DIABETES MELLITUS AND ITS COMPLICATIONS ARE NOW THE


- DIABETES MELLITUS AND ITS COMPLICATIONS ARE NOW THE THIRD LEADING CAUSE OF MORTALITY IN THE UNITED STATES AND THE SECOND LEADING CAUSE OF BLINDNESS.

-ESTIMATED PREVALENCE IN U. S. A 3 - 6 % AND INCREASING RAPIDLY -ESTIMATED PRVALENCE IN SAUDI ARABIA to 2003 18 -24%

-STROKE, M 1 AND END – STAGE RENAL DISEASE ARE FREQUENT CAUSES OF MORTALITY. -THE DISEASE IS FOUND THROUGHOUT THE WORLD AT VARYING PRVALENCE RATE. - IN PIMA INDIANDS PREVALENEC RATE AT 50 %

NIDDM IS MAJOR CAUSE OF MORBIDITY AND MORTALITY PREVAILING FROM, MACROVASCULAR DISEASE , BUT ALSO FROM SPECIFIC COMPLICATIONS OF DISABETES , RETINOPATHY , NEPHROPATHY AND NEUROPATHY.

DIABETES MELLITUS IS ADISEASE COMPLEX CHARACTERISED BY RELATIVE OR ABSOLUTE INSUFFICIENCY OF INSULIN SECRETION AND A CONCMMITANT INTENSITIVITY OR RESISTANCE TO THE METABOLIC TISSUE. ACTION INSULIN TARGET

NON INSULIN DEPENDENT DABETES ( NIDDM ) IS by FAR THE MOST PREVALENT FORM OF DIABETES WORLD – WIDE , FORMING MORE THAN 95 % OF ALL DIABETES IN MANY DEVELOPING COUNTRIES.

§ Genetic Factors HLA class 2 antigens in DR + DQ regions = >90% Caucasian patients have either DR 3 or DR 4 , DR 2 is protective. § Environmental Factors: No Specific factors have been identified

( cont. ) § Viruses ØThe risk greater for children born between February-September ØIg. M antibodies against conxsackievirus found in 25 -30% of new cases suggesting recent infection

ØCoxsackievirus B RNA has been detected in 65% of children under the age of 7 years with newly diagnosed IDDM compared with 4% of controls which is consistent with recent Infection. .

(CONT) §Dietary Factors ØCow, s mild feeding fist 4 months indicated risk of subsequent IDDM, whilst breast feeting appeared protective. ØCase controlled studies in Sweden have indicated a positive association between IDDM , high protein intake and frequency of consumption of foods containing nitrosamine.

(CONT) §Loss of first- phase insulin secretion in response to intravenous glucose is highly Predictive of early onset of diabetes.

q Islet cell antibodies in ICA are present in 80% of children at the time of diagnosis and have been detected up to 15 years before diagnosis of IDDM. q Long- term follow up has shown that family members with ICA are at greatly increased risk of progression to diabetes and this risk is directly related to persistence and strength of the ICA reaction.

( cont. ) q. Other antibodies include: Ø insulin autoantibodies ( IAA) Øantibodies to GAD ( Glutamate decarboxylase ) ØProtein tyrosine phosphatase IA-2 q The presence of ICA together with 2 or more markers indicate a greater than 80% risk of progressing for insulin treatment in otherwise healthy family members.
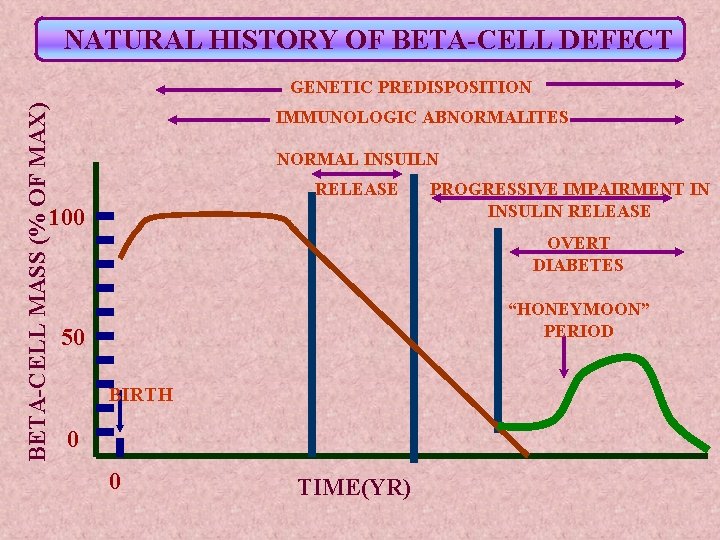
NATURAL HISTORY OF BETA-CELL DEFECT BETA-CELL MASS (% OF MAX) GENETIC PREDISPOSITION IMMUNOLOGIC ABNORMALITES NORMAL INSUILN RELEASE 100 PROGRESSIVE IMPAIRMENT IN INSULIN RELEASE OVERT DIABETES “HONEYMOON” PERIOD 50 BIRTH 0 0 TIME(YR)

DUE TO BETA-CELL RESERVE INSULIN REQUIREMENT DECREASED LASTS FOR UP TO 1 YR PATIENT ALWAYS RELAPSES TREATMENT PROPOSED TO EXTEND HONEYMOON PERIOD STILL EXPERIMENTAL

