Diabetes Management in the Hospital Bruce W Bode

Diabetes Management in the Hospital Bruce W. Bode, MD, FACE Atlanta Diabetes Associates Atlanta, Georgia
Diabetes in Hospitalized Patients 1997 • 3. 5 Million US Hospitalizations 15% of Admissions • 14 Million Hospital Days 20% of All Hospital Days • 36% First Diagnosed in Hospital 66% No Documentation by Physician 27% Labeled Hyperglycemia 2% Diagnosed on Chart

Diabetes in Hospitalized Patients 1997 Costs • $23, 500 Each Diabetes Patient vs. $12, 200 for Non-Diabetes Patient • 60% of All Diabetes-Related Costs • Only 5% DKA, HHNKC • 48% Diabetes Complications • 52% Other Conditions

Diabetes in Hospitalized Patients Reason for Higher Costs l Higher Rate of Hospitalization l Longer Stays l More Procedures, Medications l Chronic Complications l More Arteriosclerotic Disease l More Infections l Complicated Pregnancies

Diabetes in Hospitalized Patients • High-risk for Bacterial Infection – Surgery – Catheters – Intravenous Access – Anaesthesia l Problems with wound healing l Problems with tissue and organ perfusion

Infections in Diabetes l One BG >220 mg/dl results in 5. 8 times increase in nosocomial infection rate l Two hours hyperglycemia results in impaired WBC function for weeks Pomposelli, New England Deaconess, J Parenteral and Enteral Nutrition 22: 77 -81, 1998

TPN In Diabetes VA Cooperative Trial l Benefit Negated l Increased Infections l Related to Hyperglycemia Buzby et al. NEJM 325: 525 -531, 1991

Side Effects of BG >200 mg/dl l Reduced Intravascular Volume l Dehydration l Electrolyte Fluxes l Impaired WBC Function l Immunoglobulin Inactivation l Complement Disabling l Increased Collagenase, Decreased Wound Collagen

Psychology of Diabetes in Hospital l Patients expect good glycemic control as part of hospital care l They strive for recommended goals at home l Difficult to understand staff’s casual approach to BG’s >150

Evidence for Immediate Benefit of Normoglycemia in Hospitalized Patients l Numerous Publications on in Vitro Evidence – Neutrophil Dysfunction – Complement Inhibition – Altered Redox State (Pseudohypoxia) – Glucose Rich Edema as Culture Media l Six Recent Clinical Publications supporting good glucose control in the hospital setting
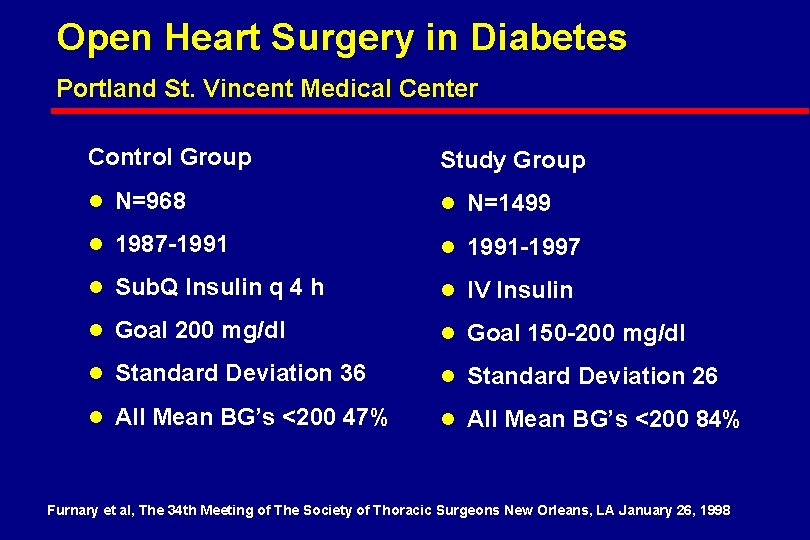
Open Heart Surgery in Diabetes Portland St. Vincent Medical Center Control Group Study Group l N=968 l N=1499 l 1987 -1991 l 1991 -1997 l Sub. Q Insulin q 4 h l IV Insulin l Goal 200 mg/dl l Goal 150 -200 mg/dl l Standard Deviation 36 l Standard Deviation 26 l All Mean BG’s <200 47% l All Mean BG’s <200 84% Furnary et al, The 34 th Meeting of The Society of Thoracic Surgeons New Orleans, LA January 26, 1998
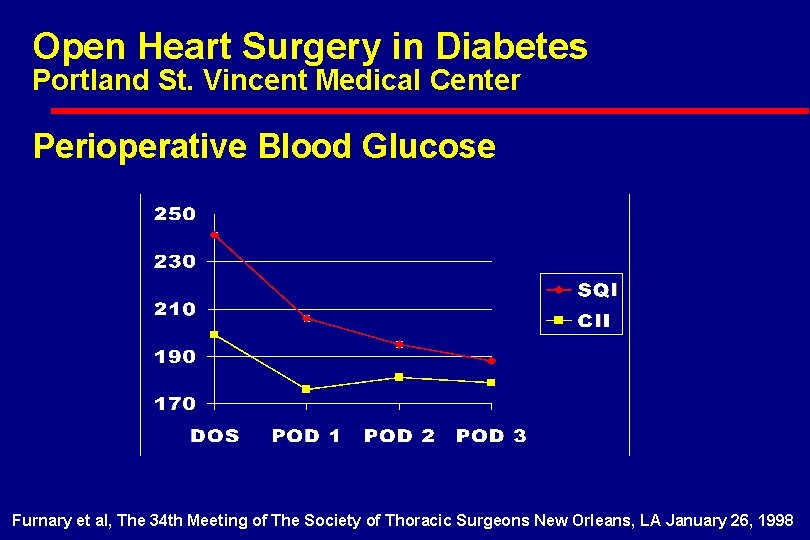
Open Heart Surgery in Diabetes Portland St. Vincent Medical Center Perioperative Blood Glucose Furnary et al, The 34 th Meeting of The Society of Thoracic Surgeons New Orleans, LA January 26, 1998
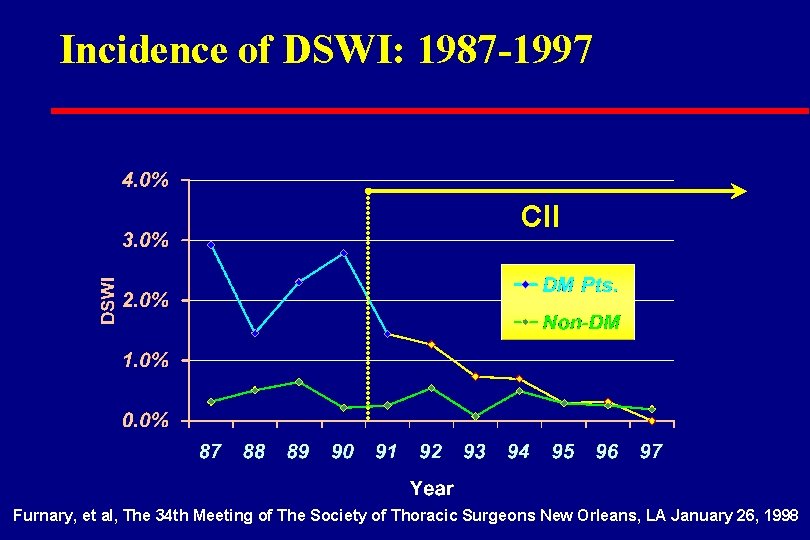
Incidence of DSWI: 1987 -1997 CII Furnary, et al, The 34 th Meeting of The Society of Thoracic Surgeons New Orleans, LA January 26, 1998
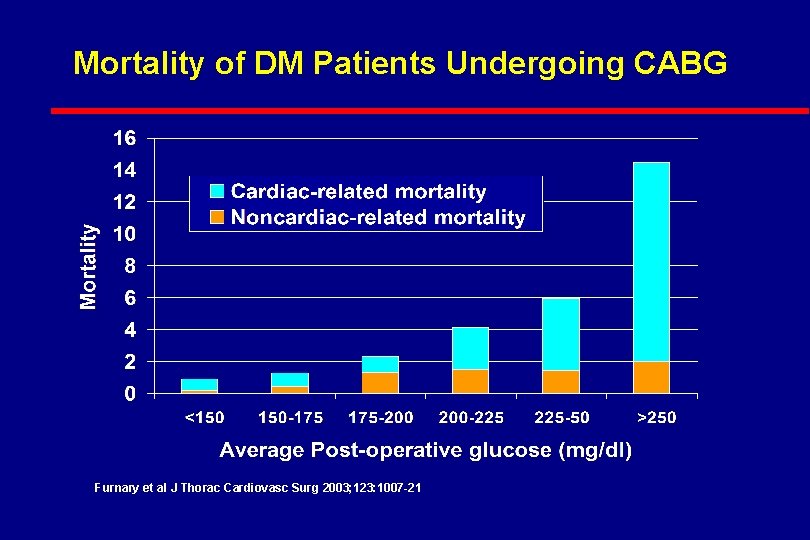
Mortality of DM Patients Undergoing CABG Furnary et al J Thorac Cardiovasc Surg 2003; 123: 1007 -21

