Diabetes Mellitus Pathophysiology NUR 210 Pathopharmacology I Wanda

Diabetes Mellitus Pathophysiology NUR 210 Pathopharmacology I Wanda Lovitz, ARNP

Diabetes Pathophyisology: Objectives n Describe the impact of diabetes mellitus in the United States. n Describe the effects of insulin deficit with regard to glucose, fat, and protein metabolism. n Describe the effect of insulin deficit with regard to fluid and electrolyte balance. n Relate the physiologic functions of insulin to the manifestations of type 1 and type 2 diabetes mellitus. n Compare the distinguishing feature of the different classification of diabetes mellitus: Type I, Type II, and gestational. n Describe the clinical manifestation associated with hypoglycemia. n Compare the pathophysiology associated with the clinical manifestations of diabetic ketoacidosis (DKA) and hyperglycemic hyperosmolar nonketotic syndrome (HHNKS). n Describe the pathophysiology and clinical manifestations associated with complications of diabetes.
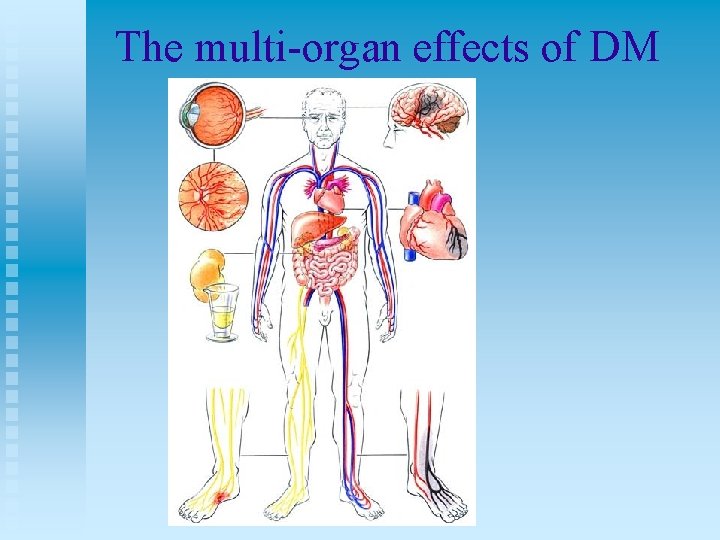
The multi-organ effects of DM

Where does the energy come from to fuel the body? n Carbohydrates (CHO)……Glucose n Fats n Proteins (amino acids)
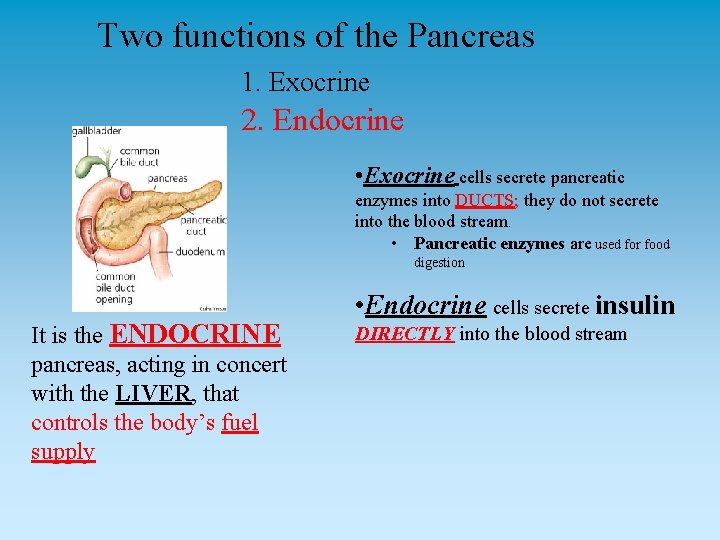
Two functions of the Pancreas 1. Exocrine 2. Endocrine • Exocrine cells secrete pancreatic enzymes into DUCTS; they do not secrete into the blood stream. • Pancreatic enzymes are used for food digestion It is the ENDOCRINE pancreas, acting in concert with the LIVER, that controls the body’s fuel supply • Endocrine cells secrete insulin DIRECTLY into the blood stream

What is the normal fasting blood glucose level? n NORMAL fasting blood sugar = 60 -99 mg/dl u u Levels of 100 -125 fasting indicate pre-diabetes Levels greater than 126 fasting on 2 or more ocassions indicate diabetes
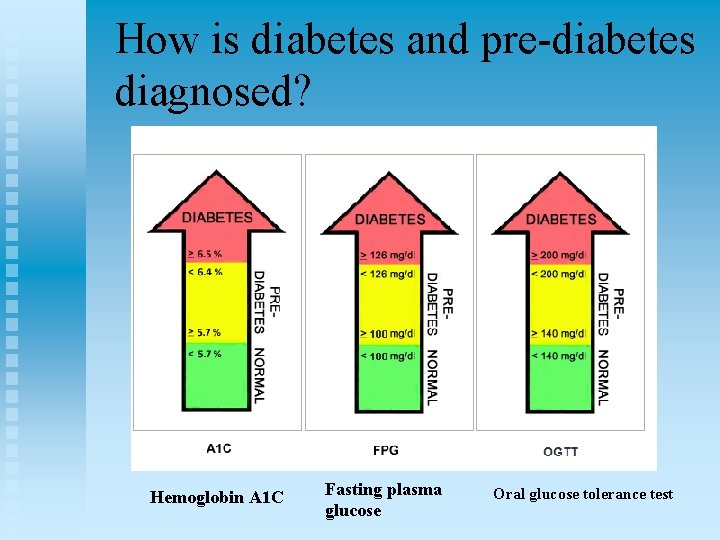
How is diabetes and pre-diabetes diagnosed? Hemoglobin A 1 C Fasting plasma glucose Oral glucose tolerance test
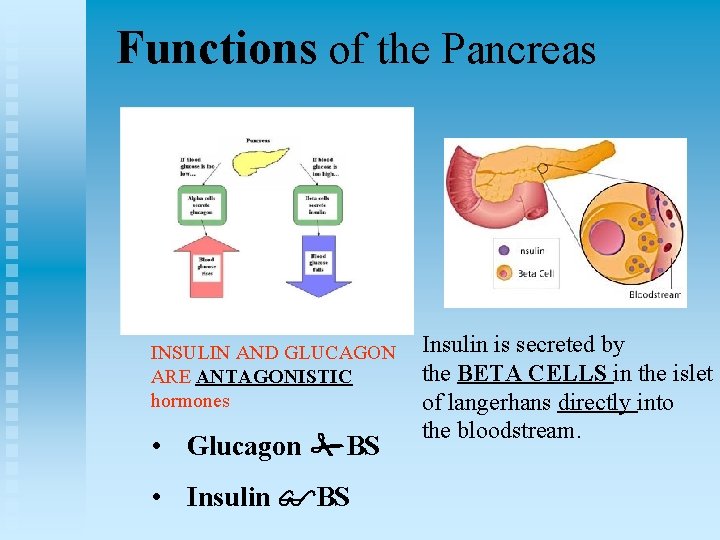
Functions of the Pancreas INSULIN AND GLUCAGON ARE ANTAGONISTIC hormones • Glucagon BS • Insulin BS Insulin is secreted by the BETA CELLS in the islet of langerhans directly into the bloodstream.