RELATIONSHIPS OF TYPE I WITH OTHER AUTOIMMUNE DISEASES ASSOCIATION BETWEEN HLA GENES AND DIABETES PRESENCE OFANTI-ISULET AND/OR ANTIINSULIN ANTIBIES PRESENCE OF INFLAMMATORY CELLS AROUND ISLETS EVIDENCE OF IMMUNE SYSTEM ACTIVATION
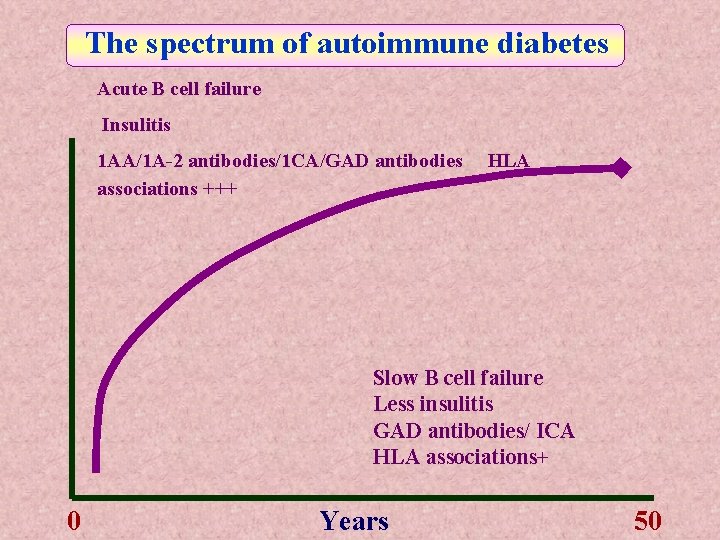
The spectrum of autoimmune diabetes Acute B cell failure Insulitis 1 AA/1 A-2 antibodies/1 CA/GAD antibodies associations +++ HLA Slow B cell failure Less insulitis GAD antibodies/ ICA HLA associations+ 0 Years 50
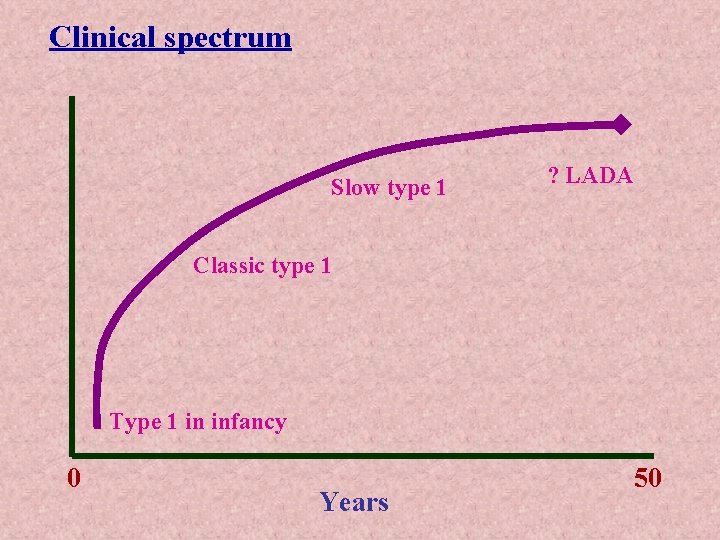
Clinical spectrum Slow type 1 ? LADA Classic type 1 Type 1 in infancy 0 Years 50

The clinical and immunogenetic characteristics of insulin dependent diabetes mellitus change according to age at presentation 1 AA, insulin auto-antibodies: 1 A 2, protein 1 A-2: GAD, glutamate decarboxylase; ICA, islet cell antibodies, LADA, latent autoimmune diabetes in the adult

DR 2 TYPE I DR 3 DR 4 A 2 ----- BW 51 -------- DR 4 B 8 -------B 15 GENERALLY LOW IN POPULATION

W. H. O. CLASSIFICATION TYPE I ( INSULIN DEPENDET DIABETES MLLITUS IDDM) §HAVE LITTLE OR NO ENDOGENOUS INSULIN §ONSET OF DISEASE IS CLNICALLYABRUPT WITH : MARKED POLYURIA, POLYDIPSIA POLYPHAGIA WEIGHT LOSS, FATIGUE. §THESE PATIENTS ARE HIGHLY PRONE TO KETOSTS §THEY FREQUENT ARE PRESNT IN AND INITIAL ATTACK OF KETOACIDOSIS

TYPE I CONTD. . §GENERALLY HAVE WEIGHT LOSS AND ARE FREQUENTLY AT OR BELOW IDEAL WEIGHT AND ARE THEREFORE PARTICULARY SENSITIVE TO INSULIN (ESPECIALLY REGULAR OR SOLUBLE INSULIN). § CAN OCCUR AT ANY AGE , BUT PEAKS IN THE MIDDLE OF THE FIST DECADE AND AGAIN AT THE TIME OF GROWTH ACCELERATION OF ADOLESCENCE. § OLD TERM – JUVENILE ONSET DIABETES MLLITUS.

