Diabetes Mellitus Diabetes care should be managed by


Diabetes Mellitus

Diabetes care should be managed by a multidisciplinary team that may draw from primary care physicians, subspecialty physicians, nurse practitioners, physician assistants, nurses, dietitians, exercise specialists, pharmacists, dentists, podiatrists, and mental health professionals.

Classification

Type 1 DM is the result of complete or near -total insulin deficiency.

Type 2 DM is a heterogeneous group of disorders characterized by variable degrees of: insulin resistance, impaired insulin secretion, increased glucose production.

type 2 DM Screening? ? (1) a large number of individuals who meet the current criteria for DM are asymptomatic, (2) type 2 DM may be present for up to a decade before diagnosis, (3) some individuals with type 2 DM have one or more diabetesspecific complications at the time of their diagnosis, and (4) treatment of type 2 DM may favorably alter the natural history of DM

Gestational Diabetes Mellitus (GDM) resistance is related to the metabolic changes of late pregnancy, and the increased insulin requirements may lead to IGT or diabetes

Study Groups now recommends that diabetes diagnosed at the initial prenatal visit should be classified as "overt" diabetes rather than GDM.

Criteria for the Diagnosis of DM

Symptoms of diabetes plus random blood glucose concentration(200 mg/d. L)

Fasting plasma glucose 126 mg/d. L

A 1 C > c 6. 5% or

Two-hour plasma glucose (200 mg/d. L) during an OGT testd

Fasting is defined as no caloric intake for at least 8 h

IFG(prediabete s) FBS(110– 125 mg/d. L);

IGT(prediabet es) plasma glucose levels between 140 and 199 mg/d. L) following an oral glucose challenge, which is termed impaired glucose tolerance (IGT);

Monitor at least annually for the development of diabetes in those with prediabetes

Screening for and diagnosis of GDM

OGTT Perform a 75 -g OGTT patient is fasting and at 1 and 2 h, , with plasma glucose measurement when

diagnosis of GDM Fasting: 92 mg/d. L (5. 1 mmol/L) 1 h: 180 mg/d. L (10. 0 mmol/L) 2 h: 153 mg/d. L (8. 5 mmol/L)

Two-step strategy Step 1: Perform a 50 -g GLu (nonfasting), If the plasma glucose level measured 1 h after the load is 140 mg/d. L :

Step 2 . : The 100 -g OGTT should be performed when the patient is fasting. The diagnosis of GDM is made if at least two of the following four plasma glucose levels (measured fasting and 1 h, 2 h, 3 h after the OGTT) are met or exceeded

diagnosis of GDM Fasting 95 mg/d. L 1 h 180 mg/d. L 2 h 155 mg/d. L 3 h 140 mg/d. L

Prevention

Prediabetes is associated with heightened cardiovascular risk; therefore, screening for and treatment of modifiable risk factors for cardiovascular disease is suggested.

The lifestyle intervention group lost 5– 7% of their body weight during the 3 years of the study. ; -

Metformin therapy for prevention of type 2 diabetes should be considered in those with prediabetes, especially for those with BMI ≥ 35 kg/m 2, those aged <60 years, and women with prior GDM.

Preventiive drug glucosidase inhibitors, metformin, thiazolidinediones, and orlistat prevent or delay type 2 DM but are not approved for this purpose

This effect was seen in individuals regardless of age, sex, or ethnic group.

Biguanides REDUCE Hepatic glucose production

Biguanides Metform in Indication Glucophage (Glucophage XR) 500, 850, 1000 mg 500, 750 mg XR tablets Type II Diabetes Mellitus Mechanism of action: Decrease hepatic glucose production decrease intestinal absorption of glucose increase insulin sensitivity therefore increasing peripheral glucose uptake

Metformin Weight neutral, Do not cause hypoglycemia inexpensive

CONTRAINDICATION CHF, GFR<30% radiographic contrast studies, seriously ill patients, acidosis

Warning Metformin and metformin XR should be temporarily discontinued in patients undergoing radiologic studies involving intravascular administration of iodinated contrast materials, because of such products may result in acute alteration of renal function.