What is Insulin? n Insulin is a HORMONE that facilitates movement of glucose into body tissues to LOWER blood sugar levels n Actions of Insulin ¶ Promotes GLUCOSE uptake by target cells & provides for glucose storage ¶ · ¸ ¸ ¸ GLUCOSE IS STORED IN LIVER AS GLYCOGEN Prevents fat and glycogen breakdown Inhibits gluconeogenesis (synthesis of glucose) in the liver and Increases protein synthesis

Insulin Deficit results in n 1. Impaired CARBOHYDRATE (CHO) metabolism . hyperglycemia n 2. Impaired FAT metabolism u ketones formed n 3. Impaired PROTEIN metabolism u muscle wasting n 4. Fluid and ELECTROLYTE IMBALANCE u dehydration & thirst

Effects of Insulin Deficit: CARBOHYDRATES n Impaired CARBOHYDRATE Metabolism u CHO cannot enter (insulin-dependent) cells t u Cells begin to STARVE with use of backup sources of energy (fatty acids) Decreased glucose use by cells results in • Rapid build up of glucose in SERUM hyperglycemia
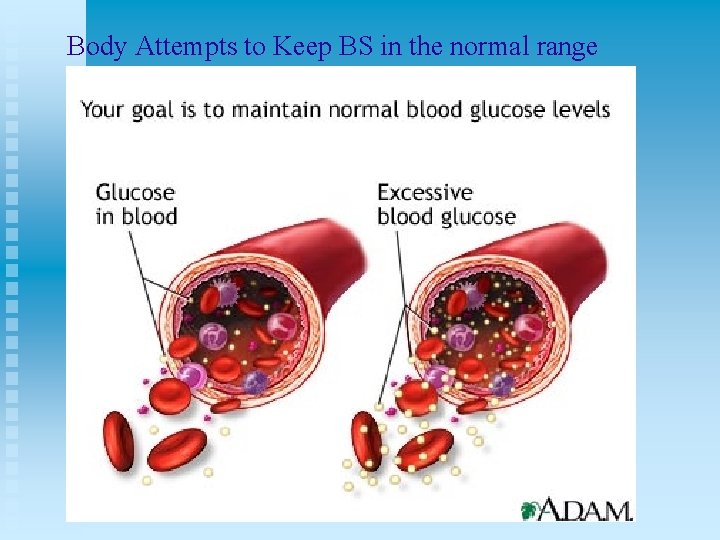
Body Attempts to Keep BS in the normal range

Effects of Insulin Deficit: FAT n Impaired FAT Metabolism u Increased lipolysis (breakdown of fats) u Decreased lipogenesis (formation of fat) Resulting in: t Free fatty acids (FFA) in serum • FFA become a major alternative energy source for tissues

Effects of impaired FAT metabolism n Impaired Fat Metabolism u Some excess FFA is converted to t u cholesterol & phospholipids FFA breaks down to t Ketone bodies • Ketone bodies are composed of ACIDS causing are composed of ketoacidosis

More Effects of impaired FAT metabolism u u Increased Serum Ketones as a result of impaired fat metabolism t “Ketosis” t • Measured in blood and/or urine If severe ketosis • Severe METABOLIC ACIDOSIS coma Severe Long-term effects of high serum lipids t RAPID onset of atherosclerosis and its complications • 2 out 3 diabetics die from stroke or heart attack

Effects of Insulin Deficit: PROTEIN n Impaired Protein Metabolism u Body unable to store protein u Increased protein catabolism u Cessation of protein synthesis
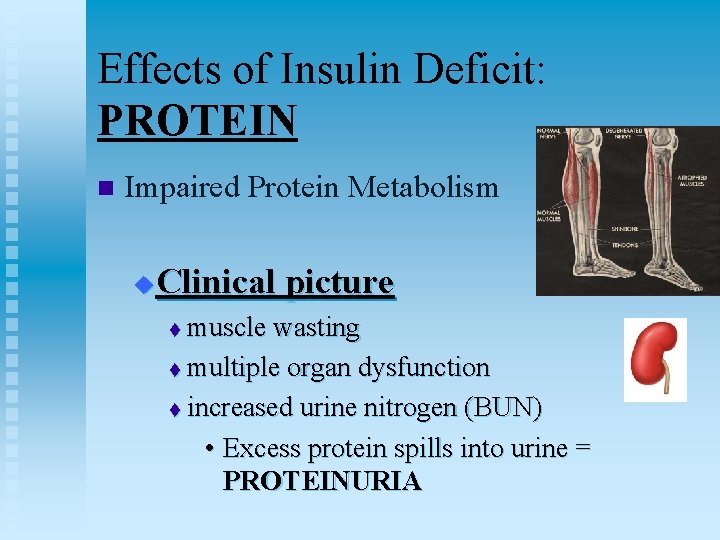
Effects of Insulin Deficit: PROTEIN n Impaired Protein Metabolism Clinical picture u muscle wasting t multiple organ dysfunction t increased urine nitrogen (BUN) • Excess protein spills into urine = PROTEINURIA t
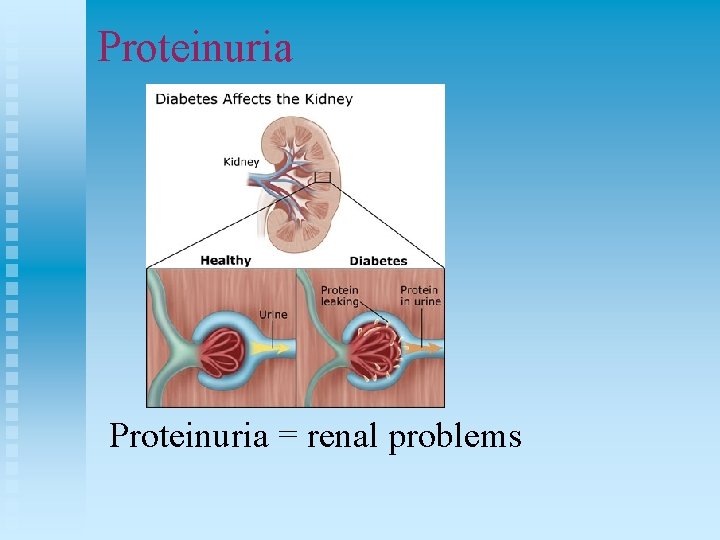
Proteinuria = renal problems

