Diabetes Mellitus Part II Treatment Acute Complications Chronic

Diabetes Mellitus (Part II) Treatment Acute Complications Chronic Complications Patient Teaching
Treatment Drug Therapy: Insulin Oral Agents Nutritional Therapy Exercise Pancreas Transplant

Treatment • The goal of any treatment for Diabetes: PReduce symptoms PPromote well-being PPrevent acute complications PPrevent or delay the onset and progression of long -term complications • Above goals can only be met by patient maintaining blood glucose levels at or near normal!

Insulin Therapy (Exogenous Insulin) • Patients with Type 1 Diabetes always require Exogenous insulin (insulin from a source outside the body) • Type 2 Diabetics may not need any insulin PBlood Glucose Levels can be controlled by diet & exercise alone PMay need insulin eventually due to chronic and progressive nature of the disease

Types of Insulin • • No longer made from beef or pork pancreas Only human insulin is used today Human insulin made from bacteria or yeast cells Insulins differ in regard to: POnset PPeak action PDuration • Characterized according to the amount of time they need to take effect • Read the label carefully êSee Insulin Comparison Chart

Insulin Therapy • Specific properties of each type of insulin are matched with the patient’s diet and activity • Can range from one injection per day to several injections of various types of insulin • Most closely resembles endogenous insulin production: PBasal-bolus regimen • The regimen chosen should be mutually selected by the patient and the HCP • Criteria for selection are based on the desired and feasible levels of glycemic control and the patient’s lifestyle

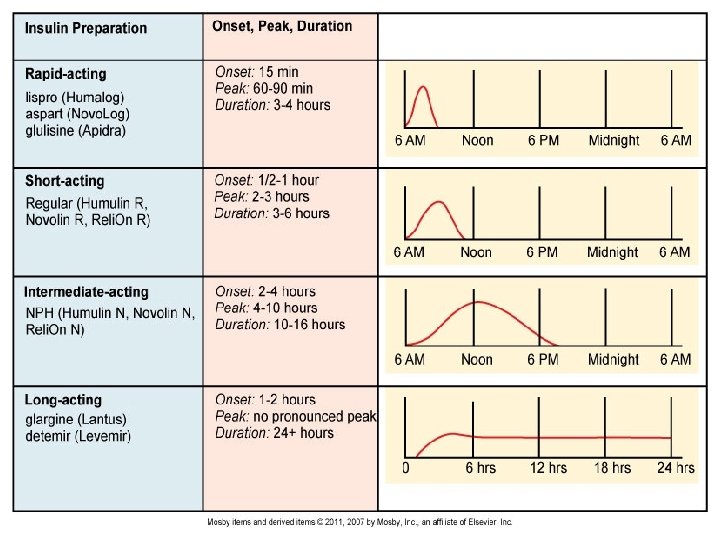
Fast/Rapid Acting Insulin Rapid-acting • Mealtime Insulin – Bolus • Used to control post-meal blood glucose levels • Rapid Acting Insulin: Onset = 15 minutes • Should be given 15 minutes before a meal üHumalog üNovolog Short acting Regular Insulin: Onset = 30 -60 minutes P “Regular” • Should be injected 20 -30 minutes before a meal

Intermediate Acting Insulin • NPH Insulin POnset 2 -4 hours PPeaks 4 -12 hours PDuration - 16 -24 hours PGenerally given twice a day before meals

Long Acting (Basal) Background Insulin • Long-acting/basal (background) insulin to control blood glucose levels between meals and overnight • Provides 24 hour steady and continual background insulin to keep blood glucose levels at a constant or controlled level PLantus PLevemir • No Peak PRisk for hypoglycemia greatly reduced
Long Acting Insulin (cont’d) • Lantus and/or Levemir: PGiven once in the morning or at bedtime PCannot be mixed (in syringe) with other insulins PCannot be pre-filled

Combination Insulin • Insulins can generally be mixed in the same syringe • Some Insulins Come Pre-mixed PNovolin 70/30 mix P 70% NPH – 30% Novolin Regular PNovolog 70/30 mix P 70% NPH – 30% Novolog Regular PHumulin 50/50 mix PHumalog 75/25