Glycemic Threshold in CABG Portland data suggest BG: < 150 mg/dl for mortality < 175 mg/dl for infection < 125 mg/dl for atrial fibrillation Furnary et al J Thorac Cardiovasc Surg 2003; 123: 1007 -21

ICU Survival l 1548 Patients (mostly OHS pts. ) l All with BG >200 mg/dl l Randomized into two groups – Maintained on IV insulin – Conventional group (BG 180 -200) – Intensive group (BG 80 -110) l Conventional Group had 1. 74 X mortality Van den Berghe et al, NEJM 2001; 345(19): 1359

ICU IV Insulin Protocol l If > 100 mg/dl, 2 U/h If > 200 mg/dl, 4 U/h l If > 140 mg/dl, increase by 1 – 2 U/h l If 121 to 140 mg/dl, increase by 0. 5 – 1 U/h l If 111 to 120 mg/dl, increase by 0. 1 – 0. 5 U/h l If 81 to 110 mg/dl, no change l If 61 to 80 mg/dl, change back to prior rate Van den Berghe et al, NEJM 2001; 345(19): 1359
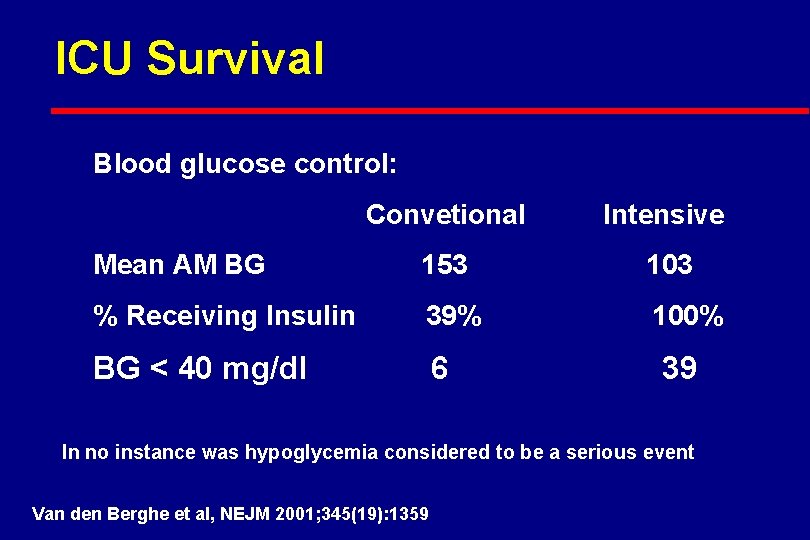

