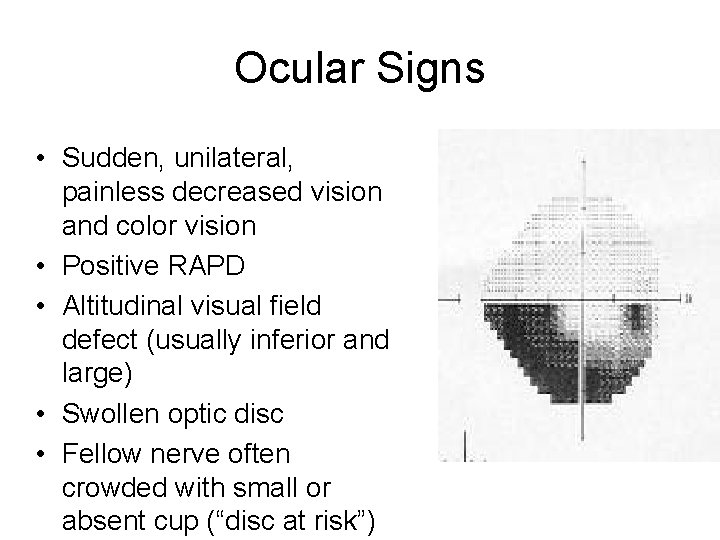
Ocular Signs • Sudden, unilateral, painless decreased vision and color vision • Positive RAPD • Altitudinal visual field defect (usually inferior and large) • Swollen optic disc • Fellow nerve often crowded with small or absent cup (“disc at risk”)

Additional Testing • Lab tests: – STAT ESR (rule out arteritic form) – CBC (low hematocrit, high platelets) – Fasting blood sugar – C reactive protein, – VDRL/FTA-ABS – ANA • Check blood pressure

Management • Arteritic: – Systemic steroids to prevent fellow eye involvement • methylprednisolone 1 g IV qd in divided doses for 3 days then, • prednisone 60 -100 mg po qd with a slow taper – Check PPD, blood glc and chest radiographs before starting systemic steroids • Non-arteritic: – Consider daily aspirin

Vision Loss Without Pain: TIA/TMB/Amaurosis Fugax �Refers to temporary visual impairment of variable duration (seconds to hours) ◦ TIA: transient ischemic attack-can be cerebral or retinal ◦ TMB: transient monocular blindness secondary to a retinal TIA ◦ Amaurosis Fugax: same as TMB �Abrupt onset, progression to involve all or part of visual field, sight usually returns �Within affected area, visual acuity maybe dimmed or completely lost

TIA’s • Stroke is 3 rd leading cause of mortality in developed countries and most common cause of neurological disability • 15 -20% of patients with stroke have a preceding TIA, though guidelines for referral and evaluation are debated – Traditional guidelines suggested that assessment should be complete within 1 week of TIA

TIA’s • Risk of stroke after TIA has traditionally been considered relatively low, but – new studies indicate that the risk is much higher than previously thought and the time window for prevention is short. • Effective secondary prevention depends on reliable identification of those at high risk and targeting treatment.

TIA’s: High Risk Factors �Five (5) risk factors are associated with a high risk (30%) of recurrent stroke at 3 months: ◦ Age over 60 ◦ Symptom duration greater than 10 minutes ◦ Motor weakness ◦ Speech impairment ◦ Diabetes �Isolated sensory of visual symptoms were associated with low risk of stroke!

TIA: Early Treatment �Several treatments are likely to be effective in preventing stroke in the acute phase after a TIA: ◦ ◦ ◦ Aspirin Anticoagulants Statins Endarterectomy (for >50% carotid stenosis) Further research needed for: �Lowering blood pressure acutely after TIA �Prophylactic use of neuroprotective drugs

Amaurosis Fugax: TMB • Most common cause is: – thromboembolic disease (eg carotid artery disease throwing emboli) or – vasospasm • Described as “curtain falling over vision” • Risk of stroke or death is about 3 -5%, – which is significantly lower than for a cerebral TIA (1520%) • Px still require work-up to determine cause: – e. g. carotid doppler
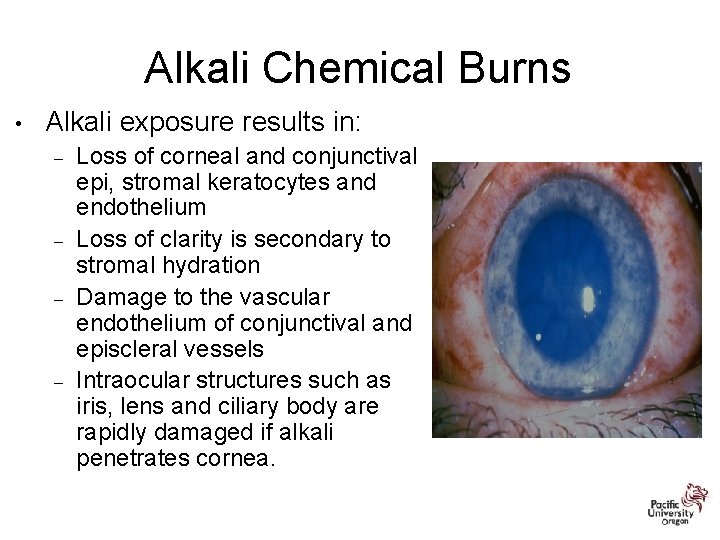
Alkali Chemical Burns • Alkali exposure results in: – – Loss of corneal and conjunctival epi, stromal keratocytes and endothelium Loss of clarity is secondary to stromal hydration Damage to the vascular endothelium of conjunctival and episcleral vessels Intraocular structures such as iris, lens and ciliary body are rapidly damaged if alkali penetrates cornea.

Acidic Chemical Burns • • Epithelium provides effective barrier to weak acids. Stronger acids cause protein precipitation in epithelium and stroma which creates a barrier to further penetration. Very strong acids penetrate as quickly as alkalis

Chemical Burn Treatment • Immediate irrigation is of paramount importance • Most patients are disabled by severe blepharospasm and disorientation so require assistance away from harm and to initiate irrigation. • Make sure to remove any solid particulate matter prior to beginning irrigation • Minimum of 15 minutes constant irrigation (some recommend 30 minutes)

Chemical Burn Treatment • Water is commonly recommended however it is hypotonic to corneal tissue and can result in increased water intake into the corneal and subsequent diffusion of corrosive materials deeper into cornea. • Recommend fluids of higher osmolarity such as sterile lactated Ringers and balanced saline solution.

Chemical Burn Treatment • Effectiveness of irrigation can be assessed using p. H paper and continued as long as p. H outside of the normal range. • For grade I and II burns will typically heal without permanent damage. – Topical steroid/antibiotic drops/ung recommended and daily follow up. – Cycloplegia for pain and further reduction of inflammation.

Chemical Burn Treatment • Severe ocular burns are difficult to treat and may require months of healing • Basic treatment of these eyes is to reduce inflammatory response caused by necrotic tissue – Corticosteroid use – Prophylactic antibiotics (consider doxycycline as it inhibits proteinase activity) – May require surgical intervention with debridement of necrotic tissue and possibly reconstructive surgery.
- Slides: 101