Administration of Insulin • Insulin is inactivated by gastric juices – cannot be taken orally PInjection PInsulin Pen PInsulin Pump PInhaled Insulin

Administration of Insulin: Subcutaneous Injection • Gently rotate insulin in hands to warm • Mixing Insulins for Injection PLantus/Levemir cannot be mixed PDon’t mix insulins from different manufacturers • Regular/NPH Insulin mix: PDraw up Regular insulin first, then add NPH
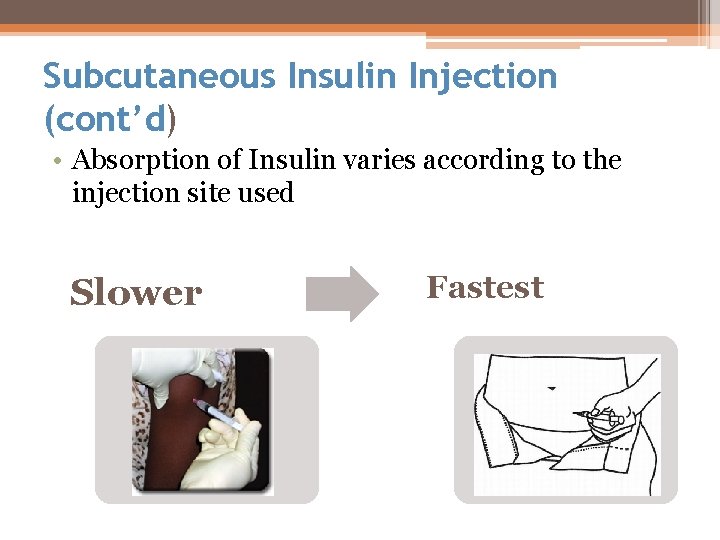
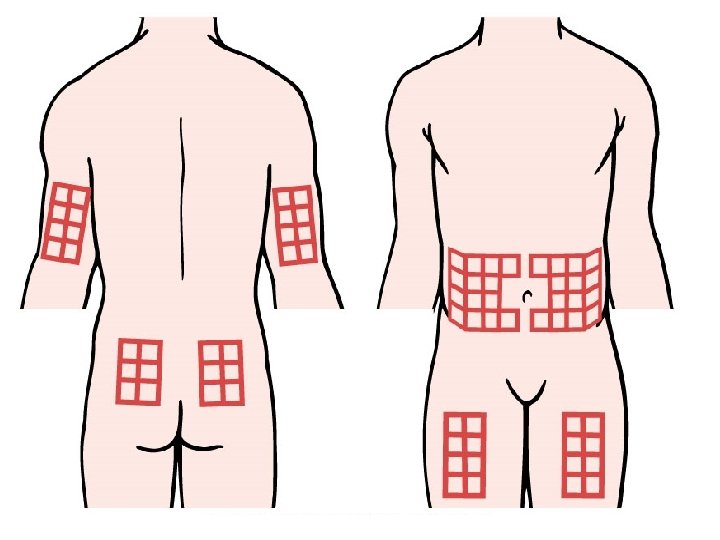
Subcutaneous Insulin Injection (cont’d) • Absorption of Insulin varies according to the injection site used Slower Fastest
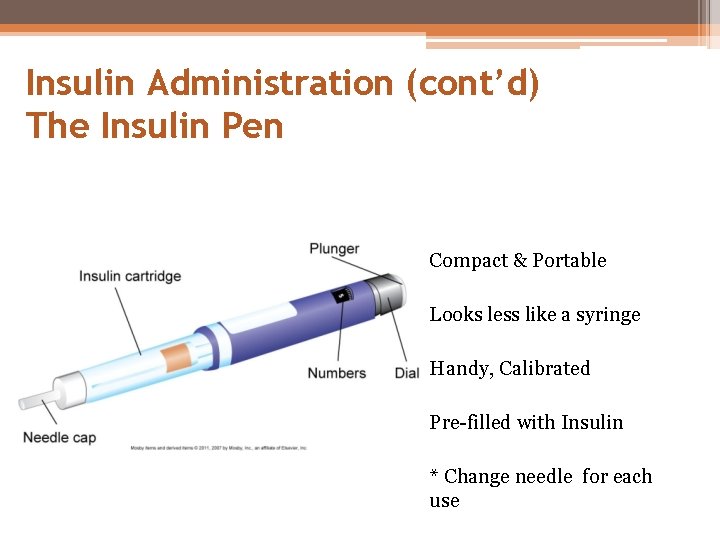
Insulin Administration (cont’d) The Insulin Pen Compact & Portable Looks less like a syringe Handy, Calibrated Pre-filled with Insulin * Change needle for each use

