Diabetes mellitus Practicals experimental diabetes mellitus in laboratory

Diabetes mellitus Practicals – experimental diabetes mellitus in laboratory animal

Definition of DM l DM is a group of metabolic disorders characterized by hyperglycemia as a reason of impaired effect of insulin – – l absolute relative chronic hyperglycemia leads to cell & tissue damage (complications) – – – retina kidney nerves

Diagnosis of DM l classical symptoms of diabetes + random plasma glycemia 11. 1 mmol/l – – l FPG (fasting plasma glucose) 7. 0 mmol/l – l any time of the day symptoms include polyuria, polydipsia and rapid loose of weight fasting means at least 8 h from the last meal 2 -h PG (postprandial glucose) 11. 1 mmol/l during o. GTT – according to WHO standard load of 75 g of glucose

Interpretation of glycemia l FPG: – – – l <6. 1 mmol/l = normal glycemia 6. 1 -7. 0 mmol/l = IGT (impaired glucose tolerance) 7. 0 mmol/l = diabetes o. GTT – 2 h PG: – – – <7. 8 mmol/l = normal glucose tolerance 7. 8 - 11. 1 mmol/l = IGT 11. 1 mmol/l = diabetes
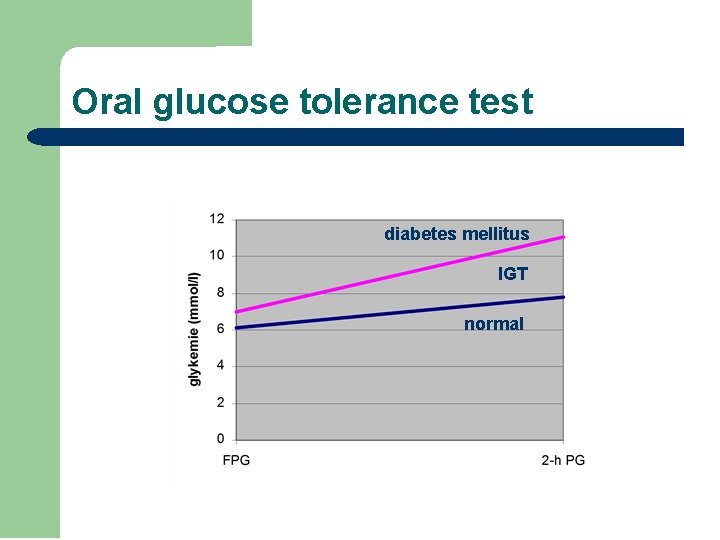
Oral glucose tolerance test diabetes mellitus IGT normal
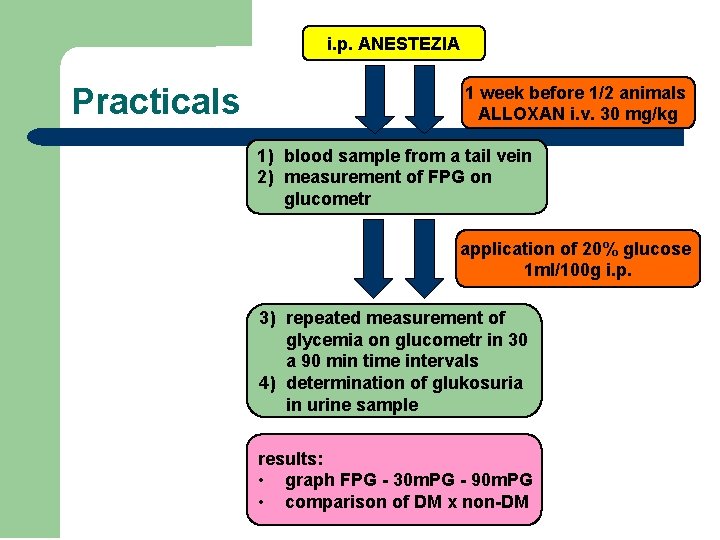
i. p. ANESTEZIA Practicals 1 week before 1/2 animals ALLOXAN i. v. 30 mg/kg 1) blood sample from a tail vein 2) measurement of FPG on glucometr application of 20% glucose 1 ml/100 g i. p. 3) repeated measurement of glycemia on glucometr in 30 a 90 min time intervals 4) determination of glukosuria in urine sample results: • graph FPG - 30 m. PG - 90 m. PG • comparison of DM x non-DM
Pathophysiology of DM
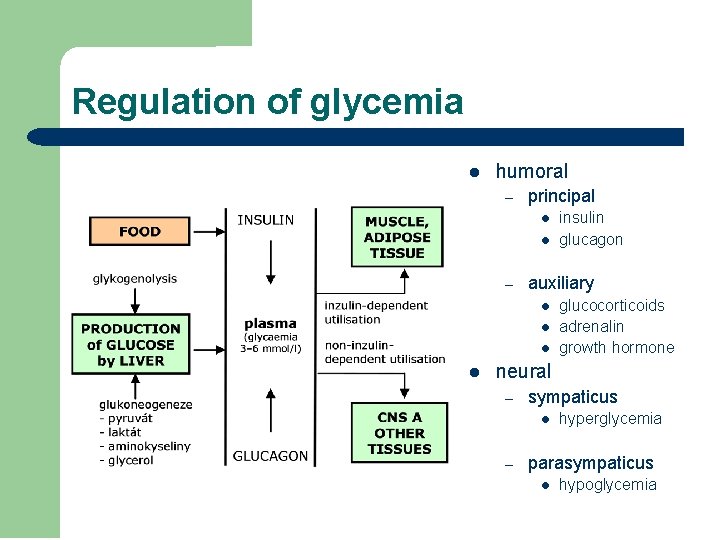
Regulation of glycemia l humoral – principal l l – auxiliary l l insulin glucagon glucocorticoids adrenalin growth hormone neural – sympaticus l – hyperglycemia parasympaticus l hypoglycemia
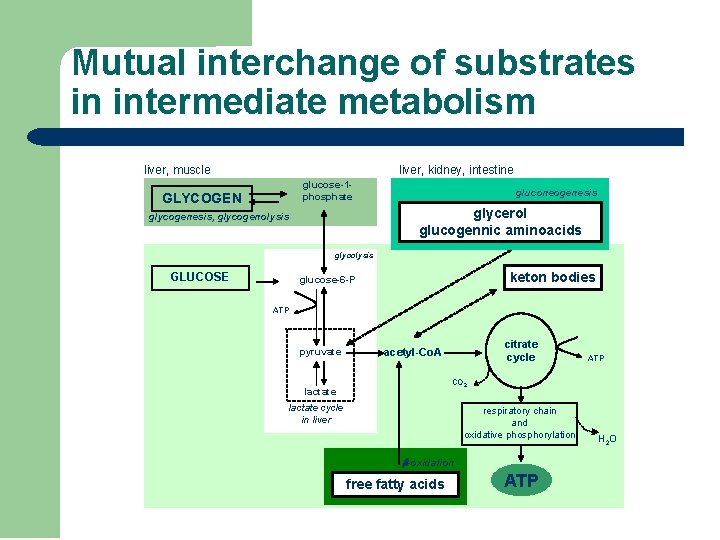
Mutual interchange of substrates in intermediate metabolism liver, muscle liver, kidney, intestine glucose-1 phosphate GLYCOGEN gluconeogenesis glycerol glucogennic aminoacids glycogenesis, glycogenolysis glycolysis GLUCOSE keton bodies glucose-6 -P ATP pyruvate citrate cycle acetyl-Co. A ATP CO 2 lactate cycle in liver respiratory chain and oxidative phosphorylation -oxidation free fatty acids ATP H 2 O

