Diabetic Ketoacidosis DKA from Primary to Intensive Care

Diabetic Ketoacidosis (DKA) from Primary to Intensive Care Wendy Nasser MSN, CPNP-AC/PC Mark Riccioni MSN, CPNP-AC/PC Pediatrics

We have no conflicts of interest to disclose Pediatrics

Objectives 1. Describe classic signs and symptoms of DKA in the new onset diabetic. 2. Summarize pertinent lab studies and acute management of DKA. 3. Identify the diabetic child in crisis 4. Describe various fluid management options 4. Explain the role of parental involvement in the care of puberty-aged diabetic children and the effect of decreased readmissions. Pediatrics Page 2 xxx 00. #####. ppt 10/25/2020 7: 53: 59 PM

Case Study Pediatrics Page 3 xxx 00. #####. ppt 10/25/2020 7: 53: 59 PM

Let’s talk about pathophysiology • Diabetes Mellitus (DM) is a syndrome that occurs secondary to the body’s inability to maintain energy homeostasis. • DM type 1 results from insulin deficiency caused by autoimmune destruction of islet cells in the pancreas and is then manifested by decreased uptake of glucose resulting in high serum glucose. Pediatrics Page 4 xxx 00. #####. ppt 10/25/2020 7: 53: 59 PM

A closer look at Pathophysiology of DM type 1 Due to lack of insulin hormone, Glucose draws water into the serum and into the kidneys. As the osmotic force of glucose builds in the kidneys (above 180), urine output increases (polyuria) and thirst is sensed (polydypsia) along with hunger (polyphagia) and weight loss occurs. As the body becomes more and more dehydrated, increased release of Growth Hormone, Glucagon and epinephrine ensues. Breakdown of fat stores and creation of ketones then results from the imbalance between catabolic (glucagon and epinephrine) and anabolic (insulin) hormones. The buildup of ketones results in ketoacidosis The body senses stress (i. e. acidosis, hyperglycemia, lactic acidosis and poor tissues perfusion) and responds by releasing cortisol, catecholamines and more growth hormone. The worsening imbalance restarts the cycle and the patient becomes more and more intravascularly depleted and symptomatic. Pediatrics Page 5 xxx 00. #####. ppt 10/25/2020 7: 53: 59 PM

Pathophysiology: • DM type 2 typically results from insulin resistance and relative insulin deficiency leading to abnormal metabolism of carbohydrates, protein and fat. Type 2 is becoming more prevalent in children with obesity on the rise. Pediatrics Page 6 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

Diabetic Ketoacidosis is the most common endocrine metabolic disorder in childhood and adolescence(add bar graph) Pediatrics Page 7 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

When all the of the symptoms coalesce Severity on presentation dictates treatment of DKA and degree of treatment required… • p. H < or > 7. 15 • HCO 3 > or < then 10 • Glasco Coma Score (GCS<13) • Respiratory status • Level of dehydration • Electrolyte derangements • Age less than 5 Pediatrics Page 8 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

We can’t forget to correct for lab values! • Corrected Na+= Na+ + 0. 016 x (Glucose-100) • Osmolarity = 2 x (Na+) + (Glu/18) + (BUN/2. 8) • K+ elevated in 1/3 of cases, do not add to IV fluids if no UOP or serum K+>5. 5 Pediatrics Page 9 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

Fluid Protocol Controversies The common concern during DKA treatment is the potential risk of brain injury to the patient as he/she undergoes correction of acidosis resulting in fluid shifts in the brain In the US, treatment of DKA across institutions varies widely with different fluid protocols in place and no consensus on which protocol is best at protecting patients from harm. Pediatrics Page 10 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

But is it all about lab correction? • Lab values can be corrected…over time • The true question is: can we protect the affected children from the effects of DKA and improve their brain’s recovery and development? Pediatrics Page 11 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

• Scan and Insert cover of DKA study paper here Pediatrics Page 12 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

