Diabetes mellitus in children By Henry Cummings MBBS

Diabetes mellitus in children By Henry Cummings MBBS, FMCPaed Delsuth, Oghara

Pre-test 1. 2. 3. 4. 5. Dm is the commonest endocrine disorder in children Only type 1 dm occurs in children TIDm is a non progressive lowinsulin catabolic state Exogenous insulin replacement remains the only form of replacement therapy In managing DKA, always add kcl to the initial rehydrating fluid.

Childhood Diabetes mellitus �Definition �Types �Patho physiology �Clinical features �Modalities of management �Complications, short term, long term �Recent advancements �Conclusion

DEFINITION BY WHO: �DM is a metabolic disorder of multiple aetiologies characterised by chronic disturbances of carbohydrate, fat & protein metabolism, resulting from defects in insulin secretion, insulin action or both. �DM is the commonest endocrine disease in childhood & adolescence.

MAGNITUDE OF THE PROBLEM �Overall incidence 1 to 2 per 1000 school age children. �Estimated prevalence of childhood DM in 2003 were: � 430, 000 globally � 250, 000 live developing countries. � 63, 000 live in 58 poorest countries(least developed countries).

TYPES OF DM Type 1 DM(IDDM) �Beta cell autoimmune destruction �Absolute insulin deficiency �Requires insulin for survival �Accounts for over 90% of childhood DM �Peak age incidence 10 -12 years �Slight male predominance �Prone to ketosis

Type 2 DM (NIDDM) �Insulin resistance with relative deficiency OR �Secretory defect with or without resistance �Does not require insulin for survival �Strong genetic component �Not prone to ketosis �Acanthosis nigrans may be present �No islet cell antibodies �Associated with overweight teenagers

Maturity onset diabetes of the youth (MODY) Early onset of dominantly inherited type 2 DM Non- obese children No islet cell antibodies Family history in several generation Identified genetic mutations e. g mutations of glucokinase or hepatic nuclear factor 1 & 2 genes Non- ketotic Two (or at least one)family member diagnosed before age of 25 years

Neonatal Diabetes �hyperglycemia requiring insulin in the first 3 months of life �Rare condition 1: 400, 000 �Associated with IUGR � 50% of cases are transient �Associated with paternal isodomy & other imprinting defects of Chr 6 �In transient NND permanent DM may appear later in life

Secondary diabetes mellitus �May be associated with cystic fibrosis, hemochromatosis, drugs such as LAsparaginase
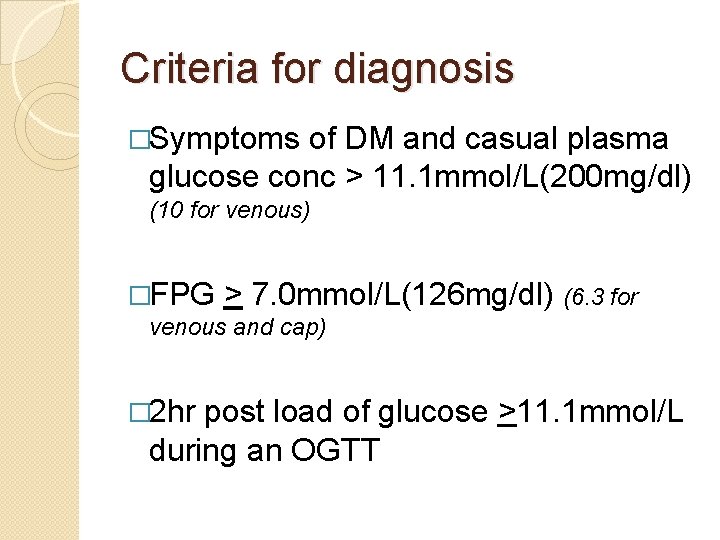
Criteria for diagnosis �Symptoms of DM and casual plasma glucose conc > 11. 1 mmol/L(200 mg/dl) (10 for venous) �FPG > 7. 0 mmol/L(126 mg/dl) (6. 3 for venous and cap) � 2 hr post load of glucose >11. 1 mmol/L during an OGTT