Effects of Insulin Deficit n Fluid & Electrolyte Imbalance u HYPEROSMOLARITY u u t u Increased serum glucose levels causes increased plasma OSMOTIC pressure WATER FOLLOW GLUCOSE Fluids shifts (pulled) into intravascular compartment • this increased fluid causes urination/POLYURIA) Intra. CELLULAR dehydration results in t thirst/ POLYDIPSIA

Clinical Picture: insulin deficit u GLYCOSURIA - excretion of sugar in urine - excretion of t Occurs when hyperglycemia increases beyond what kidneys can reabsorb t Positive urine dipstick t ACETONES in the urine (causes acidosis)
Clinical picture with insulin deficit: the 3 P’s u POLYPHAGIA --increased hunger R/T catabolism of fat and protein, and relative cellular starvation t u POLYURIA – increased urination t t t u Due to osmotic diuresis Excretion of excessive water Loss of electrolytes -- K+, Na+, Cl-, others POLYDIPSIA -- excessive thirst t As person becomes dehydrated increased serum osmolarity - excessive urination triggers thirst

Diabetes Mellitus n n Meaning: u diabetes (Greek for "passing or running through of sugar. ") u mellitus (Latin for honey or sweet). Definition of DM u A complex metabolic disorder in which the person has either an A ABSOLUTE or RELATIVE insulin deficit u Pancreas secretes either no insulin or not enough insulin u Is a disease of the endocrine pancreas u Two major forms: type 1 and type 2

Incidence and morbidity of diabetes in United States n n n n n Dramatic increase in diabetes in this country. … 23 million Americans now have diabetes 7% of the entire population have DM 29% of hospitalized patients have DM 57 million have pre-diabetes About 1/3 of these do not even know they have DM 44% fail to achieve ADA target control Leading cause of heart failure, new blindness, and amputations Each year 15% will develop a foot ulcer In 2004, 71, 000 nontraumatice amputations were performed on people with DM n n n n 7 th leading cause of death 10% will die from stroke each year 100, 000 will go on dialysis each year Type I constitutes about 5 -10% of the total cases Type II constitutes the remaining 9095% of cases Most people with type II have had the disease about 10 years before they are diagnosed Significant increase in the number of children diagnosed with type II. Studies have shown that good glycemic control can prevent or delay disease progression
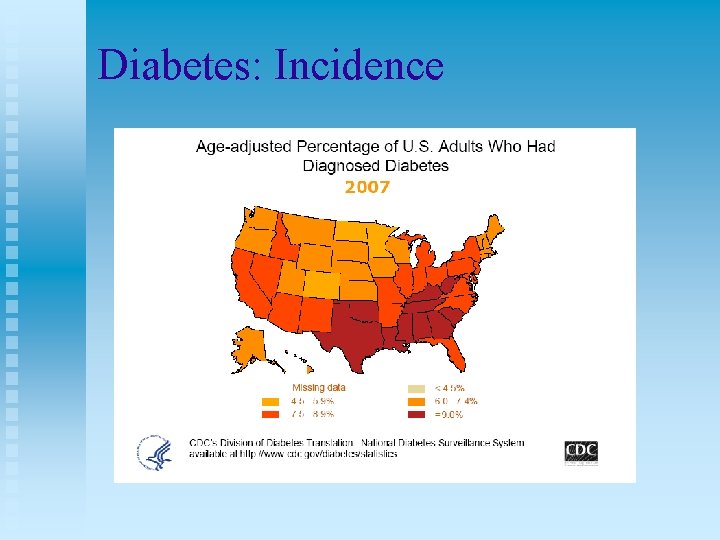
Diabetes: Incidence
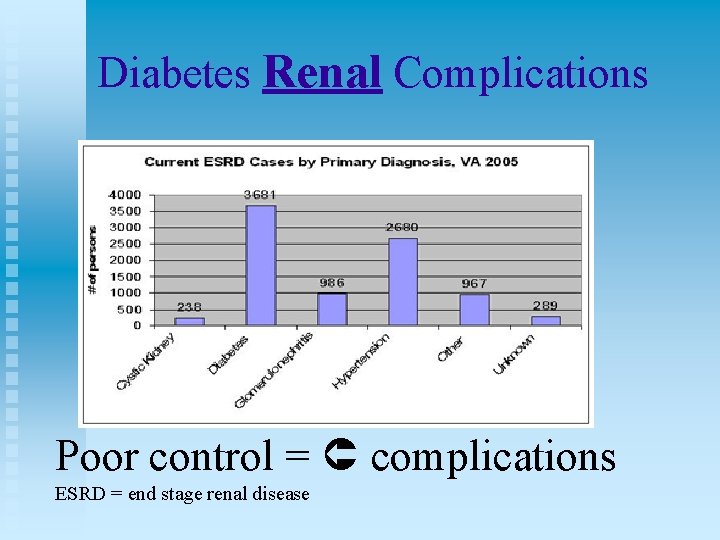
Diabetes Renal Complications Poor control = complications ESRD = end stage renal disease
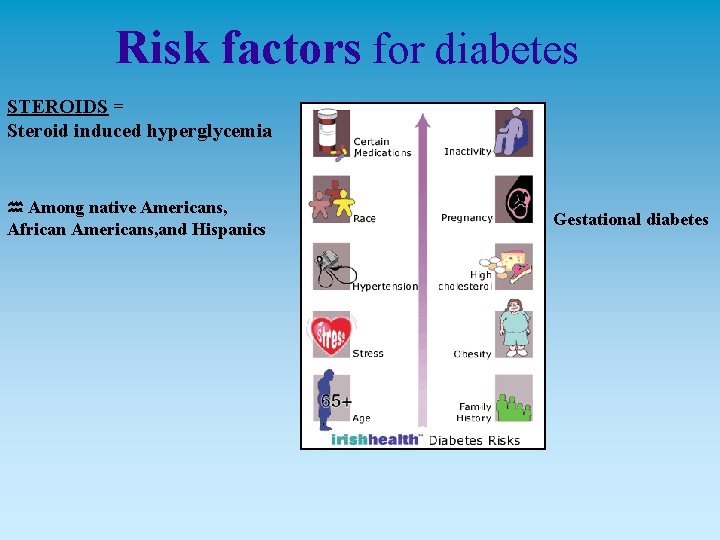
Risk factors for diabetes STEROIDS = Steroid induced hyperglycemia Among native Americans, African Americans, and Hispanics Gestational diabetes