Insulin Pump Can be worn on belt or clothing Tubing inserted into subcutaneous tissue in abdomen Site must be changed every 3 days Can deliver basal rate, short and long acting insulin User programs according to exercise, diet, etc. )
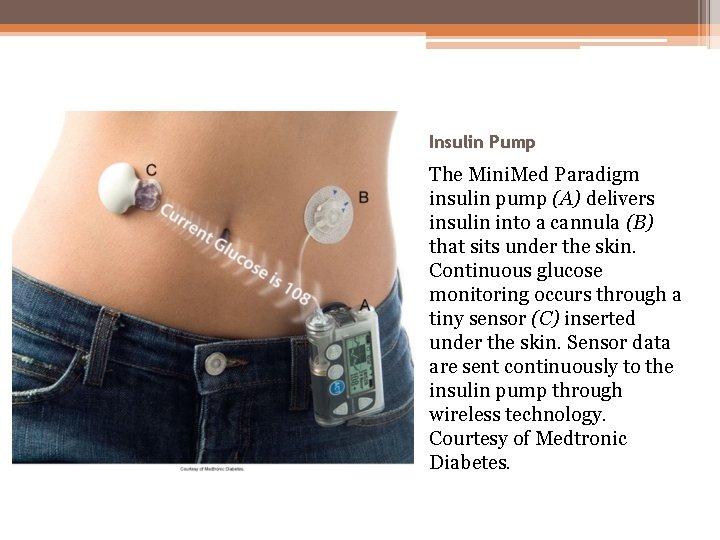
Insulin Pump The Mini. Med Paradigm insulin pump (A) delivers insulin into a cannula (B) that sits under the skin. Continuous glucose monitoring occurs through a tiny sensor (C) inserted under the skin. Sensor data are sent continuously to the insulin pump through wireless technology. Courtesy of Medtronic Diabetes.
Inhaled Insulin (Exubera) • Alternative to injectable insulin • Rapid Acting; replaces short-acting ‘coverage’ insulins • Inhaled before meals • Usually added to longer acting insulins for type 1 diabetics • Type 2 diabetics: Alone or with any combination of prescribed insulins • Contraindications: ü ü Smoker Quit smoking within last 6 months Asthma PFTs before prescribed

Problems with Insulin Therapy • Allergic Reactions PLocal; itching, burning usually due to additives PTrue insulin allergy is rare, but can be anaphylactic • Lipodystrophy: Atrophy of subcutaneous tissue PPrevented by rotation of sites PMay result in poor absorption of insulin • Somogyi Effect • Dawn Phenomenon

Somogyi Effect • Somogyi Effect is a ‘rebound’ effect POverdose of insulin induces hypoglycemia PUsually occurs during hours of sleep • Normal/elevated blood glucose at bedtime, a decrease at 2 -3 am hypoglycemic levels, and increase caused by the production of counterregulatory hormones released, producing rebound hyperglycemia • The danger the morning BGL can be high in response to the counterregulatory hormones and the MD may increase the insulin dose

Dawn Phenomenon • Similar to Somogyi • Relatively normal glucose until about 3 am then the glucose level begins to rise. • Hyperglycemia is present on awakening in the morning due to the release of counterregulatory hormones in the pre-dawn hours. PPossibly caused by growth hormone PAffects all diabetics at one time or another, more severe when growth hormone is at it’s peak o Adolescence and young adulthood üCareful monitoring of insulin, snacks and BGLs