Concerning data • 1% of patients in DKA have clinically overt signs of cerebral edema • 50% of affected children die or sustain permanent neurological injury. • (Ref 5, 6 from k&G) Pediatrics Page 13 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

DKA Fluid Protocol (Kuppermann and Glaser) 2011 • Reported that Cerebral edema (CE) resulting from diabetic ketoacidosis (DKA) is the most frequent diabetes-related cause of death in children. • Ref (2, 4 from k &g) Pediatrics Page 14 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

Kuppermann and Glaser’s Preliminary Animal Studies Data from rat studies suggested that decreased cerebral blood flow during DKA may be part of the cause behind DKA-related brain injury The rat models also indicated that the brain metabolic state actually worsens initially during DKA treatment, theorized to be a result of reperfusion injury Pediatrics Page 15 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM
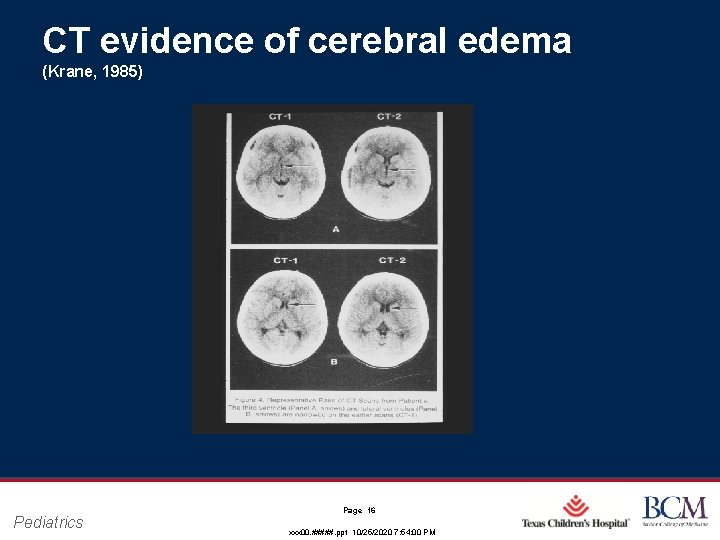
CT evidence of cerebral edema (Krane, 1985) Pediatrics Page 16 xxx 00. #####. ppt 10/25/2020 7: 54: 00 PM

What is the cause of Cerebral Edema? • The study aims to look at the two varying treatment strategies • 1. Conservative fluid therapy protocols: CE may result from osmotic shifts caused by rapid rehydration with intravenous fluids drives • 2. More liberal and rapid correction of DKA: Cerebral hypoperfusion may play a prominent role in the development of cerebral injury and CE • Best practice has not yet been determined Pediatrics Page 17 xxx 00. #####. ppt 10/25/2020 7: 54: 01 PM

Aspiring for Safe Change • Several institutions across the country are currently collaborating in Kuppermann and Glaser’s study with the overall goal to optimize DKA treatment and prevent neurological injury. • The hope is that collaboration of data acquisition will improve therapy and enhance long-term neurocognitive outcomes for children with diabetes Pediatrics Page 18 xxx 00. #####. ppt 10/25/2020 7: 54: 01 PM