ICU Survival Blood glucose control: Convetional Intensive Mean AM BG 153 103 % Receiving Insulin 39% 100% BG < 40 mg/dl 6 39 In no instance was hypoglycemia considered to be a serious event Van den Berghe et al, NEJM 2001; 345(19): 1359
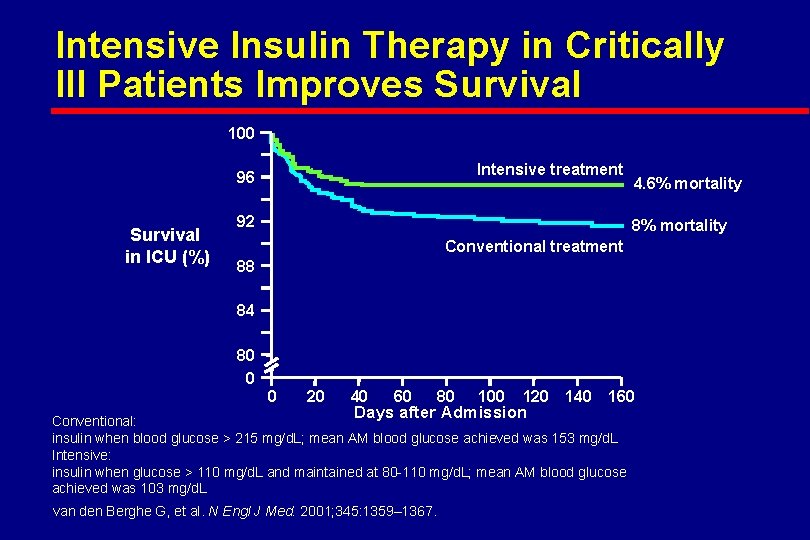
Intensive Insulin Therapy in Critically Ill Patients Improves Survival 100 Intensive treatment 96 Survival in ICU (%) 92 4. 6% mortality 8% mortality Conventional treatment 88 84 80 0 0 20 40 60 80 100 120 140 Days after Admission 160 Conventional: insulin when blood glucose > 215 mg/d. L; mean AM blood glucose achieved was 153 mg/d. L Intensive: insulin when glucose > 110 mg/d. L and maintained at 80 -110 mg/d. L; mean AM blood glucose achieved was 103 mg/d. L van den Berghe G, et al. N Engl J Med. 2001; 345: 1359– 1367.
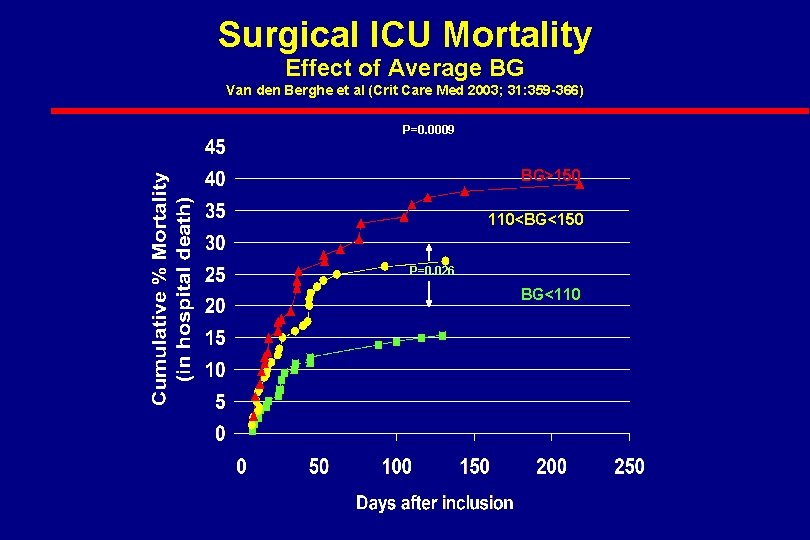
Surgical ICU Mortality Effect of Average BG Van den Berghe et al (Crit Care Med 2003; 31: 359 -366) P=0. 0009 BG>150 110<BG<150 P=0. 026 BG<110
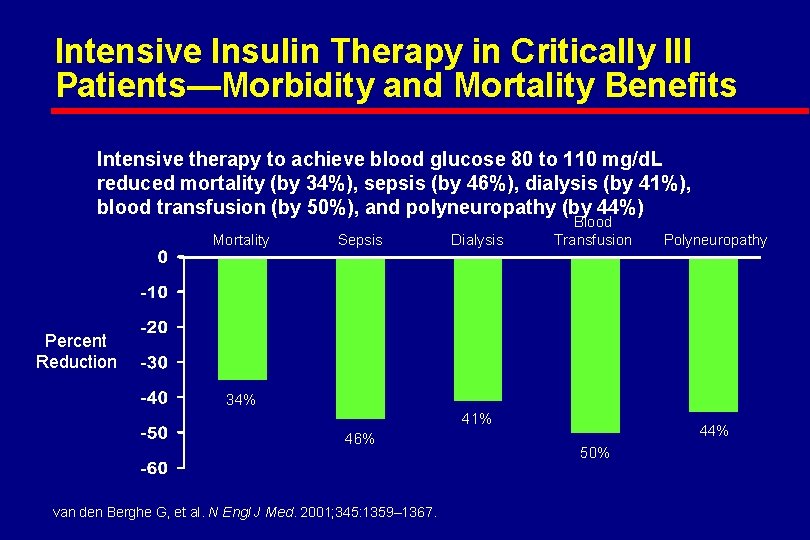
Intensive Insulin Therapy in Critically Ill Patients—Morbidity and Mortality Benefits Intensive therapy to achieve blood glucose 80 to 110 mg/d. L reduced mortality (by 34%), sepsis (by 46%), dialysis (by 41%), blood transfusion (by 50%), and polyneuropathy (by 44%) Mortality Sepsis Dialysis Blood Transfusion Polyneuropathy Percent Reduction 34% 41% 46% van den Berghe G, et al. N Engl J Med. 2001; 345: 1359– 1367. 44% 50%

Glycemic threshold in Surgical ICU l BG < 110 mg/dl Van den Berghe et al Crit Care Med 2003; 31(2): 359 -66 Finney SJ et al JAMA 2003; 290(15): 2041 -47

What About Medical Patients?