Metformin had to be stopped 48 hors before and after contrast

SGLT 2 Inhibitors
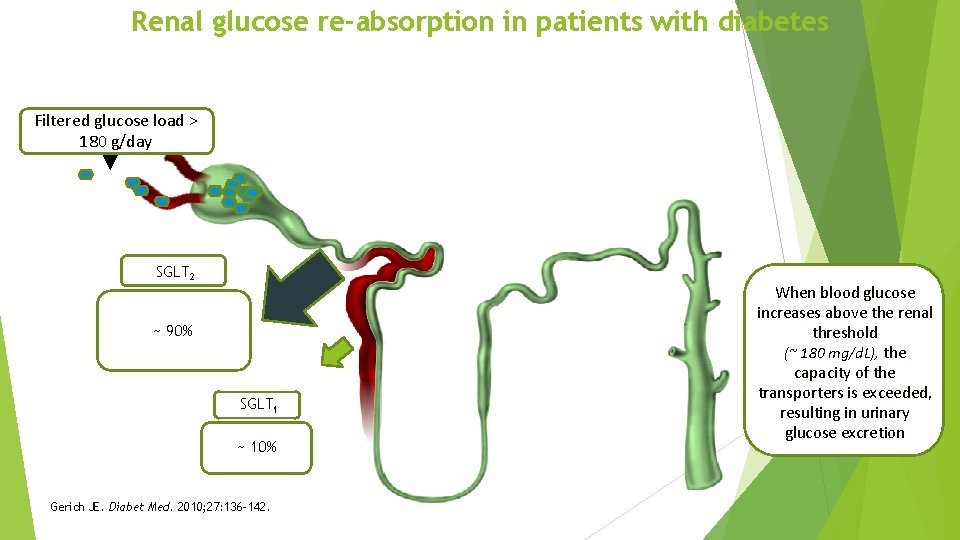
Renal glucose re-absorption in patients with diabetes Filtered glucose load > 180 g/day SGLT 2 ~ 90% SGLT 1 ~ 10% Gerich JE. Diabet Med. 2010; 27: 136– 142. When blood glucose increases above the renal threshold (~ 180 mg/d. L), the capacity of the transporters is exceeded, resulting in urinary glucose excretion
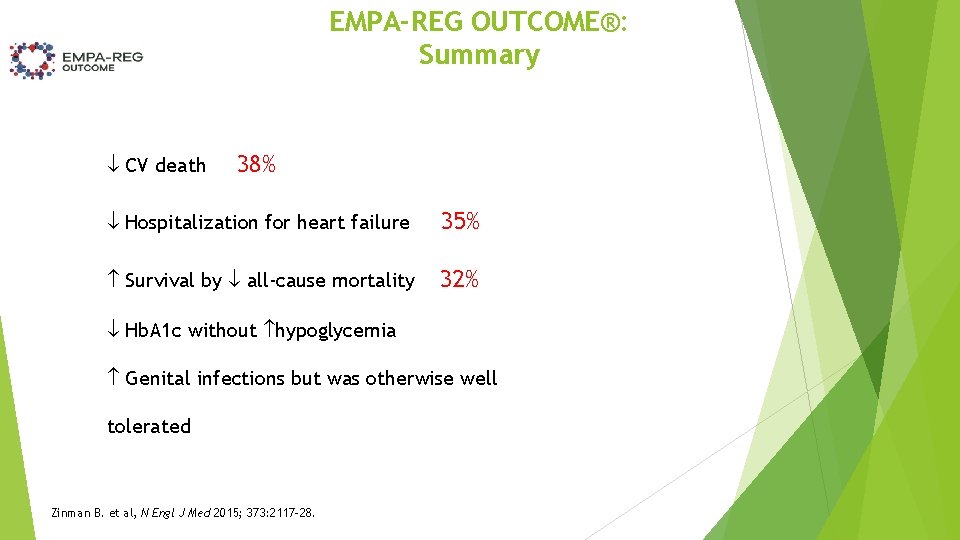
EMPA-REG OUTCOME®: Summary CV death 38% Hospitalization for heart failure 35% Survival by all-cause mortality 32% Hb. A 1 c without hypoglycemia Genital infections but was otherwise well tolerated Zinman B. et al, N Engl J Med 2015; 373: 2117 -28.