TYPE I CONTD… §A PRODOMAL PHAE OF POLYUREA , POLYDYPSIA AND WEIGH LOSS MAY PRECEDE THE DEVELOPMENT OF KETOACIDOSIS BY A PERIOD OF MONTHS ( MOST COMMONLY 2 4 WEEKS ). § GENETIC PREDISPOSISTION ( FAMILY HISTORY LESS STRONGLY ASSOCIATED THAN WITH TYPE II ). § ASSOCIATED WITH SOME HLA HITOCMPATIBILTY ANTIGENS EG. B 8, B 15, DW 3, DW 4.

TYPE I CONTD. . . § ASSOCIATED WITH ISLET CELL ANTIBODIES § VIRUS AETIOLOGY IS IMPLICATED ESPECIALLY COXACKIE B 4 AND MUMPS. § SIGNIFICANT ASSOCIATION WITH CERTAIN AUTOIMMUNE DISORDERS - ADDISON ‘ S , HASHIMOTO’S TYROIDITS, HYPOPARATHYROIDISM, PERNICIOUS ANAEMIA

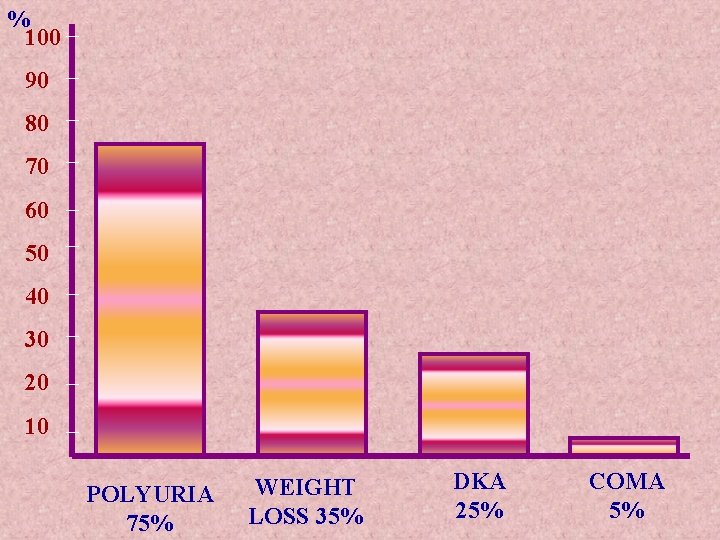
% 100 90 80 70 60 50 40 30 20 10 POLYURIA 75% WEIGHT LOSS 35% DKA 25% COMA 5%

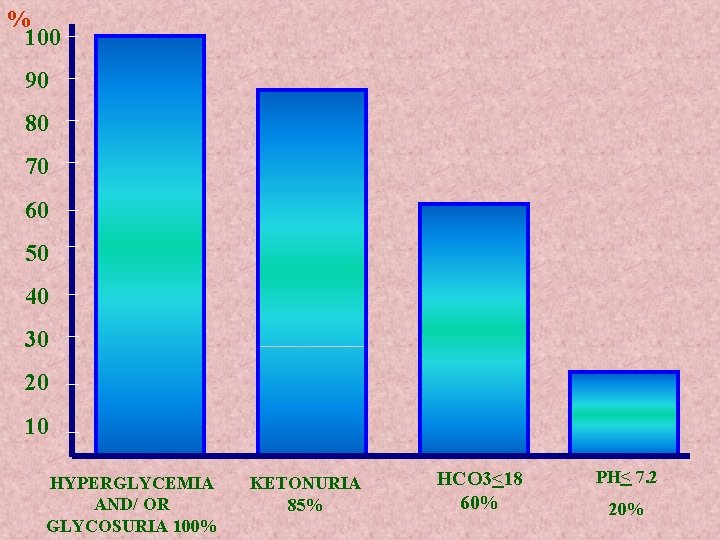
% 100 90 80 70 60 50 40 30 20 10 HYPERGLYCEMIA AND/ OR GLYCOSURIA 100% KETONURIA 85% HCO 3<18 60% PH< 7. 2 20%

NIDDM IS ALMOSTCERTAINLY A HETEOGENOUS MIXTURE OF CONDITIONS CHARACTERISEDBY HYPERGLYCAEMIA , OF INSULIN RESISTANCE AND INSULIN HYOPSECRETION AND LACK OF DEPENDENCE ON EXOGENOUS INSULIN TO MAINTAIN LIFE

TYPE II ( NIDDM ) FOR MAJOR ABNORMLITIES APPEAR TO ACCOUNT FOR THE INAPPROPRIATE HYPERGLYCMIA SEEM IN TYPE II ( NIDDM) PATIENTS 1 - DESCREASE IN QUANTITY INSULIN SECRETED 2 - DELAY IN THE TIME OF RELEASE OF INSULIN 3 - IMPAIRMET OF THE EFFCTS OF INSULIN ON THE PEREPHERAL TISSUES ( INSULIN RESISTANCE ) 4 - INCREASE IN HEPATIC GLUCOSE PRODUCTION

DIABETES MELLITUS TYPE I ( IDDM ) TYPE II ( NIDDM) - OBESE - NONBESE GESTATIONAL DIABETES OTHER TYPES IMPAIRED GLUCOSE TOLERANCE ( IGT)

§ Due primarily to a Beta cell defect resulting in inadequate insulin secretion for a given blood glucose level. § There is no significant increase in insulin resistance. § Various mutations in the giucokinase gene on chromosomes 7 p, probably account for 10 -50% of cases of MODY. § Giucokinase – Mody is characterized by early onset ( often less than 18 months of age ) mild hyperglycaemia which is usually contro. IIed by diet alone until old age.