Oral Drug Therapy êOral Agents are NOT oral forms of insulin • Oral agents work to improve the mechanisms by which insulin and glucose are produced and used by the body – they work on the 3 defects of type 2 diabetes: 1. Insulin resistance 2. Decreased insulin production 3. Increased hepatic glucose production • May be taken in combination with each other or with insulin to achieve BGL targets

Oral Hypoglycemic Agents • Sulfonylureas: increases insulin production from the pancreas • Drug of choice in Type 2 Diabetes because of decreased chance of hypoglycemia o glipizide (Glucotrol, Glucatrol XL) o glyburide (Micronase, Dia. Beta, Glynase) o glimiperide (Amaryl) êInteracts with oral anticoagulants

Oral Hypoglycemics (cont’d) • Biguanides: Primary action is to reduce glucose production by the liver o Metformin (Glucophage) • Can be used alone or with other oral agents or insulin to treat Type 2 Diabetes • Also used in prediabetics to prevent type 2 diabetes • Does not promote weight gain ê Cannot be taken with contrast dye!

Oral Hypoglycemic Agents (cont’d) • a -Glucosidase Inhibitors: (starch blockers) work by slowing down absorption of carbohydrates in the small intestine o Acarbose (Precose) o Miglitol (Glyset) • Taken with first bite of each meal • Most effective in lowering post-prandial BGLs

Oral Hypoglycemic Agents (cont’d) • Thiazolidinediones: a/k/a Insulin Sensitizers, work by improving insulin sensitivity, transport and utilization at target tissues o Pioglitazone (Actos) o Rosiglitazone (Avandia) • Most effective for people with insulin resistance üDo not cause hypoglycemia because they don’t increase insulin production êCan cause edema – do not use in patients with heart failure

Diabetes Treatment êThe Priority Nursing Considerations for any diabetic patient on Insulin or oral Hypoglycemic agents is êMonitor/prevent Hypoglycemia êHypoglycemia is an emergency and needs to be treated immediately

Nutritional Therapy Type 1 Diabetes Mellitus Type 2 Diabetes Mellitus • Meal planning based on patient’s usual food intake • Balance with insulin and exercise programs • Plan is developed with the person’s eating habits and activity pattern in mind • Emphasis is based on achieving glucose, lipid and blood pressure goals • Reduce total fat, simple sugars, carbohydrates • Space Meals • Weight loss of even 5 – 7% can improve glycemic control

Diabetes: Nutritional Therapy • The Cornerstone of Care for the patient with Diabetes êThe Goal (according to the ADA) is to assist people with diabetes to make good food choices and maintain healthy exercise habits that lead to: 1. 2. 3. 4. 5. ü Good Metabolic Control Maintain blood glucose levels at or near normal Achieve lipid profiles and BP levels Modify Lifestyle changes as appropriate Improve health through healthy food choices and physical activity Must address individual nutritional needs, personal and cultural preferences and respect the individual’s willingness to change

Patient Teaching (Nutritional Tx) • Nurses often assume responsibilities of teaching • Ideally: Diabetic teacher or interdisciplinary diabetes care team • Include PPatient’s family and significant others PCulture PTeach the person who does the cooking PCaloric intake

Patient Teaching: Exercise Therapy • Regular, consistent exercise is an essential part of diabetes and prediabetes management êExercise increases insulin receptor sites in the tissue and has a direct effect on lowering blood glucose levels PCan also decrease triglycerides, LDL cholesterol PCan increase HDL PCan reduce blood pressure PCan improve circulation

Exercise Therapy (cont’d) • Exercise can lower BGLs to dangerously low levels PSmall carbohydrate snacks can be taken 1 hour before, 1 hour after exercise PPatient should exercise and carry a fast acting carbohydrate • Exercise can also raise BGLs PThe body sometimes perceives the exercise as a stress PCounterregulatory hormones released, raising BGLs • BGLs should be monitored before, during & after when beginning an exercise regimen, especially if the patient formerly led a sedentary lifestyle