blood sugars �Normal RPG: �Normal FBS: �Hypoglycemia: ◦ Mild ◦ Severe ◦ Neonatal 70 – 140 mg/dl 70 – 100 mg/dl 40 – 70 mg/dl 40 mg/dl <50 mg/dl
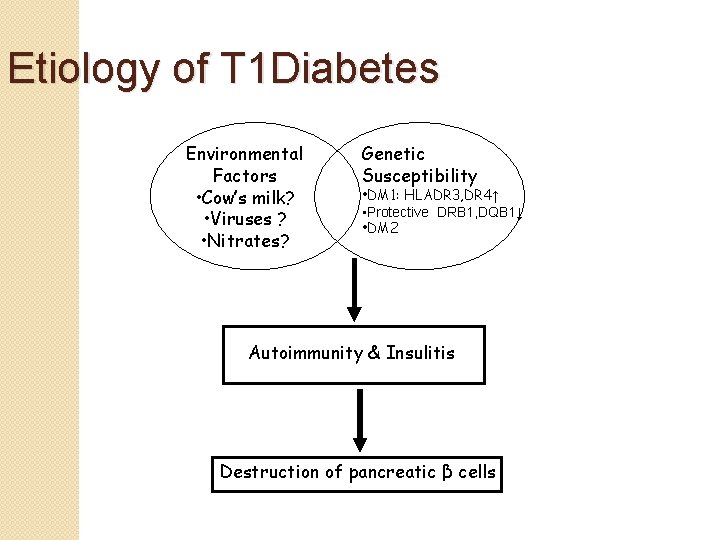
Etiology of T 1 Diabetes Environmental Factors • Cow’s milk? • Viruses ? • Nitrates? Genetic Susceptibility • DM 1: HLADR 3, DR 4↑ • Protective DRB 1, DQB 1↓ • DM 2 Autoimmunity & Insulitis Destruction of pancreatic β cells

Pathophysiology Insulin �essential to process CHO, fat, protein blood glucose levels by glucose uptake into muscle cells and fat cells �It � stimulates �inhibits � glycogenesis glycogenolysis the breakdown of fat to triglycerides, free fatty acids, and ketones. (lipolysis)

Pathophysiology Lack of Insulin � glucose oxidation in muscle & fat cells �Proteolysis & amino acid release �Glycogenolysis �all & gluconeogenesis result in Hyperglycaemia �Glucose intake still continues

Pathophysiology �The kidneys cannot reabsorb the excess glucose load, causing glycosuria, osmotic diuresis(polyuria), thirst, and dehydration. �Untreated pt excrete high glucose load causing polyphagia �Increased fat and protein breakdown leads to ketone production and weight loss.

Pathophysiology contd �Acidosis result from ketosis �Acidosis leads to renal excretion of K+ and �Na+ loss is due to osmotic diuresis & vomiting Po 4 �Hypokalemia is due to vomiting, osmotic diuresis & hyperaldosteronism �Coma likely due to ketosis, acidosis, dehydration & hyperosmolality
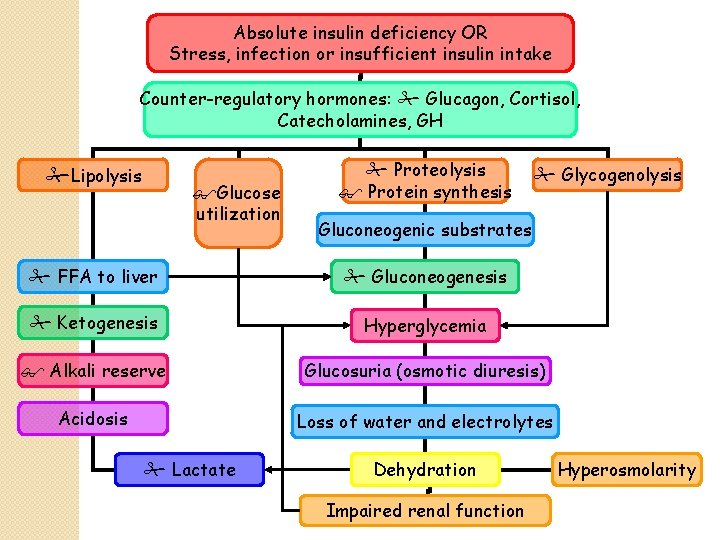
Absolute insulin deficiency OR Stress, infection or insufficient insulin intake Counter-regulatory hormones: Glucagon, Cortisol, Catecholamines, GH Lipolysis Glucose utilization Proteolysis Protein synthesis Glycogenolysis Gluconeogenic substrates FFA to liver Gluconeogenesis Ketogenesis Hyperglycemia Alkali reserve Glucosuria (osmotic diuresis) Acidosis Loss of water and electrolytes Lactate Dehydration Impaired renal function Hyperosmolarity

Phases of T 1 DM Preclinical diabetes 2. Presentation of DM 3. Partial remission or honeymoon phase 4. Chronic phase of lifelong dependency on administered insulin 1.