§Autosmal Dominant §Diagnostic Criteria • Diagnosis before 25 years of age in atleast 2 family member. • No requirement of insulin treatment 5 years afte diagnosis and/or C- Peptide positivity. • Convincing vertical transmission of type II Diabetes mellitus through at least three generations. • Accounts upto 1% of Diabetes Mellitus populatio

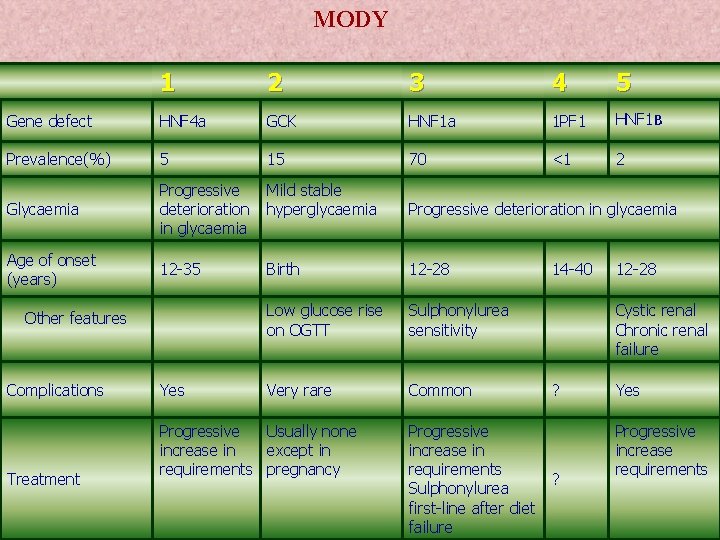
MODY 1 2 3 4 5 Gene defect HNF 4 a GCK HNF 1 a 1 PF 1 HNF 1 B Prevalence(%) 5 15 70 <1 2 Glycaemia Progressive deterioration in glycaemia Mild stable hyperglycaemia Progressive deterioration in glycaemia Age of onset (years) 12 -35 Birth 12 -28 Low glucose rise on OGTT Sulphonylurea sensitivity Very rare Common Other features Complications Treatment Yes Progressive Usually none increase in except in requirements pregnancy 14 -40 12 -28 Cystic renal Chronic renal failure ? Progressive increase in requirements ? Sulphonylurea first-line after diet failure Yes Progressive increase requirements

GENETICS : ( STRONG FAMILY AGGREGATES ALMOST 100% CONCORDANCE RATE IN IDENTICAL TWINS ( PYKE ET AL ) RACE : ( DIABETES IN MIGRANT INDIANS)

OBSITY : (PIMA INDIANS NAURANS) PHYSICAL INACTIVITY LONGIVITY : (DIABETES PREVALENCE INCREASES WITH AGE E. G. PREVALENCE RATE > 30 % IN ELDERLY IN FINLAND)