Empagliflozin Clinical Pharmacokinetics Tablet intake: 10 mg, QD 25 mg, QD Metabolism: No active metabolite Jardiance FDA label 2017 Jardiance (empagliflozin) Summary of Product Characteristics. Available at: https: //www. medicines. org. uk/emc/medicine/28973 (accessed July 2016). Absorption: Peak levels at 1. 5 hrs after dosing No clinically relevant food effect Half-life: Estimated to be 12. 4 hrs, steady state reached by ~ Day 5
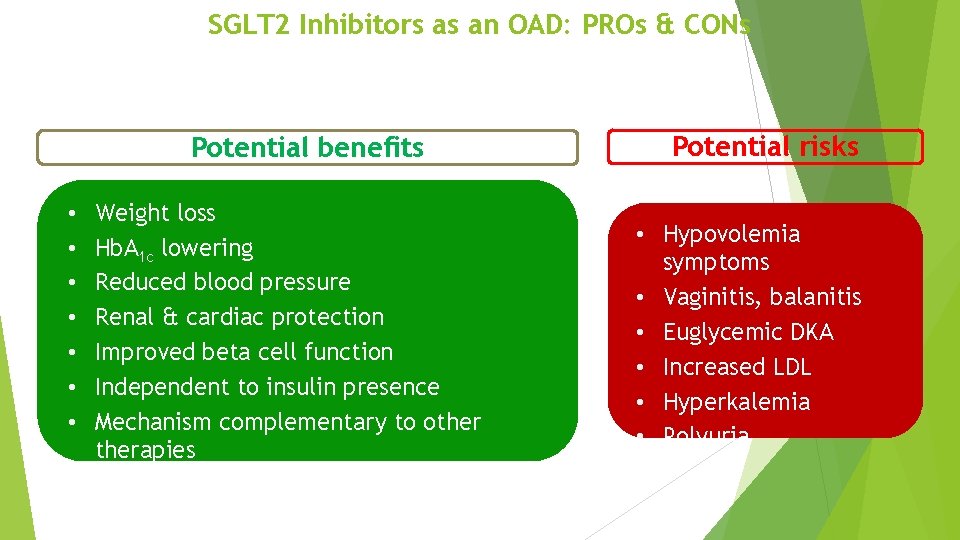
SGLT 2 Inhibitors as an OAD: PROs & CONs Potential benefits • • Weight loss Hb. A 1 c lowering Reduced blood pressure Renal & cardiac protection Improved beta cell function Independent to insulin presence Mechanism complementary to otherapies Potential risks • Hypovolemia symptoms • Vaginitis, balanitis • Euglycemic DKA • Increased LDL • Hyperkalemia • Polyuria