Monitoring Blood Glucose Levels • Self-Monitoring of Blood Glucose (SMBG) = a cornerstone of diabetes management • SMBG enables the patient to make selfmanagement decisions regarding PDiet PExercise PMedications • Important for detecting episodes of hyperglycemia and hypoglycemia • Teaching SMBG is an important nursing responsibility

Pancreatic Transplant • Treatment option for Type 1 Diabetics with poorly controlled BGLs PRare, usually not done alone PCan be done following kidney transplant to protect the new kidney from further damage from high BGLs PPancreas transplant only partially successful in reversing long-term damage PPatient must take life-long immunosuppressants

Acute Complications of Diabetes Mellitus Hypoglycemia Diabetic Ketoacidosis (DKA) Hyperosmolar Hyperglycemic Syndrome (HHS)

Hypoglycemia • Hypoglycemia occurs when there is too much insulin in proportion to available glucose in the blood. BGL drops to <70 êCommon Manifestations of hypoglycemia: PConfusion PIrritabililty PDiaphoresis PTremors PHunger PWeakness PVisual Disturbances

Hypoglycemia • The brain requires a constant supply of glucose in sufficient quantities to function properly, hypoglycemia can affect mental function • Manifestations of hypoglycemia can mimic alcohol intoxication • Untreated hypoglycemia can progress to loss of consciousness, seizures, coma, death

Low Blood Glucose Levels • Hypoglycemia may also result if high glucose levels are treated too aggressively and brought down too quickly • It is important to ascertain why the BGL dropped

Treatment of Hypoglycemia Conscious Patient Unconscious Patient êHypoglycemia is an emergency and needs to be treated immediately • Give the patient 15 -20 grams of quick acting carbohydrate ü 4 -6 oz Regular soda ü 8 -10 Candies ü 4 -6 oz Orange Juice • Repeat in 15 minutes if no improvement • Longer acting carbohydrate PCrackers with peanut butter or cheese ê Immediate notification of health care provider especially if symptoms do not subside • Subcutaneous or IM injection of 1 mg Glucagon • IV administration of 50 mls of 50% Glucose

Diabetic Ketoacidosis (DKA) • Also known as Diabetic Coma • Caused by: A profound deficiency of insulin and characterized by: Phyperglycemia Pketosis Pacidosis Pdehydration • Most likely to occur in Type 1 Diabetics, but sometimes occurs in Type 2 Diabetics during conditions of severe illness and/or stress

Diabetic Ketoacidosis (cont’d) • Ketones are the acidic by-products of fat metabolism • Ketosis (presence of ketones in the blood) alters the Ph balance causing metabolic acidosis • Ketonuria begins – ketone bodies are excreted in the urine • The kidneys use more water to eliminate the ketones – causes dehydration • The existing insulin deficiency causes proteins to break down and stimulates production of glucose (in the liver) leading to worsening hyperglycemia

Diabetic Ketoacidosis (cont’d) • The rise in glucose levels and lack of insulin make the blood glucose levels rise even further • With cell death, potassium is released from cell into the bloodstream -> hyperkalemia • Kidneys continue to excrete ketones – leading to a severe depletion of Potassium & other electrolytes

Diabetic Ketoacidosis • Acidosis causes nausea & vomiting which results in severe hypovolemia, possibly shock • Renal failure results from hypovolemic shock (which causes retention of ketones & glucose and the acidosis progresses)

Diabetes Ketoacidosis (cont’d) • Result: Patient becomes comatose as the result of dehydration, electrolyte imbalance and acidosis P Coma P Cardiac irregularities (due to hyperkalemia) P Renal insufficiency P Eventual death

DKA: Clinical Manifestations • Dehydration- Early signs include: PPoor Skin Turgor PDry mucous membranes PTachycardia POrthostatic Hypotension PLethargy, weakness • Severe Dehydration: PSkin dry & loose PEyeballs soft, sunken

DKA: Clinical Manifestations (cont’d) • Abdominal Pain accompanied by anorexia & vomiting • Kussmaul respirations (rapid, deep breathing associated with dyspnea) PThe body is attempting to reverse the metabolic acidosis through exhalation of excess Co 2. PAcetone noted on the breath v. Sweet, fruity breath odor v. Ketonuria

Management • Correct dehydration • Correct electrolyte loss • Acidosis

Hyperosmolar Hyperglycemic Syndrome • Formerly known as Hyperosmolar Hyperglycemic Non-Ketoacidosis (HHNK) • HHS is a life-threatening syndrome that can occur when the person is able to produce enough insulin to prevent DKA (and ketoacidosis) but not enough to prevent severe hyperglycemia, osmotic diuresis and extracellular fluid depletion.

