Diabetes Mellitus DM By Ms Santoshi Naik Assistant

Diabetes Mellitus (DM) By: Ms. Santoshi Naik Assistant Professor Yenepoya Pharmacy College and Research Centre 1
DEFINITION • DM is defined as a heterogeneous metabolic disorder characterized by chronic hyperglycemia with disturbance of carbohydrate, fat and protein metabolism. • Diabetes is due to either the pancreas not producing enough insulin or the cells of the body not responding properly to the insulin produced. 2
Classification & Etiology of Diabetes Mellitus Type 1 DM Type 2 DM Other specific types of Diabetes Gestational DM 3

TYPE 1 DM • Earlier called Insulin-dependent(IDDM) because it was known that these patients have absolute requirement for insulin replacement as treatment, or juvenile-onset diabetes due to its occurrence in younger age. • Incidence of occurrence – 10% cases of Diabetes Mellitus. Subtype 1 A DM Subtype 1 B DM • Immune-mediated DM • Autoimmune destruction of β-cells which usually leads to insulin deficiency. • Idiopathic DM • Characterised by insulin deficiency 4

Type 2 DM • Earlier called Non-insulin-dependent or maturity-onset diabetes since it predominantly affects older individuals but, it is now known that it also occurs in obese adolescent children. • It is characterised by insulin resistance (sensitization of insulin receptors), impaired or delayed insulin secretion & excessive or inappropriate glucagon secretion. 5

Other specific types of Diabetes A. Genetic defect of β-cell function due to mutations in various enzymes (earlier called maturity-onset diabetes of the young or MODY). B. Genetic defect in insulin action (e. g. type A insulin resistance). C. Diseases of exocrine pancreas (e. g. chronic pancreatitis, pancreatic tumours, post-pancreatectomy). D. Endocrinopathies (e. g. acromegaly, Cushing's syndrome). 6

E. Drug- or chemical-induced (e. g. steroids, thyroid hormone, thiazides, β-blockers etc). F. Infections (e. g. congenital rubella). G. Other genetic syndromes (e. g. Down's syndrome, Turner's syndrome). 7

Gestational DM • About 4% pregnant women develop DM due to metabolic changes during pregnancy. • Although they revert back to normal glycaemia after delivery, these women are prone to develop DM later in their life. 8

PATHOGENESIS OF DIABETES MELLITUS 9

• Depending upon etiology of DM, hyperglycaemia may result from the following: 1. Reduced insulin secretion 2. Reduced insulin action 3. Decreased glucose use by the body 4. Increased glucose production 10

Normal Insulin Metabolism Insulin is synthesised in the β-cells of pancreas Glucose is the key regulator of insulin secretion from β-cells Half of insulin is degraded in the liver while the remaining half enters the systemic circulation 11

Pathogenesis of Type 1 DM • The basic phenomenon in type 1 DM is destruction of β-cell mass, usually leading to absolute insulin deficiency. • Pathogenesis of type 1 A DM is explained on the basis of 3 mutually-interlinked mechanisms. 1. Genetic susceptibility • • In identical twins - 50% chance of the second twin About half the cases with genetic predisposition have the susceptibility gene located in the HLA region of chromosome 126.

2) Autoimmune Factors a) Presence of islet cell antibodies against GAD (glutamic acid decarboxylase), insulin etc. b) Occurrence of lymphocytic infiltrate in and around the pancreatic islets termed insulitis. c) Selective destruction of beta cells while other islet cell types remain unaffected. d) Assocaition of type 1 A DM with other autoimmune diseases such as Graves disease, Addisons disease, etc. 13

3) Environmental Factors: • Certain viral infections eg: mumps, measles etc. • Experimental induction of type 1 A DM with certain chemicals has been possible. eg alloxan, pentamidine, etc. • Geographic and Seasonal Variations. • Possible relationship of early exposure to bovine milk proteins. 14

Pathogenesis of Type 2 DM • The basic metabolic defect in type 2 DM is either delayed insulin secretion (impaired insulin secretion) or the peripheral tissues are unable to respond to insulin (insulin resistance) or excess glucagon secretion. 1. Genetic Factors • There is approximately 80% chance of developing diabetes in the other identical twin if one twin has the disease. • A person with one parent having type 2 DM is at an increased risk of getting diabetes, but if both parents have type 2 DM the risk in the offspring rises to 40%. 15

2. Constitutional Factors • Certain environmental factors such as obesity, hypertension, and level of physical activity play contributory role and modulate the disease. 3. Insulin Resistance Lack of responsiveness of peripheral tissues to insulin. Mechanism of Hyperglycemia in these cases is explained as under: a) Resistance to action of insulin impairs glucose utilisation and hence hyperglycaemia b) There is increased hepatic synthesis of glucose. c) Hyperglycaemiainobesityisrelatedtohighlevelsof free fatty acids and cytokines. 16

4. Impaired Insulin Secretion In type 2 DM, insulin resistance and insulin secretion are interlinked : A) Early in the course of disease, in response to insulin resistance there is compensatory increased secretion of insulin (hyperinsulinaemia) in an attempt to maintain normal blood glucose level. B) Eventually there is failure of beta cell function to secrete adequate insulin, although there is some secretion of insulin i. e. cases of type 2 DM have mild to moderate deficiency of insulin but not its total absence. 17

