Diabetic Ketoacidosis DKA Hyperglycemic Hyperosmolar State HHS Ulrich

Diabetic Ketoacidosis (DKA) & Hyperglycemic Hyperosmolar State (HHS) Ulrich K. Schubart, MD JMC/AECOM

DKA/HHS Presenting Symptoms l Nausea and Vomiting l Polyuria and Polydipsia l Weakness and/or Anorexia l Abdominal Pain l Visual Disturbances l Somnolence

DKA/HHS Presenting Signs l Tachycardia l Hypotension l Dehydration l Hypothermia l Warm dry Skin l Kussmaul Respiration l Lethargy or Coma l Fruity Odor
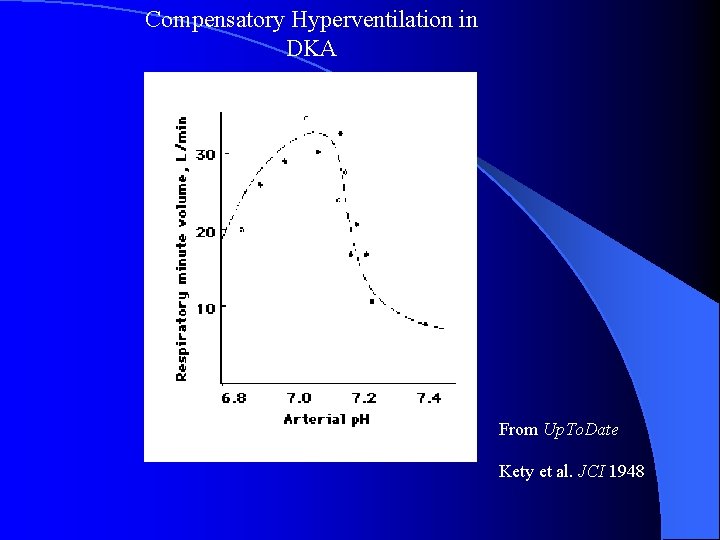
Compensatory Hyperventilation in DKA From Up. To. Date Kety et al. JCI 1948

DKA/HHS Precipitating Factors Any major Stress/Acute Illness • Infection Pneumonia Gastroenteritis UTI Sepsis Meningitis Influenza Mucormycosis • Emotional Problems • Trauma • Acute Pancreatitis • Myocardial Infarction • Stroke • Endocrine Acromegaly Thyrotoxicosis Cushing’s S. • Omission of Antidiabetic Mx’s • Drugs