DPP-4 inhibitor
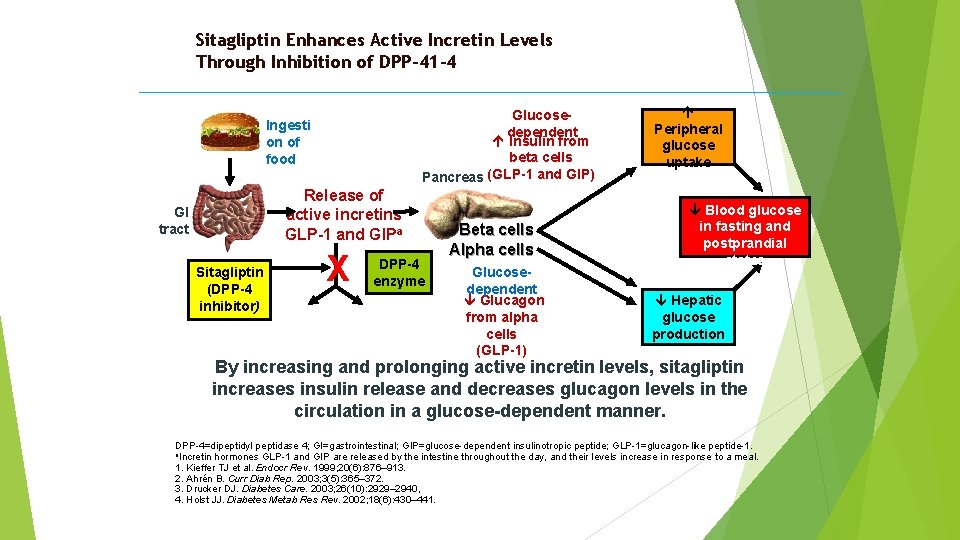
Sitagliptin Enhances Active Incretin Levels Through Inhibition of DPP-41– 4 Glucosedependent Insulin from beta cells Pancreas (GLP-1 and GIP) Ingesti on of food Release of active incretins GLP-1 and GIPa GI tract Sitagliptin (DPP-4 inhibitor) X Inactive GLP-1 DPP-4 enzyme Inactive GIP Beta cells Alpha cells Glucosedependent Glucagon from alpha cells (GLP-1) Peripheral glucose uptake Blood glucose in fasting and postprandial states Hepatic glucose production By increasing and prolonging active incretin levels, sitagliptin increases insulin release and decreases glucagon levels in the circulation in a glucose-dependent manner. DPP-4=dipeptidyl peptidase 4; GI=gastrointestinal; GIP=glucose-dependent insulinotropic peptide; GLP-1=glucagon-like peptide-1. a. Incretin hormones GLP-1 and GIP are released by the intestine throughout the day, and their levels increase in response to a meal. 1. Kieffer TJ et al. Endocr Rev. 1999; 20(6): 876– 913. 2. Ahrén B. Curr Diab Rep. 2003; 3(5): 365– 372. 3. Drucker DJ. Diabetes Care. 2003; 26(10): 2929– 2940, 4. Holst JJ. Diabetes Metab Res Rev. 2002; 18(6): 430– 441.
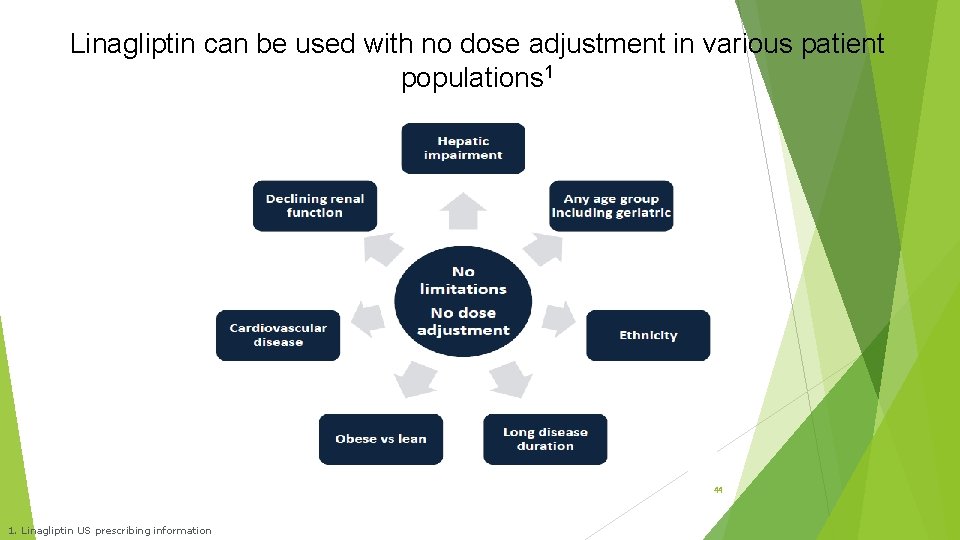
Linagliptin can be used with no dose adjustment in various patient populations 1 44 1. Linagliptin US prescribing information
q q q Both diabetes and CKD are strongly associated with cardiovascular disease (CVD). The control blood glucose and blood pressure to reduce the risk of kidney disease up to 40% of people with diabetes will develop chronic kidney disease. More than 80% of cases of end-stage renal disease (ESRD) are caused by diabetes , hypertension or a combination of both.

Linagliptin has the broadest clinical evidence in the DPP-4 i class Monotherapy Vildagliptin 1 Saxagliptin 2 Alogliptin 3, 4 Sitagliptin 5, 6 Linagliptin 7 Dual therapy Triple therapy * ** High CV risk Heart failure High kidney risk Limited evidence‡ Limited evidence Proven safety Safety signal Limited evidence Proven safety Uncertain§ Limited evidence Proven safety Proven safety † 46 *No CVOT of vildagliptin has been conducted; †Not studied in combination with metformin and thiazolidinedione(s); ‡Not studied in combination with metformin and sulphonylurea(s); §Numerical, nonsignificant increase in hospitalisation for heart failure, CV, cardiovascular; CVOT, cardiovascular outcomes trial; DPP-4, dipeptidyl peptidase-4 1. Novartis Europharm Ltd. Galvus® (vildagliptin) summary of product characteristics; 2. Scirica B et al. N Engl J Med 2013; 369: 1317; 3. White W et al. N Engl J Med 2013; 369: 1327; 4. Takeda Pharma A/S. Vipidia® (alogliptin) summary of product characteristics; 5. Green J et al. N Engl J Med 2015; 373: 232; 6. Engel SE et al. Diabetes Obes Metab 2017; 19: 1587; 7. Rosenstock J, et al. JAMA. 2018 Nov 9. doi: 10. 1001/jama. 2018. 18269