DIGAMI Study Diabetes, Insulin Glucose Infusion in Acute Myocardial Infarction(1997) l Acute MI With BG > 200 mg/dl l Intensive Insulin Treatment l IV Insulin For > 24 Hours l Four Insulin Injections/Day For > 3 Months l Reduced Risk of Mortality By: 28% Over 3. 4 Years 51% in Those Not Previous Diagnosed Malmberg BMJ 1997; 314: 1512
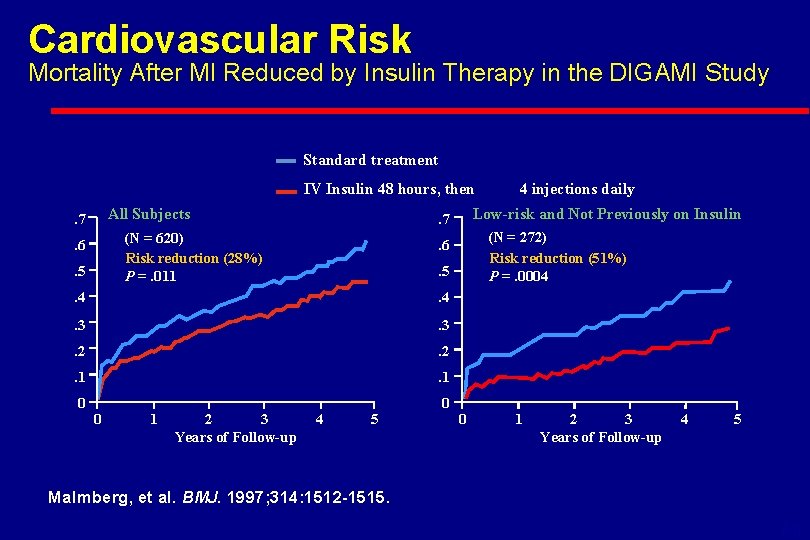
Cardiovascular Risk Mortality After MI Reduced by Insulin Therapy in the DIGAMI Study Standard treatment IV Insulin 48 hours, then All Subjects . 7. 5 . 5. 4 . 3 . 2 . 1 0 0 1 2 3 Years of Follow-up (N = 272) Risk reduction (51%) P =. 0004 . 6 . 4 0 Low-risk and Not Previously on Insulin . 7 (N = 620) Risk reduction (28%) P =. 011 . 6 4 5 4 injections daily 0 1 2 3 Years of Follow-up 4 5 Malmberg, et al. BMJ. 1997; 314: 1512 -1515. 6 -11

Glycemic Threshold in Acute MI and Intervention (PTCA) l DIGAMI supports BG < 180 mg/dl l Minimal other data: - PTCA reflow better with BG 159 than 209 mg/dl Malmberg BMJ 1997; 314: 1512 Iwakura K: JACC 2003; 41: 1 -7

Other Medical Conditions l Infection data supports BG < 130 mg/dl Hartford ICU study 125 mg/dl vs 179 mg/dl 10 X decrease in infections l Stroke data supports BG < 140 mg/dl l Pregnancy data supports BG < 100 mg/dl

Stamford CT ICU Study (Retrospective): Description of Patient Subgroups (N = 1826) l Cardiac (medical): 28. 6% (540) l Pulmonary: 15. 8% (289) l Septic Shock: 5. 0% (92) l Other Medical: 14. 9% (272) l Neurological: 13. 2% (241) l Surgical: 7. 1% (313) l Trauma: 4. 3% (79) Krinsley JS: Mayo Clin Proc 2003; 78: 1471 -1478
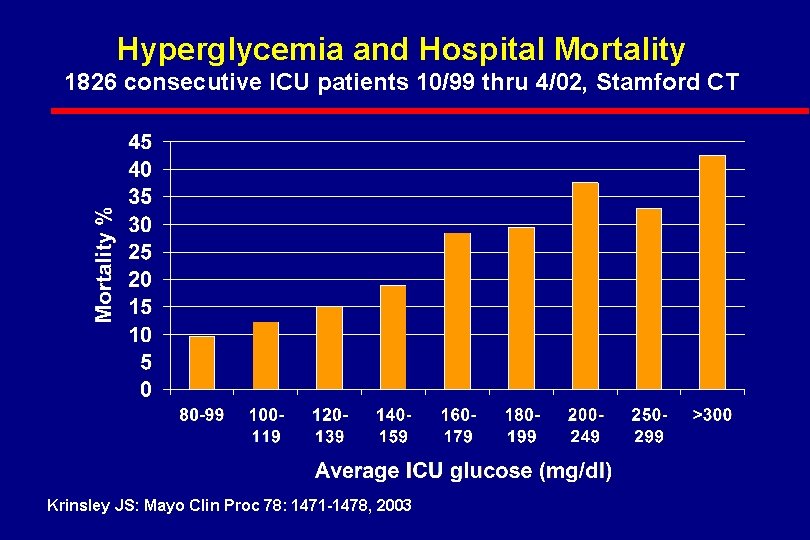
Hyperglycemia and Hospital Mortality 1826 consecutive ICU patients 10/99 thru 4/02, Stamford CT Krinsley JS: Mayo Clin Proc 78: 1471 -1478, 2003