DKA/HHS Drugs that can Precipitate • Psychotropic Drugs Chlorpromazine Clozapine Risperidone Loxapine • Steroids • Immunosuppressants • Beta Blockers • Calcium Channel Blockers • Diuretics • Anticonvulsants • Diazoxide
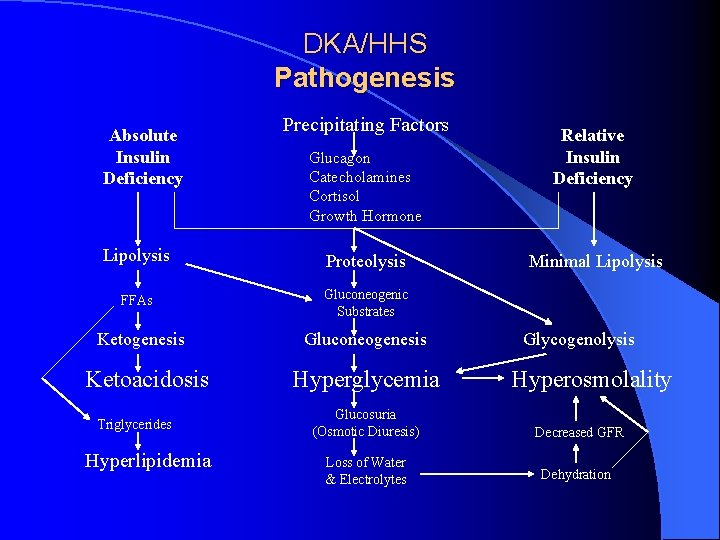
DKA/HHS Pathogenesis Absolute Insulin Deficiency Precipitating Factors Glucagon Catecholamines Cortisol Growth Hormone Lipolysis Proteolysis FFAs Gluconeogenic Substrates Ketogenesis Ketoacidosis Triglycerides Hyperlipidemia Gluconeogenesis Hyperglycemia Relative Insulin Deficiency Minimal Lipolysis Glycogenolysis Hyperosmolality Glucosuria (Osmotic Diuresis) Decreased GFR Loss of Water & Electrolytes Dehydration
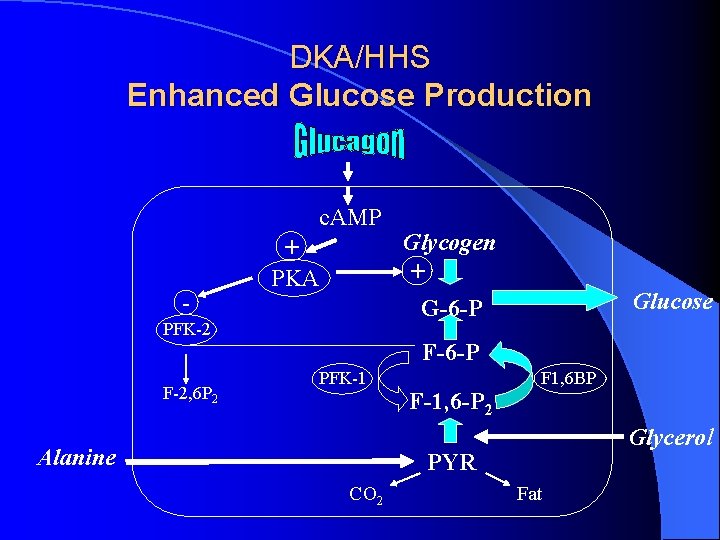
DKA/HHS Enhanced Glucose Production c. AMP - + PKA PFK-2 F-2, 6 P 2 Glycogen + G-6 -P Glucose F-6 -P PFK-1 Alanine F-1, 6 -P 2 F 1, 6 BP Glycerol PYR CO 2 Fat