Limitations of Use Should not be used in patients with type 1 diabetes Treatment of diabetic ketoacidosis Has not been studied in patients with a history of pancreatitis

There have been post marketing reports of acute pancreatitis, including fatal pancreatitis. if pancreatitis is suspected, promptly discontinue Linagliptin. Heart failure has been observed with two other members of the dpp-4 inhibitor class. consider risks and benefits of Linagliptin in patients who have known risk factors for heart failure. Monitor for signs and symptoms. When used with an insulin secretagogue (e. g. , sulfonylurea) or insulin, consider lowering the dose of the insulin secretagogue or insulin to reduce the risk of hypoglycemia
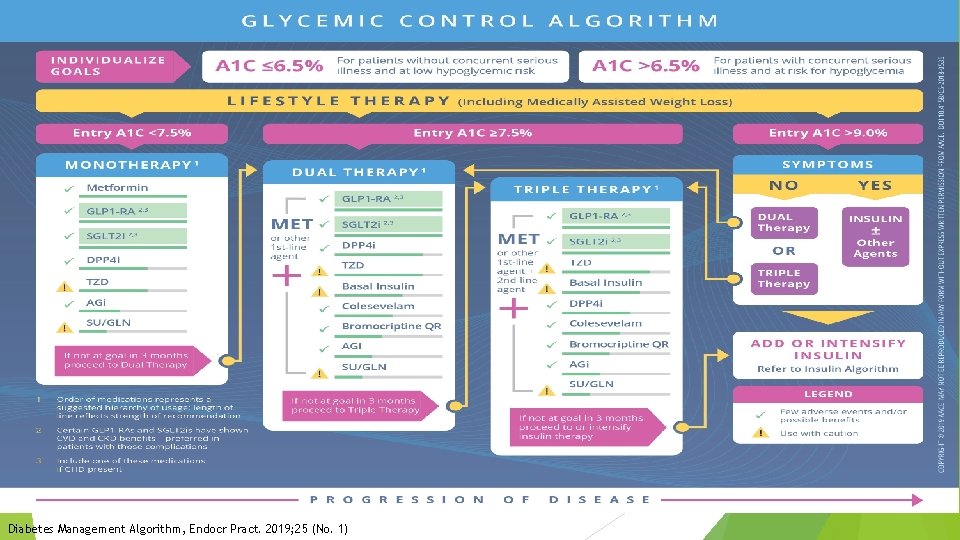
49 Diabetes Management Algorithm, Endocr Pract. 2019; 25 (No. 1)

Advantages of Fixed dose combination v Improving patient adherence. 1 v Improving quality of life and tolerability. 1 v Improving compliance by reducing polypharmacy. 2 v Lower overall costs. 3 50 [1] Adv Ther 2012; 29: 993 -1004 [2] The American Journal of Medicine (2007) 120, 713 -719 [3] Diabetes Obes Metab. 2013; 15(4): 291– 300.

Conclusions There was a reduction in all-cause mortality for patients treated with metformin combined with DPP-4 i versus metformin plus SU.

Combination therapy with DPP-4 Inhibitors and metformin improves glycemic control in appropriate patients with type 2 diabetes, with a low risk of hypoglycemia and no weight gain

Glorenta as the combination of Gloripa & Lirenta with their complementary mechanisms of action

CONCLUSIONS Combination of empagliflozin/linagliptin: v Significantly Reduced Hb. A 1 c compared with the individual components and were well tolerated. v FPG was significantly reduced with empagliflozin 25 mg/linagliptin 5 mg compared with individual components v The combination of empagliflozin and linagliptin added on to metformin offered a sustained reduction in Hb. A 1 c, FPG, weight, and blood pressure, which persisted up to week 52. 54

Gloripa, the only OAD indicated to reduce cardiovasular death in T 2 D among ASCVD patients. Lirenta, which is proven CV safe among patients with CV risks and renal disease

Hypoglycemia and DM

Hypoglycemia is an important limiting factor in glycemic management and may be a significant barrier to treatment adherence.