What is the normal fasting glucose level? n Normal fasting glucose 60 -99 mg/dl FPG = Fasting plasma glucose FBS = Fasting blood sugar FSBS = finger stick blood sugar

How high does the blood sugar have to be to diagnose diabetes? n FBG of 126 or greater on 2 or more occasions = diabetes

Can you name these celebrities who have Diabetes?

Pre-diabetes n Is characterized by glucose levels higher than normal but not high enough to be classified as diabetes n FPG of 100 -125 (normal fasting should be less than 100) u n Remember normal FBG is 60 -99 and diabetes is FBG 126 or higher PREDIABETES is generally ASYMPTOMATIC u People have it and don’t even know it is present u Meanwhile it is believed that this “pre-diabetes” state is causing vascular damage to vital organs such as heart, kidneys, brain

Impaired glucose tolerance n Pre-diabetes is also known as “IMPAIRED GLUCOSE TOLERANCE” u Glucose levels do not return to normal as quickly as they should after glucose/CHO consumption n New trend is to identify these people and treat during the prediabetic stage with “insulin sensitizing” agents to help the glucose get OUT OF SERUM and INTO THE CELL where it can be utilized.

New recommendations from the ADA (2010) Prediabetes = HA 1 c of 5. 7 – 6. 4 Diabetes = HA 1 c 6. 5 or higher The ADA recommends that most people with diabetes maintain a goal of keeping A 1 c levels at or below 7 percent in order to properly manage their disease.

Gestational Diabetes n Development of diabetes during pregnancy u Will have a 50% chance of developing diabetes mellitus later in life n Also, moms who deliver babies weighing over 9 pounds have increased risk to develop DM
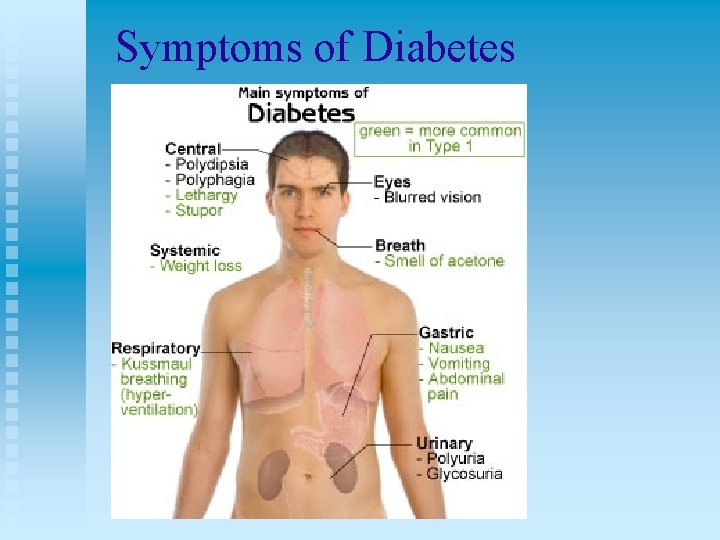
Symptoms of Diabetes

Olivia Type 1 Diabetes Mellitus n n Old names u Insulin dependent diabetes mellitus t IDDM t Juvenile onset diabetes Defined u An ABSOLUTE lack of endogenous insulin t The pancreas is producing little to NO insulin