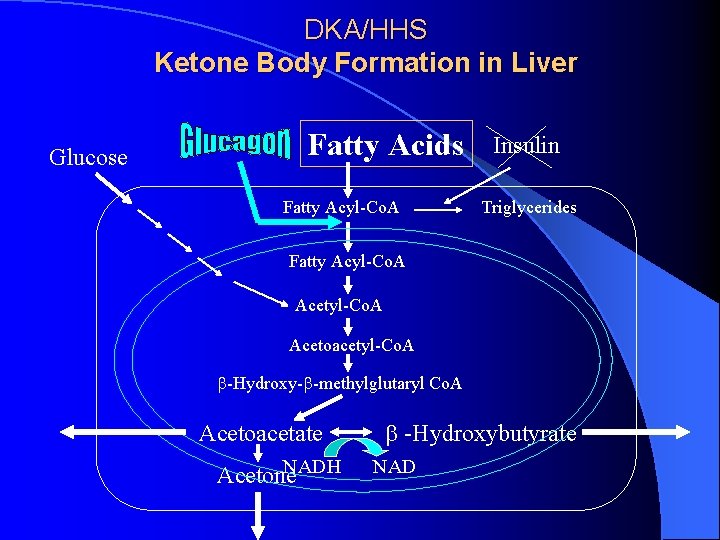
DKA/HHS Ketone Body Formation in Liver Glucose Fatty Acids Fatty Acyl-Co. A Insulin Triglycerides Fatty Acyl-Co. A Acetoacetyl-Co. A b-Hydroxy-b-methylglutaryl Co. A Acetoacetate NADH Acetone b -Hydroxybutyrate NAD
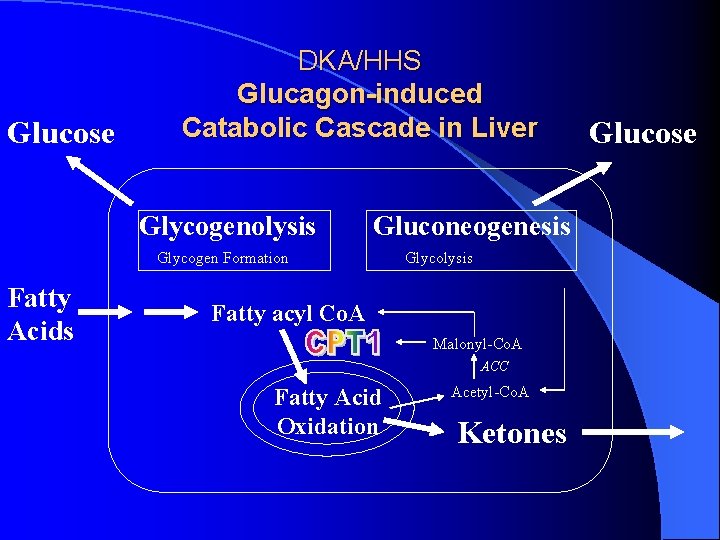
Glucose DKA/HHS Glucagon-induced Catabolic Cascade in Liver Glycogenolysis Gluconeogenesis Glycogen Formation Fatty Acids Glycolysis Fatty acyl Co. A Malonyl-Co. A ACC Fatty Acid Oxidation Acetyl-Co. A Ketones Glucose
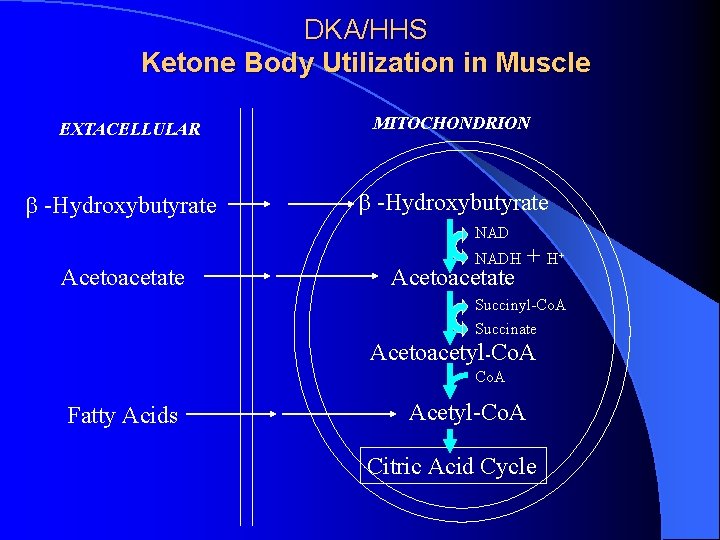
DKA/HHS Ketone Body Utilization in Muscle EXTACELLULAR b -Hydroxybutyrate MITOCHONDRION b -Hydroxybutyrate NAD Acetoacetate NADH Acetoacetate + H+ Succinyl-Co. A Succinate Acetoacetyl-Co. A Fatty Acids Acetyl-Co. A Citric Acid Cycle