Determining “best practice” is complicated at best • Children in the study are assigned to one of several fluid protocols all of which are used at some hospitals in the US • The aim is to determine which protocol has the best outcomes while nothing new or “experimental” is utilized Pediatrics Page 19 xxx 00. #####. ppt 10/25/2020 7: 54: 02 PM
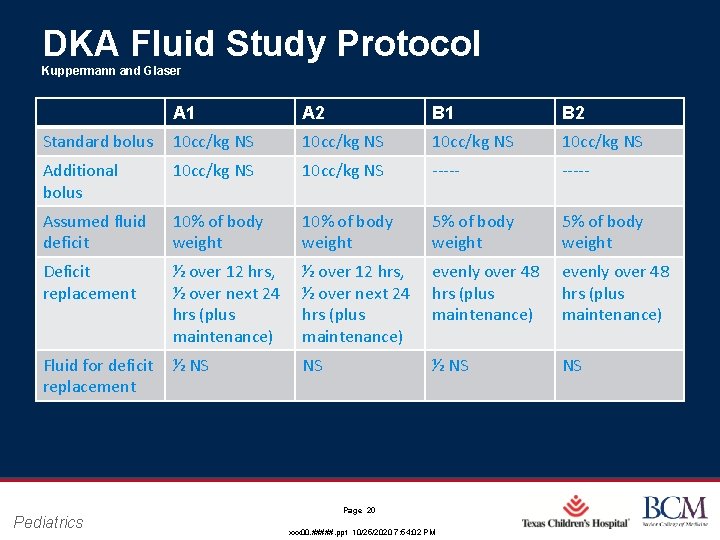
DKA Fluid Study Protocol Kuppermann and Glaser A 1 A 2 B 1 B 2 Standard bolus 10 cc/kg NS Additional bolus 10 cc/kg NS ‐‐‐‐‐ Assumed fluid deficit 10% of body weight 5% of body weight Deficit replacement ½ over 12 hrs, ½ over next 24 hrs (plus maintenance) evenly over 48 hrs (plus maintenance) Fluid for deficit replacement ½ NS NS Pediatrics Page 20 xxx 00. #####. ppt 10/25/2020 7: 54: 02 PM
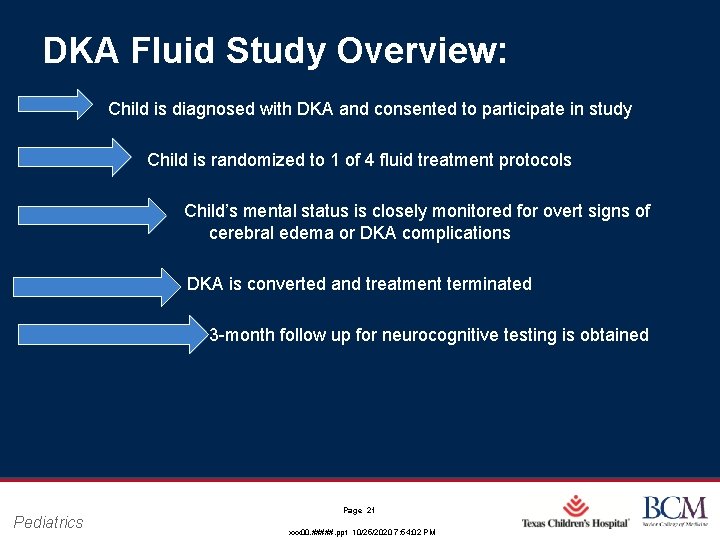
DKA Fluid Study Overview: Child is diagnosed with DKA and consented to participate in study Child is randomized to 1 of 4 fluid treatment protocols Child’s mental status is closely monitored for overt signs of cerebral edema or DKA complications DKA is converted and treatment terminated 3 -month follow up for neurocognitive testing is obtained Pediatrics Page 21 xxx 00. #####. ppt 10/25/2020 7: 54: 02 PM

Traditional Texas Children’s Hospital DKA Protocol The Two-Bag System Pediatrics Page 22 xxx 00. #####. ppt 10/25/2020 7: 54: 02 PM

Calculating IVF rate in DKA • Determine the number of IV boluses the patient received prior to start of correction • Subtract the total amount of fluid given from the total 24 h volume to be given for correction • (2500/m 2/d – total IV boluses)=correction volume to be given in 24 h. Divide the result by 24 to reveal the hourly rate in ml/h Pediatrics Page 23 xxx 00. #####. ppt 10/25/2020 7: 54: 04 PM