Preclinical DM �Occurs months to years preceding the clinical presentation of T 1 DM �Antibodies can be detected as markers of beta cell auto immunity: - GAD, IA, ICA, IA 2 etc �IVGTT
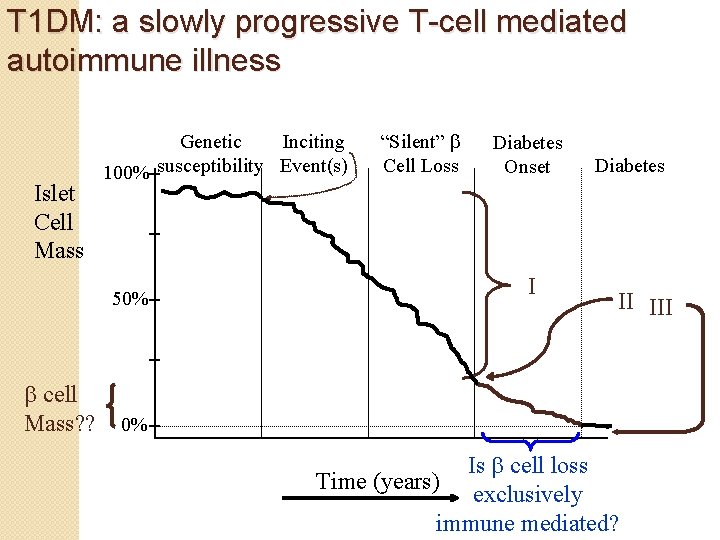
T 1 DM: a slowly progressive T-cell mediated autoimmune illness Islet Cell Mass Genetic Inciting 100% susceptibility Event(s) 50% cell Mass? ? “Silent” Cell Loss Diabetes Onset I Diabetes II III 0% Is cell loss Time (years) exclusively immune mediated?

Clinical presentation �Vary from non-emergency px( polydipsia, polyuria, weight loss, enuresis) to severe dehydration, shock and DKA �Onset may be acute, precipitated by an acute illness, or more chronic and insidious over weeks or even months.

Lab Investigations �Glucose �E levels &U �Ketones �C peptides �Islets cell antibodies

Other Lab Investigations �Lipids �Microalbumin �Thyroid �Hb fxn test A 1 c �fructosamine

Modalities of management �requires Multidisciplinary team �Insulin therapy �Diabetic education �Exercise �Diet �Psychological care �Monitoring �Others: - sick day mx, adjusting to school
Insulin therapy �Exogenous insulin replacement remains the only form of replacement therapy

The Basal/bolus Insulin Concept �Basal Insulin - Suppresses glucose production btw meals and overnight - 40% to 50% of daily needs �Bolus Insulin (meal time) - Limits hyperglycaemia after meals - Immediate rise and sharp peak at 1 hour - 50% -60% total daily insulin requirement for meals

Basal/bolus therapy regimens Intensive management: �MDI – Multiple Dose Insulin ◦ Once-daily IA or LA insulin usually given at night and 3 -ce daily SA or VA before each meal ◦ Mixed preps e. g. Mixtard, humulin 70/30 �CSII – Continuous Subcutaneous Insulin Infusion (Insulin pump therapy)

INSULIN THERAPY contd. �Twice daily regimen: �Split dose regimen (2/3 morning, 1/3 evening; 2/3 intermediate acting, 1/3 soluble). Aim at maintaining blood glucose within 80 -150 mg/dl, with the occurrence of as few hypoglycaemic episodes as possible.
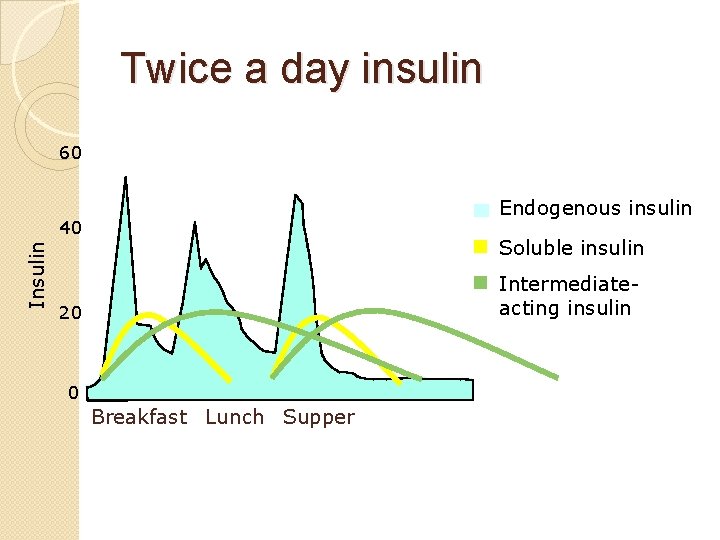
Twice a day insulin 60 Endogenous insulin Insulin 40 Soluble insulin Intermediateacting insulin 20 0 Breakfast Lunch Supper

DIET �Complex carbohydrates (CBHs) are preferred to simple refined CBHs. �Dietary regimen should be adjusted according to convenience of the family and school timings to ensure better compliance. �Total CBH content of the meal &snacks should be kept constant.