DKA/HHS Glucotoxicty & Lipotoxicity 1. Relatively Short Term: Reversible Inhibition of: a) Glucose Uptake and Utilization in Insulin-Responsive Target Tissues b) Insulin Secretion 2. Long-term: a) & b) + Apoptosis of Beta-Cells

DKA/HHS Essential to R/o Infection l l l Look for meningeal signs - Head CT/MR followed by LP may be indicated Look for necrotic lesions in nasal turbinates to r/o mucormycosis For abdominal pain consider appendicitis cholecystitis pancreatitis diverticulitis PID Obtain CXR Check urine sediment

DKA/HHS Hyperosmolality Measure and Calculate Serum Osmolality = 2 x measured Na+ (m. Eq/l) + glucose (mg/dl) /18 + BUN (mg/dl)/2. 8 Osmolar Gap = Measured – Calculated Serum Osmolality Effective Serum Osmolality Osm. Eff (>320 =HHS) = 2 x measured Na+ (m. Eq/l) + glucose (mg/dl) /18

DKA/HHS Sodium Correction Corrected Sodium = Measured Sodium + 1. 6 x plasma glucose (mg/dl) – 100
![DKA/HHS Metabolic Acidosis Plasma Anion Gap = Na+ - [Cl- + HCO 3 -] DKA/HHS Metabolic Acidosis Plasma Anion Gap = Na+ - [Cl- + HCO 3 -]](http://slidetodoc.com/presentation_image_h/a572d146a85dcd58dbf3a0c3195403c6/image-16.jpg)
DKA/HHS Metabolic Acidosis Plasma Anion Gap = Na+ - [Cl- + HCO 3 -] (m. Eq/l)
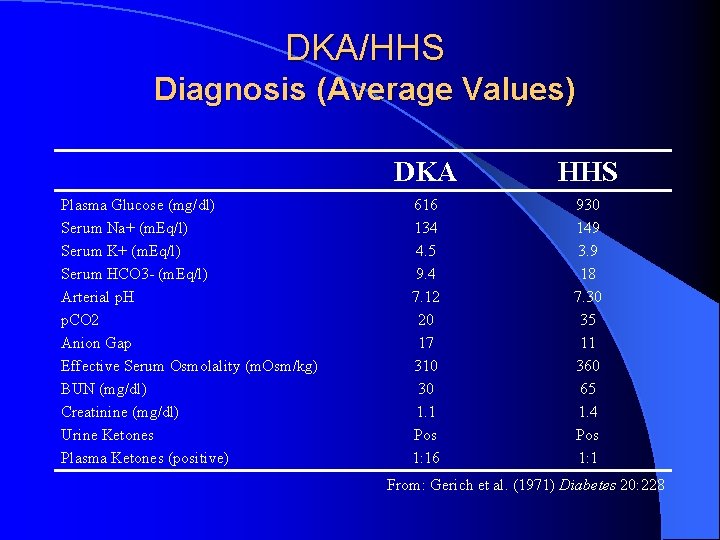
DKA/HHS Diagnosis (Average Values) Plasma Glucose (mg/dl) Serum Na+ (m. Eq/l) Serum K+ (m. Eq/l) Serum HCO 3 - (m. Eq/l) Arterial p. H p. CO 2 Anion Gap Effective Serum Osmolality (m. Osm/kg) BUN (mg/dl) Creatinine (mg/dl) Urine Ketones Plasma Ketones (positive) DKA HHS 616 134 4. 5 9. 4 7. 12 20 17 310 30 1. 1 Pos 1: 16 930 149 3. 9 18 7. 30 35 11 360 65 1. 4 Pos 1: 1 From: Gerich et al. (1971) Diabetes 20: 228

DKA/HHS Typical Water and Electrolyte Deficits Total Water (ml/kg) Na+ (m. Eq/kg) Cl- (m. Eq/kg) K+ (m. Eq/kg) PO 4 (mmol/kg) Mg++ (m. Eq/kg) Ca++ (m. Eq/kg) DKA HHS 6 50 -100 7 -10 4 -7 3 -12 1 1 1 9 100 -200 5 -13 5 -15 4 -6 3 -7 1 -2

DKA/HHS Poor Prognostic Indicators l Advanced l Low Age p. H l Hypotension l Marked Hyperosmolality l High BUN l Associated Diseases