Two genes have been implicated so far : NIDDM 1 and NIDDM 2 MODY (Autosomal Dominant ) -MODY 1, (HNF-4) extremely uncommon) -MODY 2, (Glucokinase gene-impairs B-cell glucose sensing) -MODY 3, ( Hepatocyte Nuclear factor 1 - ( HNF-1) are more common Maternally inherited diabetes with deafness ( MIDD) Late onset IDDM
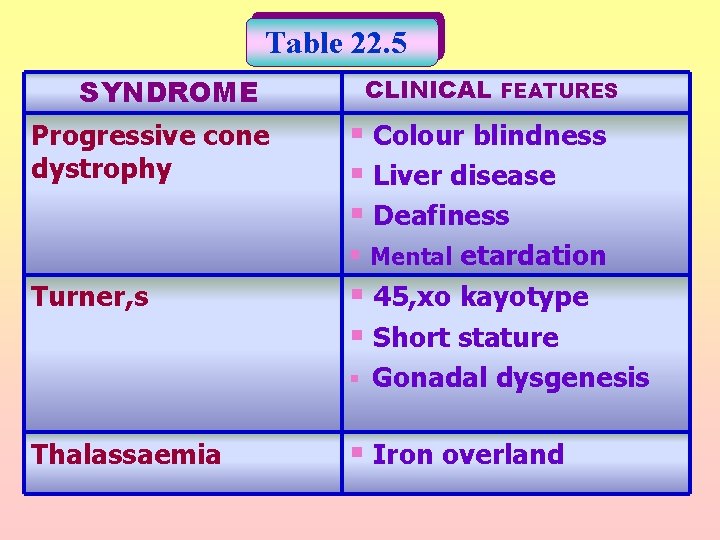
Table 22. 5 SYNDROME Progressive cone dystrophy Turner, s Thalassaemia CLINICAL FEATURES § Colour blindness § Liver disease § Deafiness § Mental etardation § 45, xo kayotype § Short stature § Gonadal dysgenesis § Iron overland
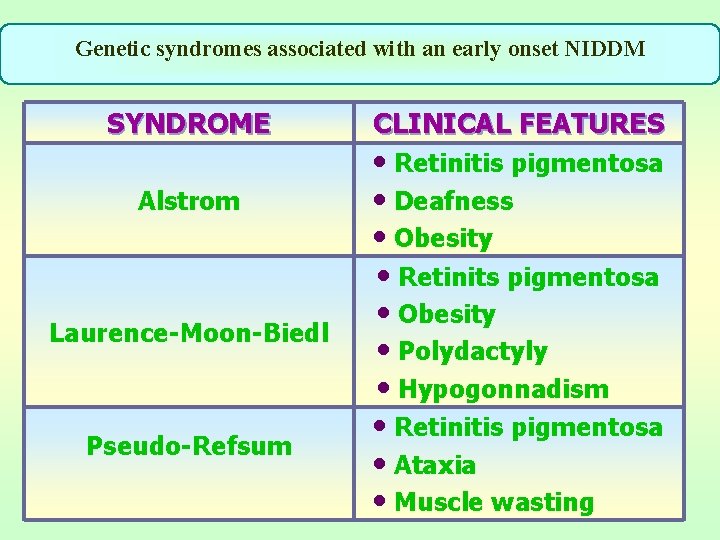
Genetic syndromes associated with an early onset NIDDM SYNDROME Alstrom Laurence-Moon-Biedl Pseudo-Refsum CLINICAL FEATURES • Retinitis pigmentosa • Deafness • Obesity • Retinits pigmentosa • Obesity • Polydactyly • Hypogonnadism • Retinitis pigmentosa • Ataxia • Muscle wasting
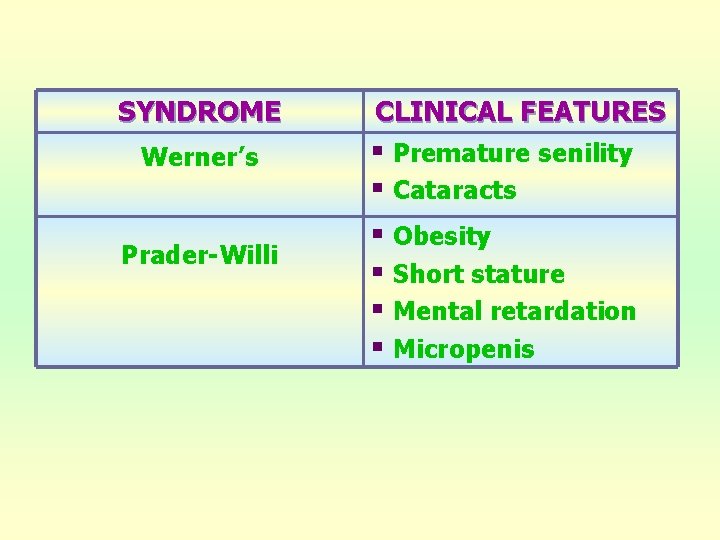

SYNDROME Werner’s Prader-Willi CLINICAL FEATURES § Premature senility § Cataracts § Obesity § Short stature § Mental retardation § Micropenis

TYPE II CONTD. . . § THE CLINICALPRESENTATION VARIES GREATLY: I. THEY MANIFEST DM AFTER THE DEVELOPMENT OF COMPLICTIONS ( E. G. RE TIOPATHY ). II. MAY HAVE SIGNIFICANT POLYRIA , POLYDIPSIA , EASY FATIGUABILITY ETC. III. MAY BE FOUND BY CHANCE ON ROUTINE examination

TYPE II CONTD. . . § MILDTO AMRKED OBES IS PRESENT IN 80% TYPE II AT THE TIME OF DIAGNOSIS. § OBESITY IS A MAJOR RISK FACTOR RROBABLY DUE TO THE DECREASE INSULIN RECEPTOR DENSITY AND ABNORMAL COUPLING OF RECEPTOR TO METABOLIC PROCESS THAT OCCUR IN THE OBESE STATE

§MOSTPATIENTS ARE DIAGNOSED AFTER THE AGE OF 40 YEARS §OLD NAME - MANTURIY ONSET D. M.

A GTT IS DOME FOR THOSE IN THE IMPAIRED TOLERANCE RANGE COMMON CAUSES OF TRANSIENT CARBOHYDRTE INTOLERANCES : PHYSICAL OR EMOTIONAL STRESS INFECTION UNDER NUTRITION BED REST TRAUMA

NONOREGNANT ADULITS

PLASMA OTHER CRITERIA GLUCOSE ( mg/d. I) RANDOM > 200 CLASSIC SIGNS AND SYMPTOMS OR FASTING >126 ON AT LEST 2 OCCASIONS OR FASTING < 126 SUSTAINED ELEVATED LASMA GLUCOSE DURING AT LEAST 2 OGTTs

Dx OF IMPAIRED GLUCOSE TOLERANCE IN ADULTS* OGTT SAMPLE PLASMA GLUCOSE VALUES ( mg/d. I) FASTING < 126 2 HOUR 126 - 199 INTERVENING *NONPREGANT >200

WHO DIABETIC ASTING > 8 MMOL /L HRS >11 MMOL / L IMPAIRED GT 6 - 8 MMOL / L 8 – 11 MMOL / L

Key Points v. Diabetes mellitus in older adults is the commonest metabolic disorder in mainstream clinical practice v. The disorder present an interplay between metabolic dysfunction, vasculopathy and the ageing process

vcardinal features with enable clinicians to focus diabetes risk associated with functional decline, visual cognitive disorder depression, and vulnerability to hypoglycemia

v. Interventions based on both vascular and rehabilitation models complement the metabolic approach to restructuring diabetes care for elderly