EXERCISE �Encourage �Insulin regular exercise. requirement may be lower, metabolic control improved and selfesteem & body image better in physically fit child.

SELF- CARE EDUCATION �Should include nature of illness, acute & chronic complications, insulin action, duration and timing, injection techniques, nutrition information, self blood glucose monitoring and urine ketone checks. �Education must be appropriate to child’s age & family educational background.

Monitoring �Monitoring of growth & development: the use of percentile charts is a crucial element in the care of children & adolescents with DM �Poor gain of height & weight, hepatomegaly and delayed puberty might be seen in children with persistently poorly controlled DM

Monitoring �Hb. A 1 c at least twice a year �Screening for long term complications

Partial remission (honeymoon) phase �Defined as when the patient requires < 0. 5 units of insulin/kg/day and has an Hb. A 1 c <7% �Due to partial recovery of the damaged beta cells �Commences within days or weeks of start of insulin therapy and may last for weeks to months �Ketoacidosis at presentation & young age reduces the likelihood of a remission phase

Complications �comprised of 3 major categories: 1. acute complications - reflect the difficulties of maintaining a balance between insulin therapy, dietary intake, and exercise. 2. long-term complications 3. complications caused by associated autoimmune diseases

ACUTE COMPLICATIONS �Hypoglycaemia �Diabetic ketoacdosis �Infections

HYPOGLYCAEMIA �Defined as blood glucose level < 60 mg/dl (3. 3 mmol/L). For preschool children, values below 70 mg/dl (3. 9 mmol/L) should be a cause for concern. �Severe episodes occur 10 -25% of pts per year �Commonest 1 DM acute complication of Type

WHY WORRY ABOUT HYPOGLYCAEMIA? Recurrent severe hypoglycaemia can lead to: �Hypoglycaemia unawareness(25% of DM pts) �Epilepsy �Learning difficulty �Death (accounts for 4% of deaths in DM as a result of unintentional trauma).

Diabetic ketoacidosis �creates a life-threatening medical emergency. �is the most important cause of mortality and severe morbidity in children with diabetes, particularly at the time of first diagnosis. �Early recognition and careful management are essential if death and disability are to be avoided.

Diagnosis � 3 cardinal features: 1. Hyperglycemia - >200 mg/dl(11. 1 mmol/l) 2. Ketonuria >5 mmol/l, ketonemia 3. Venous ph<7. 3 or metabolic acidosis < 15 mmol/l � Clinical features ◦ Severe dehydration, shock ◦ Frequent vomitng ◦ Polyuria despite dehydration ◦ Weight loss in spite of good intake ◦ Acetone breath – (Kussmaul respiration) deep and rapid ◦ Altered sensorium ◦ Signs of raised intracranial pressure – bradycardia, HT, anisocoria

RISK FACTORS �AS INITIAL PRESENTATION: �Young age: < 5 years �Low socioeconomic background �IN ESTABLISHED TYPE 1 DM: �Higher Hb. A 1 c �Adolescents, particularly females �Psychiatric disorders �Longer duration of diabetes

severity �mild �moderate mmol/L � severe = p. H < 7. 30 or bicarb < 15 mmol/L = p. H < 7. 20 or bicarb < 10 = p. H < 7. 10 or bicarb < 5 mmol/L

Goals of therapy �Correct dehydration �Correct acidosis and reverse ketosis �Restore blood glucose to near normal �Avoid complications of therapy �Identify and treat any precipitating event

Emergency assessment �Brief history to find cause �Weigh the child �Assess degree of dehydration �Assess level of consciousness(glasgow coma scale) �Biochemical assessment

Biochemical assessment � Blood samples: ◦ ◦ ◦ ◦ Plasma glucose E&U, Cr, Ca, PO 4, Mg Hb. A 1 c Venous p. H p. CO 2 Hb FBC( Leucocytosis could exist without infection due to stress) ◦ Beta hydroxybutyrate

Biochemical assessment �Urine sample ◦ Urinalysis for ketones (acetoacetate) Others include culture samples: - (blood , urine, throat) ECG: - k status

Supportive therapy �Secure airway �A peripheral IV catheter should be placed in for convenient and repetitive sampling �Cardiac monitor �Give oxygen to pts with severe circulatory impairment or shock �Give anitbiotics to febrile patients after cultures have been taken