Target blood glucose in mg/d. L l 80 – 110 in Surgical ICU patients l 90 – 140 in other Surgical and Medical Patients l 70 – 100 in Pregnancy

Hospital Targets for Glucose AACE and ADA Guidelines: Dec 2003 New 80– 110 mg/d. L ICU 110– 180 mg/d. L other units Modify if: cardiac disease (unstable) hypoglycemic unawareness recurrent hypoglycemia

Conclusion All hospital patients should have normal glucose

Insulin only The most powerful agent we have to control glucose
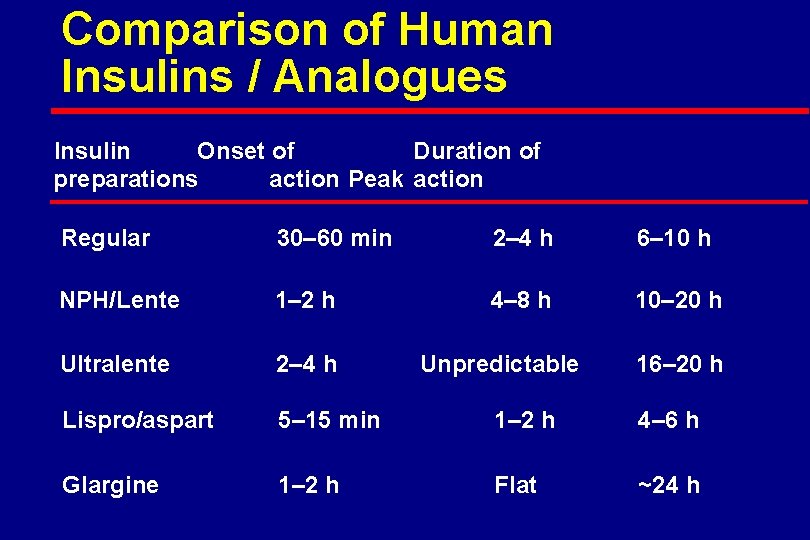
Comparison of Human Insulins / Analogues Insulin Onset of Duration of preparations action Peak action Regular 30– 60 min 2– 4 h 6– 10 h NPH/Lente 1– 2 h 4– 8 h 10– 20 h Ultralente 2– 4 h Lispro/aspart 5– 15 min 1– 2 h 4– 6 h Glargine 1– 2 h Flat ~24 h Unpredictable 16– 20 h
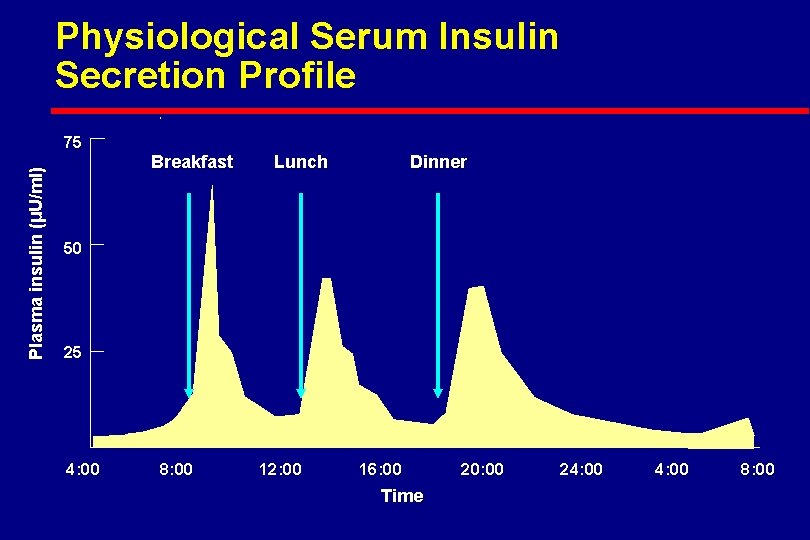
Physiological Serum Insulin Secretion Profile Plasma insulin (µU/ml) 75 Breakfast Lunch Dinner 50 25 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

Methods For Managing Hospitalized Persons with Diabetes l Continuous Variable Rate IV Insulin Drip Major Surgery, NPO, Unstable, MI, DKA, Hyperglycemia, Steroids, Gastroparesis, Delivery, etc l Basal / Bolus Therapy (MDI) when eating
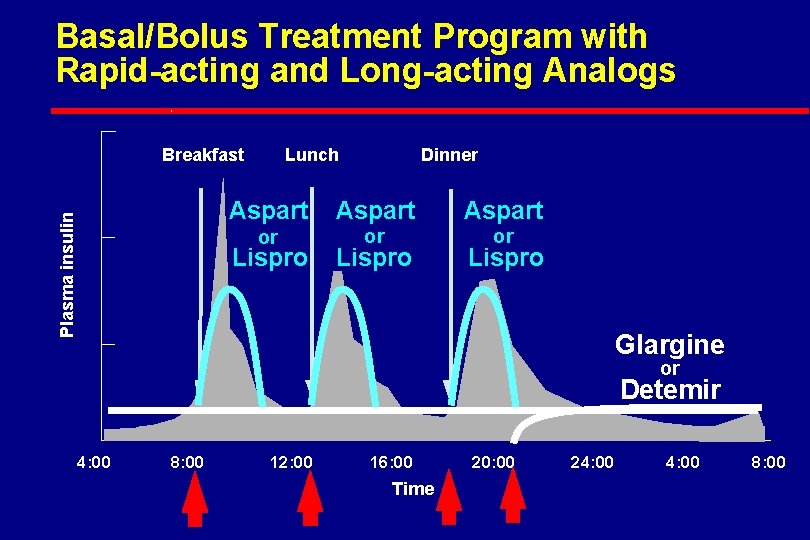
Basal/Bolus Treatment Program with Rapid-acting and Long-acting Analogs Plasma insulin Breakfast Lunch Dinner Aspart or or or Lispro Glargine or Detemir 4: 00 8: 00 12: 00 16: 00 Time 20: 00 24: 00 8: 00