DKA/HHS Treatment Considerations l l l l Precipitating Cause evident in 80% ECG indicated in all adult patients Isotonic Na. Cl preferred for initial rehydration IV Insulin preferred mode of administration Potassium depletion in all patients Prevention is long-term goal of management Bicarbonate administration rarely indicated

DKA/HHS Other Considerations in Tx l Type & Cross-match as indicated l Blood (and other) Cultures as indicated l Aspirate Gastric Contents if Comatose l Catherize if needed for Output Measurement l Give Oxygen if indicated l Keep patient NPO

DKA/HHS Essential Components in Tx l IV Fluids l Insulin l Potassium

DKA/HHS Essential Components in Tx IV Fluids l 2 -3 L 0. 9% saline during first 3 h l Subsequently, 0. 45% saline at 150 -300 ml/h l Add 5% dextrose when plasma glucose reaches 250 mg/dl

DKA/HHS Essential Components in Tx Insulin l 10 U/h iv infusion of short-acting insulin l Increase rate 2 -10 fold if no response by 4 h l Decrease to 1 -2 U/h when acidosis is corrected l Administer sc insulin before stopping iv infusion

DKA/HHS Essential Components in Tx Potassium l 10 -20 m. Eq/h when plasma K<6. 0, ECG normal, urine flow documented l 40 -80 m. Eq/h when plasma K <3. 5 or if bicarb is given

DKA/HHS Clinical Monitoring Clinical Parameters Monitoring Interval Mental Status Vital Sg’s Body Weight ECG 1 h 1 h 6 -12 h As indicated

DKA/HHS Monitoring Lab Values Laboratory Glucose Potassium, p. H Sodium, Chloride, Bicarb BUN, Creatinine Phosphate, Magnesium Urine Ketones Calcium Hematocrit Monitoring Interval 1 h 1 -2 h 2 -4 h 4 -6 h 2 -4 h As indicated

DKA/HHS Monitoring Therapy Monitoring Interval Fluid Intake & Output Insulin (U/h) Potassium (m. Eq/h) Glucose (g/h) Bicarb & Phos (m. Eq/h) 1 -4 h 1 -4 h
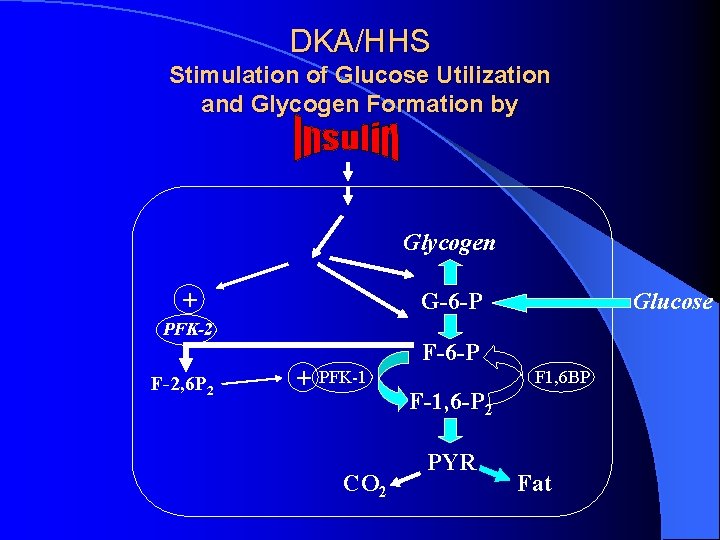
DKA/HHS Stimulation of Glucose Utilization and Glycogen Formation by Glycogen + G-6 -P PFK-2 F-2, 6 P 2 Glucose F-6 -P + PFK-1 F 1, 6 BP F-1, 6 -P 2 CO 2 PYR Fat
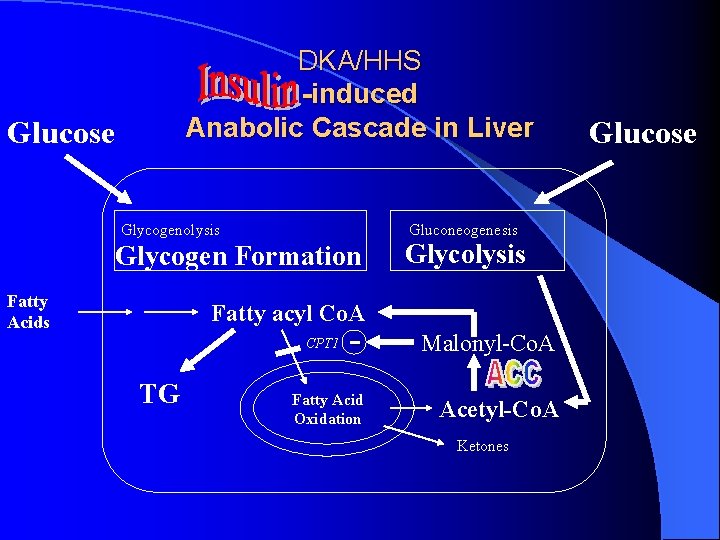
DKA/HHS -induced Anabolic Cascade in Liver Glucose Glycogenolysis Gluconeogenesis Glycogen Formation Fatty Acids Glycolysis Fatty acyl Co. A - Malonyl-Co. A Fatty Acid Oxidation Acetyl-Co. A CPT 1 TG Ketones Glucose