Insulin l l preproinsulin + C-peptide exocytosis into portal circulation – l total daily production 20 - 40 U – l 1/2 basal secretion, 1/2 stimulated basal secretion pulsatile – l 50% degraded during first pass through liver 5 - 15 min intervals stimulated – glucose, amino acids, FFA, GIT hormones – – early phase (ready insulin) late phase (synthesis de novo)
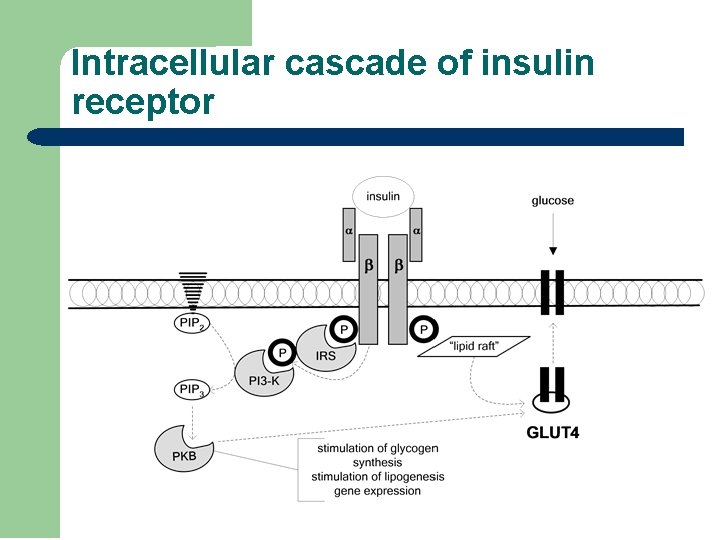
Intracellular cascade of insulin receptor

Classification of tissues according to insulin action: l insulin-sensitive – – – muscle, adipose tissue, liver facilitated diffusion by GLUT 4 integration into cytoplasmic membrane regulated by insulin l insulin-non-sensitive – others – facilitated diffusion by GLUT 1, 2, 3, 5, …. – transport of glucose depend solely on concentration gradient

Diabetes mellitus l heterogeneous syndrome characterized by hyperglycemia due to deficiency of insulin action (as a result of complete depletion or peripheral resistance) l prevalence of DM in general population 5%, over the age of 65 already 25%

Causes of insulin deficiency l absolute – destruction of the -cells of the islets of Langerhan´s l relative – insulin l l l – abnormal molecule of insulin (mutation) defective conversion of preproinsulin to insulin circulating antibodies against insulin or receptor insulin resistance in peripheral tissue l l receptor defect post-receptor defect