Threshold blood glucose in mg/d. L for starting IV insulin infusion l Peri-operative care: > 140 l Surgical ICU care: > 110 - 140 * l Non-surgical illness: > 140 - 180 * * l Pregnancy > 100 * Van den Berghe’s study supports 110; Finney’s study supports 145 * * If drip indication is failure of SQ therapy, use 180 ; if indication is specific condition ( DM 1/ NPO, MI, etc ), use 140

The Ideal IV Insulin Protocol l Easily ordered (signature only) l Effective (Gets to goal quickly) l Safe (Minimal risk of hypoglycemia) l Easily implemented l Able to be used hospital wide

Essentials of a good IV Insulin Algorithm l Easily implemented by nursing staff l Able to seek BG range via: - Hourly BG monitoring - Adjusts to the insulin sensitivity of the patient
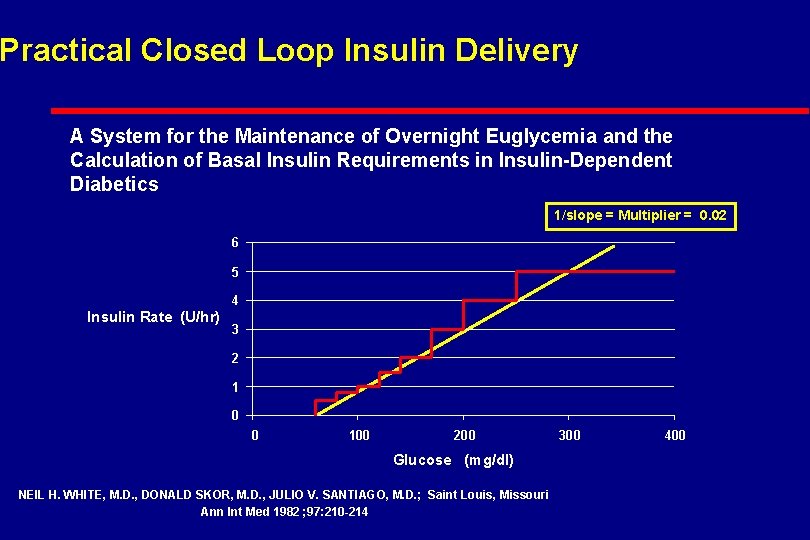
Practical Closed Loop Insulin Delivery A System for the Maintenance of Overnight Euglycemia and the Calculation of Basal Insulin Requirements in Insulin-Dependent Diabetics 1/slope = Multiplier = 0. 02 6 5 4 Insulin Rate (U/hr) 3 2 1 0 0 100 200 Glucose (mg/dl) NEIL H. WHITE, M. D. , DONALD SKOR, M. D. , JULIO V. SANTIAGO, M. D. ; Saint Louis, Missouri Ann Int Med 1982 ; 97: 210 -214 300 400

Continuous Variable Rate IV Insulin Drip l Mix Drip with 125 units Regular Insulin into 250 cc NS l Starting Rate Units / hour = (BG – 60) x 0. 02 where BG is current Blood Glucose and 0. 02 is the multiplier l Check glucose every hour and adjust drip l Adjust Multiplier to keep in desired glucose target range (100 to 140 mg/dl)

Continuous Variable Rate IV Insulin Drip l Adjust Multiplier (initially 0. 02) to obtain glucose in target range 100 to 140 mg/d. L If BG > 140 mg/d. L, increase by 0. 01 If BG < 100 mg/d. L, decrease by 0. 01 If BG 100 to 140 mg/d. L, no change in Multiplier l If BG is < 80 mg/d. L, Give D 50 cc = (100 – BG) x 0. 4 l Give continuous rate of Glucose in IVF’s l Once eating, continue drip till 2 hours post SQ insulin
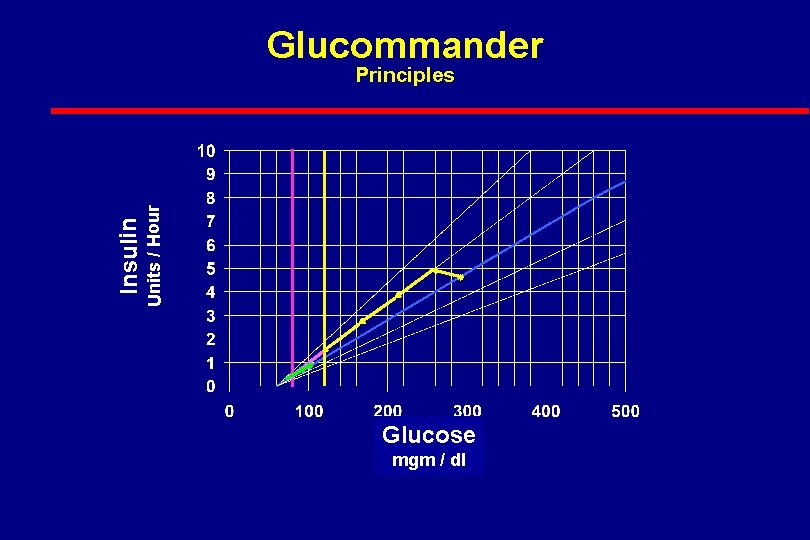
Glucommander Units / Hour Insulin Principles Glucose mgm / dl