TCH 2 -bag system protocol • Bag A: LR + KPO 4 2 mmol/100 ml + KCL 1. 5 m. Eq/100 ml • Bag B: D 10 LR + KPO 4 2 mmol/100 ml + KCL 1. 5 m. Eq/100 ml • Total IVF ml/h= Bag A ml/h + Bag B ml/h dependent on blood glucose • Blood Glucose >300__ml/h (100% bag A) • 251 -300__ml/h (75% bag A) __ml/h (25% bag B) • 201 -250__ml/h (50% bag A) __ml/h (50% bag B) • 151 -200__ml/h (25% bag A) __ml/h (75% bag B) • Blood Glucose <150__ml/h (100% bag B) Pediatrics Page 24 xxx 00. #####. ppt 10/25/2020 7: 54: 04 PM

Insulin Administration • Insulin drips are recommended for patients less than or equal to 5 yo if HCO 3 </=15 m. Eq/L or if </= 12 m. Eq/L and older than 5 years of age • Recommended dose is 0. 1 units/kg/hr • If patient is less than 5 years of age or “Hyper osmolar” the recommended dose is 0. 05 units/kg/hr Pediatrics Page 25 xxx 00. #####. ppt 10/25/2020 7: 54: 04 PM

Extenuating Circumstances that Affect the Titration of Correction • When p. H is not improving, the insulin gtt may have to be titrated up • If glucose is decreasing too quickly (more than 100 mg/d. L per hour), the correction must be slowed down and the patient must be monitored closely Pediatrics Page 26 xxx 00. #####. ppt 10/25/2020 7: 54: 04 PM

Intensive Monitoring • Labs required for IVF titration and correction: • Gucose q 1 h • Lytes q 2 h x 2 then q 4 h • Initial blood gas • Q 1 h vitals and neuro vitals • Strict I&Os Pediatrics Page 27 xxx 00. #####. ppt 10/25/2020 7: 54: 04 PM

Insulin Administration • Without mental status changes on initial presentation, subcutaneous insulin can be given if HCO 3 is greater than 15 m. Eq/L in patients 5 yo or younger, or greater than 12 m. Eq/L in patients older than 5 yo • If 2 -bag system is required, once HCO 3 is greater than or equal to 15, the patient can be converted to subcutaneous therapy Pediatrics Page 28 xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM

• The role of parental involvement in the care of puberty-aged diabetic children and the effect of decreased readmissions Pediatrics Page 29 xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM

Criteria for Discharge • Corrected acidosis and return to “neurological baseline” • Completion of Diabetes education and agreement of responsible adult who assumes responsibility of minor’s welfare • Completed Endocrine Social Work consult to determine barrier to resources and medications • Follow up appointment is scheduled with Endocrinologist Pediatrics Page 30 xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM

Case Study Pediatrics Page 31 xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM

Questions? ? Pediatrics Page 32 xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM
![Starter Page 1 [36 pt bold] palette/guides • Text [Arial 28 pt] Work area Starter Page 1 [36 pt bold] palette/guides • Text [Arial 28 pt] Work area](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-34.jpg)
Starter Page 1 [36 pt bold] palette/guides • Text [Arial 28 pt] Work area (Guide set 2. 27) ‐ Text [Arial 22 pt] • Text [Arial 22 pt] Work area ¬ (Guide set 4. 51) Guide for Title and Appendix page ¬ (Guide set 1. 38) Work area (Guide set 4. 51) ® Primary Palette Bkgd 255 255 Text/Lines Shadows 0 0 0 128 128 Title Text Fill 1 Fill 2 Accent 3 255 255 0 37 78 63 128 205 241 90 41 192 192 Work area (Guide set 2. 87) ¯ Pediatrics Doc ID, Time stamp and page number only shows up in grayscale printing, Page 33 location is here, to edit go into slide master, this info will appear on every page, except Cover and Appendix pages xxx 00. #####. ppt 10/25/2020 7: 54: 05 PM
![Starter Page 2 [36 pt bold] just text • Text [Arial 28 pt] ‐ Starter Page 2 [36 pt bold] just text • Text [Arial 28 pt] ‐](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-35.jpg)
Starter Page 2 [36 pt bold] just text • Text [Arial 28 pt] ‐ Text [Arial 22 pt] • Text [Arial 22 pt] Pediatrics Page 34 xxx 00. #####. ppt 10/25/2020 7: 54: 06 PM