Classification of DM I. DIABETES MELLITUS Diabetes mellitus of type 1 (T 1 DM) Diabetes mellitus of type 2 (T 2 DM) Gestational diabetes mellitus Other specific types - genetic defects of β cell function (MODY) - genetic abnormalities of insulin receptor - exocrine pancreas disorders - endocrinopathies - iatrogenic - rare genetic syndromes II. IMPAIRED GLUCOSE TOLERANCE (IGT) - with obesity without obesity
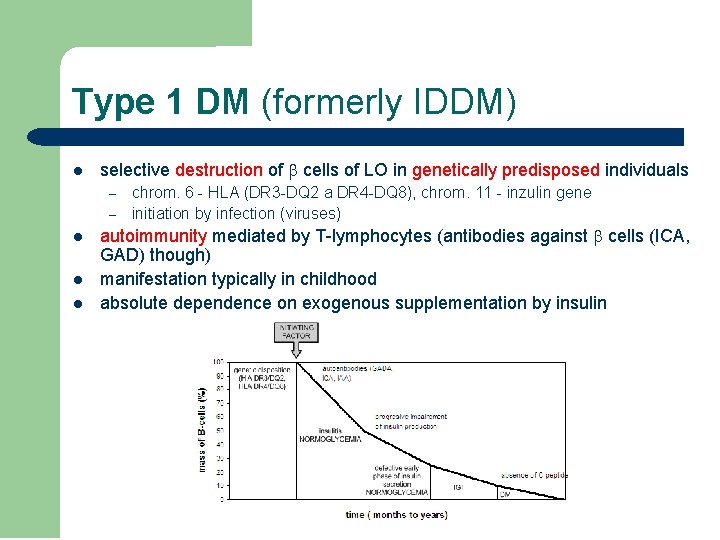
Type 1 DM (formerly IDDM) l selective destruction of cells of LO in genetically predisposed individuals – – l l l chrom. 6 - HLA (DR 3 -DQ 2 a DR 4 -DQ 8), chrom. 11 - inzulin gene initiation by infection (viruses) autoimmunity mediated by T-lymphocytes (antibodies against cells (ICA, GAD) though) manifestation typically in childhood absolute dependence on exogenous supplementation by insulin

Type 2 DM (formerly NIDDM) l l imbalance between secretion and affect of insulin genetic predisposition – polygenic – – l clinically manifested T 2 DM has concomitant insulin resistance and impairment of secretion – – l insulin resistance impairment of secretion due to epigenetic factors typically in older adults 90% of subjects is obese – metabolic syndrome!!!

Insulin resistance l l l physiologic amount of insulin does not cause adequate response compensatory hyperinsulinism further worsening by down-regulation of insulin receptors
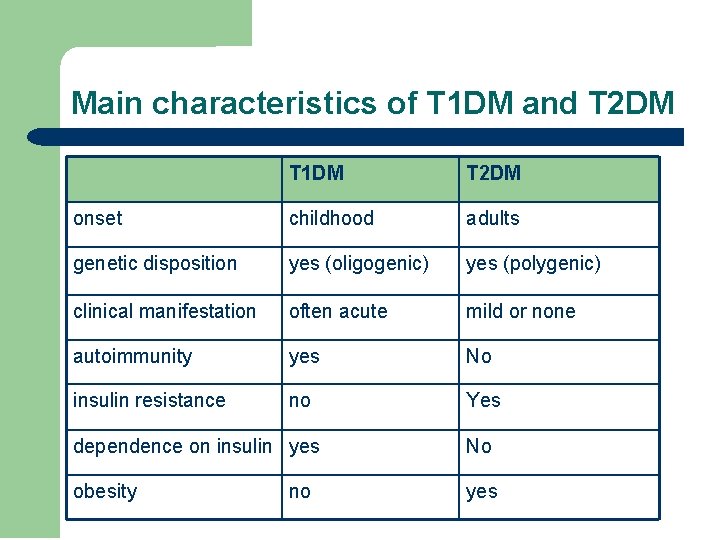
Main characteristics of T 1 DM and T 2 DM T 1 DM T 2 DM onset childhood adults genetic disposition yes (oligogenic) yes (polygenic) clinical manifestation often acute mild or none autoimmunity yes No insulin resistance no Yes dependence on insulin yes No obesity yes no

Clinical presentation of manifest DM l due to the increase of blood osmolality, osmotic diuresis and dehydratation – classical l l l polyuria thirst polydipsia weight loss temporary impairment of visus cutaneous infections l acute – hyperglycemic coma l l ketoacidotic non-ketoticidotic

Complications of DM l microvascular – – – l macrovascular – l atherosclerosis (CAD, peripheral and cerebrovascular disease) combined – l diabetic retinopathy diabetic nephropathy diabetic neuropathy (sensoric, motoric, autonomic) diabetic foot (ulcerations, amputations and Charcot´s joint) others – – – periodontitis cataract glaucoma
- Slides: 21