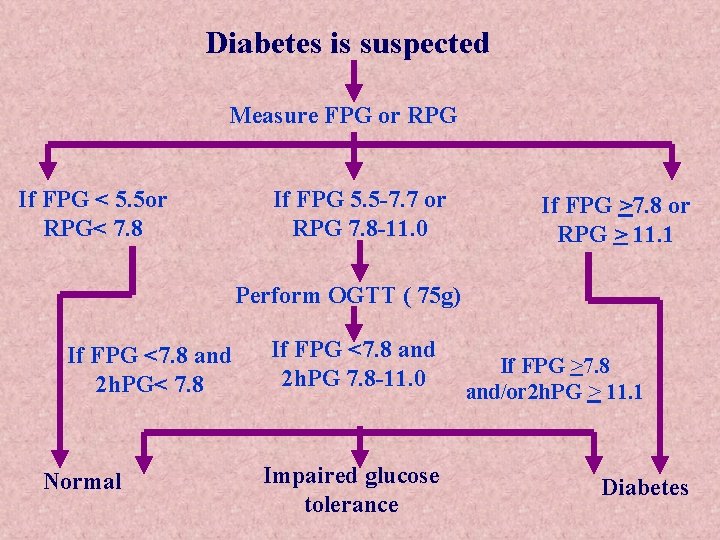
Diabetes is suspected Measure FPG or RPG If FPG < 5. 5 or RPG< 7. 8 If FPG 5. 5 -7. 7 or RPG 7. 8 -11. 0 If FPG >7. 8 or RPG > 11. 1 Perform OGTT ( 75 g) If FPG <7. 8 and 2 h. PG< 7. 8 Normal If FPG <7. 8 and 2 h. PG 7. 8 -11. 0 Impaired glucose tolerance If FPG >7. 8 and/or 2 h. PG > 11. 1 Diabetes
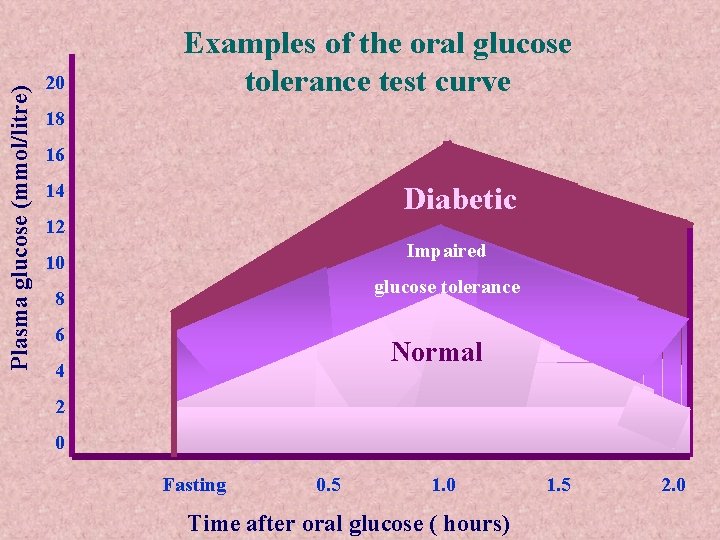
Plasma glucose (mmol/litre) 20 Examples of the oral glucose tolerance test curve 18 16 14 Diabetic 12 Impaired 10 glucose tolerance 8 6 Normal 4 2 0 Fasting 0. 5 1. 0 Time after oral glucose ( hours) 1. 5 2. 0


GLUCOSE INTOLERANCE DEVELOPS DURING PREGNANCY OCCURS IN 2% OF PRENGNANT WOMEN ONSET USUALLY IN 2 nd OR 3 rd TRIMESTER INCREASED FEATAL SIZE AND MORBIDITY GTT USUALLY RETURNS TO NORMAL AFTER PARTURITION