DKA vs. HHS (HHNK) • DKA usually Type 1 Diabetics • HHNK usually Type 2 Diabetics PSeen more often in elderly with pre-existing cardiac or renal problems PUsually patient can produce enough insulin to avoid ketoacidosis but not enough to prevent profound hyperglycemia, dehydration and hyperosmolality • Risk factors • Clinical picture

Treatment DKA/HHS • IV Fluids • IV Insulin PRapid Acting Insulin PContinual drip • Electrolyte Replacement • Assessment of Mental Status PSafety • • • I & O’s Central Venous Pressure Monitoring (if indicated) Blood Glucose Levels ECG Monitoring Cardiovascular and Respiratory Status

Chronic Complications of Diabetes Mellitus Macrovascular/Microvascular Complications Diabetic Retinopathy Nephropathy Neuropathy Complications of Feet & Lower Extremities Integumentary Complications
Complications: Diabetes Mellitus Macrovascular Microvascular • Diseases of the large & medium size blood vessels • Exact cause unknown – related to the altered lipid metabolism -> atherosclerotic plaque formation PCerebrovascular PCoronary Artery PPeripheral Vascular • Diseases resulting from the thickening of the vessel membranes in the capillaries and arterioles in response to conditions of chronic hyperglycemia (Microangiopathy) PDiabetic Retinopathy PDiabetic Nephropathy PDermopathy o Diabetic Foot Ulcers

Macrovascular Complications • Adults with Diabetes have 2 -4 x increased risk of cerebrovascular and cardiovascular disease PGenetic risk not modifiable POther risk factors can be modified (obesity, smoking, HTN, high fat intake, sedentary lifestyle) PBlood Pressure Control significantly reduces the risk of microvascular complications PEye PKidney PNerves

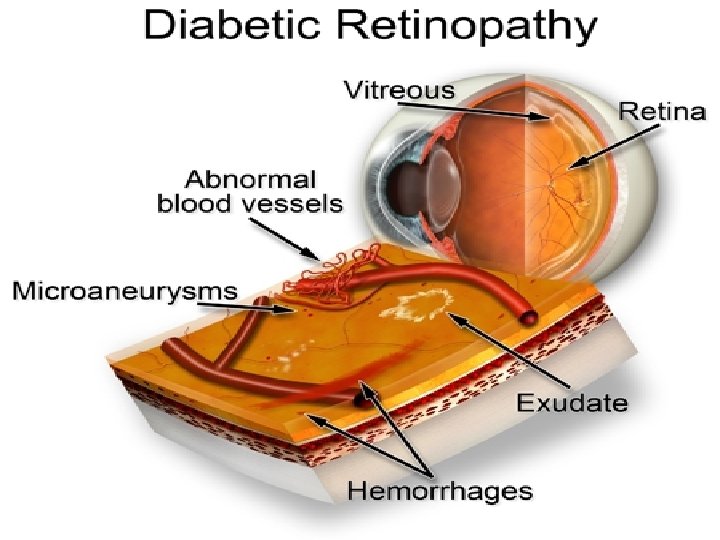
Diabetic Retinopathy • The process of microvascular damage to the retina as the result of chronic hyperglycemia in patients with diabetes • Subject to many visual complications • Assessment /Dx • Treatment: PPhotocoagulation (Laser) destroys the ischemic area producing the growth factors PVitrectomy: aspiration of fluid & fibers from the inside of the eye