Etiology n May result from combination of factors u Genetic predisposition diabetogenic genes u u Some triggering event (e. g. , an environmental agent, viral illness) Immunologically mediated ß-cell destruction (autoimmune)
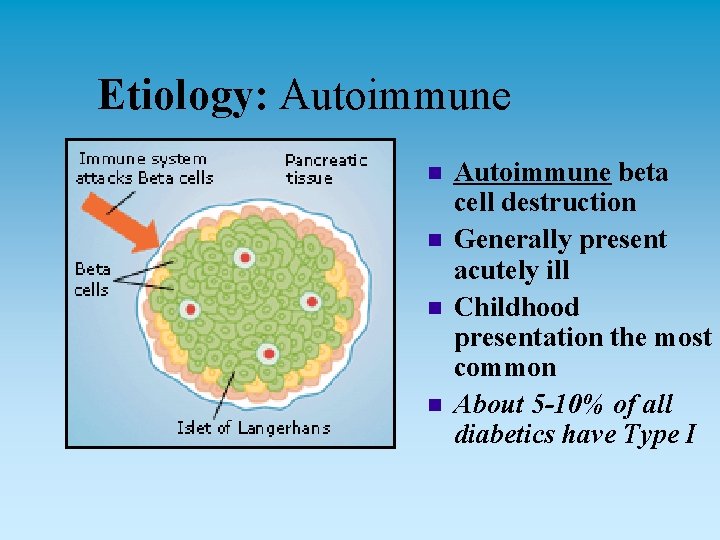
Etiology: Autoimmune n n Autoimmune beta cell destruction Generally present acutely ill Childhood presentation the most common About 5 -10% of all diabetics have Type I
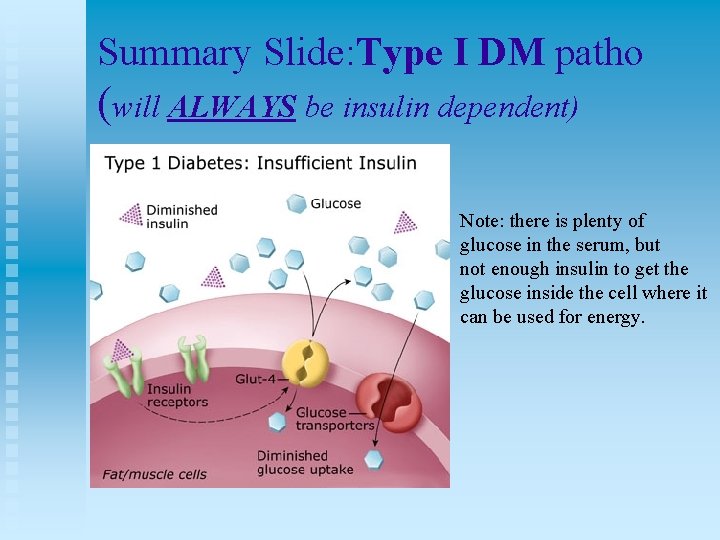
Summary Slide: Type I DM patho (will ALWAYS be insulin dependent) Note: there is plenty of glucose in the serum, but not enough insulin to get the glucose inside the cell where it can be used for energy.

Type 2 Diabetes Mellitus n Definition u A RELATIVE insulin deficiency n Different underlying problems than type 1 diabetes mellitus n Fasting hyperglycemia that develops regardless of availability of insulin u Insulin may be there but it cannot get into cells n Old names: u adult onset diabetes u non-insulin dependent diabetes u NIDDM

Three metabolic abnormalities associated with Type 2 DM 1. Impaired insulin secretion (too little insulin made by pancreas) Cause: ß-cell exhaustion due to overuse 2. Peripheral insulin resistance (insulin can’t get into cells) Cause: R/T increased visceral fat 3. Increased hepatic glucose production Cause: R/T impaired suppression of glucose production in liver **ANTI-DIABETIC DRUGS WILL TARGET ONE OR MORE OF THESE ABNORMALITIES

Insulin Resistance n Insulin resistance is a key metabolic feature of type 2 DM u A patient with Type 2 DM can produce 5 -8 X as much insulin/day as non IR person n Hyperinsulinemia enhances: u Renal tubule reabsorption of SODIUM, leading to an increase in B/P u Endothelial dysfunction via reduced nitric oxide production leading to: t Vasoconstriction, platelet aggregation, microalbuminuria • increasing the risk for HTN, AMI and STROKE, and KIDNEY FAILURE

HTN, CVD, Insulin Resistance n Hyperinsulinemia effects: u Increased vascular smooth muscle proliferation u Greater responsivity to angiotensin II u Enhanced sympathetic activation t t t B/P free fatty acid levels myocardial oxygen consumption myocardial ischemia proarrhythmic effects
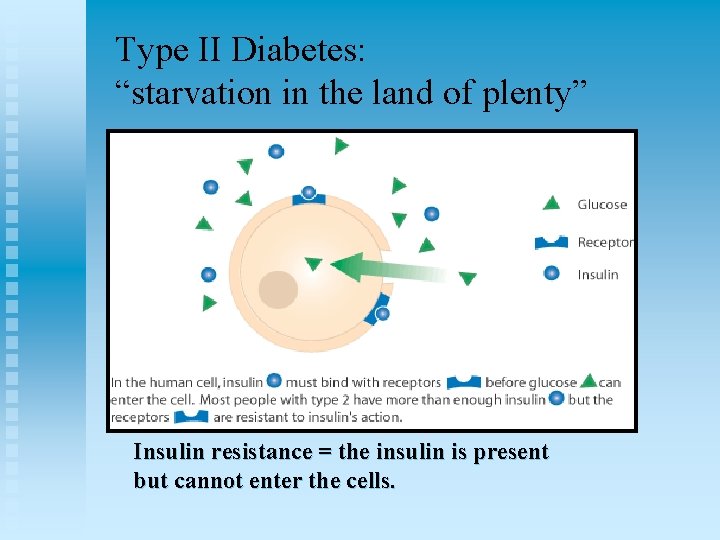
Type II Diabetes: “starvation in the land of plenty” Insulin resistance = the insulin is present but cannot enter the cells.
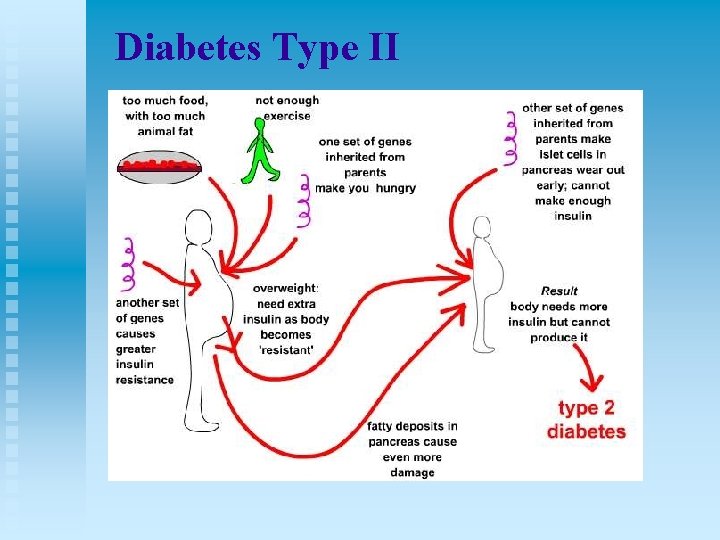
Diabetes Type II
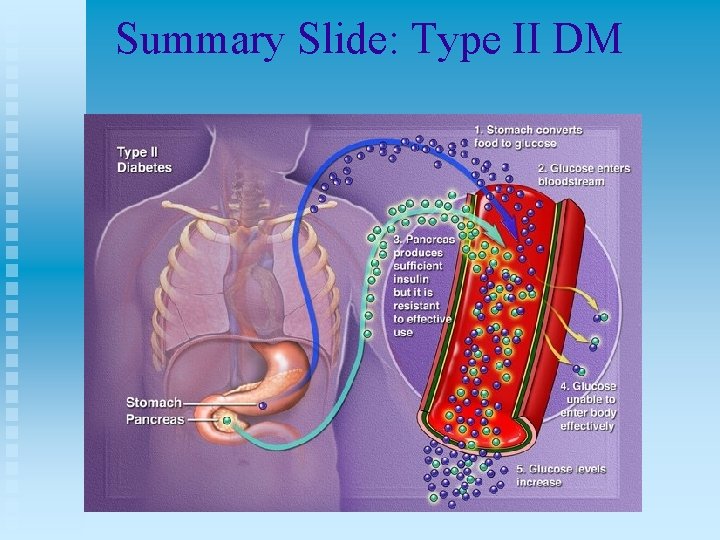
Summary Slide: Type II DM