Classification of hypoglycemia Level 3: A severe event characterized by altered mental Level 2 : Glucose , 54 mg/d. L (3. 0 mmol/L Level 1: Glucose , 70 mg/d. L) and (glucose >54 mg/Dl)

Glucose(15– 20 g) is the preferred treatment for the conscious individual with blood glucose , 70 mg/d. L although any form of carbohydrate that contains glucose may be used. Fifteen minutes after treatment, if SMBG shows continued hypoglycemia, the treatment should be repeated

Glucagon should be prescribed for all individuals at increased risk of level 2 hypoglycemia, defined as blood glucose , 54 mg/d. L, so it is available should it be needed.

Hypoglycemia unawareness or one or more episodes of level 3 hypoglycemia should trigger reevaluation of the treatment regimen.

Caregivers, school personnel, or family members of these individuals should know where it is and when and how to administer it. Glucagon administration is not limited to health care professionals.

Hypertension and DM

Patients with confirmed officebased blood pressure >140/90 mm. Hg should, in addition to lifestyle therapy, have prompt initiation and timely titration of pharmacologic therapy to achieve blood pressure goals

For patients with blood pressure. 120/80 mm. Hg, lifestyle intervention consists of weight loss if overweight or obese, a Dietary Approache

to lifestyle therapy, have prompt initiation and timely titration of two drugs or a single-pill combination of drugs demonstrated to reduce cardiovascular events in patients with diabetes and BP>160/90.

Treatment for hypertension should include drug classes demonstrated to reduce cardiovascular events in patients with diabetes (ACE inhibitors, angiotensin receptor blockers, thiazide-like diuretics, or dihydropyridine calcium channel blockers

Patients with hypertension who are not meeting blood pressure targets on three classes of antihypertensive medications (including a diuretic) should be considered for mineralocorticoid receptor antagonist therapy.

HYPERLIPIDEMIA and DM

For patient swith diabetes aged , 40 years with additional atherosclerotic cardiovascular disease risk factors, the patient and provider should consider using moderate intensity statin in addition to lifestyle therapy

However, combinations of ACE inhibitors and angiotensin receptor blockers with direct renin inhibitors should not be used

For patients treated with an ACE inhibitor, angiotensin receptor blocker, or diuretic, serum creatinine/estimated glomerular filtration rate and serum potassium levels should be monitored at least annually

Recommendations For patients of all ages with diabetes and atherosclerotic cardiovascular high-intensity statin therapy should be added to lifestyle therapy.

For patients with diabetes and atherosclerotic cardiovascular disease, if LDL cholesterol is $70 mg/d. L on maximally tolerated statin dose, consider adding additional LDL-lowering therapy (such as ezetimibe)

High-intensity statin therapy (lowers LDL cholesterol by >50%) Atorvastatin 40– 80 mg Rosuvastatin 20– 40 mg

Moderate-intensity statin therapy (lowers LDL cholesterol by 30– 50%) Atorvastatin 10– 20 mg Rosuvastatin 5– 10 mg

In adults with moderate hypertriglyceridemia (175– 499 mg/d. L), clinicians should address and treat lifestyle factors

For patients with fasting triglyceride levels 500 mg/d. L (5. 7 mmol/L), evaluate for secondary causes of hypertriglyceridemia and consider medical therapy to reduce the risk of pancreatitis

Use aspirin therapy (75– 162 mg/day) as a secondary prevention strategy in those with diabetes and a history of atherosclerotic cardiovascular disease

In asymptomatic patients, routine screening for coronary artery disease is not recommended

In asymptomatic patients, routine screening for coronary artery disease is not recommended

Among patients with atherosclerotic cardiovascular disease at high risk of heart failure or in whom heart failure coexists, sodium–glucose cotransporter 2 inhibitors are preferred

primary prevention strategy in those with diabetes who are at increased cardiovascular risk, after a discussion with the patient on the benefits versus increased risk of bleeding

Use aspirin therapy (75– 162 mg/day) as a secondary prevention strategy in those with diabetes and a history of atherosclerotic cardiovascular disease
Thank you for your attention
- Slides: 85