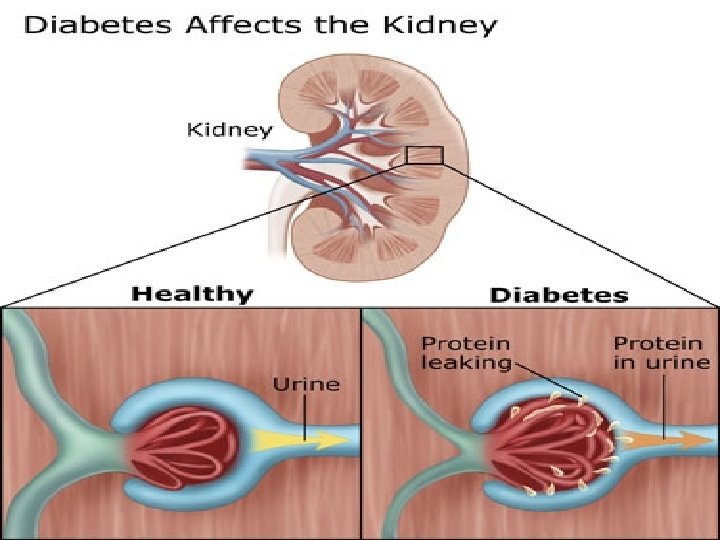
Diabetic Nephropathy • Definition: A microvascular complication associated with damage to the small blood vessels that supply the glomeruli of the kidney. • Leading cause of End Stage Renal Disease (ESRD) in the U. S. • Same risk, type 1 or type 2 Diabetics

Diabetic Nephropathy (cont’d) • The risk for kidney disease in diabetics can be significantly reduced when blood glucose levels are closely controlled to near-normal levels üTight blood glucose control critical • ACE inhibitor (Angiotensin Converting Enzyme) medications sometimes prescribed for diabetics because of the protective effect they have on the kidneys

Diabetic Neuropathy • 60 -70% of diabetics have some form of neuropathy POccurs with equal frequency in Type 1 & Type 2 • Can lead to loss of (protective) sensation in lower extremities PIncreases risk of complications that result in amputation of lower limbs o More than 60% of non-traumatic amputations are diabetics

Diabetic Neuropathy (cont’d) Sensory Neuropathy • Distal symmetric neuropathy PAffects hands and/or feet bilaterally ü Loss of Sensation: Can be complete or partial loss of sensation ü Pain: burning, crushing ü Abnormal sensations ü Paresthesias Tingling, burning or itching Autonomic Neuropathy • Autonomic Neuropathy: Can affect all body systems and lead to hypoglycemic unawareness, constipation or diarrhea or urinary retention PGastroparesis PCardiovascular abnormalities • Sexual dysfunction often the first manifestation ü Decreased libido ü Erectile dysfunction ü Vaginal infection • Neurogenic Bladder ü Urinary retention

Diabetic Neuropathy Management • diet high in sodium • avoid agents that stimulate ANS • wear elastic garments • frequent monitoring blood glucose • low-fat diet • increase gastric motility • anti-diarrhea medications • high fiber diet/hydration
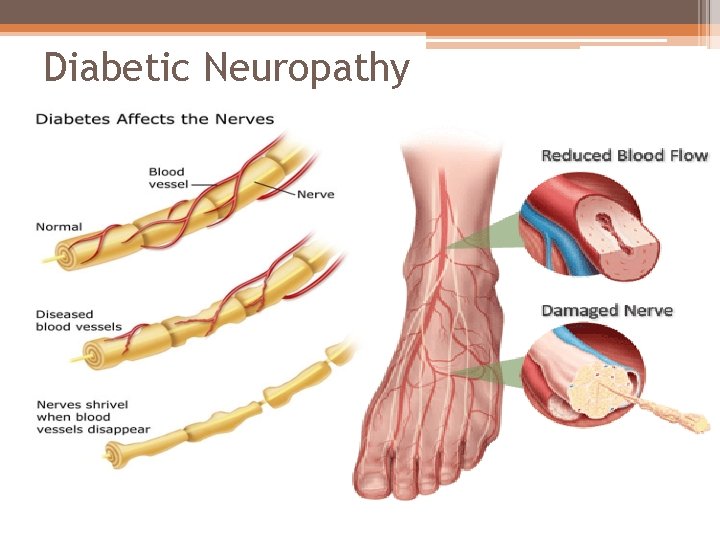
Diabetic Neuropathy