5. Increased Hepatic Glucose Synthesis • One of the normal roles played by insulin is to promote hepatic storage of glucose as glycogen and suppress gluconeogenesis. In Type 2 DM, as a part of insulin resistance by peripheral tissues, liver also shows insulin resistance. • This results in increased hepatic synthesis of glucose which contributes to hyperglycaemia in these cases. 18
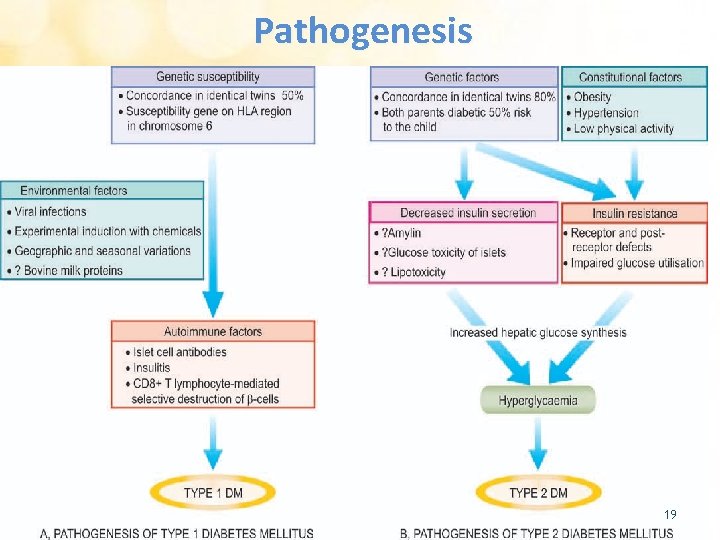
Pathogenesis 19

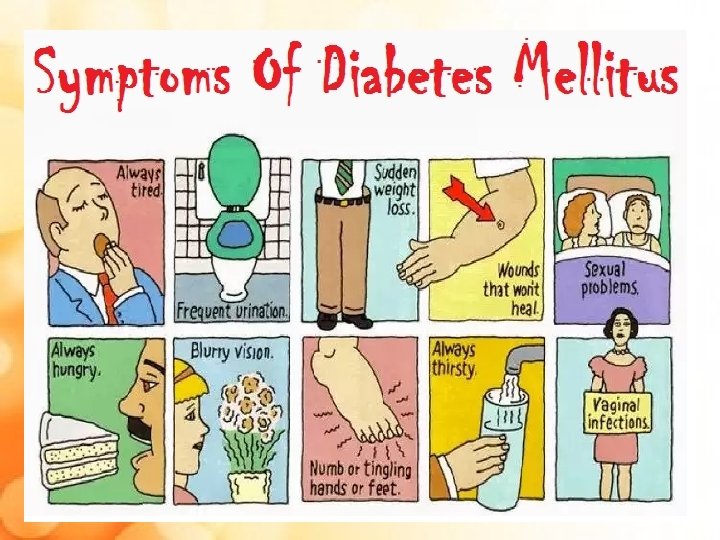
COMPLICATIONS OF DM Acute metabolic complications • Eg: Diabetic ketoacidosis, hyperosmolar hyperglycemic nonketotic coma and hypoglycaemia Late systemic complications • Eg: Atherosclerosis, diabetic microangiopathy, diabetic nephropathy, diabetic neuropathy, diabetic retinopathy and infections 20

Acute Metabolic Complications • Ketoacidosis and hypoglycaemia are complications of Type 1 DM. • Hyperosmolar hyperglycemic nonketotic coma is complication of Type 2 DM. 1. Diabetic ketoacidosis: • A serious diabetes complication where the body produces excess blood acids (ketones). • Symptoms: anorexia, nausea, vomiting, deep and fast breathing, mental confusion and coma. 21

Development of Ketoacidosis Severe lack of insulin causes lipolysis in the adipose tissues Release of free fatty acids into the plasma FFA taken up by the liver & oxidised to ketone bodies principally acetoacetic acid and β-hydroxybutyric acid Glucagon accelerates the oxidation of free fatty acids leading to Ketonaemia and Ketonuria If urinary excretion of ketone bodies is prevented due to dehydration, systemic metabolic ketoacidosis occurs. 22

2. Hyperosmolar hyperglycaemic nonketotic coma (HHS) • It is caused by severe dehydration resulting from sustained hyperglycaemic diuresis. • The loss of glucose in urine is so intense that the patient is unable to drink sufficient water to maintain urinary fluid loss. 3. Hypoglycaemia • It may result from excessive administration of insulin, missing a meal, or due to stress. • Hypoglycaemia produces permanent brain damage. 23

Late Metabolic Complications • Complications may develop after 15 -20 yrs. • Late complications are largely responsible for premature mortality in diabetes mellitus. 1. Atherosclerosis • Diabetes mellitus of both type 1 and type 2 accelerates the development of atherosclerosis. • Causes: hyperlipidaemia, reduced HDL levels, obesity and associated hypertension in diabetes 24

2. Diabetic microangiopathy • Microangiopathy of diabetes is characterised by basement membrane thickening of small blood vessels and capillaries of different organs and tissues such as the skin, skeletal muscle, eye and kidney. 3. Diabetic nephropathy • Renal involvement is a common complication and a leading cause of death in diabetes. 4. Diabetic neuropathy • Diabetic neuropathy may affect all parts of the nervous system. 25

5. Diabetic retinopathy • Diabetic retinopathy is a leading cause of blindness – damage to retina of the eye. • Diabetes also predisposes the patients to early development of cataract and glaucoma. 6. Infections • Diabetics have enhanced susceptibility to various infections such as tuberculosis, pneumonias, otitis and diabetic ulcers. 26
27

28
- Slides: 28