DKA/HHS Adverse Effects of Severe Acidosis l Impaired Cardiac Contractility l Decreased Response to Vasoconstrictors l Inhibition of Respiration

DKA/HHS Potential Adverse Effect of Bicarbonate Administration l Significantly l Decreased Increased Risk of Hypokalemia Tissue Oxygen Delivery

DKA/HHS Indications for Considering Bicarbonate Administration l p. H < 7. 0 or HCO 3 - < 5. 0 l K+ > 6. 5 l Hypotension refractory to fluid replacement l Severely impaired LV function l Respiratory depression l Marked late hyperchloremic acidosis l Significant lactic acidosis
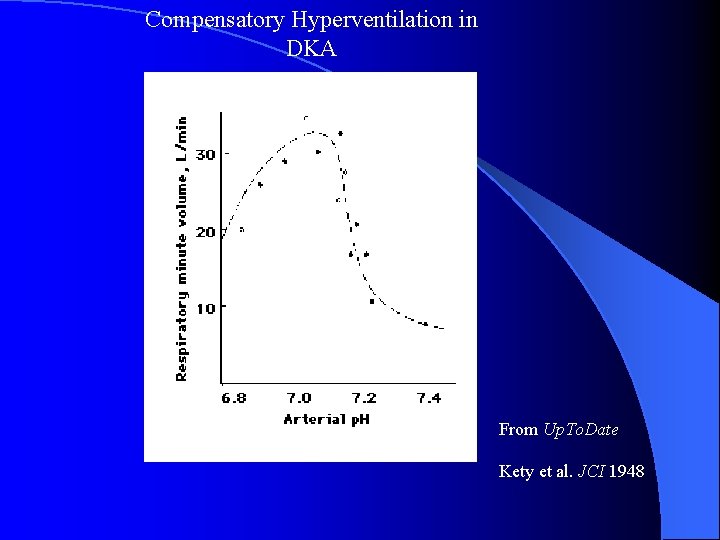
Compensatory Hyperventilation in DKA From Up. To. Date Kety et al. JCI 1948

DKA/HHS Complications of Therapy l Hypoglycemia l Hypokalemia or Hyperkalemia l Fluid Overload l Hyperchloremic Acidosis l Cerebral Edema l ARDS l Thromboembolic Episodes

DKA/HHS Prevention l Education of Patient and Health Care Providers
- Slides: 36