Complications of the Feet & Lower Extremities • Foot complications = the most common cause of hospitalization of the person with diabetes • “Diabetic Foot” is the result of both microvascular and macrovascular disease processes which frequently leads to: P Injury P Serious Infection (Cellulitis) P Amputation

Feet & Lower Extremities (cont’d) • Multifactoral Process: The Two Major Causes of Diabetic Foot Ulcers are: 1. Sensory neuropathy causes Loss of Protective Sensation (LOPS) ü Patient is unaware of injury o o o Repetitive injury Stepping on foreign objects when barefoot Ill-fitting footwear 2. Peripheral Arterial Disease ü Causes a reduction in blood flow to lower extremities ü Wounds take longer to heal o Increases the risk for infection
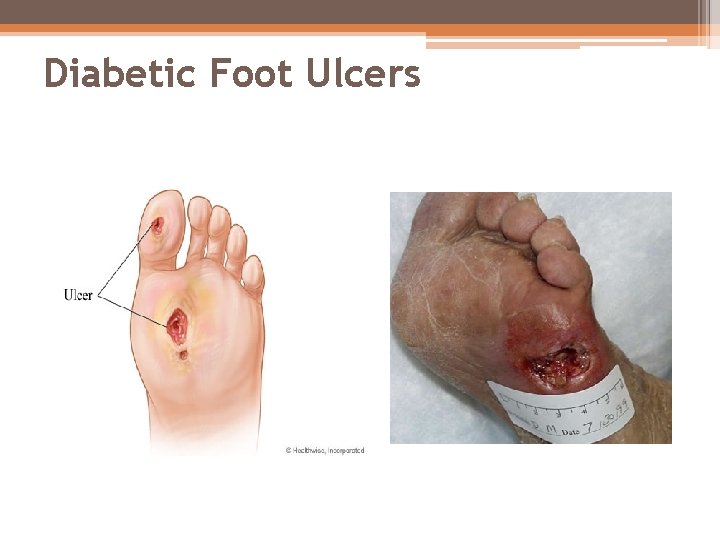
Diabetic Foot Ulcers
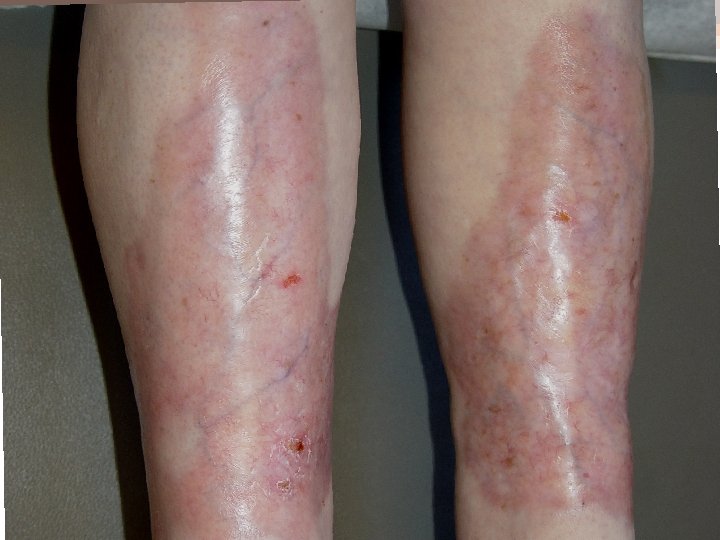
Integumentary • Diabetic Dermatopathy PRed-brown, flat-topped papules • Necrobiosis lipoidica diabeticorum PMay appear before other clinical signs & symptoms

Foot /Leg Problems Risk factors • Diabetes for more than 10 years • Older than 40 years • History of smoking • Decreased peripheral pulses • Decreased sensation • History of previous foot ulcers

Foot /Leg Problems • • • Daily assessment of the feet Examine feet at least once a year Assess for neuropathy Proper bathing/drying/lubricating Closed - toed shoes/socks Protect feet from hot/cold
- Slides: 70