Glucose Management System

Glucommander l Based on 15 Year Experience with a Computer Based Algorithm for the Administration of IV Insulin l Developed for Marketing by Mini. Med and Roche l GMS System l Shelved Pending FDA Approval of IV Use of Insulin l Useful and Safe for Any Application of IV Insulin
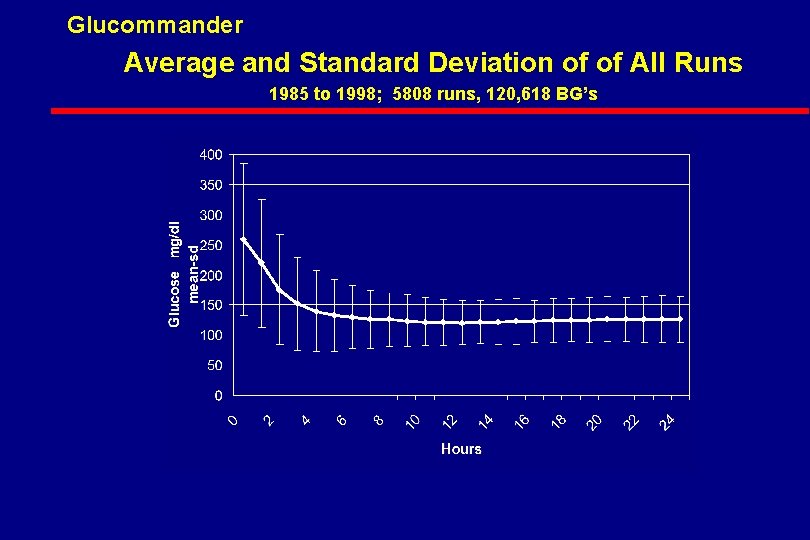
Glucommander Average and Standard Deviation of of All Runs 1985 to 1998; 5808 runs, 120, 618 BG’s
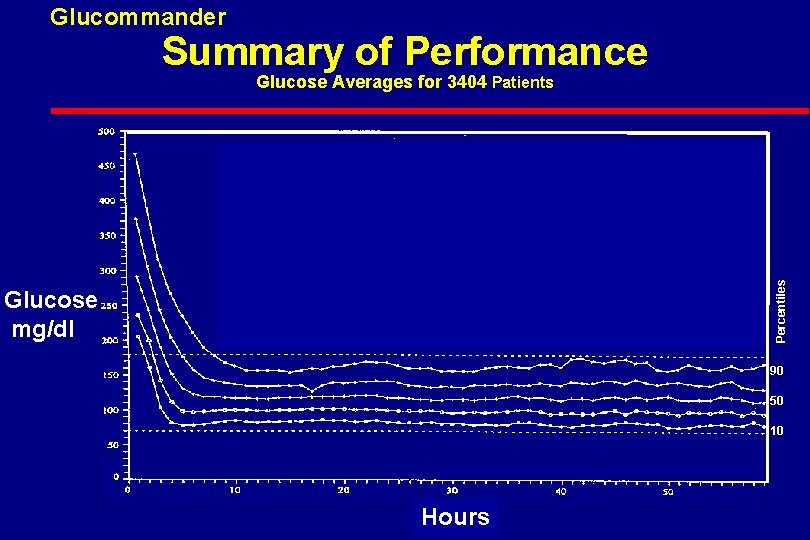
Glucommander Summary of Performance . Percentiles Glucose mg/dl Percentiles Glucose Averages for 3404 Patients 90 50 10 Hours

Converting to SC insulin l If More than 0. 5 u/hr IV insulin required with normal BG, start long-acting insulin (glargine) l Must start SC insulin at least 2 hours before stopping IV insulin l Some centers start long-acting insulin on initiation of IV insulin or the night before stopping the drip
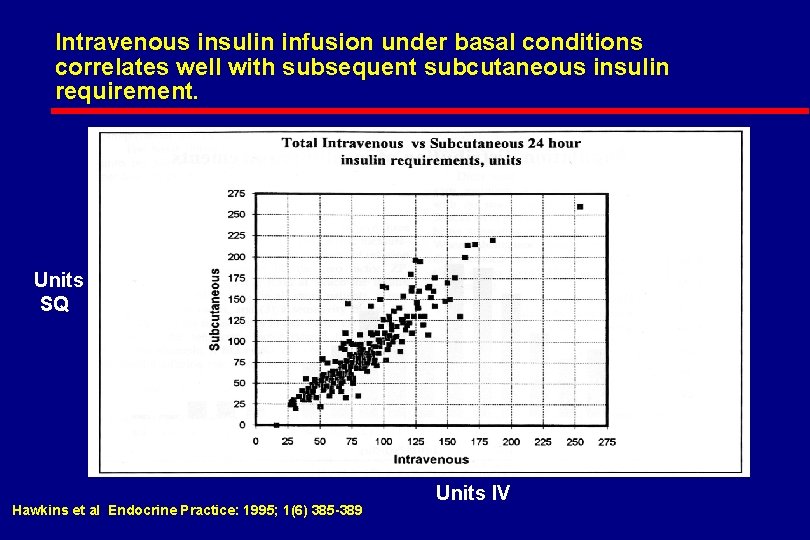
Intravenous insulin infusion under basal conditions correlates well with subsequent subcutaneous insulin requirement. Overwrite Units SQ Hawkins et al Endocrine Practice: 1995; 1(6) 385 -389 Units IV

Converting to SC insulin l Establish 24 hr Insulin Requirement – Extrapolate from average over last 6 -8 hours if stable l Give One-Half Amount As Basal l Give p. c. Boluses Based on CHO Intake – Start at CHO/Ins 1 CHO = 1. 5 units Rapid-acting l Monitor a. c. tid, hs, and 3 am l Supplement All BG >140 mg/dl – (BG-100)/(1700/Daily Insulin Requirement)

The Accurate Insulin Management (AIM) Formulae • Prescription for insulin therapy includes: • Basal Insulin (BI) • Carbohydrate-to-Insulin Ratio (CIR) • Correction Factor (CF) • 1801 Records from Pump Patients Studied • Data from best-controlled of 591 pump patients • Analyzed for optimum parameters • Resulting formulae used as model for others • The Accurate Insulin Management (AIM) formulae Davidson PC et al Diabetes Tech & Ther 2003; 5: 327