CRIERION FOR POSITIVE SCREEN 1 HOUR PLASMA GLUCOSE > 140 mg / d. I If POSITIVE SCREEN Dx TEST INDICATED

1. DISEASES PRODUCING ANTI – INSULIN HOSRMONES. PHAEOCHROMOCYTOMA CUSHING ‘S ACHROMEGALY GLUCAGONOMA THROTOXICOSIS
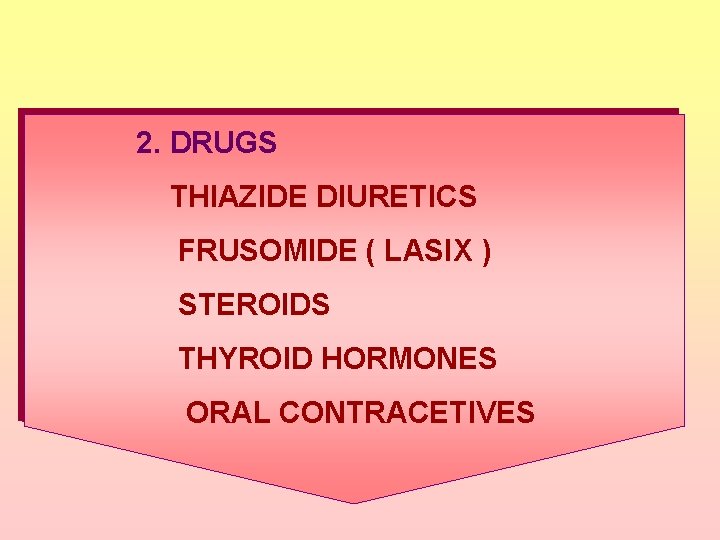
2. DRUGS THIAZIDE DIURETICS FRUSOMIDE ( LASIX ) STEROIDS THYROID HORMONES ORAL CONTRACETIVES
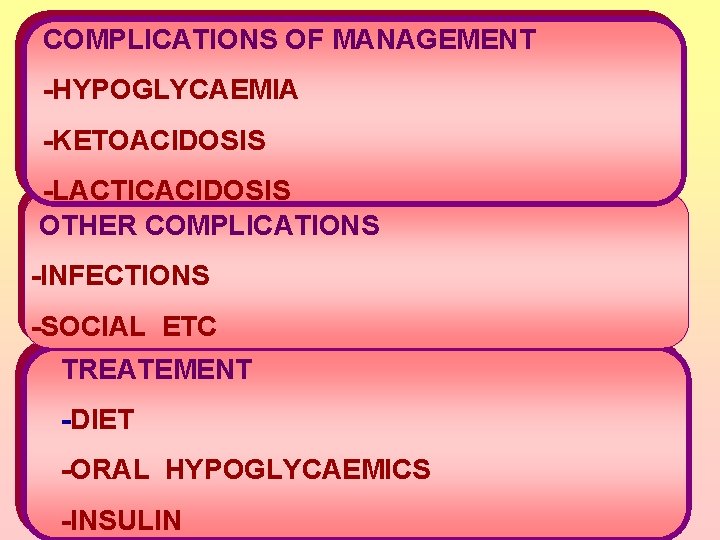

COMPLICATIONS OF MANAGEMENT -HYPOGLYCAEMIA -KETOACIDOSIS -LACTICACIDOSIS OTHER COMPLICATIONS -INFECTIONS -SOCIAL ETC TREATEMENT -DIET -ORAL HYPOGLYCAEMICS -INSULIN

3. ASSOCIATED WITH MANY OTHER DISEASES EG. MUSLAR DYSTROPHIES DOWN ‘S KLEINFELTER’S TURNER ‘S FREDERICK’ S ATAXIA GLYCOGEN STORAGE DISEASE
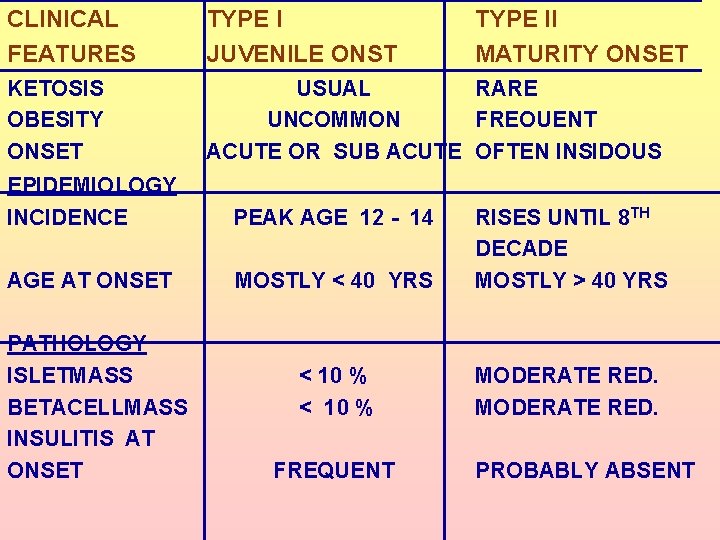
CLINICAL FEATURES TYPE I JUVENILE ONST TYPE II MATURITY ONSET KETOSIS OBESITY ONSET USUAL RARE UNCOMMON FREOUENT ACUTE OR SUB ACUTE OFTEN INSIDOUS EPIDEMIOLOGY INCIDENCE PEAK AGE 12 - 14 AGE AT ONSET MOSTLY < 40 YRS RISES UNTIL 8 TH DECADE MOSTLY > 40 YRS < 10 % MODERATE RED. PATHOLOGY ISLETMASS BETACELLMASS INSULITIS AT ONSET FREQUENT PROBABLY ABSENT
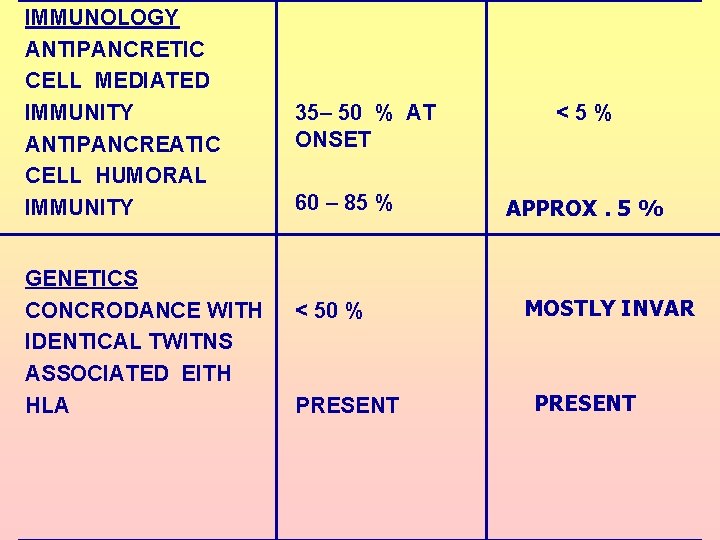
IMMUNOLOGY ANTIPANCRETIC CELL MEDIATED IMMUNITY ANTIPANCREATIC CELL HUMORAL IMMUNITY GENETICS CONCRODANCE WITH IDENTICAL TWITNS ASSOCIATED EITH HLA 35– 50 % AT ONSET 60 – 85 % < 50 % PRESENT <5% APPROX. 5 % MOSTLY INVAR PRESENT