FLUID THERAPY � 1 st hr: 10 – 20 ml/kg 0. 9% Nacl with insulin infusion at 0. 05 – 0. 1 U/kg/hr � 2 nd hr & subsequent hrs: 0. 45% Nacl plus continuous insulin drip + 20 m. Eq/L K+ � 5% dextrose if blood glucose <250 mg/dl (14 mmol/L) �IV Rate= 85 ml/kg +(maintenance minus bolus) divided by 23

TREATMENT contd Maintain IV insulin until DKA resolves: � p. H > 7. 3, bicarbonate > 15 mmol/L, stable serum Na+ 135 – 145 mmol/L, No emesis; � then switch to SC insulin (maintain IV insulin 30 min after SC) �Ketones may take longer to clear

POTASSIUM �HYPOKALEMIC = give with initial resuscitation ◦ 20 mmol/l �EUKALEMIC = at the time of insulin intro �HYPERKALEMIC = when patient makes urine

Potassium �Max dose 0. 5 mmol/kg/hr �If hypokalemia persist then reduce insulin infusion rate! �ECG monitoring helps!

Acidosis �Is given cautiously only if ◦ p. H < 6. 9 ◦ HCO 3 < 5 mmol/l 1 – 2 mmol/kg over one hour!

Monitoring/charting �Hourly monitoring and charting of ◦ ◦ ◦ ◦ ◦ Blood pressure Respiratory rate Heart rate Level of consciousness Blood sugar Blood ketones Electrolyte and urea(Ca, PO 4, Mg) Input /output Insulin given

Complications of therapy �Inadequate rehydration �Hypoglycemia �Hypokalemia �hypophosphatemia �Cerebral edema

Management of DKA � Follow up
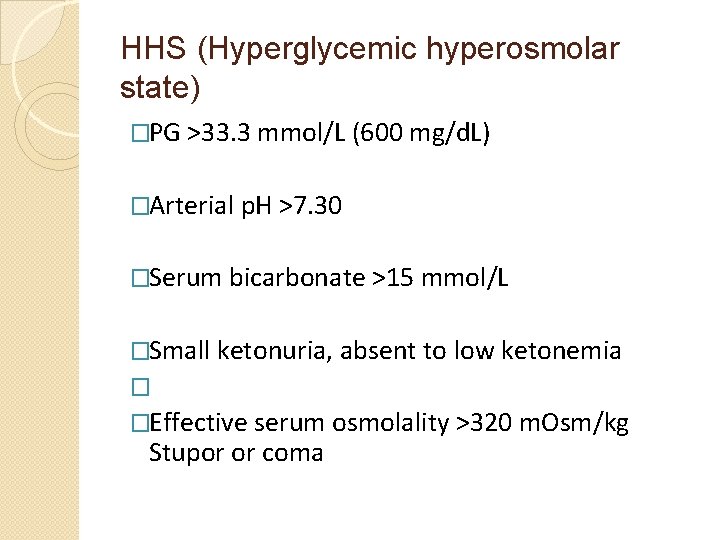
HHS (Hyperglycemic hyperosmolar state) �PG >33. 3 mmol/L (600 mg/d. L) �Arterial p. H >7. 30 �Serum bicarbonate >15 mmol/L �Small ketonuria, absent to low ketonemia � �Effective serum osmolality >320 m. Osm/kg Stupor or coma

Long-term complications Retinopathy � Cataracts � Hypertension � Progressive renal failure � Early coronary artery disease � Peripheral vascular disease � Neuropathy, both peripheral and autonomic � Increased risk of infection � Injection-site hypertrophy � Growth failure. Delayed puberty �

Recent advancements � Whole pancreas transplantation � Islet cell transplantation � Engineered stem cells manipulated genetically to produce insulin � Techniques to protect b cells from autoimmune attack – Immunotherapy � Alternate non invasive routes for insulin administration � Chemical alteration of insulin molecule � Artificial pancreas � Adding c peptide to insulin � Implantable insulin pumps � New blood glucose meters

Conclusion �DM (particularly T 1 DM), a common and potentially life threatening endocrine disorder in children is often misdiagnosed or poorly managed �Having a regularly updated management protocol in our Paediatric units will greatly improve the level and quality of care these children receive. �Thank you for listening.

Post test 1. 2. 3. 4. 5. Dm is the commonest endocrine disorder in children Only type 1 dm occurs in children TIDm is a non progressive lowinsulin catabolic state Exogenous insulin replacement remains the only form of replacement therapy In managing DKA, always add kcl to the initial rehydrating fluid.
- Slides: 62