The Accurate Insulin Management (AIM) Formulae Davidson PC et al Diabetes Tech & Ther 2003; 5: 327
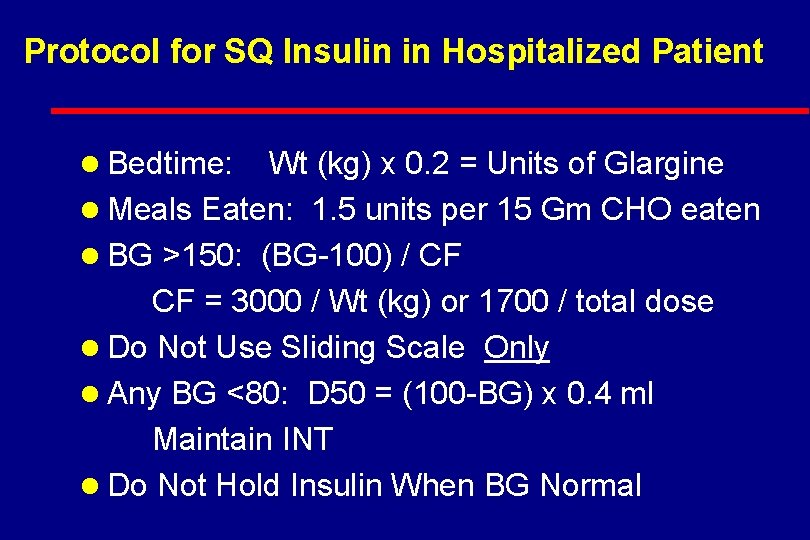
Protocol for SQ Insulin in Hospitalized Patient l Bedtime: Wt (kg) x 0. 2 = Units of Glargine l Meals Eaten: 1. 5 units per 15 Gm CHO eaten l BG >150: (BG-100) / CF CF = 3000 / Wt (kg) or 1700 / total dose l Do Not Use Sliding Scale Only l Any BG <80: D 50 = (100 -BG) x 0. 4 ml Maintain INT l Do Not Hold Insulin When BG Normal

How to Initiate MDI l Starting dose = 0. 4 to 0. 5 x weight in kilograms l Bolus dose (aspart/lispro) = 20% of starting dose at each meal l Basal dose (glargine) = 40% of starting dose given at bedtime or anytime l Correction bolus = (BG - 100)/ Correction Factor, where CF = 1700/total daily dose

How to Initiate MDI l Starting dose = 0. 45 x wgt. in kg l Wt. is 80 kg; 0. 45 x 80 = 36 units l Bolus dose (aspart / lispro) = 20% of starting dose at each meal; 0. 2 x 36 = 7 units ac (tid) l Basal dose (glargine) = 40% of starting dose at HS; 0. 4 x 36 = 14 units at HS l Correction bolus = (BG - 100)/ CF, where CF = 1700/total daily dose; CF = 50

Correction Bolus Formula Current BG - Ideal BG Glucose Correction factor Example: – Current BG: – Ideal BG: 250 mg/dl 100 mg/dl – Glucose Correction Factor: 50 mg/dl 250 - 100 =3. 0 u 50

Piedmont Diabetes Plan What Can We Do For Patients Admitted To Hospital? l NPO Pathway For All Diabetes Patients l Finger Stick BG ac qid on ALL Admissions l Check All Steroid Treated Patients l Diagnose Diabetes FBG >126 mg/dl Any BG >200 mg/dl

Piedmont Diabetes Plan What Can We Do For Patients Admitted To Hospital? l Document Diagnosis in Chart Hyperglycemia Is Diabetes Until Proven Bring to All Physician’s Attention Note on Problem List and Face Sheet l Check Hemoglobin A 1 C l Hold Metformin; Hold TZD with CHF, Liver Dysfunction l Start Insulin in All Hospitalized Patients with BG >140 mg/dl

Piedmont Diabetes Plan What Can We Do For Patients Admitted To Hospital? l Get Diabetes Education Consult l Instruct Patient in Monitoring and Recording See That Patient Has Meter on Discharge l Decide on Case Specific Program for Discharge l Arrange Early F/U with PCP

Protocol for Insulin in Hospitalized Patient l Treat Any Patient With BG >140 mg/dl With Insulin – Treat Any BG >140 mg/dl with Rapid-acting Insulin (BG-100) / (3000 / wt kg) or 1700 / total daily insulin – Treat Any Recurrent BG >180 mg/dl with IV Insulin if failing SC therapy or >140 mg/dl if NPO, acute MI, perioperative, ICU, or >100 mg/dl if pregnant l If More than 0. 5 u/hr IV Insulin Required with Normal BG Start Long Acting Insulin

Protocol for Insulin in Hospitalized Patient l Daily Total: Pre-Admission or Weight (#) x 0. 2 u – 40 % as Glargine (Basal) – 60% as Rapid-acting insulin (Bolus) • Give in Proportion to Meal’s CHO Eaten l BG >140 mg/dl: (BG-100) / CF CF = 1700 / Total Daily Insulin Do Not Use Sliding Scale As Only Diabetes Management

Protocol for Insulin in Hospitalized Patient Treatment of Hypoglycemia l Any BG <80 mg/dl: D 50 = (100 -BG) x 0. 4 ml IV l Do Not Hold Insulin When BG Normal

Diabetes at Piedmont Hospital Conclusions 3 l Discharge Plan For BG Control l You Are the Link Between the Best Diabetes Care and the Patient l Use Your Diabetes Resources Diabetes Education Center Endocrinologists

The Paradigm for the Millenium Hyperglycemia: A Mortal Sin A blood glucose over 200 in a hospitalized patient causes increased morbidity and mortality. In the 21 st Century Neglecting a BG >200 Will Be Malpractice

Conclusion All hospital patients should have normal glucose

QUESTIONS l For a copy or viewing of these slides, contact l WWW. adaendo. com
- Slides: 67