Acute Complications Diabetic Ketoacidosis (DKA) = Type I DM complication u A type of metabolic acidosis associated with diabetes produced by excessive levels of KETONES in the body t Develops when ketone production exceeds cellular use and renal excretion t Often associated with increased stress ((physical or emotional) u Associated primarily with type 1 diabetes

Diabetic Ketoacidosis n Three major metabolic derangements u Hyperglycemia u Ketosis u Metabolic acidosis ( increased acetones in urine and blood) Positive urine dipstick

Diabetic Ketoacidosis n Diagnosis u Hyperglycemia t (blood glucose > 300 mg/d. L) u Low bicarbonate (< 15 m. Eq/L) u Low p. H (< 7. 3) u Ketonemia (positive ketones or acetones in blood) u Ketonuria – ( positive ketones or acetones in urine)

Diabetic Ketoacidosis n Clinical Manifestations u u Rate of onset t rapid - 1 to 24 hours t Polyuria, polydipsia, polyphagia Dehydration (FVD) t warm, dry skin t tachycardia, weak, thready pulse t acute weight loss t hypotension

Diabetic Ketoacidosis n Clinical Manifestations u Ketoacidosis t KETONE BREATH -- sweet, fruity odor t Nausea and vomiting, anorexia t Mental status changes • lethargy, fatigue, stupor, COMA t Compensatory responses • Kussmaul’s respirations – rapid, deep respirations

Summary: Diabetic Ketoacidosis

Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) = Type II complication n Characterized by u u n Serum osmolality of > 310 m. Osm/L (normal 195 -295) Serum glucose of > 600 mg/d. L Absence of ketoacidosis Depressed sensorium Associated with u Type 2 diabetes mellitus (most common)
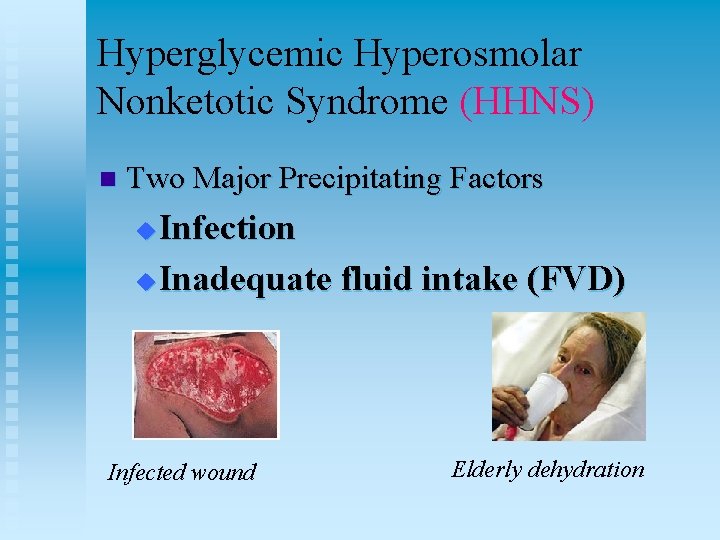
Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) n Two Major Precipitating Factors Infection u Inadequate fluid intake (FVD) u Infected wound Elderly dehydration

Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) n Pathogenesis u u Develop hyperglycemia r/t t acceleration of hepatic gluconeogenesis and decreased peripheral glucose utilization Do NOT develop ketoacidosis because t secrete moderate levels of insulin, which prevents use of FFA as energy source – so no significant ketone development

Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) n Pathogenesis u u u Extremely high glucose levels develop See very high serum osmolality --> t Blood Glucose levels of 600 or more! Pulls water from everywhere with resulting cellular dehydration

Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) n Clinical Manifestations u u Rate of onset: t Slow -- 24 hrs to 2 weeks Severe Dehydration t Dry skin & mucous membranes t Extreme thirst