THE PRESENCE OF COMMONLY ASSOCIATAED CONDITIONS SHOULD BE EVALUATED EG: - • • OBESITY HYPERTENSION • HYPERLIPIDAEMIA • MACROVASCULARDISEASE

AT DIAGNOSIS , A COMPLETE HISTORY AND PHYSICAL EXAMINATION ARE ANDATORY AS MACROVASCLUAR ISEASE , AND SOMETIONS MICROVASCULAR COMPLICATIONS ARE RESENT AT DIAGNSIS OF NIDDM

HETEROGENEOUS DISORDER CHARACTERIZED BY : DEFICIENT INSULIN SECRETION § INSULIN RESISTANCE

• * Mature onset diabetes of the young is inherited in an autsomal dominant manner and associated with 8 cell dysfunction. * Environmental factors important for NIDDM include physical inactivity, excessive consumption of food leading to obesity stress and some drugs

Practice points • * Non-insulin dependent diabetes mellitus ( NIDDM ) is a heterogeneous disease in which a number of genetic and environmental factors interact to cause diabetes • * Maternally inhented diabetes and deafness is a distinct subtype of NIDDM
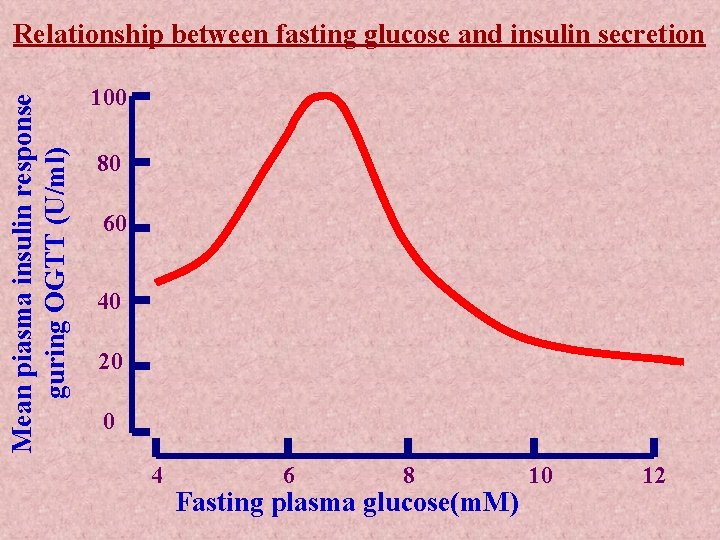
Mean piasma insulin response guring OGTT (U/ml) Relationship between fasting glucose and insulin secretion 100 80 60 40 20 0 4 6 8 Fasting plasma glucose(m. M) 10 12

HETEROGENEOUS DISORDER CHARACTERIZED BY : § DEFICIENT INSULIN SECRETION INSULIN RESISTANCE

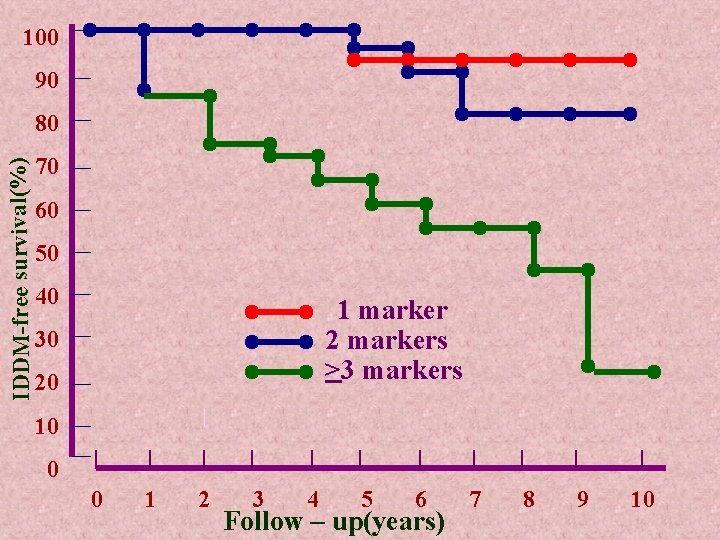
100 90 IDDM-free survival(%) 80 70 60 50 40 1 marker 2 markers >3 markers 30 20 10 0 0 1 2 3 4 5 6 Follow – up(years) 7 8 9 10

- Slides: 75