Section Header Subtitle Pediatrics
![Starter Page 4 [36 pt bold] 2 text columns • Text [Arial 28 pt] Starter Page 4 [36 pt bold] 2 text columns • Text [Arial 28 pt]](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-37.jpg)
Starter Page 4 [36 pt bold] 2 text columns • Text [Arial 28 pt] ‐Text [Arial 22 pt] • Text [Arial 22 pt] Pediatrics • Text [Arial 22 pt] Page 36 xxx 00. #####. ppt 10/25/2020 7: 54: 06 PM
![Starter Page 5 [36 pt bold] text box w/chart Subtitle • Text [Arial 28 Starter Page 5 [36 pt bold] text box w/chart Subtitle • Text [Arial 28](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-38.jpg)
Starter Page 5 [36 pt bold] text box w/chart Subtitle • Text [Arial 28 pt] ‐ Text [Arial 22 pt] Unit of measure • Text [Arial 22 pt] Pediatrics Page 37 xxx 00. #####. ppt 10/25/2020 7: 54: 06 PM
![Starter Page 6 [36 pt bold] text w/chart Subtitle • Text [Arial 28 pt] Starter Page 6 [36 pt bold] text w/chart Subtitle • Text [Arial 28 pt]](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-39.jpg)
Starter Page 6 [36 pt bold] text w/chart Subtitle • Text [Arial 28 pt] ‐ Text [Arial 22 pt] Unit of measure • Text [Arial 22 pt] Pediatrics Page 38 xxx 00. #####. ppt 10/25/2020 7: 54: 07 PM
![Starter Page 6 [36 pt bold] text w/bar chart Subtitle • Text [Arial 28 Starter Page 6 [36 pt bold] text w/bar chart Subtitle • Text [Arial 28](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-40.jpg)
Starter Page 6 [36 pt bold] text w/bar chart Subtitle • Text [Arial 28 pt] ‐ Text [Arial 22 pt] • Text [Arial 22 pt] Unit of measure Pediatrics Page 39 xxx 00. #####. ppt 10/25/2020 7: 54: 08 PM
![Starter Page 7 [36 pt bold] graphic w/chart Unit of measure Subtitle Pediatrics Page Starter Page 7 [36 pt bold] graphic w/chart Unit of measure Subtitle Pediatrics Page](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-41.jpg)
Starter Page 7 [36 pt bold] graphic w/chart Unit of measure Subtitle Pediatrics Page 40 xxx 00. #####. ppt 10/25/2020 7: 54: 08 PM
![Starter Page 8 [36 pt bold] 1 pie Legend 10 pt Label Legend 10 Starter Page 8 [36 pt bold] 1 pie Legend 10 pt Label Legend 10](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-42.jpg)
Starter Page 8 [36 pt bold] 1 pie Legend 10 pt Label Legend 10 pt Label Pediatrics Page 41 xxx 00. #####. ppt 10/25/2020 7: 54: 09 PM
![Starter Page 9 [36 pt bold] 2 pie Label Label Label Pediatrics Label Page Starter Page 9 [36 pt bold] 2 pie Label Label Label Pediatrics Label Page](http://slidetodoc.com/presentation_image/0b44c2743334ab0be653739b2aa37c3b/image-43.jpg)
Starter Page 9 [36 pt bold] 2 pie Label Label Label Pediatrics Label Page 42 xxx 00. #####. ppt 10/25/2020 7: 54: 10 PM

Pediatrics Page 43 xxx 00. #####. ppt 10/25/2020 7: 54: 11 PM
Video would be placed here, as would still images Pediatrics Page 44 xxx 00. #####. ppt 10/25/2020 7: 54: 11 PM
- Slides: 45