Hyperglycemic Hyperosmolar Nonketotic Syndrome (HHNS) n More Clinical Manifestations u Neurologic manifestations t Depressed sensorium --> COMA t Seizures possible
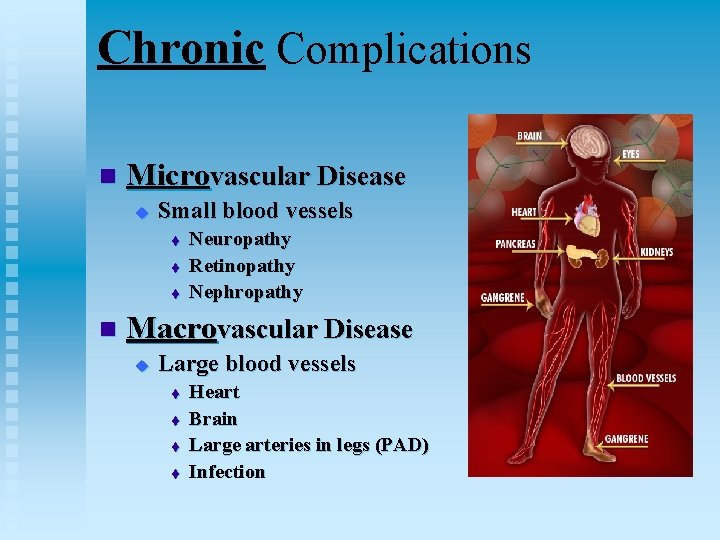
Chronic Complications n Microvascular Disease u Small blood vessels t t t n Neuropathy Retinopathy Nephropathy Macrovascular Disease u Large blood vessels t t Heart Brain Large arteries in legs (PAD) Infection

Microvascular Disease Seems to be related to duration of diabetes not the degree of glucose control n Associated with capillary membrane thickening u Results in microangiopathy t small blood vessel disease n Diabetic neuropathy – monofilament test
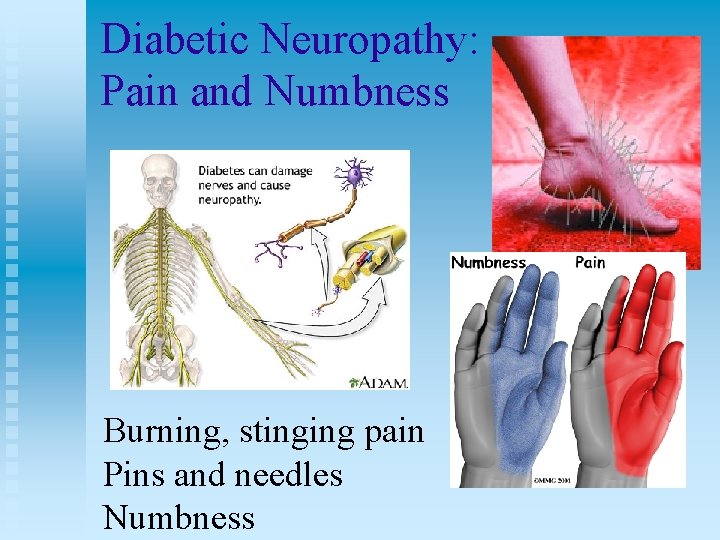
Diabetic Neuropathy: Pain and Numbness Burning, stinging pain Pins and needles Numbness
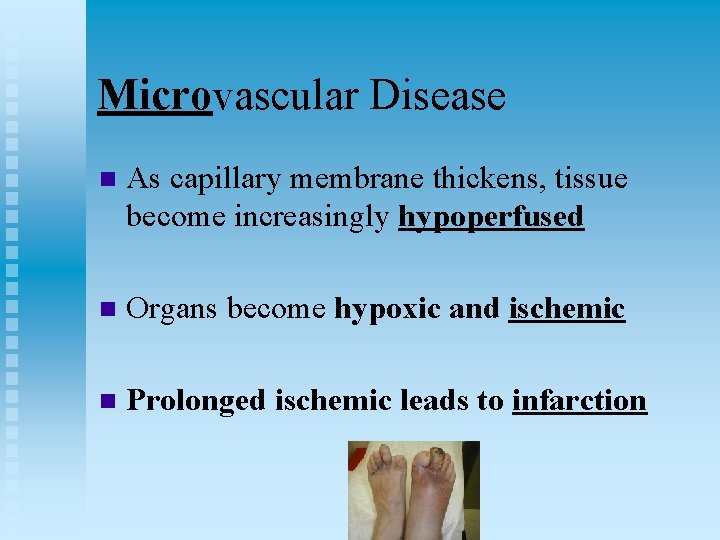
Microvascular Disease n As capillary membrane thickens, tissue become increasingly hypoperfused n Organs become hypoxic and ischemic n Prolonged ischemic leads to infarction

Microvascular Disease n Two major organs are involved (eyes & kidneys) u Eyes t Retinopathy • Major cause of blindness in US • Small vessels in retina become occluded, causing areas of infarction
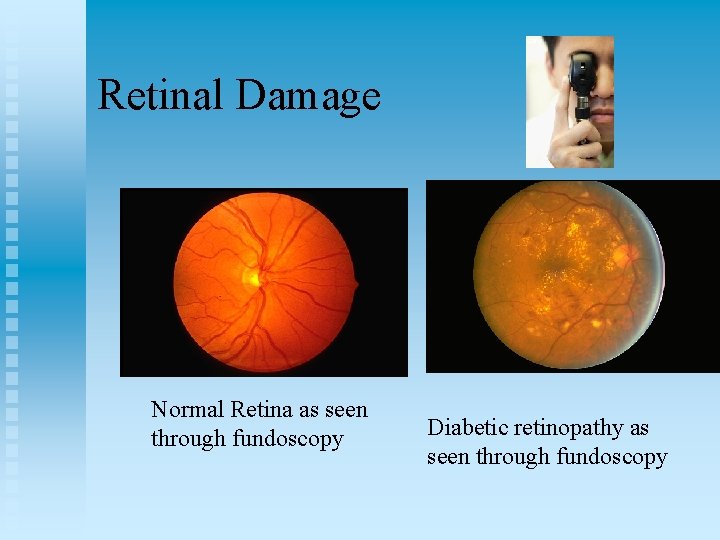
Retinal Damage Normal Retina as seen through fundoscopy Diabetic retinopathy as seen through fundoscopy
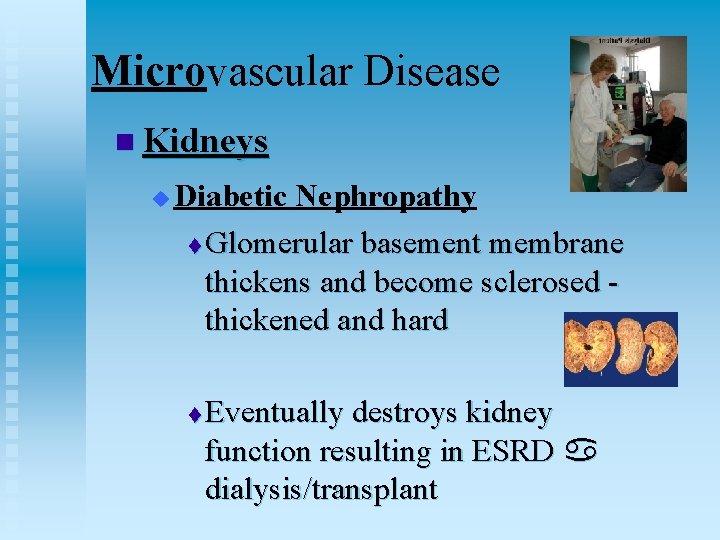
Microvascular Disease n Kidneys u Diabetic Nephropathy t Glomerular basement membrane thickens and become sclerosed - thickened and hard t Eventually destroys kidney function resulting in ESRD dialysis/transplant

Macrovascular Disease n More associated with type 2 DM n Atherosclerosis u thickening, hardening of large arteries n Related disorders u u Coronary Artery Disease (CAD) Peripheral Arterial Disease (PAD) Cerebrovascular accidents (CVA) Increased risk of infection

Why an Increased Risk of Infection? n Diminished early warning system u R/T impaired vision & peripheral neuropathy t May not see/feel breaks in skin integrity n Tissue hypoxia u When skin integrity is broken - t may not be able to get sufficient O 2 & nutrients to heal

Why an Increased Risk of Infection? n Rapid proliferation of pathogens u Once inside of body - tend to proliferate rapidly. Why? t increased glucose in serum & tissue t decreased circulation hurts WBC response n Impaired WBCs t Develop abnormal WBCs-- less effective
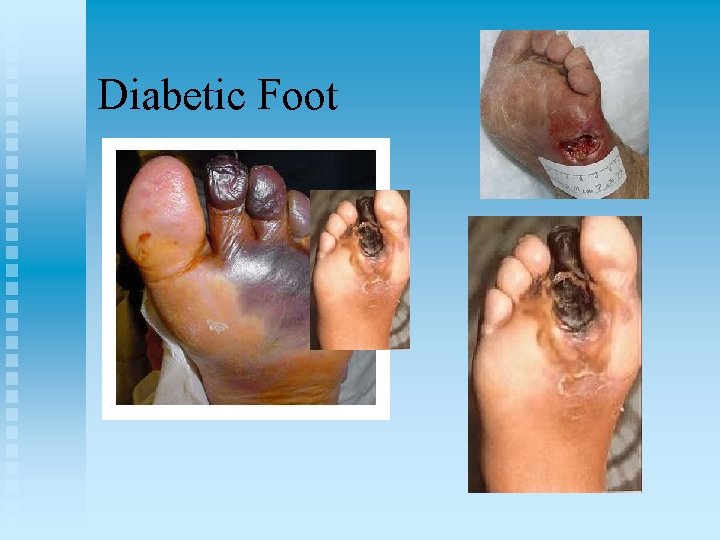
Diabetic Foot
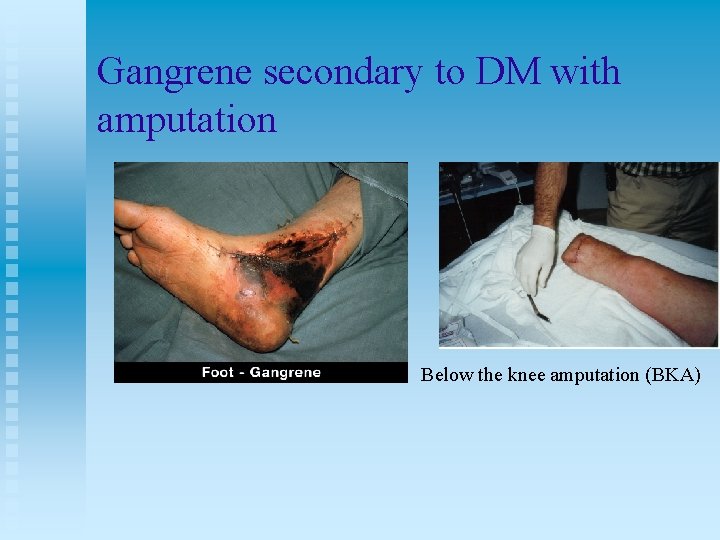
Gangrene secondary to DM with amputation Below the knee amputation (BKA)

Patient Education: You CAN make a difference in patient outcomes
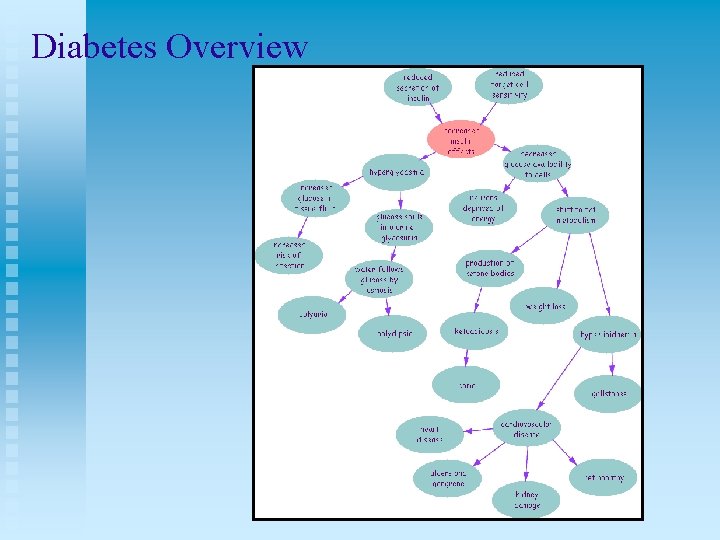
Diabetes Overview

THE END
- Slides: 72